The Clinical Management of Bipolar Disorder: A Review of Evidence-Based Guidelines
Objective: To discuss the criteria used to diagnose the mood episodes that constitute bipolar disorder, the approach to the differential diagnosis of these presentations, and the evidence-based treatments that are currently available.
Data Sources: A search for evidence-based guidelines for the diagnosis and treatment of adults with bipolar disorder was performed on May 5, 2010, using the National Guideline Clearinghouse database, the Agency for Healthcare Research and Quality Evidence Reports database, and the Cochrane Database of Systematic Reviews. In addition, a clinical query of the PubMed database (completed March 1, 2010) and searches of drug manufacturers’ Web sites (for unpublished trials) were performed to identify randomized, controlled trials and meta-analyses evaluating strategies to treat resistant depression.
Study Selection: Guidelines were selected based on data from randomized, controlled trials; meta-analyses; and well-conducted naturalistic trials that were published since 2005.
Data Extraction: Four evidence-based treatment guidelines for bipolar disorder were included. Three were published in 2009: those put forth as part of an Australian project, those of the British Association for Psychopharmacology, and those produced by the International Society for Bipolar Disorders and the Canadian Network for Mood and Anxiety Treatments. The most recent US guidelines are that of the Texas Implementation of Medication Algorithms project, last updated in 2005.
Data Synthesis: Recommendations from all 4 guidelines were reviewed and are presented with a focus on using them to improve clinical care. The recommendations with the most agreement and highest level of clinical evidence were as follows: (1) mania should be treated first-line with lithium, divalproex, or an atypical antipsychotic medication; (2) mixed episodes should be treated first-line with divalproex or an atypical antipsychotic; (3) bipolar depression should be treated with quetiapine, olanzapine/fluoxetine combination, or lamotrigine; and (4) all patients should be offered group or individual psychoeducation. Additionally, recommendations for therapeutic drug monitoring are presented due to their importance for patient safety, particularly for the primary care physician, although these are based on consensus guidelines.
Conclusions: Bipolar disorder is a lifelong illness that is complicated by high comorbidity and risk of poor health outcomes, making the primary care physician’s role vital in improving patient quality of life. The management of acute mood episodes should focus first on safety, should include psychiatric consultation as soon as possible, and should begin with an evidence-based treatment that may be continued into the maintenance phase. Long-term management focuses on maintenance of euthymia, requires ongoing medication, and may benefit from adjunctive psychotherapy.
Prim Care Companion CNS Disord 2011;13(4):doi:10.4088/PCC.10r01097
© Copyright 2011 Physicians Postgraduate Press, Inc.
Submitted: October 14, 2010; accepted November 30, 2010.
Published online: July 14, 2011 (doi:10.4088/PCC.10r01097).
Corresponding author: Kevin R. Connolly, MD, Philadelphia VA Medical Center, Behavioral Health, 3800 Woodland Ave, Philadelphia, PA 19104 ([email protected]).
Bipolar disorder is a mental disorder characterized by dramatic shifts in mood, thinking, behavior, and energy that is seen in up to 5% of primary care patients.1 In collaboration with a psychiatrist, the family physician plays a vital role in supporting the long-term stability and general health of these patients. In order to effectively treat such patients, it is important that the family physician have a good grasp of the disease, its long-term management, and its impact on overall health.
Clinical Points
- Mania should be treated with lithium, divalproex, or an atypical antipsychotic medication.
- Bipolar depression should be treated with quetiapine, olanzapine/fluoxetine combination, or lamotrigine.
- Once mood episodes are successfully treated, effective acute phase medications should be continued for maintenance of euthymia with appropriate medication monitoring.
- All patients should be offered individual or group psychoeducation to prevent relapse and improve treatment adherence.
A search for evidence-based guidelines for the diagnosis and treatment of adults with bipolar disorder was performed on May 5, 2010, using the National Guideline Clearinghouse database, the Agency for Healthcare Research and Quality Evidence Reports database, and the Cochrane Database of Systematic Reviews. In addition, a clinical query of the PubMed database (completed March 1, 2010) and searches of drug manufacturers’ Web sites (for unpublished trials) were performed to identify randomized, controlled trials and meta-analyses evaluating strategies to treat resistant depression.
Guidelines were selected based on data from randomized controlled trials, meta-analyses, and well-conducted naturalistic trials that were published since 2005. We present recommendations from 4 evidence-based treatment guidelines with a focus on using them to improve clinical care. Additionally, recommendations for therapeutic drug monitoring are presented due to their importance for patient safety, particularly for the primary care physician, although these are based on consensus guidelines.
EPIDEMIOLOGY
Most frequently diagnosed before age 30 years, bipolar disorder includes bipolar I disorder, characterized by manic or mixed episodes (nearly always alternating with depressive episodes), and bipolar II disorder, marked by recurrent episodes of depression and less severe or briefer hypomanic episodes. Related are cyclothymia, characterized by hypomania and subthreshold depression, and bipolar disorder not otherwise specified, a “catch-all” diagnosis for conditions that do not fit neatly into bipolar disorder but that are felt to be properly classified with the bipolar spectrum.2 Some experts argue that up to 50% of recurrent depressions might be so classified, but others have disagreed with this widening of the diagnosis.3,4
Lifetime prevalence of bipolar I disorder is 1% to 2% in both men and women; prevalence of bipolar II disorder is at least 2% and may be underestimated due to the likelihood of recall bias in reporting hypomania.1,5 Estimates of the prevalence of bipolar disorder not otherwise specified vary widely, but the total lifetime prevalence of these 3 disorders is at least 2.4% to 6%.1,5
COMORBIDITY
Patients with bipolar disorder have high rates of medical, psychiatric, and substance abuse disorders, which contribute to reduced life expectancy and lower quality of life.6 A majority meet criteria for at least 1 other mental disorder; anxiety and substance abuse disorders are most common, with a 40% to 60% lifetime prevalence.7-10 Compared to the general population, patients with bipolar disorder have higher rates of diabetes mellitus and liver and cardiovascular disease and experience increased disability and mortality from these illnesses.11,12 The family physician has a valuable opportunity to improve outcomes by aggressive screening for, and maintenance of, these comorbid conditions.
