This work may not be copied, distributed, displayed, published, reproduced, transmitted, modified, posted, sold, licensed, or used for commercial purposes. By downloading this file, you are agreeing to the publisher’s Terms & Conditions.
Objective: Nonadherence is a major challenge in schizophrenia treatment. While long-acting (depot) antipsychotic medications are often recommended to address adherence problems, evidence on the comparative effectiveness of depot versus oral antipsychotics is inconsistent. We hypothesize that this inconsistency could be due to systematic differences in study design. This review evaluates the effect of study design on the comparative effectiveness of antipsychotic formulations. The optimal use of different antipsychotic formulations in a general clinical setting depends on better understanding of the underlying reasons for differences in effectiveness across research designs.
Data Sources: A PubMed literature review targeted English-language studies (2000-2011) with information on relapse, hospitalization, or all-cause discontinuation for depot and oral antipsychotic treatment arms in schizophrenia. The time frame was chosen to reflect research focused on the newer generation of antipsychotic agents. The search required at least 1 term from each of the following categories: (1) schizophrenia; (2) inject, injection, injectable, injectables, injected, depot, long-acting; and (3) iloperidone, fluphenazine, haloperidol, paliperidone, risperidone, olanzapine, asenapine, flupentixol, flupenthixol, lurasidone, clopenthixol, fluspirilene, zuclopentixol, zuclopenthixol.
Study Selection: Thirteen relevant studies were identified by 2 independent reviewers; these studies included information on 19 depot-oral comparisons.
Data Extraction: Age- and gender-adjusted risk ratios (RRs) (depot/oral) were calculated for the identified endpoints and pooled by study design (randomized controlled trial [RCT], prospective observational, and retrospective observational). Meta-analysis with random effects was used to estimate the pooled RRs, by study design. Average conversion factors between study designs were calculated as the ratios of pooled RRs.
Results: Meta-analysis of adjusted endpoints showed no apparent benefit of depot over oral formulations in RCTs, with an RR of 0.89 (P = .416). In contrast, there was a significant advantage for depot formulations in other study designs (prospective RR = 0.62 [P < .001]; retrospective RR = 0.56 [P < .001]). These imply conversion factors of 1.43 and 1.59 between RCTs and prospective and retrospective designs, respectively.
Conclusions: The comparative effectiveness of antipsychotic formulations is sensitive to research design. Depot formulations displayed significant advantages in nonrandomized observational studies, whereas in RCTs no difference was observed. The estimated conversion factors may facilitate comparison across studies.
J Clin Psychiatry
© Copyright 2013 Physicians Postgraduate Press, Inc.
Submitted: September 14, 2012; accepted March 4, 2013.
Online ahead of print: April 19, 2013 (doi:10.4088/JCP.12r08167).
Corresponding author: Noam Y. Kirson, PhD, Analysis Group, Inc, 111 Huntington Ave, 10th Fl, Boston, MA 02199 ([email protected]).
Efficacy and Effectiveness of Depot
Versus Oral Antipsychotics in Schizophrenia:
Synthesizing Results Across Different Research Designs
ABSTRACT
Objective: Nonadherence is a major challenge in schizophrenia treatment. While long-acting (depot) antipsychotic medications are often recommended to address adherence problems, evidence on the comparative effectiveness of depot versus oral antipsychotics is inconsistent. We hypothesize that this inconsistency could be due to systematic differences in study design. This review evaluates the effect of study design on the comparative effectiveness of antipsychotic formulations. The optimal use of different antipsychotic formulations in a general clinical setting depends on better understanding of the underlying reasons for differences in effectiveness across research designs.
Data Sources: A PubMed literature review targeted English-language studies (2000–2011) with information on relapse, hospitalization, or all-cause discontinuation for depot and oral antipsychotic treatment arms in schizophrenia. The time frame was chosen to reflect research focused on the newer generation of antipsychotic agents. The search required at least 1 term from each of the following categories: (1) schizophrenia; (2) inject, injection, injectable, injectables, injected, depot, long-acting; and (3) iloperidone, fluphenazine, haloperidol, paliperidone, risperidone, olanzapine, asenapine, flupentixol, flupenthixol, lurasidone, clopenthixol, fluspirilene, zuclopentixol, zuclopenthixol.
Study Selection: Thirteen relevant studies were identified by
2 independent reviewers; these studies included information on
19 depot-oral comparisons.
Data Extraction: Age- and gender-adjusted risk ratios (RRs) (depot/oral) were calculated for the identified endpoints and pooled by study design (randomized controlled trial [RCT], prospective observational, and retrospective observational). Meta-analysis with random effects was used to estimate the pooled RRs, by study design. Average conversion factors between study designs were calculated as the ratios of pooled RRs.
Results: Meta-analysis of adjusted endpoints showed no apparent benefit of depot over oral formulations in RCTs, with an RR of 0.89 (P = .416). In contrast, there was a significant advantage for depot formulations in other study designs (prospective RR = 0.62 [P < .001]; retrospective RR = 0.56 [P < .001]). These imply conversion factors of
1.43 and 1.59 between RCTs and prospective and retrospective
designs, respectively.
Conclusions: The comparative effectiveness of antipsychotic formulations is sensitive to research design. Depot formulations displayed significant advantages in nonrandomized observational studies, whereas in RCTs no difference was observed. The estimated conversion factors may facilitate comparison across studies.
J Clin Psychiatry
© Copyright 2013 Physicians Postgraduate Press, Inc.
Submitted: September 14, 2012; accepted March 4, 2013.
Online ahead of print: April 19, 2013 (doi:10.4088/JCP.12r08167).
Corresponding author: Noam Y. Kirson, PhD, Analysis Group, Inc, 111 Huntington Ave, 10th Fl, Boston, MA 02199 ([email protected]).
The cornerstone of long-term maintenance therapy of schizophrenia patients is relapse prevention. Relapse prevention is necessary—albeit not sufficient—for eventual successful rehabilitation.1 In practice, the effectiveness of maintenance antipsychotic treatment is often undermined by poor adherence to therapy. Not only is nonadherence the single greatest modifiable risk factor for relapse,2,3 it is also often undetected, resulting in lost opportunities to employ psychosocial interventions for adherence, as well as uncertainty as to the relative contribution of lack of efficacy versus adherence problems to poor outcomes.
