Open Trial of Brief Behavioral Activation Psychotherapy for Depression in an Integrated Veterans Affairs Primary Care Setting
Objective: Major depressive disorder (MDD) is highly prevalent and impairing and highly likely to present in primary care settings. Recent efforts by the Department of Veterans Affairs (VA) have sought to integrate mental health services into primary care settings, leading to new specialty pharmacotherapy and psychotherapy treatment options for primary care patients. However, little is known about the effectiveness of these new services in primary care patients with MDD. The present study investigated the effectiveness of a brief, easy-to-administer, evidence-based psychotherapy behavioral activation in an integrated mental health/primary care setting in a southeastern VA medical center during the first year of the program.
Method: Thirty-five veterans with MDD (DSM-IV criteria) completed an initial clinical intake, were given the Mini International Neuropsychiatric Interview, and began a 4-week behavioral activation program. Patients also completed the Hospital Anxiety and Depression Scale (HADS) at intake, posttreatment, and at 1-month follow-up. The study was conducted from November 2009 to November 2010.
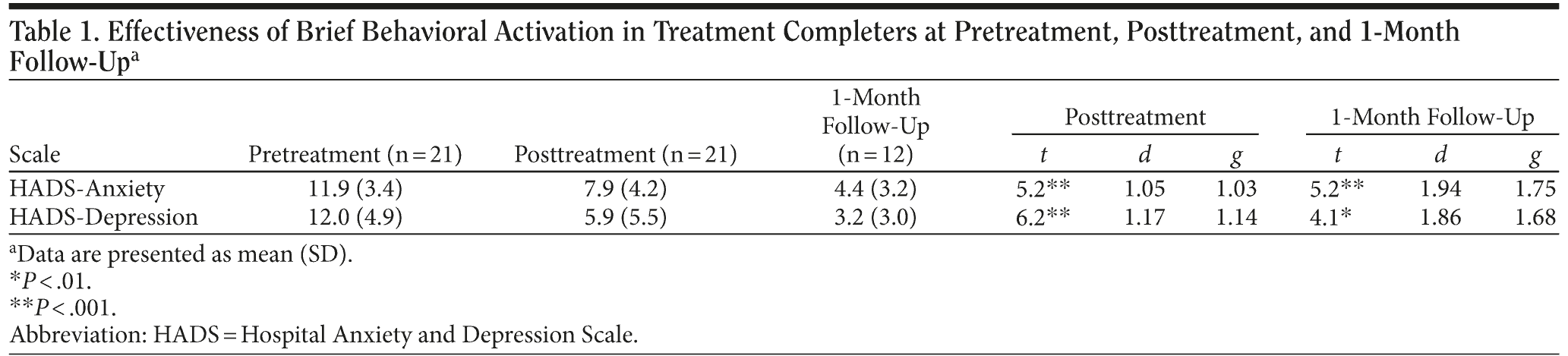
Results: Sixty percent (n = 21) of patients completed the brief behavioral activation. Treatment completers demonstrated significant reductions in symptoms of both anxiety and depression on the HADS at posttreatment (t values > 5.2, P values < .001, d values > 1.16, g values > 1.02) and follow-up (t values > 4.0, P values < .01, d values > 1.74, g values > 1.67) when compared to pretreatment levels.
Conclusions: The present findings support the use of behavioral activation as an effective treatment for patients with MDD in a primary care setting. These findings suggest that new integrated primary care settings should incorporate behavioral activation to offer brief, evidence-based treatments that provide reliable symptom reductions in addition to possible reductions in treatment needs and better management of related physical health conditions.
Prim Care Companion CNS Disord 2011;13(4):doi:10.4088/PCC.11m01136
© Copyright 2011 Physicians Postgraduate Press, Inc.
Submitted: January 10, 2011; accepted March 7, 2011.
Published online: July 21, 2011 (doi:10.4088/PCC.11m01136).
Corresponding author: Daniel F. Gros, PhD, Mental Health Service 116, Ralph H. Johnson VAMC, 109 Bee St, Charleston, SC 29401 ([email protected]).
