Objective: Repetitive skin picking that culminates in skin lesions and excoriations has a fairly common prevalence and causes clinically significant distress. Myriads of agents have been used to treat the condition with no convincing results.
Methods: Ten patients (8 women and 2 men) with skin-picking disorder (per DSM-5 criteria) were enrolled in the study. The study was conducted from December 1, 2013, to December 29, 2014. The patients were treated with 12-week open-label topiramate in a titrating-upward dose (25-200 mg/d). Different measures to evaluate the efficacy of topiramate included subjective and objective assessment, photographs, the Skin Picking Scale modified after the Yale-Brown Obsessive-Compulsive Scale (SPS-Y-BOCS), the Skin Picking Impact Scale, the Clinical Global Impressions-Improvement (CGI-I) and CGI-Severity scales, and the Beck Anxiety Inventory and Beck Depression Inventory.
Results: Topiramate improved time spent skin picking from 85 minutes to 30 minutes per day. Seven patients (70%) were very much improved (n = 4) and much improved (n = 30) on the CGI-I. The scores on the Skin Picking Impact Scale and SPS-Y-BOCS also improved. The mean time to respond to topiramate was about 8 to 10 weeks. Anxiety and depression symptoms improved after reduction in skin-picking symptoms (the Beck Anxiety Inventory score improved from a mean of 38.8 to 13.8 and the Beck Depression Inventory score from 28.9 to 10.1).
Conclusions: Topiramate appears to be a promising agent in the treatment of skin-picking symptoms. Double-blind controlled trials are needed to further evaluate the safety and efficacy of topiramate in larger population samples.
Trial Registration: ISRCTN registry identifier: ISRCTN15791118
Use of Topiramate in Skin-Picking Disorder: A Pilot Study

ABSTRACT
Objective: Repetitive skin picking that culminates in skin lesions and excoriations has a fairly common prevalence and causes clinically significant distress. Myriads of agents have been used to treat the condition with no convincing results.
Methods: Ten patients (8 women and 2 men) with skin-picking disorder (per DSM-5 criteria) were enrolled in the study. The study was conducted from December 1, 2013, to December 29, 2014. The patients were treated with 12-week open-label topiramate in a titrating-upward dose (25-200 mg/d). Different measures to evaluate the efficacy of topiramate included subjective and objective assessment, photographs, the Skin Picking Scale modified after the Yale-Brown Obsessive-Compulsive Scale (SPS-Y-BOCS), the Skin Picking Impact Scale, the Clinical Global Impressions-Improvement (CGI-I) and CGI-Severity scales, and the Beck Anxiety Inventory and Beck Depression Inventory.
Results: Topiramate improved time spent skin picking from 85 minutes to 30 minutes per day. Seven patients (70%) were very much improved (n = 4) and much improved (n = 30) on the CGI-I. The scores on the Skin Picking Impact Scale and SPS-Y-BOCS also improved. The mean time to respond to topiramate was about 8 to 10 weeks. Anxiety and depression symptoms improved after reduction in skin-picking symptoms (the Beck Anxiety Inventory score improved from a mean of 38.8 to 13.8 and the Beck Depression Inventory score from 28.9 to 10.1).
Conclusions: Topiramate appears to be a promising agent in the treatment of skin-picking symptoms. Double-blind controlled trials are needed to further evaluate the safety and efficacy of topiramate in larger population samples.
Trial Registration: ISRCTN registry identifier: ISRCTN15791118
Prim Care Companion CNS Disord 2017;19(1):16m01961
https://doi.org/10.4088/PCC.16m01961
© Copyright 2017 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Central Michigan University College of Medicine, Saginaw
*Corresponding author: Mohammad Jafferany, MD, Department of Psychiatry, Central Michigan University College of Medicine, 1000 Houghton Ave, Saginaw, MI 48602 ([email protected]).
Skin-picking disorder is characterized by repetitive or compulsive picking of skin on various parts of the body, resulting in raw areas and tissue damage, with accompanying significant distress or functional impairment.1 Different ways to pick skin include excessive scratching, digging, gouging, squeezing, and rubbing healthy skin. Various terms used in the literature to describe skin-picking disorder include pathological skin-picking disorder, dermatillomania, psychogenic excoriation, neurotic excoriation, and impulse-control disorder not otherwise specified.2 Skin picking is typically seen on areas within easy reach of the dominant hand such as the face, scalp, arms, back, abdomen, and extremities.3 Some studies4 have attempted to estimate the exact prevalence rates of skin-picking disorder, with values ranging from 1.4% to 5.4% in the general population and overrepresentation of female patients.