While no single adherence intervention is universally effective, long-acting injectable (depot) formulations are considered one of the most important pharmacologic interventions available to address adherence problems in schizophrenia.4 Relative to oral formulations, long-acting depot delivery systems are thought to help maintain adherence (or delay nonadherence) in many individuals who would otherwise discontinue their oral therapy. Therefore, long-acting depot formulations are often recommended for individuals who are known to have patterns of nonadherence to oral antipsychotic medication.5,6
However, the findings in the clinical literature regarding the comparative effectiveness of depot versus oral antipsychotics in schizophrenia have been inconsistent.7–9 These findings have challenged the field to consider the proper role of long-acting depot therapy. Some argue that the widely held notion of superiority of long-acting medication is overstated.7,10,11 If so, then efforts to increase long-acting depot utilization will not yield hoped-for improvements in relapse prevention. The lack of consistent findings in the literature raises important practical questions of therapy in managing schizophrenia.
One hypothesis for the inconsistency in the literature is that the type of study design may influence the comparative effectiveness of oral and depot formulations. While identification of outcome differences based on study methods will not identify which method is “correct,” it may provide clues to further research on explanatory factors that may account for such differences. From a methodological perspective, RCTs are considered the gold standard in terms of identifying differences in treatment efficacy. RCTs avoid many of the issues associated with confounding and bias that plague observational studies. However, in a disease like schizophrenia, in which adherence is a particularly challenging aspect of disease management, a question arises as to whether RCTs adequately capture all relevant aspects of general clinical practice. For example, researchers in RCTs more carefully monitor patients’ adherence to either oral or depot treatment, ensuring that randomized treatment regimens are upheld. In addition, adherence to medications is a behavior that may be affected by patients’ knowledge that they are being observed (ie, the Hawthorne effect).12 However, in clinical practice, where the default adherence monitoring may be more lax than in RCTs, there may be differential benefits to depot patients who, by default, may be more closely monitored than their oral-therapy counterparts. These examples are mentioned not because we have evidence that these relative benefits occur. Rather, we believe that these are reasonable scientific arguments that justify further investigation into the impact of study methods in estimating relative effectiveness of depot therapy.
Prior studies have not comprehensively examined the effect of study design on the comparative effectiveness of depot and oral formulations of antipsychotics in schizophrenia. Building on a cross-design synthesis methodology13 and using meta-analysis techniques,14 this article aims to quantify the effect of study design on the comparative effectiveness of oral and depot formulations of antipsychotics in schizophrenia to facilitate comparisons across studies.
METHOD
Data Source and Study Selection
A targeted literature review was conducted using PubMed. The PubMed database was queried for publications between January 1, 2000, and December 31, 2011. The time frame was chosen to reflect research focused on the newer generation of antipsychotic agents.
The search required at least 1 term from each of the following categories: (1) schizophrenia; (2) inject, injection, injectable, injectables, injected, depot, long-acting; and (3) iloperidone, fluphenazine, haloperidol, paliperidone, risperidone, olanzapine, asenapine, flupentixol, flupenthixol, lurasidone, clopenthixol, fluspirilene, zuclopentixol, zuclopenthixol.
Abstracts of all of the studies meeting these search criteria were screened by 2 independent reviewers (W.H. and T.S.) to ensure that they met the following criteria: (1) full text was available in English, (2) the study was of human subjects, (3) schizophrenia was the primary disease area investigated, (4) both depot and oral formulations of antipsychotics of the same generation (ie, first or second generation of antipsychotics) were available, and (5) the publication was not a review article.
The full manuscripts were retrieved for studies with abstracts that met these criteria. The studies were again reviewed by the 2 reviewers to ensure that all of the above criteria were met on the basis of the full text. In addition, in order to compute comparable endpoints across studies, only studies that reported findings on relapse, hospitalization, or all-cause discontinuation were included.
Data Extraction and Statistical Analysis
The selected studies were summarized and data were extracted for reported clinical endpoints, treatment dosages, baseline characteristics, inclusion/exclusion criteria, follow-up duration, and frequency of follow-up. When reported, information on event counts and patient population in each treatment arm was used to compute risk ratios (RRs) (depot/oral; RR < 1 favors depot, representing a lower relative risk for depot formulations compared with oral formulations) for all relevant endpoints (ie, relapse, hospitalization, all-cause discontinuation). In a limited number of cases, the number of patients with a given event was derived from reported hazard rates and sample sizes.
Adjusting for Baseline Differences in Gender and Age
Using reported gender and age at baseline, we reweighted endpoints to account for demographic differences across treatment arms. Gender was adjusted on the basis of the gender distribution of schizophrenia patients in the general population. An average prevalence RR in the general population of 1.14 for gender (male/female) was used, based on figures reported by McGrath et al,15 Saha et al,16 and Perälä et al.17 The effect of gender on time to relapse was based on Robinson et al,18 risk of hospitalization by gender was based on Mortensen and Eaton,19 and time to all-cause discontinuation by gender was based on Tiihonen et al8 and Ciudad et al.20
For age, Kozma and Weiden21 report a 26.1% decline in risk of rehospitalization per 10-year increase in age. This effect was assumed to hold for relapse and discontinuation as well. Using the mean reported age at baseline, we conducted adjustment to a common age across treatment arms within each study, typically rounding to the nearest 10-year mark. As the age adjustment was based on a single estimate from the literature, we chose to limit it to a common age within each study, rather than a possibly larger adjustment across studies.
Adjustment calculations were performed separately for the depot and oral treatment groups, and RRs were recalculated. Note that adjustments could not be applied when the gender and age distributions within each treatment arm were not reported at baseline. In addition, age adjustment was conducted after RRs were adjusted for gender, assuming independence.
