ABSTRACT
Objective: To assess the efficacy and safety evidence for adjunct minocycline in treatment-resistant depression (TRD).
Data Sources: In this systematic review, PubMed, PubMed Central, Embase, and Google Scholar were searched from inception to October 2022. The following keywords were utilized in the search: “depression” AND “minocycline” AND “treatment, pharmacological intervention, management.” Medical Subject Heading terms for “minocycline” and “depression, depressive disorder, treatment-resistant,” and “disease management” were also used. Relevant peer-reviewed, English-language articles that included adults and children were selected for final evaluation.
Study Selection: Two authors independently searched and selected 1,004 relevant articles. Only randomized controlled trials were considered. Five articles were identified that fulfilled the inclusion criteria.
Data Extraction: The PICO algorithm (Population, Intervention, Comparison, Outcomes, and Study Design) framework was utilized, and Preferred Reporting Items for Systematic Reviews and Meta-Analyses criteria guidelines were followed. The Cochrane risk of bias tool was used to categorize the included study as a low, unclear, or high risk of bias.
Results: Minocycline as an adjunct immunomodulator shows inconsistent benefit in TRD. Minocycline has some beneficial effect on depression scale scores and inflammatory markers in TRD patients with inflammatory disequilibrium (C-reactive protein elevation exceeds 3 mg/L). However, minocycline showed an inconclusive effect in TRD with no clear immunologic dysregulation. Minocycline might have a neuroprotective, rather than therapeutic, effect at a small dose.
Conclusions: The results were inconsistent regarding the clinical and neuroprotective role of minocycline in TRD. More study is needed to clarify the pathophysiologic and clinical role of minocycline as an immunomodulator in TRD.
Prim Care Companion CNS Disord 2023;25(5):22r03467
Author affiliations are listed at the end of this article.
Neuroinflammation has increasingly received attention as one of the potential etiologic explanations for treatment-resistant depression (TRD).1–3 TRD is major depressive disorder (MDD) with an unsatisfactory response to 2 different classes of antidepressant medications at an optimal dosage and duration.2 The neuroinflammation theory of MDD has been supported by the elevated level of C-reactive protein (CRP), interleukin-1β (IL-1β), IL-6, prostaglandin-E2 (PGE2), cyclo-oxygenase-2 expression, tumor necrosis factor-α (TNF-α), interferon (IFN) α or β, catalase, and malondialdehyde in chronic depression without medical illness.1,3–6 CRP is a sensitive early phase reactive protein that can be used as a psychiatric marker for treatment resistance, medication adverse effects, or prognostic factors.7 Also, CRP levels ≥ 3 mg/L were reported in 30%–50% of patients with TRD.7 Elevated plasma CRP correlated with cerebrospinal fluid elevation of CRP, TNF-α, and IL-6 inflammatory markers in MDD.4 Inflammatory and immune modulators such as infliximab, celecoxib, curcumin, aspirin, statins, and N-acetylcysteine have shown various antidepressant properties.3 Also, IFN-α therapy, a proinflammatory modulator cytokine, may lead to clinical depression in around 50% of patients.1 Furthermore, hypothalamic pituitary adrenal (HPA) axis disturbance with hypercortisolism and subsequent neuroinflammation dysregulates the HPA axis in TRD.1 Hypercortisolism due to HPA activation is a trigger factor for inflammatory disequilibrium, leading to low levels of brain-derived neurotrophic factor and serotonin, which explains the mechanism for TRD.1
Anti-inflammatory agents (eg, minocycline) can thus play a crucial role in treatment of TRD. Minocycline is a lipophilic protease inhibitor (easily crosses the blood-brain barrier) with central and peripheral anti-inflammatory, antioxidant, and antiapoptotic properties with a wide range of inflammatory mediator inhibitions.1 Minocycline has inflammatory, modulatory, and neuroprotective properties with beneficial effects for TRD, schizophrenia, and other neurodegenerative diseases like multiple sclerosis, head injury, Huntington’s disease, and Parkinson disease.1,8 Minocycline elevates brain serotonin levels via an inhibitory effect on the kynurenine inflammatory pathway and indoleamine 2,3-dioxygenase enzymatic activity.1 Furthermore, minocycline inhibits central immunologic inflammatory–triggering enzymes like nitric oxide synthase, matrix metalloproteinases, and caspase-1 and caspase-3 activation.4 Moreover, minocycline has a glutamate and monoamine neurotransmission modulation effect.1 Also, minocycline can suppress microglial, astrocyte hyperactivation, and brain lymphocyte infiltration, leading to overall promotion of brain neurogenesis and neuroplasticity.3,4 Minocycline can clinically reverse the depressive effects of IFN-α therapy.3 Several preclinical and clinical studies1,3,4 have shown the antidepressant therapeutic benefits of minocycline in clinical depression. The objective of this systematic review was to analyze randomized controlled trials (RCTs) assessing the efficacy and safety of adjunct minocycline in TRD.