PRESENTATION AND DIAGNOSIS
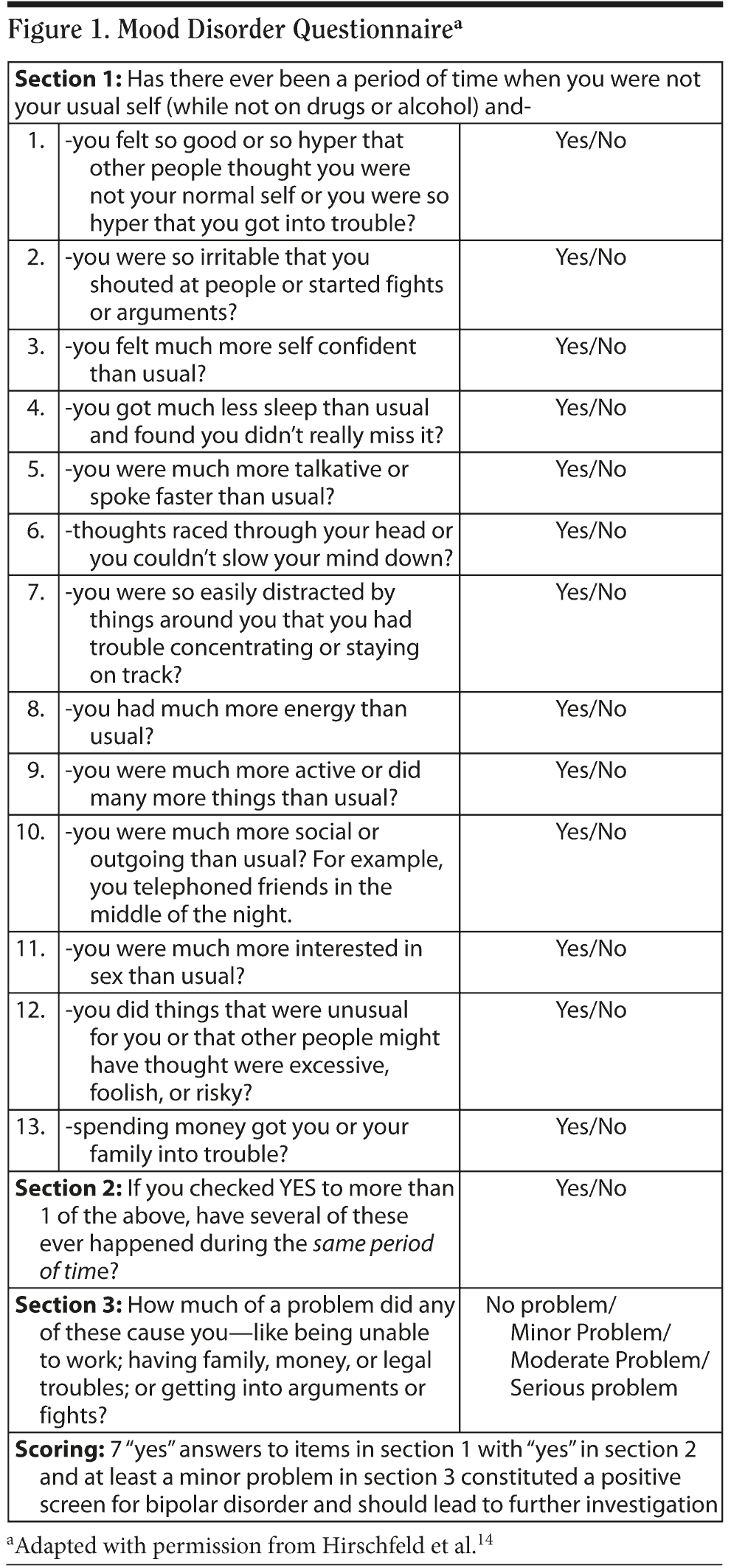
As at least one-half of patients with bipolar I disorder and most patients with bipolar II disorder will initially present during a major depressive episode, a careful history to probe for past manic or hypomanic symptoms is vital to assure a correct diagnosis.13 To screen for historical manic or hypomanic symptoms that might otherwise be overlooked, the self-report Mood Disorders Questionnaire is a validated and useful instrument14,15 (Figure 1).
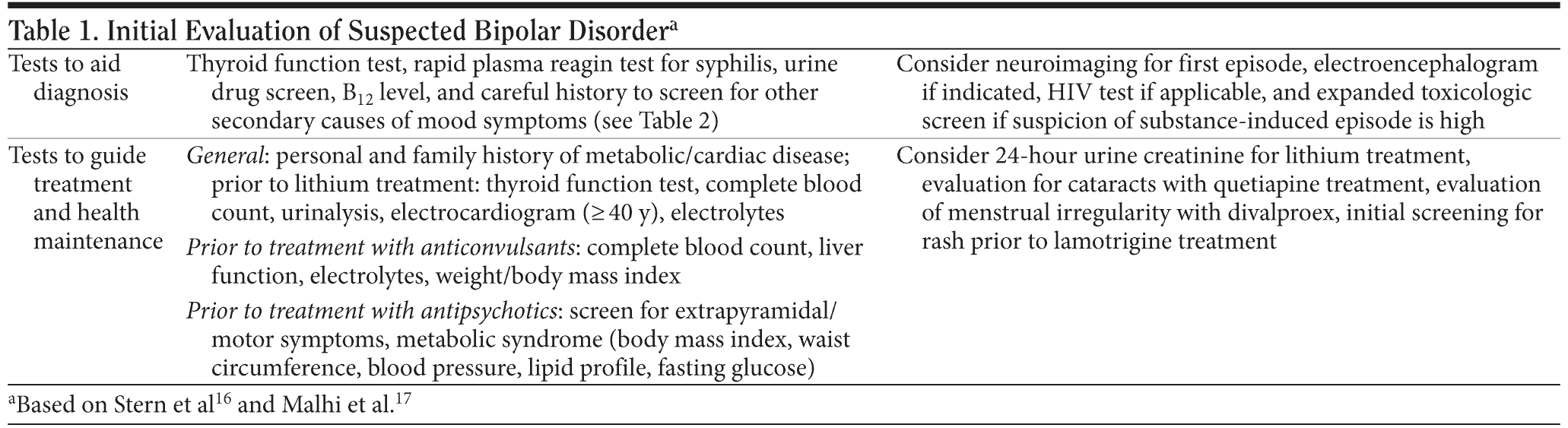
The initial evaluation should aim to collect historical and laboratory data that will help to rule out other disorders and provide essential information to assure a safe and effective medication treatment plan (Table 1 and 2).16,17
Manic Episode
Though classically in a euphoric state, manic patients may also display intense irritability and agitation and profound impairments in reality testing and judgment. About two-thirds of manic episodes are psychotic, with delusions and hallucinations. Mania usually requires psychiatric hospitalization (see appropriate diagnostic criteria in the DSM-IV-TR18).