Meta-Analysis by Research Design
Adjusted endpoints were pooled by research design. We broadly classified studies as RCTs or observational studies, with observational studies further divided into prospective and retrospective designs. This classification corresponds to qualitative differences in the level of researcher control over patient treatment and the likelihood that patient knowledge of the study may alter behavior. Studies were defined as retrospective if the analysis was conducted after patients were treated and evaluated (often by clinicians other than those conducting the research). As such, researchers of retrospective studies had no control over patient treatment. For example, Tiihonen et al8 analyzed a study cohort identified from the Finnish National Hospital Discharge Register, linked to databases on mortality and prescription medications. Prospective observational studies were ones in which patients were followed over time to identify outcomes, although they were not randomized.
Within each study design grouping, meta-analysis with random effects14 was used to estimate the pooled RR and 95% confidence interval (CI) of all endpoints combined. Following the literature,22 heterogeneity (I2) was assessed for each study design grouping separately. The ratios of resulting point estimates were used to calculate average conversion factors between study designs.
Sensitivity Analyses and Duration Adjustment
To test the robustness of the statistical findings to the inclusion of particular studies and endpoints, various sensitivity analyses were conducted (see further detail in Results).
In addition, we tested the sensitivity of the results to the length of study follow-up. The meta-analysis described above is based on the assumption that duration had no differential effect across treatment arms within a given study, implying that the RRs were not sensitive to study duration. The sensitivity analysis addresses this assumption. Using a meta-regression technique,23 the pooled RR for each study design was adjusted to a common duration of 21.3 months (the mean of the studies included).
All analyses were conducted using Stata 12.1, Stata Corp LP, College Station, Texas.
RESULTS
Literature Review
Figure 1 summarizes the findings of the literature review. Preliminary literature search criteria resulted in 416 studies. Further refinement and systematic review of full-text versions yielded 13 relevant studies, including 5 RCTs, 4 prospective observational studies, and 4 retrospective observational studies. The studies included information on 19 depot-oral comparisons, as some studies reported findings for multiple drugs and/or endpoints.
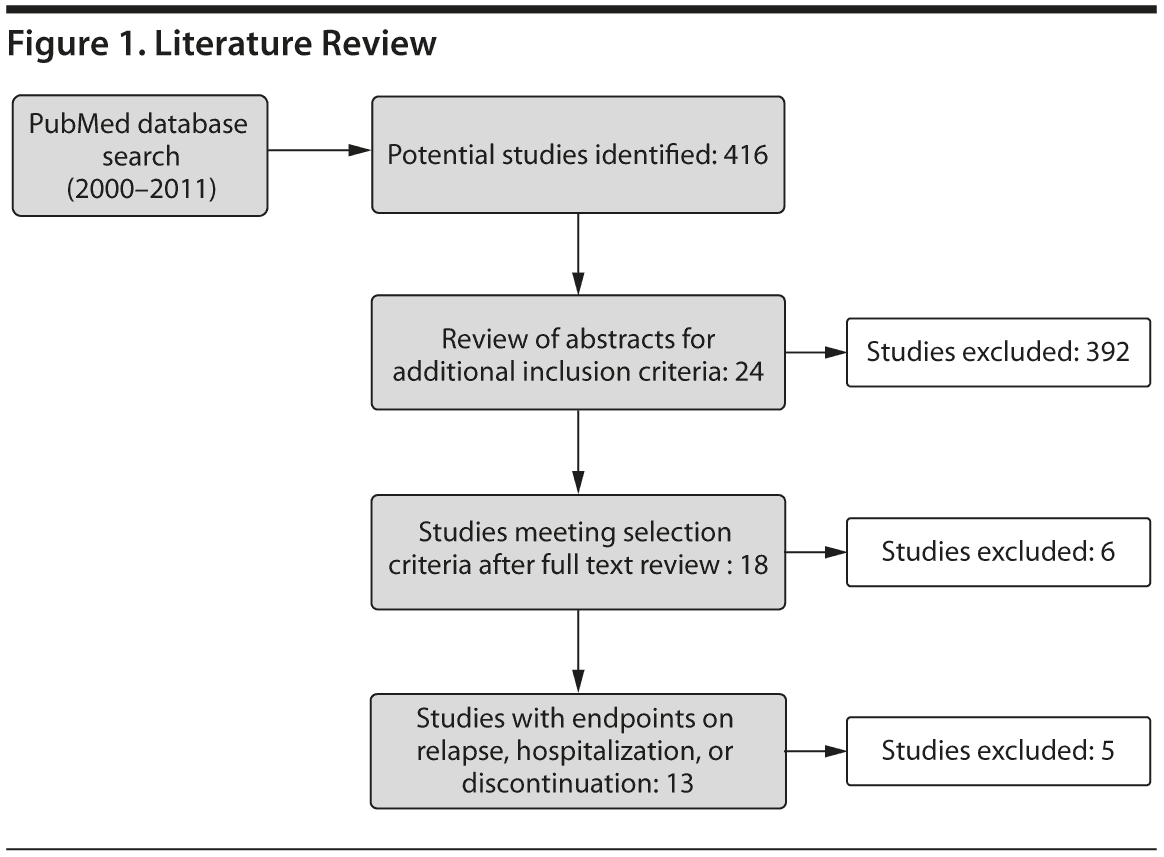
Table 1 reports key characteristics of the included studies in terms of study population, treatment arm comparisons, length of follow-up, and endpoints included. Table 2 provides a complete list of all the studies and depot-oral comparisons, grouped by research design. For each study, the relevant sample size (ie, the numbers of patients in the treatment arms of interest) and study duration are listed.