METHODS
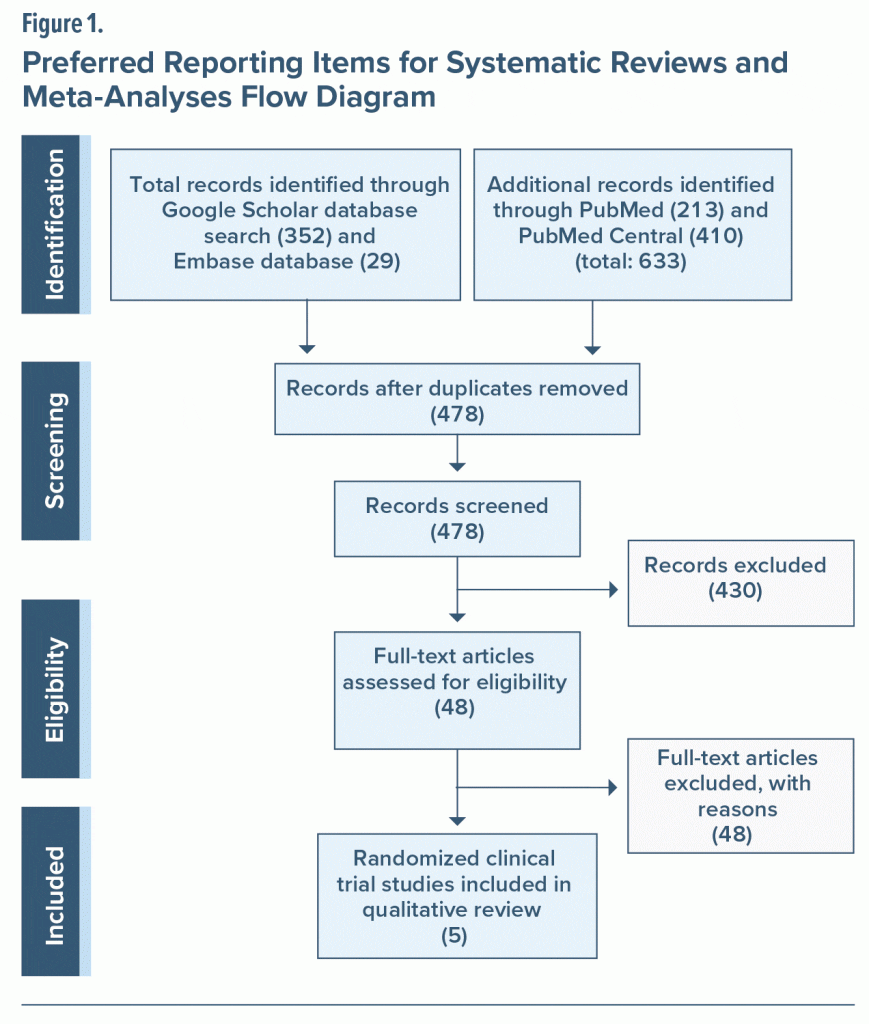
The PubMed, PubMed Central, Embase, and Google Scholar databases were searched for clinical trial studies from inception to October 2022. The following keywords were used in the search: “depression” AND “minocycline” AND “treatment, pharmacological intervention, management.” Medical Subject Heading terms for “minocycline” and “depression, depressive disorder, treatment-resistant,” and “disease management” were also used. Two authors (W.A.J. and C.T.) independently searched and selected relevant articles. We used the PICO (Population, Intervention, Comparison, Outcomes, and Study Design) algorithm for the search framework as follows: participants (adults or children and treatment-resistant depression), intervention (minocycline), comparison (placebos or minocycline), outcomes (improvement of depression symptoms or improvement of depression rating scale), study design (clinical trial or RCT). The Cochrane risk of bias tool was utilized to categorize the included study as having a low, unclear, or high risk of bias using Review Manager 5.4 software. The following biases were evaluated: (1) random sequence generation, (2) allocation concealment, (3) blinding of participants and personnel, (4) blinding outcome assessment, (5) incomplete outcome data, and (6) selective reporting for each included RCT. A study flow diagram, per Preferred Reporting Items for Systematic Reviews and Meta-Analyses criteria,9 is included in Figure 1.
