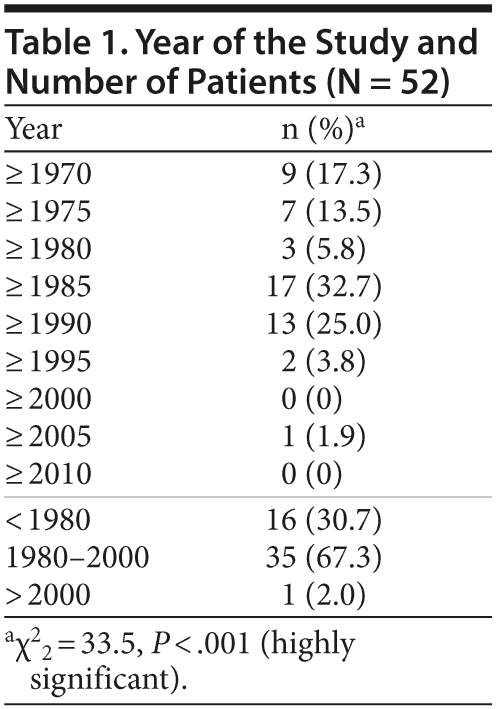Reversible Lithium Neurotoxicity: Review of the Literature

ABSTRACT
Objective: Lithium neurotoxicity may be reversible or irreversible. Reversible lithium neurotoxicity has been defined as cases of lithium neurotoxicity in which patients recovered without any permanent neurologic sequelae, even after 2 months of an episode of lithium toxicity. Cases of reversible lithium neurotoxicity differ in clinical presentation from those of irreversible lithium neurotoxicity and have important implications in clinical practice. This review aims to study the clinical presentation of cases of reversible lithium neurotoxicity.
Data Sources: A comprehensive electronic search was conducted in the following databases: MEDLINE (PubMed), 1950 to November 2010; PsycINFO, 1967 to November 2010; and SCOPUS (EMBASE), 1950 to November 2010. MEDLINE and PsycINFO were searched by using the OvidSP interface.
Study Selection: A combination of the following search terms was used: lithium AND adverse effects AND central nervous system OR neurologic manifestation. Publications cited include articles concerned with reversible lithium neurotoxicity.
Data Extraction: The age, sex, clinical features, diagnostic categories, lithium doses, serum lithium levels, precipitating factors, and preventive measures of 52 cases of reversible lithium neurotoxicity were extracted.
Data Synthesis: Among the 52 cases of reversible lithium neurotoxicity, patients ranged in age from 10 to 80 years and a greater number were female (P = .008). Most patients had affective disorders, schizoaffective disorders, and/or depression (P < .001) and presented mainly with acute organic brain syndrome. In most cases, the therapeutic serum lithium levels were less than or equal to 1.5 mEq/L (P < .001), and dosage regimens were less than 2,000 mg/day. Specific drug combinations with lithium, underlying brain pathology, abnormal tissue levels, specific diagnostic categories, and elderly populations were some of the precipitating factors reported for reversible lithium neurotoxicity. The preventive measures were also described.
Conclusions: Reversible lithium neurotoxicity presents with a certain clinical profile and precipitating factors for which there are appropriate preventive measures. This recognition will help in early diagnosis and prompt treatment of lithium neurotoxicity.
Prim Care Companion CNS Disord 2012;14(1): doi:10.4088/PCC.11r01197
© Copyright 2012 Physicians Postgraduate Press, Inc.
Submitted: April 12, 2011; accepted June 22, 2011.
Published online: January 26, 2012.
Corresponding author: Vivek H. Phutane, MD, Department of Psychiatry, Yale University School of Medicine, 34 Park St, New Haven, CT 06519 ([email protected]).
Lithium is an efficacious treatment, especially for the prophylaxis of bipolar mood disorders. There is a continuum from simple side effects of lithium to early reversible lithium neurotoxicity and irreversible lithium neurotoxicity. Most often, lithium neurotoxicity is reversible but sometimes may be irreversible. Reversible lithium neurotoxicity has been defined as cases of lithium neurotoxicity in which patients recovered without any permanent neurologic sequelae, even after 2 months of an episode of lithium toxicity.
Irreversible lithium neurotoxicity presents with permanent neurologic sequelae such as cerebellar impairment, dementia, parkinsonian syndromes, choreoathetosis, brain stem syndromes, and peripheral neuropathies. The sequelae are defined as irreversible if they persist more than 2 months after the discontinuation of lithium treatment following an episode of lithium toxicity.1
Precipitating factors other than overdose are not well identified. Lithium neurotoxicity can occur during the initial few days of treatment as well as after years of maintenance therapy. Sometimes, the early signs of lithium neurotoxicity are missed, and patients gradually slip into severe neurotoxicity. Lithium neurotoxicity rarely presents as a serotonin-like syndrome, a neuroleptic malignant-like syndrome, or a Creutzfeldt-Jakob-like syndrome.2
There are no typical clinical features to clearly identify a case of reversible lithium neurotoxicity. The clinical features of irreversible lithium toxicity are permanent and easier to detect, whereas reversible lithium neurotoxicity is transitory and difficult to evaluate. There are reviews on irreversible lithium neurotoxicity but none on reversible lithium neurotoxicity.
