Objective: To determine clinical and psychosocial variables associated with increased depression severity in patients who consult public primary health care clinics (PHCs) in Chile.
Methods: The study included 394 patients diagnosed with major depressive disorder (MDD) according to ICD-10 criteria who were evaluated between February and September 2014 using a sociodemographic interview, the Mini-International Neuropsychiatric Interview (MINI), a screening for childhood trauma, a scale for partner violence, the Life Events Survey (LES), and the Hamilton Rating Scale for Depression (HRSD).
Results: Positive correlations were determined between greater severity of depression and more frequency of depressive episodes (r = 0.2, P < .01), psychiatric comorbidities (r = 0.36, P < .01), number of childhood traumatic events (r = 0.19, P < .01), intimate partner violence events (r = 0.155, P < .01), and stressful life events (r = 0.13, P < .05). Inverse correlation was determined with the age at first episode (r = −0.16, P < .01). The psychiatric comorbidities explained most of the variability of depressive symptoms (11.7%); addition of child abuse to the comorbidities increased the correlation to 12.7%.
Conclusions: The different covariates considered in this sample showed that psychiatric comorbidity played the principal role in explaining the severity of depression.
Factors Associated With Greater Severity
of Depression in Chilean Primary Care Patients
ABSTRACT
Objective: To determine clinical and psychosocial variables associated with increased depression severity in patients who consult public primary health care clinics (PHCs) in Chile.
Methods: The study included 394 patients diagnosed with major depressive disorder (MDD) according to ICD-10 criteria who were evaluated between February and September 2014 using a sociodemographic interview, the Mini-International Neuropsychiatric Interview (MINI), a screening for childhood trauma, a scale for partner violence, the Life Events Survey (LES), and the Hamilton Rating Scale for Depression (HRSD).
Results: Positive correlations were determined between greater severity of depression and more frequency of depressive episodes (r = 0.2, P < .01), psychiatric comorbidities (r = 0.36, P < .01), number of childhood traumatic events (r = 0.19, P < .01), intimate partner violence events (r = 0.155, P < .01), and stressful life events (r = 0.13, P < .05). Inverse correlation was determined with the age at first episode (r = −0.16, P < .01). The psychiatric comorbidities explained most of the variability of depressive symptoms (11.7%); addition of child abuse to the comorbidities increased the correlation to 12.7%.
Conclusions: The different covariates considered in this sample showed that psychiatric comorbidity played the principal role in explaining the severity of depression.
Prim Care Companion CNS Disord 2017;19(3):16m02051
https://doi.org/10.4088/PCC.16m02051
© Copyright 2017 Physicians Postgraduate Press, Inc.
aSchool of Medicine, Universidad de Talca, Talca, Chile
bPrivate practice, Curico, Chili
cRegional Hospital, Talca, Chile
dDepartment of Psychology, Universidad de Talca, Talca, Chile
*Corresponding author: Verónica Vitriol, MD, MSc, School of Medicine, Universidad de Talca, Av. Lircay s/n Talca, Chile ([email protected]).
In Chile, as in the world, major depressive disorder is a significant public health problem.1,2 It is estimated that among the adult Chilean population, the lifetime prevalence of a major depressive episode is 9%,3 and the prevalence of depressive symptoms in the last year reached 17.2% in 2011.4
In 2001, the Chilean Health System implemented a national program to treat depression.5 According to national clinical guidelines,6 90% of depression cases are treated in primary health care clinics (PHCs). At the primary care level, the lifetime prevalence reaches 23.6%, and the 12-month prevalence is 10.2%.7 Patients with treatment-refractory depressions with suicide attempt and those with suspected bipolar disorder are referred to the general hospital for evaluation by a psychiatrist.6 According to national clinical guidelines,6 psychiatrists must carry out weekly consultations with the PHC.
