This work may not be copied, distributed, displayed, published, reproduced, transmitted, modified, posted, sold, licensed, or used for commercial purposes. By downloading this file, you are agreeing to the publisher’s Terms & Conditions.
Objective: The ACCESS treatment model offers assertive community treatment embedded in an integrated care program to patients with psychoses. Compared to standard care and within a controlled study, it proved to be more effective in terms of service disengagement and illness outcomes in patients with schizophrenia spectrum disorders over 12 months. ACCESS was implemented into clinical routine and its effectiveness assessed over 24 months in severe schizophrenia spectrum disorders and bipolar I disorder with psychotic features (DSM-IV) in a cohort study.
Method: All 115 patients treated in ACCESS (from May 2007 to October 2009) were included in the ACCESS II study. The primary outcome was rate of service disengagement. Secondary outcomes were change of psychopathology, severity of illness, psychosocial functioning, quality of life, satisfaction with care, medication nonadherence, length of hospital stay, and rates of involuntary hospitalization.
Results: Only 4 patients (3.4%) disengaged with the service. Another 11 (9.6%) left because they moved outside the catchment area. Patients received a mean of 1.6 outpatient contacts per week. Involuntary admissions decreased from 34.8% in the 2 previous years to 7.8% during ACCESS (P < .001). Mixed models repeated-measures analyses revealed significant improvements among all patients in psychopathology (effect size d = 0.64, P < .001), illness severity (d = 0.84, P = .03), functioning level (d = 0.65, P < .001), quality of life (d = 0.50, P < .001), and client satisfaction (d = 0.11, P < .001). At 24 months, 78.3% were fully adherent to medication, compared to 25.2% at baseline (P = .002).
Conclusions: ACCESS was successfully implemented in clinical routine and maintained excellent rates of service engagement and other outcomes in patients with schizophrenia spectrum disorders or bipolar I disorder with psychotic features over 24 months.
Trial Registration: ClinicalTrials.gov identifier: NCT01888627
Effectiveness of Integrated Care Including Therapeutic Assertive Community Treatment in Severe Schizophrenia Spectrum and Bipolar I Disorders: The 24-Month Follow-Up ACCESS II Study

ABSTRACT
Objective: The ACCESS treatment model offers assertive community treatment embedded in an integrated care program to patients with psychoses. Compared to standard care and within a controlled study, it proved to be more effective in terms of service disengagement and illness outcomes in patients with schizophrenia spectrum disorders over 12 months. ACCESS was implemented into clinical routine and its effectiveness assessed over 24 months in severe schizophrenia spectrum disorders and bipolar I disorder with psychotic features (DSM-IV) in a cohort study.
Method: All 115 patients treated in ACCESS (from May 2007 to October 2009) were included in the ACCESS II study. The primary outcome was rate of service disengagement. Secondary outcomes were change of psychopathology, severity of illness, psychosocial functioning, quality of life, satisfaction with care, medication nonadherence, length of hospital stay, and rates of involuntary hospitalization.
Results: Only 4 patients (3.4%) disengaged with the service. Another 11 (9.6%) left because they moved outside the catchment area. Patients received a mean of 1.6 outpatient contacts per week. Involuntary admissions decreased from 34.8% in the 2 previous years to 7.8% during ACCESS (P < .001). Mixed models repeated-measures analyses revealed significant improvements among all patients in psychopathology (effect size d = 0.64, P < .001), illness severity (d = 0.84, P = .03), functioning level (d = 0.65, P < .001), quality of life (d = 0.50, P < .001), and client satisfaction (d = 0.11, P < .001). At 24 months, 78.3% were fully adherent to medication, compared to 25.2% at baseline (P = .002).
Conclusions: ACCESS was successfully implemented in clinical routine and maintained excellent rates of service engagement and other outcomes in patients with schizophrenia spectrum disorders or bipolar I disorder with psychotic features over 24 months.
Trial Registration: ClinicalTrials.gov identifier: NCT01888627
J Clin Psychiatry 2014;75(12):1371-1379
© Copyright 2014 Physicians Postgraduate Press, Inc.
Submitted: September 30, 2013; accepted February 18, 2014.
Online ahead of print: August 19, 2014 (doi:10.4088/JCP.13m08817).
Corresponding author: Daniel Schöttle, MD, Department of Psychiatry and Psychotherapy, Psychosis Centre, Centre of Psychosocial Medicine, University Medical Center Hamburg-Eppendorf, Martinistr 52, 20246 Hamburg, Germany ([email protected]).
In recent years, researchers and practitioners have increasingly realized that mental health services should be adapted to and targeted at those suffering from severe mental illness, particularly from schizophrenia spectrum disorders and bipolar disorder.1 It is particularly concerning that patients with schizophrenia spectrum disorders and bipolar disorders tend to have high rates of nonadherence and service disengagement varying between 23% and 30% even in specialized early psychosis programs.2,3
Various diagnosis-nonspecific outpatient care models have been developed to treat patients with severe mental illness (eg, community mental health teams,4 intensive case management,5 and assertive community treatment).6-9
Most previous assertive community treatment studies10 have included patients with various psychiatric disorders. However, assertive community treatment teams in many studies lack diagnostic specialization. This may or may not reduce quality of care. Furthermore, there are few studies in which assertive community treatment was embedded into specialized integrated care. This approach may be of great importance, as other studies without such integrated care found no (major) differences between assertive community treatment and standard care nor sustained improvement after discontinuation.
To this end, our group implemented and evaluated an integrated care treatment model including assertive community treatment (ACCESS model) for patients with schizophrenia spectrum disorders.6,11 Compared to a reference catchment area offering standard care, the ACCESS I study showed a markedly better 1-year efficacy of the ACCESS model at comparable costs of both treatments. Furthermore, patients treated in ACCESS were less extensively hospitalized (11 days vs 33 days in standard care). Importantly, the service disengagement rate was much lower in ACCESS (6.3%) compared to standard care (23.2%) within 1 year.11
On the basis of these positive results, in May 2007, the ACCESS model was implemented in routine care in collaboration with health insurance agencies. The ACCESS was concurrently extended to patients with bipolar I disorder with psychotic features. Additionally, slightly more rigid inclusion criteria led to the inclusion of more severely ill patients. The ACCESS II study was designed as a pragmatic cohort study to continuously evaluate the effectiveness of the ACCESS model under real-life conditions in schizophrenia spectrum disorders and in bipolar I disorder with psychotic features.
We report the 2-year results of the ACCESS II study. We were particularly interested in whether the ACCESS model produced comparably low service disengagement rates and hospital days under real-life conditions in both schizophrenia spectrum disorders and bipolar I disorder with psychotic features over the extended period of 2 years. We also compare schizophrenia spectrum disorders and bipolar I disorder with psychotic features with regard to improvements of psychopathology, social functioning, quality of life, satisfaction with care, compulsory admissions, and medication adherence.