This review presents the reported cases of reversible lithium neurotoxicity and its clinical profile. The precipitating factors with probable mechanisms and the preventive measures to avoid lithium neurotoxicity are also examined.
METHOD
A comprehensive electronic search was conducted in the following databases: MEDLINE (PubMed), 1950 to November 2010; PsycINFO, 1967 to November 2010; and SCOPUS (EMBASE), 1950 to November 2010. MEDLINE and PsycINFO were searched by using the OvidSP interface. A combination of the following search terms was used: lithium AND adverse effects AND central nervous system OR neurologic manifestation. All references of the articles included in this review were searched.
Only articles reporting about reversible lithium neurotoxicity were selected. We (I.N. and V.H.P.) independently inspected all reports of identified studies and resolved any disagreement by consensus; however, when doubts arose, the full article was inspected. We also independently decided whether these studies met our inclusion criteria. In this review, reversible lithium neurotoxicity is defined as cases of lithium neurotoxicity in patients who recovered without any permanent neurologic sequelae, even after 2 months of an episode of lithium toxicity. All cases of reversible lithium neurotoxicity in adults irrespective of their gender, ethnicity, functioning level, and inpatient or outpatient status were included. Cases of irreversible lithium neurotoxicity, cases without a clear outcome of reversibility or partial recovery from lithium neurotoxicity, and cases reporting minor neurologic side effects of lithium were excluded. Also, special studies of children, adolescents, or elderly patients regarding lithium neurotoxicity were not included.
Data from the included studies were extracted according to the following criteria: author, year of publication of the article, age, sex, diagnosis, lithium dosage, lithium level, drug combinations with lithium, investigations, clinical features (physical and mental), precipitating factors, and preventive measures. The results obtained were tabulated, and statistical analysis was completed using the 1-variable goodness-of-fit χ2 test.
RESULTS
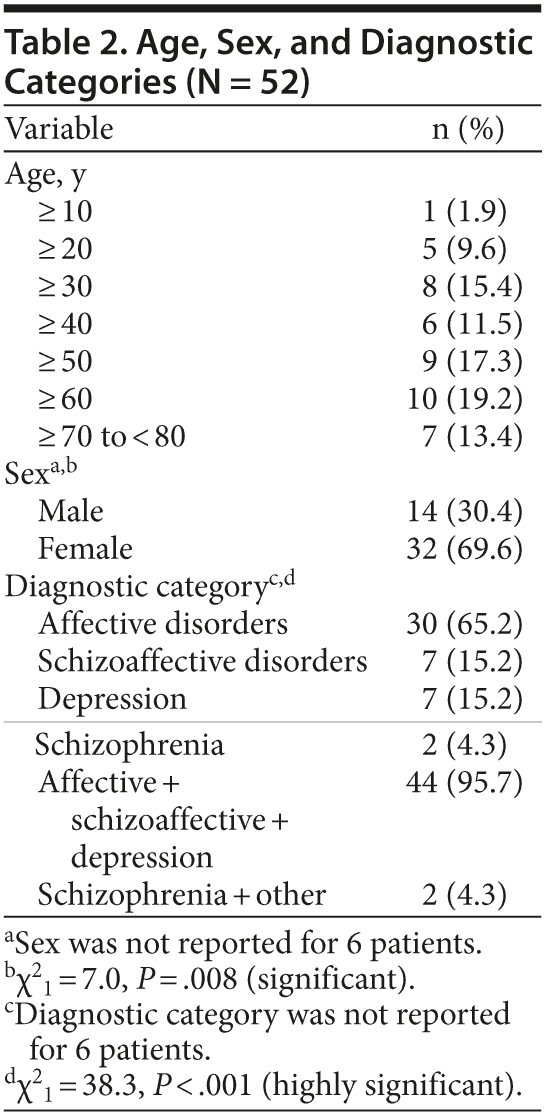
Thirty-five (67.3%) of the studies were published during the period 1980-2000,3,15,17-25,28,30,32-35,37-39,43 16 (30.7%) were published before 1980,4,5,26,40,41 and 1 (2.0%) was published after 2000 (Table 1).36 The ages of the patients ranged from 10 to 80 years (Table 2). Of 52 patients, 14 (30.4%) were male and 32 (69.6%) were female; sex was not reported for 6 patients (χ21 = 7.0, P < .008) (Table 2). Forty-four studies (95.7%) included the diagnostic categories of affective disorders, schizoaffective disorders, and depression3-5,15,17-21,24-26,28-30,32-41,43; 2 studies (4.3%) included schizophrenia and other disorders35; and the diagnostic category was not reported in the combined study that included 6 cases (χ21 = 38.3, P < .001) (Table 2).3
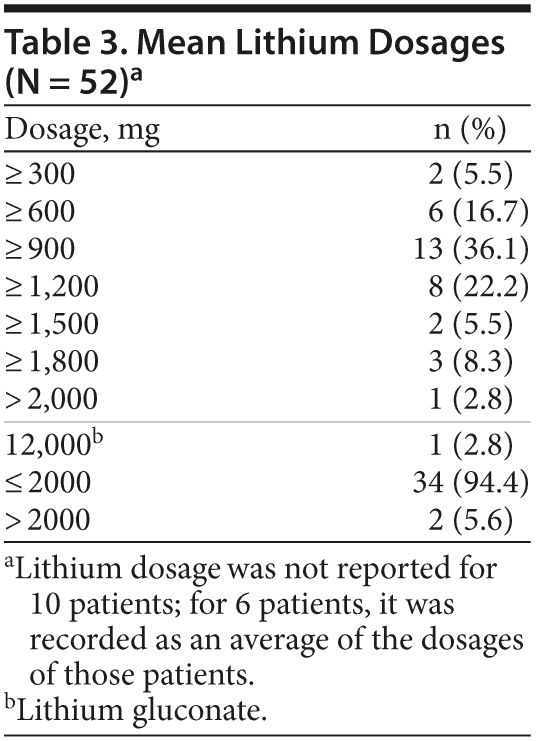
The lithium dosages were in the range of 300 to 2,000 mg/day. In 10 cases, the lithium dose was not mentioned,5,24,26,30,38 whereas in 6 cases, the lithium dose was recorded as an average of the dosages of the 6 patients,3 and in 1 case, the dose was 12,000 mg/day of lithium gluconate (Table 3).22 The serum lithium levels in 31 patients (79.5%) were in the range below or equal to 1.5 mEq/L. In 8 patients (20.5%), the serum lithium level was greater than 1.5 mEq/L (Table 4).
Year of Publication
Most of the studies of reversible lithium neurotoxicity were published during the period 1980-2000. The oldest report was in 1984, and the most recent was in 2008. Since 2000, there has been a decline in reported cases of reversible lithium neurotoxicity (Table 1).