Major depressive disorder (MDD) is highly prevalent in primary care settings, presenting in between 10% to 30% of patients.1-3 MDD is associated with disability, functional impairment, and an impact on physical health.4-6 MDD also is related to increased use of health care resources in addition to increased mortality across all age groups.7-9 Although highly prevalent and impairing, the recognition and treatment of MDD in primary care settings has been challenging, leading to both poorer health outcomes and demand for new coordinated, integrated services for MDD within primary care settings.1,10,11
In an attempt to address these concerns, the Veterans Health Administration and Department of Veterans Affairs (VA) have sought to integrate mental health care in primary care settings through the development of colocated/collaborative care models in which mental health professionals are embedded directly in primary care.11 The primary goals of these programs are to increase mental health care access and rates of treatment, improve treatment adherence, enhance clinical and functional outcomes, and improve cost-effectiveness of care. These programs also seek to ease or even avoid the referral process for specialty mental health services that can result in low rates of patient follow-up.12
Clinical Points
- Integration of mental health services directly into primary care settings has received growing support in the literature.
- In the present study, brief behavioral activation psychotherapy for depression was found to be effective in reducing symptoms of depression and anxiety in a Veterans Affairs integrated primary care setting.
- Clinicians should support and encourage the integration of brief evidence-based psychotherapies into primary care settings to improve patient mental health outcomes within the settings that these patients are most likely to present.
In VA primary care settings, routine screening for MDD, posttraumatic stress disorder, substance use disorders, and military sexual trauma already are mandated. If veterans screen positive, colocated mental health providers, including psychiatrists, psychologists, social workers, and/or psychiatric nurses, provide immediate evaluation and treatment recommendations. However, many questions still remain regarding the effectiveness of these integrated treatments, in particular the psychotherapeutic treatments. While psychopharmacologic treatments can be administered relatively quickly and already are common in most primary care settings, evidence-based psychotherapeutic options may be more complicated, typically involving intensive training for staff and weekly appointments for several months for patients.10 Interestingly, when given a choice, there is a general preference for psychological over pharmacologic interventions across a variety of disorders and studies.13
One appealing psychotherapeutic option for integrated primary care settings may be behavioral activation for depression. As reviewed by Hopko and colleagues14 and Jacobson and colleagues,15 behavioral activation is based on early behavioral models that suggest that decreases in positive reinforcement of healthy behaviors are associated with the development of depressive affect.16-18 In general, behavioral activation treatment models involve teaching patients to monitor their mood and daily activities with the goal of increasing pleasant, reinforcing activities and reducing unpleasant events.19 Behavioral activation is a brief treatment (ranging between 2 to 20 sessions), can be administered in either individual or group formats, and has demonstrated reliable effectiveness across a wide range of university, community, and civilian clinical samples with depression.19,20 In addition, recent research has supported the feasibility of training primary care providers in similar cognitive-behavioral therapies (CBT).21 However, to date, there is limited research on behavioral activation for MDD in primary care settings,22 and even less with veteran samples with MDD.19
The present study investigated a brief behavioral activation protocol delivered to veterans with MDD in a colocated, integrated mental health/primary care program within a VA medical center. The study sought to extend previous findings with behavioral activation in civilian outpatient settings to VA primary care settings and therefore provide a model for continued research, dissemination, and implementation of these programs to improve outcomes for patients with MDD in primary care settings. It was hypothesized that brief behavioral activation would be effective in producing significant pretreatment to posttreatment and pretreatment to 1-month follow-up symptom reductions in VA medical center primary care patients.
METHOD
Participants
Seventy-seven veteran primary care patients were referred for mental health services within an integrated mental health/primary care (MHPC) setting in a southeastern VA medical center during the first year of the program. The study was conducted from November 2009 to November 2010. This was a naturalistic study of a new VA initiative (ie, standard clinical care); therefore, the study received exempt status by the local institutional review board and research and development committees without the requirement of informed consent.
Patient referrals were based upon patient request, primary care provider recommendation, and/or a score ≥ 10 on the 9-item Primary Health Questionnaire (PHQ-9) depression screen.23 Upon initial referral, patients met with a colocated mental health provider and completed a brief clinical interview, the Hospital Anxiety and Depression Scale (HADS),24 and the Mini International Neuropsychiatric Interview (MINI).25 On the basis of their level of impairment and interests in treatment, patients were offered a medication consultation with an MHPC psychiatrist and brief behavioral activation psychotherapy with an MHPC psychologist. Patients with more severe psychopathology and/or impairment were referred directly to more intensive interventions in the mental health clinic on the basis of a case-by-case clinical judgment (eg, bipolar disorder, personality disorders, and psychotic symptoms).