METHOD
Context, Design, and Sample
The Psychosis Center of the University Medical Center Hamburg-Eppendorf is responsible for the treatment of adult patients with severe schizophrenia spectrum disorders or bipolar I disorder with psychotic features in an urban catchment area of 300,000 inhabitants.
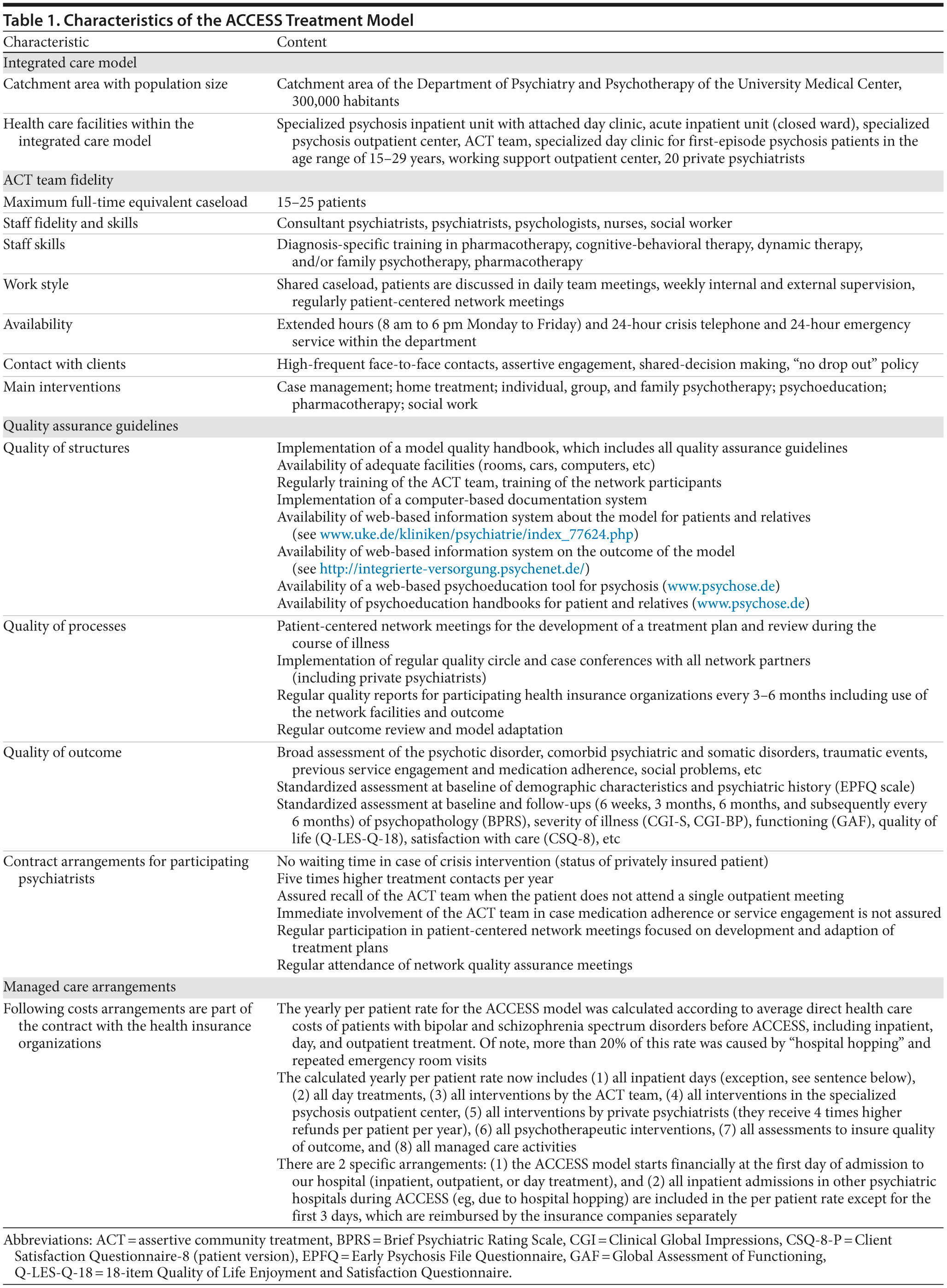
The ACCESS treatment model is described in detail in Lambert et al6 and did not differ from the originally used treatment model, with the exception that the newly included bipolar I disorder with psychotic features patients received psychopharmacology and psychotherapy specific for bipolar I disorder with psychotic features. The main characteristics of the integrated care concept, including details on assertive community treatment and quality assurance measures, are outlined in Table 1. Compared to traditional assertive community treatment models for severe mental illness, the model was specifically aimed at the treatment of psychotic disorders. All team members were trained and experienced in cognitive-behavioral therapy, dynamic therapy, and/or family psychotherapy.
From May 2007 to October 2009, 115 patients with schizophrenia spectrum disorders or bipolar I disorder with psychotic features and severe mental illness were treated in the ACCESS model. Of all eligible patients, 4.5% refused treatment in the ACCESS model. All treated patients participated in the assessments, which were administered as part of the clinical routine. Furthermore, all gave informed consent for these data to be used in the context of the ACCESS II study whenever they were sufficiently stabilized. The local institutional review board approved the study (registration number: PV4059). The study was registered at ClinicalTrials.gov (identifier: NCT01888627).

- The ACCESS model was successfully implemented in routine care in patients with schizophrenia spectrum disorders and bipolar I disorder with psychotic features.
- Low rates of service disengagement, a significant decrease in involuntary admissions, and significant improvements regarding secondary outcomes were achieved.
- Two important factors beyond the principles of assertive community treatment could be related to the successful implementation: first, the embedment of assertive community treatment in an integrated care program allowing need-adapted treatments and, second, the expertise of the assertive community treatment team, including their commitment to psychotherapy and family involvement.
Inclusion and Exclusion Criteria
The following new inclusion criteria for treatment in ACCESS under real-life conditions were chosen to ensure treatment for patients with severe psychotic disorders:
- Diagnosis of a schizophrenia spectrum disorder (ie, schizophrenia, schizophreniform disorder, schizoaffective disorder, delusional disorder, or psychotic disorder not otherwise specified) or bipolar disorder with psychotic features, all assessed with the Structured Clinical Interview for DSM-IV Axis I Disorders (SCID-I)12;
- Aged ≥ 18 years;
- Present confinement for hospitalization because of an acute illness state as assessed by a psychiatrist;
- Presence of a certain severity of illness as assessed with the Brief Psychiatric Rating Scale, 24-item version (BPRS),13 with (1) BPRS total score > 40 points and (2) fulfillment of 1 of the following 8 criteria: ≥ 6 points on item 10 (hallucinations); ≥ 6 points on item 11 (unusual thought content); ≥ 6 points on item 15 (conceptual disorganization); ≥ 10 total points on items 3 and 4 (depressive-suicidal syndrome); ≥ 6 points on item 4 (suicidality); ≥ 15 total points on items 8, 9, and 21 (manic syndrome); ≥ 15 total points on items 6, 12, and 20 (disruptive behavior syndrome); or ≥ 15 total points on items 13, 16, and 17 (negative syndrome). Psychotic disorders due to a medical condition were excluded.
