Combined Deficiencies of Vitamins B1 and C in Well-Nourished Patients

ABSTRACT
Vitamin deficiencies such as scurvy and Wernicke’s encephalopathy are poorly recognized in Western populations. Inadequate intake of these micronutrients and low levels when measured are more frequent than expected. Cases of combined vitamin deficiencies such as that of ascorbic acid and thiamine are seldom reported. Two patients with clinical and biochemical evidence of vitamin deficiencies are described. Signs and symptoms rapidly responded to vitamin replacement. Neither patient was overtly malnourished, but nutritional histories and physical examination were strongly suggestive. Vitamin replacement may require large intravenous doses but is inexpensive and potentially of great benefit.
Prim Care Companion CNS Disord 2014;16(4):doi:10.4088/PCC.14br01649
© Copyright 2014 Physicians Postgraduate Press, Inc.
Submitted: March 4, 2014; accepted March 21, 2014.
Published online: July 3, 2014.
Corresponding author: Thomas M. Brown, MD, Department of Psychiatry, Mailstop 116A, Audie Murphy Veterans Affairs Medical Center, 7400 Merton Minter Blvd, San Antonio, TX 78229 ([email protected])
Vitamin deficiencies may occur frequently in the Western world, yet go unrecognized. We present 2 cases in which deficiencies of both vitamin B1 and C were identified and comment on the clinical settings, diagnosis, and treatment.
CASE REPORTS
Case 1
Mr A, a 56-year-old Hispanic man with a history of hepatitis C, nicotine dependence, cocaine abuse, and alcohol abuse, presented to the emergency room with progressive lower extremity edema, increasing abdominal girth, orthopnea, and dyspnea on exertion. He reported gingival bleeding when brushing his teeth for the past 2 years and intermittent, spontaneous epistaxis of several months’ duration. He drank 24 12-ounce cans of beer daily and had ingested no solid food for 2 to 3 months. He smoked a pack of cigarettes daily for more than 20 years. He was 5 ft 11 in tall and weighed 279 lb (127 kg), with a body mass index (BMI) of 40 kg/m2. Mr A was in mild respiratory distress. No icterus, nystagmus, or fundal changes were seen. Soft palate petechiae were noted, as well as gingival hypertrophy, which bled with minimal contact. He had jugular venous distention, bibasilar rales, a third heart sound, and pitting edema to the knees. Asterixis was noted. Mr A was alert and oriented in all spheres and had intact short-term memory, no abnormal cerebellar findings, no ophthalmoplegia, and no localizing neurologic findings. A chest film showed mild central pulmonary edema. A complete blood count was normal, including platelets of 100,000/mm3, and the international normalized ratio was 1.4. His serum vitamin C level was 0.0 mg/dL (normal range, 0.4-2.0 mg/dL), zinc was low at 64 µg/dL (normal range, 70-150 µg/dL), vitamin B1 was low at 68 nmol/L (normal range, 87-280 nmol/L), and magnesium was normal. Wet beriberi and scurvy were diagnosed.
Furosemide, spironolactone, intravenous thiamine and ascorbic acid, and oral multivitamins were given daily. Over 7 days, Mr A’s weight fell to 233 lb (106 kg), with resolution of edema. Within 4 days, his active gingival bleeding had stopped, even with brushing. Mr A was discharged much improved 2 days later.
Case 2
Mr B, a 63-year-old white man, was admitted to the hospital after a suicide attempt by tramadol ingestion. He had a history of schizoaffective disorder, type II diabetes, chronic kidney disease (baseline creatinine of 3.0 mg/dL), vitamin B12 deficiency, anemia, hypothyroidism, and hypertension. He typically ate "fast food" and avoided fruits and vegetables. He did not smoke tobacco, drink alcohol, or use illicit agents. He was 5 ft 9 in tall and weighed 220 lb (100 kg), with a BMI of 33 kg/m2. On examination, Mr B displayed profound lassitude. He rested supine, speaking slowly and without purposeful movement. He had bibasilar crackles, 1+ pitting edema bilaterally of his lower extremities, bilateral nystagmus on extreme horizontal gaze, and upper extremity dystaxia. Short-term memory was impaired. He had no other localizing neurologic findings. He lacked easy bruising, gingival or periungual bleeding, or corkscrew hairs. His serum vitamin C level was 0.1 mg/dL and his zinc level was low at 64 µg/dL, while his vitamin B1 and magnesium levels were normal. Early, or latent, scurvy as well as Wernicke’s encephalopathy were diagnosed.