The available evidence regarding the clinical characteristics of patients treated for depression in Chilean PHCs is still limited.7 Alvarado et al8 showed that in most cases patients were middle-aged women with recurrent depressive disorders, a history of intimate partner violence, and reduced social support network. Also, the authors8 reported the existence of a subdiagnosis of depression severity by the physicians during the initial evaluation in a Chilean PHC.9 This result is relevant considering the national clinical guidelines6 impart a standardized treatment according to the initial severity of this disease. Moreover, there is evidence in depressive samples from developed countries linking greater depressive severity at baseline with a worse prognosis during the first year of treatment.10
The current Chilean clinical guideline6 typifies severity of depression based on number of depressive symptoms according to the tenth version of the International Classification of Diseases (ICD-10).11 However, there are clinical and psychosocial factors, such as psychiatric comorbidities, biomedical conditions, and adverse biographical events,12–14 that are associated with a worse evolution in depression patients. These factors can be recognized in the initial evaluations by primary care physicians.15
Most of the evidence regarding the impact of psychiatric comorbidity, biomedical conditions, and biographical trauma events on depression comes from studies12–14 conducted in developed countries. For example, this evidence shows that biographical trauma and psychiatric comorbidities are not adequately assessed among subjects with depression.15,16 The lack of recognition of psychiatric comorbidities is associated with a worsening of depressive symptoms.12,17 Additionally, childhood abuse history is linked to unresponsiveness to pharmacologic treatments for depression.18–20 Moreover, there is a lack of evidence regarding which of these clinical or psychosocial factors are associated with initial greater severity of depression shown in PHCs. A better understanding of these issues may contribute to greater recognition of the subgroup of depressive patients that need a more specific treatment approach in PHCs.
The objective of this study is to determine which clinical and psychosocial variables are associated with greater depressive symptomatic severity in a sample of patients consulting for depression in primary care in Chile.
METHODS
Study Design
This descriptive correlational study was conducted in the Maule Region in Chile. The protocol was approved by the ethical committees of Universidad de Talca and Maule Regional Health Service. All subjects provided verbal and written informed consent prior to participation.
Participants and Procedures
The sample (440 patients) was generated from 2,978 patients older than age 15 years admitted to primary care treatment for depression at 8 PHCs in the Maule Region in Chile between February and September 2014. Patients with psychiatric or physical disorders that prevented them from being interviewed or that undermined their ability to provide accurate information (brain damage, sensory impairment, severe suicide risk, and psychosis) and those who declined participation in the study were excluded. On the basis of ICD-10 criteria,11 depressive episode diagnosis was confirmed by 8 experienced psychiatrists and psychologists using the Mini-International Neuropsychiatric Interview (MINI).21 Forty-six patients did not meet criteria for depressive episode according to the ICD-10. So, the final sample was reduced to 394 patients.
Instruments
Participants were interviewed by the specialized team using the following instruments:
- Clinical interview. The interview collected sociodemographic background (age, sex, marital status, education, and employment status), clinical information about depressive illness (age at onset and duration of illness), and presence of biomedical chronic diseases (diabetes, hypertension, other cardiovascular disease, thyroid dysfunction, arthritis or osteoarthritis, and other diseases).
- Screening Scale for Childhood Trauma. This scale was developed by Marshall et al22 and adapted and validated in Chile by Cuneo et al.23 It is administered by the clinician and evaluates whether the patient remembers having suffered 1 of the following events before the age of 15 years: traumatic separation from father, mother, or caregiver for more than a month; alcohol or drug abuse by a family member; physical abuse; physical injury associated with the physical abuse; domestic violence between parents or caregivers; and sexual abuse by relative or nonrelative. This particular instrument has been used in Chile in previous work.24,25
- Survey of Life Experiences. Designed by Sarason et al26 and translated into Spanish,27 the LES consists of 47 items that investigate vital changes in the previous 6 months with both positive and negative connotations. For the purposes of this study, only the negative life events were considered.
- Intimate partner violence questionnaire. This questionnaire28 consists of 12 questions based on the World Health Organization definition for physical, psychological, and sexual violence, with frequencies of never, once or twice, and 3 or more times. This questionnaire has been used in previous studies in Chile.28
- MINI.21 This brief and highly structured interview investigates major psychiatric disorders listed in the ICD-10 and DSM-IV.
- 17-item Hamilton Rating Scale for Depression.29 The HRSD was used to determine the severity of depression.