Major Depressive Episode
The diagnostic criteria for a major depressive episode are the same for bipolar disorder as those used for so-called “unipolar” depression. Some clinical characteristics are more common in bipolar depressions, however, including “atypical” symptoms such as oversleeping and weight gain, delusions, an earlier age at first onset, and prominent mood lability19 (see appropriate diagnostic criteria in the DSM-IV-TR18).
Hypomanic Episode
Hypomanic episodes are similar to mania but more limited in degree and duration. Hypomanias, by definition, are not psychotic and do not require hospitalization. Many patients will not seek medical attention during hypomanic episodes as they are often times of relative productivity and pleasant mood (see appropriate diagnostic criteria in the DSM-IV-TR18).
Mixed Episode
During a mixed episode, patients simultaneously meet full criteria for both mania and depression that co-occur for at least 1 week; women are more commonly affected than men.20 The presence of mixed episodes is associated with poorer prognosis due to a greater risk of chronicity and a higher risk of suicide during the episode.20
Rapid Cycling
Patients who experience more than 4 episodes per year are diagnosed with the rapid-cycling subtype of bipolar disorder; this is associated with treatment resistance and overall poorer prognosis.21 There is some evidence that iatrogenic factors (ie, an “on again-off again” pattern of antidepressant prescription or lithium-induced hypothyroidism) and nonadherence contribute to the risk of rapid cycling.
SPECIAL POPULATIONS
Children and Adolescents
Table 3 summarizes 2007 guidelines for the assessment of child and adolescent bipolar disorder published by the American Academy of Child and Adolescent Psychiatry.22,23 Recommendations for treatment are similar to those of adults with the caveat that research is lacking in this area and that the US Food and Drug Administration (FDA)-approved agents for childhood bipolar disorder are more limited. Currently, the FDA-approved medications for child bipolar disorder include olanzapine (age 13+), lithium (age 12+ years), and, for children aged 10 years and above, quetiapine, risperidone, and aripiprazole (Table 3).
Pregnancy
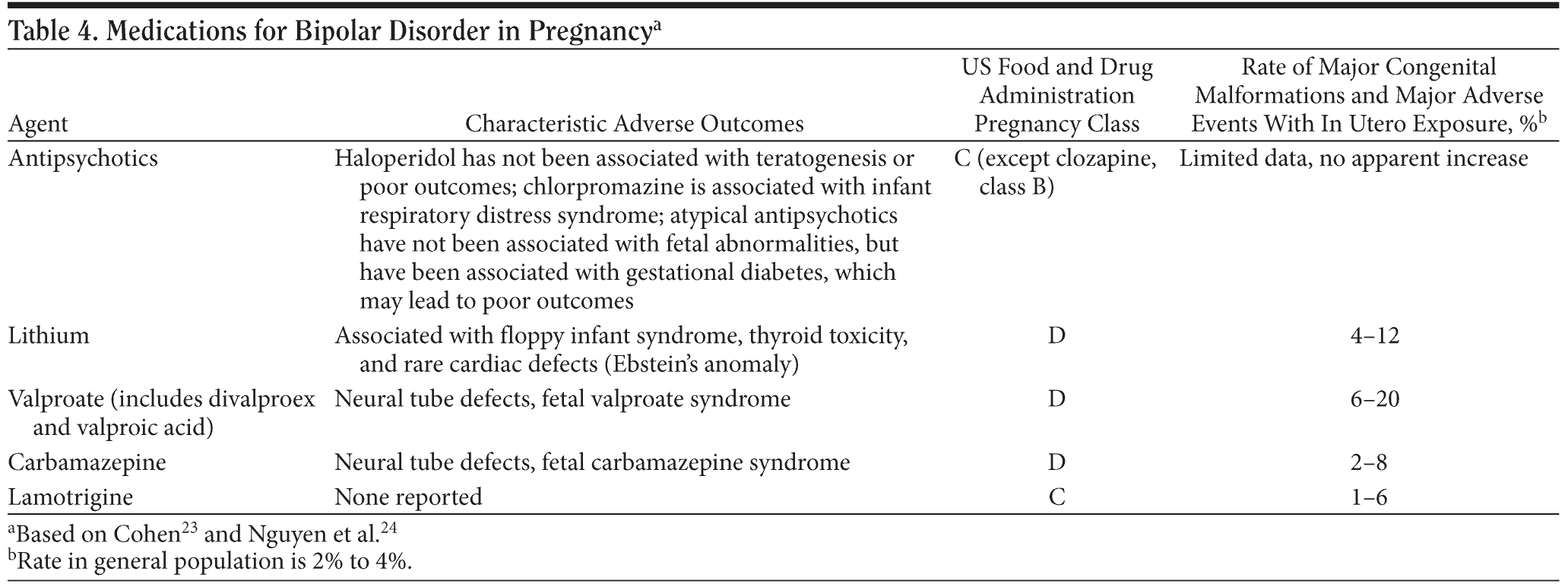
The clinical lore that pregnancy is protective against mood episodes is most likely a myth; treatment to ensure mood stability during pregnancy is vital.23,24 Careful discussion and collaboration between the family physician or obstetrician and psychiatrist are essential to balance maternal and fetal risks, however, given the teratogenicity of many medications used for bipolar disorder (Table 4).
Postpartum
Between 25% to 40% of mothers with bipolar disorder will experience a postpartum mood episode, and up to 30% may be affected by postpartum psychosis; thus, all new mothers should be screened for mood symptoms.25,26 Postpartum psychosis is a psychiatric emergency with gross disturbances in mood, cognition, and behavior and frank hallucinations and delusions.27 Hospitalization should be strongly considered for these indications.
The Elderly
While the course of bipolar disorder sometimes becomes less severe with advancing age, mood episodes may occur at any time. Recommendations for bipolar disorder in the elderly are similar to those in adults, with the caveat that lower doses of medications should be tried in order to minimize adverse effects. For this reason, electroconvulsive therapy may be used earlier in the treatment course, as it is often better tolerated in geriatric populations.28
URGENT AND EMERGENT CARE
Acute mania, depression, and mixed states may all include psychosis, poor insight, and high risks of suicide and thus must be assessed urgently; psychiatric consultation should be sought as soon as possible, and the family should be recruited to help support the patient. Urgent evaluation should focus on safety, and inpatient hospitalization should be strongly considered except in mild cases with no risk to self or others and strong social support. Patients suffering from manic or mixed states may display agitated behavior and may require rapid-acting medication. Under these circumstances, the family practitioner should have a plan for transport of the patient to a nearby emergency center and be familiar with state laws concerning involuntary hospitalization.
