Objective: To examine family caregiver perspectives on cooperative communication surrounding pharmacologic and nonpharmacologic resources for the treatment of dementia-related behavioral symptoms.
Methods: Personal narrative interviews were conducted by the primary investigator with 13 family caregivers from October 2014 to April 2015. The recorded interviews were then transcribed and coded. Models detailing the caregivers’ resource utilization in regard to behavioral symptom management were produced for each participant and then summarized on the basis of recurring themes.
Results: There is a significant gap in the coordination and communication between physician services and caregiver community resources to aid in the behavioral management of family members with dementia. Physicians tend to rely on pharmacologic management independent of community resources and did not seem to be integrated or involved with recommendations from community resources.
Conclusions: Better integration of caregiver resources is necessary to help caregivers in the management of dementia-related behavioral symptoms.
The Communication Gap Between the Medical System and Community Resources for Dementia-Related Behavioral Symptom Management:
Family Caregiver Perspectives

ABSTRACT
Objective: To examine family caregiver perspectives on cooperative communication surrounding pharmacologic and nonpharmacologic resources for the treatment of dementia-related behavioral symptoms.
Methods: Personal narrative interviews were conducted by the primary investigator with 13 family caregivers from October 2014 to April 2015. The recorded interviews were then transcribed and coded. Models detailing the caregivers’ resource utilization in regard to behavioral symptom management were produced for each participant and then summarized on the basis of recurring themes.
Results: There is a significant gap in the coordination and communication between physician services and caregiver community resources to aid in the behavioral management of family members with dementia. Physicians tend to rely on pharmacologic management independent of community resources and did not seem to be integrated or involved with recommendations from community resources.
Conclusions: Better integration of caregiver resources is necessary to help caregivers in the management of dementia-related behavioral symptoms.
Prim Care Companion CNS Disord 2018;20(2):17m02238
To cite: Xiong GL, Godwin H, Ziegahn L, et al. The communication gap between the medical system and community resources for dementia-related behavioral symptom management: family caregiver perspectives. Prim Care Companion CNS Disord. 2018;20(2):17m02238.
To share: https://doi.org/10.4088/PCC.17m02238
© Copyright 2018 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry and Behavioral Sciences, University of California, Davis, Sacramento, California
bClinical and Translational Science Center, University of California, Davis, Sacramento, California
cDepartment of Public Health Sciences, University of California, Davis, Sacramento, California
dDepartment of Epidemiology and Biostatistics, University of California, San Francisco, California
*Corresponding author: Glen L. Xiong, MD, Department of Psychiatry and Behavioral Sciences, University of California, Davis, 2230 Stockton Blvd, Sacramento, CA 95817 ([email protected]).
The prevalence of dementia-related behavioral symptoms, also known as neuropsychiatric symptoms, may be as high as 60% in people with Alzheimer’s disease and other dementias living in community settings1,2 and more than 80% in people living in nursing homes.3,4 Neuropsychiatric symptoms have been shown to increase caregiver burden and lead to earlier nursing home placement.5-8 Nonpharmacologic interventions are considered first-line treatment for dementia-related neuropsychiatric symptoms, except in emergency situations.9-11 However, the use of nonpharmacologic treatments has gained little popularity in real-world settings.12 Instead, pharmacologic treatment for neuropsychiatric symptoms, namely antipsychotic use, ranges from 10%-40% depending on the setting13-19 despite US Food and Drug Administration black box warnings.20 Moreover, antipsychotics are continually used to treat neuropsychiatric symptoms despite increased risks of cardiac arrhythmias, cardiovascular disease, pneumonia, and all-cause mortality.21-24
Currently, there is a tremendous knowledge gap in translating nonpharmacologic interventions and minimizing use of pharmacologic treatment to manage dementia-related behavioral symptoms.25 For example, one study found that those who lived with their caregivers were significantly less likely to use antipsychotics than those who lived alone and that caregiver input is highly important in assessing effectiveness of dementia-related interventions.15 However, there is little to no research detailing family caregiver accounts on the relationship between pharmacologic and nonpharmacologic resources for dementia-related behaviors. While nonpharmacologic interventions have been shown to be effective in the management of dementia-related neuropsychiatric symptoms,9-11 it is uncertain if family caregivers are aware of such interventions. These interventions include formal and informal caregiver support groups, online resources, and spiritual resources. Thus, this study aims to understand the communicative relationship, or lack thereof, among caregiver resources for dementia-related behavioral symptoms via family caregiver narratives.
