Patients With Treatment-Resistant Insomnia Taking Nightly Prescription Medications for Sleep: A Retrospective Assessment of Diagnostic and Treatment Variables
Background: Some chronic insomnia patients who take nightly prescription medication achieve less than optimal results. The US Food and Drug Administration (FDA) and the American Academy of Sleep Medicine (AASM) recommend reevaluation of this type of patient to assess for potential psychiatric or medical causes to explain this “failure for insomnia to remit.”
Method: A retrospective chart review examined a consecutive series of chronic insomnia patients with persistent insomnia complaints despite current nightly use of prescription medication from May 2005 to February 2008. To assess the role of psychiatric influences on insomnia symptoms, our sample (N = 218) was divided into 2 subgroups: a group with a history of psychiatric complaints (psychiatric insomnia, n = 189) and a control group of no psychiatric complaints (insomnia, n = 29).
Results: The average patient reported insomnia for a decade and took prescription medication for sleep for a mean of 4.5 years. Although 100% of the sample used nightly sleep drugs, only 20% believed medication was the best solution for their condition. As evaluated by self-report and polysomnography, these patients exhibited moderately severe insomnia across most measures. Only a few differences were noted between groups. Subjective perception of insomnia severity was worse in the psychiatric insomnia group, which also reported significantly more insomnia-related interference in daily functioning, symptoms of sleep maintenance insomnia, and a trend toward greater daytime fatigue. The mean Apnea-Hypopnea Index score was 19.5 events/hour, yielding an obstructive sleep apnea diagnosis in 75% of patients per conservative AASM nosology (79% in the insomnia group and 74% in the psychiatric insomnia group, P = .22).
Conclusions: In this treatment-seeking sample of patients regularly taking sleep medications, residual insomnia was widespread, and patients with psychiatric insomnia may have perceived their condition as more problematic than a control group of insomnia patients without mental health complaints. Both groups exhibited high rates of objectively diagnosed obstructive sleep apnea, a medical condition associated with pervasive sleep fragmentation. These findings support FDA and AASM guidelines to reassess chronic insomnia patients who manifest residual symptoms despite nightly use of prescription medication for sleep.
Prim Care Companion J Clin Psychiatry 2010;12(4):e1-e10
© Copyright 2010 Physicians Postgraduate Press, Inc.
Submitted: August 20, 2009; accepted November 24, 2009.
Published online: August 12, 2010 (doi:10.4088/PCC.09m00873bro).
Corresponding author: Barry Krakow, MD, Sleep & Human Health Institute, 6739 Academy NE, Ste 380, Albuquerque, NM 87109 ([email protected]).
Chronic insomnia is a common complaint in the general population as well as in various subpopulations such as the elderly,1 psychiatric patients,2,3 and shift workers4; however, longitudinal data are lacking on their long-term treatment course. Initially, insomnia patients navigate through 4 common pathways: no discernible treatment, over-the-counter sleep aids,5,6 substances or alcohol at bedtime,6,7 and basic sleep hygiene instructions obtained through various media or from primary care providers and educators.8-10 There is often overlap among these 4 pathways. And, in a progression through these approaches, albeit in no fixed order, some insomnia patients broach the issue with a physician or other provider with whom they regularly interact. This type of health care encounter most frequently involves primary care physicians or mental health providers, including psychiatrists, psychologists, and other therapists. In these environments, insomnia patients may receive exposure to evidenced-based treatments for unwanted sleeplessness,8,9,11 for example, prescription medications for sleep and cognitive-behavioral therapies (CBTs).
Evidence for CBT as the ideal first-line treatment for insomnia is persuasive and substantial, but the lack of behavioral sleep medicine specialists both at sleep medical centers and in the medical community at large8 has limited the application of this therapeutic option. In contrast, pharmacotherapy for insomnia is well established throughout all fields of medicine. Traditional standards indicate prescribed medication for acute, transient, or situational insomnia, and the prescribing instructions may recommend nightly use for a few weeks or a few times per week for longer intervals.12 However, in clinical settings, it is not unusual for various subgroups of patients, for example psychiatric patients, to rely on the regular, long-term use of prescription medications for sleep. Interestingly, these prescription medications may include standard sedatives as well as sedating antidepressants. Indeed, for years trazodone13 was the single most-prescribed medication for sleep, and although there is scant evidence describing the efficacy of antidepressants for insomnia, there can be no doubt that these drugs are often prescribed for the combination of insomnia and depression.14
Recently published American Academy of Sleep Medicine (AASM) guidelines provide support for the use of long-term pharmacologic modalities to treat insomnia.12 However, the guidelines are not a “practice parameter” but rather a “working overview for disease or disorder evaluation and management.”(p490) In fact, when dealing with duration of pharmacologic treatment, it is clearly stated that “the empirical database for long-term treatment remains small.”12(p501) Conversely, government regulatory actions from the US Food and Drug Administration (FDA) established indications for long-term use of the hypnotics eszopiclone, zolpidem controlled release, and ramelteon to treat chronic insomnia.15,16 But, this same agency subsequently posted (March 2007) an important warning about the first 2 medications: “The failure of insomnia to remit after 7 to 10 days of treatment may indicate the presence of a primary psychiatric and/or medical illness that should be evaluated.”17(p3),18(p1) In a similar vein, the AASM practice parameters, which ordinarily do not recommend polysomnography for insomnia patients, state, “‘ ¦ polysomnography is indicated when initial diagnosis (of insomnia) is uncertain, treatment fails (behavioral or pharmacologic), or precipitous arousals occur with violent or injurious behavior.”12(p487) Notwithstanding these paradoxical perspectives, newer agents are now routinely advertised in scientific journals, in popular magazines, on television, and through the Internet as nightly long-term solutions to insomnia.
Despite the increase in prescribing patterns for chronic insomnia,19 scant longitudinal data describe how patients respond to these drugs and whether or not FDA and AASM guidelines are invoked subsequent to the “failure of insomnia to remit.” One speculation would comprise a spectrum of patient outcomes, which at one end include responders who continue care with their prescribing physician, whereas those on the opposite end of the spectrum, nonresponders (extreme treatment-resistant cases), might drop out of treatment entirely. In the middle ground, a sizable proportion of partial treatment-resistant insomnia patients manifest mixed results while continuing to use nightly prescription medications.
Clinical Points
- Patients with treatment-resistant insomnia taking hypnotic medication require additional medical and psychiatric evaluations.
- Overnight polysomnography appears to be a useful evaluation tool for patients with treatment-resistant insomnia.
- Sleep-disordered breathing may be common in patients with treatment-resistant insomnia.
We are interested in this middle group because they commonly present to sleep centers and request further treatment for insomnia despite regularly taking prescription medications. In most cases, these patients align with AASM and FDA guidelines in that further psychiatric evaluations and polysomnography are indicated to assess residual insomnia complaints. For example, prior studies show higher than expected rates of obstructive sleep apnea (OSA) in chronic insomnia patients.20-24
In the current study, we gathered data on a consecutive series of chronic insomnia patients who presented to our sleep medical centers with a history of nightly use of prescription medications for sleep and the failure of insomnia to remit. From this pool of consecutive patients, a retrospective chart review was conducted, coinciding with FDA and AASM guidelines, to assess our sample for psychiatric or medical conditions that might be associated with worse insomnia outcomes. For this descriptive study, we developed 2 hypotheses: (1) psychiatric insomnia patients would report or demonstrate worse insomnia outcomes than a nonpsychiatric insomnia group and (2) both psychiatric and nonpsychiatric insomnia groups would show high rates of the medical condition sleep-disordered breathing (SDB) and its resultant sleep fragmentation, which might be associated with residual insomnia symptoms.