PHARMACOLOGIC MANAGEMENT
A number of evidence-based treatment guidelines for bipolar disorder were published in 2009: those put forth in Mahli et al17 as part of an Australian project, those of the British Association for Psychopharmacology,29 and those produced by the International Society for Bipolar Disorders and the Canadian Network for Mood and Anxiety Treatments.30 The most recent US guidelines are those of the Texas Implementation of Medication Algorithms project, which were last updated in 2005.8 These guidelines are reflected in the recommendations below.
Acute Manic or Mixed Episode
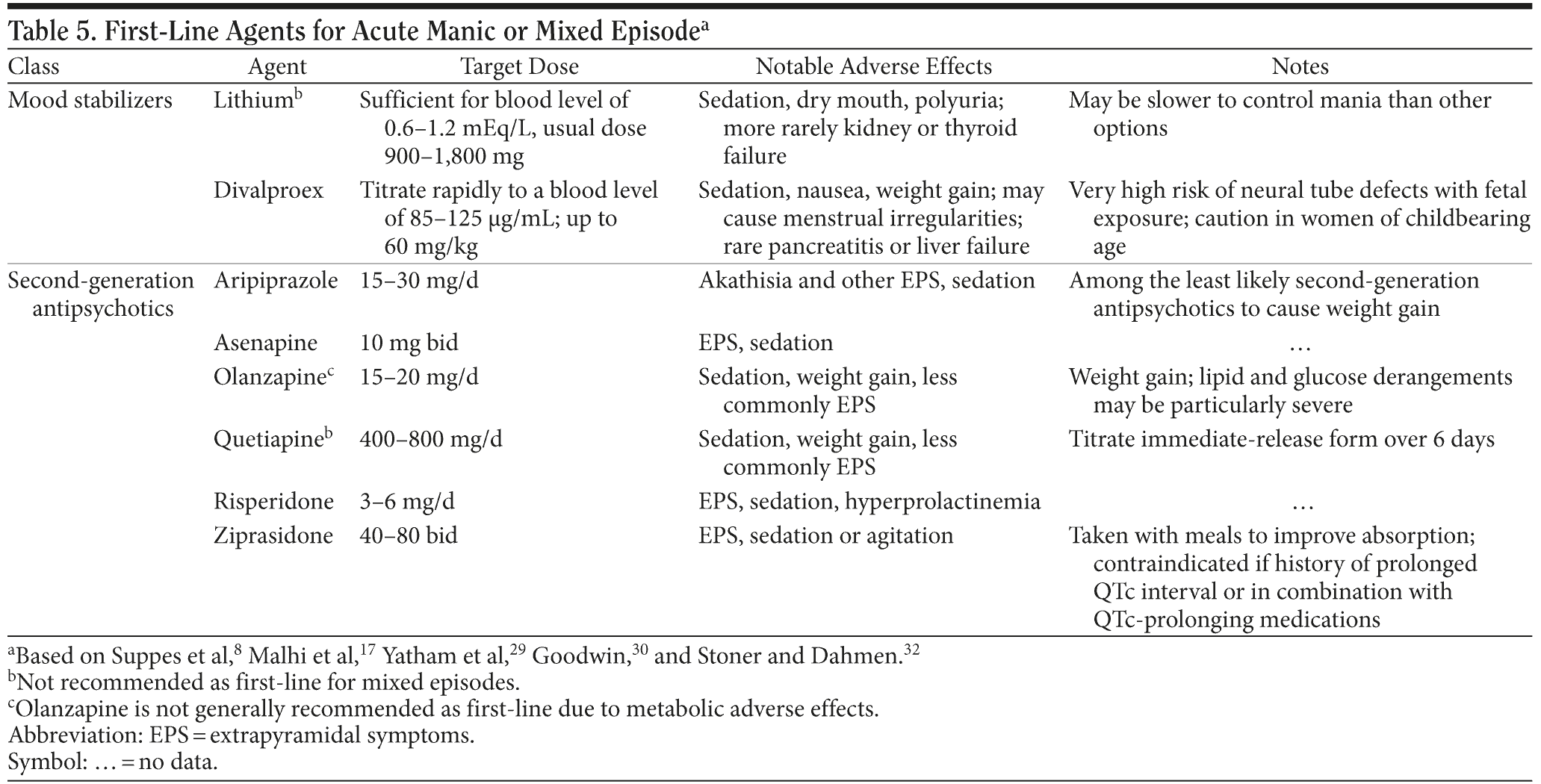
In the case of acute mania, discontinuation or tapering of antidepressant medication should be considered and optimization of any antimanic medication should be undertaken. In the case that the patient is naive to antimanic medication, a first-line antimanic agent such as lithium carbonate should be chosen (Table 5). In addition to lithium salts, divalproex, carbamazepine, and most of the second-generation antipsychotics (SGAs) are FDA-approved treatments for acute mania. While these agents are all effective as monotherapy, results of meta-analysis suggest that a combination of an SGA and either lithium or divalproex is the most effective treatment of acute mania or mixed states, though combination treatment significantly increases adverse effect burden.31
Among the antimanic agents, olanzapine may have a significantly higher liability to cause weight gain and glucose intolerance and so should likely not be used first.8 Divalproex and carbamazepine are significantly associated with neural tube defects and should be used with care in women who may become pregnant; divalproex may additionally lead to menstrual abnormalities and hyperandrogenism in women.33 Carbamazepine also leads to rare but potentially life-threatening blood dyscrasias and is a potent cytochrome P450 inducer.
Once efficacy has been weighed with tolerability and safety, reasonable first-line treatment for an acute manic episode should begin with lithium, divalproex, or SGA monotherapy, with the caveats that olanzapine should be reserved for later steps and that divalproex is not a good first choice in women when other options are available (Table 5).