METHODS
Participants
Participants within the surrounding Sacramento, California, area were recruited from Alzheimer’s disease support groups; the University of California, Davis Alzheimer’s Disease Center; caregiver support groups; and adult day health centers. Participants were required to be the primary caregivers making medical decisions for a family member with dementia. The family member with dementia had to exhibit distressing behavioral symptoms that caused the caregiver to seek medical or other outside help.
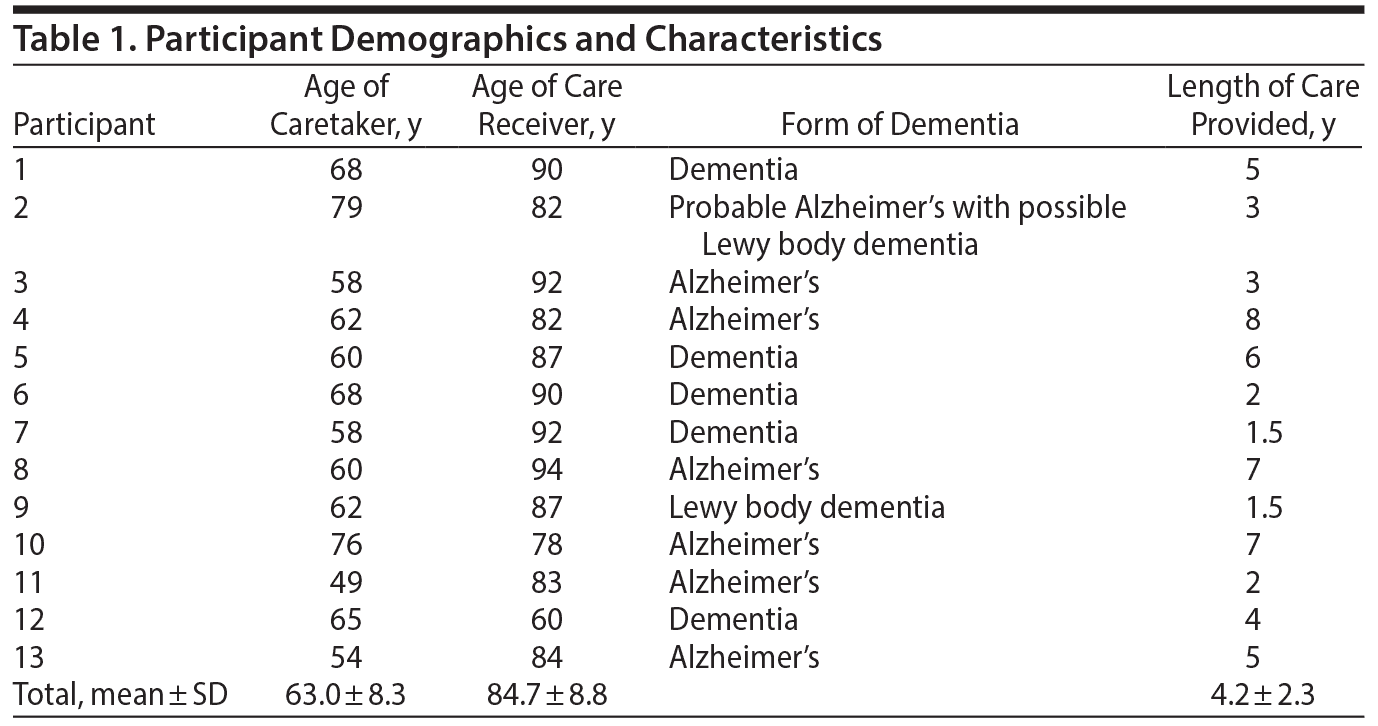
Of 35 people who responded to the study advertisement, 10 did not meet study entry criteria because the potential participants did not take care of an individual with dementia-related distressing behaviors. Five did not call back to complete the screening, and 7 did not complete the interview due to scheduling or other logistical reasons. A total of 13 caregivers, 12 female and 1 male, completed the interview process. A total of 10 participants were caring for a parent, 2 were caring for a spouse, and 1 was caring for a sibling. A summary of participant demographics can be found in Table 1. Participants were compensated with a gift card for their participation in the study.

