Objective: Associations between depression, personality traits, and emotions are complex and reciprocal. The aim of this study is to explore these interactions in dynamical networks and in a linear way over time depending on the severity of depression.
Methods: Participants included 110 patients with depressive symptoms (DSM-5 criteria) who were recruited between October 2015 and February 2016 during their inpatient stay in a general psychiatric hospital in Hall in Tyrol, Austria. The patients filled out the Beck Depression Inventory-II, a German emotional competence questionnaire (Emotionale Kompetenz Fragebogen), Positive and Negative Affect Schedule, and the German versions of the Big Five Inventory-short form and State-Trait-Anxiety-Depression Inventory regarding symptoms, emotions, and personality during their inpatient stay and at a 3-month follow-up by mail. Network and regression analyses were performed to explore interactions both in a linear and a dynamical way at baseline and 3 months later.
Results: Regression analyses showed that emotions and personality traits gain importance for the prediction of depressive symptoms with decreasing symptomatology at follow-up (personality: baseline, adjusted R2 = 0.24, P < .001; follow-up, adjusted R2 = 0.65, P < .001). Network analyses additionally showed that the interaction network of depression, emotions, and personality traits is significantly denser and more interconnected (network comparison test: P = .03) at follow-up than at baseline, meaning that with decreased symptoms interconnections get stronger.
Conclusions: During depression, personality traits and emotions are walled off and not strongly interconnected with depressive symptoms in networks. With decreasing depressive symptomatology, interfusing of these areas begins and interconnections become stronger. This finding has practical implications for interventions in an acute depressive state and with decreased symptoms. The network approach offers a new perspective on interactions and is a way to make the complexity of these interactions more tangible.
Depressive Symptoms and Their Interactions
With Emotions and Personality Traits Over Time:
Interaction Networks in a Psychiatric Clinic
ABSTRACT
Objective: Associations between depression, personality traits, and emotions are complex and reciprocal. The aim of this study is to explore these interactions in dynamical networks and in a linear way over time depending on the severity of depression.
Methods: Participants included 110 patients with depressive symptoms (DSM-5 criteria) who were recruited between October 2015 and February 2016 during their inpatient stay in a general psychiatric hospital in Hall in Tyrol, Austria. The patients filled out the Beck Depression Inventory-II, a German emotional competence questionnaire (Emotionale Kompetenz Fragebogen), Positive and Negative Affect Schedule, and the German versions of the Big Five Inventory–short form and State-Trait-Anxiety-Depression Inventory regarding symptoms, emotions, and personality during their inpatient stay and at a 3-month follow-up by mail. Network and regression analyses were performed to explore interactions both in a linear and a dynamical way at baseline and 3 months later.
Results: Regression analyses showed that emotions and personality traits gain importance for the prediction of depressive symptoms with decreasing symptomatology at follow-up (personality: baseline, adjusted R2 = 0.24, P < .001; follow-up, adjusted R2 = 0.65, P < .001). Network analyses additionally showed that the interaction network of depression, emotions, and personality traits is significantly denser and more interconnected (network comparison test: P = .03) at follow-up than at baseline, meaning that with decreased symptoms interconnections get stronger.
Conclusions: During depression, personality traits and emotions are walled off and not strongly interconnected with depressive symptoms in networks. With decreasing depressive symptomatology, interfusing of these areas begins and interconnections become stronger. This finding has practical implications for interventions in an acute depressive state and with decreased symptoms. The network approach offers a new perspective on interactions and is a way to make the complexity of these interactions more tangible.
Prim Care Companion CNS Disord 2017;19(2):16m02043
https://doi.org/10.4088/PCC.16m02043
© Copyright 2017 Physicians Postgraduate Press, Inc.
aUMIT-Health and Life Sciences University, Institute of Psychology, Hall in Tyrol, Austria
bGeneral Hospital for Psychiatry and Psychotherapy, Hall in Tyrol, Austria
cTeacher Training College, Feldkirch, Vorarlberg, Austria
*Corresponding author: Laura N. Semino, MSc, Eduard-Wallnöfer-Zentrum 1, 6060 Hall in Tyrol, Austria ([email protected]).
Affect impacts various levels of human existence such as thoughts, feelings, and behavior. The same applies to affective disorders, the effects of which, however, are generally unwanted and impact almost every aspect of human existence. Thus, broadening the horizon and encompassing interactions with adjacent psychological constructs such as personality traits or emotions can widen our understanding of the cause and impact of affective disorders in individuals.
Research1–9 showed that depression interacts with personality traits and emotions in several ways and that the distinction between cause and effect of depression and interactions with emotions and personality traits is not always easy to ascertain. The “Big Five” (neuroticism, extraversion, openness, agreeableness, and conscientiousness)1 is an important and well-established model of personality when reporting associations between personality traits and depression. High neuroticism and low conscientiousness and extraversion were found to be associated with depression in meta-analyses.2,3 These domains act as predictors for the development of depression,4 and there is evidence that the connection between personality traits and depression might be bidirectional, meaning that depression also influences personality.3 However, this evidence could also suggest that there is no causal relationship but rather a coevolvement and that the relationship between depression and personality traits is more complex and reciprocal than one would expect.5
Also, associations between emotions and depression are reciprocal, and it is unclear whether emotional deficiencies predict depression, are a consequence of depression, or both. For the development and treatment of depression, emotion-related abilities such as emotion regulation and emotion malleability beliefs play a key role.6 It has been shown that depression is associated with maladaptive emotion-regulation strategies and negative affectivity.7 It was further shown that emotion-regulation difficulties are a predictor of depression over a period of 5 years.8 Another study9 found that experience of depressive symptoms in the past can lead to higher difficulties in emotion regulation.
In regard to clinical practice, single associations are relevant, but the interplay between personality traits, emotions, and depression is also of interest. For example, emotional intensity can explain the association between personality and depressive symptoms.10 High neuroticism facilitates the experiencing of negative emotions, which in turn leads to a higher vulnerability for depression, while high agreeableness leads to higher experiencing of positive emotions, which is a protective factor for depressive symptoms.10 Emotion-regulation deficits were found to be a full mediator for the association between depression and neuroticism,11 meaning that emotion-regulation deficits are the reason for the connection between neuroticism and depression.