METHOD
Per standard protocol at our sleep facilities in Albuquerque and Los Alamos, New Mexico, all patients provide written and verbal consent for their medical information to be used anonymously for research purposes in the context of subsequent chart reviews. This study was a retrospective chart review of existing data on patients treated from May 2005 to February 2008. The study was reviewed and approved by the Los Alamos Medical Center Institutional Review Board, Los Alamos, New Mexico.
Sample and Inclusion Criteria for Chart Review
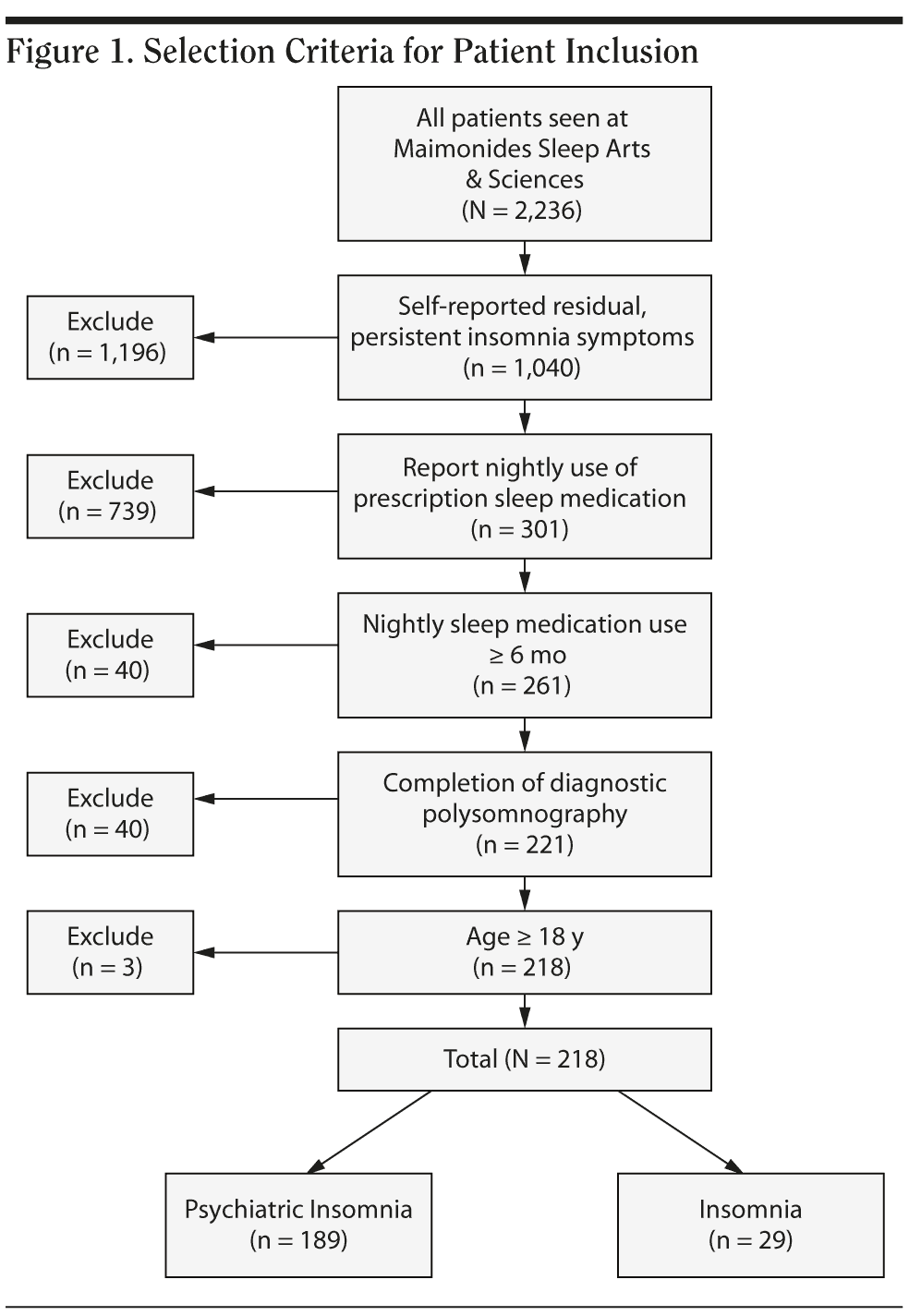
This study contained 4 inclusion criteria: (1) insomnia ranked as the primary reason for seeking treatment despite nightly use of prescription medication for sleep, (2) minimum duration of medication use of 6 months, (3) completion of overnight diagnostic polysomnography or split-night protocol with at least 2 hours of diagnostic sleep data, and (4) at least 18 years of age. Figure 1 (flowchart) shows nearly half the clinic population of 2,236 patients ranked insomnia as their primary problem, but only 301 patients reported both residual insomnia and nightly sleep medication use. Each individual patient’s medications were reviewed to determine whether or not their reported nightly agent was in fact being used to treat sleep problems. For example, 3 patients were excluded because the only nighttime medication was lithium, a drug not typically used for insomnia. Additional exclusions were duration of use less than 6 months, no polysomnography testing, or age less than 18 years. And, as anticipated from our introduction, no patients presented to our sleep medical facility with a self-reported optimal response to nightly use of prescription medication for sleep.
Psychiatric Assessment
No formal psychiatric interviewing or instruments were used to evaluate historical complaints of psychiatric conditions; therefore, the information used in this retrospective study relies entirely on subjective reports from the patients’ intake questionnaires. However, the intake questionnaire does not ask patients to speculate about their mental health; rather, it specifically asks patients to check those conditions that they believe they suffer from currently or have suffered from in the past. The checklist comprises 4 columns: a list of 8 psychiatric conditions and 2 additional lines for “none” or “other,” a list of current medications taken for a condition checked, a list of past medications taken for the condition, and any other therapies used to treat the condition. Two additional questions are asked about a history of traumatic exposure and/or claustrophobia. For trauma, patients are asked if they have suffered a threat to their life, a serious injury, or a serious assault (physical, sexual, etc), which elicited a feeling of fear, helplessness, and/or horror.
Although these data do not corroborate formal psychiatric diagnoses, 87% of the patients in our sample reported a history of at least 1 of the following: depression, anxiety disorder, posttraumatic stress disorder (PTSD), panic disorder, schizophrenia, bipolar disorder, obsessive-compulsive disorder (OCD), traumatic exposure, or claustrophobia. To be clear, however, these data are only describing the association of a putative psychiatric condition with the presence of insomnia; the data do not indicate whether or not the psychiatric condition is a cause or contributor to the patient’s insomnia. Therefore, in this article, the term psychiatric insomnia is only used to distinguish this group of patients from those with no self-reported psychiatric condition(s).
Sleep Intake, Measurements, and Procedures
All patients seen at both sleep facilities completed an online intake set of questionnaires, including an extensive sleep medicine history25 on self-reported subjective sleep measures, sleep history, and medication use for sleep. The sleep medicine history also contained 3 questions about patient perceptions on chronic use of sedating medications, and these were scored on a disagree/unsure/agree 3-point scale. These questions dealt with whether medication was perceived as the best solution for their sleep problems, whether they had been seeking help for their sleep problems for an extended period of time, and the level of frustration with past efforts in getting help for their sleep problem(s). Answers to these questions were not considered for inclusion or exclusion in the current study.