The statistical data analysis was conducted using the 14th version of the Statistical Package for the Social Sciences (SPSS) program (IBM, Armonk, New York). To analyze the clinical and psychosocial characteristics of the sample, a univariate descriptive statistical analysis was performed. To determine the relationship between greater severities of depression and continuous variables, a Pearson bivariate correlation was completed. Finally, in order to quantify the relevance of the variables over the severity of depression, a multiple linear regression model (stepwise method) was performed. The significance level was .05.
RESULTS
Sociodemographic and Clinical Characteristics
The sample group comprised 87.3% women (n = 344), and the mean age was 47.5 (SD = 15.1) (Table 1). Less than half of the sample was in a relationship. A quarter of the sample had not completed high school, and only 13.2% had paid jobs.

The mean age of the first major depressive episode was 30.7 years (SD = 17.2); 72.2% of patients experienced recurrent depression with approximately 4 episodes (mean = 3.6, SD = 4.2).
Comorbidities
With regard to biomedical chronic diseases, 55% of patients had at least 1 medical condition (21.4% had only 1, 18.9% had 2, and 15% had ≥ 3). Regarding psychiatric comorbidities, 89.1% of the sample had a psychiatric comorbid disorder (20.6% had only 1, 20.3% had 2, and 19.5% had 3). The most prevalent were panic disorder (29%), generalized anxiety disorder (25%), agoraphobia (23%), social anxiety disorder (16%), and posttraumatic stress disorder (14%).
Adverse Biographical Events
In the sample, 82% of the patients were found to have experienced at least 1 traumatic childhood event. One event was experienced by 17.0% of the sample, 16.7% reported 2 events, 17.0 reported 3 events, and 31.2% reported ≥ 4 events. The most common traumatic events were witnessing domestic violence at home (49.5%) and alcohol or drug abuse by a family member (48.0%). Sexual abuse by a nonrelative had a lower incidence (19.1%).
Regarding negative life experiences indicated in the LES, 21.1% of the sample reported having experienced 1 stressful life event during the 6 months prior to the assessment, 22.1% reported 2 events, 16.2% experienced 3 events, and 34.6% indicated more than 3 events.
Finally, 58.1% of the sample reported having experienced some form of intimate partner violence during their lifetime (psychological: 58.1%, physical: 38.1%, and sexual: 19.8%); 6.4% experienced 1 event, 4.7% reported 2 events, and 47.2% reported 3 or more events.
Severity of Depressive Symptoms
The mean intensity of depressive symptoms as rated by the HRSD was 20.67 points (SD = 6.14).
Correlations Between Continuous Variables
and Severity of Depression
The data analysis revealed positive correlations between greater severity of depression and number of depressive episodes (r = 0.2, P < .01), number of psychiatric comorbidities (r = 0.36, P < .01), number of childhood traumatic events (r = 0.19, P < .01), number of intimate partner violence events (r = 0.15, P < .01), and stressful life events (r = 0.13, P < .05). Furthermore, an inverse correlation between greater severity of depression and age at first depressive episode (r = −0.16, P < .01) was determined
(Table 2).

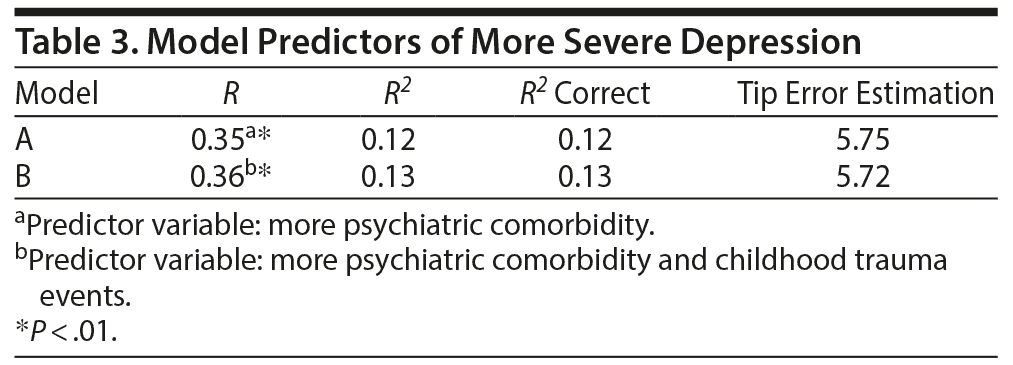
In the linear regression model considering the continuous significant variables, only psychiatric comorbidities explain most of the variability of depressive symptoms (11.7%). If the variable childhood trauma is included, 12.7% of total variability of depressive symptoms is explained (Table 3). It is important to note that in this population psychiatric comorbidities were also positively correlated with childhood traumatic events (r = 0.23, P < .01).
