Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: In 2013, we published a study of the levels of serum cytokines from 47 patients with schizophrenia and 20 healthy controls. We found significantly increased levels of GRO, MCP-1, MDC, and sCD40 L and significantly decreased levels of IFN-γ, IL-2, IL-12p70, and IL-17 in schizophrenia patients compared to controls. We also identified a potential role for the IL-17 pathway in worsening of schizophrenia symptoms.
Disequilibrium of Cytokine Serum Levels in Veterans With Chronic Schizophrenia Medicated With Antipsychotics: Association With Measures of Excitement and Hostility
To the Editor: In 2013, we published a study1 of the levels of serum cytokines from 47 patients with schizophrenia and 20 healthy controls. We found significantly increased levels of GRO, MCP-1, MDC, and sCD40 L and significantly decreased levels of IFN-γ, IL-2, IL-12p70, and IL-17 in schizophrenia patients compared to controls. We also identified a potential role for the IL-17 pathway in worsening of schizophrenia symptoms.1 We now have expanded this study by enrolling an additional 24 patients. Further, we obtained sequential samples and psychometric measures from 35 patients at a second visit, and 18 patients at a third visit. We hypothesized that cytokines within the Th17 pathway and their ratios to each other would be linked to distinct symptoms of psychopathology as measured by Positive and Negative Syndrome Scale (PANSS)2 scores. We utilized the total PANSS scores, general psychopathology scores, negative scale scores, and positive scale scores and the individual positive subscale symptoms: delusions, hallucinatory behavior, suspiciousness/persecution, conceptual disorganization, excitement, grandiosity, and hostility.
Method. In patients, symptom severity was evaluated using the PANSS. Cytokine/chemokine levels were tested with Millipore bead-based flow immunoassays in a Luminex 100 system (Luminex Corporation, Austin, Texas). The levels of 38 cytokines at each visit were correlated with PANSS scores. All statistical analyses were performed using SAS version 9.3 (SAS Institute Inc, Cary, North Carolina). A P value < .05 was considered to be statistically different for all comparisons.
Results. Subject demographics included 34.3% Hispanic, 44.3% white, 17.1% black, and 4.3% Asian. The mean ± SD patient age was 53.7 ± 10.4 years and control age was 41 ± 11.6 years. Gender distribution was 84% male and 16% female. No statistically significant differences in gender, ethnicity, body mass index, or weight were found between groups. All patients had a long-standing diagnosis of chronic paranoid schizophrenia and were undergoing treatment with antipsychotic medications. Of the patients, 35 (49.29%) were also treated with antidepressants. The mean ± SD PANSS scores in patients were 21.5 + 8.5 for positive symptoms, 21.9 ± 7 for negative symptoms, 40.8 ± 11 for general psychopathology symptoms, and 83.7 ± 24.2 for total scores. Clinical factors of illness (currently hospitalized or not, in-patient or out-patient), treatment with antidepressants, history of posttraumatic stress disorder, or substance abuse did not associate with psychopathology.
By performing the Hochberg method for multiple testing, 4 molecules were found to be increased in patients across all 3 visits: GRO, MCP-1, MDC, and sCD40 L. Levels of IFN-γ were decreased in patients compared to controls across all 3 time points. IL-17 levels were reduced only at visit 1, while levels of IL-4 were significantly decreased only at visit 3 (Table 1).