In contrast to the ACCESS I study, bipolar patients were included in the ACCESS II study, the rate of first-episode patients was lower, and 1 inclusion criterion of the ACCESS I study, ie, “multiple-episode patients required that patients had at least 1 psychotic relapse with subsequent hospitalization caused by medication nonadherence within the last 24 months,” was omitted. Furthermore, initial antipsychotic treatment was not restricted to quetiapine as it was the case in the ACCESS I study.
Assessments and Measures
Assessments were carried out at baseline, week 6, and months 3, 6, 12, 18, and 24 by trained raters independent of the treatment team to avoid bias.
Diagnosis of the psychotic disorder and comorbid Axis I disorder(s) was assessed with the SCID-I.12 The main outcome, service disengagement for nonpractical reasons, was considered to be present if a patient repeatedly refused further treatment despite need and several attempts at reengagement (phone calls to patient and potential home visits from the assertive community treatment team).2 Service use data were systematically assessed.
Furthermore, at baseline, the following variables were assessed: sociodemographic, functional, and pretreatment characteristics with the German version of the Early Psychosis File Questionnaire14 and employment/occupation at entry and ability of independent living with the Modified Vocational Status Index15 and the Modified Location Code Index.15 “Employed/occupied” comprised paid or unpaid full- or part-time employment or being an active student in university or full- or part-time volunteer; “independent living” comprised living alone, with a partner, or with peers. Homeless patients with bipolar I disorder with psychotic features and schizophrenia spectrum disorders were, by definition of the catchment area, treated in a different hospital and thus not included in ACCESS. Durations of untreated psychosis and untreated illness were assessed with the Duration of Untreated Psychosis Scale.16-18 Prevalence of previous inpatient treatment and any involuntary admission in lifetime and within 2 years before ACCESS was assessed by interviewing patients, relatives, and health service staff previously responsible for the respective patient. Data were validated by cross checking the hospital database. Involuntary admissions were due to danger to self or others.
Medication adherence was assessed by using the criteria of Kane et al.19 Therapists rated their patients as being fully adherent in the last 4 weeks if they were taking ≥ 80% of the prescribed medication, partially adherent if they were taking 20%-80% of the prescribed medication, and nonadherent if they were taking ≤ 20% of the prescribed medication.
At baseline and follow-up time points, the following structured assessments were applied:
- psychopathology with the BPRS at baseline and every 6 months;
- severity of illness with the Clinical Global Impressions-Severity of Illness scale (CGI-S)20;
- level of functioning with the Global Assessment of Functioning (GAF) scale21;
- quality of life with the 18-item Quality of Life Enjoyment and Satisfaction Questionnaire (Q-LES-Q-18).22 The Q-LES-Q-18 is a self-report instrument scored on a 5-point scale, with higher scores indicating better enjoyment and satisfaction with specific life domains. A score of 4.1 points characterizes good quality of life (healthy controls);
- patients’ satisfaction with care with the Client Satisfaction Questionnaire (CSQ-8),23 an 8-item instrument scored from 1 to 4 per item. The mean item score is computed; and
- medication adherence (see previous paragraph).19
All raters received extensive training, particularly for SCID-I interviews, BPRS, CGI-S, and GAF.
Fidelity to the assertive community treatment model was assessed yearly with the Dartmouth Assertive Community Treatment Scale.24 At initiation of ACCESS, the total score was 4.5 and varied yearly between 4.2 and 4.6 points, indicating that fidelity to the model was good.
Statistical Analysis
Descriptive analyses consisted of absolute and relative frequencies in categorical variables and either means and standard deviations (SDs) or medians with upper and lower quartile for continuous variables.
Baseline differences between diagnostic groups (schizophrenia spectrum disorders and bipolar I disorder with psychotic features) were assessed by using an independent-samples t test when the dependent variable was continuous. There are 2 Tweedie-distributed,25 ie, ties at 0, variables (duration of untreated psychosis and untreated illness), which were evaluated by Mann-Whitney U test. Categorical variables were assessed with χ2 tests.
To compare baseline with the 24-month follow-up for the binary outcomes (involuntary admissions, full adherence with medication, employment/occupation, living independently), we used McNemar test.
We evaluated the changes from baseline (admission) in mixed model repeated measures, considering the follow-up times as repeated measures, the patients as the random effect, the group (if applicable) and time as fixed effects, and the baseline values of the dependent variable as covariates. Outcomes were changes from baseline in BPRS total score, CGI-S score, GAF, Q-LES-Q-18, and CSQ-P. We examined the interaction between time and diagnostic group (if applicable). In every model, the interaction was not significant. Therefore, we eliminated the interaction in the resulting models.
We used the baseline values as covariates to minimize the variance.26 The main effects (F), significance levels (P), and effect sizes (d) are reported. Effect sizes (d) were calculated by dividing the differences of adjusted mean scores by the standard deviation of residuals.27
Level of significance was set at P < .05 (2-sided hypothesis). Statistical analyses were performed with SPSS Version 20.0 (IBM Corp, 2011).