The decline in publications correlates with the declining secular trends of lithium use. Although there is increasing evidence for lithium treatment, there has been a decrease in use of lithium.6-8 This decrease is due to the use of anticonvulsants such as valproate,9 carbamazepine,10 lamotrigine,11 topiramate,12 and atypical antipsychotics,13,14 which have proved efficacy for the management of bipolar disorders. Another reason for decreased use could be the early detection of toxicity due to the increased awareness among clinicians about lithium toxicity and its consequences.
Age
The age ranges of the patients were from 10 to 80 years. The study with a combined report of 6 cases, however, did not report the respective ages of each patient but did provide a mean age of 33.7 years for males and 38.4 for females.3 Age does not seem to be correlated in cases of lithium toxicity.1,2
Sex
A greater number of female patients were reported among the cases of reversible lithium neurotoxicity. This result was statistically significant (P = .008); however, this finding does not mean that women are more prone to develop lithium neurotoxicity. Two reviews have also confirmed this observation that more female cases of lithium toxicity have been reported in the literature.1,2
Diagnostic Categories
Most cases of reversible lithium neurotoxicity were in patients with affective disorders, schizoaffective disorders, and depression. This result was highly statistically significant (P < .001). There were 2 reports of patients with schizophrenia. The diagnostic categories in the combined study of 6 cases were not reported. The older studies reported older diagnostic categories as compared to the recent studies. Psychiatric diagnosis does not seem to correlate with the development of lithium toxicity.1,2
Clinical Features: Physical
Most patients included in this study presented with pyramidal, extrapyramidal, and cerebellar signs. In 1 report, cerebellar signs were the first and only neurologic signs to appear.15 Some of the important findings were tremor, ataxia, gait problems, myoclonus, hyperreflexia, dysarthria, convulsions, and incontinence. This result is in keeping with the general observation that there is usually pyramidal tract involvement in acute lithium neurotoxicity. Extrapyramidal syndromes do occur alone or in combination with neuroleptic drugs. Some authors have also found cerebellar signs in cases of reversible lithium neurotoxicity. This view contrasts with that of Schou who considered that cerebellar signs did not occur in acute lithium toxicity.16
There was 1 case of reversible lithium neurotoxicity that presented as a serotonin-like syndrome17 and another that presented as a neuroleptic malignant-like syndrome,18 6 cases presented as Creutzfeldt-Jakob-like syndromes,19-23 and 2 cases presented as pseudotumor cerebri.24 The case of reversible lithium neurotoxicity with serotonin-like syndrome included akathisia, myoclonus, increased reflexes, shivering, tremor, increased diarrhea, and incoordination.25 The case of the patient with reversible lithium neurotoxicity who developed a neuroleptic malignant-like syndrome showed increased pulse rate, blood pressure, and temperature.15 The other features were intention tremor, rigidity, confusion, disorientation, urinary retention, and increased creatine kinase levels.15
Six cases of reversible lithium neurotoxicity presented as a Creutzfeldt-Jakob-like syndrome with a rapidly progressive dementia, myoclonus, ataxia, dysphasia, pyramidal tract signs, and personality and behavioral changes.19-23 Electroencephalographic (EEG) findings of a disorganization background and burst patterns were present in the cases.19-23 Two cases of reversible lithium neurotoxicity showed pseudotumor cerebri.24 These patients had increased intracranial pressures, normal or even small ventricles observed on neuroradiologic evaluation, normal cerebrospinal fluid constituents, and papilledema.24 None of the patients with reversible lithium neurotoxicity showed any permanent choreoathetoid movements, brain stem involvement, peripheral neuropathies, or other permanent postneurotoxic sequelae that are usually seen in cases of irreversible lithium neurotoxicity.
