Rapid Transition to Telehealth in a Community Mental Health Service Provider During the COVID-19 Pandemic
Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is a novel coronavirus causing the clinical syndrome of coronavirus disease 2019 (COVID-19), which can lead to significant morbidity and mortality, especially in those with elevated risk or preexisting conditions.1,2 Individuals with serious mental illnesses (SMI) (eg, schizophrenia, schizoaffective disorder, major depressive disorder) have high rates of comorbid cardiopulmonary and medical conditions3,4 that put them at higher risk for developing serious illness with COVID-19. In Michigan, executive orders established policies requiring all Michigan residents to stay at home and adhere to social distancing guidelines and temporarily limited all gatherings and activities deemed unnecessary to sustain life from March 13, 2020-May 28, 2020. As a result, many behavioral health care organizations within Michigan rapidly moved services for those with SMI to telehealth when possible. This transition has been facilitated by changes in payment methods.5 Accordingly, the Michigan Department of Health and Human Services revised place-of-service requirements, significantly expanding allowable services to be delivered via telehealth under a COVID-19 telehealth exception, effective March 1, 2020.
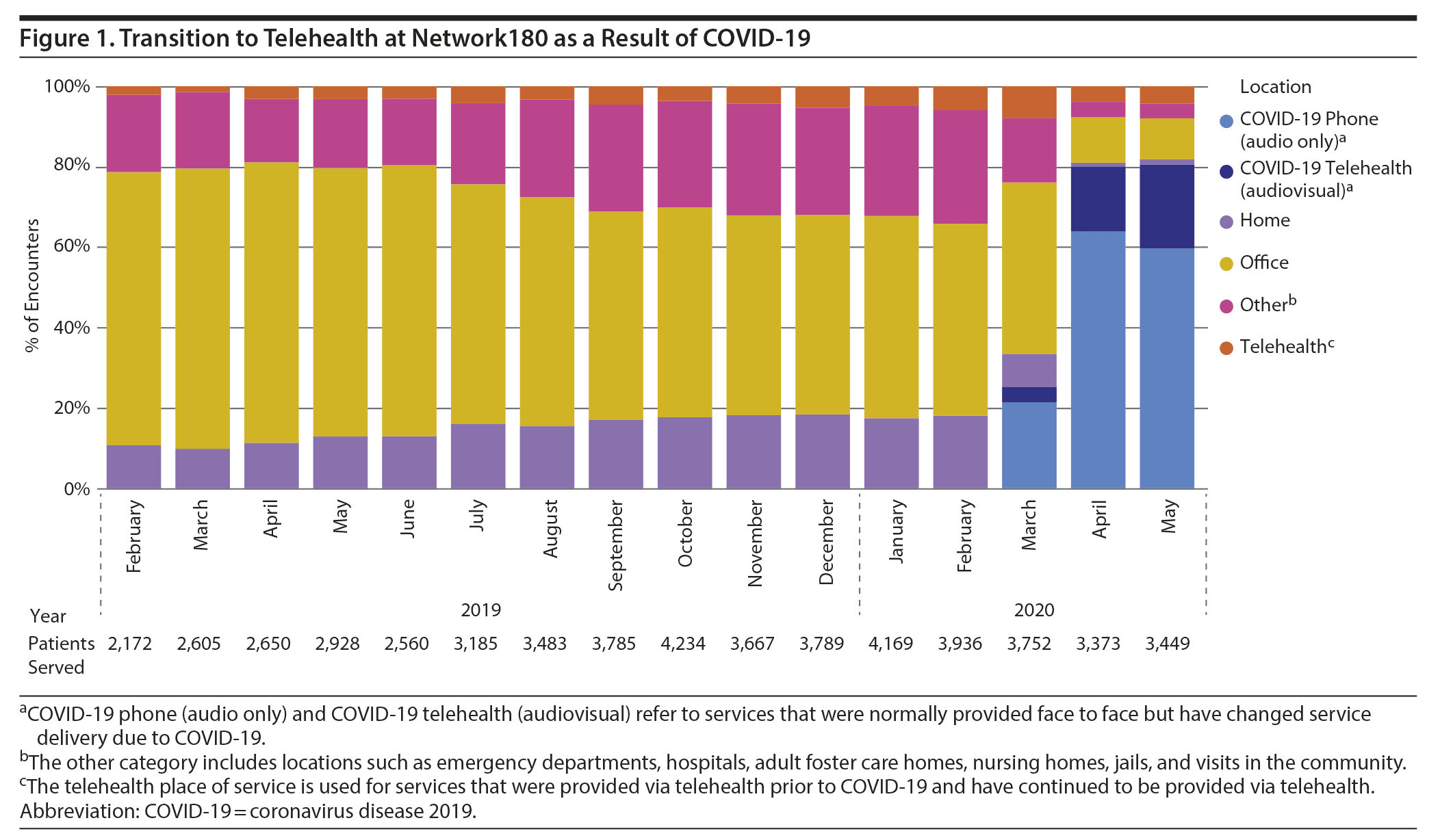
Herein, we describe the transition from in-person to telehealth interventions at Network180, a community mental health (CMH) authority in Kent County, Michigan, which is home to approximately 655,000 people.6 As a CMH, Network180 manages behavioral health care needs for approximately 16,000 patients annually. Half receive services provided directly by Network180 staff, and the remaining patients receive services through a provider network. In Kent County, the first confirmed COVID-19 case was identified on March 1, 2020, and as of July 31, 2020, there were 6,426 cases and 149 COVID-19-related deaths.7
Methods
As Network180 sought to understand the transition to telehealth, a multipart ongoing report was developed to monitor service delivery. The data were sourced from an internal service activity log, which captured all billable services performed by Network180 clinicians. Analyses compared telehealth use prior to COVID-19 (October 1, 2019-February 28, 2020) with telehealth use during COVID-19 (April 1, 2020-May 31, 2020). Data for March 1, 2020-March 31, 2020 are available but considered separately as the transition time from normal operations to COVID-19 operations.