RESULTS
Baseline Characteristics
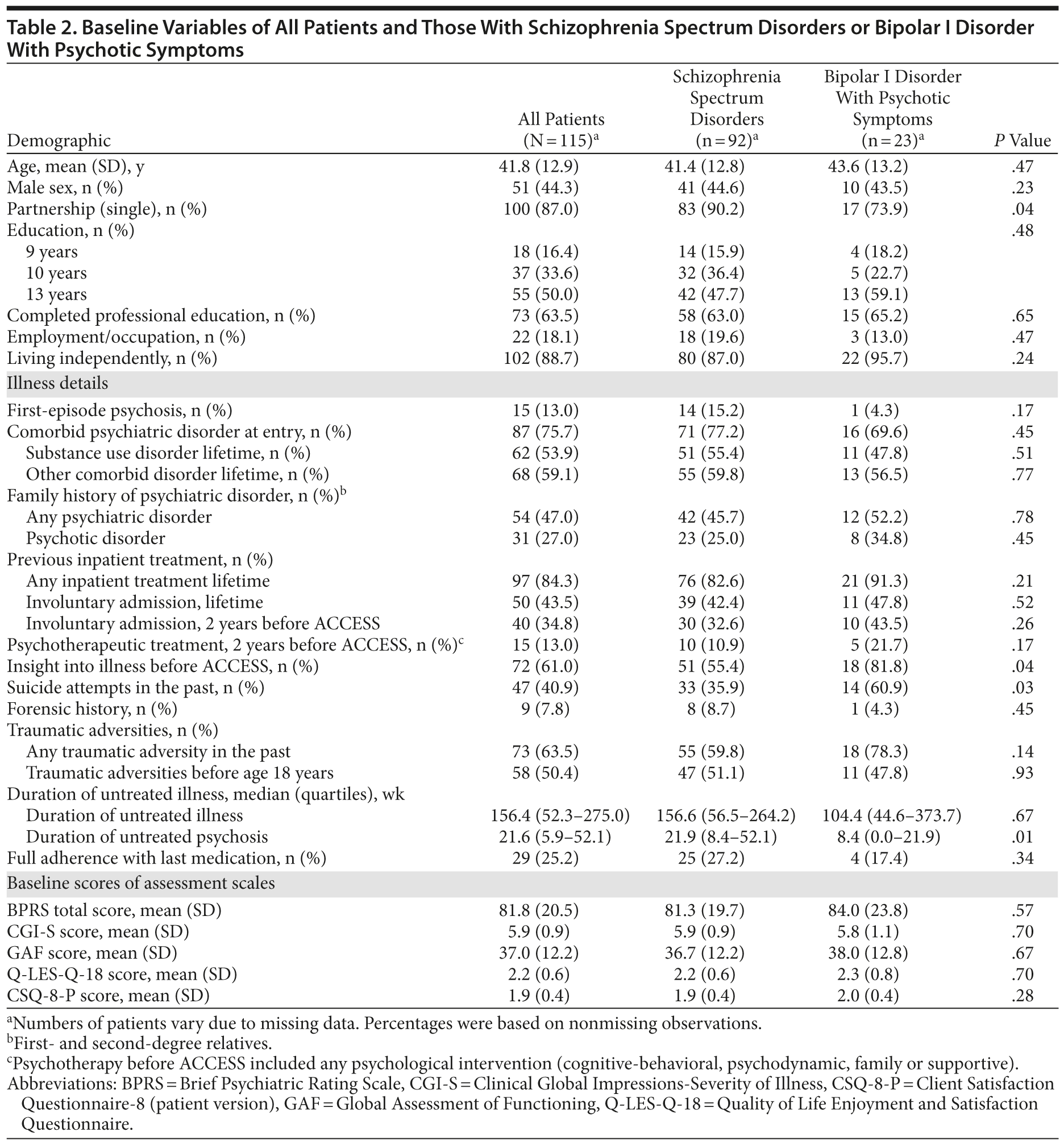
One hundred fifteen patients with schizophrenia spectrum disorders or bipolar I disorder with psychotic features (44.3% male; mean age = 41.8 years [SD = 12.9]) were treated in the ACCESS model and participated in the ACCESS II study. Baseline details are displayed in Table 2. Patients with both schizophrenia spectrum disorders (n = 92) and bipolar I disorder with psychotic features (n = 23) were severely ill (high CGI-S and BPRS scores and low GAF scores). Quality of life and satisfaction with care before entry into the ACCESS treatment model were low; 43.5% of all patients had involuntary admissions to inpatient treatment in the past, and only 25.2% (n = 29) were adherent to their most recent medication. As expected, patients with schizophrenia spectrum disorders and bipolar I disorder with psychotic features had similar baseline characteristics, except that those with schizophrenia spectrum disorders had a longer duration of untreated psychosis, fewer previous suicide attempts, and less insight into illness. Only 15 of 115 patients (13%) had received psychotherapeutic treatment in the 2 years before admission.
Service Use
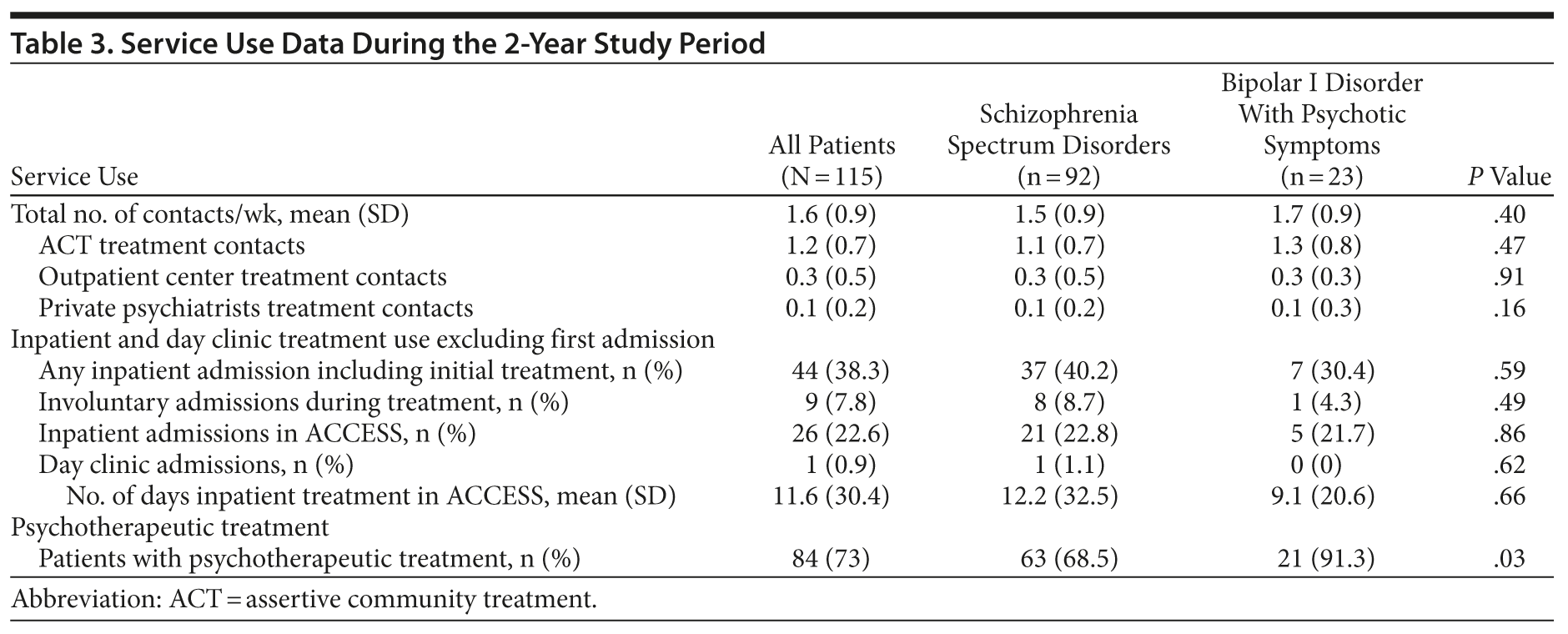
Service use data are displayed in Table 3. Within the 24-month treatment period, 26 patients (22.6%) were hospitalized, and 1 patient (0.9%) received day treatment. The mean duration of inpatient treatment was 11.6 days. Rates of involuntary admissions declined significantly (n = 9, 7.8%) compared to those at 2 years before ACCESS (n = 40, 34.8%; McNemar test, P < .001).