Acute Depression
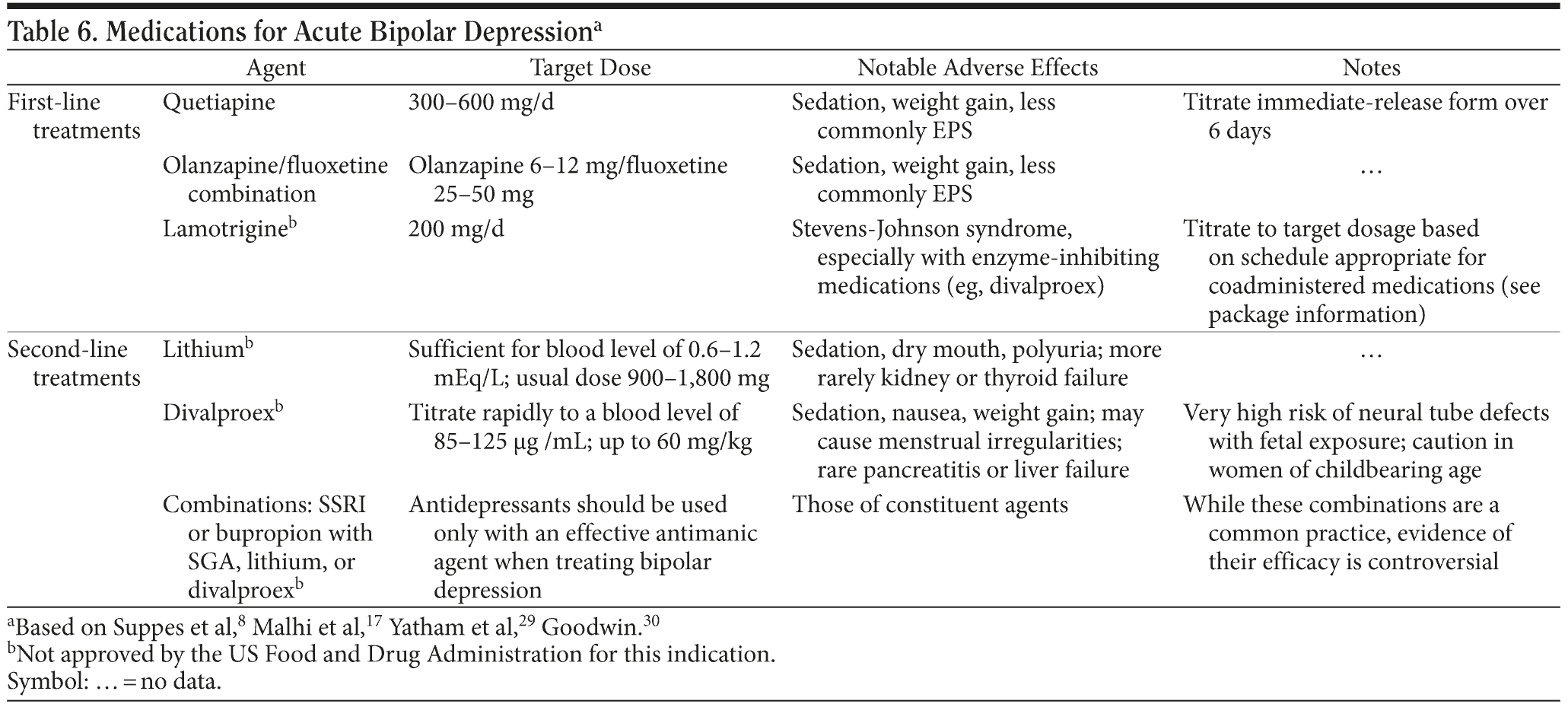
Recommendations differ among the most recent guidelines as to the best treatment for bipolar depression, highlighting the need for more research in this area.8,17,29,30 FDA-approved treatments for acute bipolar depression include only quetiapine and olanzapine/fluoxetine combination. Lamotrigine is approved for the prevention of depressive episodes but has not been effective as a monotherapy for acute depression in clinical trials. A meta-analysis found, however, that overall, lamotrigine monotherapy improved the rate of clinical response in bipolar depression, and this agent is currently in widespread clinical use for this indication.34 Lithium or divalproex, alone or in combination with SSRI antidepressants or bupropion, may be considered as second-line options, though the evidence supporting the efficacy of such combinations remains equivocal17,35,36 (Table 6).
Maintenance
Maintenance of euthymia is the primary goal in the long-term treatment of bipolar disorder and is best achieved through the use of long-term medication.30 Current evidence best supports the use of lithium as first-line treatment: it has been shown to prevent both manic and depressive relapse, as well as suicide in meta-analytic reviews of randomized controlled trials.37,38 Divalproex has somewhat less evidence than lithium, but may also be considered a first-line treatment.39 Lamotrigine has demonstrated efficacy in preventing depressive relapse and may be a good option for more depression-prone patients. Among the SGAs, olanzapine and aripiprazole have demonstrated efficacy in preventing relapse among acute responders, and quetiapine and ziprasidone have some evidence as adjuncts to divalproex or lithium.40-45 Most recently, a long-acting injectable preparation of risperidone was approved by the FDA to prevent relapse on the basis of 2 positive, randomized trials.46,47 For many patients, maintenance therapy will be the medication to which they responded acutely; this should be borne in mind when selecting an acute agent. Careful consideration of the adverse effects of these agents (discussed above) should be undertaken as well before embarking on long-term treatment. One important additional caveat pertains to the cessation of an effective medication: there is evidence that abrupt discontinuation of mood stabilizers may actually hasten relapses, even after sustained periods of remission. As such, patients should be cautioned to not stop their medications abruptly, and when a medication must be discontinued, if possible, it should be slowly tapered.
PSYCHOSOCIAL TREATMENT
Psychoeducation focusing on recognition of early warning signs of relapse is an effective adjunct to medication management and should be offered to all patients with bipolar disorder.48 More intensive psychotherapies (cognitive-behavioral therapy, family focused therapy, interpersonal and social rhythm therapy) have also demonstrated benefit as adjuncts to improve both symptoms and function and should be considered when available and financially feasible49-51 (Table 7).