All of these results can seem vague to the point that it remains unclear how the mechanism of influence works and especially where the connecting points are located. This may be because most previous studies explored the interactions between personality traits, emotional abilities, and depression by examining one-on-one association only, thus hindering the unearthing of possible direct connections and the dynamics of the associations. The aim of this study is to explore all associations between depression, personality traits, and emotions (affectivity and emotional abilities) dynamically by applying a new method called network analysis12 and to juxtapose this analysis for comparative purposes to classical data analysis. Further, we want to explore whether depression-personality-emotion interactions change depending on the severity of depressive symptoms at a 3-month follow-up.
METHODS
Study Design
The study was conducted at the ward for depressive and anxiety disorders of the general psychiatric hospital in Hall in Tyrol, Austria. Ethical approval was obtained at the local medical ethics committee Innsbruck (AN2015-0116 349/4.8). Participants were recruited between October 2015 and February 2016 during their inpatient stay. Participants gave written informed consent and individually filled out 5 self-report questionnaires (time needed to complete was approximately 40 minutes). A 3-month follow-up was conducted by mail. Participants completed 1 data sheet concerning outpatient treatment and subjective well-being and completed the same 5-questionnaire battery for a second time.
Participants
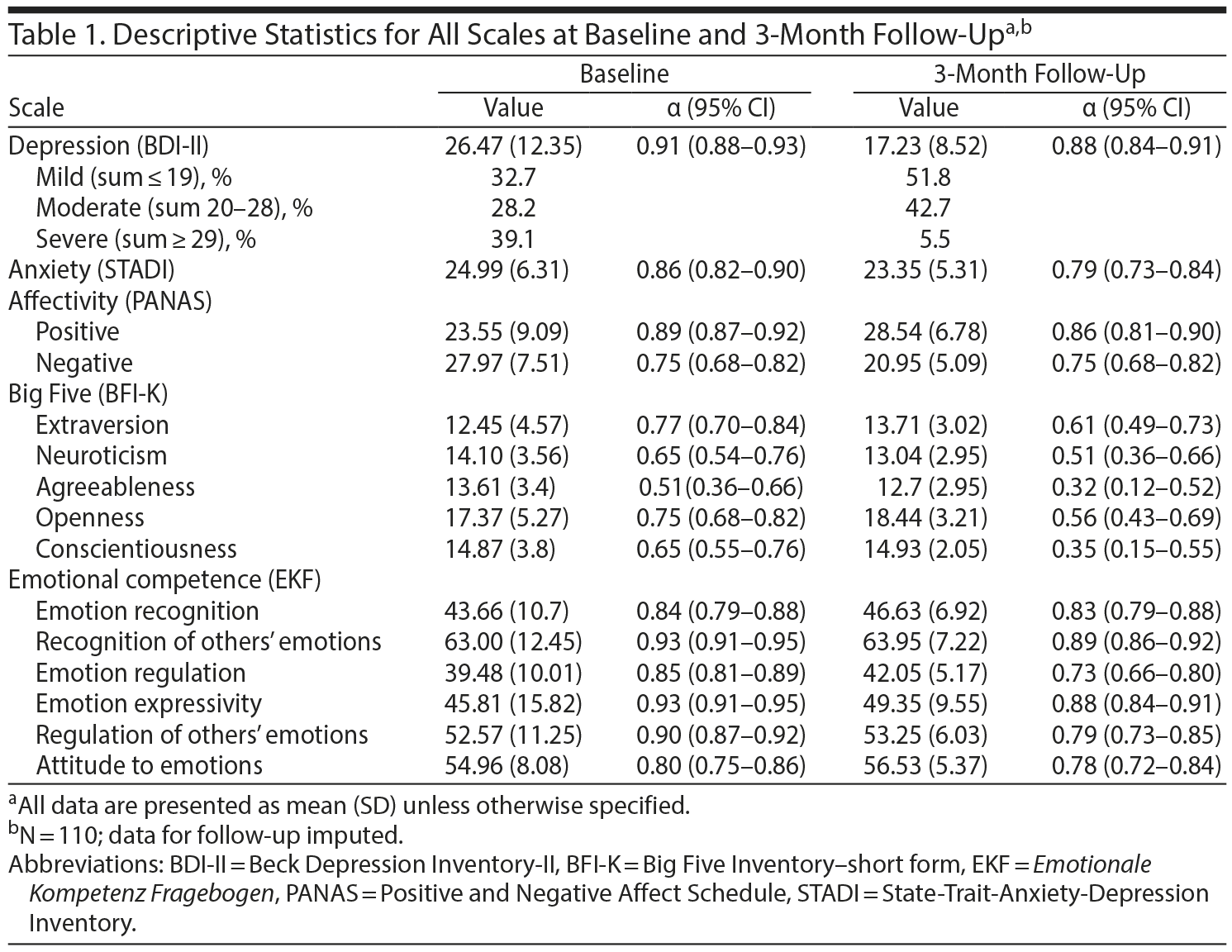
As correlations are the basis of networks, the sample size of N = 110 was chosen to get robust correlations, with a confidence interval of 80%, according to the simulation study by Schönbrodt and Perugini.13 The key inclusion criterion for the study was depressive symptomatology according to the DSM-514 as the primary admission reason for the inpatient stay. All participants were taking antidepressant medication prescribed by psychiatrists during the inpatient stay. For sample homogeneity reasons, patients who had suffered from manic or psychotic symptoms at any time were excluded. Participants (N = 110, 53.6% female) were between 18 and 60 years old with a mean age of 43.2 years (SD = 11.01). The response rate of the 3-month follow-up was 47.27% (n = 52). Of the follow-up participants, 65.38% (n = 34) reported that they were feeling better or much better than during the inpatient stay, 23.07% (n = 12) reported that they were feeling the same, and 11.54% (n = 6) reported feeling worse than 3 months before. Of the participants, 76.92% (n = 40) received further outpatient treatment by a psychiatrist or psychotherapist. All participants were still taking antidepressant medication at follow-up. Because of the lower return rate for the follow-up, imputation of the data was performed in R using the package “mice”15 as recommended best practice.16 Table 1 shows descriptive statistics of all scales and the degree of severity of depressive symptoms17 at baseline and 3-month follow-up.