- There is a significant gap in the coordination and communication between physician services and caregiver community resources to aid in the behavioral management of family members with dementia.
- Physicians tend to rely on pharmacologic management independent of community resources and did not seem to be integrated or involved with recommendations from community resources.
- Having a single, region-specific resource to provide direction to caregivers may prove to be extremely helpful in the caregiver decision-making process, in tandem with the physician’s role.
Materials
A standardized interview guide was used by researchers to examine caregiver perspectives on the communicative relationship between physician services and community resources for dementia-related behavioral management. Interview questions were based on a predetermined interview guide developed by 5 members of the research team. The interview guide covered the following 4 domains: (1) description of the behavioral problems, including the caregiver’s understanding of the nature and seriousness of the symptoms (ie, their explanatory model); (2) narrative of how the decision to either accept or decline (nonpharmacologic vs pharmacologic) treatment unfolded, including the nature of and satisfaction with discussions with the primary care provider and the role of other factors (eg, social resources); (3) understanding of the risks and benefits of pharmacologic treatment, namely antipsychotic use; and (4) caregiver description of therapeutic choices and their perceived outcomes.
Procedures
From October 2014 to April 2015, family caregiver interviews were conducted by the principal investigator (G.L.X.) both in-home and at the office at the University of California, Davis. All interviews were conducted in English, and no translation was necessary. These single-visit, audiotaped sessions typically lasted 30 minutes to an hour, wherein the principal investigator asked questions from the predetermined interview guide. Once complete, participant interviews were transcribed into text, which were subsequently qualitatively coded.
Qualitative analysis of the narrative transcription data included both coding and charting. Each transcription was reviewed by at least 2 authors, who then identified recurrent and definitive themes around resource utilization and communication for dementia-related behavioral symptom management. The qualitative data software package Dedoose version 5.0.11 (Dedoose, Manhattan Beach, California) was used to assign codes, analyze data, and find recurrent patterns.