DISCUSSION
This study carried out in PHCs in Chile shows a high frequency of different psychiatric comorbidities, mainly anxiety disorders, among depressive patients. This result is consistent with the literature.12,17,30 Nevertheless, an important distinction from reports12,16,19 of other countries is the higher prevalence of agoraphobia in this sample. This result may be explained by the high frequency of this disorder among the Chilean population.3
Also, in this study a high prevalence of adverse biographic events was found. The most important of these records is the childhood trauma history, particularly sexual abuse. This result supports data from previous studies conducted in Chile31; however, the prevalence is higher than that reported in other clinical samples.32 This finding is relevant when considering the evidence that childhood trauma is associated with early age at onset of depression,33 presence of psychiatric comorbidity,32,34 chronicity of depression,33 stressful life events as an adult,35 and intimate partner violence.36
Teicher and Samson37 support the idea that the complex clinical picture presented by patients with depression maltreated as children represents the expression of a distinct ecophenotype, a clinical subtype of depression that needs to be recognized and boarded in clinical practice through a specific approach. In this sense, this study provides evidence that can guide the approach to this subtype of depression in PHCs.
Two statistical analyses were derived from our data. The first analysis shows that the factors associated with an increased severity of depressive symptoms at baseline are psychiatric comorbidity, recurrence, early age at onset of depression, and the presence of adverse events, mainly childhood trauma. This conclusion is indeed correct when each of these variables is independently regressed on the severity of the depression. However, if we take the variables together in the linear regression, the second analysis shows that psychiatric comorbidity is the most relevant covariate for explaining greater severity of depression.
This result is consistent with findings reported by other studies. In the Netherlands Mental Health Survey and Incidence study,38 it was found that child abuse and anxiety comorbidities, among others, clearly constitute potential factors associated with suicide (considered as an indicator of severity of depression). However, in the multivariate analysis, the association of child abuse was lost.38 Another recent study39 conducted in a Japanese depressive population determined that child abuse and personality traits were associated with the severity of depression. However, the study39 showed that personality traits had the most direct association to increased symptom severity.
Considering previous research,38,39 the Chilean experience as reflected in our data is consistent with and might be explained by the early trauma hypothesis. According to investigations during the last 20 years,37,40 there is enough evidence from clinical and preclinical studies40,41 that shows a preeminent role of childhood trauma in vulnerability to developing major psychiatric disorders such as depression. This vulnerability is an expression of increased stress responsiveness, a consequence of neurobiological alterations in circuitry involved in the regulation of stress and emotion.41 These alterations predispose to the development of complex clinical pictures characterized mainly by the presence of anxious-depressive comorbidities.37 Taking into account the results of our study, these comorbidities should be prioritized in the approach to the clinical complexity exhibited by patients with depression and early trauma who present to PHCs. At this point, according to a recent study,42 there seems to be a link between specific anxious comorbidities and adverse childhood events that could guide the treatment of patients with depression in PHCs.
In this study, unexpectedly, biomedical comorbidity was not associated with higher depressive severity at the time of consultation. These results warrant further investigation since the prevalence of medical conditions in depressive patients is 2 to 3 times higher than that reported in patients without depression,43 and medical comorbidity has also been associated with increased chronicity of depression and lower response to treatment.15,44
The main strengths of this study are the sample size of depressive patients seeking help at PHCs in a Latin country and the quality of data. During the investigation, mental health experts were able to access highly confidential patient records and ensure that their assessments were conducted using standardized instruments.
A limitation of this research is the inherent disadvantage of retrospectively inquiring about past biographical adverse events. Regarding the psychiatric comorbidities, the MINI does not explore other important mental disorders often present in depressive patients such as borderline personality disorder and somatization disorder.25,45
It is important to note that the effects of comorbidities and adverse biographical events on the intensity of depressive symptoms, although they are significant, do not have an important effect size. This finding implies that other genetic, clinical, and environmental factors may influence the intensity of depressive symptoms.