The Insomnia Severity Index (ISI)26 was also completed by all patients. The ISI is the sum of 7 individual questions dealing with the following: (1) difficulty falling asleep, (2) difficulty staying asleep, (3) waking up too early, (4) satisfaction with current sleep pattern, (5) extent of interference sleep problem has on daily functioning, (6) impairment of quality of life noticeable to others, and (7) level of distress surrounding current sleep problem. Each question is scored on a scale of 0 to 4 based on increasing severity of the symptom, and the total score ranges from 0 to 28 with scores greater than 20 equal to moderately severe to severe insomnia.
Two visual analog scales (VAS) were used to measure daytime sleepiness and tiredness,27,28 scored on a 0 to 10 metric with scores > 6 indicative of severe symptoms.
Intake questionnaires are reviewed by the sleep specialist (B.K.), and patients are scheduled for polysomnography when criteria are met for apparent risks of physiologic disorders such as SDB. In our clinical experience, we follow FDA and AASM guidelines and recommend diagnostic polysomnography testing in the large majority of these patients17-18 for failing to achieve a satisfactory or optimal response to pharmacologic treatment of insomnia. However, as noted in Figures 1, 40 patients refused or did not undergo polysomnography testing and were therefore excluded from the study.
Polysomnography Protocol
Overnight sleep studies were performed using standard polysomnography on all Maimonides Sleep Arts & Sciences and Los Alamos Medical Center Sleep Laboratory patients. Technicians prepared patients using the international 10-20 system of electrode placement. The recording had a 14-channel montage: left outer canthus-A2, right outer canthus-A1, C3-A2, C4-A1, O1-A2, O2-A1, chin, electrocardiogram, left leg-right leg, snore, nasal pressure transducer via nasal canula, chest effort, abdominal effort, pulse oximetry, and position. Polysomnography sleep staging was scored manually by registered technologists using Rechtschaffen and Kales’ 29 scoring criteria. Three types of events were scored. An apnea was a > 70% decrease in airflow for at least 10 seconds. Hypopnea was a 30%-70% decrease in airflow coupled with either a 4% oxygen desaturation or an arousal. Flow limitation was a decrease in airflow of ≤ 30% in the form of classic flattening or notching of the airflow limb for at least 2 consecutive breaths, lasting > 10 seconds, ending in an arousal. Minimum oxygen saturation was recorded by pulse oximetry. All patients were tested using their regular bedtime regimen of medications. The Apnea-Hypopnea Index (AHI) was calculated for each patient and per AASM nosology.30 An AHI score ≥ 5 was used as a diagnostic cut point for the diagnosis of SDB. A total of 18 patients completed split nights, and their data were extrapolated as if they completed a full-night study by using their objective sleep efficiency from the diagnostic portion of the polysomnography testing to estimate relevant objective sleep indices.
Data Analysis
To compare outcomes among those patients with and without self-reported psychiatric conditions, 2 groups were created: insomnia group (no psychiatric complaints, n = 29) and psychiatric insomnia group (self-report of psychiatric complaints, n = 189). One post hoc analysis compared patients with OSA (n = 163) and no OSA (n = 55).
Analysis of variance and χ2 analyses were performed for continuous and dichotomous variables, respectively. Cohen d effect sizes, the standardized mean difference, were calculated from the difference in 2 means, divided by the pooled standard deviation, and used for select comparisons of statistically significant findings only. Statistical significance was .05. Power analysis (α = .5, β = .80) revealed that the 2 unequal samples for the insomnia and psychiatric insomnia groups were slightly underpowered to detect medium-sized effects.
RESULTS
Sample Characteristics
Of the 2 contrasted groups, the psychiatric insomnia group comprised 189 patients who reported the following prevalence of psychiatric conditions: depression (56.4%), traumatic exposure (50.2%), anxiety (42.7%), claustrophobia (41.6%), panic (25.7%), PTSD (17.95%), bipolar illness (9.2%), OCD (2.8%), dissociative disorder (3.2%), and schizophrenia (0.5%).
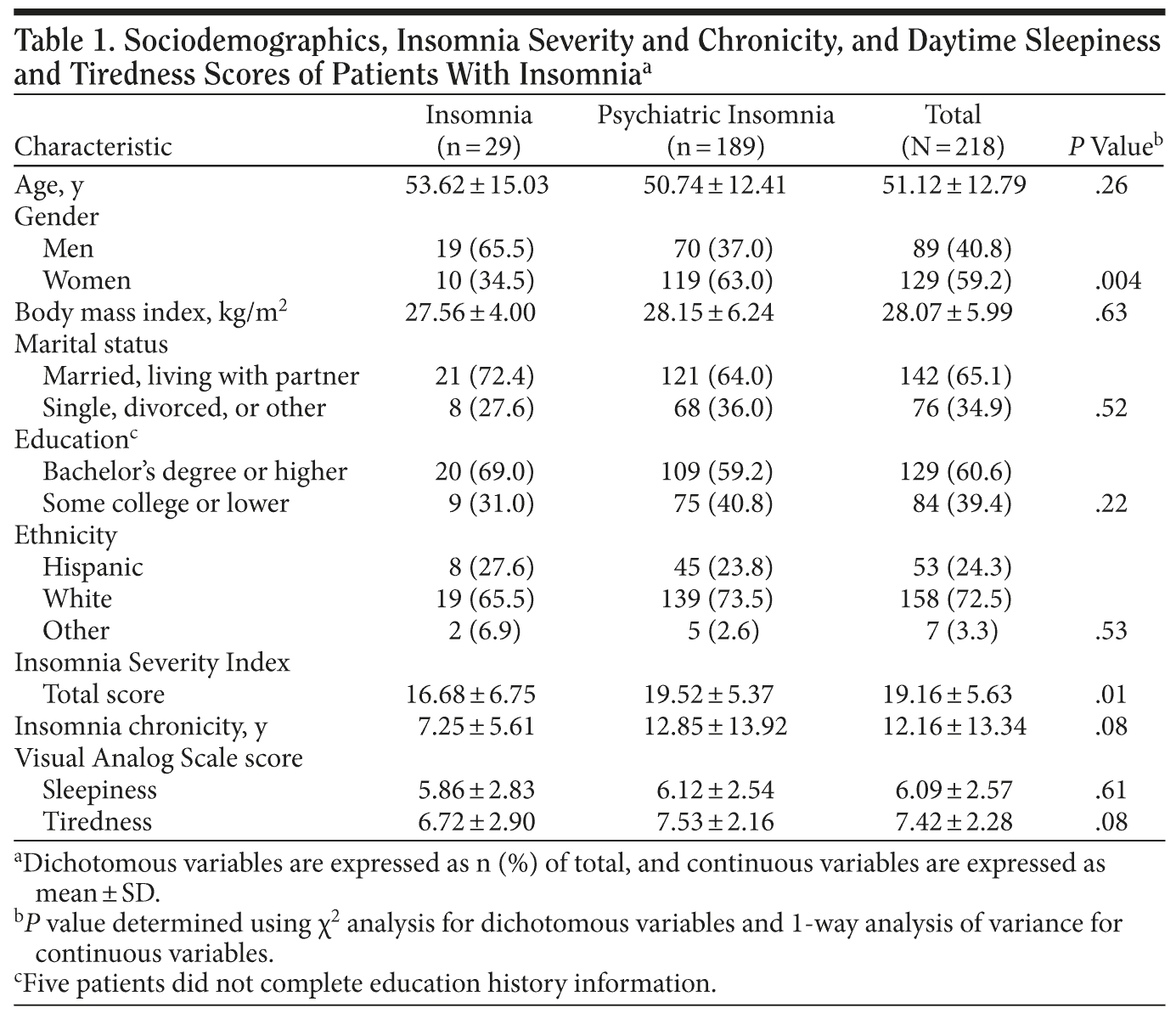
Table 1 shows that the full sample of unresolved insomnia patients was largely middle-aged and slightly overweight. Distinctions between groups revealed predominantly women in the psychiatric insomnia group and predominantly men in the insomnia group (P = .004). Insomnia severity, based on ISI score, was in the moderate to severe range (mean ± SD = 19.16 ± 5.63) with the psychiatric insomnia group having a significantly higher ISI (19.52 ± 5.37) than the insomnia group (16.68 ± 6.75) (P = .01, d = 0.47). The mean ± SD duration of insomnia was 12.2 ± 13.32 years. Sedating medication use ranged from 6 months to 30 years with a mean of 54.68 months (SD = 69.84) and a median of 25.0 months.