Patients received a mean of 162.3 (SD = 92.5) treatment contacts within 2 years (1.6 contacts per week). The assertive community treatment team conducted most contacts. Eighty-four patients (73%) received psychotherapeutic treatment conducted by the assertive community treatment team or private psychotherapists. A significantly higher percentage of patients with bipolar I disorder with psychotic features than patients with schizophrenia spectrum disorders received psychotherapy (91.3% vs 68.5%; McNemar test, P = .03).
Service Disengagement
Over the 24-month treatment period, 4 patients (3.4%) were service disengaged after a median of 36.9 weeks (quartiles: 17.64-78.90): 1 patient (1.1%) in the group with schizophrenia spectrum disorders after 22.6 weeks and 3 patients (13.0%) in the group with bipolar I disorder with psychotic features after a median of 51.1 weeks (range, 16.0-88.14). Furthermore, 11 patients (9.6%) dropped out of the study due to practical reasons (moved out of catchment area) after a median duration of treatment of 53.7 weeks (range, 5.4-96.6).
Secondary Outcomes in Schizophrenia Spectrum Disorders and Bipolar I Disorder With Psychotic Features
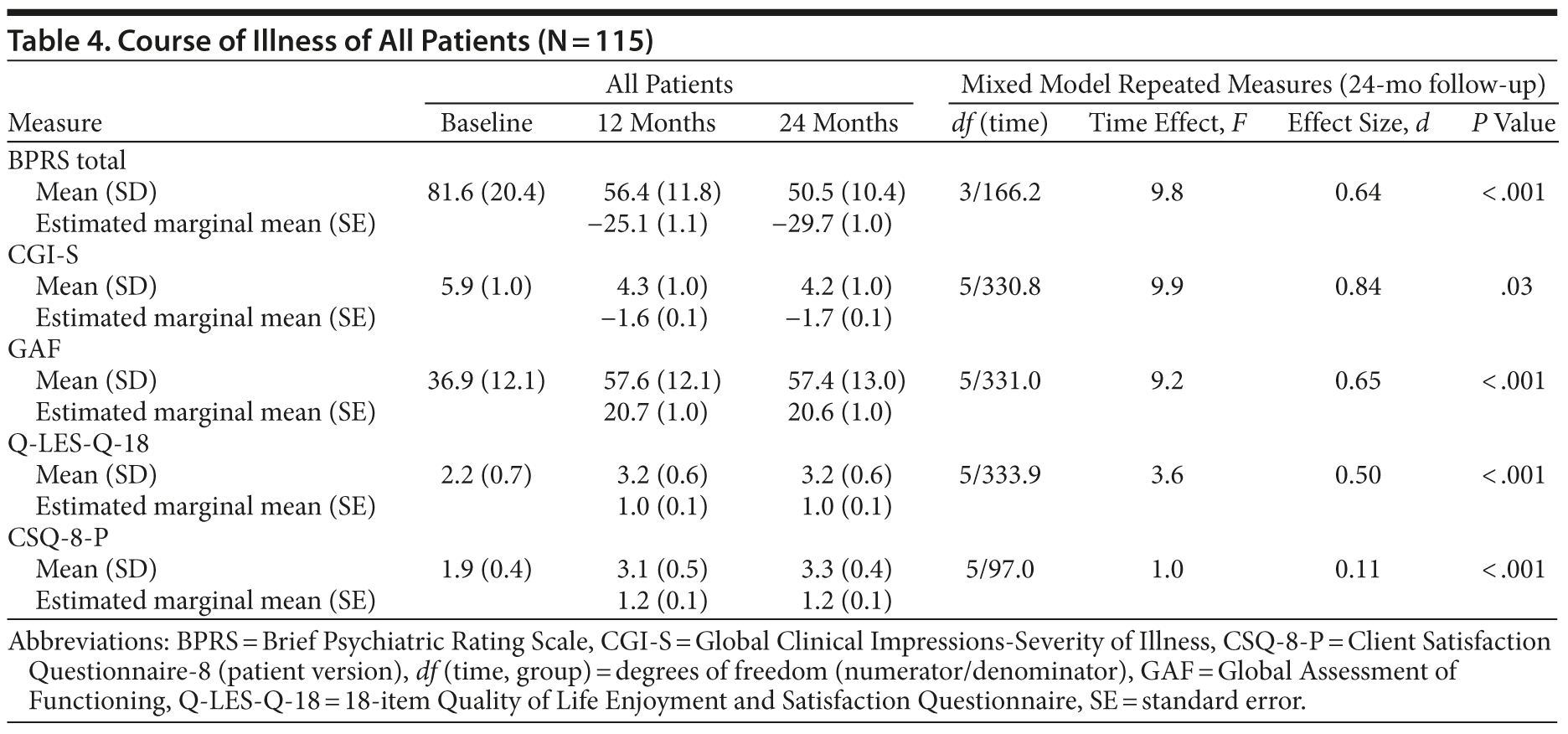
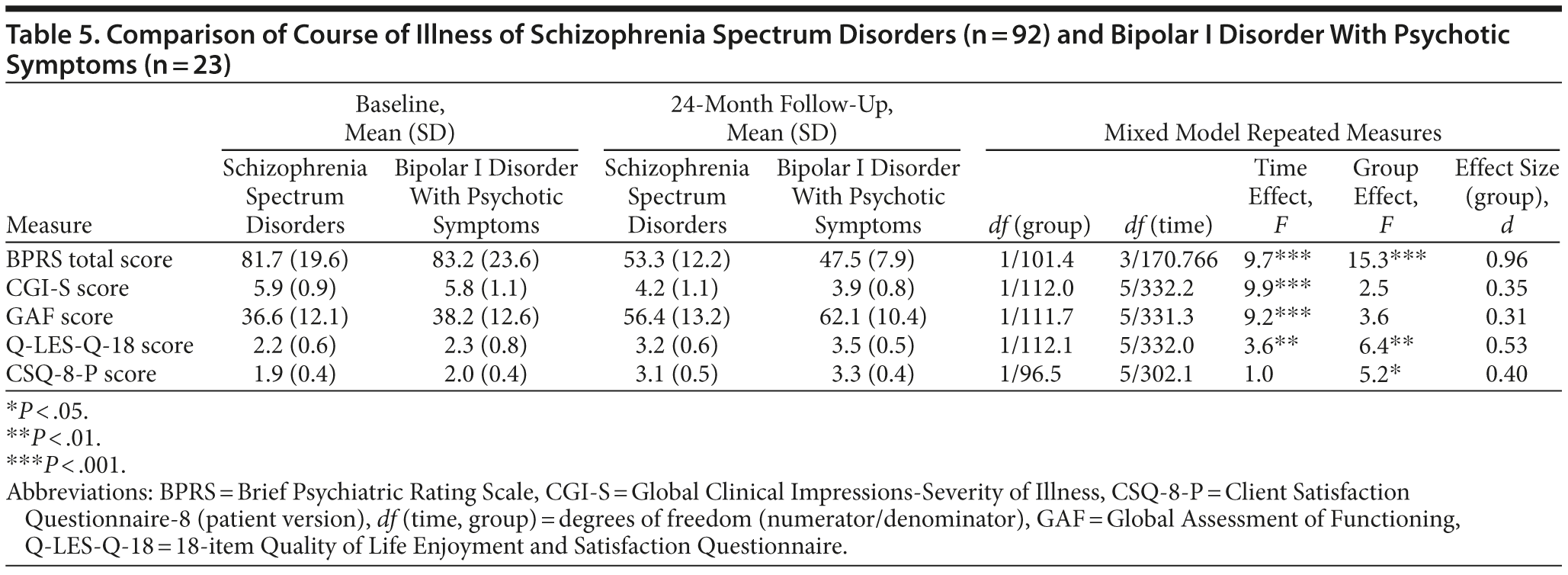
At 24-month follow-up, 78.3% were fully adherent compared to 25.2% at baseline (McNemar test, P = .002), with no differences between schizophrenia spectrum disorders and bipolar I disorder with psychotic features. All follow-up assessments indicated improved psychopathology, illness severity, global functioning, and quality of life (Table 4). Larger improvements in psychopathology and quality of life as denoted by medium to large effect sizes were detected in bipolar I disorder with psychotic features (Table 5). Significant improvements in test scores occurred during the first 18 months on the BPRS, during the first 6 months on the CGI-S and GAF, within the first 3 months on the Q-LES-Q-18, and during the first 6 weeks on the CSQ-8. After these time points, no further significant changes were detected and improvements were sustained. Furthermore, significantly more patients were employed/occupied after 24 months (n = 32, 28.3% vs 18.1% at baseline; McNemar test, P = .02), while rates of living independently remained stable (n = 93, 82.3% vs 88.7% at baseline) with no significant differences between schizophrenia spectrum disorders and bipolar I disorder with psychotic features.
The CSQ-8 scores indicated a significantly better than baseline satisfaction with care, with a mean rating of “good” at 12- and 24-month follow-ups. Satisfaction with treatment improved significantly more in patients with bipolar I disorder with psychotic features than in patients with schizophrenia spectrum disorders.
DISCUSSION
The ACCESS treatment model was created to offer assertive community treatment embedded in an integrated care program to patients with schizophrenia spectrum disorders. Compared to standard care, and within research settings, it proved to be more effective in terms of service disengagement, medication adherence, and improvements in secondary outcomes. Further, fewer inpatient days but more outpatient treatment contacts were used.6 This model was incorporated into clinical routine and its effectiveness assessed with the ACCESS II study over 24 months in a new sample of patients with schizophrenia spectrum disorders and bipolar I disorder with psychotic features. This is important, as many treatment effects in research settings are not sustained under “real-life” conditions.28,29 One reason is the exclusion of more severely ill patients with more complex treatment needs in research