Results
Prior to COVID-19, Network180 served an average of 2,390 patients/month. During the COVID-19 crisis, Network180 served an average of 1,921 patients/month; this decrease was noted most significantly in crisis services (averaging 822 patients/month before COVID-19 and 640 patients/month during COVID-19). Overall, telehealth increased from 5% of all services prior to COVID-19 to 84% of all services during COVID-19 (Figure 1). The majority of services provided via telehealth were audio only (versus audiovisual), with a ratio of 1.9:1 for crisis services and 4:1 for noncrisis services.
Discussion
The transition to telehealth for those with SMI has been rapid in the CMH system in Michigan. Other behavioral health care organizations have also adapted to providing care in this manner.8,9 This transition has provided an important tool for clinicians to minimize the risk of spreading COVID-19 while still providing critical services to those with SMI who are at elevated risk not only for serious illness with COVID-19, but also for developing worsened symptoms of their underlying mental illnesses due to the strain of necessary public health pandemic management strategies like social distancing. The rapid broadening of telehealth codes allowed provision of mental health care to those most at risk. On June 24, 2020, Michigan governor Gretchen Whitmer signed legislation (HB5412-5416) mandating Medicaid and private insurers to continue to cover telehealth visits even after the COVID-19 crisis subsided. This practice could help address disparities in access to care for many of those with SMI who face barriers (eg, lack of transportation, physical limitations) to in-person visits.10
Conclusion
The expansion of telehealth has provided a needed alternate method for delivering behavioral health care to those with SMI during the COVID-19 pandemic and may enhance access to care post pandemic.
Received: August 11, 2020.
Published online: October 1, 2020.
Author contributions: Conceptualization and design of the study: Dr Achtyes and Mss Kopec, Spykerman, and Ryskamp. Data analysis: Ms Kopec. Drafting of the first version of the manuscript: Drs Achtyes and Janney, Mss Kopec and Spykerman, and Mr Johnson. Revision and approval of the final version of the manuscript: all authors.