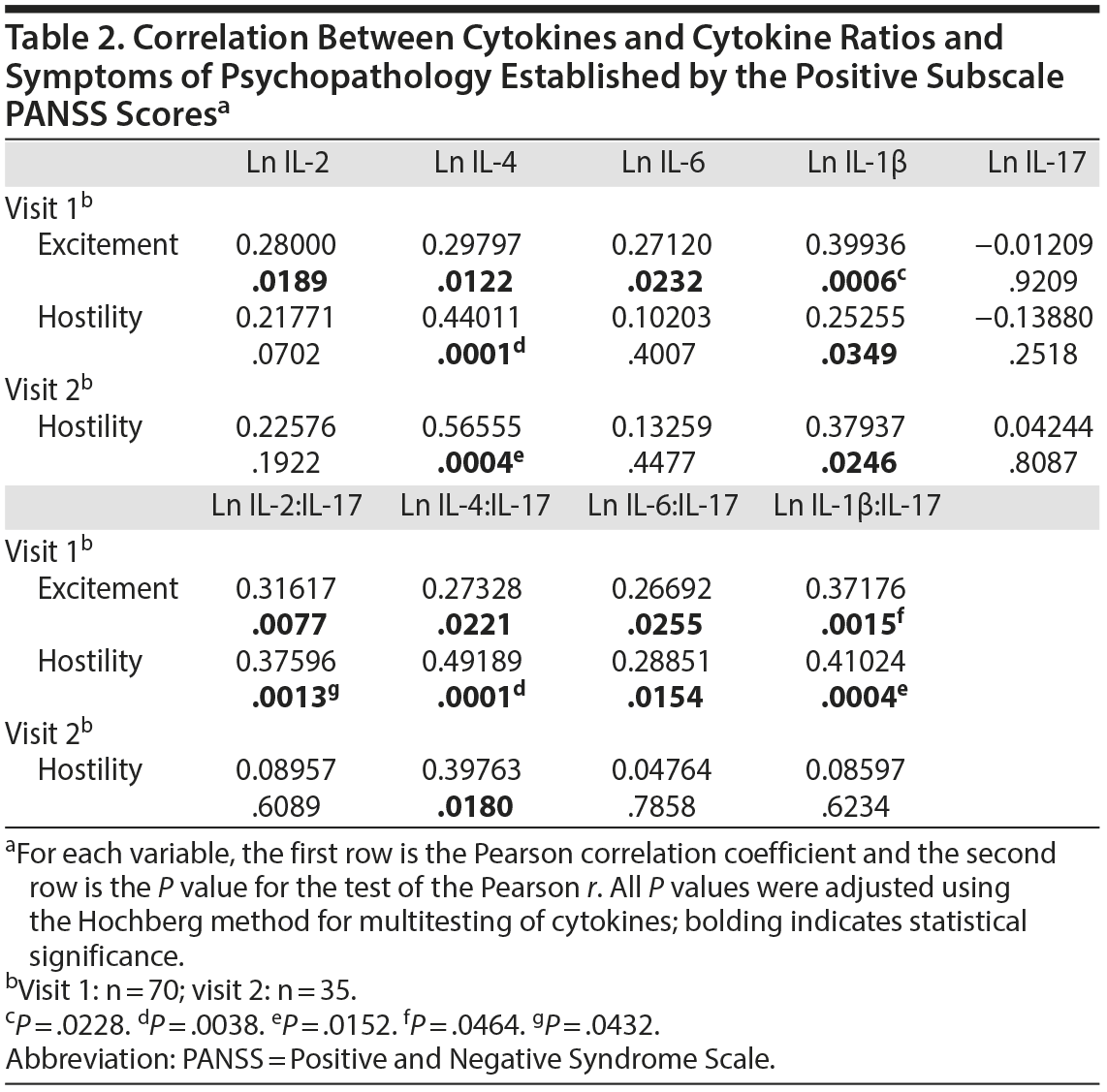
We established a significant correlation between IL-4 and hostility at visit 1 and visit 2 with adjusted P values of .0028 and .0152 using the Hochberg method. There was also a significant correlation between IL-1β and excitement at visit 1 with an adjusted P value of .0228 using the Hochberg method (Table 2).
The ratios of IL-2:IL-17, IL-4:IL-17, and IL-1β:IL-17 were associated with hostility in veterans with schizophrenia compared to control subjects. The ratio of IL-4:IL-17 was also associated with excitement. The adjusted P values of the above ratios using the Hochberg method were significant (Table 2).
Limitations of this study include the relatively small sample size. Also, we were unable to control for the effects of antipsychotic medications, which may modulate cytokine levels. Importantly, a higher proportion of Th17 cells and elevated plasma levels of IL-17 were described in drug-naive patients with a first episode of schizophrenia.3,4 However, after 4 weeks of risperidone treatment, there was a trend toward decreased plasma levels of IL-17.3
Our findings of decreased levels of IL-4, IL-17, and IL12p70 are in agreement with previous studies.5,6 When the levels of IFN-γ and IL-2 are low, the production of IL-17 is suppressed.6 Further, differentiation of naive T cells (To) to Th17 is mediated by IL-12 and IFN-γ.6 The low levels of IL-17 we observed could be influenced by the low levels of IL12p70, IL-2, or IFN-γ.7 Also, it is possible that the observed dysregulation of cytokines in veterans with chronic schizophrenia could be due to treatment with antipsychotics.
