Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: In the 1990s, Fink and Taylor proposed that catatonia is a syndrome, eventually influencing the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), which defined catatonia as a syndrome associated with neurodevelopmental disorders, psychotic disorders, depressive disorders, bipolar disorder, other medical conditions, or unspecified conditions. Although there are no well-designed randomized clinical trials for acute stuporous catatonia, the literature agrees that the first line of treatment is benzodiazepines, in particular lorazepam, administered by intravenous (IV), intramuscular, or oral routes. If treatment with benzodiazepines fails, electroconvulsive therapy (ECT) should be considered.
Rapid Development of Lorazepam Tolerance Within 48 Hours in an Adult With Intellectual Disability Who Presented With Stuporous Catatonia and Refused Electroconvulsive Therapy
To the Editor. In the 1990s, Fink and Taylor1 proposed that catatonia is a syndrome, eventually influencing the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5),2 which defined catatonia as a syndrome associated with neurodevelopmental disorders, psychotic disorders, depressive disorders, bipolar disorder, other medical conditions, or unspecified conditions. Although there are no well-designed randomized clinical trials for acute stuporous catatonia, the literature3-7agrees that the first line of treatment is benzodiazepines, in particular lorazepam, administered by intravenous (IV), intramuscular, or oral routes. If treatment with benzodiazepines fails, electroconvulsive therapy (ECT) should be considered.
Guidelines for the appropriate dosing of benzodiazepines are limited and do not define the maximum dose (above which signals failure). Furthermore, some case reports8,9 have described tolerance after long periods of treatment, resulting in larger lorazepam doses. ECT may help recover benzodiazepine response after tolerance develops.10
The patient presented here initially returned to baseline with 1 mg of oral lorazepam but rapidly developed benzodiazepine tolerance in a short period of 48 hours. To our knowledge, this type of rapid benzodiazepine tolerance has not been described.