Adjusting for Baseline Differences in Gender and Age
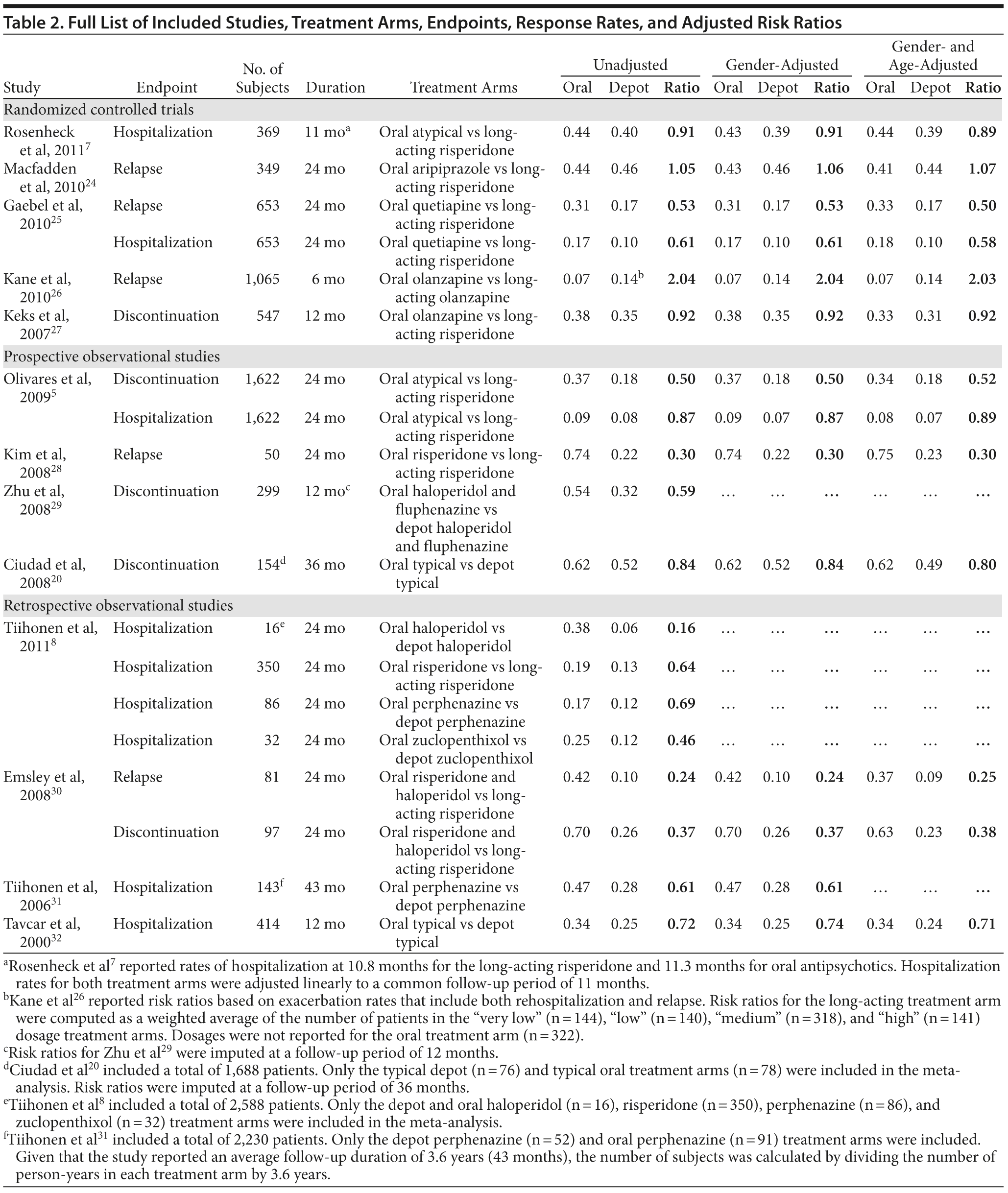
The effect of gender and age adjustment of study endpoints is described in Table 2. The table reports the absolute risks for each treatment arm and the RR prior to adjustment, followed by the adjusted figures. Note that RR < 1 reflects an advantage to depot formulations. A comparison of the adjusted and unadjusted endpoints suggests that the adjustment for gender and age had little effect on RRs.
For RCTs, the adjusted RRs range from 0.50 (Gaebel et al,25 oral quetiapine vs long-acting risperidone) to 2.03 (Kane et al,26 oral olanzapine vs long-acting olanzapine). Among prospective observational studies, adjusted RRs range from 0.30 (Kim et al,28 oral risperidone vs long-acting risperidone) to 0.89 (Olivares et al,5 oral atypical vs long-acting risperidone). Risk ratios for retrospective observational studies range from 0.16 (Tiihonen et al,8 oral haloperidol vs depot haloperidol) to 0.71 (Tavcar et al,32 oral typical vs depot typical).
Meta-Analysis by Research Design
Figure 2 reports the results of the meta-analysis of adjusted RRs by study design. Meta-analysis of adjusted endpoints resulted in an RR of 0.89 (95% CI, 0.64–1.22; P = .416) for RCTs, meaning that the null hypothesis that depot and oral formulations have similar efficacy cannot be rejected. Note that this analysis includes an adjusted RR of 2.03 from Kane et al,26 which appears to be an outlier among RCTs, possibly due to the inclusion of depot patients with a very low treatment dose (see Sensitivity Analyses).
