Can Primary Care Sleep Medicine Integration Work?

ABSTRACT
Sleep disorders are common in the veteran population. There is an increasing need for sleep medicine services in returning veterans. Primary care providers are uncomfortable diagnosing and treating sleep disorders. Patients often have to wait several days before they can be seen by a sleep clinician. This pilot project evaluated the feasibility of providing sleep medicine services to patients in a primary care setting. Primary care providers were involved in decision-making, resulting in improved satisfaction with sleep medicine services among primary care clinicians.
Prim Care Companion CNS Disord 2014;16(2):doi:10.4088/PCC.13br01593
© Copyright 2014 Physicians Postgraduate Press, Inc.
Submitted: October 6, 2013; accepted December 26, 2013.
Published online: April 24, 2014.
Corresponding author: Imran S. Khawaja, MD, Minnesota Regional Sleep Disorders Center, Hennepin County Medical Center, 701 Park Ave, Minneapolis, MN 55415 ([email protected]).
Sleep disorders are common in the United States, affecting approximately 50-70 million people.1 Sleep problems have a major impact on health, including effects on psychological and cognitive functioning and decreased quality of life.2 Sleep disturbances are extremely common in returning veterans. In one report, 86% of returning soldiers had a sleep disturbance at the time of return that persisted during 45-day follow-up.3 Such disturbances could affect the ability of these individuals to integrate back into their work and family life.
Evidence suggests a role of sleep disturbance in the emergence and worsening of posttraumatic stress disorder.4 One meta-analysis concludes that sleep disturbance is a risk factor for suicidal ideation, suicide attempt, and completed suicide.5
In spite of the prevalence, negative impact on health, and availability of effective treatments, sleep disorders are underdiagnosed and insufficiently treated by health care providers.6 The annual Sleep in America Poll1 notes that 86% of respondents report that their physician has never discussed sleep disturbance with them. In addition, 6 of 10 health care professionals report having insufficient time to discuss sleep issues during clinic appointments.1 In one study, 90% of primary care providers regard their knowledge of sleep disorders as fair to poor.7 There is often a severe delay in diagnosing a sleep disorder by general physicians.8
In a recent study evaluating challenges and performance gaps for general internists providing care to sleep disorder patients, 1 of every 3 providers expressed hesitancy in addressing obstructive sleep apnea and shift work sleep disorder.6 These providers did not generally screen patients for sleep disorders and were reluctant to bring up the topic, which they regarded as too complex to manage in their setting.6 Therefore, Lavie9 proposes collaboration between generalists and sleep specialists to reduce gaps in providers’ knowledge of sleep disturbances. This collaboration is further supported by American Academy of Sleep Medicine guidelines for treatment of obstructive sleep apnea, which recommend a multidisciplinary team mode.10
Because of the difficulty in implementation of a collaborative approach, a pilot project for primary care-sleep medicine integration was established at the Minneapolis Veterans Affairs (VA) Medical Center (Minneapolis, Minnesota) to explore this challenge. Data were collected from July 2012 to August 2012. Human subject approval was not obtained, as this project was part of leadership effectiveness and development training for 2 of the authors (I.S.K. and A.H.). A board-certified sleep physician attended primary care team meetings and spent 2 hours weekly in the primary care clinic in order to respond to informal requests for consultation. Additional telephone and pager availability was offered, and the program was monitored for 2 months.
The authors created a preproject questionnaire to assess primary care providers’ satisfaction with the current sleep medicine services and a postproject questionnaire to assess if the project increased their satisfaction with this model of primary care-sleep medicine integration. The questionnaire was created after consultation with the primary care-mental health integration staff and the mentor of the primary care-sleep medicine integration project (B.C.).
One of our board-certified sleep medicine physicians (I.S.K.) met with a primary care team and described the model in order to obtain a “buy in” for the project. The decision-making process was explained, and a preproject questionnaire was administered anonymously. The questionnaire was left with the primary care staff. The primary care staff completed and returned the questionnaire to the office manager of the clinic, who gave it back to the sleep physician.
