Responses to the Medical Review of Systems: Borderline Versus Nonborderline Patients in an Internal Medicine Outpatient Clinic
Objective: In both clinical and empirical reports, individuals with borderline personality disorder have been characterized by tendencies toward somatization. In this study, we examined the relationship between somatic symptoms, in the context of a traditional medical review of systems, and borderline personality disorder, using 2 self-report measures for this Axis II dysfunction.
Method: In a cross-sectional consecutive sample of 381 internal medicine outpatients being seen predominantly by resident providers in a midsized, midwestern city in October 2010, we assessed 35 physical symptoms, which constitute 1 version of a medical review of systems, and borderline personality disorder using the Borderline Personality Disorder Scale of the Personality Diagnostic Questionnaire-4 (PDQ-4) and the Self-Harm Inventory (SHI).
Results: The total number of symptoms endorsed on the medical review of systems was positively correlated with scores on the PDQ-4 (r = 0.42, P < .001, n = 369) and scores on the SHI (r = 0.36, P < .001, n = 366). In addition, the percentages of participants with borderline personality disorder increased as the number of endorsed symptoms increased. No individual symptom, or symptom pattern, was particularly related to participants with borderline personality disorder features.
Conclusions: In an internal medicine outpatient sample from a resident provider clinic, patients with borderline personality disorder characteristics endorsed significantly more physical symptoms on a medical review of systems than those without such characteristics, suggesting a somatic overlay in individuals with this Axis II disorder. No specific physical symptom pattern or cluster was evident among those with these Axis II features.
Prim Care Companion CNS Disord 2011;13(3):e1-e5
© Copyright 2011 Physicians Postgraduate Press, Inc.
Submitted: November 29, 2010; accepted February 3, 2011.
Published online: June 9, 2011 (doi:10.4088/PCC.10m01120).
Corresponding author: Randy A. Sansone, MD, Sycamore Primary Care Center, 2115 Leiter Rd, Miamisburg, Ohio, 45342 ([email protected]).
Over the years, clinicians have intermittently reported somatization in some patients with borderline personality disorder. For example, as far back as 1980, Schreter1 described a relationship between chronic somatic symptoms and borderline personality disorder among patients in group psychotherapy. In the early 1990s, Giovacchini2,3 described associations between psychosomatic symptoms and borderline personality disorder. Bernstein4 indicated that somatic symptoms could potentially mask underlying borderline personality disorder. Spitzer and Barnow5 reported a relationship between somatoform disorders and borderline personality disorder. Hull and colleagues6 described a patient with borderline personality disorder whose acting-out behaviors were synchronized with exacerbations of physical illness. Finally, Janssen7 described 2 patients with borderline personality disorder who initially presented with somatic symptoms.
Clinical Points
- According to the findings of this study, patient endorsement of multiple symptoms on the review of systems suggests the possible presence of borderline personality symptomatology.
- In this study, there was no pattern of symptom endorsement on the medical review of systems by patients with borderline personality symptomatology (ie, no specific symptoms suggest this Axis II pathology).
In addition to clinical reports, empirical research supports a relationship between somatic symptoms and borderline personality disorder. For example, Lloyd and colleagues8 found increased reporting of somatic complaints among patients with borderline personality disorder. Snyder and Pitts9 reported that patients with borderline personality disorder had elevated psychological scores on scales of somatization, hypochondriasis, and hysteria compared with controls. Ross and colleagues10 examined a sample of patients with dissociative identity disorder, many of whom had comorbid borderline personality disorder, and reported 15 somatic symptoms per participant. In addition, researchers have found associations between a formal diagnosis of DSM-defined somatization disorder and borderline personality disorder.11,12 For example, in a sample of patients with borderline personality disorder, Hudziak and colleagues12 found that 36% had comorbid somatization disorder.