Nonpharmacologic treatments such as habit-reversal therapy, Internet-based treatments, and acceptance-enhanced behavior therapy have shown minimal effectiveness so far. Many pharmacologic treatment modalities, which include selective serotonin reuptake inhibitors, serotonin-norepinephrine reuptake inhibitors, opioid antagonists, atypical antipsychotics, and glutamatergic agents, have also been tried with limited success.4
Due to similarities in symptoms and comorbidity, skin-picking disorder has been suggested to share etiology with a growing list of other neuropsychiatric disorders that make up the obsessive-compulsive spectrum including body dysmorphic disorder, Tourette’s syndrome, and trichotillomania (compulsive hair pulling).5 Multiple lines of evidence have suggested glutamatergic dysfunction in the pathophysiology of the obsessive-compulsive spectrum and efficacy of glutamatergic metabolites in the treatment of repetitive and compulsive disorders.6
Dysfunction in the dopamine reward pathway has also been speculated as a possible cause of skin picking since dopamine agonist drugs such as cocaine and methamphetamine have been associated with an uncontrollable urge to pick the skin among users.7 The promise shown by opioid antagonists such as naltrexone somewhat supports the aforementioned narrative.
Topiramate modulation of γ-aminobutyric acid (GABA)-ergic neurotransmitters in addition to sodium and calcium channels has elicited interest that it might be a useful agent for treating skin-picking disorder.8 Topiramate has been used in treatment of recreational substance addiction and obsessive-compulsive disorder (OCD).7 Due to the limited success of most of the pharmacologic treatments documented in the literature so far, we elected to conduct an open-label trial of topiramate in a series of patients.
METHODS
The design was an open-label, flexible-dose trial that recruited adult psychiatry patients. The study was conducted according to the declaration of Helsinki guidelines, and applicable ethical review committee approval was received (ISRCTN registry identifier: ISRCTN15791118).
Patients were informed about the nature of the study and medication-related side effects, allowing ample opportunity for them to consider all options. Informed consent was obtained from the patients who agreed to take part in the study. Baseline information regarding age, sex, marital status, job, duration of picking, and type of skin picking was collected.
Participants
The participants consisted of 8 women and 2 men, with ages ranging from 18 to 34 years prior to being recruited into the trial. The study was conducted from December 1, 2013, to December 29, 2014. Patients satisfied the following inclusion criteria per the DSM-59: (1) recurrent skin picking resulting in skin lesions; (2) repeated attempts to decrease or stop skin picking; (3) the skin picking causes clinically significant distress or impairment in social, occupational, or other important areas of functioning; (4) the skin picking is not attributable to the physiologic effects of a substance (eg, cocaine) or another medical condition (eg, scabies); and (5) the skin picking is not better explained by symptoms of another mental disorder (eg, delusions or tactile hallucinations in a psychotic disorder, attempts to improve a perceived defect or flaw in appearance in body dysmorphic disorder, stereotypies in stereotypic movement disorder, or intention to harm oneself in nonsuicidal self-injury).

- Treatment of skin-picking disorder is challenging for most physicians.
- Current literature suggests that most pharmacologic treatments for skin-picking disorder have shown limited success.
- A trial of topiramate may help patients with skin-picking disorder.
Exclusion criteria included chronic unstable medical illness, pregnancy or lactation, being on other psychotropic medications, current substance abuse, and psychotherapy in the last 6 weeks. Criteria for past substance abuse was delineated according to the DSM-5.
Procedures
Baseline laboratory values were obtained for every participant at the onset of the study and at 3 months, including pregnancy test, comprehensive metabolic panel, and complete blood count. After a washout period as applicable, patients were initially started on topiramate 25 mg once a day for the first week. The washout period depended on the elimination half-lives of whatever medication the patient was currently taking. Side effects were carefully monitored during the first week, and if a patient tolerated the medication, the dose of topiramate was increased to 25 mg twice a day during the second week. In the next month, the dose was increased to 50 mg twice a day, and, in the third month, the dose was increased to 100 mg twice a day. If the desired effect was obtained at a lower dose, such dose was maintained. One patient dropped out of the study due to intolerable side effects of dizziness and sedation. Careful follow-up was conducted at 2, 4, 6, 8, and 12 weeks.