Measures
The Beck Depression Inventory-II (BDI-II)18 was used to assess depressive symptomatology. The German BDI-II17 shows good internal consistency (α ≥ 0.84) and retest reliability (α ≥ 0.75) and has satisfactory discriminant and convergent validity.19 Twenty-one symptoms are rated between 1 and 3 and result in a sum score of a maximum of 63 points. A sum score > 19 corresponds with moderate depression according to the DSM-5.14,17
The German State-Trait-Anxiety-Depression Inventory (STADI)20 was used to measure anxiety as a trait. The STADI has good internal consistency (α = 0.93). Retest reliability estimates for the trait scales for different time intervals (1 week to 14 months) ranged between rtt = 0.50 and rtt = 0.87.
To measure personality according to the Big Five1 (openness, agreeableness, consciousness, extraversion, and neuroticism), the German Big Five Inventory–short form (BFI-K) was used.21 The BFI-K is a 21-item short version of the Big Five Inventory22 and has good reliability (α = 0.64–0.86) and discriminant and convergent validity.21,23
The Positive and Negative Affect Schedule (PANAS)24 was used to measure general positive and negative affectivity, with the instruction to assess the previous 2 weeks. The questionnaire consists of 20 adjectives rated between 1 (not at all) and 5 (extremely). The PANAS has good construct validity,25 and the German version26 has good internal consistency (α ≥ 0.84).
To measure emotional abilities, the German emotional competence questionnaire Emotionale Kompetenz Fragebogen (EKF)27 was used. The EKF measures emotional competency by the following scales: recognition and comprehension of own emotions, recognition and comprehension of others’ emotions, emotion regulation, emotion expressivity, regulation of others’ emotions, and attitude to emotions.
All scales were optically inspected for normal distribution and showed no violation of normal distribution, with the exception of “positive affectivity” showing right-skewed distribution and “regulation of others’ emotions” showing left-skewed distribution, which does not affect the analyses.
Statistical Analysis
All statistical analyses were performed in the statistical program R version 3.3.128 using routines from the packages psych,29 qgraph,30 mice,15 and bootnet.31
In a first step, raw scores of the items were transformed into factor scores of the scales. Factor scores were used instead of sum scores for all scales because, in general, tau equivalence is a prerequisite but rarely met criterion for using sum scores. Use of sum scores would assume that all symptoms are equally important for a sum score, while the factor score takes the weight of items (symptoms) into account separately. As the network approach underlines this assumption, factor scores were used instead of sum scores.
Second, for classical data analysis, a multiple linear regression, regressing depressive symptoms on emotions and personality, was performed for baseline and follow-up. Preliminary analysis was conducted to ensure there was no violation of the assumption of normality, homoscedasticity, linearity, and multicollinearity. A paired t test was used to calculate the mean difference of depressive symptomatology at baseline and follow-up.
Third, network analysis12 was conducted for depressive symptomatology and for interactions with emotions and personality. Network analysis is a new method to explore interaction in graphs in net-like structures.12 The construction of networks is based on the observed covariance or correlation matrix and can be done in the package qgraph30 in R.32 Variables are entered as nodes in networks. According to their connections (observed correlation or covariance matrix in the sample), connecting lines (called edges) between the variables are plotted.12 Edges can be interpreted according to their color and width. Green edges represent positive connections, and red edges represent negative connections; the thicker an edge between 2 nodes, the stronger the connection. Network regularization is necessary to counteract multiple testing problems.33 The Gaussian graphical model (Graphical Lasso regularization) was used for all networks and sets spurious edges to zero.34 This regularization technique leads to sparse networks and allows interpretation of existing edges as partial correlations (ie, the unique correlation between 2 variables when controlling for all other variables). Regularized networks have high sensitivity, meaning that represented edges can be trusted as true positive or negative edges.34 The second point of interpreting networks is the position of the nodes (variables) in networks. Nodes are placed centrally or peripherally based on the Fruchterman-Reingold algorithm.35 Important nodes for the network are plotted centrally, and less important nodes are plotted peripherally. Centrality parameters (strength, closeness, and betweenness) give additional information about the importance of each node in networks. Centrality parameters are given in z-transformed scores. The higher a degree of a centrality parameter, the more important the node is in the network. Strength of a node gives information about the number of weighted edges (number of edges and width of edges) connected to a node, closeness measures the mean distance from a node to all other nodes, and betweenness measures the extent of a node lying on a connection between 2 other nodes (connectivity function).36 Additionally, stability analysis of all networks was conducted using routines from the package bootnet.31 In stability analysis, the goal is to explore how stable the position of the nodes is in the network, especially for smaller sample sizes. This is to assure that the position of the nodes is not random and allows for the transfer of the results of the networks to other patients (external validity). To compare the 2 networks at baseline and follow-up, the network comparison test37 was applied. The network comparison test analyzes the invariance (ie, the comparability of 2 networks regarding structure, strength, and connections).
RESULTS
First, a multiple linear regression to predict depression through personality and emotions was conducted for baseline and follow-up. Results in Table 2 show that personality (model 2) in the follow-up compared to baseline explains a lot more variance of the depression score. A paired sample t test was conducted to compare depressive symptoms at baseline (mean = 26.47, SD = 12.35) and follow-up (mean = 17.23, SD = 8.52). Depressive symptoms decreased significantly in the follow-up, denoting a large effect according to Cohen38 (t109 = 7.23, P < .001, d = 0.71). Second, network analyses were conducted. For all networks, results were stable concerning centrality parameters.