Clinical Features: Mental
Most cases of reversible lithium neurotoxicity presented as an acute organic brain syndrome (delirium). Six patients did not show any mental change. The clinical features of delirium were mainly disorientation, distractibility, memory impairment, fluctuating of consciousness, impaired concentration, auditory hallucinations, visual hallucinations, and visual illusions. The patients with Creutzfeldt-Jakob-like syndrome showed mainly features of dementia. The finding that acute lithium neurotoxicity presents with delirium has also been confirmed in 1 study.2
Investigations
Nine cases reported normal investigations despite lithium toxicity.4,15,17,32,34,36,37,41,43 Ten cases did not report any investigation findings.4,5,35,40,41 Five normal5,24,28,30,32,37 and 1 abnormal38 computed tomography scans were reported. One magnetic resonance image was normal.35 Two studies reported lumbar pressure findings,24 and 3 cerebrospinal fluid reports were normal.17,21,28 Ten cases reported abnormal EEG findings.19-23,26,30,32 These findings were confirmed by another study that found that patients with EEG abnormalities, cerebral impairment, and epilepsy are at high risk for lithium neurotoxicity.26 The diffuse slowing of the EEG may be of great diagnostic significance, and its monitoring would be useful to detect early lithium neurotoxicity.26
Lithium Dosage
Most cases of reversible lithium neurotoxicity developed on dosages below 2,000 mg/day, which were within the therapeutic range. In 10 cases, the lithium doses were not reported. In the study with combined data of 6 patients, the mean lithium dose was 1,047 and the peak lithium doses were 1,550 (in chlorpromazine equivalents).3 A lithium gluconate dose of 12,000 mg/day was reported in 1 case study.22 No cases of toxic/fatal overdoses of reversible lithium neurotoxicity were reported (Table 4).
Lithium neurotoxicity commonly occurs at high dosages but can also occur at therapeutic dosages. Lithium toxicity is at times unpredictable, and there is no definite correlation between serum lithium levels and neurotoxicity.1,2,27 One study maintained that lithium-neuroleptic-induced neurotoxicity is dose dependant.3 Miller and Menninger3 reported that the dosage of the neuroleptic and not the serum lithium level or lithium dose predicts neurotoxicity.
Serum Lithium Levels
Serum lithium levels below 1.5 mEq/L were reported in 31 cases,1,4,5,15,17-19,21,24,26,28,30,32-35,38,39 and 8 reported serum lithium levels above 1.5 mEq/L.4,19,23,37,40 Seven cases did not report serum lithium levels,5,20-22,24,25,29 and the study with a combined data of 6 cases reported a mean serum lithium level of 1.23 mEq/L.3 Most cases of reversible lithium neurotoxicity had serum lithium levels below 1.5 mEq/L. This finding was highly statistically significant (χ2 = 13.5, P < .001). In another study, the red blood cell lithium level was 1.0 mmol/L and the serum lithium level was 0.2 mmol/L.28 The lithium toxicity occurring at low or therapeutic serum lithium levels has been referred to as paradoxical or pathological lithium neurotoxicity.
Generally, serum lithium levels of 1.0-1.5 mEq/L have been recommended for the treatment of acute manic episodes and levels of 0.8-1.0 mEq/L for the prophylaxis of bipolar mood disorders. Severe lithium intoxication is usually at serum lithium levels < 3.0 mEq/L and levels ≥ 5.0 mEq/L can be fatal.29
The lithium pump regulates lithium transfer from intracellular to extracellular space, and its activity is an index of lithium toxicity. Many cases of death due to lithium neurotoxicity have been due to increased intracellular lithium concentration. Red blood cell lithium levels are a better indicator of brain levels and lithium neurotoxicity than serum lithium levels. Some authors recommend red blood cell lithium level monitoring in addition to serum level, as it is a more sensitive index of brain lithium levels.28,30 Young and Hammond6 reported the development of neurotoxicity when serum lithium levels were in the lower range due to intracellular transfer of lithium and regretted that red blood cell lithium levels were not monitored in their study. There may be interindividual differences in red blood cell levels (ie, plasma ratios that are partly genetic).31
Precipitating Factors
Various reasons have been described as precipitating factors for reversible lithium neurotoxicity.