settings.28 Furthermore, it is often unclear whether treatment effects can be sustained for longer periods. In line with these common limitations, the generalizability of the ACCESS I study was limited by the inclusion of less severely ill patients, the fact that all patients were treated with quetiapine at study entry, and limited follow-up time (1 year). With the implementation of ACCESS into routine care, more severely ill patients and patients with bipolar I disorder with psychotic features were included, and no specific antipsychotic treatment was mandatory. The Dartmouth Assertive Community Treatment Scale scores indicated that fidelity to assertive community treatment principles was as good as in ACCESS I.
Patients received intensive outpatient treatment at 1.6 contacts per week on average. The mean duration of inpatient treatment during ACCESS was very low considering the high severity of illness and common inpatient treatment before ACCESS (87.6%). This indicates a high level of stabilization resulted from this intensive assertive community treatment-based integrated care program. Service use data did not differ between patients with schizophrenia spectrum disorders and bipolar I disorder with psychotic features, except that significantly more patients with bipolar I disorder with psychotic features received psychotherapy, which may be due to a specific group psychotherapy treatment offered to most patients with bipolar I disorder with psychotic features.
Key Findings
The service disengagement rate was extremely low at 3.4% over 24 months and even lower than in the ACCESS I study (6.3%). It should be noted, however, that an additional 11 patients (9.6%) were disengaged for moving out of the catchment area. Some of these patients moved to sheltered homes due to their high need for care (n = 5). Counting these as service disengaged, nevertheless, even at a disengagement rate of 13% over 24 months, the adherence to ACCESS was excellent and comparable to the ACCESS I study. A good, yet lower, service engagement rate was reported by other assertive community treatment studies,6,7,9,30 which, however, included patients with less severe illness. Patients with less severe illness and little improvement tend to have lower rates of service engagement than those with severe illness.31 Yet, in ACCESS, those patients whose psychopathology improved during treatment also remained in treatment. The positive effect of assertive community treatment on sustained service engagement may be explained by the high team fidelity, lower and shared case load, higher contact frequency, no drop-out policy, 24-hour-per-day availability, and possibility of visiting patients in the community, especially if at risk for disengagement. Furthermore, psychotherapeutic orientation and intensive involvement of family members or significant others (open dialogue) may have strengthened the therapeutic alliance. Additional factors that may explain the high service engagement rate are the longstanding dialogue between our service and self-help groups as well as our general approach of active involvement of patients toward recovery. All these factors may also explain the much lower number of involuntary admissions compared to the 2 years prior to ACCESS treatment, the low number of inpatient days (at least in schizophrenia spectrum disorders compared to the benchmark of 63 days/2 years in this catchment area),6 and the higher rates of medication adherence compared to baseline.
Further, patients were more satisfied with ACCESS than with their previous treatment. This is important, as satisfaction with treatment is closely related to service engagement.