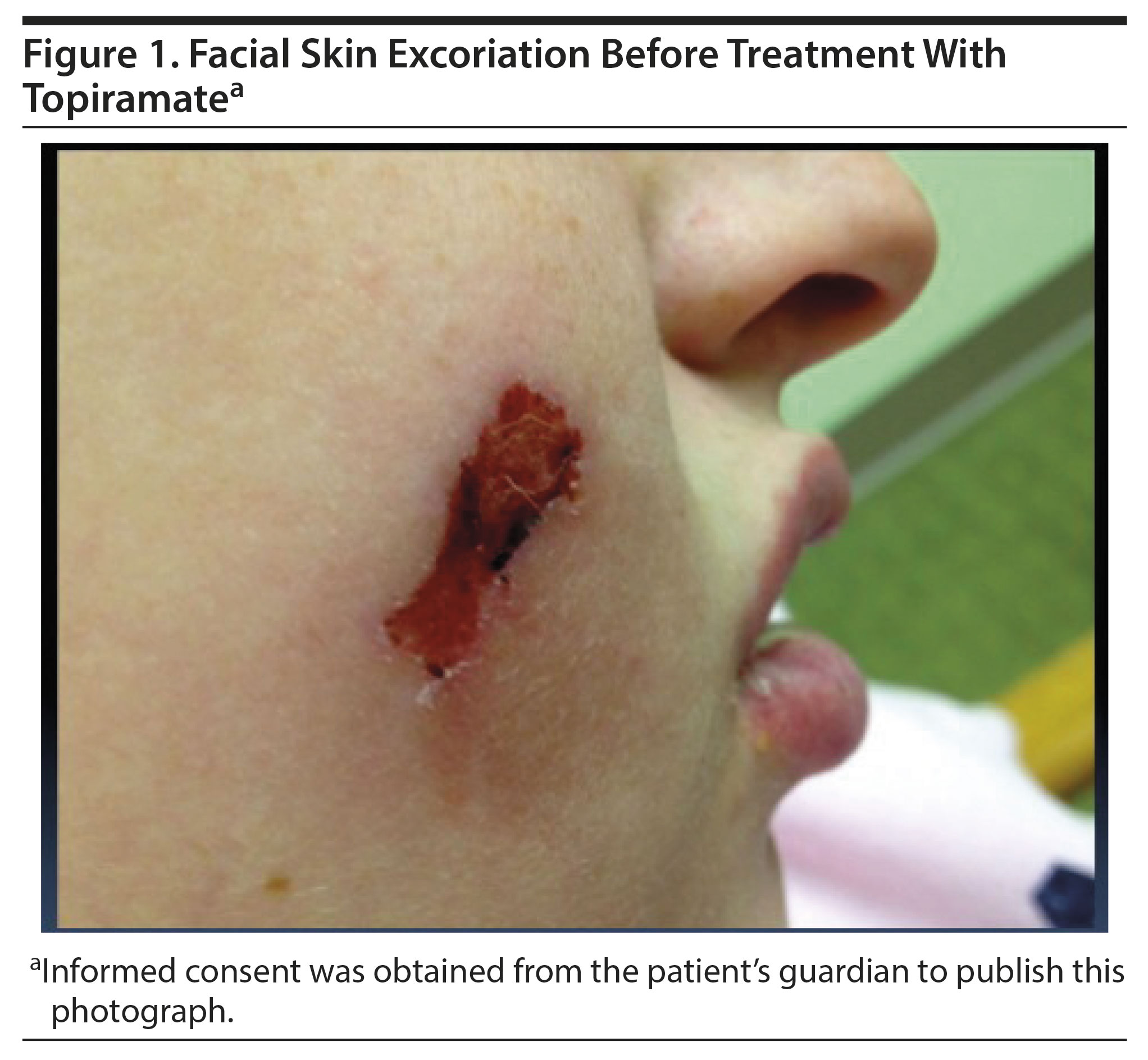
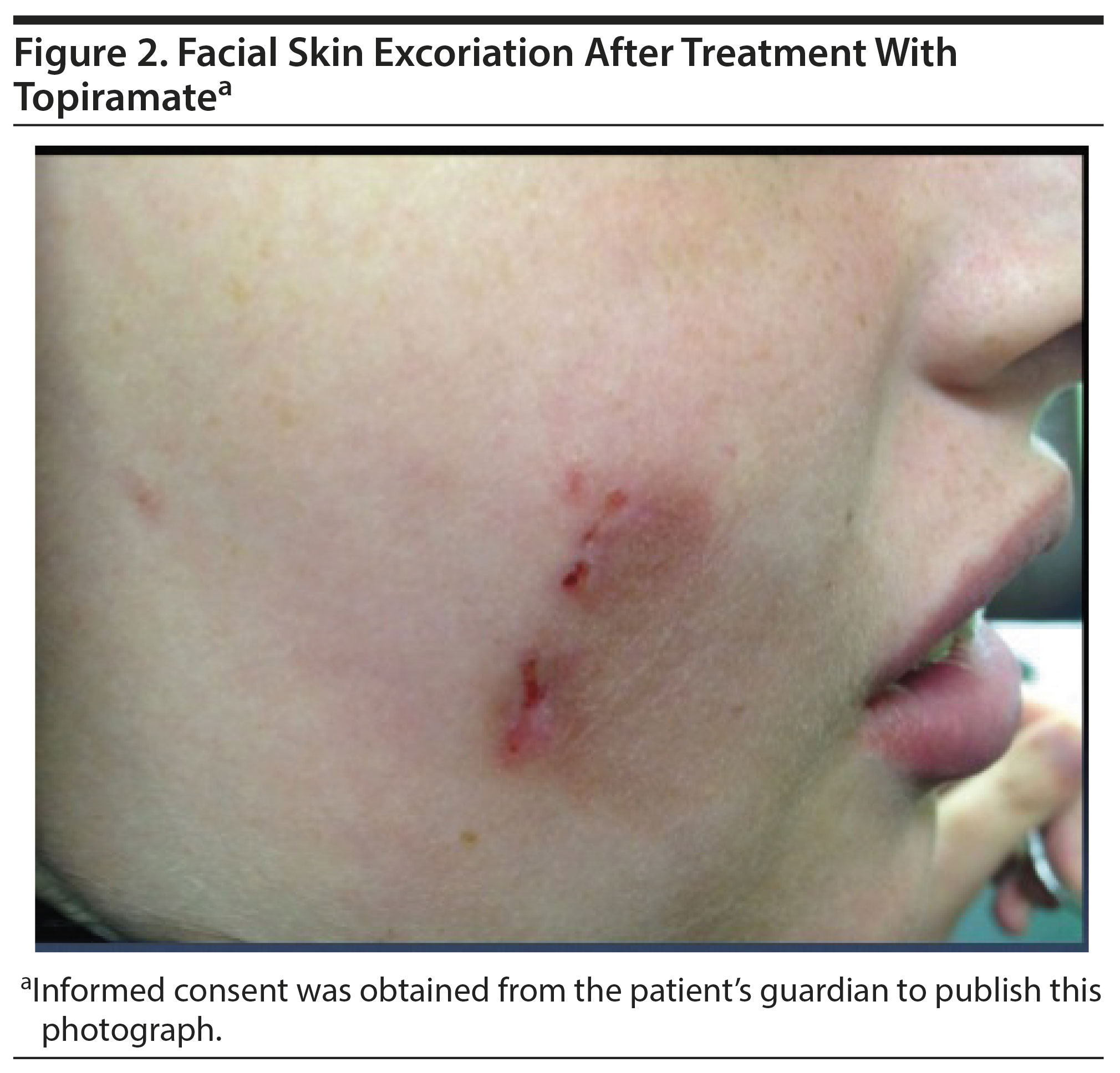
Participants were seen weekly for 2 weeks and every 2 weeks for the remainder of the 12-week open-label study. Representative images of the skin lesion prior to treatment (Figure 1) and with improvement after topiramate (Figure 2) were captured. The primary outcome measure included mean time spent picking per day, as each participant was asked to keep a diary. Secondary efficacy outcomes were measured using the Skin Picking Scale10 modified after the Yale-Brown Obsessive-Compulsive Scale11 (SPS-Y-BOCS), Beck Anxiety Inventory and Beck Depression Inventory,12 Skin Picking Impact Scale,13 and Clinical Global Impressions-Severity (CGI-S) and