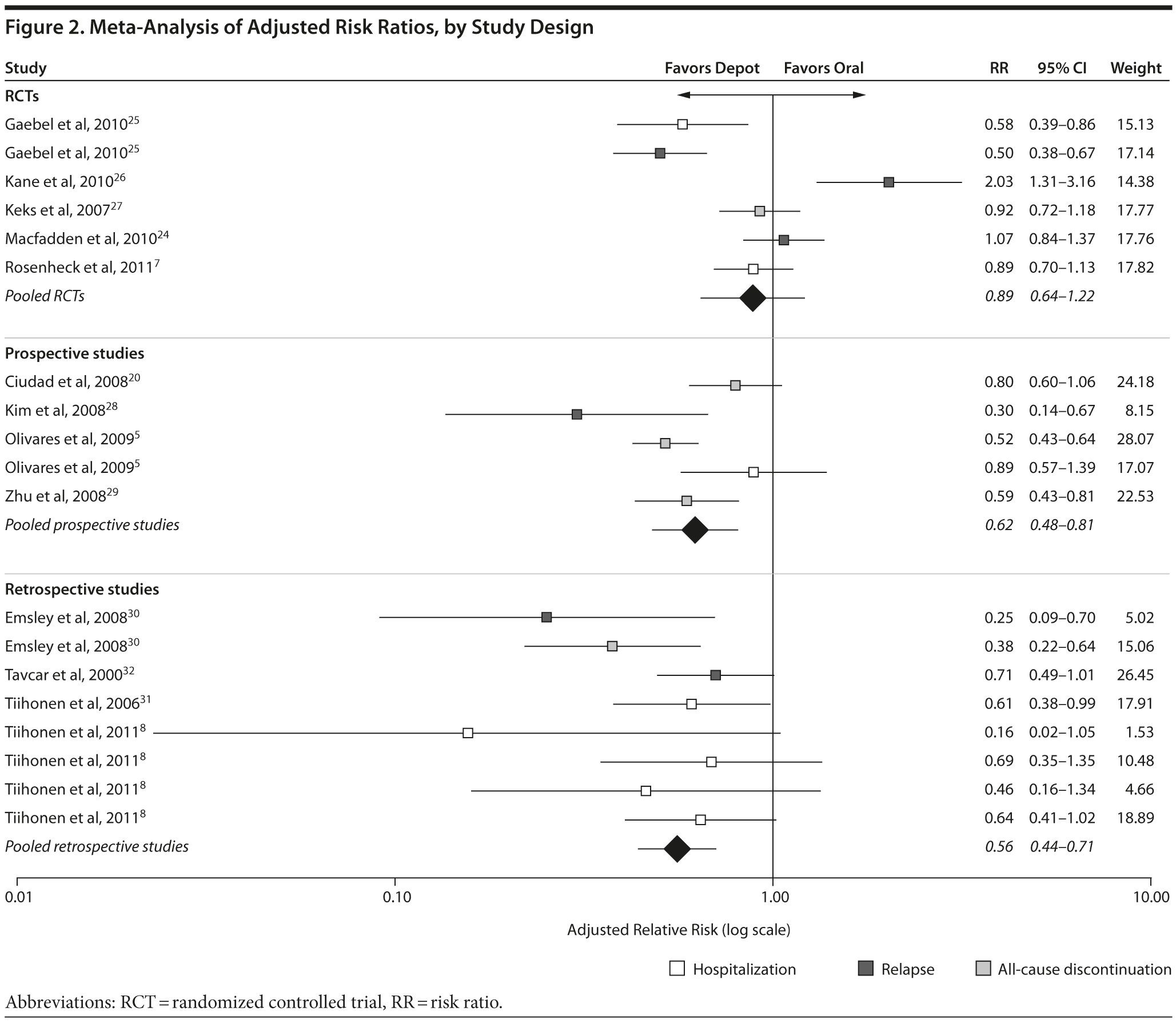
In contrast, there was a significant advantage for depot formulations in both prospective observational (RR = 0.62 [95% CI, 0.48–0.81; P < .001]) and retrospective observational (RR = 0.56 [95% CI, 0.44–0.71; P < .001]) studies.
To assess the degree of inconsistency within each study design grouping, we calculated the percentage of total variation across studies that is due to heterogeneity (rather than chance), I2. The I2 measure is high for RCTs (85.8%), moderate for prospective observational studies (65.5%), and low for retrospective observational studies (19.4%). I2 measures the degree of inconsistency across studies in a meta-analysis and has the advantage that it can be compared between meta-analyses with different numbers of studies and different types of outcome data.22
The pooled RRs calculated in the meta-analysis imply conversion factors between study designs, relying on the pooled effect of each study design. Comparing RCTs with prospective studies, one can calculate as follows:
RR RCT
__________ = 1.43
RR Prospective
Similarly, comparing RCTs with retrospective studies:
RR RCT
___________ = 1.59
RR Retrospective
These ratios would suggest, for instance, that in order to compare the results of an individual RCT with those of a prospective observational study, the depot/oral RR from the RCT would need to be divided by 1.43 to account for differences between the 2 study designs.
Sensitivity Analyses
Table 3 reports the findings from various sensitivity analyses conducted. “Base case” summarizes the key findings reported in Figure 2. Subsequent rows report the various sensitivity analyses.
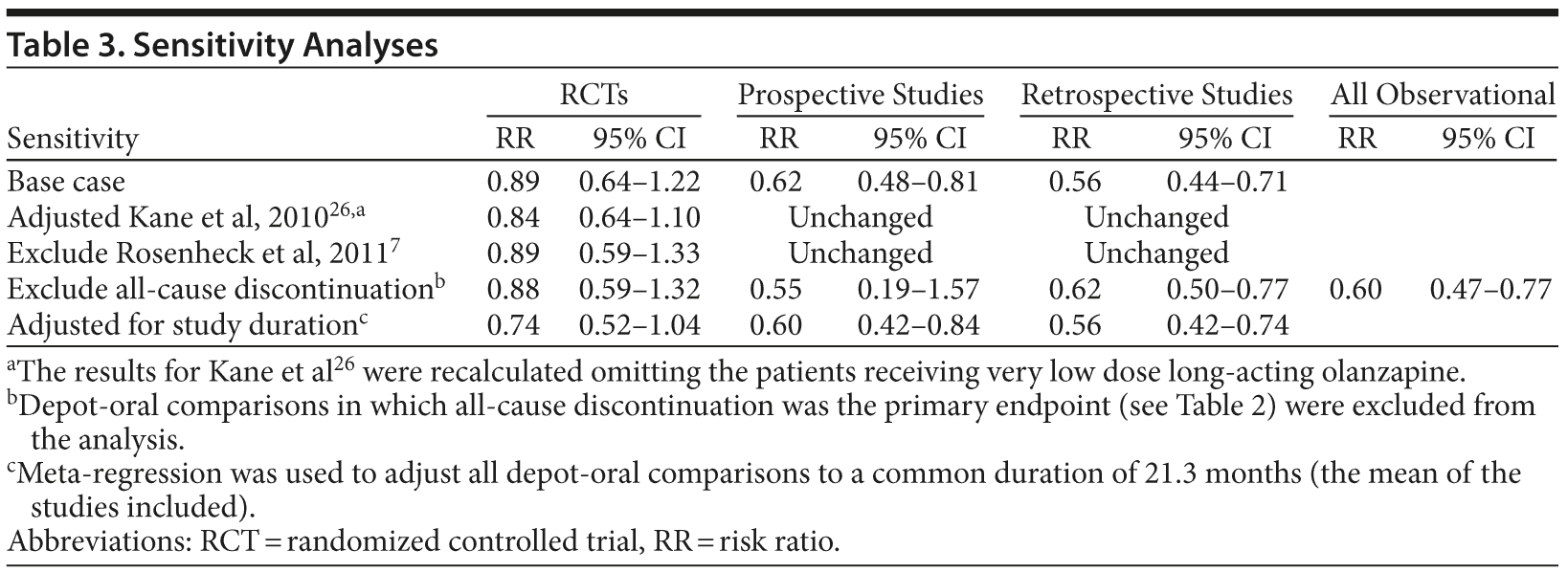
The study by Kane et al26 included multiple long-acting olanzapine treatment arms with very low, low, medium, and high dosages, with the very low dose serving as a “reference dose.” To test the effect of the very low dose long-acting injectable, we re-estimated the results excluding patients receiving the “reference dose.” Removing them reduces the adjusted RR for Kane et al26 from 2.03 to 1.42, with the pooled RCT estimate falling from 0.89 (95% CI, 0.64–1.22) to 0.84 (95% CI, 0.64–1.10).