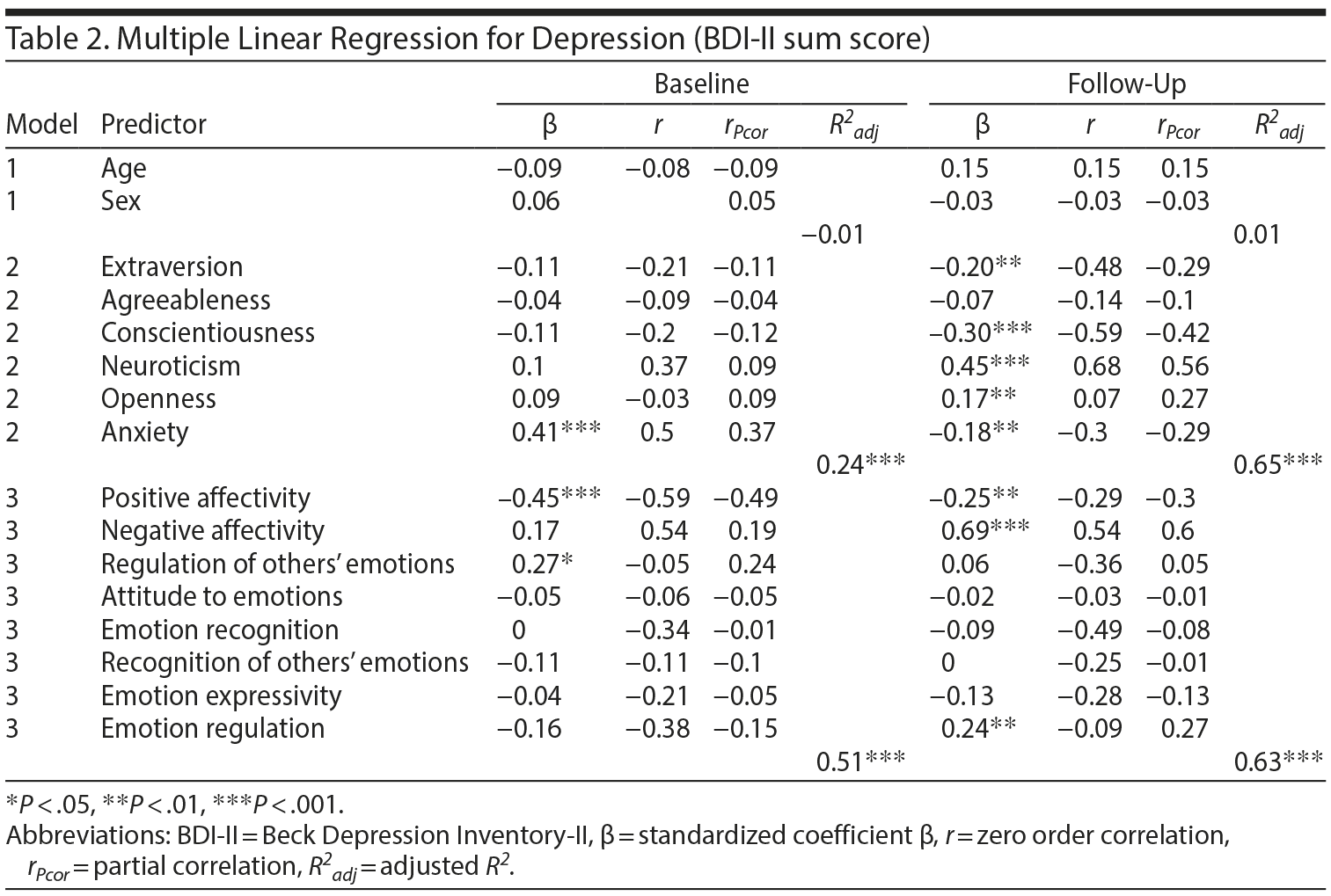
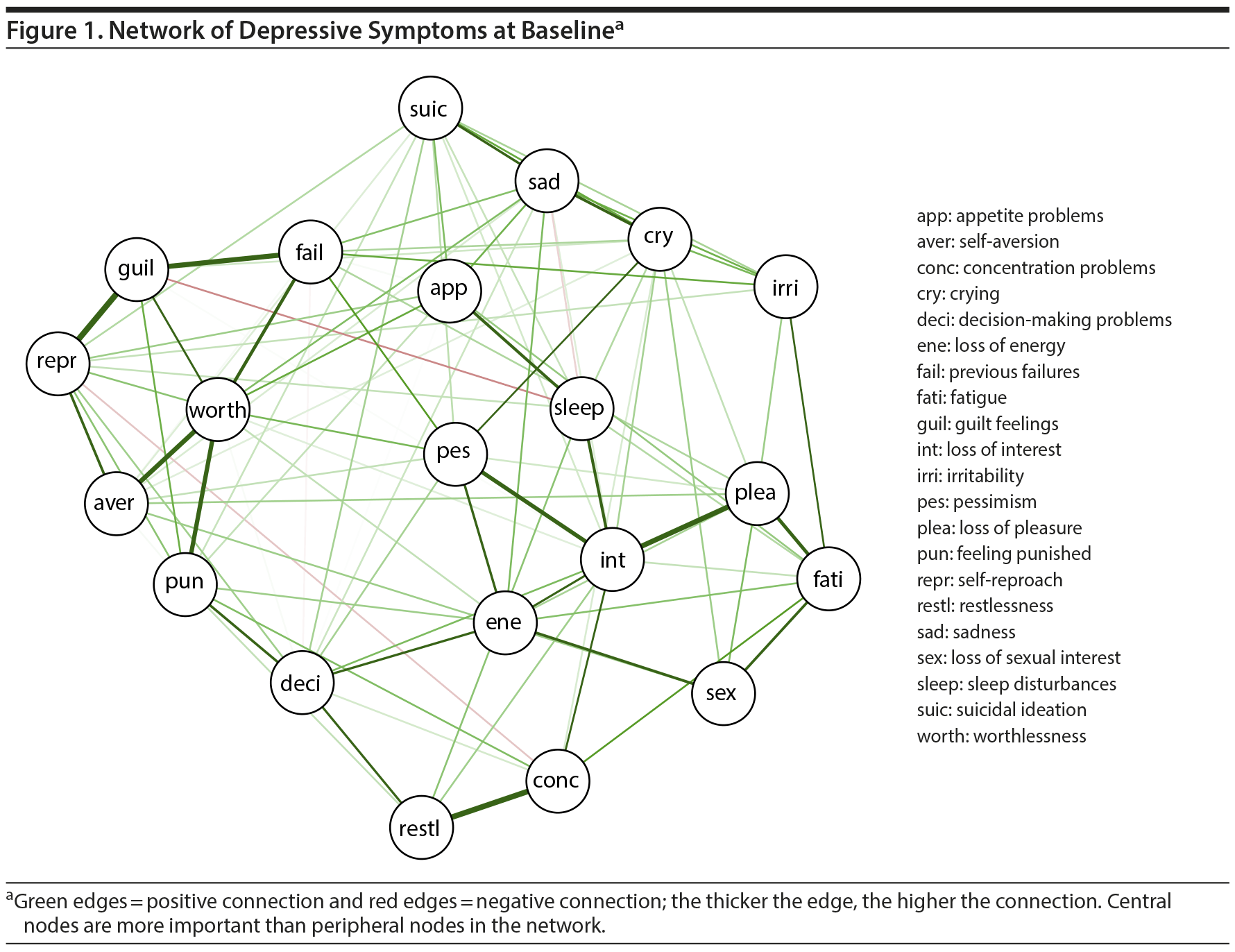
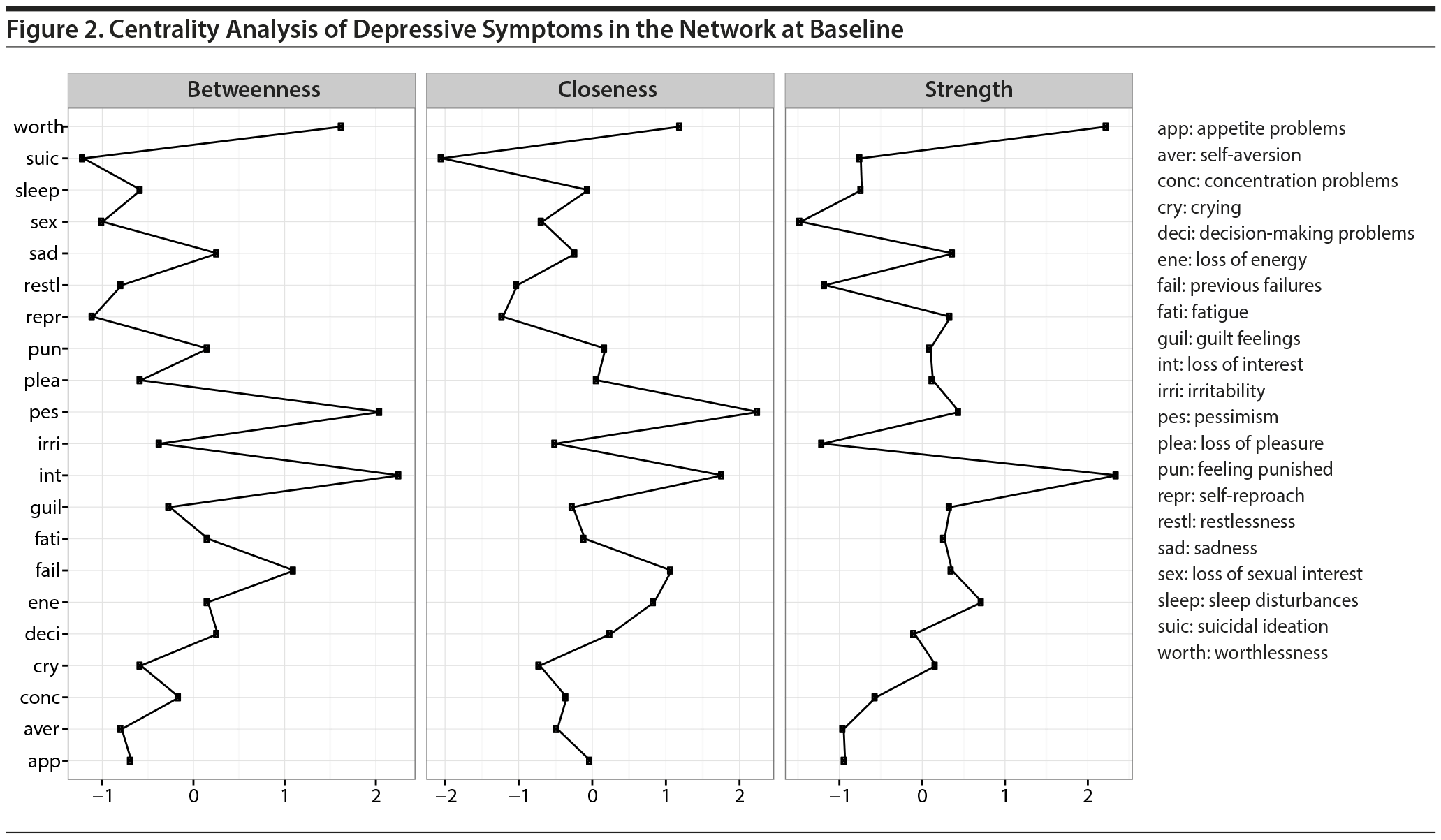
Figure 1 shows depressive symptoms according to the BDI-II at baseline in the network approach. Additionally, centrality parameters per node are given in Figure 2. The most central node in the network (highest closeness degree) is “pessimism.” The graph (Figure 1) shows that pessimism is only 1 or 2 steps away from all other symptoms, while, for example, the path from suicidal ideation (smallest closeness degree) to concentration deficits goes through several other symptoms that are not directly associated to each other. The symptom “loss of interest” has the highest number and the strongest connections to other symptoms (strength). Loss of interest is strongly connected to “being pessimistic” and has a connectivity function in the depressive network; it connects other symptoms the most compared to other variables. Also “worthlessness” has a high strength, and as is apparent from Figure 1 (right side), the symptom is connected to a cluster of other symptoms (feelings of previous failures, self-aversion, or guilt). Thus, if a depressed patient feels worthless, this feeling will be strongly associated to feelings of guilt and self-aversion or vice-versa. To get a dynamical view on interactions, 2 network analyses of depressive symptoms, personality, and emotions were conducted, once for baseline and once for follow-up (Figure 3).