CGI-Improvement scales.14 No statistical analysis was performed on these data, and results are reported as percentages.
RESULTS
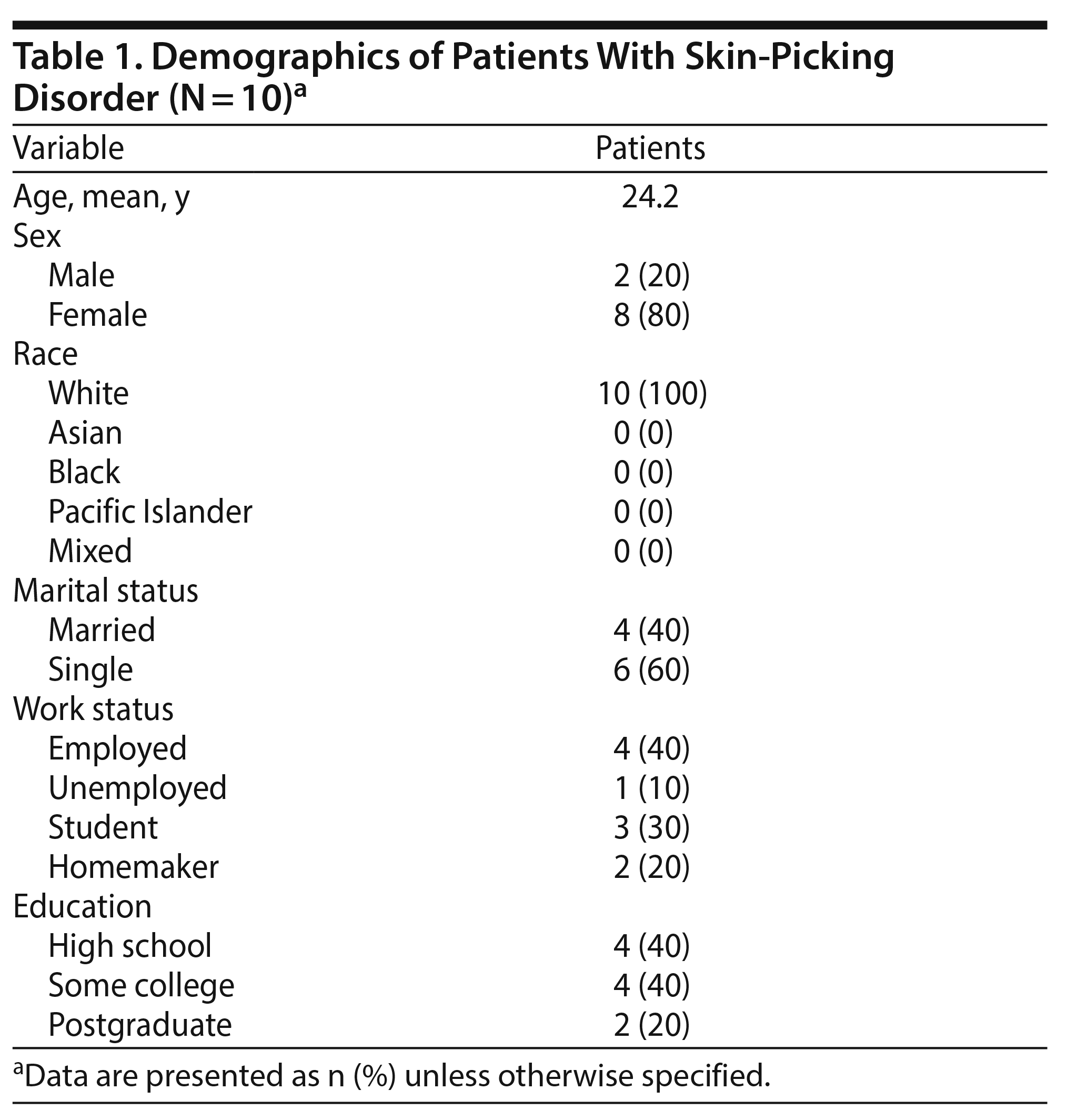
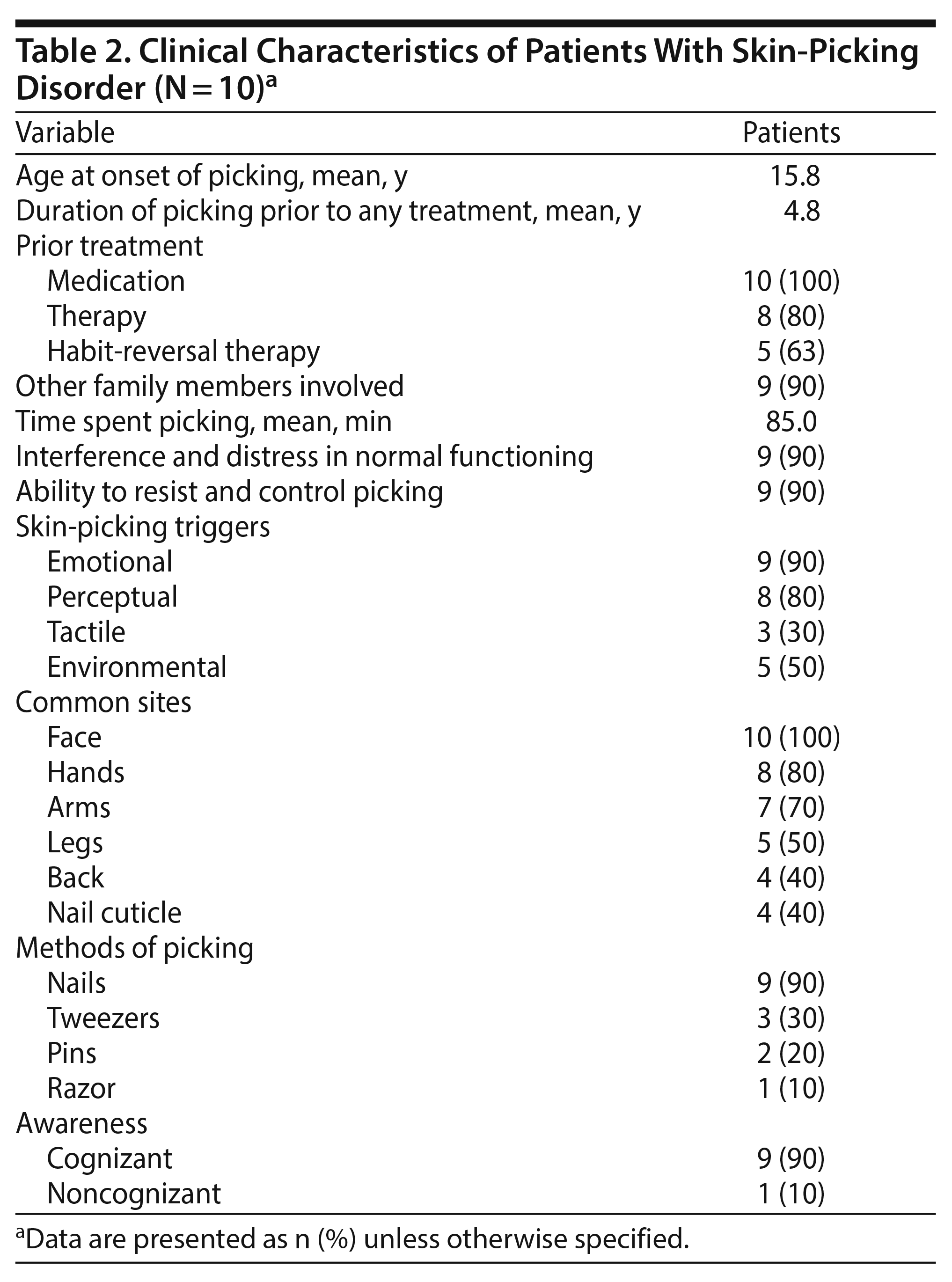
Demographics of the sample are shown in Table 1. The clinical characteristics of the sample are shown in Table 2. The baseline laboratory values and those taken at the end of the study showed no abnormalities. The mean age at onset of skin picking was about 15.8 years (range, 12-34 years). The mean duration of skin picking prior to any treatment was about 4.8 years. Patients reported shame and guilt associated with their skin-picking behavior, which resulted in delay of treatment. All of the participants reported seeking different kinds of treatment for skin-picking behavior prior to the study. All of them had tried different antidepressants, antipsychotics, mood stabilizers, and other medications. The overwhelming majority had received therapy, of which about two-thirds received habit-reversal therapy and more than a third sought cognitive-behavioral therapy with and without medications. About 11/2 hours was the mean duration of skin picking at various times of the day. The majority of the participants reported interference with daily activities and functioning in both social and work areas, as well as being unable to control the urge for picking, including feeling overly anxious, interpersonal rejection, depression, and dysthymia.