MAINTENANCE OF GENERAL HEALTH
As discussed, bipolar disorder carries with it the burden of higher comorbidity and medication effects that may pose risks to the general health of the patient. The family physician plays a vital role in mitigating these risks by careful monitoring of a number of health parameters (Table 8).52
KEY RECOMMENDATIONS
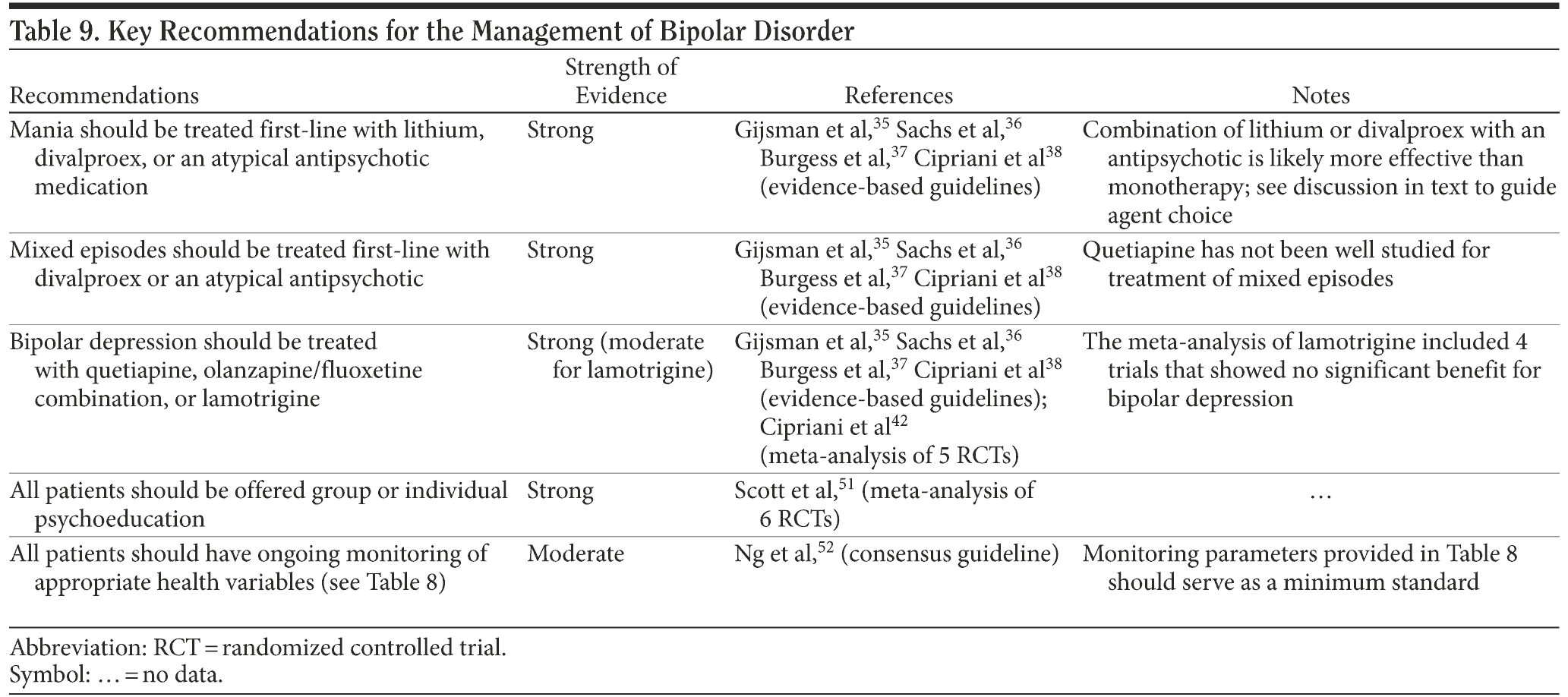
Bipolar disorder is a lifelong illness that is complicated by high comorbidity and risk of poor health outcomes. The family physician has a vital role in improving patient quality of life as the primary care provider. The management of acute mood episodes should focus first on safety, should include psychiatric consultation as soon as possible, and should begin with an evidence-based treatment that may be continued into the maintenance phase (Table 9). Long-term management focuses on maintenance of euthymia, requires ongoing medication, and may benefit from adjunctive psychotherapy. In the longitudinal management of these patients, the family physician may be particularly helpful in working to mitigate the unfortunate effects of the comorbidity that this disorder carries with it and the adverse effects inherent in even its best treatments.
Drug names: aripiprazole (Abilify), asenapine (Saphris), bupropion (Wellbutrin, Aplenzin, and others), carbamazepine (Carbatrol, Equetro, and others), clozapine (Clozaril, FazaClo, and others), fluoxetine (Prozac and others), haloperidol (Haldol and others), lamotrigine (Lamictal and others), lithium (Lithobid and others), olanzapine (Zyprexa), olanzapine/fluoxetine combination (Symbyax), quetiapine (Seroquel), risperidone (Risperdal and others), valproic acid (Depakene, Stavzor, and others), ziprasidone (Geodon).
Author affiliations: Department of Behavioral Health, Philadelphia VA Medical Center (Dr Connolly); and Department of Psychiatry, University of Pennsylvania School of Medicine (Dr Thase), Philadelphia, Pennsylvania.
Potential conflicts of interest: Dr Thase has served as a consultant to or on the advisory boards of AstraZeneca, Bristol-Myers Squibb, Dey Pharma, Eli Lilly, Forest, Gerson Lehman Group, GlaxoSmithKline, Guidepoint Global, H. Lundbeck A/S, MedAvante, Merck, Neuronetics, Novartis, Otsuka, Ortho-McNeil, Pamlab, Pfizer, Schering-Plough, Shire, Supernus, Takeda, and Transcept; has received grant/research support from Agency for Healthcare Research and Quality, Eli Lilly, GlaxoSmithKline, National Institute of Mental Health, and Sepracor; has served on the speakers bureaus of AstraZeneca, Bristol-Myers Squibb, Eli Lilly, Merck, and Pfizer; has equity holdings in MedAvante; and receives royalty income from American Psychiatric Publishing, Guilford Publications, Herald House, and W.W. Norton. Dr Thase’s wife is employed by Embryon (formerly Advogent). Dr Connolly reports no financial or other affiliations relevant to the subject of this article.
Funding/support: None reported.