Prescription Medications for Sleep
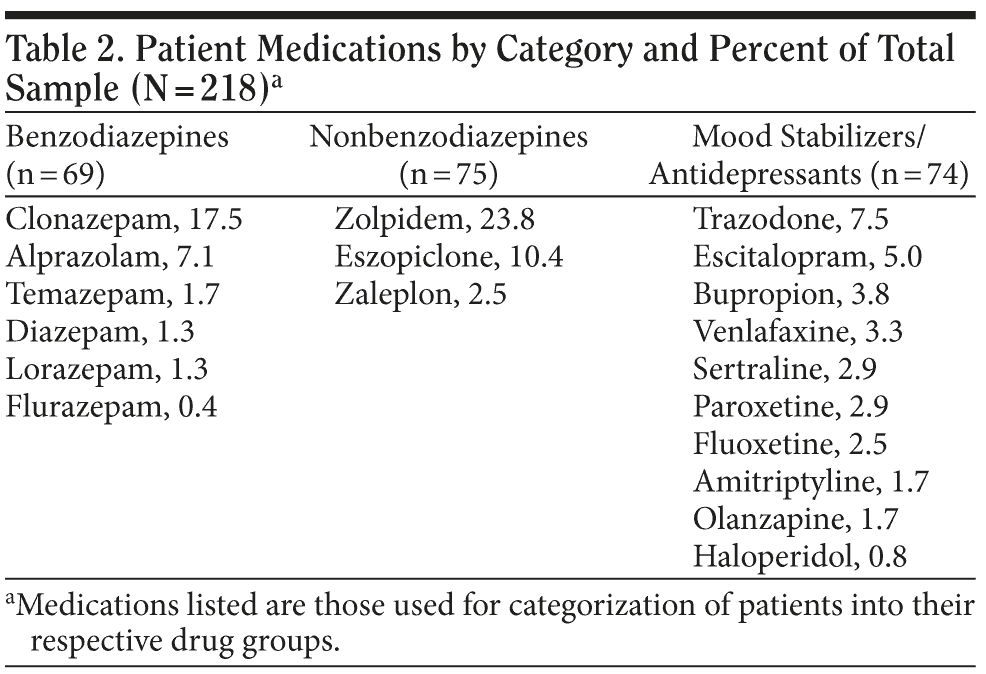
All patients were using a prescription medication designated by their prescribing physician for the primary purpose of treating a sleep disturbance. Of our total sample, 67% were prescribed sleep medications by their primary care physician, 24% by a psychiatrist, 8% by physicians of various specialties, and 1% by a sleep doctor. However, due to patient inconsistency, we did not collect or report specific dosages used by the patients in this sample. We identified 3 main categories of drugs prescribed (Table 2): benzodiazepines (n = 69), nonbenzodiazepines (n = 75), and mood stabilizers/antidepressants (n = 74). No patients were taking the melatonin agonist ramelteon.
In the psychiatric insomnia group, roughly one-half of the patients were also taking other psychotropic medications that influence sleep,31,32 although these drugs were not the primary medication prescribed for sleep. No systematic differences were evident between these 3 prescribed groups of medications for any of the variables of interest in this study; therefore, no additional analyses were conducted on the basis of medications.
Patient Perceptions
On the basis of 3 questions about patient perceptions, 74% of the total sample reported that they had been seeking help for their sleep problems for a long time, which is consistent with a mean duration of insomnia of 12 years. Nearly half the sample (47%) reported frustration with previous physicians in their attempts to solve their sleep problems, whereas only 26% reported no frustration and 27% were unsure how to respond. At this point in their care, only 20% of patients believed that the correct medication would solve their sleep problems, whereas 55% were undecided on this question, and 24% believed medications would not solve their problems. There were no statistical differences on these perceptions between the insomnia and psychiatric insomnia groups.
Two individual items on the ISI relating to patient perceptions showed differences between the 2 groups. First, those patients in the psychiatric insomnia group reported more difficulty staying asleep (P = .05, d = 0.36). Second, the psychiatric insomnia group also perceived that their sleep problems interfered with their daily functioning to a greater degree than the insomnia group (P = .04, d = 0.38), and these 2 items account for most of the differences between the 2 groups on the total ISI score of self-reported insomnia severity.
Regarding impairment, there were no significant differences among groups for the VAS sleepiness scale (Table 1); however, the VAS for tiredness showed that the psychiatric insomnia group trended toward greater severity than the insomnia group (P = .08, d = 0.32).
Self-Reported and Objective Sleep Indices
Subjective sleep indices including mean ± SD sleep-onset latency (69.11 ± 65.67 minutes), total sleep time (6.01 ± 1.93 hours), wake time after sleep onset (100.43 ± 89.72 minutes), and calculated sleep efficiency (73.24 ± 19.98%) consistently showed moderate to severe insomnia. Patients also reported other signs of sleep fragmentation including difficulty maintaining sleep, increased awakenings, and difficulties returning to sleep once awakened. There were no statistical differences between the 2 groups.