In 2 different internal medicine samples, we reported correlations between somatic preoccupation and borderline personality symptomatology.13,14 In addition, in a study among family medicine outpatients, using path analysis, we again found evidence for a relationship between somatic preoccupation and borderline personality disorder.15
When assessing somatization in patients with borderline personality disorder, past researchers have used a variety of measures, including formal psychological scales, somatic symptom counts, DSM criteria for somatization disorder, and other somatization measures. For example, in all 3 of our previous studies,13-15 we used the Bradford Somatic Inventory.16 However, no study to date has examined patient response patterns to a medical review of systems, which is oftentimes an early endeavor in the patient/clinician relationship. If an association exists between borderline personality disorder and an overendorsement of symptoms on the medical review of systems, this might be an early and potentially important indicator of this complex disorder. In an effort to broaden the understanding of the relationship between somatization and borderline personality disorder, we investigated whether patients with this Axis II disorder overendorse the physical symptoms commonly encountered in the traditional medical review of systems.
METHOD
Participants
At the outset of this cross-sectional study, 471 individuals were consecutively approached and 417 agreed to participate, for a participation rate of 88.5%. Of these subjects, 381 completed the relevant study measures. Participants were men and women, aged 18 years or older, who were being seen in an outpatient internal medicine clinic for nonemergent medical care in October 2010. The outpatient clinic is staffed by both faculty and residents in the Department of Internal Medicine and is located in a midsized, midwestern city. The majority of participants in this study were patients being seen by resident providers. We excluded individuals with compromising medical (eg, pain), cognitive (eg, dementia), intellectual (eg, mental retardation), or psychiatric symptoms (eg, psychotic) that would preclude the candidate’s ability to successfully complete a survey.
Respondents consisted of 132 men and 249 women, who ranged in age from 19 to 97 years (mean = 50.32, SD = 15.45). Age was normally distributed around the mean: 10.4% were aged 19-29, 17.3% were aged 30-39, 19.6% were aged 40-49, 23.6% were aged 50-59, 17.3% were aged 60-69, and 11.9% were aged 70-97. Most respondents were white (88.2%), followed by black (7.9%), other (2.1%), Hispanic (1.0%), and Asian (0.8%). With regard to highest level of educational attainment, all but 6.6% of respondents reported having at least attained a high school diploma, with 14.3% of the sample attaining a bachelor’s degree and 13.3% earning a graduate or professional degree.
Procedure
During clinic hours, one of the authors (C.L.) positioned herself in the lobby of the outpatient internal medicine clinic, approached incoming patients, and informally assessed exclusion criteria. With potential candidates, the recruiter then reviewed the focus of the project and invited each to participate. Each participant was asked to complete a 5-page survey, which took about 10 minutes. Participants were directed to place completed surveys into sealed envelopes and then to place these into a collection box in the lobby.
The survey consisted of 3 basic sections. The first section was a demographic query, in which we asked participants about their sex, age, marital status, racial/ethnic origin, and educational achievement.
In the second section of the survey, we queried participants about 35 general physical symptoms from 14 different body areas/systems, which constitute one clinical version of a medical review of systems. These items were adapted from a preappointment questionnaire developed by Sinsky.17 Items were preceded by the statement, “Have you experienced any of the following symptoms in the past week?” with yes/no response options.
The third section of the survey contained 2 measures for borderline personality disorder. The first measure, the Borderline Personality Disorder Scale of the Personality Diagnostic Questionnaire-4 (PDQ-4),18 is a 9-item, true/false, self-report measure that consists of the diagnostic criteria for borderline personality disorder that are listed in the DSM-IV.19 A score of 5 or higher is highly suggestive of borderline personality disorder. Previous versions of the PDQ have been found to be useful screening tools for borderline personality disorder in both clinical20,21 and nonclinical samples,22 including the use of the freestanding Borderline Personality Disorder Scale.23
The second borderline personality disorder measure was the Self-Harm Inventory,24 a 22-item, yes/no, self-report measure that explores participants’ histories of self-harm behavior. Each item in the inventory is preceded by the statement, “Have you ever intentionally, or on purpose, ‘ ¦ .” Individual items include “overdosed, cut yourself on purpose, burned yourself on purpose, and hit yourself.” Each endorsement increases the possibility of pathology, with the SHI total score being the summation of “yes” responses. SHI total scores of 5 or higher are highly suggestive of the diagnosis of borderline personality disorder.24 Indeed, in comparison with the Diagnostic Interview for Borderlines,25 a benchmark measure for the diagnosis of borderline personality disorder in research settings, the SHI demonstrated an 84% accuracy in diagnosis.24
RESULTS
Each of the individual symptoms in the medical review of systems was endorsed by at least 5 respondents, and the total number of symptoms endorsed per participant ranged from 0 to 32 (mean = 0.56, SD = 1.62). Only 38 participants (10.0%) did not endorse any of the listed symptoms, and only 24 participants (6.3%) endorsed more than half of the 35 listed symptoms. The total number of symptoms endorsed was positively correlated with scores on the PDQ-4 (r = 0.42, P < .001, n = 369) and scores on the SHI (r = 0.36, P < .001, n = 366). We also created a combination variable by converting each respondent’s PDQ-4 score and SHI score to a respective Z score, and then summed the 2 Z scores to create a combination assessment of borderline personality disorder. The total number of symptoms endorsed was positively correlated with scores on this combination measure of borderline personality disorder (r = 0.43, P < .001, n = 362) as well.