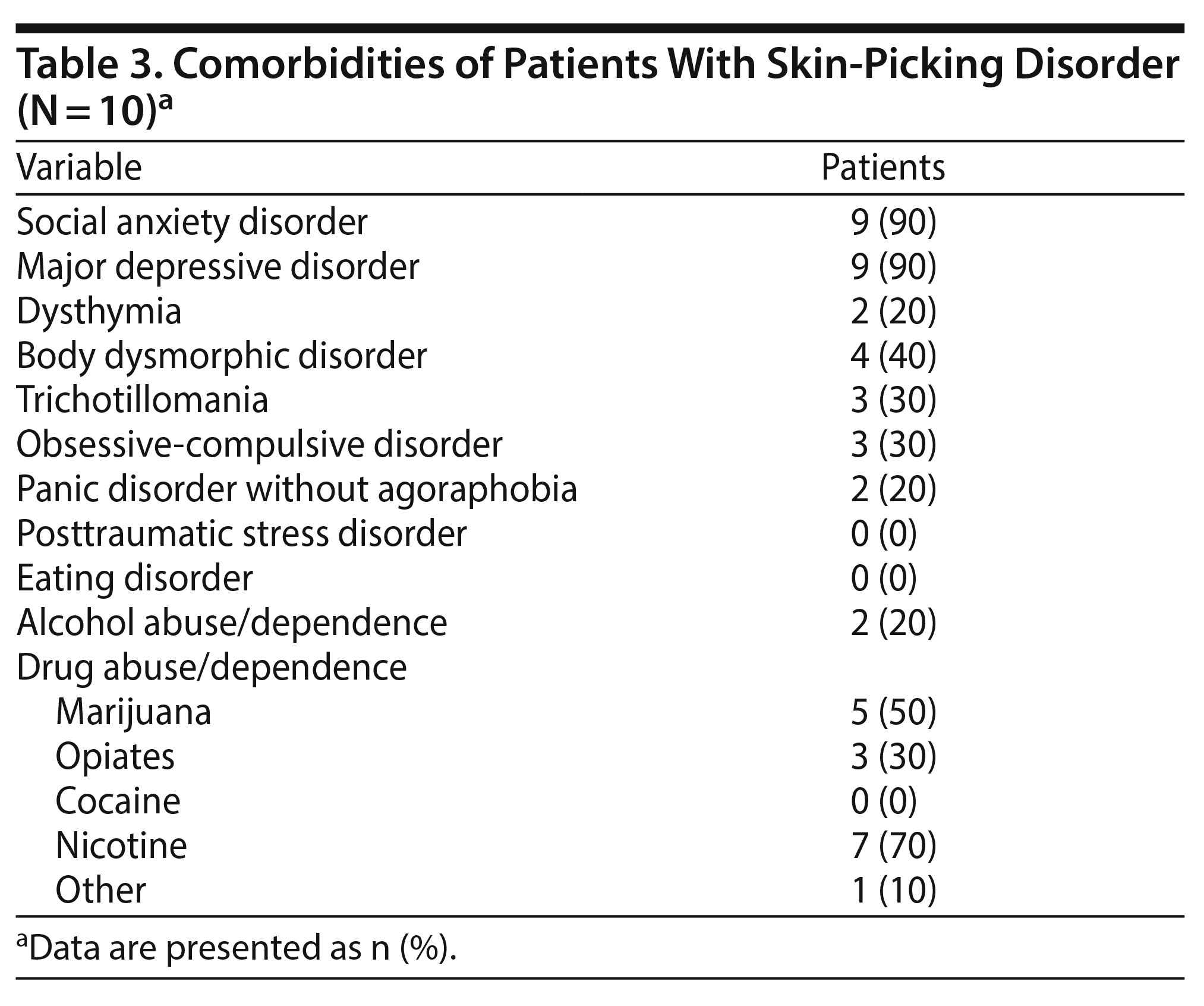
Table 3 outlines the comorbidities associated with skin picking. Some participants felt uneven skin, pimples, scabs, and scars they wanted to get rid of and thus engaged in continuous skin-picking habits. Some participants reported itchiness and uncomfortable sensations on the skin before starting to pick. Various environmental influences also affected the participants’ skin-picking behavior, such as going out to public places, parties, or family gatherings.
The most common site affected was the face, followed by the dorsum of the hands, arms, legs, back, and nail cuticles, respectively. The majority of participants used their nails to pick their skin, but some also used tweezers, pins, and razors, and they were aware of their skin-picking episodes.