Case report. A 47-year-old white man with a diagnosis of intellectual disability presented to a community hospital emergency department (ED) with mild cognitive confusion, fever, headache, and eye and throat pain. His brain imaging and lumbar puncture results were within normal limits. He was discharged home the same day with a diagnosis of streptococcal infection and provided antibiotics, which were discontinued the next day by the same ED doctor. The patient deteriorated with obvious stuporous catatonia and was admitted to the same ED for observation. He initially improved, but on the third day of hospitalization, he had a fever above 101°F. Despite treatment with broad-spectrum antibiotics, he remained febrile and was transferred to an internal medicine service in a university hospital. The fever disappeared with antibiotics. Medical etiologies of catatonia including infection and metabolic and neurologic diseases were ruled out by a comprehensive panel of medical tests ordered by the neurology and medicine departments. The tests included brain imaging (both computed tomography and magnetic resonance imaging), repeated spinal fluid analysis, and blood cultures, all of which were within normal limits. Therefore, we concluded that the catatonia was secondary to what the DSM-5 calls a neurodevelopmental disorder, namely intellectual disability. We have described 3 prior cases of catatonia in adults with intellectual disability.9
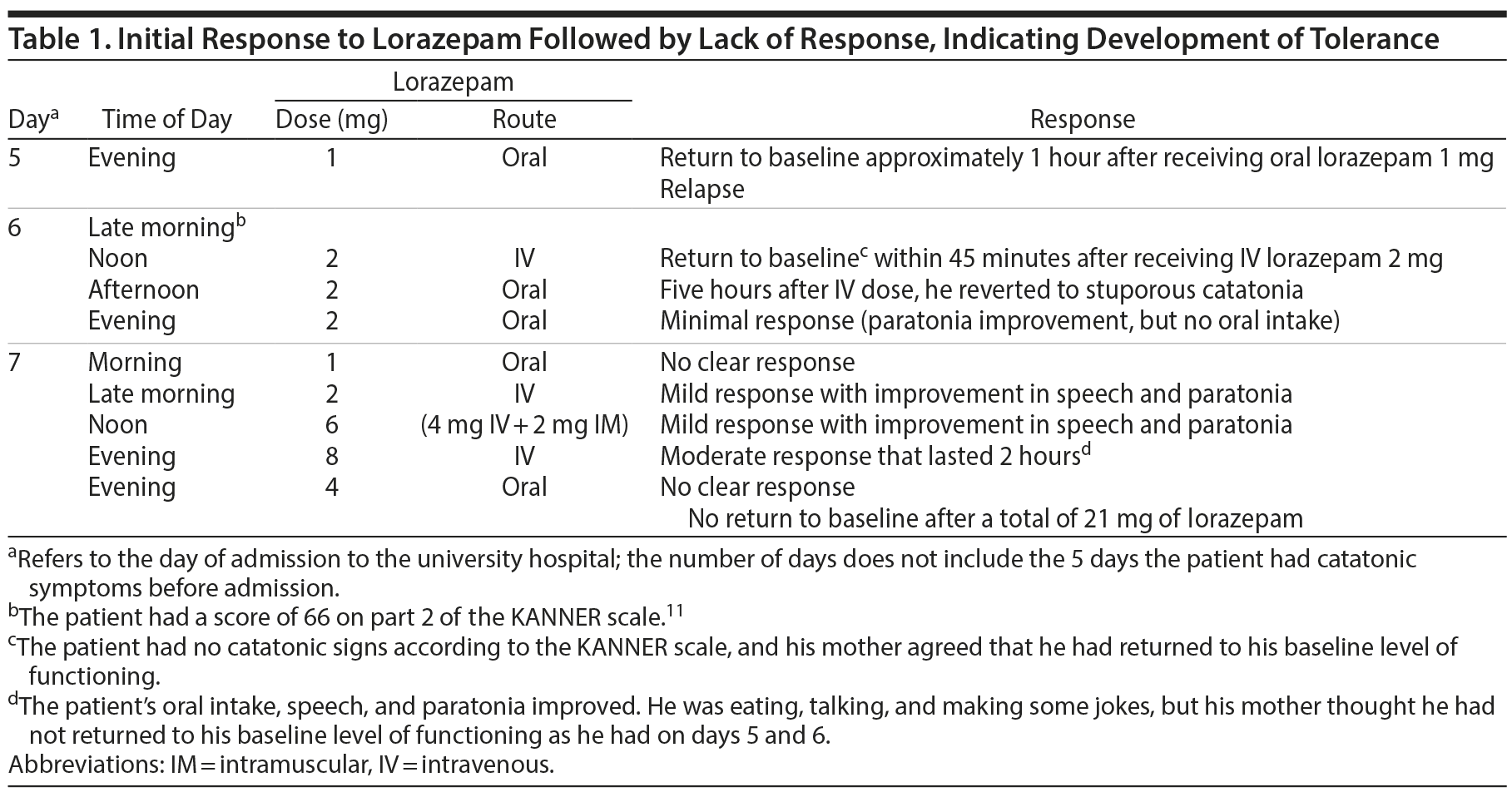
Due to agitation on the fifth evening of the university hospital admission, the patient received 1 mg of oral lorazepam and, according to his mother and the treating internist’s notes, returned to baseline within 30 minutes (Table 1). Unfortunately, lorazepam was not scheduled for administration that night, and he returned to a catatonic stupor. On the morning of day 6, after the internist consulted the psychiatry department, the first author (N.W.) assessed the patient, who met DSM-5 criteria for catatonia using the KANNER catatonia scale.11 The patient returned to baseline for a second time on day 6 after receiving lorazepam 2 mg IV but did not respond to a total of 21 mg of lorazepam on day 7. The patient did not receive another large dose of lorazepam after hospital day 7. It is important to stress that response to oral lorazepam on day 5 after 1 hour and to lorazepam IV on day 6 after 30 minutes suggests that these were specific responses, further demonstrated by relapse after lorazepam’s effect wore off, probably as the serum lorazepam peaks disappeared.