Inclusion Criteria
(1) Prospective studies, including clinical studies, RCTs, double-blinded studies, and case-control series.
(2) Studies evaluating minocycline as the adjunct treatment in TRD.
(3) Publication type: Only peer-reviewed journal publications.
(4) Age: Adults and children.
Exclusion Criteria
(1) Study design: Case reports, open-label extension literature reviews, editorials, retrospective observational studies, and unpublished theses.
(2) Bipolar depression clinical studies.
(3) Publication type: Articles published in non–peer-reviewed journals.
(4) Articles published in non-English languages.
(5) Trial study including nonhumans.
Risk of Bias Assessment
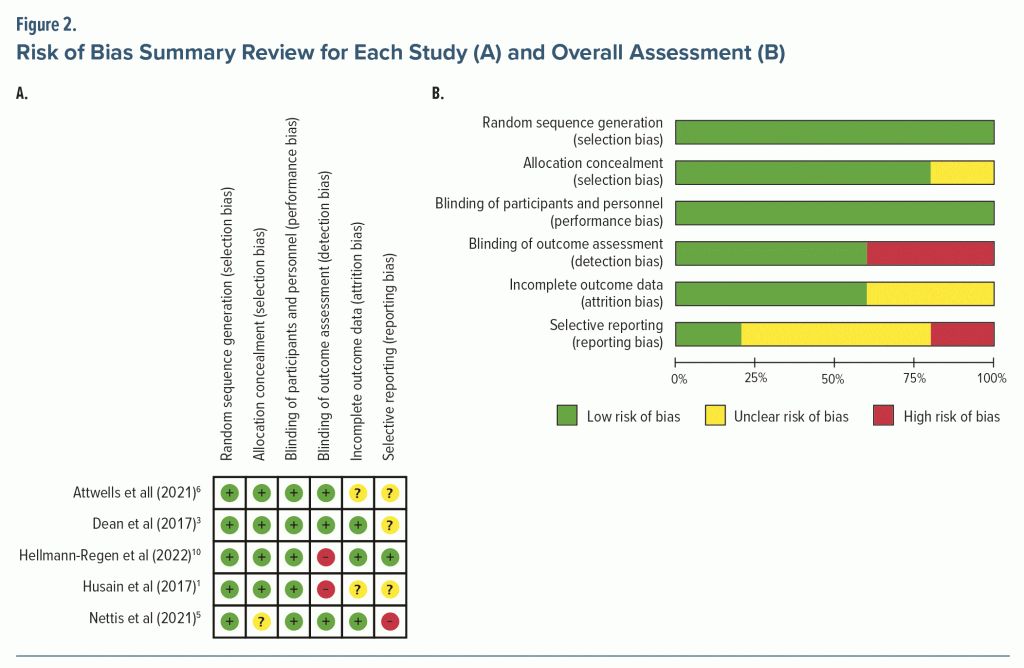
Figure 2 shows the risk of bias assessment. Five RCTs were included in the risk of bias assessment using the Cochrane risk of bias tool. Most of the studies had a low risk of bias except for Husain et al,1 in which blinding was not performed. In addition, for the study by Nettis et al,5 the data on failed medication for TRD were not included in the outcome analysis.