Combination therapies. Neuroleptic-lithium combinations were involved in precipitating lithium neurotoxicity in 18 cases.3,26,32-36 Both typical and atypical antipsychotics such as haloperidol, thioridazine, risperidone, and clozapine have been implicated.3,26,32-36
Haloperidol. Some authors have described cases of reversible lithium neurotoxicity precipitated by a combination of lithium and haloperidol.3,32,33 Haloperidol is commonly used as an antimanic agent together with lithium, and there is an increased risk for lithium neurotoxicity, but the mechanism of action is unclear. Increased intracellular concentration of lithium has been attributed as a probable mechanism for lithium neurotoxicity.33
Thioridazine. Four cases of reversible lithium neurotoxicity were due to the lithium-thioridazine combination.26 The combination has a strong dopamine-blocking effect.26
Risperidone. One study described reversible lithium neurotoxicity in a patient receiving a combination of lithium and risperidone.36 The probable mechanism for neurotoxicity was due to increased dopamine receptor blockage and increased intracellular lithium concentrations.36
Clozapine. Reversible lithium neurotoxicity was reported in patients receiving a combination of lithium and clozapine. Lithium neurotoxicity was attributed to the interaction of the serotonergic effects of clozapine with lithium in 2 studies.34,35
Various other drug combinations with lithium are reported to have precipitated reversible lithium neurotoxicity. Cases of reversible lithium neurotoxicity that occurred with a lithium and fluoxetine combination have been described.17,25,37 Muly et al17 described a serotonin-like syndrome with the lithium-fluoxetine combination. The possible mechanism is due to the acute shift in the balance of dopaminergic and cholinergic transmitters in the putamen and caudate nucleus.25
Reversible lithium neurotoxicity presented as Creutzfeldt-Jakob-like syndrome that was precipitated when lithium was combined with levodopa, nortriptyline, amitriptyline, and polypharmacy.19-22 The possible mechanism is that polypharmacy has multiple synergistic and hepatic effects that can cause cognitive decline. The myoclonus was probably due to serotonin agonism activity.22
One case of a neuroleptic malignant-like syndrome was described when lithium was combined with doxepin.26 Idiosyncratic and intermittent deficiency in the compensatory mechanism following blockage of dopamine regulation of muscle tone and temperature has been attributed as a possible mechanism.
Underlying neurologic disease. Some authors described patients who developed reversible lithium neurotoxicity due to underlying brain pathology. All patients had paradoxically low lithium levels and recovered without any postsequelae.38-40 Various mechanisms for these findings have been given. Kemperman et al38 suggest that an abnormal affinity for lithium in pathological brain tissue and also the diminished capacity for lithium removal in pathological transformed brain tissue are causes for neurotoxicity. Another study by Ghadirian and Lehmann39 described a case of alcoholism causing a subclinical encephalopathy and thus inducing a central pathological hypersensitivity to lithium. One case of reversible lithium neurotoxicity was precipitated by unusual sensitivity to lithium due to cerebral impairment.40
Abnormal tissue levels. Van der Velde41 described 3 cases of reversible lithium neurotoxicity precipitated by abnormal tissue levels. A possible mechanism that has been proposed is that acute manic patients store lithium ions in the intracellular water of certain tissues or in extracellular space other than plasma that precipitates lithium toxicity.42 Some patients do not excrete lithium properly, and the lower blood lithium levels reflect an affinity for such nonplasma compartments for the lithium ion against the concentration gradient that is even steeper for manic patients, leading to abnormal tissue lithium levels that could result in toxic changes.4
No Precipitating Factors
There were some cases wherein no precipitating factors could be attributed as the cause of reversible lithium neurotoxicity.15,21,23,28,30
Preventive Measures
Various measures to prevent reversible lithium neurotoxicity have been suggested in light of clinical findings. Most authors state that the combination of lithium with neuroleptics is useful but warn of the potential for lithium neurotoxicity. A special caution has been recommended when high-potency neuroleptics such as haloperidol are used in high doses combined with lithium to control severe manic excitement.33 Also, lower doses and strict monitoring have been suggested when clozapine and lithium are combined.34 When thioridazine is used with lithium, baseline and subsequent follow-up EEG monitoring are recommended.26
Neurotoxicity that develops at therapeutic serum lithium levels should alert the clinician to the possibility of a treatable intracranial pathology.38 Ghadirian and Lehmann39 caution about the possibility of a subclinical encephalopathy leading to lithium neurotoxicity in patients with alcoholism. Finelli21 recommends that all patients suspected to have pseudotumor cerebri due to receiving lithium should have a fundoscopy examination and an inquiry should be made regarding the lithium treatment history. Fluctuating serum lithium levels may point to the possibility of abnormal tissue levels.41 Caution has been recommended when lithium is used in the elderly population.41 Manic patients with prominent psychotic symptoms and intense anxiety are more prone to lithium neurotoxicity.5
Increased awareness about the possibility of a serotonin-like syndrome when lithium is combined with fluoxetine has been highlighted, although the combination is not contraindicated.17,43 In a study of EEG findings in lithium neurotoxicity, Broussolle et al20 emphasized that periodic sharp waves detected by serial EEGs should alert the clinician to the possibility of neurotoxicity.