Another potential issue may arise from the inclusion of the study by Rosenheck et al,7 which permitted a limited degree of crossover between treatment arms. Removal of the study has no substantive effect on the estimated RR, although the 95% CI increases due to smaller sample size (RR = 0.89 [95% CI, 0.64–1.22] to RR = 0.89 [95% CI, 0.59–1.33]).
The base case pools findings across multiple endpoints. Discontinuation of treatment may be better viewed as a proxy measure for possible subsequent adverse outcomes than as a direct outcome measure. We re-estimated the pooled RR after removing all-cause discontinuation. Whereas there was little measurable effect on RCTs (RR = 0.88 [95% CI, 0.59–1.32]) and retrospective studies (RR = 0.62 [95% CI, 0.50–0.77]), only 2 prospective studies remained, resulting in a statistically insignificant finding (RR = 0.55 [95% CI, 0.19–1.57]). However, the pooled finding for all observational studies combined (both prospective and retrospective) resulted in a significant estimate (RR = 0.60 [95% CI, 0.47–0.77]).
The findings from the duration adjustment are also reported in Table 3. After adjustment, the pooled RR for RCTs fell to 0.74 (0.52–1.04), while the findings for prospective studies (RR = 0.60 [95% CI, 0.42–0.84]) and retrospective studies (RR = 0.56 [95% CI, 0.42–0.74]) were largely unchanged.
DISCUSSION
The effectiveness of long-acting therapies has been debated, in part, because of the inconsistent findings in the clinical literature. However, it appears that study design is an important factor possibly affecting estimates of comparative effectiveness of antipsychotic medications. We find that in a meta-analysis of RCTs, the benefits of depot antipsychotics were not significantly superior to those of oral formulations. In contrast, as study design shifts toward prospective and retrospective observational studies, depot formulations display significant advantage.
These findings highlight an important methodological tension between the study designs. While randomization is the best strategy to estimate treatment effects from a statistical perspective (in terms of eliminating bias due to selection into treatment), it is possible that the RCT setting does not fully reflect other aspects of how oral therapies are used in general clinical practice. As the RCT has to match services and prescription monitoring for the oral subjects to equal those of long-acting depot subjects—possibly eliminating differences that would manifest themselves in general clinical practice—the study design may have limitations with respect to demonstrating significant differences between formulations in a real-world setting.
In contrast, observational studies may capture a more realistic treatment setting, but possibly at the expense of fully controlling for other possible confounding factors and selection bias (due to lack of randomization). While researchers may implement statistical techniques to account for such issues, any remaining bias could contribute to the differences in treatment effects identified in observational settings.
The issue of appropriate use of study design is hardly a new one in the statistical and clinical literature. Conclusive answers about treatment effectiveness require both methodological rigor in comparing treatment outcomes and generalizability to the conditions of medical practice.13 While the former may be most adequately addressed using the RCT, the latter may be best served by an observational design. As noted by Sackett and Wennberg, “Each method [RCT and observational] should flourish, because each has features that overcome the limitations of the others when confronted with questions they cannot reliably answer.”33(p1636)
Given the tension highlighted above, our findings should not be interpreted as pointing to which research methodology is “correct,” and they do not resolve the debate over the relative effectiveness of depot versus oral formulations. However, we believe that they offer a reasonable explanation for some of the inconsistencies in the literature on comparative effectiveness of depot and oral formulations in the treatment of schizophrenia. Moreover, the analysis presented above did not attempt to ascertain the reasons for the variation in relative effectiveness of depot formulations across study designs. As a matter of clinical practice, the findings may be informative, as clinicians can attempt to ascertain which study design more closely resembles the nature of their practice.
While prior research on cross-design synthesis has attempted to merge results across study types to achieve a common effect measure, the present study does not, in fact, combine the findings across research designs. Rather, our goal was to document whether there were differences in the measure of effectiveness between oral and depot antipsychotics across study designs and to quantify the difference to facilitate future comparison between studies. The conversion factors presented above provide a simple tool to put 2 studies of divergent designs on comparable footing. While based on a limited number of studies, the conversion factors can be interpreted as capturing the average effect of study design in the context of depot and oral antipsychotics in schizophrenia.
The study has several limitations. The number of studies and comparisons meeting the inclusion criteria was small. As more research is conducted to directly compare oral and depot agents in schizophrenia, it will be important to revisit these findings, as a small number of studies could potentially affect the overall results.
In addition, each study design category included a combination of different endpoints, which were treated equally in the meta-analysis. While relapse, hospitalization, and all-cause discontinuation are closely related in schizophrenia, they are not perfectly homogenous. First, definitions of relapse and hospitalization may vary across studies. Second, while relapse and hospitalization are direct outcome measures, discontinuation of treatment should be viewed as a proxy measure for possible subsequent adverse outcomes. The analysis relies on the assumption that the depot-to-oral RRs are comparable across endpoints. In addition, Table 3 confirms that the omission of all-cause discontinuation has little substantive effect on the overall findings.
Another limitation is that the RR adjustments only accounted for baseline differences in gender and age across studies (when feasible). Other baseline characteristics, including various clinical measures, were not adjusted for due to lack of relevant estimates in the literature. Prior research suggests that longer duration studies show greater benefit in terms of relapse prevention for depot formulations.9,34–37 However, in the studies included in this review, a 24-month follow-up was the mode across all 3 study design groupings. In addition, comparing RCTs and observational studies of similar duration suggests that duration is most likely not a key factor in the results.
