Successful Electroconvulsive Therapy in a Young Woman With Chronic Catatonia
To the Editor: Catatonia is a motor dysregulation syndrome with multiple etiologies and is associated with a variety of neurologic disorders, general medical conditions, and reactions to medications.1-3 Recent studies suggest that catatonia should be conceptualized as an independent syndrome, which facilitates accurate diagnosis and appropriate anticatatonic treatments.2 Catatonia typically responds to anticonvulsants, mainly benzodiazepines, and electroconvulsive therapy (ECT).2 However, the therapeutic value of benzodiazepines and ECT in chronic catatonia is less well established.4 Only 20% to 30% of schizophrenic patients with catatonic symptoms respond to benzodiazepines. Thus, identifying those patients with potentially reversible symptoms is important.
Here, we report the case of a patient with chronic catatonia who presented with a chronic fluctuating course of idiopathic catatonia and responded well to subsequent ECT.
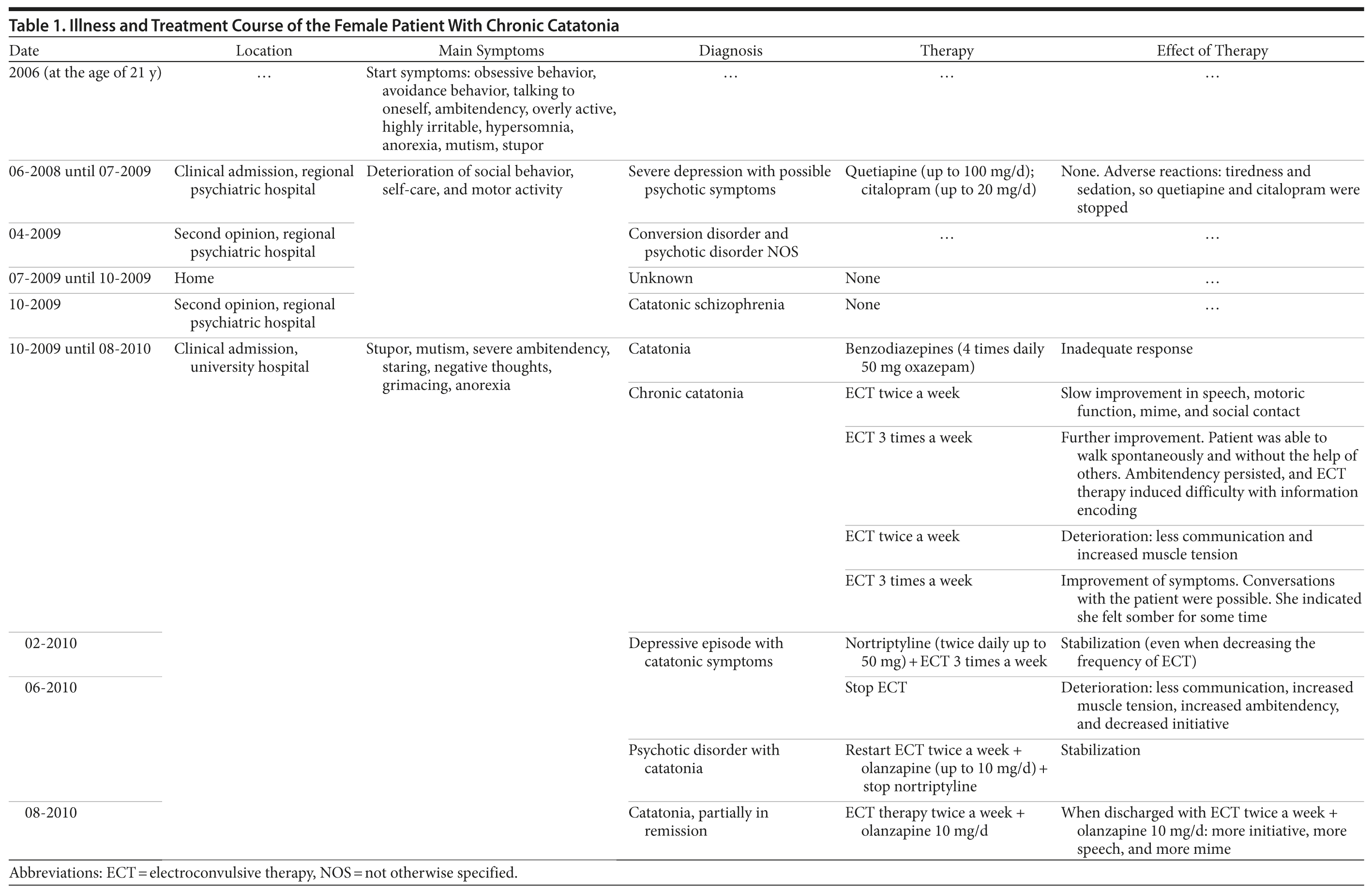
Case report. Ms A, a 25-year-old Dutch woman, was admitted to our clinic due to the uncertainty of the diagnosis and to exclude a somatic origin of symptoms. She was initially diagnosed with DSM-IV major depressive disorder with psychotic symptoms at age 22 years and over time had been prescribed quetiapine, initially 100 mg/d and subsequently 50 mg/d for 11 days, at which time she was switched to citalopram 20 mg/d and subsequently 10 mg/d for 6 months (Table 1). Meanwhile, at another psychiatric hospital, a diagnosis of conversion disorder was suggested, with psychotic disorder as a possible differential diagnosis.