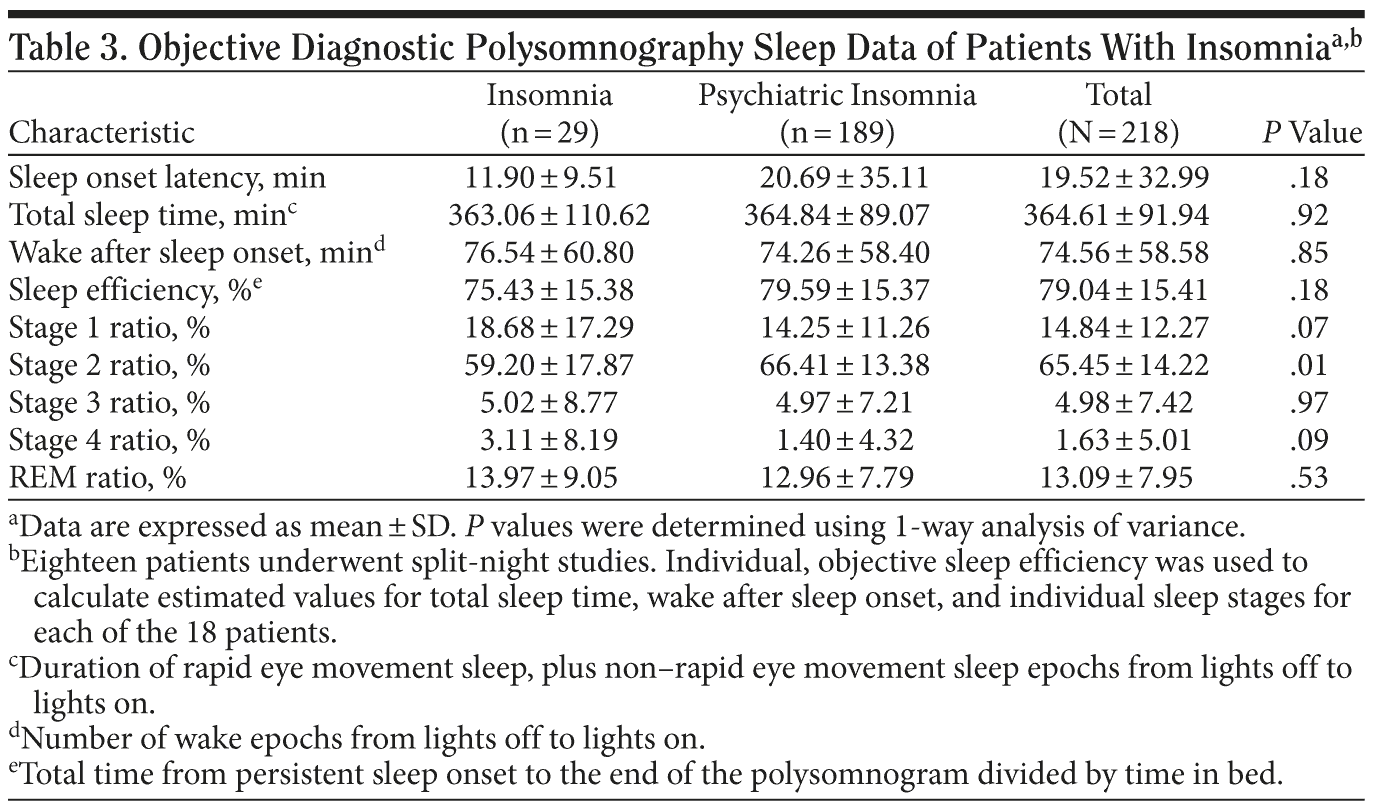
For objective sleep indices, the polysomnography testing consisted of 1 night in the sleep laboratory, and the patients used their standard nightly regimen of medications including their primary sleep medication. As expected, consistent signs of moderate to severe insomnia were documented for total sleep time, wake time after sleep onset, and sleep efficiency without significant differences between the 2 groups (Table 3). And, as often seen with first-night effects in sleep laboratory testing of insomnia patients,33 mean ± SD sleep-onset latency was within normal limits in both groups (insomnia group: 11.90 ± 9.51, psychiatric insomnia group: 20.69 ± 35.11, P = .18). When looking at individual sleep stage ratios (Table 3), the psychiatric insomnia group showed a significantly higher ratio (66.41 ± 13.38) of stage 2 non-rapid eye movement (NREM) sleep than the insomnia group (59.20 ± 17.87, P = .01) with a medium effect size (d = 0.46). The ratio of stage 1 NREM sleep trended lower in the psychiatric insomnia group (14.25 ± 11.26) versus the insomnia group (18.68 ± 17.29, P = .07, d = 0.30), whereas the ratio of stage 4 NREM sleep in the psychiatric insomnia group trended lower (1.40 ± 4.32) than the insomnia group (3.11 ± 8.19, P = .09, d = 0.26).
Breathing Event Indices and Sleep-Disordered Breathing Diagnoses
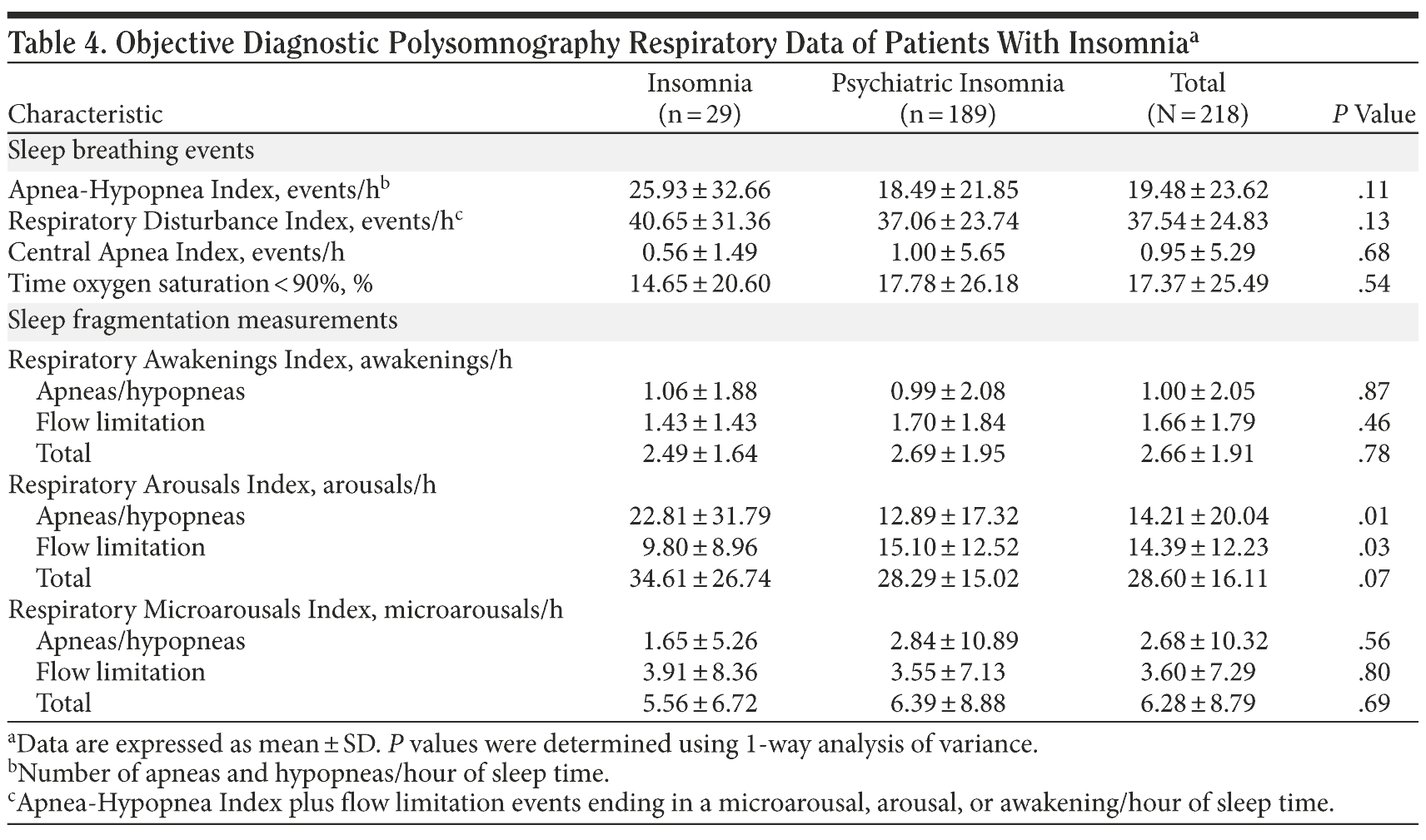
The mean ± SD AHI score was 19.48 ± 23.62 events/hour with no significant differences between the 2 groups (Table 4). Given a significant difference in men versus women between groups (more men in the insomnia group) and the consequent greater severity of OSA (AHI) found in men (men: 29.83 ± 29.76, women: 12.34 ± 14.52, P = .001), further analysis showed that the finding of more severe OSA in the insomnia group was primarily due to differences in gender ratios between groups (F2,235 = 8.210, P = .0001).
According to AASM nosology,30 we found that 163 (75.0%) patients met criteria for OSA based solely on AHI score (≥ 5) (79% of the insomnia group and 74% of the psychiatric insomnia group). For exploratory purposes only and not reported in our tables, we scored flow limitation events 2 ways: (1) according to AASM guidelines,30 yielding a mean ± SD Respiratory Disturbance Index (RDI) of 37.54 ± 24.83 events/hour, and (2) with so-called “subcortical arousals” using Rapoport’s criteria,31 which would have raised the mean ± SD RDI to 46.53 ± 25.24 events/hour, thereby potentially yielding an even higher proportion of diagnosed cases of OSA. There was no significant difference of mean RDI values between the 2 groups.