Mr B was started on intravenous vitamins, and, otherwise, his home medications were continued without change. After receiving 800 mg of thiamine and 400 mg of ascorbic acid over 2 days, Mr B sat up in bed and stated that he felt vastly improved. His mood was much better, his short-term memory was restored, and his cerebellar findings were resolved.
DISCUSSION
The striking reduction in the prevalence of severe protein-calorie malnutrition in the developed world may diminish the ability of Western medical providers to recognize micronutrient deficiencies. Other barriers to the recognition of deficiencies include the general unfamiliarity with their clinical presentations, the assumption that deficiencies must present with classical presentations, and, finally, the misperception that frank starvation and other overt nutritional calamities are required for their development.1 Vitamin deficiencies were suspected in our patients not because they were emaciated but because their medical histories and physical examinations were suggestive.
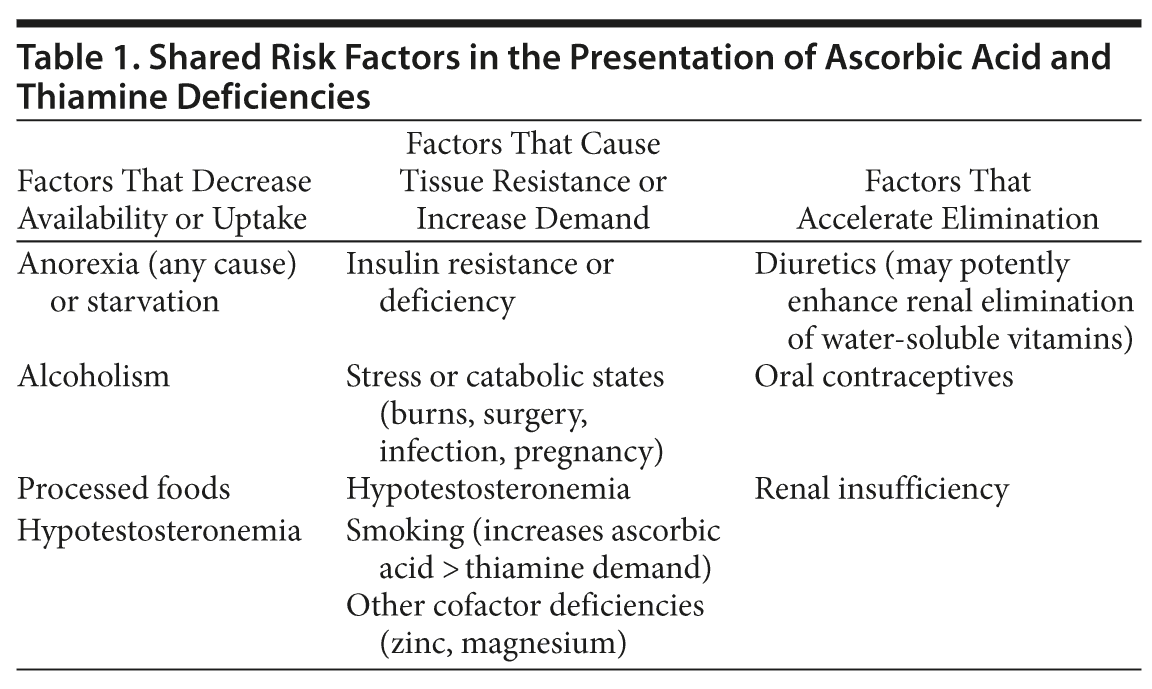
We emphasize that classical presentations in developed countries are no longer the norm. The gingival bleeding seen in our first patient, for instance, may be found in only 30% of patients with scurvy.2 In Wernicke’s encephalopathy, the triad of confusion with impaired short-term memory, cerebellar findings, and ophthalmoplegia is found in a distinct minority (10%-30%) of cases. Caine and colleagues3 recommend a diagnosis of Wernicke’s encephalopathy when 2 of the following 4 findings are present: dietary deficiencies, oculomotor abnormalities, some evidence of cerebellar dysfunction, and either acute confusion or impaired short-term memory. In the right clinical context, any one of these findings should trigger serum assays and possibly empiric therapy.4 Table 1 outlines risk factors for deficiencies of vitamins B1 and C.5-9
If 1 vitamin deficiency is recognized in patients with the above risk factors, other major essential micronutrients should be assayed and, if deficiency is suspected, replaced empirically while awaiting results. The traditional "banana bag," with its small doses of multiple vitamins, may serve as a platform for the delivery of adequate doses of deficient vitamins, although included amounts are commonly suboptimal. Typical thiamine replacement regimens should include administration of a total of 500 to 1,000 mg of thiamine intravenously daily in divided doses.10 Oral thiamine is discouraged, since the bioavailability of oral thiamine is very low. The same is true for ascorbic acid: intravenous ascorbic acid yields serum levels that may be 100 times that of an oral dose.11 Replacement recommendations range from 500 mg intravenously daily for postoperative patients to up to 3 g intravenously daily for patients in high-risk groups, such as the septic patient.5,7
