Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: Agitated patients commonly present to the emergency department (ED), posing immediate safety risks to themselves, the staff, and other patients. Management of severe agitation is best accomplished by a protocolized, team-based "alert"-type response that incorporates specific systems to deliver a series of patterned actions and immediate availability of calming medications to ensure prompt, best-practice care of this vulnerable patient group. While the intricacies of categorization and contingency plans for management of various levels of agitation have not been laid out in much detail, the protocol devised by Wilson et al in 2012 guides the overall management strategy.
Management of Severe Agitation in the Emergency Department of a Community Hospital in Brooklyn, New York: Establishing "Code White"
To the Editor: Agitated patients commonly present to the emergency department (ED), posing immediate safety risks to themselves, the staff, and other patients. Management of severe agitation is best accomplished by a protocolized, team-based "alert"-type response that incorporates specific systems to deliver a series of patterned actions and immediate availability of calming medications to ensure prompt, best-practice care of this vulnerable patient group. While the intricacies of categorization and contingency plans for management of various levels of agitation have not been laid out in much detail, the protocol devised by Wilson et al1 in 2012 guides the overall management strategy. A revised algorithm and tailored approach are warranted as more information becomes available about the etiologies of agitation and variety of management techniques.
To address this need, we undertook (1) a literature review that culminated in the development of an algorithm for treatment of different levels of agitation and (2) a survey of ED staff to identify difficulties in providing care for agitated patients, which informed a set of "code white" procedures for managing severely agitated patients.
Methods. The project was a collaborative effort by the Departments of Emergency Medicine and Psychiatry at a large community hospital and academic training center in Brooklyn, New York, and it resulted in the development of an algorithm to identify various levels of agitation of all etiologies, not limited to acute psychiatric emergencies, by means of a comprehensive literature review for established best practices and existing guidelines.
Staff in both departments were also surveyed to determine the problems perceived as major obstacles in implementing optimal patient care for severely agitated patients. A total of 38 staff members of various levels and in different roles, including attending physicians, residents, registered nurses, security guards, and technicians, were approached and asked a 10-question survey (available from the authors on request), with their responses recorded and transcribed. These responses identified obstacles that were addressed to create a uniform hospital team response protocol for managing severely agitated patients.
Results.
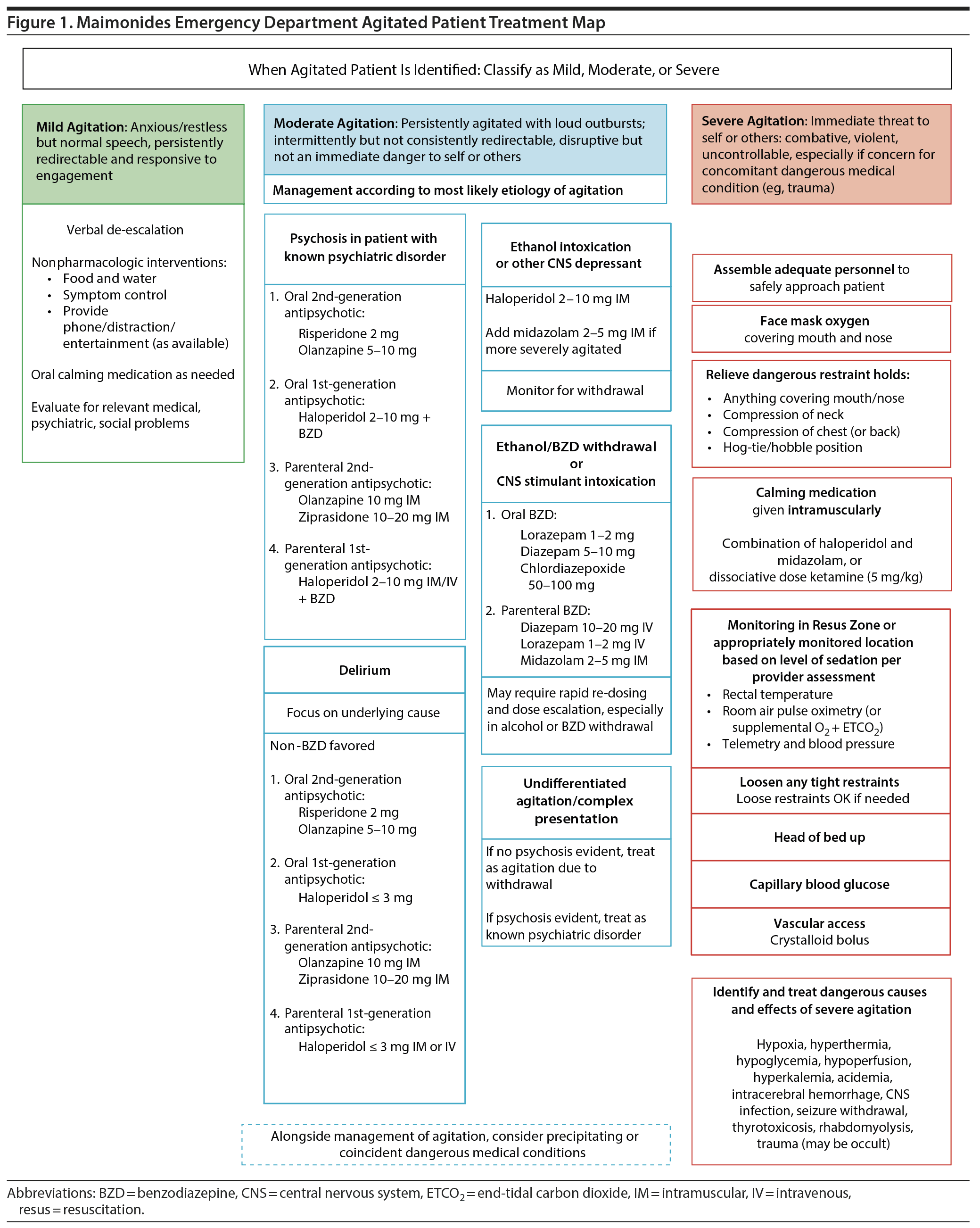
Algorithm development. The literature review supports an approach that is tailored to the potential cause of the agitation; therefore, our algorithm (Figure 1) is divided on the basis of tentative etiologies. A safe approach for undifferentiated agitation is also included in the algorithm for cases in which the intervention is time sensitive and needs to be performed before further assessment can be completed. The algorithm includes the following points.