It is also important to stress that while the findings are consistent with the hypothesis that differences in level of researcher control across the various study designs affect adherence and, subsequently, certain clinical endpoints, there are potentially other differences between RCTs and observational designs that could account for the apparent systematic differences between designs (academic settings, funding sources, unknown confounding, etc).
In conclusion, our study has found a systematic difference across research designs in the measure of comparative effectiveness of oral versus depot formulations of antipsychotic agents in schizophrenia.
Drug names: aripiprazole (Abilify), asenapine (Saphris), haloperidol (Haldol and others), iloperidone (Fanapt), lurasidone (Latuda), olanzapine (Zyprexa), paliperidone (Invega), quetiapine (Seroquel), risperidone (Risperdal, Risperdal Consta, and others).
Author affiliations: Analysis Group, Inc, Boston, Massachusetts (Dr Kirson and Messrs Yermakov, Huang, Samuelson, and Greenberg); Department of Psychiatry, University of Illinois, Chicago (Dr Weiden); Otsuka America Pharmaceutical, Inc, Princeton, New Jersey (Dr Offord); and Center for Clinical Epidemiology, University of Pennsylvania, Philadelphia (Dr Wong).
Potential conflicts of interest: Dr Kirson and Messrs Yermakov, Huang, and Greenberg are employees of Analysis Group, Inc, and Mr Samuelson is a prior employee of Analysis Group, Inc. Dr Weiden has served as a consultant for or on the advisory board of Delpor, Johnson & Johnson (Janssen), Lundbeck, Otsuka America Pharmaceutical, Inc (OAPI), Merck, Novartis, Sunovion, Genentech/Roche, and Vanda; has received research funding from Genentech/Roche, Johnson & Johnson (Janssen), Novartis, and Sunovion; and is on the speakers bureau for Johnson & Johnson (Janssen), Novartis, Sunovion, and Genentech/Roche. Dr Offord is an employee of OAPI. Dr Wong is a consultant for OAPI.
Funding/support: Research support was provided to Analysis Group, Inc
by Otsuka America Pharmaceutical, Inc.
Previous presentations: Findings from this study were presented at the 165th Annual Meeting of the American Psychiatric Association; May 5–9, 2012; Philadelphia, Pennsylvania; and at the 52nd Annual NCDEU Meeting; May 29–June 1, 2012; Phoenix, Arizona.
REFERENCES
1. Kane JM. Pharmacologic treatment of schizophrenia. Biol Psychiatry. 1999;46(10):1396–1408. doi:10.1016/S0006-3223(99)00059-1 PubMed
2. Velligan DI, Weiden PJ, Sajatovic M, et al. Strategies for addressing adherence problems in patients with serious and persistent mental illness: recommendations from the expert consensus guidelines. J Psychiatr Pract. 2010;16(5):306–324. doi:10.1097/01.pra.0000388626.98662.a0 PubMed
3. Weiden PJ, Olfson M. Cost of relapse in schizophrenia. Schizophr Bull. 1995;21(3):419–429. doi:10.1093/schbul/21.3.419 PubMed
4. Velligan DI, Weiden PJ, Sajatovic M, et al; Expert Consensus Panel on Adherence Problems in Serious and Persistent Mental Illness. The Expert Consensus Guideline Series: Adherence Problems in Patients With Serious and Persistent Mental Illness. J Clin Psychiatry. 2009;70(suppl 4):1–46, quiz 47–48. doi:10.4088/JCP.7090su1cj PubMed
5. Olivares JM, Rodriguez-Morales A, Diels J, et al; e-STAR Spanish Study Group. Long-term outcomes in patients with schizophrenia treated with risperidone long-acting injection or oral antipsychotics in Spain: results from the electronic Schizophrenia Treatment Adherence Registry (e-STAR). Eur Psychiatry. 2009;24(5):287–296. doi:10.1016/j.eurpsy.2008.12.002 PubMed
6. Haddad P, Taylor M, Niaz OS. First-generation antipsychotic long-acting injections v oral antipsychotics in schizophrenia: systematic review of randomised controlled trials and observational studies.
Br J Psychiatry. 2009;195:s20–s28. doi:10.1192/bjp.195.52.s20
7. Rosenheck RA, Krystal JH, Lew R, et al; CSP555 Research Group. Long-acting risperidone and oral antipsychotics in unstable schizophrenia.
N Engl J Med. 2011;364(9):842–851. doi:10.1056/NEJMoa1005987 PubMed
8. Tiihonen J, Haukka J, Taylor M, et al. A nationwide cohort study of oral
and depot antipsychotics after first hospitalization for schizophrenia. Am J Psychiatry. 2011;168(6):603–609. doi:10.1176/appi.ajp.2011.10081224 PubMed
9. Leucht C, Heres S, Kane JM, et al. Oral versus depot antipsychotic drugs for schizophrenia—a critical systematic review and meta-analysis of randomised long-term trials. Schizophr Res. 2011;127(1–3):83–92. doi:10.1016/j.schres.2010.11.020 PubMed
10. Mohamed S, Rosenheck R, Harpaz-Rotem I, et al. Duration of pharmacotherapy with long-acting injectable risperidone in the treatment of schizophrenia. Psychiatr Q. 2009;80(4):241–249. doi:10.1007/s11126-009-9111-9 PubMed
11. Barnett PG, Scott JY, Krystal JH, et al; CSP 555 Research Group. Cost and cost-effectiveness in a randomized trial of long-acting risperidone for schizophrenia. J Clin Psychiatry. 2012;73(5):696–702. doi:10.4088/JCP.11m07070 PubMed
12. French JRP. Field experiments: changing group productivity. In: Miller JG, ed. Experiments in Social Process: A Symposium on Social Psychology. New York, NY: McGraw-Hill; 1950: 79–96.