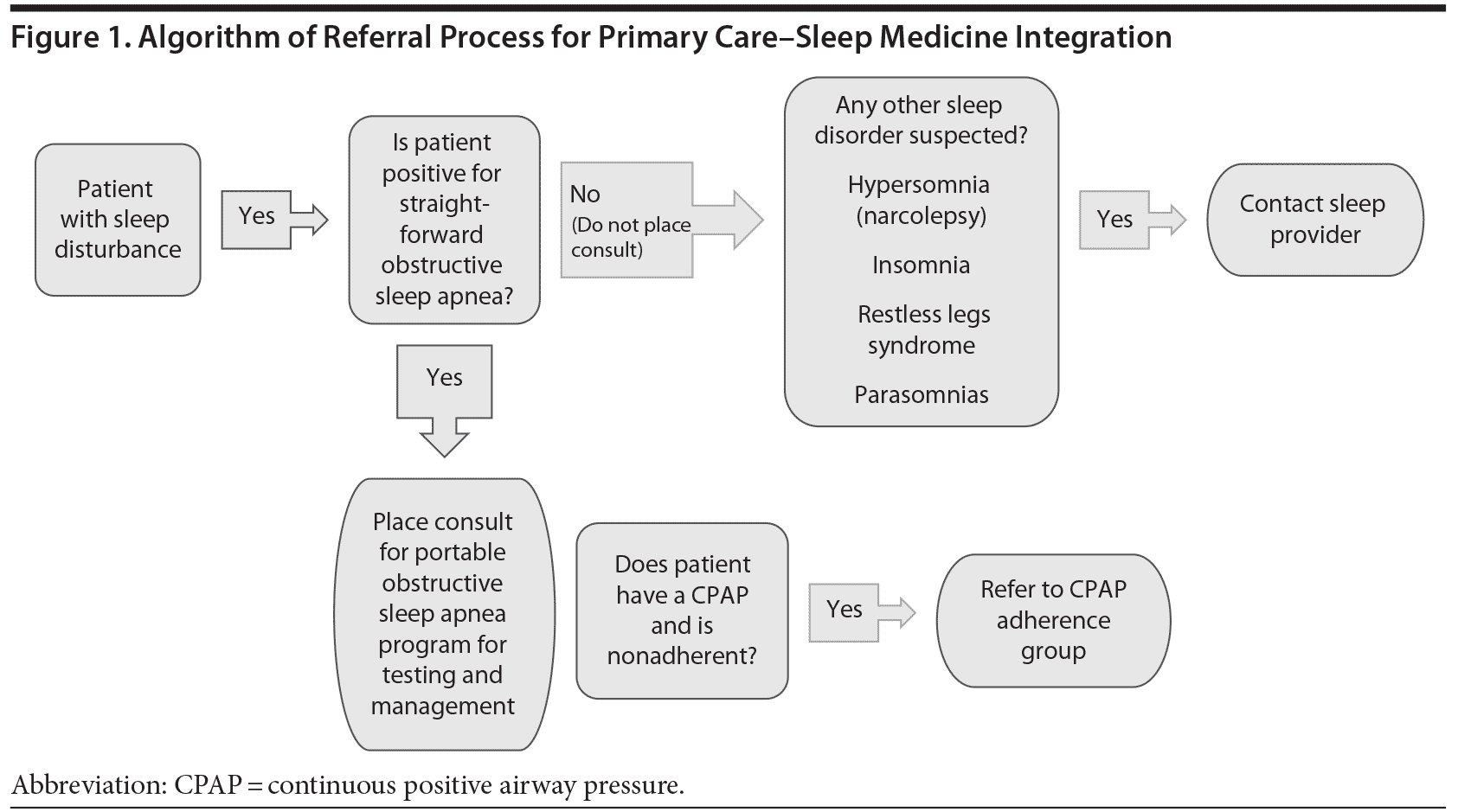
Primary care clinicians were educated about the algorithm for the referral process. If they had a patient with sleep disturbance or complaint, a determination was made as to whether the patient was positive for high probability obstructive sleep apnea. If the patient was high probability for obstructive sleep apnea and did not have any other sleep-related complaints, then he or she was referred to the sleep apnea clinic for portable sleep study. If the patient had obstructive sleep apnea and was not adherent to continuous positive airway pressure (CPAP) therapy, he or she was referred to the CPAP group that was started in concurrence with this pilot project. If the patient had sleep-related complaints other than obstructive sleep apnea such as excessive daytime sleepiness, restless legs syndrome, insomnia, and parasomnias, the collaborating sleep physician was contacted via telephone, pager, or a note in the patient’s chart. The sleep physician saw the patient in the primary care clinic, talked to the patient on the telephone, or had the patient come to the sleep clinic to be seen as a walk-in patient. The flowchart in Figure 1 describes the decision-making process for referrals.
Our hypotheses were that primary care-sleep medicine integration will (1) decrease the time to complete sleep medicine consultations and (2) increase satisfaction of primary care physicians and staff regarding sleep medicine services provided in a collaborative manner.
Over a 2-month period, a total of 27 patients of the 790 visits to that particular clinic were referred by primary care clinicians. Insomnia was the most common reason for referral to the sleep medicine physician. The mean ± SD age of the patients was 68 ± 14 years, and 99% were men. The percentages of consult resolution were E-consult (advice via electronic records): 7.4%, telephone call to the patient: 48.1%, patients seen in the primary care clinic: 37%, and other: 7%.