Age was negatively and weakly correlated with the total number of symptoms endorsed (r = 0.12, P < .05, n = 377) and negatively and more strongly correlated with scores on the PDQ-4 (r = 0.43, P < .001, n = 362), the SHI (r = -0.37, P < .001, n = 375), and the combined measure of borderline personality disorder (r = -0.39, P < .001, n = 359). In other words, older respondents tended to report fewer physical symptoms and fewer indications of borderline personality disorder. Accordingly, we performed the analyses reported above, controlling for age. Even after excluding age, the total number of symptoms endorsed was positively correlated with scores on the PDQ-4 (r = 0.41, P < .001, n = 363), scores on the SHI (r = 0.34, P < .001, n = 363), and scores on the combined measure of borderline personality disorder (r = 0.42, P < .001, n = 356). Note that the magnitude of the correlation coefficients remained virtually unchanged.
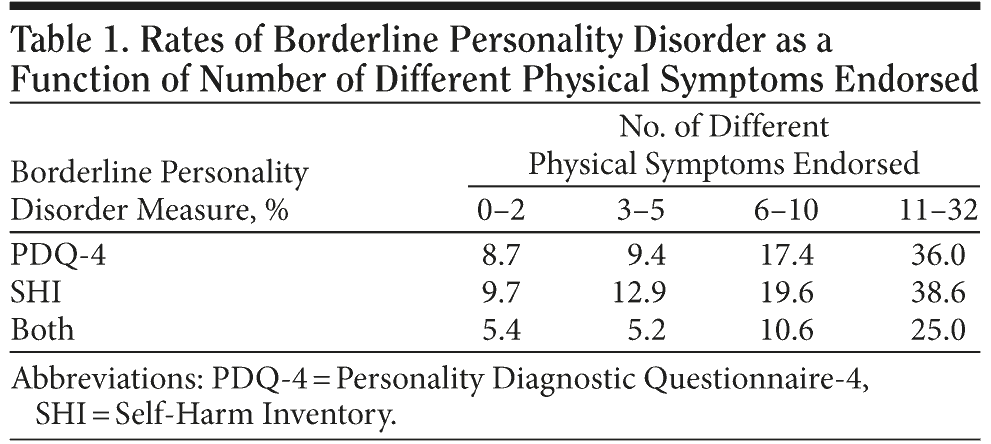
With regard to exceeding the clinical cutoff score indicative of borderline personality disorder, 65 of the 369 participants (17.6%) who completed the PDQ-4 did so, compared to 73 of the 366 (19.9%) who completed the SHI. Of the 362 respondents who completed both the PDQ-4 and the SHI, 42 (11.6%) exceeded the clinical cutoff score on both measures. The relative rates of borderline personality disorder as a function of the number of symptoms endorsed on the medical review of systems checklist are presented in Table 1. Each of the 4 levels of symptom endorsement was determined by quartiles based upon the distribution of symptom endorsement for the sample. In other words, the numbers of respondents in each of the 4 categories of symptom endorsement are approximately equal.