This study provides evidence in the Chilean population regarding the clinical complexity presented by patients seeking help for depression in PHCs. Within this complexity, the presence of psychiatric comorbidity associated with the biographical history of trauma becomes important for its influence on the depressive symptom severity at baseline.
Although current clinical guidelines for treatment of depression in Chile deliver recommendations based on the ICD-10, psychiatric comorbidities and adverse events are often underdiagnosed and inadequately treated in PHCs.15,46 In this sense, the evidence found in this study merits incorporating new strategies aimed at the recognition of psychiatric comorbidity and its relation to biographical adverse events in depressive patients presenting to PHCs.
Submitted: September 17, 2016; accepted February 16, 2017.
Published online: May 4, 2017.
Potential conflicts of interest: None.
Funding/support: Funding for this study was received from CONICYT-Chile through project FONIS SA13/ 20135: “Factors associated with the different evolutions by patients admitted to GES depression in primary care region VII; following a cohort.” The sponsor was the University of Talca, Talca, Chile.
Role of the sponsor: The sponsor approved the project and provided funding for its development.
REFERENCES
1. World Health Organization. Depression fact sheet no. 369. 2012. WHO website. http://www.who.int/mediacentre/factsheets/fs369/es.
2. Kessler RC, Merikangas KR, Wang PS. Prevalence, comorbidity, and service utilization for mood disorders in the United States at the beginning of the twenty-first century. Annu Rev Clin Psychol. 2007;3:137–158. PubMed doi:10.1146/annurev.clinpsy.3.022806.091444
3. Vicente B, Kohn R, Rioseco P, et al. Lifetime and 12-month prevalence of DSM-III-R disorders in the Chile psychiatric prevalence study. Am J Psychiatry. 2006;163(8):1362–1370. PubMed doi:10.1176/ajp.2006.163.8.1362
4. MINSAL. National Health Survey, ENS, 2009–2011. Santiago, Chile: Ministry of Health Chile Government; 2011.
5. Araya R, Alvarado R, Sepúlveda R, et al. Lessons from scaling up a depression treatment program in primary care in Chile. Rev Panam Salud Publica. 2012;32(3):234–240. PubMed doi:10.1590/S1020-49892012000900009
6. MINSAL. Clinical Guide for the Treatment of People with Depression. Santiago, Chile: Ministry of Health, Chile Government; 2013.
7. Salvo G L. Magnitude, impact and recommended management strategies for depression, with reference to Chile. Rev Med Chil. 2014;142(9):1157–1164. PubMed doi:10.4067/S0034-98872014000900010
8. Alvarado R, Vega J, Sanhueza G, et al. Evaluation of the program for depression detection, diagnosis, and comprehensive treatment in primary care in Chile [in Spanish]. Rev Panam Salud Publica. 2005;18(4–5):278–286. PubMed doi:10.1590/S1020-49892005000900008
9. Alvarado R, Rojas G. Evaluation of the program for detection and treatment of depression in Chilean primary health care centers [in Spanish]. Rev Med Chil. 2011;139(5):592–599. PubMed doi:10.4067/S0034-98872011000500005
10. Lamers F, Beekman AT, de Jonge P, et al. One-year severity of depressive symptoms: results from the NESDA study. Psychiatry Res. 2011;190(2-3):226–231. PubMed doi:10.1016/j.psychres.2011.07.005
11. World Health Organization. Clinical descriptions and diagnostic guidelines. ICD-10: International Classification of Diseases. 10th ed. Madrid, Spain: Ediciones Meditor; 1992.