RESULTS
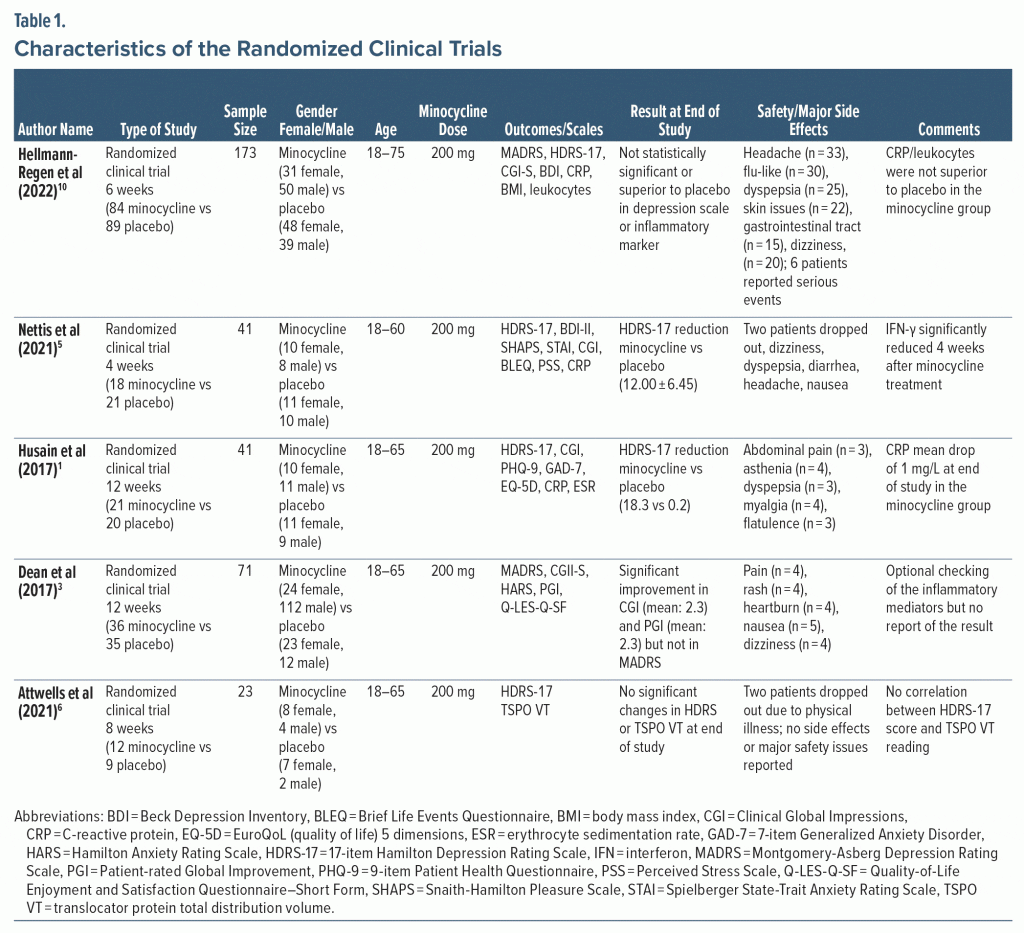
Five studies were included in this systemic review. The study characteristics are shown in Table 1.