Of the 77 initial intakes, 35 patients requested behavioral activation. Of these patients, the average patient was a mean of 53.4 years old (SD = 11.2), male (65.7%, n = 23), and white (54.3%, n = 19); endorsed DSM-IV criteria for MDD (100%, n = 35); and was stabilized on an antidepressant medication (57.1%, n = 20). Forty-five percent of patients endorsed at least 1 comorbid Axis I mood, anxiety, and/or substance use disorder, with the most common being posttraumatic stress disorder (20.0%, n = 7) and generalized anxiety disorder (14.3%, n = 5). Baseline scores on the HADS-Anxiety (HADS-A, mean = 11.7, SD = 3.8) and HADS-Depression (HADS-D, mean = 11.4, SD = 4.3) subscales were indicative of the probable presence or caseness of a mood disorder.26
Prior to initiating behavioral activation, 88.6% (n = 31) of patients requested and completed a brief medication consultation with the MHPC psychiatrist. Although no medication changes were made in the majority of patients (54.3%, n = 19), several patients chose to start a new antidepressant (25.7%, n = 9), increase their existing dose of an antidepressant (11.4%, n = 4), or reduce their existing dose of an antidepressant (5.7%, n = 2). Several patients chose to begin a new medication to treat sleep disruption (11.4%, n = 4).
Procedures
All procedures were part of a new clinical initiative in the local VA medical center and were approved for research purposes by the local VA’s research and development committee and the local university’s institutional review board. Following the initial MHPC intake, all patients requesting behavioral activation were assigned to the MHPC psychologist for brief psychotherapy (2-4 sessions). As the study served as part of standard clinical practices through the VA medical center, no treatment fidelity checks were completed. However, the MHPC psychologist had over 10 years of experience delivering behavioral activation and other evidence-based psychotherapies.
Patients completed the HADS at pretreatment intake and in the final session of behavioral activation. In addition, patients who both successfully completed behavioral activation and refused additional mental health services following termination were readministered the HADS at 1-month follow-up to determine the long-term effects of the brief behavioral activation and to determine if additional treatment was needed (n = 12). Treatment completers were defined as patients who successfully completed the behavioral activation protocol altogether in 4 sessions or less on the basis of therapist and patient agreement on treatment progress and termination (treatment completers, n = 21), with the average completer attending a mean of 3.3 sessions (SD = 0.7).
Behavioral Activation
The brief behavioral activation used in the present study was consistent with the theoretical and treatment traditions outlined in the previous literature of behavior therapy for depression13-15 and more recent treatment models of behavioral activation.14 The behavioral activation protocol, developed by the authors and based on other recent models, was focused on increasing patient participation in positive, reinforcing activities to elevate one’s mood.
In the first session, psychoeducation on MDD was provided with an emphasis on the connection between MDD and withdrawal from reinforcing, positive activities and behaviors. Patients were asked to identify interesting/enjoyable activities and complete a weekly behavioral schedule with several new reinforcing activities planned each day. The remaining sessions involved (1) reviewing patients’ homework success and its influence on their general mood, (2) reinforcing the treatment model and highlighting early successes, and (3) scheduling the following week’s activities. The final session also included a readministration of the HADS and review of treatment progress, a review of the treatment model and relapse prevention skills, and a discussion of ongoing treatment options (eg, discontinue mental health treatments and return to primary care versus referral to additional, long-term services in the mental health clinic).
Measures
Mini International Neuropsychiatric Interview. The MINI is a structured diagnostic interview designed to provide a brief, but accurate, assessment of a wide range of DSM-IV disorders.25 The MINI has demonstrated adequate interrater and test-retest reliability across most disorders.25 The MINI diagnoses also demonstrated adequate concordance with other popular diagnostic interviews across most disorders.25
Hospital Anxiety and Depression Scale. The HADS is a 14-item questionnaire that assesses the symptoms of anxiety (HADS-A) and depression (HADS-D).24 All items are rated on a 4-point Likert rating scale that varies item by item and assesses symptoms “over the past week.” The HADS has been used extensively in the literature, with repeated demonstrations of its use as a reliable and valid measure of self-reported anxiety and depression.26,27 The probable presence or caseness of a mood disorder has been defined as a score ≥ 11 on the HADS-D.26
RESULTS
Treatment Completion
Differences in demographic background, medication status, changes in medications at pretreatment, and baseline symptomatology were investigated across treatment completers (n = 21) and noncompleters (n = 14). No reliable differences were found across any of the comparisons (all P > .30).