12. Howland RH, Rush AJ, Wisniewski SR, et al. Concurrent anxiety and substance use disorders among outpatients with major depression: clinical features and effect on treatment outcome. Drug Alcohol Depend. 2009;99(1–3):248–260. PubMed doi:10.1016/j.drugalcdep.2008.08.010
13. Lamers F, van Oppen P, Comijs HC, et al. Comorbidity patterns of anxiety and depressive disorders in a large cohort study: the Netherlands Study of Depression and Anxiety (NESDA). J Clin Psychiatry. 2011;72(3):341–348. PubMed doi:10.4088/JCP.10m06176blu
14. Nanni V, Uher R, Danese A. Childhood maltreatment predicts unfavorable course of illness and treatment outcome in depression: a meta-analysis. Am J Psychiatry. 2012;169(2):141–151. PubMed doi:10.1176/appi.ajp.2011.11020335
15. Hirschfeld RM. The comorbidity of major depression and anxiety disorders: recognition and management in primary care. Prim Care Companion J Clin Psychiatry. 2001;3(6):244–254. PubMed doi:10.4088/PCC.v03n0609
16. Sigurdardottir S, Halldorsdottir S. Repressed and silent suffering: consequences of childhood sexual abuse for women’s health and well-being. Scand J Caring Sci. 2013;27(2):422–432. PubMed doi:10.1111/j.1471-6712.2012.01049.x
17. Fava M, Rush AJ, Alpert JE, et al. What clinical and symptom features and comorbid disorders characterize outpatients with anxious major depressive disorder: a replication and extension. Can J Psychiatry. 2006;51(13):823–835. PubMed doi:10.1177/070674370605101304
18. Douglas KM, Porter RJ. The effect of childhood trauma on pharmacological treatment response in depressed inpatients. Psychiatry Res. 2012;200(2–3):1058–1061. PubMed doi:10.1016/j.psychres.2012.06.015
19. Johnstone JM, Luty SE, Carter JD, et al. Childhood neglect and abuse as predictors of antidepressant response in adult depression. Depress Anxiety. 2009;26(8):711–717. PubMed doi:10.1002/da.20590
20. Nemeroff CB, Heim CM, Thase ME, et al. Differential responses to psychotherapy versus pharmacotherapy in patients with chronic forms of major depression and childhood trauma. Proc Natl Acad Sci U S A. 2003;100(24):14293–14296. PubMed doi:10.1073/pnas.2336126100
21. Sheehan DV, Lecrubier Y, Sheehan KH, et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry. 1998;59(suppl 20):22–33, quiz 34–57. PubMed
22. Marshall RD, Schneier FR, Lin SH, et al. Childhood trauma and dissociative symptoms in panic disorder. Am J Psychiatry. 2000;157(3):451–453. PubMed doi:10.1176/appi.ajp.157.3.451
23. Cuneo C, Gonzalez I, Jara M, et al. External Validation of the Trauma Marshall Scale. Trauma—Infant–Juvenile and Adult Psychopathology, 1st ed. Chapter 9. Bogota, Columbia: Andes University; 2005.
24. Weil K, Florenzano R, Vitriol V, et al. Child battering and adult psychopathology: an empiric study. Rev Med Chil. 2004;132(12):1499–1504. PubMed
25. Vitriol VG, Ballesteros ST, Florenzano RU, et al. Evaluation of an outpatient intervention for women with severe depression and a history of childhood trauma. Psychiatr Serv. 2009;60(7):936–942. PubMed doi:10.1176/ps.2009.60.7.936
26. Sarason IG, Johnson JH, Siegel JM. Assessing the impact of life changes: development of the Life Experiences Survey. J Consult Clin Psychol. 1978;46(5):932–946. PubMed doi:10.1037/0022-006X.46.5.932