Overall, patients’ psychopathology, illness severity, global functioning, and quality of life improved, with medium to large effect sizes. Patients with bipolar I disorder with psychotic features had larger improvements in psychopathology and quality of life than patients with schizophrenia spectrum disorders, a finding in line with the literature.32-34 Improvements occurred within the first 6 months, except for psychopathology, which improved further over 18 months.
Regardless of diagnosis, many patients lived independently at baseline and follow-ups (> 80%), despite their high severity of illness and low baseline employment/occupation rate. The high baseline rate of independent living may be explained by the fact that most of our patients had no support from sheltered homes and, thus, were severely ill enough to fulfill the inclusion criteria of ACCESS, while those living in sheltered homes already received enough support to be treated with standard (mostly outpatient) care.35 The high rate of continuous independent living during ACCESS may be viewed as a success of ACCESS and related to the intensive work with significant others.
Strength and Limitations
The real-life setting led to the inclusion of patients that were too ill for study participation in a (randomized) controlled trial. A team of experts in the treatment of psychotic disorders provided the intervention with a focus on psychotherapy. The 2-year follow-up time allowed for the assessment of sustained effects beyond initial improvements.
The main inherent limitation is the absence of a control group. Instead, comparisons with findings of the controlled ACCESS I study were made. The Dartmouth Assertive Community Treatment Scale showed comparable adherence to the principles of assertive community treatment. Another unavoidable limitation was the nonblinded assessment of patients. We used experienced raters to assure assessment quality and to reduce—but not to fully avoid—social desirability bias in patients’ answers and too positive ratings of psychopathology. Our main outcome—service disengagement—was not biased by social desirability or nonblinded assessments. However, the external assessments themselves may have further increased service engagement. As the sample size of the bipolar I disorder with psychotic features group is rather small, analyses of differences between schizophrenia spectrum disorders and bipolar I disorder with psychotic features may be underpowered and should therefore be interpreted with caution. Also, the representativeness of the sample may be limited by the exclusion of homeless patients, who were—by definition of the catchment area—treated elsewhere. Furthermore, we cannot rule out the possibility that important confounders were not assessed, among those the specific effect of antipsychotic or mood stabilizer treatment on outcomes.
CONCLUSION
The ACCESS treatment model was confirmed to be efficacious in a clinical routine setting for patients with severe and mostly multiple-episode schizophrenia spectrum disorders and bipolar I disorder with psychotic features over 24 months. In our clinical experience, the high rate of service engagement as well as improvements in psychopathology, functioning, and quality of life may be related to 2 important factors beyond the principles of assertive community treatment. These are the embedment of assertive community treatment in an integrated care program allowing need-adapted treatments and the expertise of the assertive community treatment team in treating psychoses, including their commitment to psychotherapy and family involvement. The specific effect of psychotherapy and family involvement on service engagement needs further study.
Drug names: quetiapine (Seroquel and others).
Author affiliations: Psychosis Centre, Department of Psychiatry and Psychotherapy (Drs Schöttle, Karow, Bussopulos, Nika, Schödlbauer, Lange, Bock, and Lambert; Mss Ruppelt, Sauerbier, Frieling, and Kerstan; and Mr Golks), Department of Psychiatry and Psychotherapy (Drs Ohm, Meigel-Schleiff, Naber, and Wiedemann; and Mr Lange), University Center of Psychosocial Medicine, and Department of Medical Biometry and Epidemiology (Dr Wegscheider and Ms Daubmann), University Medical Center, Hamburg-Eppendorf, Germany; and University Hospital of Child and Adolescent Psychiatry, University of Bern, Bern, Switzerland (Dr Schimmelmann).
Author contributions: Drs Schöttle and Schimmelmann contributed equally to the study.
Potential conflicts of interest: Dr Schöttle has received honoraria from AstraZeneca. Dr Schimmelmann has served on speakers or advisory boards of AstraZeneca, Bristol-Meyers Squibb, Eli Lilly, Janssen, and Novartis. Dr Karow has received honoraria from and serves on speakers boards of AstraZeneca. Dr Lambert has received grant/research support from and served on speakers or advisory boards of AstraZeneca and has received honoraria from AstraZeneca, Eli Lilly, Janssen-Cilag, and Bristol-Myers Squibb. Dr Naber has received grant/research support and honoraria from and has served on speakers or advisory boards of AstraZeneca. Dr Wiedemann has served on speakers or advisory boards of Janssen and Otsuka. Drs Bussopulos, Nika, Schödlbauer, Wegscheider, Lange, Meigel-Schleiff, and Bock; Mss Ruppelt, Sauerbier, Frieling, Kerstan, Daubmann, and Ohm; and Mssrs Golks and Lange report no conflicts of interest.
Funding/support: None reported.
Acknowledgments: The authors express their gratitude to all participating patients and private psychiatrists who were involved in the ACCESS program.
REFERENCES
1. Ruggeri M, Leese M, Thornicroft G, et al. Definition and prevalence of severe and persistent mental illness. Br J Psychiatry. 2000;177(2):149-155. PubMed doi:10.1192/bjp.177.2.149
2. Conus P, Lambert M, Cotton S, et al. Rate and predictors of service disengagement in an epidemiological first-episode psychosis cohort. Schizophr Res. 2010;118(1-3):256-263. PubMed doi:10.1016/j.schres.2010.01.032
3. Stowkowy J, Addington D, Liu L, et al. Predictors of disengagement from treatment in an early psychosis program. Schizophr Res. 2012;136(1-3):7-12. PubMed doi:10.1016/j.schres.2012.01.027
4. Malone D, Newron-Howes G, Simmonds S, et al. Community mental health teams (CMHTs) for people with severe mental illnesses and disordered personality. Cochrane Database Syst Rev. 2007;(3):CD000270. PubMed
5. Dieterich M, Irving CB, Park B, et al. Intensive case management for severe mental illness. Cochrane Database Syst Rev. 2010;(10):CD007906. PubMed
6. Lambert M, Bock T, Schöttle D, et al. Assertive community treatment as part of integrated care versus standard care: a 12-month trial in patients with first- and multiple-episode schizophrenia spectrum disorders treated with quetiapine immediate release (ACCESS trial). J Clin Psychiatry. 2010;71(10):1313-1323. PubMed doi:10.4088/JCP.09m05113yel
7. Marshall M, Lockwood A. Assertive community treatment for people with severe mental disorders. Cochrane Database Syst Rev. 2000;(2):CD001089. PubMed
8. Stein LI, Test MA. Alternative to mental hospital treatment, 1: conceptual model, treatment program, and clinical evaluation. Arch Gen Psychiatry. 1980;37(4):392-397. PubMed doi:10.1001/archpsyc.1980.01780170034003
9. Sytema S, Wunderink L, Bloemers W, et al. Assertive community treatment in the Netherlands: a randomized controlled trial. Acta Psychiatr Scand. 2007;116(2):105-112. PubMed doi:10.1111/j.1600-0447.2007.01021.x
10. Schöttle D, Karow A, Schimmelmann BG, et al. Integrated care in patients with schizophrenia: results of trials published between 2011 and 2013 focusing on effectiveness and efficiency. Curr Opin Psychiatry. 2013;26(4):384-408. PubMed doi:10.1097/YCO.0b013e328361ec3b
11. Karow A, Reimer J, König HH, et al. Cost-effectiveness of 12-month therapeutic assertive community treatment as part of integrated care versus standard care in patients with schizophrenia treated with quetiapine immediate release (ACCESS trial). J Clin Psychiatry. 2012;73(3):e402-e408. PubMed doi:10.4088/JCP.11m06875
12. First MB, Spitzer RL, Miriam G, et al. Structured Clinical Interview for DSM-IV-TR Axis I Disorders, Research Version, Patient Edition. (SCID-I/P). New York, NY: Biometrics Research, New York State Psychiatric Institute; 2002.