In a 6-week RCT, Hellmann-Regen et al10 found that adjunct minocycline 200 mg for TRD was statistically insignificant and not superior to placebo after 2 weeks and at 6-month follow-up. The study10 included 173 nonobese adult patients aged 18–75 years (minocycline: 84 vs placebo: 89) with TRD (17-item Hamilton Depression Rating Scale [HDRS-17] ≥ 16 points), who failed standard treatment for MDD. The primary outcome was the Montgomery-Asberg Depression Rating Scale (MADRS) score, while the HDRS-17, Clinical Global Impressions (CGI)–severity, Beck Depression Inventory (BDI), Trail Making Test A and B, and Symptom Checklist 90-R were assessed as secondary outcomes. No significant change in baseline CRP and body mass index (BMI) was seen after 6 weeks. Six serious adverse events were reported during the trial.10
Nettis et al5 found that adjunct minocycline can augment the antidepressant action in MDD patients with CRP ≥ 3 mg/L. This 4-week RCT included 39 TRD patients (minocycline: 18 vs placebo: 21, aged 25–60 years, HDRS-17 score ≥ 17) with elevated CRP levels ≥ 1 mg/L. Minocycline (200 mg/d) was added as an augmenting agent.5 Overall, the minocycline patients with CRP ≥ 3 showed a statistically significant reduction (P < .001) in HDRS-17 scores (12.00 ± 6.45) compared with the minocycline patients with CRP < 3 mg/L (2.42 ± 3.20).5 However, no significant changes were seen in the scores of the placebo group regarding CRP levels.5 HDRS-17 changes were similar in the placebo patients with CRP ≥ 3 (3.50 ± 4.34) compared to the placebo group with CRP < 3 mg/L (2.11 ± 3.26).5 Also, IFN-γ was reduced at the end of treatment in the minocycline group.5 Dizziness, dyspepsia, diarrhea, headache, and nausea were the noted side effects in the study.5
The RCT by Husain et al1 included 41 adult patients randomized to receive minocycline 200 mg or placebo in addition to treatment as usual. Overall, 63% of the minocycline patients showed significant response per HDRS-17 scores (primary outcome) compared with 22% of the placebo patients (P = .035).1 The CGI, Patient Health Questionnaire, Generalized Anxiety Disorder scale, and EuroQoL 5 dimensions scale (evaluating health-related quality of life) were also assessed. The mean reduction in HDRS-17 score was 18.3 at 12 weeks (P = .001), with moderate improvement in CGI scores.1 Erythrocyte sedimentation rate (ESR) and CRP levels were inconsistently recorded during the study. Abdominal pain (n = 3), asthenia (n = 4), dyspepsia (n = 3), myalgia (n = 4), and flatulence (n = 3) were the primary side effects reported in the minocycline group.1
Dean et al3 conducted a 12-week placebo-controlled trial (N = 71) with minocycline 200 mg/d. The minocycline group showed significant improvement in CGI scores (P = .022) but not in the MADRS. CGI improvement was based on improvement in the Quality of Life Enjoyment and Satisfaction Questionnaire (P = .004) and Patient Global Impression (P = .017) rather than the MADRS.3 CRP and ESR levels were electively checked for some patients willing to consent. The mean reduction of CRP was 1 mg/L in the minocycline group at week 12.3 Pain (n = 4), rash (n = 4), heartburn (n = 4), nausea (n = 5), and dizziness (n = 3) were the primary side effects reported in the minocycline group.3
In an 8-week RCT (minocycline vs placebo), Attwells et al6 found that the addition of minocycline 200 mg in TRD patients showed no significant change in HDRS-17 scores or in the marker of brain gliosis translocator protein (TSPO). In addition, no correlation between HDRS-17 score and TSPO total distribution volume (VT) readings was recorded.6 Twenty-three patients aged 18–65 years with HDRS-17 scores > 19, not responding to antidepressants, were included. TSPO VT–brain positron emission tomography (PET) was utilized in the study as a marker of brain inflammation. No significant safety issues were reported.6
DISCUSSION
This is the most up-to-date review, to the best of our knowledge, of RCTs for the role of minocycline as an inflammatory mediator in the treatment of TRD. The review showed inconsistent results of adjunct minocycline for TRD but revealed that minocycline has a beneficial effect on depression scales and inflammatory markers in TRD patients with inflammatory disequilibrium (CRP elevation > 3 mg/L).1,5
Minocycline showed an inconclusive effect on HDRS-17, MADRS, CGI, and/or TSPO VT in TRD with no clear immunologic dysregulation.3,6,10 Minocycline showed mild curbing in TSPO VT gliosis, but it was not statistically significant, indicating that minocycline might have a neuroprotective, rather than therapeutic, effect at a 200-mg dose and 8-week length study.6 The most common minocycline side effects reported were dizziness, nausea, and gastrointestinal upset, which were minor.1,3–6,10