Treatment Outcome
All treatment findings for the brief behavioral activation are presented in Table 1. Paired t tests were used to investigate pretreatment to posttreatment and pretreatment to follow-up changes in each of the self-report symptom measures. As predicted, significant reductions were evidenced across both the HADS-A and HADS-D at posttreatment (t values > 5.2, P values < .001, d values > 1.16, g values > 1.02) and follow-up (t values > 4.0, P values < .01, d values > 1.74, g values > 1.67) when compared to pretreatment levels. In addition, 80% (12/15) of completers at posttreatment and 100% (7/7) of completers at follow-up evidenced a shift from above the threshold for caseness on the HADS-D to a score below the threshold. There were no reliable differences between posttreatment and follow-up on either the HADS-A or HADS-D (t values < 1.3, P values > .23). Interestingly, only 1 of the 12 patients (8.3%) requested additional mental health services at follow-up assessment.
As medication use and medication changes co-occurred with the behavioral activation intervention in some patients, analysis of covariance (ANCOVA) was used to investigate the effectiveness of behavioral activation as demonstrated by posttreatment scores across medication use (yes or no) and medication changes (yes or no), with the pretreatment scores entered as covariates. Separate ANCOVAs were run for the HADS-A and HADS-D. These analyses demonstrated that there was a significant effect of medication use on the posttreatment HADS-A (F = 4.3, P = .055, d = 0.84, g = 0.82) and HADS-D (F = 5.3, P = .035, d = 0.81, g = 0.79) scores after controlling for pretreatment scores, suggesting that patients with pretreatment medications evidenced poorer symptom reductions on both measures. There were no reliable effects for medication change on either measure (F values < 2.6, P values > .13).
DISCUSSION
Brief behavioral activation psychotherapy was administered to 35 patients within a VA integrated primary care setting by colocated providers. Although only 60% of patients completed behavioral activation, treatment completers evidenced significantly reduced symptoms of anxiety and depression at both posttreatment and 1-month follow-up. The size of the effect was similarly large as those presented in other recent preliminary investigations of behavioral activation in primary care settings.22 The present study included a larger sample size and a veteran population, supporting the generalizability of the effectiveness of behavioral activation in integrated primary care settings.
The present study also investigated the influence of medication use on the effectiveness of behavioral activation. Interestingly, the present study suggests that patients stabilized on a medication prior to behavioral activation demonstrated significantly poorer outcomes than patients who were not taking medications. Although patients were not randomized into medication conditions and thus interpretations of these findings should be tempered, there are a few possible explanations for these findings.
Although no baseline differences were present between patients with and without medications, it is possible that patients stabilized on medications were more severe and/or treatment resistant prior to baseline, received marginal improvements from the medications, and still required additional treatments. Alternatively, it is possible that the addition of pharmacotherapy reduced the effectiveness of behavioral activation. In a review of the literature, Otto and colleagues28 suggested that adding pharmacotherapy to CBT provides little, if any, benefit to treatment outcome over CBT alone in patients with acute MDD and may worsen treatment outcome in patients with anxiety disorders. Additional research is needed to better understand these findings and to inform future combinations of treatments in primary care settings.
The present findings demonstrated that an easy-to-administer psychosocial treatment led to reliable symptom reduction and reduced need for a referral to additional specialty services (only 8.3% requested additional services at 1-month follow-up). This study was the first investigation of these practices with veterans with MDD in a VA primary care setting. With the growing demands in primary care and the additional health care needs of patients with depression,1,7,29 behavioral interventions delivered to primary care patients may represent an alternative treatment that could reduce patient symptomatology quickly and therefore improve patient morbidity and mortality.21 On the basis of its demonstrated effectiveness in the present findings, brief behavioral activation has the potential to reduce physician workload by transferring care to other providers and successfully treating the symptoms of depression and anxiety that result in frequent patient visits for mental health and other related/unrelated physical health concerns. These findings are supportive of efforts by the VA and other organizations to integrate specialty mental health services directly into primary care settings to address these highly prevalent and distressing psychiatric disorders within the settings that they are most likely to present.1,11
The present study was not without its limitations. As part of a new clinical initiative at the VA medical center, the study was an open trial of behavioral activation, lacked a comparison group, and did not randomize between-subject factors such as medication use and/or changes. Although dropout rates were consistent with previous studies on psychotherapy for depression in primary care settings,30 the high rate of treatment discontinuation resulted in a small sample of treatment completers. In addition, the HADS self-report measure was administered by the treating psychologist, which could have influenced patient response. Future research should incorporate control and treatment-as-usual (eg, pharmacotherapy) groups and independent assessors blind to the treatment condition to further investigate incorporating behavioral activation into integrated primary care settings, including both treatment completion and outcome across the various groups.
