ABSTRACT
Stroke is the second most common cause of death worldwide. It is a medical emergency demanding immediate recognition to provide time-sensitive acute management. The coronavirus disease 2019 (COVID-19) pandemic has challenged acute stroke care, and alternate models of treatment are needed. Telestroke is well proven as a valid tool for acute stroke assessment and has been utilized successfully to manage patients remotely in many parts of the world, though it is underutilized in the Middle East and North Africa region. Given the challenges associated with the COVID-19 pandemic, such as risk of physician exposure to infection, implementation of a telestroke system is critical to provide consultant stroke physician coverage. This article provides a proposed model for coordinated telestroke. Implementation of telestroke in the Middle East and North Africa region and other underdeveloped areas will optimize stroke management, especially during the COVID-19 era.
Prim Care Companion CNS Disord 2021;23(5):21nr02919
To cite: Shahid R, Al-Jehani HM, Zafar A, et al. The emerging role of telestroke in the Middle East and North Africa region in the era of COVID-19. Prim Care Companion CNS Disord. 2021;23(5):21nr02919.
To share: https://doi.org/10.4088/PCC.21nr02919
© Copyright 2021 Physicians Postgraduate Press, Inc.
aDepartment of Neurology, College of Medicine, King Fahad University Hospital, Imam Abdulrahman bin Faisal University, Alkhobar, Saudi Arabia
bDepartment of Neurosurgery, Critical Care Medics and Radiology, King Fahad University Hospital, Imam Abdulrahman bin Faisal University, Alkhobar, Saudi Arabia
cDepartment of Neurology and Neurosurgery, Montreal Neurological Institute and Hospital, McGill University, Montreal, Quebec, Canada
dDepartment of Medicine and Neurology, University of Alberta, Edmonton, Alberta, Canada
eHamad General Hospital, Doha, Qatar
*Corresponding author: Rizwana Shahid, MBBS, FCPS, Department of Neurology, College of Medicine, Imam Abdulrahman bin Faisal University, King Fahad University Hospital, PO Box 1982, Dammam, 31952, Saudi Arabia ([email protected]).
Stroke is a common neurologic emergency and remains a major cause of short- and long-term disability.1 As per 2019 statistics from the American Heart Association,2 1 in 6 people in their lifetime are affected by stroke worldwide and more than 13.7 million people have a stroke each year, resulting in 5.8 million deaths per year secondary to stroke.
Although there has been a decline in stroke incidence in the developed world, the Middle East and North Africa region (MENA), comprising 23 countries, has observed an increase. Differences in prevalence of risk factors and strategies to prevent and treat stroke could be potential reasons for this discrepancy.3
Advancements in stroke management and prevention strategies have been made in the past few years, including intravenous thrombolysis and mechanical thrombectomy, but these interventions are highly time dependent. Timely management of acute ischemic stroke has a great effect on the survival and prognosis of such patients, and the extended time window to manage acute stroke of up to 24 hours has enabled stroke physicians to treat a greater number of patients than in the past.4 However, the provision of acute stroke care has been put to the test during the coronavirus disease 2019 (COVID-19) outbreak. Since its emergence in December 2019 in China, the virus has rapidly evolved into a global pandemic, crippling health care services around the world.
Management of a patient with acute stroke from the emergency department (ED) to intravenous thrombolysis and then mechanical thrombectomy in the stroke unit to rehabilitation is more challenging during the COVID-19 pandemic.5,6 The challenges could stem from suboptimal care due to lack of medical staff, possibly due to infection; a conservative approach due to high risk of infection; deferral of medical resources to fight the pandemic; and patient deferral to come to the ED or seek medical attention.7,8 Therefore, the development of urgent stroke protocols or novel methods of stroke management such as telestroke is critical during the era of COVID-19.9–12
Telestroke has been utilized as a successful tool in the stroke clinic and in the acute stroke setting.13 It is well proven as a valid tool for acute stroke assessment based on American Heart Association guidelines.2 Telestroke has played a critical role during the COVID-19 pandemic by providing stroke consultation coverage to different areas (ie, in the same hospital, a different hospital, or other parts of the world) and thus decreasing the chance of physicians being infected.