In comparison, the study by Emadi-Kouchak et al11 showed a significant reduction in HDRS-17 scores (> 50%) after 6 weeks with minocycline 200 mg as an adjunct treatment for HIV-associated mild-to-moderate depression. In the study,11 46 antidepressant-naive participants aged 18–55 years were randomly assigned to minocycline or placebo. A mean reduction in HDRS-17 scores of 3.83 ± 1.92 was noted. No significant side effects were reported.11 The study did not meet the inclusion criteria for this review, since the patients had treatment-naive mild-to-moderate depression. Miyaoka et al,12 in a 6-week open-label trial, found a substantial reduction in HDRS-17 scores (6.7 ± 1.9) after adding minocycline 150 mg/d to a selective serotonin reuptake inhibitor in 25 adult inpatients diagnosed with MDD with psychosis. The beneficial effect was observed in 80% of the patients (n = 20), and no severe side effects were reported.12 There were no inflammatory marker data in that study.12 Also, Avari et al,13 in another open-label trial, found a significant reduction in MADRS/HDRS-17 scores (31% achieved remission) after 8 weeks of adjunct minocycline 200 mg/d for unipolar or bipolar TRD. The 13 older adults (aged ≥ 55 years, mean age of 73.1 ± 11 years) with hopelessness and apathy included in the trial showed significant improvement with no safety concerns.13 Soczynska et al,14 in an 8-week open-label study in which minocycline 200 mg/d was added to the regimens of 27 adults with antidepressant bipolar TRD, found a significant reduction in depression scale scores (MADRS ≤ 10 and HAM-D-17 ≤ 7). The improvement was 25% in the MADRS, 22% in the HAM-D-17, and 33% in both scales.14 Inflammatory cytokines C-C motif chemokine ligand 26 reduction was observed after 8 weeks of minocycline treatment.13 Early life adversity, which includes trauma, abuse, neglect, and childhood trauma, is favorable for good response.14
Savitz et al,15 in a 6-week RCT of minocycline (200 mg) with/without aspirin versus placebo for adult patients (n = 107) with bipolar depression, found a combination of minocycline/aspirin was more effective than each medication alone or placebo in reducing the MADRS score. Also, in the same study, minocycline/aspirin antidepressant augmentation response (MADRS score visit 1: 28.0 ± 5.7 vs visit 7: 14.5 ± 8.9) was positively correlated with an initial high IL-6 (at visit 1) level but not with the CRP level.15 However, in a 12-week RCT of adjunct minocycline (200 mg) with or without celecoxib versus placebo in bipolar or unipolar depression, Husain et al16 found no clinical benefit as per the HDRS-17. The trial included 267 adult patients, with < 10% (n = 26) having an initial CRP level > 10 mg/L. No serious side effects were reported other than 31 patients had manic episodes.16
Augmenting the antidepressant medication with other anti-inflammatory medications like celecoxib, cytokine inhibitors, glucocorticoids, and/or statins showed a wide range of efficacy and safety in a meta-analysis of RCTs by Köhler-Forsberg et al17; however, no similar studies were found in TRD. In an RCT that included 60 adults with CRP ≥ 5 mg/L, the anti-inflammatory tumor necrosis factor antagonist infliximab was ineffective in curbing depressive symptoms in bipolar depression associated with chronic diseases.15 Compared to other inflammatory mediators, minocycline has a limited systemic effect, is more efficacious, has superior blood-brain barrier penetration, and has a neuroprotective effect on microglial cell overactivation.4
Minocycline showed conflicting efficacy in improving the negative and depressive symptoms of PET-TSPO in schizophrenia.4 While minocycline showed positive results in schizophrenia in 2 RCTs (total N = 148), these results failed to be replicated in a larger RCT (N = 207).4 Several clinical studies have demonstrated the effect of minocycline in altering the gut microbial system and subsequent reduction in hippocampal and systemic inflammation.4 However, no similar studies were replicated in the human model.4 Minocycline’s role in decreasing TSPO VT/PET showed a wide sensitivity range between preclinical rodents and human models.6,17 Minocycline efficacy in reducing the TSPO VT/PET as a marker of neuroinflammation and microglial activity in depression was reported in up to 33% of case-control studies (n = 20).16 Cerebrospinal fluid analysis and/or utilizing other microglial markers like purinergic receptors, transmembrane protein 119 (TMEM119), microglial response factor (MRF-1), vimentin, or ferritin could increase the sensitivity of detecting the neuroinflammatory changes.18
Limitation
The limited number of studies with heterogeneous study designs, short duration of follow-up, and small sample sizes in some studies restrict the power and generalizability of the results. In addition, the patient populations were from different ethnic and social backgrounds. Also, inflammatory biomarkers were inconsistent among studies that included CRP, IL-6, TNF, and correlation with depression scales. No subanalysis was reported on the effect of age, sex, or BMI on minocycline antidepressant efficacy. There was no report of the pharmacokinetic interaction between minocycline and different antidepressants. No results were reported on the impact of long-term use of minocycline antibiotics on gut microbial flora and/or antibiotic-resistant bacteria. There was limited information on TRD regarding the number of previous failed therapeutic trials, dose of the antidepressant, comorbidities, specifiers, and duration of depression limits in the interpretation of the results.
