Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: Clinicians prescribe antimuscarinic compounds to treat the extrapyramidal side effects of neuroleptic medications. However, scopolamine has not been used for the management of such side effects. To the best of our knowledge, this is the first case of using scopolamine transdermal patch for management of extrapyramidal side effects of antipsychotic medications.
Scopolamine for Management of Extrapyramidal Side Effects as a Result of Antipsychotic Medication Use: A Case Report and Brief Review of the Literature
To the Editor: Clinicians prescribe antimuscarinic compounds to treat the extrapyramidal side effects of neuroleptic medications. However, scopolamine has not been used for the management of such side effects. To the best of our knowledge, this is the first case of using scopolamine transdermal patch for management of extrapyramidal side effects of antipsychotic medications.
Case report. Mr A is a 58-year-old white man with a protracted history of schizoaffective disorder, bipolar type, and nonadherence with medical treatment who was transferred to the state psychiatric hospital after being found asleep on the street. At admission, the patient was disheveled, malnourished, and disoriented to time, place, and situation with pressured speech and labile affect and demonstrated active, bizarre delusions and disorganized thought process. The initial laboratory workup, including blood counts, blood chemistries, urinalysis, and urine toxicology, was unremarkable.
Mr A was initially treated with oral haloperidol, valproic acid, and lorazepam as well as long-acting, injectable paliperidone 234 mg intramuscularly (IM) every 30 days, with an early improvement in agitation and aggression but with persistently disorganized, delusional, and impulsive behavior. Mr A’s hospital course was complicated by an increasing reluctance to take oral medications of any formulation for fear that he would become nauseous and vomit despite his ability to take food normally and no such observed adverse events. This refusal became adamant, and a psychopharmacology consultation was obtained in the hope of continuing Mr A’s current regimen. Options were limited, however, and as a result, valproic acid was discontinued, and the remainder of the patient’s medical treatment was administered, at the patient’s insistence, by injection only. On hospital day 38, long-acting, injectable haloperidol decanoate 300 mg IM was added to Mr A’s treatment plan. His condition gradually improved, and by hospital day 42, his behavior, thought content, and thought process were grossly organized. On hospital day 43, new-onset extrapyramidal symptoms (EPS) were noted with perioral gesticulations, bilateral hand tremor, elbow rigidity, and shuffling gait. Over 47 hospital days, Mr A received 61 IM injections of short-acting antipsychotics for psychosis and 40 IM injections of diphenhydramine for EPS prophylaxis.
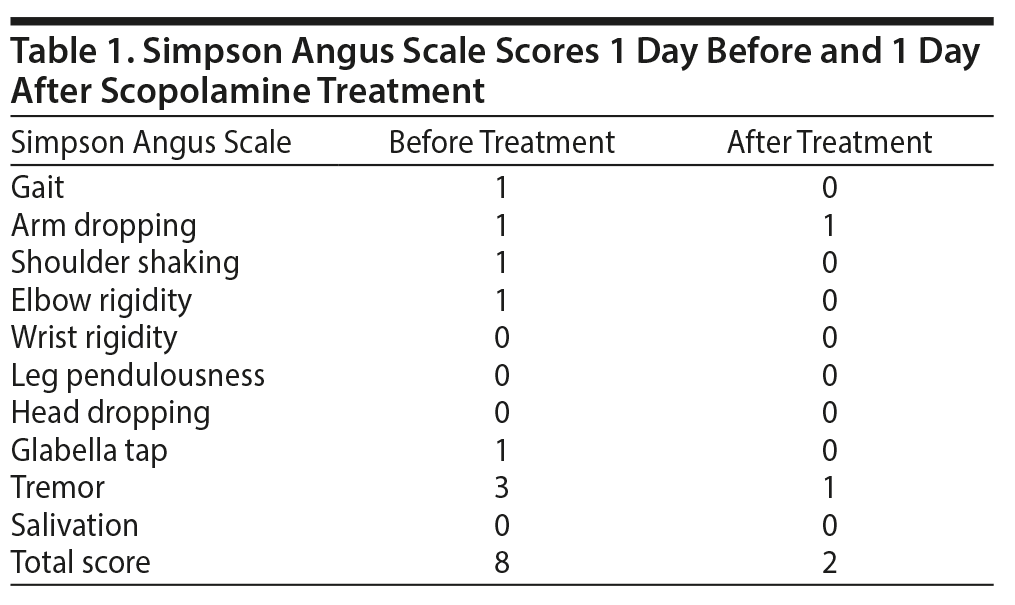
Despite an understanding that these symptoms were neuroleptic induced and required anticholinergic agents for treatment, Mr A remained steadfast in his refusal of oral medications. As daily multiple injections for the treatment of his condition were considered unviable, both as an inpatient and outpatient, an alternative was sought. A 1.5-mg transdermal scopolamine patch was administered. Mr A’s score on the Simpson Angus Scale1 was 8 one day before treatment and 2 one day after treatment initiation (Table 1). The patient denied any dry mouth, urinary hesitancy, or blurred vision, and no increased sedation was observed.