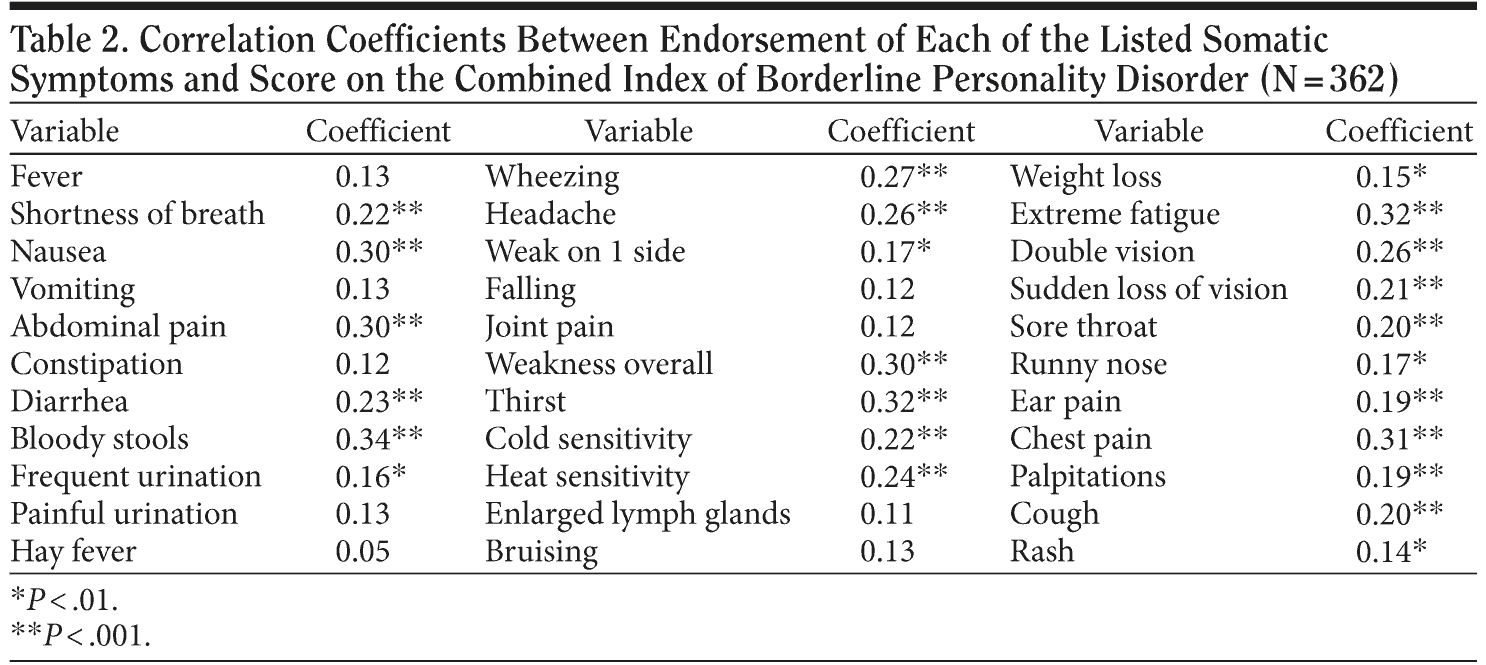
With regard to individual symptoms, 2 (bloody urine and mole change) were endorsed by fewer than 12 respondents and did not allow for comparison between those with and without these particular symptoms. The relationship between endorsement of each of the remaining symptoms and the combination score for borderline personality disorder is presented in Table 2. Note that scores on the combined measure of borderline personality disorder were positively correlated with endorsement of the majority of the individual symptoms.
DISCUSSION
Our findings underscore 2 important conclusions. First, among outpatients in a resident provider internal medicine clinic, an increasing number of endorsements on a medical review of systems evidenced statistically significant correlations with 2 measures of borderline personality disorder, individually and for participants who were positive on both measures, strongly suggesting that somatization is associated with borderline personality disorder in this cohort. Note that the borderline personality disorder measures used in this study both have very different constructs, so individuals scoring positively on both measures are, in our opinion, more likely to harbor higher levels of borderline personality disorder symptomatology. Second, in this population, there was no coherent symptom “profile” or group of symptoms, in particular, that suggested borderline personality disorder—symptom endorsements were diffuse and nonspecific.