Drug names: furosemide (Lasix and others), tramadol (Ultram, Ryzolt, and others).
Author affiliations: Departments of Medicine and Psychiatry, South Texas Veterans Health Care System and University of Texas Health Science Center, San Antonio.
Potential conflicts of interest: None reported.
Funding/support: None reported.
REFERENCES
1. Igata A. Clinical studies on rising and rerising neurological diseases in Japan: a personal contribution. Proc Jpn Acad, Ser B, Phys Biol Sci. 2010;86(4):366-377. PubMed doi:10.2183/pjab.86.366
2. Fouron JC, Chicoine L. Scurvy: special aspects of the association rickets—scurvy[article in French]. Can Med Assoc J. 1962;86:1191-1196. PubMed
3. Caine D, Halliday GM, Kril JJ, et al. Operational criteria for the classification of chronic alcoholics: identification of Wernicke’s encephalopathy. J Neurol Neurosurg Psychiatry. 1997;62(1):51-60. PubMed doi:10.1136/jnnp.62.1.51
4. Thomson AD, Cook CC, Touquet R, et al; Royal College of Physicians, London. The Royal College of Physicians report on alcohol: guidelines for managing Wernicke’s encephalopathy in the accident and Emergency Department. Alcohol Alcohol. 2002;37(6):513-521. PubMed doi:10.1093/alcalc/37.6.513
5. Berger MM. Vitamin C requirements in parenteral nutrition. Gastroenterology. 2009;137(suppl):S70-S78. PubMed doi:10.1053/j.gastro.2009.08.012
6. Egoramaiphol S, Migasena P, Supawan V. Effect of oral contraceptive agents on thiamine status. J Med Assoc Thai. 1985;68(1):19-23. PubMed
7. Fukushima R, Yamazaki E. Vitamin C requirement in surgical patients. Curr Opin Clin Nutr Metab Care. 2010;13(6):669-676. PubMed doi:10.1097/MCO.0b013e32833e05bc
8. Mydl×k M, Derzsiovס K, Zemberovס E. Influence of water and sodium diuresis and furosemide on urinary excretion of vitamin B(6), oxalic acid and vitamin C in chronic renal failure. Miner Electrolyte Metab. 1999;25(4-6):352-356. PubMed doi:10.1159/000057474
9. Thorp VJ. Effect of oral contraceptive agents on vitamin and mineral requirements. J Am Diet Assoc. 1980;76(6):581-584. PubMed
10. Brown TM. A case of Shoshin Beriberi: lessons old and new for the psychiatrist. Psychosomatics. 2013;54(2):175-180. PubMed doi:10.1016/j.psym.2012.01.010
11. Levine M, Espey MG, Chen Q. Losing and finding a way at C: new promise for pharmacologic ascorbate in cancer treatment. Free Radic Biol Med. 2009;47(1):27-29. PubMed doi:10.1016/j.freeradbiomed.2009.04.001