Sleep Fragmentation
We assessed sleep fragmentation in the form of awakenings (> 15.0 seconds), arousals (3.0-15.0 seconds), and microarousals (1.5-3.0 seconds) caused by sleep breathing events that might be associated with insomnia outcomes (Table 4). For both groups, SDB events produced a mean of 1 awakening/hour due to apneas (including central apneas) or hypopneas with an additional 1.7 awakenings/hour for flow limitation events (Table 5). The Respiratory Arousal Index showed a mean of 14.21 ± 20.04 arousals/hour for apneas and hypopneas with an increase to 28.60 ± 16.11 arousals/hour when flow limitation events were included. There was a trend toward a higher total of SDB-related arousals in the insomnia group (34.61 ± 26.74) when compared to the psychiatric insomnia group (28.29 ± 15.02, P = .07, d = 0.29). And finally, OSA caused 2.68 ± 10.32 microarousals/hour with an increase to 6.28 microarousals/hour when flow limitation events were included. However, none of these awakenings, arousals, and microarousals individually or in combination correlated with ISI severity.
OSA Versus Non-OSA Patients
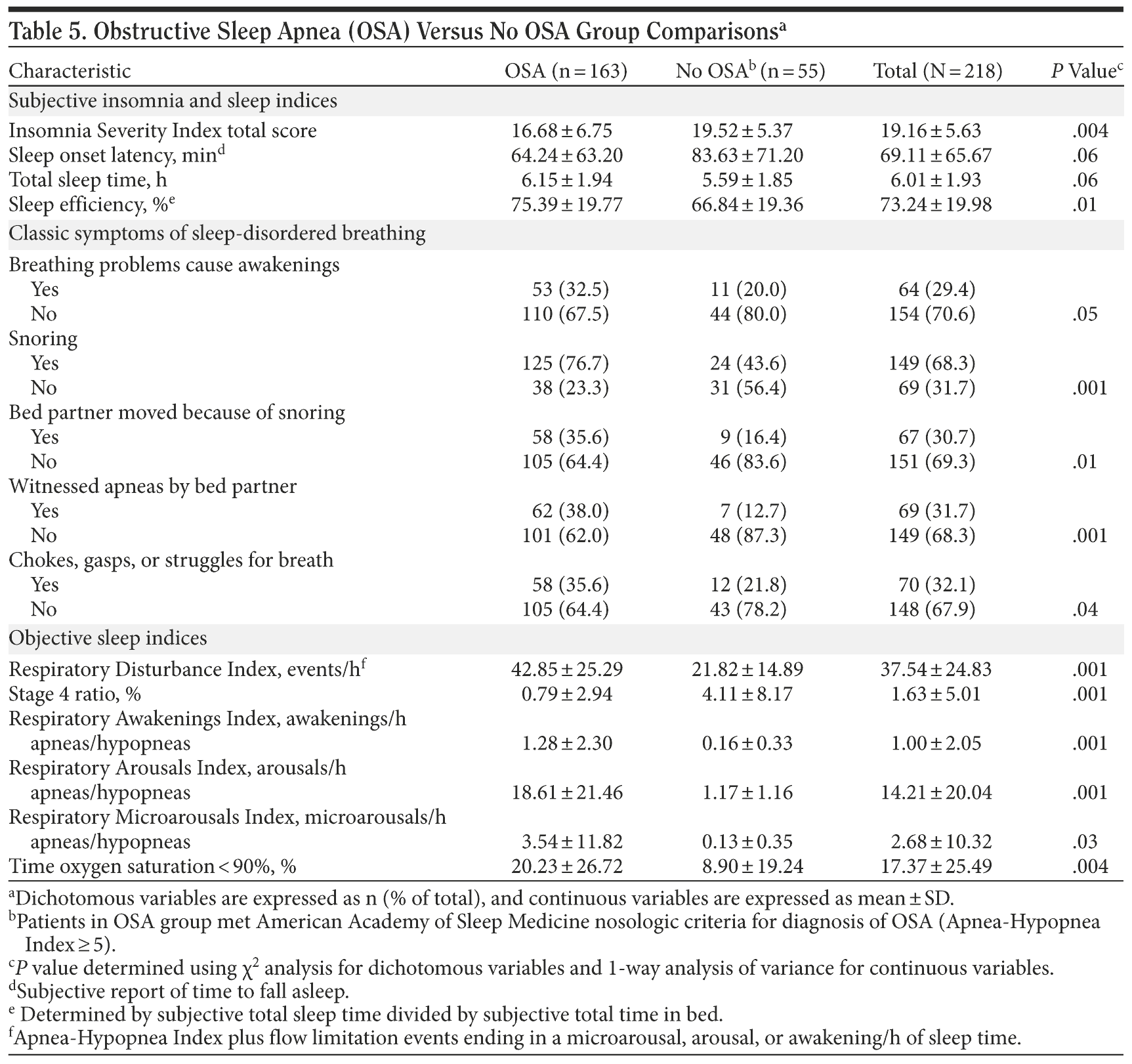
A final analysis was performed comparing those patients meeting AASM nosology for the diagnosis of OSA (AHI ≥ 5) and those who did not (AHI < 5). Significant or trending differences are found in Table 5. In sum, OSA patients were older and more likely to be men and overweight. Patients with OSA were more likely to report classic breathing symptoms including snoring, history of moving from the bed because of patient’s snoring, witnessed apneas, and choking, gasping, or struggling for breath during sleep.
Subjective sleep indices showed the following: OSA patients trended toward shorter sleep-onset latency, longer total sleep time, and more consolidated sleep efficiency. Interestingly, insomnia severity based on mean ± SD total ISI score was worse in the non-OSA group (19.52 ± 5.37) than in the OSA group (16.68 ± 6.75, P = .004, d = 0.47). Objective measures show expected results of worse values in the OSA group compared to the non-OSA group (Table 5).
Last, we compared all of our subjective sleep data for the 40 individuals who were excluded for not undergoing polysomnography testing with those 218 patients in our study, and we found no significant differences on any variable between the 2 groups.
DISCUSSION
In this retrospective chart review, there were 3 primary findings in this consecutive series of treatment-resistant chronic insomnia patients who averaged reports of insomnia for more than a decade and regular use of prescription medication for sleep for 4 years. First, the findings of moderate to severe residual insomnia clearly indicated a failure to respond adequately to sleep medications. Second, patients reporting psychiatric problems were far more common than insomnia patients without such complaints, but there were only a few differences between these groupings in contrast to what we had predicted. Third, objective polysomnography diagnosed obstructive sleep apnea in three-fourths of this select sample along with the innate sleep fragmentation that invariably accompanies this disorder of sleep respiration. However, despite the potential importance of these findings, no systematic links unequivocally connected psychiatric influences or SDB to the etiology or severity of the residual insomnia reported by this sample.
Regarding psychiatric influences, the only distinctions were that the psychiatric insomnia group believed their sleep maintenance insomnia and daytime impairment were worse than the insomnia group, and the psychiatric insomnia group showed a trend toward worse daytime fatigue. Similarly, there were only a few differences with respect to objective findings on sleep stage comparisons; but these findings might be related to greater use of psychotropic medications in the psychiatric insomnia group.32,34 The most relevant objective finding was that the psychiatric insomnia group (comprised of more women) showed a greater severity of flow limitation or upper airway resistance compared to the insomnia group (comprised of more men) that showed greater apneas and hypopneas.