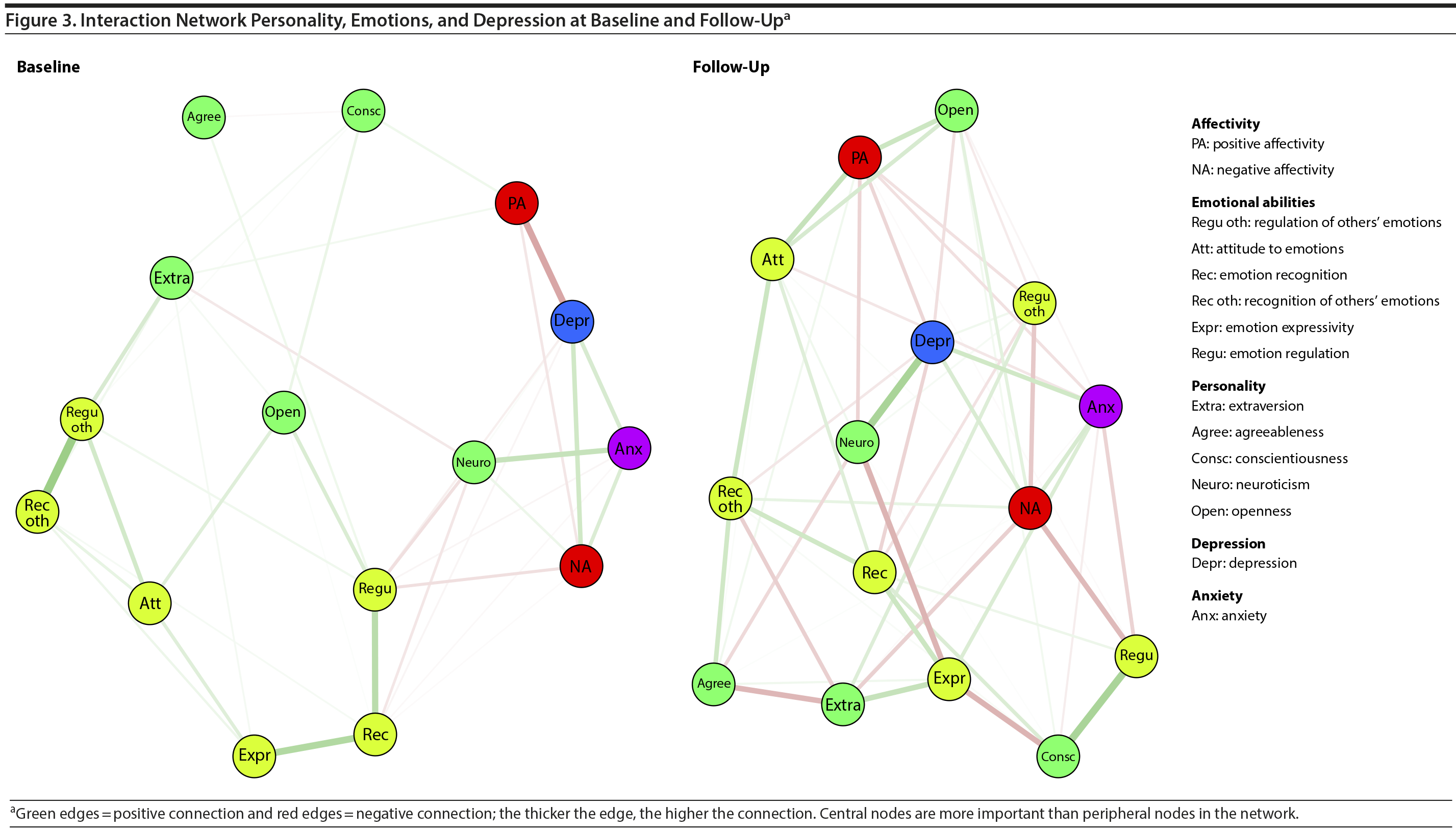
The network comparison test showed a significant difference in global strength between the networks at baseline and follow-up (P = .03). Follow-up network is significantly denser than baseline network. This means that depression, personality, and emotions are significantly more strongly associated to each other with decreasing symptomatology. Figure 3 (left side) shows that neuroticism has no direct connection to depression at baseline, but the connection runs through anxiety, while at follow-up (Figure 3, right side), neuroticism connects directly with depression. Depression at baseline is more peripheral of the network, while at follow-up, depression moves closer to the center of associations.
Centrality parameters show the node “emotion regulation” with the highest betweenness, closeness, and strength degree in the network at baseline. Therefore, emotion regulation is a highly important variable in the network of depression, personality, and emotions. Figure 3 (left) shows that emotion regulation connects not only to emotional abilities and personality (neuroticism and openness) but also through negative affectivity to depression itself.
At follow-up, the node “emotion expressivity” has the shortest distance to all other nodes (closeness) and interconnects other nodes the most (betweenness). The node depression shows the highest degree of strength in the network at follow-up (Figure 3, right). Thus, depression is the node that is most strongly connected to all other nodes in the follow-up, making it like a gravitational pull on all other variables.
DISCUSSION
The aim of this study was to explore the interactions between personality traits, emotions, and depression both in the network approach and in a linear way and to explore how the interactions, visible in the network approach, change depending on the severity of depressive symptoms in a 3-month follow-up. Our results show that the interactions of depressive symptoms with personality traits and emotions get stronger (network analysis and regression analysis) with decreasing symptoms.
The first question to address is what these results mean in the context of daily clinical practice. As previously stated, it emerged that patients with high depression scores during the inpatient stay showed personality traits and emotional abilities less connected to depression compared to 3 months later when depression symptoms had decreased. First, in methodological terms, the overlapping variance between depression and personality and emotions is smaller when depression is more severe compared to when it is less severe. In daily clinical practice, this is reflected by the dominance of depressive symptoms within a patient. Depression is the state that pushes personality traits and emotional abilities to the sideline. Predominant within the person is the feeling of sadness, loss of energy, or suicidal ideation instead of the awareness that he or she is or could be an outgoing person (extraversion) and sensitive to the feelings of others (recognition of others’ emotions). But, in methodological terms, since after remission depression moves to the center of the interaction network and shares more variance with personality and emotions and becomes “normal,” it is obviously a state and not something that “will not go away.” In practical terms, patients who felt depressed or who still have mild depressive symptoms become aware of their personality traits and their emotional abilities. As the depressive symptoms decline, depression is no longer predominant, and patients become aware that the current state could, for example, cause them to be somewhat sensitive or fearful.