CONCLUSION
Although neuromodulation is promising in TRD, minocycline as an immunomodulator has shown inconsistent outcomes in the clinical setting and in depression scales and inflammatory markers. Adjunct minocycline shows beneficial effect in TRD in some studies with elevated inflammatory biomarkers, but these findings failed to be replicated in larger studies. Consistent utilization of inflammatory biomarkers such as CRP, IL-6, and TNF in conjunction with clinical assessment is a reasonable next step in TRD management guidelines before starting an immunoinflammatory mediator. We need a robust RCT with a large sample size and appropriate duration that includes a wide list of inflammatory biomarkers, including microglial overactivation, to appropriately subcategorize TRD patients who could benefit from adjunct inflammatory mediators like minocycline as novel augmentation treatment. Future studies can be helpful with other inflammatory mediators like P2X7 inhibitors, PGE4 inhibitors, or peroxisome proliferator γ agonists.
Article Information
Published Online: September 14, 2023. https://doi.org/10.4088/PCC.22r03467
© 2023 Physicians Postgraduate Press, Inc.
Submitted: December 15, 2022; accepted March 21, 2023.
To Cite: Al Jumaili W, Vora D, Trivedi C, et al. Role of minocycline as an adjunct neuroinflammatory modulator in treatment-resistant depression: a systematic review of randomized controlled trials. Prim Care Companion CNS Disord. 2023;25(5):22r03467.
Author Affiliations: Texas Tech University Health Science Center at Odessa/Permian Basin, Odessa (all authors).
Corresponding Author: Wisam Al Jumaili, MD, Texas Tech University-Health Science Center 2301 W Michigan Ave Midland, TX 79707 ([email protected]).
Author Contributions: Dr Al Jumaili worked on the title, introduction, discussions, limitations, and results. Dr Trivedi worked on the methodology. Drs Al Jumaili and Trivedi independently reviewed the selected relevant articles. Dr Vora worked on data extraction and summarization of the clinical trials. All authors equally searched and cross-summarized relevant articles and independently reviewed and edited this review. Dr Jain provided senior authorship and supervision.
Relevant Financial Relationships: None.
Funding/Support: None.
Clinical Points
- Minocycline has shown inconsistent immunomodulator clinical effect in treatment-resistant depression (TRD).
- Minocycline showed promising clinical and neuroprotective results in TRD patients with initial abnormal inflammatory markers.
- Well-designed randomized controlled trials that utilize a wide list of inflammatory biomarkers, including microglial overactivation markers, are needed to study the immunomodulation benefit of adjunct minocycline in TRD.