Clinicians should obtain a lithium treatment history for all patients who present with a rapidly progressive dementia and EEG findings suggestive of a Creutzfeldt-Jakob-like syndrome. This will prevent lithium toxicity and avoid expensive, unnecessary neurologic investigations and invasive brain procedures such as brain biopsy.19,21 Gangadhar et al28 recommend the use of both red blood cell and serum lithium levels whenever possible in patients showing signs of lithium neurotoxicity, as serum lithium levels alone are not reliable to detect lithium toxicity. The possibility of finding the precipitating factor for lithium neurotoxicity may not be possible in some cases, as has been noted in some studies.15
Reversible Lithium Neurotoxicity and Irreversible Lithium Neurotoxicity
Cases of reversible lithium neurotoxicity and irreversible lithium neurotoxicity have no specific correlation with age or sex distribution. Most cases of reversible lithium neurotoxicity included serum lithium levels in the therapeutic range without any reported overdosages, whereas most cases of irreversible lithium neurotoxicity included levels above the therapeutic range, and some were even fatal or dangerously high due to suicidal intent.16 After 2 months of the lithium neurotoxicity episode, no permanent postneurologic sequelae were seen in reversible lithium neurotoxicity, but this was seen in irreversible lithium neurotoxicity.16 Cerebellar signs seen in reversible lithium neurotoxicity were completely reversible, whereas those seen with irreversible lithium neurotoxicity were permanent. Choreoathetosis and peripheral neuropathies were seen only in irreversible lithium neurotoxicity.44 Reversible lithium neurotoxicity presented as an acute brain syndrome (delirium) with complete recovery, whereas irreversible lithium neurotoxicity presented as a chronic brain syndrome requiring rehabilitation. Among the precipitating factors, lithium overdoses and drug interactions were seen in irreversible lithium neurotoxicity but not in reversible lithium neurotoxicity.1,2
DISCUSSION
Fifty-two cases of reversible lithium neurotoxicity were reviewed. The clinical profiles of these patients with reference to age, sex, diagnostic categories, clinical features, lithium dosages, and serum lithium levels were examined. The precipitating factors with their possible mechanisms and the preventive measures recommended were also studied. Thirty-five studies reported single case reports, 11 reported more than 1 case report, and 1 study was a combined report of 6 cases.3 Only 2 studies reported that grant funding was received for their publication.4,5
Limitations
The data in this review were secondary and heterogeneous in nature. There could be some minimal bias in selection of cases. The studies were published mainly during the period from 1980 to 2000. Some of the older studies had older diagnostic classifications compared to the more recent ones. We may have missed some articles in our search strategy. Many of the studies reported various clinical doses and serum lithium levels during the period of lithium neurotoxicity, but the most significant level was chosen. A few studies did not report certain data such as age, sex, specific lithium doses, and lithium levels. One study reported a combined data analysis of 6 cases.3 Most authors described precipitating factors for reversible lithium neurotoxicity in their respective cases, but other confounding factors could have also been present. All of these limitations were clearly stated whenever possible in the review and taken care of during the statistical analysis.
Strengths
Fifty-two cases of reversible lithium neurotoxicity were examined, and the data were carefully extracted and synthesized. A clearer profile of reversible lithium neurotoxicity emerges and has been compared with that of irreversible lithium neurotoxicity. The precipitating factors and the precautions to prevent reversible lithium neurotoxicity have also been described.
CONCLUSION
The following clinical profile emerges after evaluation of the 52 cases of reversible lithium neurotoxicity. Reversible lithium neurotoxicity was observed in all age groups, and a greater number of reported patients were female. Reversible lithium neurotoxicity was seen mainly in patients with affective disorders, schizoaffective disorders, and depression, and lithium carbonate doses were mostly in the therapeutic range of less than 2,000 mg/day and serum lithium levels were below 1.5 mEq/L. The common clinical features (physical) were mainly pyramidal, extrapyramidal, and cerebellar neurologic signs, and the common clinical features (mental) were mainly of an acute brain syndrome (delirium). The most common abnormal investigations reported were abnormal EEGs. The common precipitating factors for reversible lithium neurotoxicity were antipsychotic drug combinations with lithium, brain pathology, abnormal tissue levels, advanced age (elderly), acute manic psychotic symptoms and anxiety, and other drugs, and for some cases the precipitating factor could not be ascertained.
Clinical Implications
This review has described the clinical profile of and precipitating factors and preventive measures for reversible lithium neurotoxicity. This review will help in the prevention of lithium neurotoxicity through early detection, conservative prescribing, careful monitoring, care in combining other drugs with lithium, prompt management, and proper psychoeducation of patients and caregivers.
Drug names: carbamazepine (Carbatrol, Equetro, and others), clozapine (Clozaril, FazaClo, and others), doxepin (Zonalon, Silenor, and others), fluoxetine (Prozac and others), haloperidol (Haldol and others), lamotrigine (Lamictal and others), lithium (Lithobid and others), risperidone (Risperdal and others), topiramate (Topamax and others), valproate (Depacon and others).