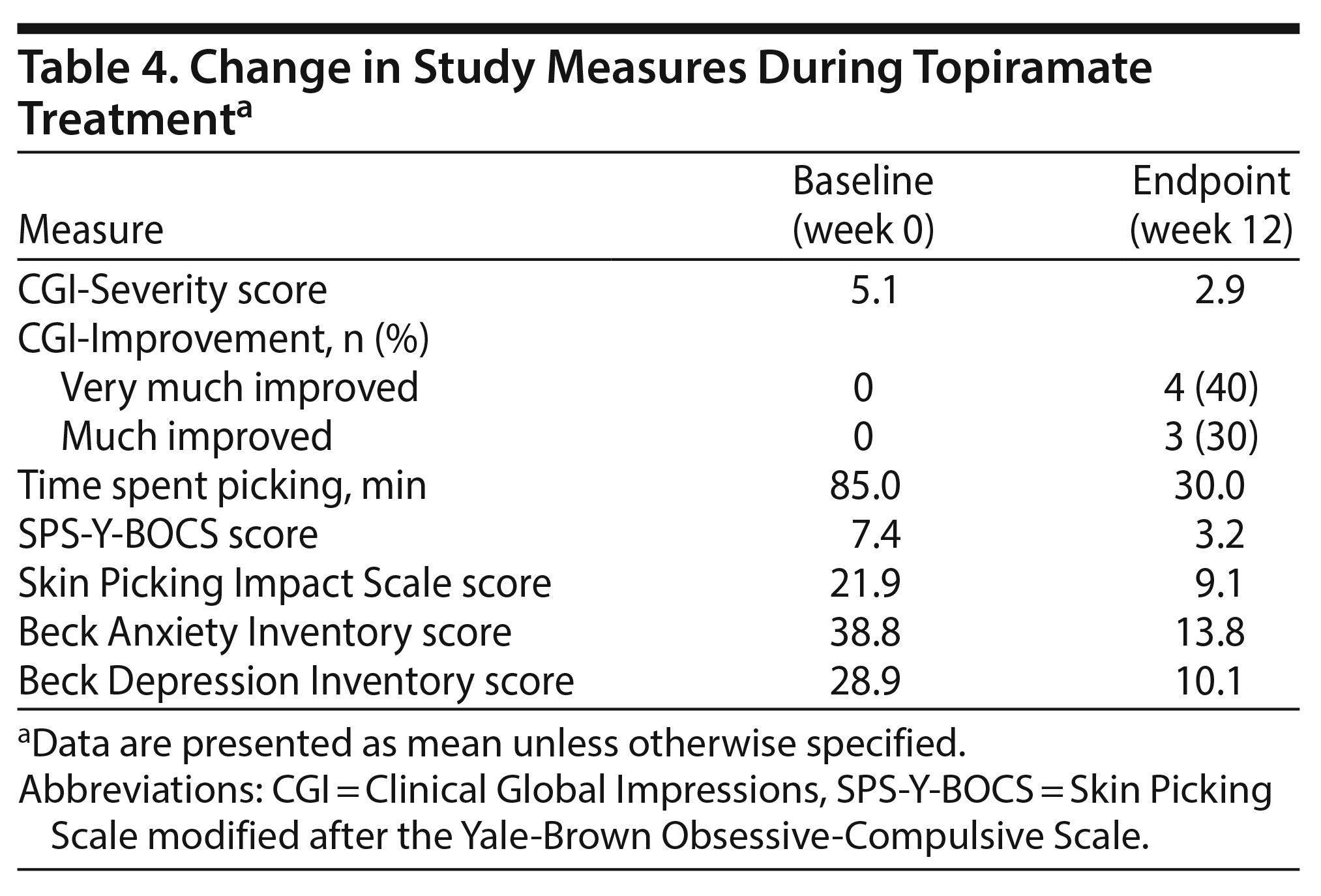
The total time spent skin picking per day was reduced from 85 minutes per day at baseline to 30 minutes per day at the end of the study (Table 4). The CGI-S score improved from 5.1 to 2.9. At the end of the study, 7 patients did not report picking their skin and were much improved (n = 3, 30%) and very much improved (n = 4, 40%) on the CGI-I. Positive effects of topiramate were noted in those participants whose skin-picking symptoms were relatively mild and of short duration, in those who had good family support systems, and in those who were married and more educated. All measures used in this study showed improvement between baseline and end point. The SPS-Y-BOCS score improved from a mean of 7.42 to 3.2, and the Skin Picking Impact Scale score improved from 21.9 to 9.1. The Beck Anxiety Inventory score improved from a mean of 38.8 to 13.8, and the Beck Depression Inventory from 28.9 to 10.1. Topiramate was generally well tolerated. Three patients experienced nausea, drowsiness, headaches, and confusion, which disappeared in a week, thus not warranting exclusion from the study.
DISCUSSION
Topiramate (2,3:4,5-bis-O-[1-methylethylidene]-β-d-fructopyranose sulfamate) exerts inhibitory effects on neuronal excitability and enhances GABAergic neurotransmitters by increasing GABA-mediated chloride influx through GABAA receptors. Topiramate also inhibits sodium and calcium channels, thus decreasing kainite-evoked current through the α-amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid receptor.8 Topiramate has been used in treatment of dopamine reward dysfunction in the addiction spectrum that ranges from alcoholism to methamphetamine and cocaine addiction.7 Topiramate has also been found to be useful in the management of patients with OCD.7 Additional studies are needed to elucidate more clearly the basic mechanistic processes that underlie topiramate efficacy.