Consultation requests were resolved within the same day in more than 90% of cases compared to a mean of 20 days during the 6-month period prior to implementation of the pilot integration project. Primary care clinicians expressed clear appreciation for accessible sleep medicine expertise. The program was regarded as “very helpful” by 54.5% of respondents, and 87.5% reported that it “helped most of [their] patients.” In retrospect, 87.5% of respondents felt “very satisfied” with the novel process when compared with the conventional consultation system prior to this project.
Primary care providers in busy clinical settings typically request sleep medicine consultation without expectation of timely response. The informality of this project enabled the development of a comfortable rapport when the sleep specialist was so easily available. It remains to be seen if the economics of this arrangement can sustain it, but there is no reason that advanced practice providers such as physician assistants and nurse practitioners could not have sufficient training to offer guidance and triage in the primary care setting. Knowledge about sleep disorders is increasing, but there is still need for further education about the impact of sleep disorders on general and psychiatric illnesses.
Primary care clinicians appreciated primary care-sleep medicine integration and cited several reasons for their satisfaction with the process. For example, easy access to a sleep specialist and quick resolution of the consultation were mentioned as the main reasons. In addition, they could obtain a curbside consultation without formally referring the patient.
In our opinion, the availability and personality style of sleep specialists are important, so that the sleep specialist is not “imposing” his or her knowledge on the primary care clinicians but is working in a collaborative fashion. It is also difficult to generalize this model to any clinician or clinic, as the success of such integration depends on personality styles and individual preferences of primary care providers.
Since there is a shortage of sleep physicians in the VA system, utilizing advanced practice providers is a potential option. In addition, advanced practice providers and psychologists working in the primary care mental health program in the VA system could be trained in sleep medicine and could work in this model as well.
Author affiliations: Minnesota Regional Sleep Disorders Center, Hennepin County Medical Center, Minneapolis (Dr Khawaja); Departments of Psychiatry (Drs Khawaja, Thuras, and Hurwitz) and Neurology (Dr Khawaja), University of Minnesota Medical School, Minneapolis; Office of Mental Health, Veterans Integrated Service Network 23 (400 South Clinton, Ste 241, Iowa City, Iowa 52240-4105), and Department of Psychiatry, University of Iowa (Dr Cook), Iowa City; and VA Medical Center, Minneapolis, Minnesota (Mr Herr).
Potential conflicts of interest: None reported.
Funding/support: None reported.
Disclaimer: The views expressed in this article are those of the authors and do not necessarily represent the views of VISN 23, the Minneapolis VA Health Care System, the US Department of Veterans Affairs, the US Government, or the University of Minnesota.
REFERENCES
1. National Sleep Foundation. 2008 Sleep in America Poll. Washington, DC: National Sleep Foundation. http://www.sleepfoundation.org/sites/default/files/2008%20POLL%20SOF.PDF. Accessed July 8, 2009.
2. Banks S, Dinges DF. Behavioral and physiological consequences of sleep restriction. J Clin Sleep Med. 2007;3(5):519-528. PubMed
3. Garner B, Landis CA, Jarrett M, et al. Sleep disturbances in US soldiers returning from wartime deployment: preliminary findings. 24th Annual Meeting of the Associated Professional Sleep Societies; June 6-9, 2010; San Antonio, TX.
4. Wright KM, Britt TW, Bliese PD, et al. Insomnia as predictor versus outcome of PTSD and depression among Iraq combat veterans. J Clin Psychol. 2011;67(12):1240-1258. PubMed doi:10.1002/jclp.20845
5. Pigeon WR, Pinquart M, Conner K. Meta-analysis of sleep disturbance and suicidal thoughts and behaviors. J Clin Psychiatry. 2012;73(9):e1160-e1167. PubMed doi:10.4088/JCP.11r07586
6. Hayes SM, Murray S, Castriotta RJ, et al. (Mis) perceptions and interactions of sleep specialists and generalists: obstacles to referrals to sleep specialists and the multidisciplinary team management of sleep disorders. J Clin Sleep Med. 2012;8(6):633-642. PubMed
7. Papp KK, Penrod CE, Strohl KP. Knowledge and attitudes of primary care physicians toward sleep and sleep disorders. Sleep Breath. 2002;6(3):103-109. PubMed doi:10.1055/s-2002-34317
8. Kryger MH, Walid R, Manfreda J. Diagnoses received by narcolepsy patients in the year prior to diagnosis by a sleep specialist. Sleep. 2002;25(1):36-41. PubMed
9. Lavie P. Sleep medicine: time for a change. J Clin Sleep Med. 2006;2(2):207-211. PubMed
10. Epstein LJ, Kristo D, Strollo PJ Jr, et al; Adult Obstructive Sleep Apnea Task Force of the American Academy of Sleep Medicine. Clinical guideline for the evaluation, management and long-term care of obstructive sleep apnea in adults. J Clin Sleep Med. 2009;5(3):263-276. PubMed