Note that the prevalence of borderline personality disorder in this population appears somewhat high. There may be several explanations for this. First, self-report measures for Axis II disorders tend to be overinclusive, so the borderline personality disorder measures used in this study may be reflecting at times borderline personality disorder symptomatology rather than the bona fide disorder. Second, this is a resident provider clinic and tends to attract uninsured patients (ie, perhaps this partially reflects lower functioning individuals and greater levels of personality pathology). Third, there may be other unaccounted influences that may be artificially inflating borderline personality disorder scores, such as anxiety, depression, pain, medication-seeking (ie, feigning “bad”), illness burden, and substance abuse. Fourth, while the community rate of borderline personality disorder is designated at 2% in the DSM-V-TR,26 according to Grant and colleagues,27 the rate is actually much higher at 6%. In addition, in a private practice internal medicine setting, Gross and colleagues28 reported a prevalence rate of 7%. Therefore, the 11.6% rate determined in this study by the combined measures appears less inflated.
What might explain the association between somatization and borderline personality disorder? First, it may be that multiple somatic symptoms function to promote a victim role in adulthood (ie, a medical victim). The victim dynamics of borderline personality disorder have been well described by Kroll,29 who stated that victimization is a “basic theme in understanding borderlines.”(p46) Kroll described the way in which individuals with borderline personality disorder engage others to “act upon [them], usually in a negative, rejecting, or aggressive way, but sometimes in a caretaking ‘ ¦ way.”29(p46) Kroll further emphasized the importance to such patients in portraying helplessness and incompetence.29
A second possibility may be that multiple physical symptoms are mediated by trauma-related dynamics. Childhood histories of trauma are frequently encountered in patients with borderline personality disorder, and the resulting posttraumatic stress spectrum of symptoms might result in hypervigilance. While hypervigilance is traditionally viewed as an external process, it might also manifest on an internal level, with excessive scrutiny and attention to various bodily sensations and functions.
Third, it could be that early developmental trauma results in impaired immunity, thus resulting in diffuse and numerous somatic symptoms in these types of patients. There may be other explanations as well, and the preceding possibilities are not necessarily mutually exclusive.
This study has a number of potential limitations, the most important being the self-report nature of the data. In addition, we do not know whether any of the individuals with borderline personality disorder symptomatology in this study have been formally diagnosed with the disorder or in mental health treatment. However, the sample was consecutive in nature and reasonable in size, the study query is unique to the literature (ie, a medical review of systems), and the findings echo the current literature from a different perspective. It appears that in primary care settings, patients with borderline personality disorder may demonstrate an extensive medical review of systems; this may be an important and initial nonspecific clinical marker for this type of pathology in such settings.
Author affiliations: Departments of Psychiatry and Internal Medicine, Wright State University School of Medicine, Dayton, Ohio (Dr Sansone); Kettering Medical Center, Kettering, Ohio (Drs Sansone and Lam); and Department of Human Relations, Columbia College, South Carolina (Dr Wiederman).
Potential conflicts of interest: None reported.
Funding/support: None reported.
REFERENCES
1. Schreter RK. Treating the untreatables: a group experience with somaticizing borderline patients. Int J Psychiatry Med. 1980;10(3):205-215. PubMed doi:10.2190/DRYP-4URY-BVBP-V3CY
2. Giovacchini PL. The regressed patient and the psychosomatic focus. In: Boyer LB, Giovacchini PL, eds. Master Clinicians on Treating the Regressed Patient. Vol 2. Northvale, NJ: Aronson; 1993:85-106.
3. Giovacchini PL. Treatment issues with borderline patients and the psychosomatic focus. Am J Psychother. 1993;47(2):228-244. PubMed
4. Bernstein AE. The mind body interface revisited. Psychother Patient. 1988;4(2):45-56. doi:10.1300/J358v04n02_05
5. Spitzer C, Barnow S. Somatization as a unique dimension in personality disorders. Personlichkeitsstorungen Theorie und Therapie. 2005;9:106-115.
6. Hull JW, Okie J, Gibbons B, et al. Acting up and physical illness: temporal patterns and emerging structure. J Am Psychoanal Assoc. 1992;40(4):1161-1183. PubMed