The pathoplastic effect of psychopathology on personality could be an explanatory model for understanding these results. For patients with high depressive symptoms (eg, our sample at baseline), it is sometimes challenging to describe their usual or former personality because depression is predominant. Usually, highly neurotic personality traits then find expression in depression, which would support a dimensional view on the continuum between personality traits and mental illness.5,39
Another explanation for the results could be the causal effect of psychopathology on personality. Experiencing high depressive symptomatology at baseline could change personality and lead to higher experiencing of neuroticism at follow-up.39 A combination of the pathoplastic and the causal perspective could offer a viable explanation for the results: depressive symptoms could make it more difficult to ascertain personality traits of patients, and symptoms could also influence personality traits or emotions in the future.
Contrary to our results, many studies found significant interactions with Big Five3 and emotional abilities6 during clinical depression, which supports the idea that personality predicts and alters psychopathology.39 Our results, however, do not support such a view, which could be because we examined a broader picture of personality and emotions than other studies. While other studies focused on only the Big Five or emotional abilities, in this study, we expanded the borders of personality and emotions by also examining anxiety and emotional affectivity. In this study, interactions with depressive symptoms during clinical depression run more through anxiety and affectivity than through emotional abilities and the Big Five.
Limitations of the study have to be considered. First, while the follow-up interval of 3 months could be seen as too short an interval considering the length of depressive symptomatology, it is long enough to expect changes.40 Second, considering the study inclusion and exclusion criteria, we focused on depressive symptoms instead of diagnoses, referring to the network approach, and excluded patients with psychotic and manic symptoms. One might argue that this focus could reduce severity of depressive symptoms in the sample (by excluding manic and psychotic patients) and reduce homogeneity (by focusing on symptoms instead of diagnoses). However, this would only reduce the specificity of the depression nodes. Nevertheless, in our sample at the time of stronger symptoms, those symptoms aggregate themselves into a distinct cluster in the network.
There are some practical implications for clinical interventions to be drawn from the results: network analysis of depressive symptoms makes it apparent that depressive symptoms are not equally important within each patient. Therefore, after an initial screening, in clinical daily practice it makes sense to not add symptoms equally to sum scores41 but to look at a symptom level of depression. The clinician can pick 1 central symptom to target with a clinical intervention, knowing that this will affect most of the other depressive symptoms connected to the targeted symptom. Therefore, individual networks of patients should be constructed during clinical practice to envision an individual depressive symptom network and steer clinical intervention. Further, practical implications can be drawn from the interaction network analyses. Network analysis of the interactions of depression with personality and emotions shows that during inpatient stay, depression arranges itself peripherally on the interaction network. This finding suggests that the higher the degree of depression, the more walled off and impenetrable the illness, however trivial this insight might be. For interventions, this could mean that one should directly and immediately zero in on symptoms during the inpatient stay and that a focus during severe depression on, for example, emotional abilities will not affect depression directly because the patient does not have full access to his or her personality or emotions—feeling depressed is predominant. However, our results suggest that especially in outpatient treatment, which usually coincides with a decrease in symptoms, it is sensible to focus on problematic personality traits and low emotional abilities because intervention in these areas will also affect symptomatology.
Our results show that network analysis is a helpful tool to view complex associations during a mental illness. Personality, emotions, and depression interact differently with each other depending on the severity of symptoms. Network analysis brought additional clarity above and beyond regression analysis regarding the complexity of associations. Future studies should use network analysis to understand complex associations between other mental illnesses (eg, between bipolar disorders and personality traits and emotions). Network analysis aligns with the complex reality of interactions and brings new insights into associations of mental illnesses with adjacent areas of human experiences such as personality or emotions.
Submitted: September 2, 2016; accepted December 23, 2016.
Published online: April 13, 2017.
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1. Goldberg LR. An alternative “description of personality”: the big-five factor structure. J Pers Soc Psychol. 1990;59(6):1216–1229. PubMed doi:10.1037/0022-3514.59.6.1216
2. Kotov R, Gamez W, Schmidt F, et al. Linking “big” personality traits to anxiety, depressive, and substance use disorders: a meta-analysis. Psychol Bull. 2010;136(5):768–821. PubMed doi:10.1037/a0020327
3. Hakulinen C, Elovainio M, Pulkki-Råback L, et al. Personality and depressive symptoms: individual participant meta-analysis of 10 cohort studies. Depress Anxiety. 2015;32(7):461–470. PubMed doi:10.1002/da.22376
4. Boyce P, Parker G, Barnett B, et al. Personality as a vulnerability factor to depression. Br J Psychiatry. 1991;159(1):106–114. PubMed doi:10.1192/bjp.159.1.106
5. Andersen AM, Bienvenu OJ. Personality and psychopathology. Int Rev Psychiatry. 2011;23(3):234–247. PubMed doi:10.3109/09540261.2011.588692
6. Kneeland ET, Dovidio JF, Joormann J, et al. Emotion malleability beliefs, emotion regulation, and psychopathology: integrating affective and clinical science. Clin Psychol Rev. 2016;45:81–88. PubMed doi:10.1016/j.cpr.2016.03.008
7. Aldinger M, Stopsack M, Barnow S, et al. The association between depressive symptoms and emotion recognition is moderated by emotion regulation. Psychiatry Res. 2013;205(1–2):59–66. PubMed doi:10.1016/j.psychres.2012.08.032
8. Berking M, Wirtz CM, Svaldi J, et al. Emotion regulation predicts symptoms of depression over five years. Behav Res Ther. 2014;57:13–20. PubMed doi:10.1016/j.brat.2014.03.003
9. Ehring T, Fischer S, Schnülle J, et al. Characteristics of emotion regulation in recovered depressed versus never depressed individuals. Pers Individ Dif. 2008;44(7):1574–1584. doi:10.1016/j.paid.2008.01.013
10. Karreman A, van Assen MA, Bekker MH. Intensity of positive and negative emotions: explaining the association between personality and depressive symptoms. Pers Individ Dif. 2013;54(2):214–220. doi:10.1016/j.paid.2012.08.040
11. Paulus DJ, Vanwoerden S, Norton PJ, et al. Emotion dysregulation, psychological inflexibility, and shame as explanatory factors between neuroticism and depression. J Affect Disord. 2016;190:376–385. PubMed doi:10.1016/j.jad.2015.10.014
12. Borsboom D, Cramer AO. Network analysis: an integrative approach to the structure of psychopathology. Annu Rev Clin Psychol. 2013;9:91–121. PubMed doi:10.1146/annurev-clinpsy-050212-185608
13. Schönbrodt FD, Perugini M. At what sample size do correlations stabilize? J Res Pers. 2013;47(5):609–612. doi:10.1016/j.jrp.2013.05.009
14. American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
15. Buuren S, Groothuis-Oudshoorn K. Mice: multivariate imputation by chained equations in R. J Stat Softw. 2011;45(3). doi:10.18637/jss.v045.i03
16. Newman DA. Missing data techniques and low response rates: the role of systematic nonresponse. In: Lance CE, Vandenberg RJ, eds. Statistical and Methodological Myths and Urban Legends: Doctrine, Verity and Fable in the Organizational and Social Sciences. New York, NY: Routledge/Taylor & Francis Group;2009:7–36.