Regarding medical influences on chronic insomnia, the current study revealed that many of these patients suffered from SDB, the most common medical cause of sleep fragmentation,20 and among the OSA group, 75% reported snoring and one-third of these patients reported various breathing symptoms suggestive of OSA. Yet, it remains unclear to what extent these breathing symptoms had been discussed or evaluated prior to seeking care at our sleep medical center. Our lack of a longitudinal design prevents us from knowing whether use of sleeping pills worsened OSA through respiratory depressant effects35 or whether these medications ameliorated some of the sleep-fragmenting effects of OSA by raising arousal thresholds.36 Also, as the study was conducted at 5,200 ft above sea level, altitude may be a contributing factor to increased OSA and central sleep apnea events. We could speculate that therapeutic application of positive airway pressure therapy, the gold standard treatment for SDB, would influence insomnia outcomes or alter medication use or dosage, but there are only a few weakly designed studies20,37,38 that report improved insomnia outcomes subsequent to the treatment of OSA.
The current findings are consistent with prior research showing higher than anticipated rates of comorbid insomnia and OSA (“complex insomnia”)39 in a sample of patients who would ordinarily not be expected to suffer from a sleep breathing disorder. Of some potential clinical interest, insomnia severity was less in the OSA group compared to those without OSA, and objective measures on polysomnography testing tended to corroborate this finding, which in our view, further highlights the elusive nature of the pathophysiologic relationship between these 2 common sleep disorders.
The many limitations of this design mandate a cautious interpretation of our findings. Most importantly, this sample may prove to be highly select in that they sought treatment because medications were not working for them, and a lack of response to treatment is a well-known motivator to seek additional help or second opinions when the medical condition is vexing enough to move the patient to action.40 However, due to the design of this study, we cannot state that psychiatric influences or SDB were the causes of the patients’ residual insomnia complaints; we can only state that these influences were present to some degree but are of unknown clinical significance.
Moreover, for psychiatric influences, we only used self-report checklists and did not conduct psychiatric interviews or use psychiatric instruments to make formal diagnoses. As such, our findings on psychiatric influences only suggest information about general distress not about specific diagnostic categories. And, there was no longitudinal data on the interaction between the patients’ psychiatric and insomnia treatments, including psychotherapies or medications, so the snapshot design of the protocol limits our understanding of what transpired with these treatment-resistant insomnia patients prior to their arrival at the sleep center.
Along the same lines, 1 night of polysomnography also reflects a snapshot of sleep stages and breathing events. Again, a longitudinal design with more frequent testing and research-oriented polysomnography protocols as well as the utilization of sleep diaries would likely yield more useful clinical data. Regarding our 2 groups, our sample of nonpsychiatric insomnia patients was notably smaller and contained a greater proportion of men with only a few differences between the 2 groups, all of which might have changed with larger more balanced samples.
Last, we gathered no reliable data on specific drug dosages for insomnia used by these patients, which clearly could have influenced outcomes given that many patients do not take their medications consistently as prescribed.41,42 Moreover, the psychiatric insomnia group consistently and significantly was taking multiple psychotropic drugs compared to the insomnia group. Overall, our findings may not be generalizable to other chronic insomnia patients taking various sleep medications on a long-term basis, particularly in light of the successes that have been described in the research literature for the long-term use of newer sedative medications.
CONCLUSIONS
To our knowledge, this is the first study to examine pertinent outcomes in a sample of chronic insomnia patients maintaining nightly prescription medication for sleep despite clear-cut signs of treatment-resistant insomnia. The scientific literature does not contain much information about such patients perhaps due to a lack of interest or reluctance to look at treatment outcomes in this difficult patient population.43 Nonetheless, our study demonstrated the value in both the AASM and FDA guidelines,12,17,18 because our findings suggest psychiatric and medical factors may be associated with patients who are not responding optimally to therapy. In particular, the sleep fragmentation effects of both psychiatric and medical conditions, such as those described in this study, may prove to be important influences in these cases. Although it is tempting to imagine that additional assessment and treatments for either sleep breathing or psychiatric conditions would lead to greater improvement in insomnia severity among this select sample of patients, only randomized controlled trials with evidence-based therapies can address such speculations.
Drug names: alprazolam (Niravam, Xanax, and others), bupropion (Aplenzin, Wellbutrin, and others), clonazepam (Klonopin and others), diazepam (Diastat, Valium, and others), escitalopram (Lexapro and others), eszopiclone (Lunesta), fluoxetine (Prozac and others), flurazepam (Dalmane and others), haloperidol (Haldol and others), lorazepam (Ativan and others), olanzapine (Zyprexa), paroxetine (Pexeva, Paxil, and others), ramelteon (Rozerem), sertraline (Zoloft and others), temazepam (Restoril and others), venlafaxine (Effexor and others), zaleplon (Sonata and others), zolpidem (Ambien, Zolpimist, and others).
Author affiliations: Sleep and Human Health Institute, Maimonides Sleep Arts & Sciences, Ltd (all authors); and Los Alamos Medical Center Sleep Laboratory (Dr Krakow), Albuquerque, New Mexico.
Potential conflicts of interest: Dr Krakow owns and operates 3 Web sites that provide education and offer products and services for patients with sleep disorders (http://www.nightmaretreatment.com, http://www.sleeptreatment.com, and http:www.sleepdynamictherapy.com); markets and sells 3 books for patients with sleep disorders (Insomnia Cures, Turning Nightmares Into Dreams, and Sound Sleep, Sound Mind); owns and operates Maimonides Sleep Arts & Sciences, Ltd; and serves as president of a nonprofit sleep research center, the Sleep & Human Health Institute, which occasionally provides consultation services. Messrs Ulibarri and Romero report no financial or other affiliations relevant to the subject of this article.
Funding/support: None reported.
REFERENCES
1. Ring D. Management of chronic insomnia in the elderly. Clin Excell Nurse Pract. 2001;5(1):13-16. PubMed
2. Szelenberger W, Soldatos C. Sleep disorders in psychiatric practice. World Psychiatry. 2005;4(3):186-190. PubMed
3. Maher MJ, Rego SA, Asnis GM. Sleep disturbances in patients with post-traumatic stress disorder: epidemiology, impact and approaches to management. CNS Drugs. 2006;20(7):567-590. PubMed doi:10.2165/00023210-200620070-00003
4. Schwartz JR, Roth T. Shift work sleep disorder: burden of illness and approaches to management. Drugs. 2006;66(18):2357-2370. PubMed doi:10.2165/00003495-200666180-00007
5. Kupfer DJ, Reynolds CF III. Management of insomnia. N Engl J Med. 1997;336(5):341-346. PubMed doi:10.1056/NEJM199701303360506
6. Morin CM, Beaulieu-Bonneau S, LeBlanc M, et al. Self-help treatment for insomnia: a randomized controlled trial. Sleep. 2005;28(10):1319-1327. PubMed
7. Roehrs T, Papineau K, Rosenthal L, et al. Ethanol as a hypnotic in insomniacs: self administration and effects on sleep and mood. Neuropsychopharmacology. 1999;20(3):279-286. PubMed doi:10.1016/S0893-133X(98)00068-2
8. Murtagh DR, Greenwood KM. Identifying effective psychological treatments for insomnia: a meta-analysis. J Consult Clin Psychol. 1995;63(1):79-89. PubMed doi:10.1037/0022-006X.63.1.79
9. Holbrook AM, Crowther R, Lotter A, et al. The diagnosis and management of insomnia in clinical practice: a practical evidence-based approach. CMAJ. 2000;162(2):216-220. PubMed
10. Morin AK. Strategies for treating chronic insomnia. Am J Manag Care. 2006;12(suppl 8):S230-S245. PubMed
11. Smith MT, Perlis ML, Park A, et al. Comparative meta-analysis of pharmacotherapy and behavior therapy for persistent insomnia. Am J Psychiatry. 2002;159(1):5-11. PubMed doi:10.1176/appi.ajp.159.1.5
12. Schutte-Rodin S, Broch L, Buysse D, et al. Clinical guideline for the evaluation and management of chronic insomnia in adults. J Clin Sleep Med. 2008;4(5):487-504. PubMed
13. Brooks D, Prothero W, Bouras N, et al. Trazodone: a comparison of single night-time and divided daily dosage regimens. Psychopharmacology (Berl). 1984;84(1):1-4. PubMed doi:10.1007/BF00432013
14. Becker PM. Treatment of sleep dysfunction and psychiatric disorders. Curr Treat Options Neurol. 2006;8(5):367-375. PubMed doi:10.1007/s11940-006-0026-6
15. US Food and Drug Administration. Ambien CR approval letter. 2005 http://www.fda.gov/cder/foi/appletter/2005/021774ltr.pdf. Accessed June 2008.