- For agitation secondary to psychosis, oral antipsychotic medications that absorb rapidly are preferred (risperidone and olanzapine oral disintegrating tablets), as they are perceived as less coercive, offer proper sedation, and pose less risk of injury to staff and patients than the administration of IM or IV medications. These are followed by first-generation antipsychotics like haloperidol, which has a fair side effect profile and few drug-drug interactions.
- For severe agitation, a short- to medium-acting benzodiazepine can be added to increase the potential for sedation and decrease the risk of extrapyramidal side effects from higher doses of typical antipsychotics.
- In the case of alcohol or central nervous system depressants withdrawal, behavioral agitation should be managed with medium- to long-acting benzodiazepines, with the choice of agent depending on the formulary available, route of administration needed, and level of liver impairment (lorazepam, diazepam, chlordiazepoxide).
ED staff survey. While most staff (90% [n = 34 respondents]) agreed that the ED staff were fairly skillful in the management of agitated patients, the main obstacles to care identified were
- Lack of rapid access to calming medications (79% [n = 30])
- Lack of training and expertise among personnel in the general ED to ascertain when to deploy verbal de-escalation techniques versus medications (39% [n = 15])
- Narrower hallways and limited triage space to create adequate physical room for application of physical and chemical restraints (26% [n = 10])
- Absence of an established team with designated staff roles for safely and effectively managing the emergency
- Long lengths of time taken to triage the patients and transport them to an enclosed safe space in the Psychiatric ED
- Difficulty in predicting episodes and preemptively preparing for emergencies like severe agitation.
The lack of a protocolized targeted approach became evident by reports from staff that suggested they found themselves utilizing chemical or physical restraints more frequently if the ED was getting busier.
Code white protocol. Assimilating these survey data, we established the "code white" protocol as part of the agitated patient guideline (Figure 1) to enable staff to screen and categorize levels of agitation, identify etiologies, and treat appropriately. A virtual kit was placed in the medication dispenser (Pyxis, BD; Franklin Lakes, New Jersey) to facilitate the immediate availability of appropriate calming medications. This multidisciplinary patient-centered approach to agitation can be applied across institutions with a similar ED patient population.
Severely agitated patients often present an immediate danger to themselves and others. Skillful management of these agitated patients in the ED is therefore not only crucial for the safety of staff and but also ensures that these agitated patients receive the standard of care so their medical needs may be met. A protocolized, team-based "code white" approach to the management of severe agitation, alongside recommendations for etiology-specific treatment of mild and moderate agitation, may improve staff safety and patient outcomes.
Reference
1. Wilson MP, Pepper D, Currier GW, et al. The psychopharmacology of agitation: consensus statement of the American Association for Emergency Psychiatry Project Beta Psychopharmacology Workgroup. West J Emerg Med. 2012;13(1):26-34. PubMed CrossRef
aDepartment of Psychiatry, Maimonides Medical Center, Brooklyn, New York
Potential conflicts of interest: None.
Funding/support: None.
Published online: February 21, 2019.
Prim Care Companion CNS Disord 2019;21(1):18l02348
To cite: Virani S, Bona A, Bodic M, et al. Management of severe agitation in the emergency department of a community hospital in Brooklyn, New York: establishing "code white." Prim Care Companion CNS Disord. 2019;21(1):18l02348.
To share: https://doi.org/10.4088/PCC.18l02348
© Copyright 2019 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!