RESULTS
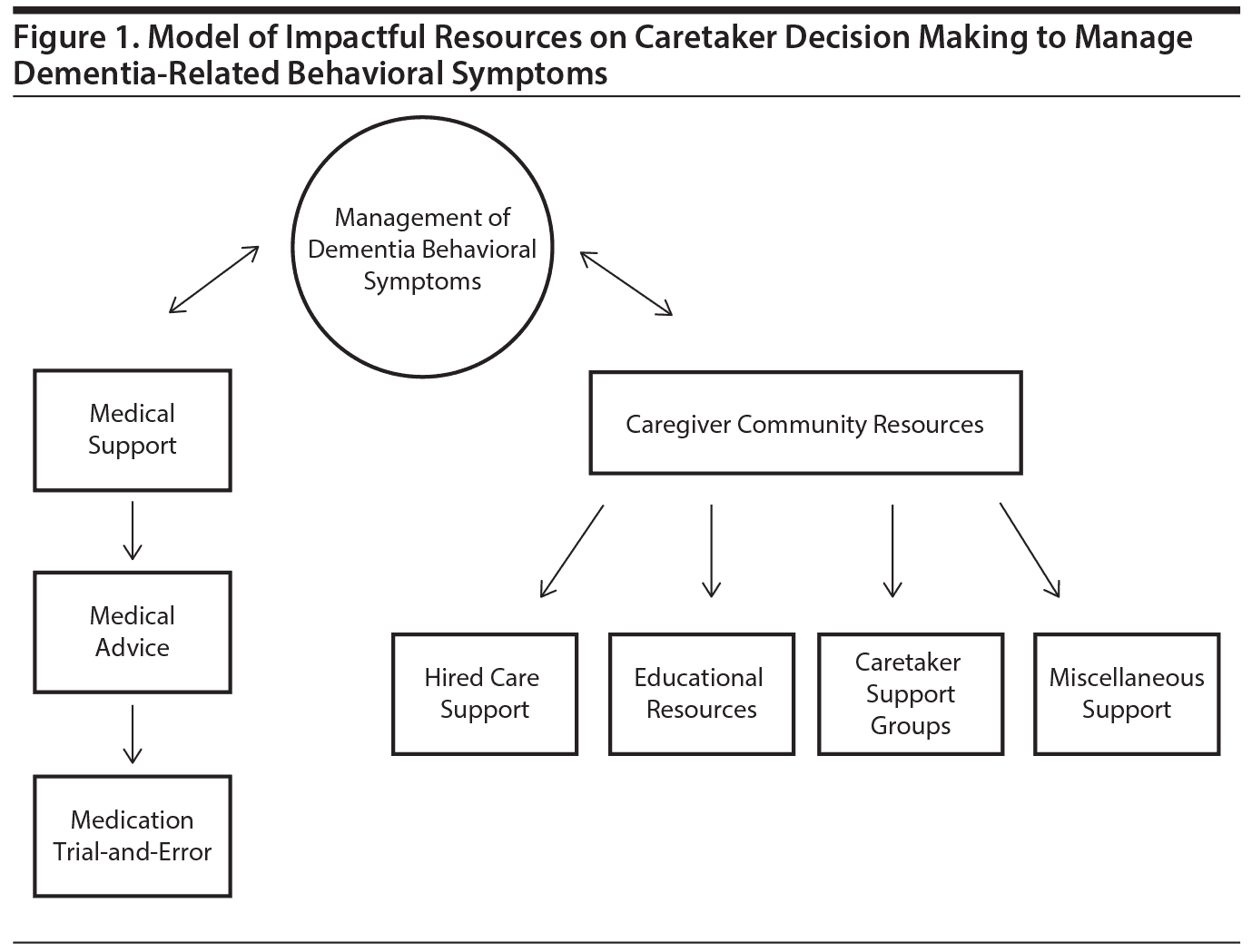
Our results include an analysis of the communicative relationship among various resources utilized by caregivers to aid in the behavioral symptom management of the care recipient and a description of the significant themes that emerged from participant narratives. Using an iterative comparison and review process, we arrived at a caregiver resource utilization model (Figure 1) that details the resources caregivers described to help them manage dementia-related behavioral problems. While participant resource utilization and caregiving approach varied, each participant used at least 1 resource, be that medical or social, to aid in the behavioral management of a loved one with dementia.
Most nonpharmacologic treatment communication and discussion came from family and friends, community resources such as caretaker support groups, hired caregivers, educational resources, and miscellaneous resources and forms of support, while pharmacologic recommendations from physicians were independent and did not seem to interact or connect with social recommendations. Overall, there was a lack of coordination and integration of community resources and physician recommendations. Participants frequently described having nonoverlapping and 1-sided conversations about treatment options with physicians, while having open discussions about behavioral treatment through community resources. Moreover, despite probing, participants did not describe any formal, evidence-based nonpharmacologic approaches that they learned from physicians or other medical resources.
DISCUSSION
The goal of this study was to better understand the experiences and perspectives of caregivers on the communication gap between physician services and caregiver resources for the treatment of dementia-related behavioral symptoms. After examining participant narratives, it was apparent that behavioral symptom management consisted of a trial-and-error process that lacked a necessary coordination between medical and community caregiver resources, leading to consistently high levels of caregiver confusion and frustration.