16. US Food and Drug Administration. Lunesta approval letter. 2008. http://www.fda.gov/cder/foi/appletter/2004/021476ltr.pdf. Accessed June 2008.
17. US Food and Drug Administration. Ambien. Highlights of prescribing information. http://www.accessdata.fda.gov/drugsatfda_docs/label/2007/019908s022lbl.pdf. Accessed July 2010.
18. US Food and Drug Administration. Lunesta (eszopiclone) tablets.http://www.fda.gov/Safety/MedWatch/SafetyInformation/Safety-RelatedDrugLabelingChanges/ucm106688.htm. Accessed July 2010.
19. Botteman MF, Ozminkowski RJ, Wang S, et al. Cost effectiveness of long-term treatment with eszopiclone for primary insomnia in adults: a decision analytical model. CNS Drugs. 2007;21(4):319-334. PubMed doi:10.2165/00023210-200721040-00005
20. Guilleminault C, Palombini L, Poyares D, et al. Chronic insomnia, premenopausal women and sleep disordered breathing, part 2: comparison of nondrug treatment trials in normal breathing and UARS post menopausal women complaining of chronic insomnia. J Psychosom Res. 2002;53(1):617-623. PubMed doi:10.1016/S0022-3999(02)00463-4
21. Krakow B, Melendrez D, Warner TD, et al. Signs and symptoms of sleep-disordered breathing in trauma survivors: a matched comparison with classic sleep apnea patients. J Nerv Ment Dis. 2006;194(6):433-439. PubMed doi:10.1097/01.nmd.0000221286.65021.e0
22. Krakow BJ, Melendrez DC, Johnston LG, et al. Sleep dynamic therapy for Cerro Grande fire evacuees with posttraumatic stress symptoms: a preliminary report. J Clin Psychiatry. 2002;63(8):673-684. PubMed
23. Krakow B, Melendrez D, Pedersen B, et al. Complex insomnia: insomnia and sleep-disordered breathing in a consecutive series of crime victims with nightmares and PTSD. Biol Psychiatry. 2001;49(11):948-953. PubMed doi:10.1016/S0006-3223(00)01087-8
24. Sivertsen B, Omvik S, Pallesen S, et al. Sleep and sleep disorders in chronic users of zopiclone and drug-free insomniacs. J Clin Sleep Med. 2009;5(4):349-354. PubMed
25. Krakow B, Melendrez D, Ferreira E, et al. Prevalence of insomnia symptoms in patients with sleep-disordered breathing. Chest. 2001;120(6):1923-1929. PubMed doi:10.1378/chest.120.6.1923
26. Bastien CH, Valliרres A, Morin CM. Validation of the Insomnia Severity Index as an outcome measure for insomnia research. Sleep Med. 2001;2(4):297-307. PubMed doi:10.1016/S1389-9457(00)00065-4
27. Lee KA, Hicks G, Nino-Murcia G. Validity and reliability of a scale to assess fatigue. Psychiatry Res. 1991;36(3):291-298. PubMed doi:10.1016/0165-1781(91)90027-M
28. Zallek SN, Redenius R, Fisk H, et al. A single question as a sleepiness screening tool. J Clin Sleep Med. 2008;4(2):143-148. PubMed
29. Rechtschaffen A, Kales A. A Manual of Standardized Terminology, Techniques and Scoring System for Sleep Stages of Human Subjects. Los Angeles, CA: Brain Information Service/Brain Research Institute; 1968.
30. American Academy of Sleep Medicine. International Classification of Sleep Disorders: Diagnostic and Coding Manual. 2nd ed. Westchester, IL: American Academy of Sleep Medicine; 2005.
31. Hosselet J, Ayappa I, Norman RG, et al. Classification of sleep-disordered breathing. Am J Respir Crit Care Med. 2001;163(2):398-405. PubMed
32. Oberndorfer S, Saletu-Zyhlarz G, Saletu B. Effects of selective serotonin reuptake inhibitors on objective and subjective sleep quality. Neuropsychobiology. 2000;42(2):69-81. PubMed doi:10.1159/000026676
33. Riedel BW, Winfield CF, Lichstein KL. First night effect and reverse first night effect in older adults with primary insomnia: does anxiety play a role? Sleep Med. 2001;2(2):125-133. PubMed doi:10.1016/S1389-9457(00)00054-X
34. Sharpley AL, Cowen PJ. Effect of pharmacologic treatments on the sleep of depressed patients. Biol Psychiatry. 1995;37(2):85-98. PubMed doi:10.1016/0006-3223(94)00135-P
35. Hedemark LL, Kronenberg RS. Flurazepam attenuates the arousal response to CO2 during sleep in normal subjects. Am Rev Respir Dis. 1983;128(6):980-983. PubMed
36. Lu B, Budhiraja R, Parthasarathy S. Sedating medications and undiagnosed obstructive sleep apnea: physician determinants and patient consequences. J Clin Sleep Med. 2005;1(4):367-371. PubMed
37. Krakow B, Melendrez D, Sisley B, et al. Nasal dilator strip therapy for chronic sleep maintenance insomnia: a case series. Sleep Breath. 2004;8(3):133-140. PubMed doi:10.1055/s-2004-834483
38. Krakow B, Melendrez D, Lee SA, et al. Refractory insomnia and sleep-disordered breathing: a pilot study. Sleep Breath. 2004;8(1):15-29. PubMed doi:10.1007/s11325-004-0015-5
39. Benetó A, Gomez-Siurana E, Rubio-Sanchez P. Comorbidity between sleep apnea and insomnia. Sleep Med Rev. 2009;13(4):287-293. PubMed doi:10.1016/j.smrv.2008.09.006
40. Meyer D, Leventhal H, Gutmann M. Common-sense models of illness: the example of hypertension. Health Psychol. 1985;4(2):115-135. PubMed doi:10.1037/0278-6133.4.2.115
41. Cooper C, Bebbington P, King M, et al. Why people do not take their psychotropic drugs as prescribed: results of the 2000 National Psychiatric Morbidity Survey. Acta Psychiatr Scand. 2007;116(1):47-53. PubMed doi:10.1111/j.1600-0447.2006.00974.x
42. Mitchell AJ. Adherence behaviour with psychotropic medication is a form of self-medication. Med Hypotheses. 2007;68(1):12-21. PubMed doi:10.1016/j.mehy.2006.07.005
43. Kramer M. Hypnotic medication in the treatment of chronic insomnia: non nocere! Doesn’ t anyone care? Sleep Med Rev. 2000;4(6):529-541. PubMed doi:10.1053/smrv.2000.0122