Author affiliations: Parmar Plaza Clinic, Fatimanagar, Pune, Maharashtra, India (Dr Netto); and Department of Psychiatry, Yale University School of Medicine, Connecticut Mental Health Center, New Haven, Connecticut (Dr Phutane).
Author contributions: Both authors contributed to the following aspects of the study: concepts, design, definition of intellectual content, literature search, clinical studies, data acquisition, data analysis, statistical analysis, manuscript preparation, manuscript editing, manuscript review, and guarantor.
Funding/support: None reported.
Potential conflict of interest: None reported.
Acknowledgment: The authors thank Saraswati Garad, MSc (consultant biostatistician in private practice, Pune, Maharashtra, India). Ms Garad reports no conflicts of interest related to the subject of this article.
REFERENCES
1. Verdoux H, Bourgeois M. [Irreversible neurologic sequelae caused by lithium]. Encephale. 1991;17(3):221-224. PubMed
2. Kores B, Lader MH. Irreversible lithium neurotoxicity: an overview. Clin Neuropharmacol. 1997;20(4):283-299. PubMed doi:10.1097/00002826-199708000-00001
3. Miller F, Menninger J. Lithium-neuroleptic neurotoxicity is dose dependent. J Clin Psychopharmacol. 1987;7(2):89-91. PubMed doi:10.1097/00004714-198704000-00007
4. Agulnik PL, Dimascio A, Moore P. Acute brain syndrome associated with lithium therapy. Am J Psychiatry. 1972;129(5):621-623. PubMed
5. West AP, Meltzer HY. Paradoxical lithium neurotoxicity: a report of five cases and a hypothesis about risk for neurotoxicity. Am J Psychiatry. 1979;136(7):963-966. PubMed
6. Young AH, Hammond JM. Lithium in mood disorders: increasing evidence base, declining use? Br J Psychiatry. 2007;191(6):474-476. PubMed doi:10.1192/bjp.bp.107.043133
7. Fieve RR. Lithium therapy at the millennium: a revolutionary drug used for 50 years faces competing options and possible demise. Bipolar Disord. 1999;1(2):67-70. PubMed doi:10.1034/j.1399-5618.1999.010201.x
8. Goodwin FK. Rationale for long-term treatment of bipolar disorder and evidence for long-term lithium treatment. J Clin Psychiatry. 2002;63(suppl 10):5-12. PubMed
9. Macritchie K, Geddes JR, Scott J, et al. Valproate for acute mood episodes in bipolar disorder. Cochrane Database Syst Rev. 2003;1(1):CD004052. PubMed
10. Emilien G, Maloteaux JM, Seghers A, et al. Lithium compared to valproic acid and carbamazepine in the treatment of mania: a statistical meta-analysis. Eur Neuropsychopharmacol. 1996;6(3):245-252. PubMed doi:10.1016/0924-977X(96)00029-6
11. Goodwin GM, Bowden CL, Calabrese JR, et al. A pooled analysis of 2 placebo-controlled 18-month trials of lamotrigine and lithium maintenance in bipolar I disorder. J Clin Psychiatry. 2004;65(3):432-441. PubMed doi:10.4088/JCP.v65n0321
12. McIntyre RS, Mancini DA, McCann S, et al. Topiramate versus bupropion SR when added to mood stabilizer therapy for the depressive phase of bipolar disorder: a preliminary single-blind study. Bipolar Disord. 2002;4(3):207-213. PubMed doi:10.1034/j.1399-5618.2002.01189.x
13. Vieta E, Goikolea JM. Atypical antipsychotics: newer options for mania and maintenance therapy. Bipolar Disord. 2005;7(suppl 4):21-33. PubMed doi:10.1111/j.1399-5618.2005.00212.x
14. Yatham LN. Atypical antipsychotics for bipolar disorder. Psychiatr Clin North Am. 2005;28(2):325-347. PubMed doi:10.1016/j.psc.2005.01.001
15. Kumar R, Deb JK, Sinha VK. Lithium neurotoxicity at therapeutic level—a case report. J Indian Med Assoc. 1999;97(11):473-474. PubMed
16. Schou M. Long-lasting neurological sequelae after lithium intoxication. Acta Psychiatr Scand. 1984;70(6):594-602. PubMed doi:10.1111/j.1600-0447.1984.tb01254.x
17. Muly EC, McDonald W, Steffens D, et al. Serotonin syndrome produced by a combination of fluoxetine and lithium. Am J Psychiatry. 1993;150(10):1565. PubMed
18. Rosenberg PB, Pearlman CA. NMS-Like syndrome with a lithium/doxepin combination. J Clin Psychopharmacol. 1991;11(1):75-76. PubMed doi:10.1097/00004714-199102000-00023