While many themes emerged from participant narratives, the most definitive pattern found was the near-constant frustration of caregivers from trying to manage their loved one’s dementia-related behavioral symptoms, as well as from attempting to coordinate communication among the available resources. Participants often utilized national websites as a reference to care management but maintained that the abundance of resources made it hard to discern those that were reliable. Most often, participants discussed behavioral management options with social and community resources but not with physicians or medical professionals. Caregiver narratives suggest that a lack of general knowledge about dementia and treatment options is inhibiting discussion between caregivers and physicians. This communication gap in caregiver resources for dementia-related behavioral symptom management undoubtedly leads to a lack of care coordination, which puts more pressure and burden onto stressed family caregivers.
To ameliorate this issue, a single, region-specific resource to provide direction to caregivers may prove to be extremely helpful in the caregiver decision-making process, in tandem with the physicians’ role. With such a resource, caregivers could connect with each other, share advice and local resources, and, ultimately, better educate themselves so that further discussion between caregiver and physician can be had. Clearly, more structured and available resources are desperately needed by family caregivers to help empower them to make more informed decisions and play a more active role in the caregiving process.
This study provides nascent information and insight into the communication gap between physician services and dementia-related behavioral symptom management resources for family caregivers. Although the small participant group may not be representative of the entire caregiver population, it is very likely that their struggles with lack of information, as well as with the communication gap, are reflective of caregivers at large. Another limitation of this study is that the participants were all informal caregivers caring for a family member and already connected to 1 or more caregiving resources. The needs of family caregivers not connected to some sort of caregiving resource may be different from the needs of this particular population. Future studies should examine methods with which to bridge the divide among caregivers, physicians, and caregiving resources so that more informed discussions and decision-making can occur between caregivers and physicians. On a larger scale, future studies could also examine the various family caregiver populations and their diverse needs in reference to resources.
Submitted: October 26, 2017; accepted December 12, 2017.
Published online: March 15, 2018.
Potential conflicts of interest: None.
Funding/support: This study was funded by the UC Davis Center for Health Care Policy and the UC Davis Research and Clinical and Translational Science Center and partly supported by resources from the UC Davis Alzheimer’s Disease Center, funded by the National Institute on Aging (P30 AG10129).
Role of the sponsor: The sponsors had no input about the design and conduct of this study; collection, management, analysis, and interpretation of data; or preparation, review or approval of the manuscript.
REFERENCES
1. Wragg RE, Jeste DV. Neuroleptics and alternative treatments: management of behavioral symptoms and psychosis in Alzheimer’s disease and related conditions. Psychiatr Clin North Am. 1988;11(1):195-213. PubMed
2. Lyketsos CG, Steinberg M, Tschanz JT, et al. Mental and behavioral disturbances in dementia: findings from the Cache County Study on memory in aging. Am J Psychiatry. 2000;157(5):708-714. PubMed CrossRef
3. Zuidema SU, Derksen E, Verhey FR, et al. Prevalence of neuropsychiatric symptoms in a large sample of Dutch nursing home patients with dementia. Int J Geriatr Psychiatry. 2006;22(7):632-638. PubMed CrossRef
4. Jeste DV, Blazer D, Casey D, et al. ACNP white paper: update on use of antipsychotic drugs in elderly persons with dementia. Neuropsychopharmacology. 2008;33(5):957-970. PubMed CrossRef
5. Gaugler JE, Wall MM, Kane RL, et al. The effects of incident and persistent behavioral problems on change in caregiver burden and nursing home admission of persons with dementia. Med Care. 2010;48(10):875-883. PubMed CrossRef