Throughout his 35 days of hospitalization at the university hospital, the patient had intermittent catatonia—some days with marked improvement and other days with complete stupor despite multiple other medication trials for catatonia. The family resisted ECT for weeks. On the day ECT was finally scheduled, the family decided against it because the patient was somewhat better, and they asked for a discharge. The patient was discharged on lorazepam 1 mg/d.
The literature has described benzodiazepine tolerance after multiple days or weeks8,9 but not within 48 hours. Our patient initially recovered with low doses: lorazepam 1 mg oral on day 5 and 2 mg IV on day 6, but the response was lost after no maintenance treatment. Clinicians should be aware that proper lorazepam maintenance is important to avoid relapse, as lorazepam tolerance may develop rapidly in some vulnerable patients such as ours.
References
1. Fink M, Taylor MA. Catatonia: A Clinician’s Guide to Diagnosis and Treatment. New York, NY: Cambridge University Press; 2003.
2. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
3. Fink M. Rediscovering catatonia: the biography of a treatable syndrome. Acta Psychiatr Scand suppl. 2013;127(441):1-47. PubMed CrossRef
4. Fricchione G. Catatonia: a new indication for benzodiazepines? Biol Psychiatry. 1989;26(8):761-765. PubMed CrossRef
5. Rosebush PI, Mazurek MF. Catatonia and its treatment. Schizophr Bull. 2010;36(2):239-242. PubMed CrossRef
6. Sienaert P, Dhossche DM, Vancampfort D, et al. A clinical review of the treatment of catatonia. Front Psychiatry. 2014;5:181. PubMed CrossRef
7. Weder ND, Muralee S, Penland H, et al. Catatonia: a review. Ann Clin Psychiatry. 2008;20(2):97-107. PubMed CrossRef
8. Manjunatha N, Saddichha S, Khess CR. Idiopathic recurrent catatonia needs maintenance lorazepam: case report and review. Aust N Z J Psychiatry. 2007;41(7):625-627. PubMed CrossRef
9. White M, Maxwell E, Milteer WE, et al. Catatonia in older adult individuals with intellectual disabilities. Case Rep Psychiatry. 2015;2015:120617. PubMed CrossRef
10. Petrides G, Divadeenam KM, Bush G, et al. A synergism of lorazepam and electroconvulsive therapy in the treatment of catatonia. Biol Psychiatry. 1997;42(5):375-381. PubMed CrossRef
11. Carroll BT, Kirkhart R, Ahuja N, et al. Katatonia: a new conceptual understanding of catatonia and a new rating scale. Psychiatry (Edgmont). 2008;5(12):42-50. PubMed
aDepartment of Psychiatry, College of Medicine, University of Kentucky, Lexington, Kentucky
bMental Health Research Center at Eastern State Hospital, Lexington, Kentucky
cPsychiatry and Neurosciences Research Group (CTS-549), Institute of Neurosciences, University of Granada, Granada, Spain
dBiomedical Research Centre in Mental Health Net (CIBERSAM), Santiago Apóstol Hospital, University of the Basque Country, Vitoria, Spain
Potential conflicts of interest: None.
Funding/support: None.
Acknowledgment: The authors thank Lorraine Maw, MA, at the UK Mental Health Research Center, for editorial assistance. Ms Maw has no conflicts of interest related to the subject of this case report.
Patient consent: The patient’s mother and guardian provided oral permission for publication of this case report, and information has been de-identified to protect patient anonymity.
Published online: May 17, 2018.
Prim Care Companion CNS Disord 2018;20(3):17l02162
To cite: Wahidi N, de Leon J. Rapid development of lorazepam tolerance within 48 hours in an adult with intellectual disability who presented with stuporous catatonia and refused electroconvulsive therapy. Prim Care Companion CNS Disord. 2018;20(3):17l02162.
To share: https://doi.org/10.4088/PCC.17l02162
© Copyright 2018 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!