19. Smith SJ, Kocen RSA. A Creutzfeldt-Jakob like syndrome due to lithium toxicity. J Neurol Neurosurg Psychiatry. 1988;51(1):120-123. PubMed doi:10.1136/jnnp.51.1.120
20. Broussolle E, Setiey A, Moene Y, et al. Reversible Creutzfeldt-Jakob like syndrome induced by lithium plus levodopa treatment. J Neurol Neurosurg Psychiatry. 1989;52(5):686-687. PubMed doi:10.1136/jnnp.52.5.686
21. Finelli PF. Drug-induced Creutzfeldt-Jakob like syndrome. J Psychiatry Neurosci. 1992;17(3):103-105. PubMed
22. Waldman AJA. A Creutzfeldt-Jakob-like syndrome due to polypharmacy. South Med J. 1990;83(12):1493. PubMed doi:10.1097/00007611-199012000-00034
23. Primavera A, Brusa G, Poeta MGA. A Creutzfeldt-Jakob like syndrome due to lithium toxicity. J Neurol Neurosurg Psychiatry. 1989;52(3):423. PubMed doi:10.1136/jnnp.52.3.423
24. Saul RF, Hamburger HA, Selhorst JB. Pseudotumor cerebri secondary to lithium carbonate. JAMA. 1985;253(19):2869-2870. PubMed doi:10.1001/jama.253.19.2869
25. Noveske FG, Hahn KR, Flynn RJ. Possible toxicity of combined fluoxetine and lithium. Am J Psychiatry. 1989;146(11):1515. PubMed
26. Spring GK. Neurotoxicity with combined use of lithium and thioridazine. J Clin Psychiatry. 1979;40(3):135-138. PubMed
27. Donaldson IM, Cuningham J. Persisting neurologic sequelae of lithium carbonate therapy. Arch Neurol. 1983;40(12):747-751. PubMed
28. Gangadhar BN, Subhash MN, Umapathy C, et al. Lithium toxicity at therapeutic serum levels. Br J Psychiatry. 1993;163(5):695. PubMed doi:10.1192/bjp.163.5.695a
29. Strayhorn JM Jr, Nash JL. Severe neurotoxicity despite “therapeutic” serum lithium levels. Dis Nerv Syst. 1977;38(2):107-111. PubMed
30. Bell AJ, Cole A, Eccleston D, et al. Lithium neurotoxicity at normal therapeutic levels. Br J Psychiatry. 1993;162(5):689-692. PubMed doi:10.1192/bjp.162.5.689
31. Speirs J, Hirsch SR. Severe lithium toxicity with “normal” serum concentrations. BMJ. 1978;1(6116):815-816. PubMed doi:10.1136/bmj.1.6116.815
32. Keitner GI, Rahman S. Reversible neurotoxicity with combined lithium-haloperidol administration. J Clin Psychopharmacol. 1984;4(2):104-105. PubMed doi:10.1097/00004714-198404020-00009
33. Coffey CE, Ross DR. Treatment of lithium/neuroleptic neurotoxicity during lithium maintenance. Am J Psychiatry. 1980;137(6):736- 737. PubMed
34. Lee SH, Yang YY. Reversible neurotoxicity induced by a combination of clozapine and lithium: a case report. Zhonghua Yi Xue Za Zhi (Taipei). 1999;62(3):184-187. PubMed
35. Blake LM, Marks RC, Luchins DJ. Reversible neurologic symptoms with clozapine and lithium. J Clin Psychopharmacol. 1992;12(4):297-299. PubMed doi:10.1097/00004714-199208000-00025
36. Boora K, Xu J, Hyatt J. Encephalopathy with combined lithium-risperidone administration. Acta Psychiatr Scand. 2008;117(5):394-395, discussion 396. PubMed doi:10.1111/j.1600-0447.2008.01165.x
37. Salama AA, Shafey M. A case of severe lithium toxicity induced by combined fluoxetine and lithium carbonate. Am J Psychiatry. 1989;146(2):278. PubMed
38. Kemperman CJ, Gerdes JH, De Rooij J, et al. Reversible lithium neurotoxicity at normal serum level may refer to intracranial pathology. J Neurol Neurosurg Psychiatry. 1989;52(5):679-680. PubMed doi:10.1136/jnnp.52.5.679-a
39. Ghadirian AM, Lehmann HE. Acquired transient CNS hypersensitivity to lithium therapy. Can J Psychiatry. 1980;25(8):662-665. PubMed
40. Rifkin A, Klein DF, Quitkin F. Organic brain syndrome during lithium carbonate treatment. Compr Psychiatry. 1973;14(3):251-254. PubMed doi:10.1016/S0010-440X(73)80018-5
41. Van der Velde CD. Toxicity of lithium carbonate in elderly patients. Am J Psychiatry. 1971;127(8):1075-1077. PubMed
42. Greenspan K, Goodwin FK, Bunney WE, et al. Lithium ion retention and distribution. Patterns during acute mania and normothymia. Arch Gen Psychiatry. 1968;19(6):664-673. PubMed
43. Shah AK, McCloskey O. Case report: acute confusional state secondary to a combination of fluoxetine and lithium. Int J Geriatr Psychiatry. 1992;7(9):687-688. doi:10.1002/gps.930070911
44. Adityanjee RJ. The syndrome of irreversible lithium-effectuated neurotoxicity (SILENT). Pharmacopsychiatry. 1989;22(2):81-83.