13. Droitcour J, Silberman G, Chelimsky E. A new form of meta-analysis for combining results from randomized clinical trials and medical-practice databases. Int J Technol Assess Health Care. 1993;9(3):440–449. doi:10.1017/S0266462300004694 PubMed
14. DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials. 1986;7(3):177–188. doi:10.1016/0197-2456(86)90046-2 PubMed
15. McGrath J, Saha S, Chant D, et al. Schizophrenia: a concise overview of incidence, prevalence, and mortality. Epidemiol Rev. 2008;30(1):67–76. doi:10.1093/epirev/mxn001 PubMed
16. Saha S, Chant D, Welham J, et al. A systematic review of the prevalence of schizophrenia. PLoS Med. 2005;2(5):e141. doi:10.1371/journal.pmed.0020141 PubMed
17. Perälä J, Suvisaari J, Saarni SI, et al. Lifetime prevalence of psychotic and bipolar I disorders in a general population. Arch Gen Psychiatry. 2007;64(1):
19–28. doi:10.1001/archpsyc.64.1.19 PubMed
18. Robinson D, Woerner MG, Alvir JM, et al. Predictors of relapse following response from a first episode of schizophrenia or schizoaffective disorder. Arch Gen Psychiatry. 1999;56(3):241–247. doi:10.1001/archpsyc.56.3.241 PubMed
19. Mortensen PB, Eaton WW. Predictors for readmission risk in schizophrenia. Psychol Med. 1994;24(1):223–232. doi:10.1017/S0033291700026982 PubMed
20. Ciudad A, Haro JM, Alonso J, et al. The Schizophrenia Outpatient Health Outcomes (SOHO) study: 3-year results of antipsychotic treatment discontinuation and related clinical factors in Spain. Eur Psychiatry. 2008;23(1):1–7. doi:10.1016/j.eurpsy.2007.09.008 PubMed
21. Kozma CM, Weiden PJ. Partial compliance with antipsychotics increases mental health hospitalizations in schizophrenic patients: analysis of a national managed care database. Am Health Drug Benefits. 2009;2(1):31–38.
22. Higgins JP, Thompson SG, Deeks JJ, et al. Measuring inconsistency in
meta-analyses. BMJ. 2003;327(7414):557–560 [review]. doi:10.1136/bmj.327.7414.557 PubMed
23. Lau J, Ioannidis JP, Schmid CH. Summing up evidence: one answer is not always enough. Lancet. 1998;351(9096):123–127. doi:10.1016/S0140-6736(97)08468-7 PubMed
24. Macfadden W, Ma YW, Thomas Haskins J, et al. A prospective study comparing the long-term effectiveness of injectable risperidone long-acting therapy and oral aripiprazole in patients with schizophrenia. Psychiatry (Edgmont). 2010;7(11):23–31. PubMed
25. Gaebel W, Schreiner A, Bergmans P, et al. Relapse prevention in schizophrenia and schizoaffective disorder with risperidone long-acting injectable vs quetiapine: results of a long-term, open-label, randomized clinical trial. Neuropsychopharmacology. 2010;35(12):2367–2377. doi:10.1038/npp.2010.111 PubMed
26. Kane JM, Detke HC, Naber D, et al. Olanzapine long-acting injection: a 24-week, randomized, double-blind trial of maintenance treatment in patients with schizophrenia. Am J Psychiatry. 2010;167(2):181–189. doi:10.1176/appi.ajp.2009.07081221 PubMed
27. Keks NA, Ingham M, Khan A, et al. Long-acting injectable risperidone v. olanzapine tablets for schizophrenia or schizoaffective disorder: randomised, controlled, open-label study. Br J Psychiatry. 2007;191(2):131–139. doi:10.1192/bjp.bp.105.017020 PubMed
28. Kim B, Lee SH, Choi TK, et al. Effectiveness of risperidone long-acting injection in first-episode schizophrenia: in naturalistic setting. Prog Neuropsychopharmacol Biol Psychiatry. 2008;32(5):1231–1235. doi:10.1016/j.pnpbp.2008.03.012 PubMed
29. Zhu B, Ascher-Svanum H, Shi L, et al. Time to discontinuation of depot
and oral first-generation antipsychotics in the usual care of schizophrenia. Psychiatr Serv. 2008;59(3):315–317. doi:10.1176/appi.ps.59.3.315 PubMed
30. Emsley R, Oosthuizen P, Koen L, et al. Oral versus injectable antipsychotic treatment in early psychosis: post hoc comparison of two studies. Clin Ther. 2008;30(12):2378–2386. doi:10.1016/j.clinthera.2008.12.020 PubMed
31. Tiihonen J, Wahlbeck K, Lönnqvist J, et al. Effectiveness of antipsychotic treatments in a nationwide cohort of patients in community care after first hospitalisation due to schizophrenia and schizoaffective disorder: observational follow-up study. BMJ. 2006;333(7561):224. doi:10.1136/bmj.38881.382755.2F PubMed
32. Tavcar R, Dernovsek MZ, Zvan V. Choosing antipsychotic maintenance therapy—a naturalistic study. Pharmacopsychiatry. 2000;33(2):66–71. doi:10.1055/s-2000-7969 PubMed
33. Sackett DL, Wennberg JE. Choosing the best research design for each question. BMJ. 1997;315(7123):1636. doi:10.1136/bmj.315.7123.1636 PubMed
34. del Giudice J, Clark WG, Gocka EF. Prevention of recidivism of schizophrenics treated with fluphenazine enanthate. Psychosomatics. 1975;16(1):32–36. PubMed
35. Johnson DA. The duration of maintenance therapy in chronic schizophrenia. Acta Psychiatr Scand. 1976;53(4):298–301. PubMed
36. Hogarty GE, Schooler NR, Ulrich R, et al. Fluphenazine and social therapy
in the aftercare of schizophrenic patients: relapse analyses of a two-year controlled study of fluphenazine decanoate and fluphenazine hydrochloride. Arch Gen Psychiatry. 1979;36(12):1283–1294. doi:10.1001/archpsyc.1979.01780120013001 PubMed
37. Johnson DA. Further observations on the duration of depot neuroleptic maintenance therapy in schizophrenia. Br J Psychiatry. 1979;135(6):524–530. doi:10.1192/bjp.135.6.524 PubMed
This PDF is free for all visitors!