References (19)

- Husain MI, Chaudhry IB, Husain N, et al. Minocycline as an adjunct for treatment-resistant depressive symptoms: a pilot randomized placebo-controlled trial. J Psychopharmacol. 2017;31(9):1166–1175. PubMed CrossRef
- Al-harbi KS. Treatment-resistant depression: therapeutic trends, challenges, and future directions. Patient Prefer Adherence. 2012;6:369–388. PubMed CrossRef
- Dean OM, Kanchanatawan B, Ashton M, et al. Adjunctive minocycline treatment for major depressive disorder: a proof of concept trial. Aust N Z J Psychiatry. 2017;51(8):829–840. PubMed CrossRef
- Nettis MA. Minocycline in major depressive disorder: and overview with considerations on treatment-resistance and comparisons with other psychiatric disorders. Brain Behav Immun Health. 2021;17(17):100335. PubMed CrossRef
- Nettis MA, Lombardo G, Hastings C, et al. Augmentation therapy with minocycline in treatment-resistant depression patients with low-grade peripheral inflammation: results from a double-blind randomised clinical trial. Neuropsychopharmacology. 2021;46:939–948. PubMed CrossRef
- Attwells S, Setiawan E, Rusjan PM, et al. A double-blind placebo-controlled trial of minocycline on translocator protein distribution volume in treatment-resistant major depressive disorder. Transl Psychiatry. 2021;11(1):334. PubMed CrossRef
- Chamberlain SR, Cavanagh J, de Boer P, et al. Treatment-resistant depression and peripheral C-reactive protein. Br J Psychiatry. 2019;214(1):11–19. PubMed CrossRef
- Plane JM, Shen Y, Pleasure DE, et al. Prospects for minocycline neuroprotection. Arch Neurol. 2010;67(12):1442–1448. PubMed CrossRef
- Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372(71):n71. PubMed CrossRef
- Hellmann-Regen J, Clemens V, Grözinger M, et al. Effect of minocycline on depressive symptoms in patients with treatment-resistant depression: a randomized clinical trial. JAMA Netw Open. 2022;5(9):e2230367. PubMed CrossRef
- Emadi-Kouchak H, Mohammadinejad P, Asadollahi-Amin A, et al. Therapeutic effects of minocycline on mild-to-moderate depression in HIV patients: a double-blind, placebo-controlled, randomized trial. Int Clin Psychopharmacol. 2016;31(1):20–26. PubMed CrossRef
- Miyaoka T, Wake R, Furuya M, et al. Minocycline as adjunctive therapy for patients with unipolar psychotic depression: an open-label study. Prog Neuropsychopharmacol Biol Psychiatry. 2012;37(2):222–226. PubMed CrossRef
- Avari JN, Kanellopoulos D, Solomonov N, et al. Minocycline augmentation in older adults with persistent depression: an open label proof of concept study. Int Psychogeriatr. 2020;32(7):881–884. PubMed CrossRef
- Soczynska JK, Kennedy SH, Alsuwaidan M, et al. A pilot, open-label, 8-week study evaluating the efficacy, safety and tolerability of adjunctive minocycline for the treatment of bipolar I/II depression. Bipolar Disord. 2017;19(3):198–213. PubMed CrossRef
- Savitz JB, Teague TK, Misaki M, et al. Treatment of bipolar depression with minocycline and/or aspirin: an adaptive, 2×2 double-blind, randomized, placebo-controlled, phase IIA clinical trial. Transl Psychiatry. 2018;8(1):27. PubMed CrossRef
- Husain MI, Chaudhry IB, Hamirani MM, et al. Minocycline and celecoxib as adjunctive treatments for bipolar depression: a study protocol for a multicenter factorial design randomized controlled trial. Neuropsychiatr Dis Treat. 2016;13:1–8. PubMed CrossRef
- Köhler-Forsberg O, N Lydholm C, Hjorthøj C, et al. Efficacy of anti-inflammatory treatment on major depressive disorder or depressive symptoms: meta-analysis of clinical trials. Acta Psychiatr Scand. 2019;139(5):404–419. PubMed CrossRef
- Setiawan E, Wilson AA, Mizrahi R, et al. Role of translocator protein density, a marker of neuroinflammation, in the brain during major depressive episodes. JAMA Psychiatry. 2015;72(3):268–275. PubMed CrossRef
- Jurga AM, Paleczna M, Kuter KZ. Overview of general and discriminating markers of differential microglia phenotypes. Front Cell Neurosci. 2020;14:198. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!