Major developments in the field of telemedicine have taken place at a rapid pace during the COVID-19 crisis.14 Telemedicine, by virtue of minimizing travel and reducing physical contact, provides a pragmatic advantage by avoiding in-person consultation of patients while providing access to both primary and specialist care. Electronic consultations (e-consults) thereby greatly assist in delivery of outpatient health care without compromising the benefits of specialty expertise, which can be made readily available to many patients.15
Of note, the concept of telemedicine is either direct contact of the physician with the patient or indirect contact in remote areas where subspecialty consultants are unavailable through the paramedical staff or ED physician for expert opinion. As stroke is a highly specialized field and requires immediate management, usual consultation occurs between the ED or general neurologist working in a primary health care setting or remote area where there is a shortage or unavailability of stroke physicians and the stroke neurologist working in a tertiary care center.
Epidemiology of Stroke and COVID-19 in the Middle East
During the COVID-19 pandemic, it has been observed that infected patients may have varied presentations, including neurologic manifestations, that are either coincident or might potentially precede fever and other pulmonary symptoms of the disease. Two retrospective case series16,17 from 3 hospitals in Wuhan, China reported that up to 36% of COVID-19 patients manifest neurologic symptoms, and of these, 5.7% with severe COVID-19 infection suffered from acute cerebrovascular disease.
According to 1 study,18 an estimated 5.9% of COVID-19 patients developed stroke at a median duration of 10 days after COVID-19 infection. Patients who developed stroke with COVID-19 were older and had more vascular risk factors and more severe pneumonia. Different mechanisms of stroke in these patients could include critical illness–induced hypercoagulability and cardiac embolism from virus-related cardiac injury.18 However, the study18 has several limitations, as these data were collected in the early phase of the pandemic and thus are preliminary, retrospective in nature, and incomplete.
Impact of COVID-19 on Stroke Management in the MENA Region
Some of the challenges related to stroke management during the COVID-19 pandemic are as follows:
- Lack of transient ischemic attack and minor stroke evaluation due to patients’ fear of catching the virus;
- Difficulty obtaining screening history in stroke patients (aphasic, drop in level of consciousness, or multiple cultures and different languages);
- Medical staff shortage due to infection or relocation due to outbreak;
- Reluctance of medical staff to treat with endovascular treatment or other invasive procedures;
- Difficulty encountered by stroke team to respond to acute stroke call due to shortage of personal protective equipment (PPE); and
- Inability to accommodate stroke patients in the ED or intensive care unit due to COVID-19.
Role of Telestroke in the Middle East
In telestroke, also called stroke telemedicine, doctors who have advanced training in stroke management can use technology to treat patients in other locations who have had strokes.
The concept of telestroke is not new. In 1999, Levine and Gorman19 introduced the term. Later on, telemedicine was utilized to provide neurologic consultation in areas that lacked stroke specialists.20
During the COVID-19 pandemic, it has become necessary to minimize the number of physicians with direct exposure to infected patients, while at the same time maintaining the standard of quality care. To reduce physical exposure and maintain social distancing as much as possible while continuing to function, private companies and institutions of higher education have made an abrupt transition to remote videoconferencing and other digital technology. However, the health care system is still managing this crisis largely through risky brick-and-mortar visits.
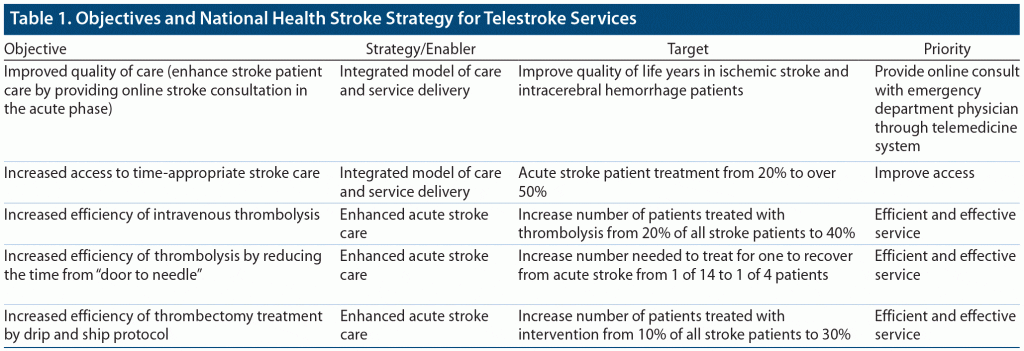
As mentioned previously, telestroke has mainly been used in the past to cover remote areas without access to stroke specialists. But, during the pandemic, stroke teams have had to remain vigilant, as every stroke patient is considered COVID-19 positive. Thus, many hospitals are adopting protected stroke code, as it is important to limit the physical exposure of stroke team members to save man power and PPE. Therefore, there is a need for modified telestroke services wherein only 1 member of the stroke team, after utilizing proper PPE, attends the stroke code, and other members of the team observe through telemedicine. The objectives and national health stroke strategy for telestroke services are provided in Table 1.21
Main Objectives of the Telestroke System
The proposed model is provided in Table 2. The objectives are as follows:
- Provide thrombolysis treatment for the acute stroke patient in the local hospital where it would otherwise be impractical for the patient to be transferred to the stroke center of another hospital;
- Decrease the time from “door to needle” for intravenous thrombolysis, which is one of the most important factors in improving stroke outcome;
- Triage the acute stroke patient for possible intervention (thrombectomy and stenting) by “drip and ship” method (treat the patient with thrombolysis in the peripheral hospital then transfer him/her to the main hospital for possible intervention); and
- The telestroke system should provide 24-hour 7 days/week coverage for evaluation and treatment of acute stroke patients (24-hour window) in 1 of the peripheral hospitals in the MENA region by connecting both the patient and physician through a videoconferencing system with the stroke consultant in the region.