Potential conflicts of interest: Dr Achtyes has served on advisory boards for Alkermes, Janssen, Lundbeck/Otsuka, Roche, and Sunovion and has received research support from Alkermes, Astellas, Biogen, Boehringer-Ingelheim, InnateVR, Janssen, National Network of Depression Centers, Neurocrine Biosciences, Novartis, Otsuka, Pear Therapeutics, and Takeda. Dr Janney; Mss Kopec, Spykerman, and Ryskamp; and Mr Johnson report no conflicts of interest related to the subject of this report.
Funding/support: None.
Acknowledgments: The authors thank William Ward, MPA, executive director of Network180, for authorizing these analyses, as well as all the clinicians and staff members of Network180 who worked so diligently to convert in-person assessments to telehealth during the COVID-19 pandemic. Mr Ward reports no conflicts of interest related to the subject of this report.
REFERENCES
1.Richardson S, Hirsch JS, Narasimhan M, et al; and the Northwell COVID-19 Research Consortium. Presenting characteristics, comorbidities, and outcomes among 5700 patients hospitalized with COVID-19 in the New York City area. JAMA. 2020;323(20):2052-2059. PubMed CrossRef
2.Zheng Z, Peng F, Xu B, et al. Risk factors of critical & mortal COVID-19 cases: a systematic literature review and meta-analysis. J Infect. 2020;81(2):e16-e25. PubMed CrossRef
3.Janssen EM, McGinty EE, Azrin ST, et al. Review of the evidence: prevalence of medical conditions in the United States population with serious mental illness. Gen Hosp Psychiatry. 2015;37(3):199-222. PubMed CrossRef
4.Bahorik AL, Satre DD, Kline-Simon AH, et al. Serious mental illness and medical comorbidities: findings from an integrated health care system. J Psychosom Res. 2017;100:35-45. PubMed CrossRef
5.Zhao M, Hamadi H, Haley DR, et al. Telehealth: advances in alternative payment models [published online ahead of print February 26, 2020]. Telemed J E Health. 2020;tmj.2019.0294. PubMed CrossRef
6.QuickFacts: Kent County, Michigan. United States Census Bureau website. https://www.census.gov/quickfacts/fact/table/kentcountymichigan. Accessed September 15, 2020.
7.Search accessKent.com. accessKent, Kent County, Michigan website. https://www.accesskent.com/Health/covid-19-data.htm. Accessed September 15, 2020.
8.Kannarkat JT, Smith NN, McLeod-Bryant SA. Mobilization of telepsychiatry in response to COVID-19—moving toward 21st century access to care. Adm Policy Ment Health. 2020;47(4):489-491. PubMed CrossRef
9.Taylor CB, Fitzsimmons-Craft EE, Graham AK. Digital technology can revolutionize mental health services delivery: the COVID-19 crisis as a catalyst for change. Int J Eat Disord. 2020;53(7):1155-1157. PubMed CrossRef
10.Smith TE, Easter A, Pollock M, et al. Disengagement from care: perspectives of individuals with serious mental illness and of service providers. Psychiatr Serv. 2013;64(8):770-775. PubMed CrossRef
aNetwork180, Grand Rapids, Michigan
bDivision of Psychiatry & Behavioral Medicine, Michigan State University College of Human Medicine, Grand Rapids, Michigan
cPine Rest Christian Mental Health Services, Grand Rapids, Michigan
dMichigan State University College of Human Medicine, Grand Rapids, Michigan
*Corresponding author: Eric D. Achtyes, MD, MS, Network180, 790 Fuller Ave, Grand Rapids, MI 49503 ([email protected]).
Prim Care Companion CNS Disord 2020;22(5):20br02787
To cite: Kopec K, Janney CA, Johnson B, et al. Rapid transition to telehealth in a community mental health service provider during the COVID-19 pandemic. Prim Care Companion CNS Disord. 2020;22(5):20br02787.
To share: https://doi.org/10.4088/PCC.20br02787
© Copyright 2020 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!