REFERENCES
1. Judd LL, Akiskal HS. The prevalence and disability of bipolar spectrum disorders in the US population: re-analysis of the ECA database taking into account subthreshold cases. J Affect Disord. 2003;73(1-2):123-131. PubMed doi:10.1016/S0165-0327(02)00332-4
2. Akiskal HS. Validating ‘ hard’ and ‘ soft’ phenotypes within the bipolar spectrum: continuity or discontinuity? J Affect Disord. 2003;73(1-2):1-5. PubMed doi:10.1016/S0165-0327(02)00390-7
3. Soares JC, Gershon S. The diagnostic boundaries of bipolar disorder. Bipolar Disord. 2000;2(1):1-2. PubMed doi:10.1034/j.1399-5618.2000.020101.x
4. Baldessarini RJ. A plea for integrity of the bipolar disorder concept. Bipolar Disord. 2000;2(1):3-7. PubMed doi:10.1034/j.1399-5618.2000.020102.x
5. Merikangas KR, Akiskal HS, Angst J, et al. Lifetime and 12-month prevalence of bipolar spectrum disorder in the National Comorbidity Survey replication. Arch Gen Psychiatry. 2007;64(5):543-552. PubMed doi:10.1001/archpsyc.64.5.543
6. Roshanaei-Moghaddam B, Katon W. Premature mortality from general medical illnesses among persons with bipolar disorder: a review. Psychiatr Serv. 2009;60(2):147-156. PubMed doi:10.1176/appi.ps.60.2.147
7. McElroy SL, Altshuler LL, Suppes T, et al. Axis I psychiatric comorbidity and its relationship to historical illness variables in 288 patients with bipolar disorder. Am J Psychiatry. 2001;158(3):420-426. PubMed doi:10.1176/appi.ajp.158.3.420
8. Suppes T, Dennehy EB, Hirschfeld RM, et al; Texas Consensus Conference Panel on Medication Treatment of Bipolar Disorder. The Texas Implementation of Medication Algorithms: update to the algorithms for treatment of bipolar I disorder. J Clin Psychiatry. 2005;66(7):870-886. PubMed doi:10.4088/JCP.v66n0710
9. Kessler RC, Rubinow DR, Holmes C, et al. The epidemiology of DSM-III-R bipolar I disorder in a general population survey. Psychol Med. 1997;27(5):1079-1089. PubMed doi:10.1017/S0033291797005333
10. El-Mallakh RS, Hollifield M. Comorbid anxiety in bipolar disorder alters treatment and prognosis. Psychiatr Q. 2008;79(2):139-150. PubMed doi:10.1007/s11126-008-9071-5
11. Perron BE, Howard MO, Nienhuis JK, et al. Prevalence and burden of general medical conditions among adults with bipolar I disorder: results from the National Epidemiologic Survey on Alcohol and Related Conditions. J Clin Psychiatry. 2009;70(10):1407-1415. PubMed doi:10.4088/JCP.08m04586yel
12. Regenold WT, Thapar RK, Marano C, et al. Increased prevalence of type 2 diabetes mellitus among psychiatric inpatients with bipolar I affective and schizoaffective disorders independent of psychotropic drug use. J Affect Disord. 2002;70(1):19-26. PubMed doi:10.1016/S0165-0327(01)00456-6
13. Bowden CL. Strategies to reduce misdiagnosis of bipolar depression. Psychiatr Serv. 2001;52(1):51-55. PubMed doi:10.1176/appi.ps.52.1.51
14. Hirschfeld RM, Williams JB, Spitzer RL, et al. Development and validation of a screening instrument for bipolar spectrum disorder: the Mood Disorder Questionnaire. Am J Psychiatry. 2000;157(11):1873-1875. PubMed doi:10.1176/appi.ajp.157.11.1873
15. Hirschfeld RM, Holzer C, Calabrese JR, et al. Validity of the Mood Disorder Questionnaire: a general population study. Am J Psychiatry. 2003;160(1):178-180. PubMed doi:10.1176/appi.ajp.160.1.178
16. Stern TA, Fricchione GL, Cassem NH, et al, eds. Massachusetts General Hospital Handbook of General Hospital Psychiatry. 5th edition. Philadelphia, PA: Mosby; 2004: 69-82, 119-134
17. Malhi GS, Adams D, Lampe L, et al; CADE Clinic, University of Sydney. Clinical practice recommendations for bipolar disorder. Acta Psychiatr Scand Suppl. 2009;119(439):27-46. PubMed doi:10.1111/j.1600-0447.2009.01383.x
18. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
19. Mitchell PB, Goodwin GM, Johnson GF, et al. Diagnostic guidelines for bipolar depression: a probabilistic approach. Bipolar Disord. 2008;10(1, pt 2):144-152. PubMed doi:10.1111/j.1399-5618.2007.00559.x
20. Gonzסlez-Pinto A, Aldama A, Mosquera F, et al. Epidemiology, diagnosis and management of mixed mania. CNS Drugs. 2007;21(8):611-626. PubMed doi:10.2165/00023210-200721080-00001
21. Schneck CD. Treatment of rapid-cycling bipolar disorder. J Clin Psychiatry. 2006;67(suppl 11):22-27. PubMed
22. McClellan J, Kowatch R, Findling RL; Work Group on Quality Issues. Practice parameter for the assessment and treatment of children and adolescents with bipolar disorder. J Am Acad Child Adolesc Psychiatry. 2007;46(1):107-125. PubMed doi:10.1097/01.chi.0000242240.69678.c4
23. Cohen LS. Treatment of bipolar disorder during pregnancy. J Clin Psychiatry. 2007;68(suppl 9):4-9. PubMed
24. Nguyen HT, Sharma V, McIntyre RS. Teratogenesis associated with antibipolar agents. Adv Ther. 2009;26(3):281-294. PubMed doi:10.1007/s12325-009-0011-z
25. Hunt N, Silverstone T. Does puerperal illness distinguish a subgroup of bipolar patients? J Affect Disord. 1995;34(2):101-107. PubMed doi:10.1016/0165-0327(95)00006-9
26. Jones I, Craddock N. Familiality of the puerperal trigger in bipolar disorder: results of a family study. Am J Psychiatry. 2001;158(6):913-917. PubMed doi:10.1176/appi.ajp.158.6.913
27. Sit D, Rothschild AJ, Wisner KL. A review of postpartum psychosis. J Womens Health (Larchmt). 2006;15(4):352-368. PubMed doi:10.1089/jwh.2006.15.352
28. Aziz R, Lorberg B, Tampi RR. Treatments for late-life bipolar disorder. Am J Geriatr Pharmacother. 2006;4(4):347-364. PubMed doi:10.1016/j.amjopharm.2006.12.007
29. Yatham LN, Kennedy SH, Schaffer A, et al. Canadian Network for Mood and Anxiety Treatments (CANMAT) and International Society for Bipolar Disorders (ISBD) collaborative update of CANMAT guidelines for the management of patients with bipolar disorder: update 2009. Bipolar Disord. 2009;11(3):225-255. PubMed doi:10.1111/j.1399-5618.2009.00672.x