Proposed Model of Coordinated Telestroke in the MENA Region
- Voluntary participation of the ED and stroke physicians in the region;
- Coordination through a reliable, encrypted videoconferencing app;
- On activation of stroke code in the participating center, announcement of the code through the app to alert other stroke physicians;
- History and examination to be described by the primary physician (could be the ED physician or general neurologist);
- Results of brain imaging should be uploaded and indications and contraindications recorded;
- Stroke physicians worldwide can participate in decision-making about intravenous thrombolysis as well as the need for thrombectomy; and
- Patients can be transferred to the nearby stroke center after starting thrombolysis if indicated or only for thrombectomy depending on the scenario.
Key Assumptions
All key assumptions that may affect the eventual success of the telestroke services should be identified. Comments about likely inflation rates in the cost, availability, recruitment time required for manpower, supply chain assumptions, and benefit estimates should be included in this section as well. Key assumptions are described in Table 3.
Risks
The safety of telestroke service has been tested in several studies22,23 and found to be safe. A delay in implementing telestroke services will lead to a delay in delivering appropriate acute stroke care to patients who live in areas far from the main stroke center.
Modified Stroke Code Protocol (partial protected stroke code + telestroke within the hospital premises)
Our hospital in Saudi Arabia has adopted a modified stroke code protocol as follows:
- After arrival of a stroke patient to the ED, a decision to initiate a stroke code will be made by the emergency physician, who has determined the patient is a candidate for acute stroke treatment (recognize stroke signs, symptoms, and time of onset);
- Once the stroke code is activated, one of the senior stroke team members (specialist/senior resident) will attend the stroke code physically after taking proper precautions, as now all stroke codes will be considered protected stroke codes;
- The patient will be examined immediately and transferred for brain imaging;
- The senior team member will connect with the stroke consultant and other stroke team members through the videoconference app system; and
- Other team members will monitor the patient through videoconference, and management will be planned accordingly.
Conclusion
Given that stroke facilities are not adequately staffed due to the lack of stroke consultants in many parts of the Middle East and the challenges associated with COVID-19, there is a dire need for coordination among MENA physicians to overcome these obstacles. As the COVID-19 pandemic is taking a toll on health care systems and resources are limited, and since the safety and efficacy of telestroke services have been evaluated previously, telestroke should be used remotely in the ED to evaluate patients with ischemic stroke. Telestroke can help to combat the challenges posed by reduced manpower due to either infection or physician relocation. It will also help minimize physician exposure to COVID-19, thus preserving the health of health care workers.
Submitted: January 10, 2021; accepted May 14, 2021.
Published online: September 30, 2021.
Potential conflicts of interest: None.
Funding/support: None.
Clinical Points
- Stroke is a medical emergency demanding immediate recognition to provide time-sensitive acute management.
- The coronavirus disease 2019 (COVID-19) pandemic has challenged the acute management of stroke, and alternate models of treatment are needed.
- Telestroke has been utilized successfully to manage patients remotely in many parts of the world and is well proven as a valid tool for acute stroke assessment.
- Implementation of telestroke in the Middle East and North Africa region and other underdeveloped areas will optimize stroke management, especially during the COVID-19 era.
References (23)

- Murray CJ, Lopez AD. Global mortality, disability, and the contribution of risk factors: Global Burden of Disease Study. Lancet. 1997;349(9063):1436–1442. PubMed CrossRef
- Benjamin EJ, Muntner P, Alonso A, et al; American Heart Association Council on Epidemiology and Prevention Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics–2019 update: a report from the American Heart Association. Circulation. 2019;139(10):e56–e528. PubMed CrossRef
- LJ Streletz, A Mushtak, H Gad, S Abbasi, DM Dimassi, N Akhtar, et al. Epidemiology of stroke in the MENA region: a systematic review. International Journal of Neurology and Neurological Disorders. 2017;1(1): 10–21.