Importantly, levels of GRO, MCP-1, MDC, and sCD40 L were significantly elevated across all 3 visits. MCP-1 mediates the transendothelial migration of inflammatory cells across the blood-brain barrier and modulates local inflammatory response by inducing production of IL-4.8 Increased levels of IL-4 may reduce the production of IL-17.7
In conclusion, our results indicate that there is a link between imbalance of cytokine levels and psychopathology in veterans with chronic schizophrenia treated with antipsychotics. When the psychopathology was analyzed by the separate items of the positive subscale of the PANSS, we found that serum levels of IL-4 may correlate with hostility and IL-1β may correlate with excitement. We suggest that such an approach should be explored further.
REFERENCES
1. Dimitrov DH, Lee S, Yantis J, et al. Differential correlations between inflammatory cytokines and psychopathology in veterans with schizophrenia: potential role for IL-17 pathway. Schizophr Res. 2013;151(1-3):29-35. PubMed doi:10.1016/j.schres.2013.10.019
2. Kay S, Opler LA, Fizbein A, et al. Positive and Negative Syndrome Scale (PANSS) Technical Manual. Toronto, Ontario, Canada: Multi-Health Systems Inc; 2006.
3. Ding M, Song X, Zhao J, et al. Activation of Th17 cells in drug naive, first-episode schizophrenia. Prog Neuropsychopharmacol Biol Psychiatry. 2014;51:78-82. PubMed doi:10.1016/j.pnpbp.2014.01.001
4. El Kissi Y, Samoud S, Mtiraoui A, et al. Increased interleukin-17 and decreased BAFF serum levels in drug-free acute schizophrenia. Psychiatry Res. 2015;225(1-2):58-63. PubMed doi:10.1016/j.psychres.2014.10.007
5. Borovcanin M, Jovanovic I, Radosavljevic G, et al. Elevated serum level of type-2 cytokine and low IL-17 in first-episode psychosis and schizophrenia in relapse. J Psychiatr Res. 2012;46(11):1421-1426. PubMed doi:10.1016/j.jpsychires.2012.08.016
6. Weaver CT, Hatton RD, Mangan PR, et al. IL-17 family cytokines and the expanding diversity of effector T cell lineages. Annu Rev Immunol. 2007;25(1):821-852. PubMed doi:10.1146/annurev.immunol.25.022106.141557
7. Sarkar S, Tesmer LA, Hindnavis V, et al. Interleukin-17 as a molecular target in immune-mediated arthritis: immunoregulatory properties of genetically modified murine dendritic cells that secrete interleukin-4. Arthritis Rheum. 2007;56(1):89-100. PubMed doi:10.1002/art.22311
8. Reale M, Patruno A, De Lutiis MA, et al. Dysregulation of chemo-cytokine production in schizophrenic patients versus healthy controls. BMC Neurosci. 2011;12(1):13-22. PubMed doi:10.1186/1471-2202-12-13
Author affiliations: South Texas Veterans Health Care System, San Antonio (Drs Dimitrov and Braida, Ms Lee, and Messrs Yantis and Honaker); Department of Psychiatry, University of Texas Health Science Center at San Antonio (Drs Dimitrov, Coelho, Braida, and Walss-Bass); Department of Psychiatry and Behavioral Sciences, University of Texas Health Science Center at Houston (Dr Walss-Bass); and Pontifical Catholic University of Rio Grande do Sul, Porto Alegre, Brazil (Dr Coelho).
Potential conflicts of interest: None reported.
Funding/support: The research was supported by a New Investigator Award grant to Dr Dimitrov from the VISN 17 of the Department of Veterans Affairs.
Role of the sponsor: The funding organization had no role in the design or conduct of the study.
Published online: November 5, 2015.
Prim Care Companion CNS Disord 2015;17(6):doi:10.4088/PCC.15l01812
© Copyright 2015 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!