7. Janssen PL. Scenarios of borderline disturbances. Prax Psychother Psychosom. 1990;35:1-12.
8. Lloyd C, Overall JE, Kimsey LR, et al. A comparison of the MMPI-168 profiles of borderline and nonborderline outpatients. J Nerv Ment Dis. 1983;171(4):207-215. PubMed doi:10.1097/00005053-198304000-00002
9. Snyder S, Pitts WM. Characterizing somatization, hypochondriasis, and hysteria in the borderline personality disorder. Acta Psychiatr Scand. 1986;73(3):307-314. PubMed doi:10.1111/j.1600-0447.1986.tb02689.x
10. Ross CA, Miller SD, Reagor P, et al. Structured interview data on 102 cases of multiple personality disorder from four centers. Am J Psychiatry. 1990;147(5):596-601. PubMed
11. Prasad RB, Val ER, Lahmeyer HW, et al. Associated diagnoses (comorbidity) in patients with borderline personality disorder. Psychiatr J Univ Ott. 1990;15(1):22-27. PubMed
12. Hudziak JJ, Boffeli TJ, Kreisman JJ, et al. Clinical study of the relation of borderline personality disorder to Briquet’s syndrome (hysteria), somatization disorder, antisocial personality disorder, and substance abuse disorders. Am J Psychiatry. 1996;153(12):1598-1606. PubMed
13. Sansone RA, Wiederman MW, Sansone LA. Medically self-harming behavior and its relationship to borderline personality symptoms and somatic preoccupation among internal medicine patients. J Nerv Ment Dis. 2000;188(1):45-47. PubMed doi:10.1097/00005053-200001000-00008
14. Sansone RA, Tahir NA, Buckner VR, et al. The relationship between borderline personality symptomatology and somatic preoccupation among internal medicine outpatients. Prim Care Companion J Clin Psychiatry. 2008;10(4):286-290. PubMed doi:10.4088/PCC.v10n0403
15. Sansone RA, Wiederman MW, Sansone LA. Adult somatic preoccupation and its relationship to childhood trauma. Violence Vict. 2001;16(1):39-47. PubMed
16. Mumford DB, Bavington JT, Bhatnagar KS, et al. The Bradford Somatic Inventory: a multi-ethnic inventory of somatic symptoms reported by anxious and depressed patients in Britain and the Indo-Pakistan subcontinent. Br J Psychiatry. 1991;158(3):379-386. PubMed doi:10.1192/bjp.158.3.379
17. Sinsky CA. Improving office practice: working smarter, not harder. Fam Pract Manag. 2006;13(10):28-34. PubMed
18. Hyler SE. Personality Diagnostic Questionniare-4. New York, NY: New York State Psychiatric Institute; 1994.
19. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition. Washington, DC: American Psychiatric Association; 1994.
20. Dubro AF, Wetzler S, Kahn MW. A comparison of three self-report questionnaires for the diagnosis of DSM-III personality disorders. J Pers Disord. 1988;2:256-266.
21. Hyler SE, Lyons M, Rieder RO, et al. The factor structure of self-report DSM-III Axis II symptoms and their relationship to clinicians’ ratings. Am J Psychiatry. 1990;147(6):751-757. PubMed
22. Johnson JG, Bornstein RF. Utility of the Personality Diagnostic Questionnaire-Revised in a nonclinical population. J Pers Disord. 1992;6:450-457.
23. Patrick J, Links P, Van Reekum R, et al. Using the PDQ-R BPD scale as a brief screening measure in the differential diagnosis of personality disorder. J Pers Disord. 1995;9:266-274.
24. Sansone RA, Wiederman MW, Sansone LA. The Self-Harm Inventory (SHI): development of a scale for identifying self-destructive behaviors and borderline personality disorder. J Clin Psychol. 1998;54(7):973-983. PubMed doi:10.1002/(SICI)1097-4679(199811)54:7<973::AID-JCLP11>3.0.CO;2-H
25. Kolb JE, Gunderson JG. Diagnosing borderline patients with a semistructured interview. Arch Gen Psychiatry. 1980;37(1):37-41. PubMed
26. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
27. Grant BF, Chou SP, Goldstein RB, et al. Prevalence, correlates, disability, and comorbidity of DSM-IV borderline personality disorder: results from the Wave 2 National Epidemiologic Survey on Alcohol and Related Conditions. J Clin Psychiatry. 2008;69(4):533-545. PubMed doi:10.4088/JCP.v69n0404
28. Gross R, Olfson M, Gameroff M, et al. Borderline personality disorder in primary care. Arch Intern Med. 2002;162(1):53-60. PubMed doi:10.1001/archinte.162.1.53
29. Kroll J. The Challenge of the Borderline Patient: Competency in Diagnosis and Treatment. New York, NY: WW Norton & Co; 1988.