- Katz JM. Latest advances in the treatment of acute stroke. US Neurol. 2018;14(2):80–81. CrossRef
- Abdullah HMA, Haq I, Lamfers R. Cardiac arrest in a young healthy male patient secondary to kratom ingestion: is this ‘legal high’ substance more dangerous than initially thought? BMJ Case Rep. 2019;12(7):e229778. PubMed CrossRef
- Aggarwal G, Lippi G, Michael Henry B. Cerebrovascular disease is associated with an increased disease severity in patients with coronavirus disease 2019 (COVID-19): a pooled analysis of published literature. Int J Stroke. 2020;15(4):385–389. PubMed CrossRef
- Morelli N, Rota E, Terracciano C, et al. The baffling case of ischemic stroke disappearance from the casualty department in the COVID-19 era. Eur Neurol. 2020;83(2):213–215. PubMed CrossRef
- Zhao J, Rudd A, Liu R. Challenges and potential solutions of stroke care during the coronavirus disease 2019 (COVID-19) outbreak. Stroke. 2020;51(5):1356–1357. PubMed CrossRef
- Khosravani H, Rajendram P, Notario L, et al. Protected code stroke: hyperacute stroke management during the coronavirus disease 2019 (COVID-19) pandemic. Stroke. 2020;51(6):1891–1895. PubMed CrossRef
- Fraser JF, Arthur AS, Chen M, et al. Society of Neurointerventional surgery recommendations for the care of emergent neurointerventional patients in the setting of COVID-19. J Neurointerv Surg. 2020;12(6):539–541. PubMed CrossRef
- Baracchini C, Pieroni A, Viaro F, et al. Acute stroke management pathway during coronavirus-19 pandemic. Neurol Sci. 2020;41(5):1003–1005. PubMed CrossRef
- Flexman AM, Abcejo AS, Avitsian R, et al. Neuroanesthesia practice during the COVID-19 pandemic: recommendations from Society for Neuroscience in Anesthesiology and Critical Care (SNACC). J Neurosurg Anesthesiol. 2020;32(3):202–209. PubMed CrossRef
- Johansson T, Wild C. Telemedicine in acute stroke management: systematic review. Int J Technol Assess Health Care. 2010;26(2):149–155. PubMed CrossRef
- Bloem BR, Dorsey ER, Okun MS. The coronavirus disease 2019 crisis as catalyst for telemedicine for chronic neurological disorders. JAMA Neurol. 2020;77(8):927–928. PubMed CrossRef
- Ahmed S, Kelly YP, Behera TR, et al. Utility, appropriateness, and content of electronic consultations across medical subspecialties. Ann Intern Med. 2020;172(10):641–647. PubMed CrossRef
- Mao L, Wang M, Chen S, et al. Neurologic manifestations of hospitalized patients with coronavirus disease 2019 in Wuhan, China. JAMA Neurol. 2020;77(6):683–690. PubMed CrossRef
- Li Y, Li M, Wang M, et al. Acute cerebrovascular disease following COVID-19: a single center, retrospective, observational study. Stroke Vasc Neurol. 2020;5(3):279–284. PubMed CrossRef
- Guo T, Fan Y, Chen M, et al. Cardiovascular implications of fatal outcomes of patients with coronavirus disease 2019 (COVID-19). JAMA Cardiol. 2020;5(7):811–818. PubMed CrossRef
- Levine SR, Gorman M. “Telestroke”: the application of telemedicine for stroke. Stroke. 1999;30(2):464–469. PubMed CrossRef
- Audebert H. Telestroke: effective networking. Lancet Neurol. 2006;5(3):279–282. PubMed CrossRef
- Meyer D, Meyer BC, Rapp KS, et al. A stroke care model at an academic, comprehensive stroke center during the 2020 COVID-19 pandemic. J Stroke Cerebrovasc Dis. 2020;29(8):104927. PubMed CrossRef
- Zajtchuk R, Gilbert GR. Telemedicine: a new dimension in the practice of medicine. Dis Mon. 1999;45(6):197–262. PubMed CrossRef
- Audebert HJ, Kukla C, Clarmann von Claranau S, et al; TEMPiS Group. Telemedicine for safe and extended use of thrombolysis in stroke: the Telemedic Pilot Project for Integrative Stroke Care (TEMPiS) in Bavaria. Stroke. 2005;36(2):287–291. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!