CONCLUSION
The present study provided preliminary support for the effectiveness of brief behavioral activation delivered in a VA integrated primary care setting. Patients demonstrated significant reductions in symptoms of anxiety and depression from pretreatment to posttreatment, and these effects were maintained at 1-month follow-up assessments and negated the need for a referral for additional mental health services. These findings are supportive of the efforts by the VA and other organizations to integrate mental health services into primary care settings. In particular, these findings suggest that the incorporation of behavioral activation could be most beneficial in treating primary care patients with MDD.
Author affiliations: Ralph H. Johnson VAMC, Charleston and Medical University of South Carolina, Charleston, South Carolina.
Potential conflicts of interest: None reported.
Funding/support: Dr Gros is a core member of the Ralph H. Johnson VAMC Research Enhancement Award Program (REA08-261), the Center for Disease Prevention and Health Interventions for Diverse Populations. This material is the result of work supported with resources and the use of facilities at the Ralph H. Johnson VAMC.
Disclaimer: The views expressed in this article are those of the authors and do not necessarily reflect the position or policy of the Department of Veterans Affairs or the United States government.
Acknowledgment: The authors thank Julia Brown, RN, of the Mental Health Service, Ralph H. Johnson VAMC, Charleston, South Carolina, for her help in the data collection process. Ms Brown reports no conflict of interest related to the subject of this article.
REFERENCES
1. Egede LE. Failure to recognize depression in primary care: issues and challenges. J Gen Intern Med. 2007;22(5):701-703. PubMed doi:10.1007/s11606-007-0170-z
2. Spitzer RL, Williams JB, Kroenke K, et al. Utility of a new procedure for diagnosing mental disorders in primary care: the PRIME-MD 1000 study. JAMA. 1994;272(22):1749-1756. PubMed doi:10.1001/jama.272.22.1749
3. McQuaid JR, Stein MB, Laffaye C, et al. Depression in a primary care clinic: the prevalence and impact of an unrecognized disorder. J Affect Disord. 1999;55(1):1-10. PubMed doi:10.1016/S0165-0327(98)00191-8
4. Spiegel D, Giese-Davis J. Depression and cancer: mechanisms and disease progression. Biol Psychiatry. 2003;54(3):269-282. PubMed doi:10.1016/S0006-3223(03)00566-3
5. Stevens DE, Merikangas KR, Merikangas JR. Comorbidity of depression and other medical conditions. In: Beckham EE, Leber WR, eds. Handbook of Depression. 2nd ed. New York, NY: Guilford; 1995:147-199.