13. Overall J, Gorham D. The Brief Psychiatric Rating scale. Psychol Rep. 1962;10(3):799-812. doi:10.2466/pr0.1962.10.3.799
14. Lambert M, Conus P, Cotton S, et al. Prevalence, predictors, and consequences of long-term refusal of antipsychotic treatment in first-episode psychosis. J Clin Psychopharmacol. 2010;30(5):565-572. PubMed doi:10.1097/JCP.0b013e3181f058a0
15. Tohen M, Hennen J, Zarate CM Jr, et al. Two-year syndromal and functional recovery in 219 cases of first-episode major affective disorder with psychotic features. Am J Psychiatry. 2000;157(2):220-228. PubMed doi:10.1176/appi.ajp.157.2.220
16. McGorry PD, Copolov DL, Singh BS. Royal Park Multidiagnostic Instrument for Psychosis, part 1: rationale and review. Schizophr Bull. 1990;16(3):501-515. PubMed doi:10.1093/schbul/16.3.501
17. McGorry PD, Singh BS, Copolov DL, et al. Royal Park Multidiagnostic Instrument for Psychosis, part 2: development, reliability, and validity. Schizophr Bull. 1990;16(3):517-536. PubMed doi:10.1093/schbul/16.3.517
18. Schimmelmann BG, Huber CG, Lambert M, et al. Impact of duration of untreated psychosis on pre-treatment, baseline, and outcome characteristics in an epidemiological first-episode psychosis cohort. J Psychiatr Res. 2008;42(12):982-990. PubMed doi:10.1016/j.jpsychires.2007.12.001
19. Kane JM, Leucht S, Carpenter D, et al; Expert Consensus Panel for Optimizing Pharmacologic Treatment of Psychotic Disorders. The expert consensus guideline series. Optimizing pharmacologic treatment of psychotic disorders: introduction: methods, commentary, and summary. J Clin Psychiatry. 2003;64(suppl 12):5-19. PubMed
20. Guy W. Clinical global impressions scale. Assessment Manual for Psychopharmacology. US Department of Health, Education and Welfare publication (ADM) 76-338. Rockville, MD: National Institute for Mental Health; 1976.
21. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition. Washington, DC: American Psychiatric Association; 1994.
22. Ritsner M, Kurs R, Gibel A, et al. Validity of an abbreviated quality of life enjoyment and satisfaction questionnaire (Q-LES-Q-18) for schizophrenia, schizoaffective, and mood disorder patients. Qual Life Res. 2005;14(7):1693-1703. PubMed doi:10.1007/s11136-005-2816-9
23. Nguyen TD, Attkisson CC, Stegner BL. Assessment of patient satisfaction: development and refinement of a service evaluation questionnaire. Eval Program Plann. 1983;6(3-4):299-313. PubMed doi:10.1016/0149-7189(83)90010-1
24. Teague GB, Bond GR, Drake RE. Program fidelity in assertive community treatment: development and use of a measure. Am J Orthopsychiatry. 1998;68(2):216-232. PubMed doi:10.1037/h0080331
25. J׸rgensen, B. Exponential dispersion models. J R Stat Soc Series B Stat Methodol. 1987; B49(2), 127-162
26. Vickers AJ, Altman DG. Statistics notes: analysing controlled trials with baseline and follow up measurements. BMJ. 2001;323(7321):1123-1124. PubMed doi:10.1136/bmj.323.7321.1123
27. Cortina J, Nouri H. Effect Size for ANOVA Designs. Thousand Oaks, CA: Sage Publications; 2000.
28. Depp C, Lebowitz BD. Clinical trials: bridging the gap between efficacy and effectiveness. Int Rev Psychiatry. 2007;19(5):531-539. PubMed doi:10.1080/09540260701563320
29. Weiss AP, Guidi J, Fava M. Closing the efficacy-effectiveness gap: translating both the what and the how from randomized controlled trials to clinical practice. J Clin Psychiatry. 2009;70(4):446-449. PubMed doi:10.4088/JCP.08com04901
30. Killaspy H, Bebbington P, Blizard R, et al. The REACT study: randomised evaluation of assertive community treatment in north London. BMJ. 2006;332(7545):815-820. PubMed doi:10.1136/bmj.38773.518322.7C
31. Schimmelmann BG, Conus P, Schacht M, et al. Predictors of service disengagement in first-admitted adolescents with psychosis. J Am Acad Child Adolesc Psychiatry. 2006;45(8):990-999. PubMed doi:10.1097/01.chi.0000223015.29530.65
32. Benabarre A, Vieta E, Colom F, et al. Bipolar disorder, schizoaffective disorder and schizophrenia: epidemiologic, clinical and prognostic differences. Eur Psychiatry. 2001;16(3):167-172. PubMed doi:10.1016/S0924-9338(01)00559-4
33. Latalova K, Prasko J, Diveky T, et al. Quality of life in patients with bipolar disorder—a comparison with schizophrenic patients and healthy controls. Psychiatr Danub. 2011;23(1):21-26. PubMed
34. Treuer T, Tohen M. Predicting the course and outcome of bipolar disorder: a review. Eur Psychiatry. 2010;25(6):328-333. PubMed doi:10.1016/j.eurpsy.2009.11.012
35. Meng H, Schimmelmann BG, Mohler B, et al. Pretreatment social functioning predicts 1-year outcome in early onset psychosis. Acta Psychiatr Scand. 2006;114(4):249-256. PubMed doi:10.1111/j.1600-0447.2006.00773.x
This PDF is free for all visitors!