Bipolar disorder (BD) is a devastating, chronic psychiatric illness. It adversely affects patients’ quality of life by impairing physical and psychological health and social relationships.1 Studies on the pathogenesis of psychiatric diseases have recently explored the role of inflammation, diet, gut microbiome, and epigenetic alterations.2
Ulcerative colitis (UC) is an inflammatory bowel disease. It is hypothesized that an inflammatory gut causes a higher prevalence of psychiatric illness.3 Inflammatory mechanisms are involved in UC and BD, and psychiatric comorbidity in UC increases morbidity and deteriorates the quality of life by increasing relapses and treatment nonresponsiveness.4,5 However, the link between UC and BD is inadequately explored.
Methods
For this study, we followed recommended methodology and used weighted National Inpatient Sample (NIS) data and complex sample designs/modules for analyses considering strata and clusters.6 We used the NIS data for all young adults admitted with a diagnosis of BD between October 2015 and December 2017.
Results
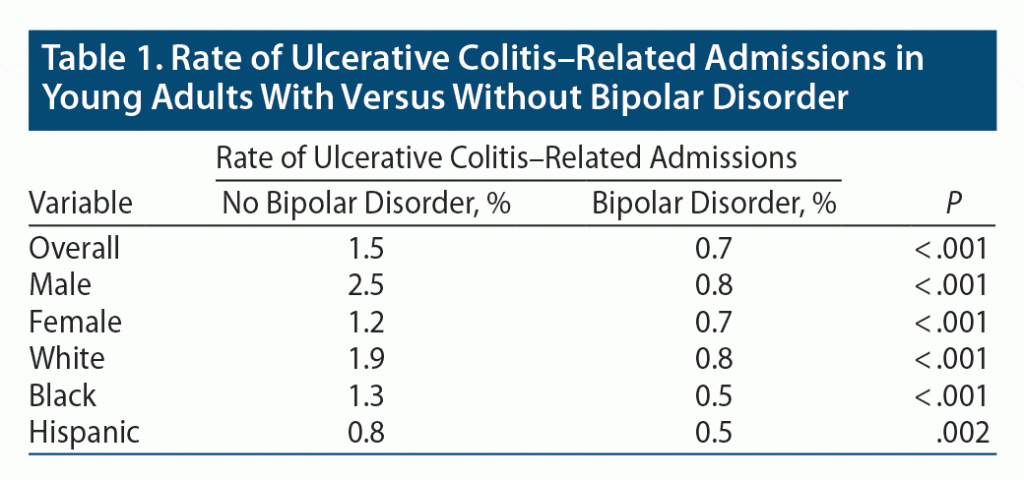
Among patients admitted with the diagnosis of BD spectrum (n = 294,640), only 0.2% (n = 595) of the patients had UC. Next, we compared the demographic characteristics of UC patients (Table 1) with and without BD. The overall prevalence of UC was less (0.7%) among patients with BD compared to those without BD (1.5%) (odds ratio [OR]: 0.47, 95% CI, 0.39–0.56). This inverse relationship persisted across all races and gender.
Further, we employed multivariable regression analysis with UC as an outcome and sociodemographic and hospital characteristics as covariates. In the multivariable analysis, the association between BD and UC remained significant (OR: 0.39, 95% CI, 0.33–0.48). The findings from our study are contrary to what we expected based on prior studies2,4 and inflammatory pathogenesis. No previous studies showed an inverse relationship between BD and UC.
Discussion
Since inflammatory mechanisms are involved in UC and BD, the findings from our analysis are counterintuitive.2,4 Our research employed a large sample size with US national population representation covering much of the US inpatient admissions. A few studies2,4 have shown a positive association between inflammatory bowel disease and major depressive disorder, BD, and anxiety. Factors like brain-gut axis interactions, immunologic disturbances, oxidative stress, and vagus nerve dysfunction can cause inflammatory bowel disease and mental disorders.5
The results of our study are surprising but worthy of further research. Our findings are noteworthy for the vast sample size and geographic representation across the US. One explanation for the inverse relationship found in our study could be a prolonged incubation of both UC and BD development after the onset of inflammation. Our analysis included a young adult population. Another possible explanation for our findings could be a dose-response relationship between inflammation and the development of UC/BD. Unfortunately, our dataset could not ascertain information about the inflammatory markers in UC and BD. Another explanation for the reciprocal relationship between UC and BD could be the use of anti-inflammatory agents in UC patients. Also, it is possible that treatment of BD could influence inflammatory markers and hence UC symptoms. The role of a missing intermediate factor that inflammation modifies differently in BD and UC is another possibility. However, NIS data pertain only to the inpatient population. Our study findings require further exploration of this relationship.
Article Information
Published Online: August 10, 2023. https://doi.org/10.4088/PCC.22br03357
© 2023 Physicians Postgraduate Press, Inc.
Submitted: July 4, 2022; accepted November 22, 2022.
To Cite: Rizvi A, Ashraf S, Desai R, et al. A study of the association of ulcerative colitis and bipolar disorder in an inpatient population. Prim Care Companion CNS Disord. 2023;25(4):22br03357.
Author Affiliations: Texas Tech University Health Science Center at Odessa/Permian Basin Odessa, Midland (Rizvi, Ashraf, Desai, Trivedi, Jain); Boston Children’s Hospital/Harvard Medical School, Boston, Massachusetts (Mansuri).
Corresponding Author: Sahar Ashraf, MD, Texas Tech University Health Sciences Center, Permian Basin, 3600N Garfield St, Mildand, TX 79705 ([email protected]).
Author Contributions: Drs Rizvi and Ashraf share equal credentials for the first authorship. Drs Jain and Mansuri share equal credentials for senior authorship.
Relevant Financial Relationships: None.
Funding source/support: None.
References (6)

- Islam MK, Islam MS, Kibria SM, et al. Quality of life among patients with bipolar disorder. Mymensingh Med J. 2020;29(3):601–608. PubMed
- Alam R, Abdolmaleky HM, Zhou JR. Microbiome, inflammation, epigenetic alterations, and mental diseases. Am J Med Genet B Neuropsychiatr Genet. 2017;174(6):651–660. PubMed
- Lee SH, Kwon JE, Cho ML. Immunological pathogenesis of inflammatory bowel disease. Intest Res. 2018;16(1):26–42. PubMed CrossRef
- Kao LT, Lin HC, Lee HC. Inflammatory bowel disease and bipolar disorder: a population-based cross-sectional study. J Affect Disord. 2019;247:120–124. PubMed CrossRef
- Nowakowski J, Chrobak AA, Dudek D. Psychiatric illnesses in inflammatory bowel diseases: psychiatric comorbidity and biological underpinnings. Psychiatr Pol. 2016;50(6):1157–1166. PubMed CrossRef
- Agency for Healthcare Research and Quality. Healthcare cost and Utilization Project: User Support. AHRQ website. Accessed May 5, 2023. https://www.hcup-us.ahrq.gov/db/nation/nis/nischecklist.jsp
Enjoy this premium PDF as part of your membership benefits!