When she was presented to our unit in October 2009, the patient was mute and displayed posturing, rigidity, staring, severe ambitendency, withdrawal, negative thoughts, and frequent grimacing. She ate and drank only modestly, with much support. Furthermore, the pattern of symptoms was extremely fluctuating.
Physical examination revealed cogwheel rigidity of the arms and emerging contractures of the hands, as well as increased reflexes of the arms and legs. Furthermore, there was an occurrence of waxy flexibility as well as acrocyanosis with a slow capillary refill of the toes, interpreted as venous stasis with immobility. A duplex ultrasound examination excluded circulatory stenosis or arterial anomalies and a rheumatoid origin of symptoms. Neurologic and internal examinations excluded a potential somatic origin of the disorder.
A few days after admission, due to the suspected catatonia, treatment with oxazepam 50 mg 4 times daily was commenced. After 4 weeks of clinical observation, the diagnosis of chronic catatonia was established and ECT treatment was started due to an inadequate response to the benzodiazepine treatment. Initially, ECT treatment was bilateral, twice a week (Thymatron System IV, Somatics, LLC, Lake Bluff, Illinois; bilateral, impulse width 0.5 msec, energy set first 53 treatments 5% to 100% and second 15 treatments 5% to 35%, adequate seizure duration > 20 sec EMG).
The patient showed slow, but gradual, improvements in speech, motoric function, mime, and social contact. The frequency of ECT treatments was therefore increased to 3 times a week, producing further improvements. Because ECT induced severe difficulty with information encoding, the frequency of ECT was, after 25 bilateral ECT treatment sessions, reduced to twice a week. The patient responded with a deterioration of symptoms such as less communication and increased muscle tension. Therefore, after 3 weeks the frequency of ECT was reinstated to 3 times a week, resulting in symptom improvement. Clinical symptoms improved significantly with ECT, and activities of daily routine improved steadily. However, when ECT was fully stopped in June 2010, symptoms deteriorated again, with the patient showing less communication, increased muscle tension, increased ambitendency, and decreased initiative. Meanwhile, a psychotic disorder with catatonia or catatonic schizophrenia was considered, and ECT was restarted twice a week along with the addition of olanzapine (up to 10 mg/d). With this treatment, she was able to speak in whole sentences, started to walk spontaneously, and showed more initiative and less ambitendency.
In August 2010, the clinical symptoms improved gradually and she was discharged with a prescription of olanzapine 10 mg/d and ECT twice a week. Between January and June 2011, the patient was further followed at the outpatient clinic of a regional hospital.
To the best of our knowledge, this unique case showed that, despite an insidious onset and an atypical, fluctuating course of catatonic symptoms, the diagnosis of catatonia should be considered and, as in acute catatonia, ECT can be effective in chronic catatonia. Studies of more patients with similar presentation are needed to develop an empirically based treatment approach.
References
1. Fink M. Delirious mania. Bipolar Disord. 1999;1(1):54-60. PubMed doi:10.1034/j.1399-5618.1999.10112.x
2. Fink M, Taylor MA. Catatonia: A Clinician’s Guide to Diagnosis and Treatment. Cambridge, UK: Cambridge University Press; 2003. doi:10.1017/CBO9780511543777
3. Fink M, Taylor MA. The catatonia syndrome: forgotten but not gone. Arch Gen Psychiatry. 2009;66(11):1173-1177. PubMed doi:10.1001/archgenpsychiatry.2009.141
4. Gibson RC, Walcott G. Benzodiazepines for catatonia in people with schizophrenia and other serious mental illnesses. Cochrane Database Syst Rev. 2008;8(4):CD006570. PubMed
Author affiliations: Department of Psychiatry and Rudolf Magnus Institute of Neuroscience, University Medical Center, Utrecht, The Netherlands.
Potential conflicts of interest: None reported.
Funding/support: None reported.
Published online: June 21, 2012.
Prim Care Companion CNS Disord 2012;14(3):doi:10.4088/PCC.11l01328
© Copyright 2012 Physicians Postgraduate Press, Inc.