A thorough review of available English literature was conducted using the search terms scopolamine, antipsychotics, and extrapyramidal symptoms. We found no published case describing scopolamine for management of EPS resulting from antipsychotic medications. To the best of our knowledge, we are reporting the first case of using scopolamine transdermal patch for this indication.
Clinicians prescribe antimuscarinic compounds to lessen the extrapyramidal side effects of neuroleptic drugs used in the treatment of psychoses. The therapeutic effects occur through antagonism of central muscarinic acetylcholine receptors, the predominate type of cholinergic receptor in the brain. Muscarinic receptors have been further subdivided pharmacologically (M1, M2, and M3). Scopolamine, benztropine, and procyclidine are considered selective for M1 receptors.2 Scopolamine is a potent anticholinergic agent available in transdermal patch form approved for the treatment of motion sickness and has been found to decrease haloperidol-induced Fos expression in the striatum and lateral septal nucleus in rats, a proposed mechanism by which haloperidol may cause EPS.3 Although little information has been published regarding the rate of adverse effects of transdermal scopolamine compared to conventional oral anticholinergics, the adverse effect profile is similar to that of other agents.4
Few published examples relate to the possible extrapyramidal effects of scopolamine. In a randomized controlled clinical trial5 of the addition of transdermal scopolamine to a standard metoclopramide and dexamethasone antiemetic regimen, the authors found that scopolamine appeared to inhibit extrapyramidal reactions to the metoclopramide, but the number of cases was too small to reach statistical significance. One case report6 noted the appearance of acute dystonia coincident with the removal of a scopolamine patch in a postoperative patient treated prophylactically with prochlorperazine, metoclopramide, and ondansetron. Another case report7 suggested that patients with organophosphate poisoning who have mainly central nervous system toxicity might benefit from scopolamine administration.
We believe that further research is indicated for using scopolamine as a viable treatment alternative for neuroleptic-induced EPS.
References
1. Simpson GM, Angus JWS. A rating scale for extrapyramidal side effects. Acta Psychiatr Scand suppl. 1970;45(S212):11-19. PubMed doi:10.1111/j.1600-0447.1970.tb02066.x
2. Larson EW, Pfenning MA, Richelson E. Selectivity of antimuscarinic compounds for muscarinic receptors of human brain and heart. Psychopharmacology (Berl). 1991;103(2):162-165. PubMed doi:10.1007/BF02244197
3. Guo N, Robertson GS, Fibiger HC. Scopolamine attenuates haloperidol-induced c-fos expression in the striatum. Brain Res. 1992;588(1):164-167. PubMed doi:10.1016/0006-8993(92)91358-L
4. Clissold SP, Heel RC. Transdermal hyoscine (Scopolamine). A preliminary review of its pharmacodynamic properties and therapeutic efficacy. Drugs. 1985;29(3):189-207. PubMed doi:10.2165/00003495-198529030-00001
5. Meyer BR, O’ Mara V, Reidenberg MM. A controlled clinical trial of the addition of transdermal scopolamine to a standard metoclopramide and dexamethasone antiemetic regimen. J Clin Oncol. 1987;5(12):1994-1997. PubMed
6. Roberge RJ. Antiemetic-related dystonic reaction unmasked by removal of a scopolamine transdermal patch. J Emerg Med. 2006;30(3):299-302. PubMed doi:10.1016/j.jemermed.2005.03.018
7. Kventsel I, Berkovitch M, Reiss A, et al. Scopolamine treatment for severe extra-pyramidal signs following organophosphate (chlorpyrifos) ingestion. Clin Toxicol (Phila). 2005;43(7):877-879. PubMed doi:10.1080/15563650500357636
aGreenville Health System, University of South Carolina School of Medicine, Greenville Psychiatry Residency Program, Greenville
bUniversity of South Carolina School of Medicine, Greenville; Medical University of South Carolina, Charleston; Edward Via College of Osteopathic Medicine, Spartanburg; and Patrick B. Harris Psychiatric Hospital, Anderson, South Carolina
Potential conflicts of interest: None.
Funding/support: None.
Published online: June 16, 2016.
Prim Care Companion CNS Disord 2016;18(3):doi:10.4088/PCC.15l01874
© Copyright 2016 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!