6. Michaud CM, Murray CJ, Bloom BR. Burden of disease: implications for future research. JAMA. 2001;285(5):535-539. PubMed doi:10.1001/jama.285.5.535
7. Greenberg PE, Stiglin LE, Finkelstein SN, et al. The economic burden of depression in 1990. J Clin Psychiatry. 1993;54(11):405-418. PubMed
8. Zheng D, Macera CA, Croft JB, et al. Major depression and all-cause mortality among white adults in the United States. Ann Epidemiol. 1997;7(3):213-218. PubMed doi:10.1016/S1047-2797(97)00014-8
9. Abas M, Hotopf M, Prince M. Depression and mortality in a high-risk population: 11-year follow-up of the Medical Research Council Elderly Hypertension Trial. Br J Psychiatry. 2002;181:123-128. PubMed
10. Wolf NJ, Hopko DR. Psychosocial and pharmacological interventions for depressed adults in primary care: a critical review. Clin Psychol Rev. 2008;28(1):131-161. PubMed doi:10.1016/j.cpr.2007.04.004
11. Zeiss AM, Karlin BE. Integrating mental health and primary care services in the Department of Veterans Affairs health care system. J Clin Psychol Med Settings. 2008;15(1):73-78. PubMed doi:10.1007/s10880-008-9100-4
12. Kilbourne AM, Pincus HA, Schutte K, et al. Management of mental disorders in VA primary care practices. Adm Policy Ment Health. 2006;33(2):208-214. PubMed doi:10.1007/s10488-006-0034-6
13. Barlow DH. Psychological treatments. Am Psychol. 2004;59(9):869-878. PubMed doi:10.1037/0003-066X.59.9.869
14. Hopko DR, Lejuez CW, Ruggiero KJ, et al. Contemporary behavioral activation treatments for depression: procedures, principles, and progress. Clin Psychol Rev. 2003;23(5):699-717. PubMed doi:10.1016/S0272-7358(03)00070-9
15. Jacobson NS, Martell CR, Dimidjian S. Behavioral activation treatment for depression: returning to contextual roots. Clin Psychol Sci Pract. 2001;8(3):255-270. doi:10.1093/clipsy/8.3.255
16. Ferster CB. A functional analysis of depression. Am Psychol. 1973;28(10):857-870. PubMed doi:10.1037/h0035605
17. Lewinsohn PM. A behavioral approach to depression. In: Friedman RM, Katz MM, eds. The Psychology of Depression: Contemporary Theory and Research. New York, NY: Wiley; 1974.
18. Lewinsohn PM, Libet J. Pleasant events, activity schedules, and depressions. J Abnorm Psychol. 1972;79(3):291-295. PubMed doi:10.1037/h0033207
19. Mazzucchelli T, Kane R, Rees C. Behavioral activation treatments for depression in adults: a meta-analysis and review. Clin Psychol Sci Pract. 2009;16(4):383-411. doi:10.1111/j.1468-2850.2009.01178.x
20. Ekers D, Richards D, Gilbody S. A meta-analysis of randomized trials of behavioural treatment of depression. Psychol Med. 2008;38(5):611-623. PubMed doi:10.1017/S0033291707001614
21. Cully JA, Teten AL, Benge JF, et al. Multidisciplinary cognitive-behavioral therapy training for the veterans affairs primary care setting. Prim Care Companion J Clin Psychiatry. 2010;12(3):e1-e8. PubMed
22. Uebelacker LA, Weisberg RB, Haggarty R, et al. Adapted behavior therapy for persistently depressed primary care patients: an open trial. Behav Modif. 2009;33(3):374-395. PubMed doi:10.1177/0145445509331924
23. Kroenke K, Spitzer RL. The PHQ-9: a new depression diagnostic and severity measure. Psychiatr Ann. 2002;32(9):1-7. PubMed
24. Zigmond AS, Snaith RP. The Hospital Anxiety and Depression Scale. Acta Psychiatr Scand. 1983;67(6):361-370. PubMed doi:10.1111/j.1600-0447.1983.tb09716.x
25. Sheehan DV, Lecrubier Y, Sheehan KH, et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry. 1998;59(suppl 20):22-33, quiz 34-57. PubMed
26. Snaith RP. The Hospital Anxiety and Depression Scale. Health Qual Life Outcomes. 2003;1(1):29. PubMed doi:10.1186/1477-7525-1-29
27. Bjelland I, Dahl AA, Haug TT, et al. The validity of the Hospital Anxiety and Depression Scale: an updated literature review. J Psychosom Res. 2002;52(2):69-77. PubMed doi:10.1016/S0022-3999(01)00296-3
28. Otto MW, Smits JAJ, Reese HE. Combined psychotherapy and pharmacotherapy for mood and anxiety disorders in adults: review and analysis. Clin Psychol Sci Pract. 2005;12(1):72-86. doi:10.1093/clipsy/bpi009
29. Yarnall KSH, Pollak KI, טstbye T, et al. Primary care: is there enough time for prevention? Am J Public Health. 2003;93(4):635-641. PubMed doi:10.2105/AJPH.93.4.635
30. Brown C, Schulberg HC, Madonia MJ, et al. Treatment outcomes for primary care patients with major depression and lifetime anxiety disorders. Am J Psychiatry. 1996;153(10):1293-1300. PubMed