Our results showed a preponderance of women at 80%, a mean age at onset of picking of 15.8 years, and a mean time spent picking of 85 minutes, which is similar to what other authors have found.2 The most common skin-picking trigger was emotional (90%), and the most common site of picking was the face, which corresponds with previous studies3 that have revealed that skin picking is typically seen on areas within easy reach of the dominant hand such as the face, scalp, arms, back, abdomen, and extremities.
Odlaug and Grant4 reported that comorbid Axis I psychiatric conditions were found in 38.3% of a patient sample with skin-picking disorder. They also reported trichotillomania (36.7%), compulsive nail biting (26.7%), depressive disorder (16.7%), and OCD (15%) as the most common current comorbid conditions.4 Our findings revealed similar percentages of comorbid disorders, with trichotillomania evident in 30% of the sample. Our cohort of patients, however, had a higher likelihood of having a depressive disorder (90%) and OCD (30%). This finding might be because our entire patient sample had sought treatment for skin picking due to significant interference and distress in normal functioning (90%). In our sample, comorbid substance abuse due to alcohol was 20%, marijuana was 50%, prescription opiates was 30%, and nicotine was 70%.
Limitations of this study include the small sample size, which may suggest caution regarding the generalizability of the study results to the general population. The study was an open-label trial, which might raise concerns for bias. The study sample was made up exclusively of patients who were seeking treatment. Despite that the patients were asked about family history, there was no collateral information obtained to validate the patients’ assertions.
In conclusion, our study suggests that topiramate ameliorates the symptoms observed in skin-picking disorder. Further studies need to be conducted in a larger population sample to validate our findings.
Submitted: April 11, 2016; accepted July 25, 2016.
Published online: January 26, 2017.
Drug names: naltrexone (ReVia and others), topiramate (Topamax and others).
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1. Gelinas BL, Gagnon MM. Pharmacological and psychological treatments of pathological skin picking: a preliminary meta-analysis. J Obsessive Compuls Relat Disord. 2013;2(2):167-175. doi:10.1016/j.jocrd.2013.02.003
2. Odlaug BL, Grant JE. Clinical characteristics and medical complications of pathologic skin picking. Gen Hosp Psychiatry. 2008;30(1):61-66. PubMed doi:10.1016/j.genhosppsych.2007.07.009
3. Jafferany M, Shireen F, Ibrahim A. An open-label trial of topiramate in the treatment of skin picking in pervasive developmental disorder not otherwise specified. Prim Care Companion J Clin Psychiatry. 2010;12(2):doi:10.4088/PCC.09l00829yel. PubMed
4. Odlaug BL, Grant JE. Pathologic skin picking. Am J Drug Alcohol Abuse. 2010;36(5):296-303. PubMed doi:10.3109/00952991003747543
5. Phillips KA. The obsessive-compulsive spectrums. Psychiatr Clin North Am. 2002;25(4):791-809. PubMed doi:10.1016/S0193-953X(02)00024-2
6. Ting JT, Feng G. Glutamatergic synaptic dysfunction and obsessive-compulsive disorder. Curr Chem Genomics. 2008;2:62-75. PubMed doi:10.2174/1875397300802010062
7. Shinn AK, Greenfield SF. Topiramate in the treatment of substance-related disorders: a critical review of the literature. J Clin Psychiatry. 2010;71(5):634-648. PubMed doi:10.4088/JCP.08r04062gry
8. Nakamura J, Kuwana Y, Yukitoshi N. Target pharmacology of topiramate, a new antiepileptic drug [article in Japanese]. Nippon Yakurigaku Zasshi. 2000;115(1):53-57. PubMed doi:10.1254/fpj.115.53
9. American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
10. Keuthen NJ, Wilhelm S, Deckersbach T, et al. The Skin Picking Scale: scale construction and psychometric analyses. J Psychosom Res. 2001;50(6):337-341. PubMed doi:10.1016/S0022-3999(01)00215-X
11. Storch EA, Larson MJ, Price LH, et al. Psychometric analysis of the Yale-Brown Obsessive-Compulsive Scale Second Edition Symptom Checklist. J Anxiety Disord. 2010;24(6):650-656. PubMed doi: 10.1016/j.janxdis.2010.04.010.
12. Leyfer OT, Ruberg JL, Woodruff-Borden J. Examination of the utility of the Beck Anxiety Inventory and its factors as a screener for anxiety disorders. J Anxiety Disord. 2006;20(4):444-458. PubMed doi:10.1016/j.janxdis.2005.05.004
13. Keuthen NJ, Deckersbach T, Wilhelm S, et al. The Skin Picking Impact Scale (SPIS): scale development and psychometric analyses. Psychosomatics. 2001;42(5):397-403. PubMed doi:10.1176/appi.psy.42.5.397
14. Busner J, Targum SD. The Clinical Global Impressions scale: applying a research tool in clinical practice. Psychiatry (Edgmont). 2007;4(7):28-37. PubMed
Enjoy this premium PDF as part of your membership benefits!