27. Páez D, et al. Salud Mental y Factores Psicosociales. Madrid, Spain: Fundamentos; 1986.
28. Illanes E, Bustos L, Vizcarra B, et al. Social and familial determinants of anxiety and depressive symptoms in middle to low income women [in Spanish]. Rev Med Chil. 2007;135(3):326–334. PubMed doi:10.4067/S0034-98872007000300007
29. Ramos-Brieva JA, Cordero-Villafafila A. A new validation of the Hamilton Rating Scale for Depression. J Psychiatr Res. 1988;22(1):21–28. PubMed doi:10.1016/0022-3956(88)90024-6
30. Thaipisuttikul P, Ittasakul P, Waleeprakhon P, et al. Psychiatric comorbidities in patients with major depressive disorder. Neuropsychiatr Dis Treat. 2014;10(10):2097–2103. PubMed
31. Vitriol V, Cancino A, Weil K, et al. Depression and psychological trauma: an overview integrating current research and specific evidence of studies in the treatment of depression in public mental health services in Chile [published online February 17, 2014]. Depress Res Treat. doi:10.1155/2014/608671 PubMed
32. Spinhoven P, Elzinga BM, Hovens JG, et al. The specificity of childhood adversities and negative life events across the life span to anxiety and depressive disorders. J Affect Disord. 2010;126(1-2):103–112. PubMed doi:10.1016/j.jad.2010.02.132
33. Bernet CZ, Stein MB. Relationship of childhood maltreatment to the onset and course of major depression in adulthood. Depress Anxiety. 1999;9(4):169–174. PubMed doi:10.1002/(SICI)1520-6394(1999)9:4<169::AID-DA4>3.0.CO;2-2
34. Hovens JG, Wiersma JE, Giltay EJ, et al. Childhood life events and childhood trauma in adult patients with depressive, anxiety and comorbid disorders vs controls. Acta Psychiatr Scand. 2010;122(1):66–74. PubMed doi:10.1111/j.1600-0447.2009.01491.x
35. Korkeila J, Vahtera J, Nabi H, et al. Childhood adversities, adulthood life events and depression. J Affect Disord. 2010;127(1–3):130–138. PubMed doi:10.1016/j.jad.2010.04.031
36. Millett LS, Kohl PL, Jonson-Reid M, et al. Child maltreatment victimization and subsequent perpetration of young adult intimate partner violence: an exploration of mediating factors. Child Maltreat. 2013;18(2):71–84. PubMed doi:10.1177/1077559513484821
37. Teicher MH, Samson JA. Childhood maltreatment and psychopathology: a case for ecophenotypic variants as clinically and neurobiologically distinct subtypes. Am J Psychiatry. 2013;170(10):1114–1133. PubMed doi:10.1176/appi.ajp.2013.12070957
38. Spijker J, de Graaf R, Ten Have M, et al. Predictors of suicidality in depressive spectrum disorders in the general population: results of the Netherlands Mental Health Survey and Incidence Study. Soc Psychiatry Psychiatr Epidemiol. 2010;45(5):513–521. PubMed doi:10.1007/s00127-009-0093-6
39. Hayashi Y, Okamoto Y, Takagaki K, et al. Direct and indirect influences of childhood abuse on depression symptoms in patients with major depressive disorder. BMC Psychiatry. 2015;15:244. doi:10.1186/s12888-015-0636-1 PubMed
40. Nemeroff CB, Binder E. The preeminent role of childhood abuse and neglect in vulnerability to major psychiatric disorders: toward elucidating the underlying neurobiological mechanisms. J Am Acad Child Adolesc Psychiatry. 2014;53(4):395–397. PubMed doi:10.1016/j.jaac.2014.02.004
41. Heim C, Nemeroff CB. The role of childhood trauma in the neurobiology of mood and anxiety disorders: preclinical and clinical studies. Biol Psychiatry. 2001;49(12):1023–1039. PubMed doi:10.1016/S0006-3223(01)01157-X
42. Vitriol V, Cancino A, Leiva-Bianchi M, et al. Childhood trauma and psychiatric comorbidities in patients with depressive disorder in primary care in Chile. J Trauma Dissociation. 2017;18(2):189–205. doi:10.1080/15299732.2016.1212449 PubMed
43. Smith DJ, Court H, McLean G, et al. Depression and multimorbidity: a cross-sectional study of 1,751,841 patients in primary care. J Clin Psychiatry. 2014;75(11):1202–1208, quiz 1208. PubMed doi:10.4088/JCP.14m09147
44. Katon W, Lin EH, Kroenke K. The association of depression and anxiety with medical symptom burden in patients with chronic medical illness. Gen Hosp Psychiatry. 2007;29(2):147–155. PubMed doi:10.1016/j.genhosppsych.2006.11.005
45. van Dijke A, Ford JD, van der Hart O, et al. Childhood traumatization by primary caretaker and affect dysregulation in patients with borderline personality disorder and somatoform disorder [published online March 28, 2011]. Eur J Psychotraumatol. 2011;2. 10.3402/ejpt.v2i0.5628 PubMed
46. Combs H, Markman J. Anxiety disorders in primary care. Med Clin North Am. 2014;98(5):1007–1023. PubMed doi:10.1016/j.mcna.2014.06.003
This PDF is free for all visitors!