30. Goodwin GM; Consensus Group of the British Association for Psychopharmacology. Evidence-based guidelines for treating bipolar disorder, revised second edition: recommendations from the British Association for Psychopharmacology. J Psychopharmacol. 2009;23(4):346-388. PubMed doi:10.1177/0269881109102919
31. Scherk H, Pajonk FG, Leucht S. Second-generation antipsychotic agents in the treatment of acute mania: a systematic review and meta-analysis of randomized controlled trials. Arch Gen Psychiatry. 2007;64(4):442-455. PubMed doi:10.1001/archpsyc.64.4.442
32. Stoner SC, Dahmen MM. Extended-release divalproex in bipolar and other psychiatric disorders: a comprehensive review. Neuropsychiatr Dis Treat. 2007;3(6):839-846. PubMed
33. Rasgon NL, Reynolds MF, Elman S, et al. Longitudinal evaluation of reproductive function in women treated for bipolar disorder. J Affect Disord. 2005;89(1-3):217-225. PubMed doi:10.1016/j.jad.2005.08.002
34. Geddes JR, Calabrese JR, Goodwin GM. Lamotrigine for treatment of bipolar depression: independent meta-analysis and meta-regression of individual patient data from five randomised trials. Br J Psychiatry. 2009;194(1):4-9. PubMed doi:10.1192/bjp.bp.107.048504
35. Gijsman HJ, Geddes JR, Rendell JM, et al. Antidepressants for bipolar depression: a systematic review of randomized, controlled trials. Am J Psychiatry. 2004;161(9):1537-1547. PubMed doi:10.1176/appi.ajp.161.9.1537
36. Sachs GS, Nierenberg AA, Calabrese JR, et al. Effectiveness of adjunctive antidepressant treatment for bipolar depression. N Engl J Med. 2007;356(17):1711-1722. PubMed doi:10.1056/NEJMoa064135
37. Burgess S, Geddes J, Hawton K, et al. Lithium for maintenance treatment of mood disorders. Cochrane Database Syst Rev. 2001;(3):CD003013. PubMed
38. Cipriani A, Pretty H, Hawton K, et al. Lithium in the prevention of suicidal behavior and all-cause mortality in patients with mood disorders: a systematic review of randomized trials. Am J Psychiatry. 2005;162(10):1805-1819. PubMed doi:10.1176/appi.ajp.162.10.1805
39. Macritchie KA, Geddes JR, Scott J, et al. Valproic acid, valproate and divalproex in the maintenance treatment of bipolar disorder. Cochrane Database Syst Rev. 2001;(3):CD003196. PubMed
40. Keck PE Jr, Calabrese JR, McQuade RD, et al; Aripiprazole Study Group. A randomized, double-blind, placebo-controlled 26-week trial of aripiprazole in recently manic patients with bipolar I disorder. J Clin Psychiatry. 2006;67(4):626-637. PubMed doi:10.4088/JCP.v67n0414
41. Keck PE Jr, Calabrese JR, McIntyre RS, et al; Aripiprazole Study Group. Aripiprazole monotherapy for maintenance therapy in bipolar I disorder: a 100-week, double-blind study versus placebo. J Clin Psychiatry. 2007;68(10):1480-1491. PubMed doi:10.4088/JCP.v68n1003
42. Cipriani A, Rendell J, Geddes JR. Olanzapine in the long-term treatment of bipolar disorder: a systematic review and meta-analysis. J Psychopharmacol. 2010;24(12):1729-1738. PubMed doi:10.1177/0269881109106900
43. Vieta E, Suppes T, Eggens I, et al. Efficacy and safety of quetiapine in combination with lithium or divalproex for maintenance of patients with bipolar I disorder (international trial 126). J Affect Disord. 2008;109(3):251-263. PubMed doi:10.1016/j.jad.2008.06.001
44. Suppes T, Vieta E, Liu S, et al; Trial 127 Investigators. Maintenance treatment for patients with bipolar I disorder: results from a North American study of quetiapine in combination with lithium or divalproex (trial 127). Am J Psychiatry. 2009;166(4):476-488. PubMed doi:10.1176/appi.ajp.2008.08020189
45. Bowden CL, Vieta E, Ice KS, et al. Ziprasidone plus a mood stabilizer in subjects with bipolar I disorder: a 6-month, randomized, placebo-controlled, double-blind trial. J Clin Psychiatry. 2010;71(2):130-137. PubMed doi:10.4088/JCP.09m05482yel
46. Johnson & Johnson Pharmaceutical Research & Development LLC. 2008. ClinicalTrials Web site. A study of the safety and efficacy of injectable risperidone in the prevention of bipolar mood episodes (NCT00132678). http://clinicaltrials.gov/ct2/show/NCT00132678. Accessed April 7, 2011.
47. Macfadden W, Alphs L, Haskins JT, et al. A randomized, double-blind, placebo-controlled study of maintenance treatment with adjunctive risperidone long-acting therapy in patients with bipolar I disorder who relapse frequently. Bipolar Disord. 2009;11(8):827-839. PubMed doi:10.1111/j.1399-5618.2009.00761.x
48. Morriss RK, Faizal MA, Jones AP, et al. Interventions for helping people recognise early signs of recurrence in bipolar disorder. Cochrane Database Syst Rev. 2007;24(1):CD004854. PubMed
49. Miklowitz DJ, Otto MW, Frank E, et al. Psychosocial treatments for bipolar depression: a 1-year randomized trial from the Systematic Treatment Enhancement Program. Arch Gen Psychiatry. 2007;64(4):419-426. PubMed doi:10.1001/archpsyc.64.4.419
50. Miklowitz DJ, Otto MW, Frank E, et al. Intensive psychosocial intervention enhances functioning in patients with bipolar depression: results from a 9-month randomized controlled trial. Am J Psychiatry. 2007;164(9):1340-1347. PubMed doi:10.1176/appi.ajp.2007.07020311
51. Scott J, Colom F, Vieta E. A meta-analysis of relapse rates with adjunctive psychological therapies compared to usual psychiatric treatment for bipolar disorders. Int J Neuropsychopharmacol. 2007;10(1):123-129. PubMed doi:10.1017/S1461145706006900
52. Ng F, Mammen OK, Wilting I, et al; International Society for Bipolar Disorders. The International Society for Bipolar Disorders (ISBD) consensus guidelines for the safety monitoring of bipolar disorder treatments. Bipolar Disord. 2009;11(6):559-595. PubMed doi:10.1111/j.1399-5618.2009.00737.x