6. Karttunen K, Karppi P, Hiltunen A, et al. Neuropsychiatric symptoms and quality of life in patients with very mild and mild Alzheimer’s disease. Int J Geriatr Psychiatry. 2011;26(5):473-482. PubMed CrossRef
7. Rocca P, Leotta D, Liffredo C, et al. Neuropsychiatric symptoms underlying caregiver stress and insight in Alzheimer’s disease. Dement Geriatr Cogn Disord. 2010;30(1):57-63. PubMed CrossRef
8. de Vugt ME, Stevens F, Aalten P, et al. Do caregiver management strategies influence patient behavior in dementia? Int J Geriatr Psychiatry. 2004;19(1):85-92. PubMed CrossRef
9. Livingston G, Kelly L, Lewis-Holmes E, et al. Non-pharmacological interventions for agitation in dementia: systematic review of randomized controlled trials. Br J Psychiatry. 2014;205(06):436-442. PubMed CrossRef
10. Ayalon L, Gum AM, Feliciano L, et al. Effectiveness of nonpharmacological interventions for the management of neuropsychiatric symptoms in patients with dementia: a systematic review. Arch Intern Med. 2006;166(20):2182-2188. PubMed CrossRef
11. Gitlin LN, Kales HC, Lyketsos CG. Nonpharmacologic management of behavioral symptoms in dementia. JAMA. 2012;308(19):2020-2029. PubMed CrossRef
12. Kales HC, Gitlin LN, Lyketsos CG. Management of neuropsychiatric symptoms of dementia in clinical settings: recommendations from a multidisciplinary expert panel. J Am Geriatr Soc. 2014;62(4):762-769. PubMed CrossRef
13. Xiong GL, Filshtein T, Beckett LA, et al. Antipsychotic use in a diverse population with dementia: a retrospective review of the National Alzheimer’s Coordinating Center Database. J Neuropsychiatry Clin Neurosci. 2015;27(4):326-332. PubMed CrossRef
14. Rapoport M, Mamdani M, Shulman KI, et al. Antipsychotic use in the elderly: shifting trends and increasing costs. Int J Geriatr Psychiatry. 2005;20(8):749-753. PubMed CrossRef
15. Rhee YJ, Csernansky JG, Emanuel L, et al. Psychotropic medication burden and factors associated with antipsychotic use: an analysis of a population-based sample of community-dwelling older persons with dementia. J Am Geriatr Soc. 2011;59(11):2100-2107. PubMed CrossRef
16. de Mauleon A, Sourdet S, Renom-Guiteras A, et al. Associated factors with antipsychotic use in long-term institutional care in eight European countries: results from the RightTimePlaceCare study. J Am Med Dir Assoc. 2014;15(11):812-818. PubMed CrossRef
17. Puyat JH, Law MR, Wong ST, et al. The essential and potentially inappropriate use of antipsychotics across income groups: an analysis of linked administrative data. Can J Psychiatry. 2012;57(8):488-495. PubMed CrossRef
18. Kamble P, Chen H, Sherer JT, et al. Use of antipsychotics among elderly nursing home residents with dementia in the US: an analysis of National Survey Data. Drugs Aging. 2009;26(6):483-492. PubMed CrossRef
19. Chen Y, Briesacher BA, Field TS, et al. Unexplained variations across US nursing home in antipsychotic prescribing rates. Arch Intern Med. 2010;170(1):89-95. PubMed CrossRef
20. Schneider LS, Dagerman KS, Insel P. Risk of death with atypical antipsychotic drug treatment for dementia: meta-analysis of randomized placebo-controlled trials. JAMA. 2005;294(15):1934-1943. PubMed CrossRef
21. Gill SS, Rochon PA, Herrmann N, et al. Atypical antipsychotic drugs and risk of ischemic stroke: population based retrospective cohort study. BMJ. 2005;330(7489):445. PubMed CrossRef
22. Liperoti R, Gambassi G, Lapane KL, et al. Cerebrovascular events among elderly nursing home patients treated with conventional or atypical antipsychotics. J Clin Psychiatry. 2005;66(9):1090-1096. PubMed CrossRef
23. Kales HC, Valenstein M, Kim HM, et al. Mortality risk in patients with dementia treated with antipsychotics versus other psychiatric medications. Am J Psychiatry. 2007;164(10):1568-1576. PubMed CrossRef
24. Trifirײ G, Verhamme KM, Ziere G, et al. All-cause mortality associated with atypical and typical antipsychotics in demented outpatients. Pharmacoepidemiol Drug Saf. 2007;16(5):538-544. PubMed CrossRef
25. Gitlin LN, Marx K, Stanley IH, et al. Translating evidence-based dementia caregiver interventions into practice: state-of-the-science and next steps. Gerontologist. 2015;55(2):210-226. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!