17. Hautzinger M, Keller F, Kühner C. BDI-II. Beck-Depressions-Inventar. Revision. Franfurt am Main, Germany: Harcourt Test Services; 2006.
18. Beck AT, Steer RA, Brown GK. Beck Depression Inventory-II. San Antonio, TX: Pearson; 1996.
19. Kühner C, Bürger C, Keller F, et al. Reliability and validity of the Revised Beck Depression Inventory (BDI-II): results from German samples [in German]. Nervenarzt. 2007;78(6):651–656. PubMed doi:10.1007/s00115-006-2098-7
20. Laux L, Hock M, Bergner-Köthner R, et al. State-Trait-Angst-Depressionsinventar, Manual. Göttinge, Germany: Hogrefe; 2013.
21. Rammstedt B, John OP. Kurzversion des Big Five Inventory (BFI-K). Diagnostica. 2005;51(4):195–206. doi:10.1026/0012-1924.51.4.195
22. John OP, Donahue EM, Kentle RL. The Big Five Inventory—Versions 4a and 54. Berkeley, CA: University of California, Berkeley, Institute of Personality and Social Research; 1991.
23. Kovaleva A, Beierlein C, Kemper C, et al. Psychometric properties of the BFI-K: a cross-validation study. Int J Educ Psychol Assess. 2013;13(1):34–50.
24. Watson D, Clark LA, Tellegen A. Development and validation of brief measures of positive and negative affect: the PANAS scales. J Pers Soc Psychol. 1988;54(6):1063–1070. PubMed doi:10.1037/0022-3514.54.6.1063
25. Crawford JR, Henry JD. The Positive and Negative Affect Schedule (PANAS): construct validity, measurement properties and normative data in a large non-clinical sample. Br J Clin Psychol. 2004;43(pt 3):245–265. PubMed doi:10.1348/0144665031752934
26. Krohne HW, Egloff B, Kohlmann C-W, et al. Untersuchungen mit einer deutschen Version der” Positive and Negative Affect Schedule” (PANAS). Diagnostica. 1996;42(2):139–156.
27. Rindermann H. Emotionale-Kompetenz-Fragebogen (EKF). Manual. Göttingen, Germany: Hogrefe; 2009.
28. R: a language and environment for statistical computing [computer program]. Vienna, Austria: R Foundation for Statistical Computing; 2015.
29. Revelle W. Psych: Procedures for Psychological, Psychometric, and Personality Research. Evanston, IL: Northwestern University; 2014:165.
30. Epskamp S, Cramer AO, Waldorp LJ, et al. Qgraph: network visualizations of relationships in psychometric data. J Stat Softw. 2012;48(4):1–18. doi:10.18637/jss.v048.i04
31. Epskamp S, Fried EI. Bootnet: bootstrap methods for various network estimation routines [computer program]. Vienna, Austria: R Foundation for Statistical Computing; 2015.
32. Network Analysis in R Cookbook. http://sachaepskamp.com/files/Cookbook.html. Accessed March 21, 2017.
33. Shaffer JP. Multiple hypothesis testing. Annu Rev Psychol. 1995;46:561. doi:10.1146/annurev.ps.46.020195.003021
34. Costantini G, Epskamp S, Borsboom D, et al. State of the aRt personality research: a tutorial on network analysis of personality data in R. J Res Pers. 2015;54:13–29. doi:10.1016/j.jrp.2014.07.003
35. Fruchterman TM, Reingold EM. Graph drawing by force-directed placement. Softw Pract Exper. 1991;21(11):1129–1164. doi:10.1002/spe.4380211102
36. Newman M. Networks: an Introduction. Oxford, UK: Oxford University Press; 2010. doi:10.1093/acprof:oso/9780199206650.001.0001
37. Van Borkulo C. Network comparison test: permutation-based test of differences in strength of networks [computer program]. Vienna, Austria: R Foundation for Statistical Computing; 2015.
38. Cohen J. The Effect Size Index: d. Statistical Power Analysis for the Behavioral Sciences. 2nd ed. Mahwah, NJ: Lawrence Erlbaum Associates; 1988:20–26.
39. A Widiger T. Personality and psychopathology. World Psychiatry. 2011;10(2):103–106. PubMed doi:10.1002/j.2051-5545.2011.tb00024.x
40. Simon GE, VonKorff M. Recognition, management, and outcomes of depression in primary care. Arch Fam Med. 1995;4(2):99–105. PubMed doi:10.1001/archfami.4.2.99
41. Fried EI, Nesse RM. Depression sum-scores don’t add up: why analyzing specific depression symptoms is essential. BMC Med. 2015;13(1):72. PubMed doi:10.1186/s12916-015-0325-4
Please sign in or purchase this PDF for $40.00.

