Objective: To describe the prevalence of posttraumatic stress disorder (PTSD) and comorbid psychiatric disorders and identify correlates of PTSD in a contemporary, nationally representative sample of US veterans.
Method: Data were analyzed from Wave 1 of the National Health and Resilience in Veterans Study, a cross-sectional, retrospective, web-based survey of a population-based sample of 3,157 US veterans conducted between October and December 2011. The main outcome measure was probable lifetime PTSD, which was assessed by using a DSM-IV version of the PTSD Checklist (PCL), the PCL-Specific Stressor version.
Results: The weighted lifetime and current prevalence of probable PTSD was 8.0% (standard error [SE] = 0.48) and 4.8% (SE = 0.40), respectively. 87.0% of veterans reported exposure to at least 1 potentially traumatic event (PTE); veterans reported a mean of 3.4 (SD = 2.8) different PTE types in their lifetime. Sudden death of a loved one was the most frequently endorsed PTE (61.3%), and sexual abuse in adulthood had the highest conditional probability of PTSD (37.3%). PTSD was associated with increased odds of mood, anxiety, and substance use disorders (odds ratios [ORs] = 2.2-19.1, P values < .001); suicidal ideation (OR = 9.7, P < .001); and suicide attempts (OR = 11.8, P < .001). Psychosocial factors, including resilience, community integration, and secure attachment, were associated with decreased odds of PTSD (ORs = 0.5-0.7, P values < .05).
Conclusions: In a nationally representative sample of US veterans, the prevalence of lifetime and current PTSD was 8.0% and 4.8%, respectively, and PTSD was associated with elevated risk for several psychiatric conditions and suicidality. Veterans reported exposure to many PTE types in addition to combat, and conditional risk for PTSD was high for noncombat-related trauma. Prevention and treatment efforts designed to bolster protective psychosocial factors may help mitigate PTSD risk in this population.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
See Commentary by Hoge and Warner.
ABSTRACT
Objective: To describe the prevalence of posttraumatic stress disorder (PTSD) and comorbid psychiatric disorders and identify correlates of PTSD in a contemporary, nationally representative sample of US veterans.
Method: Data were analyzed from Wave 1 of the National Health and Resilience in Veterans Study, a cross-sectional, retrospective, web-based survey of a population-based sample of 3,157 US veterans conducted between October and December 2011. The main outcome measure was probable lifetime PTSD, which was assessed by using a DSM-IV version of the PTSD Checklist (PCL), the PCL-Specific Stressor version.
Results: The weighted lifetime and current prevalence of probable PTSD was 8.0% (standard error [SE] = 0.48) and 4.8% (SE = 0.40), respectively. 87.0% of veterans reported exposure to at least 1 potentially traumatic event (PTE); veterans reported a mean of 3.4 (SD = 2.8) different PTE types in their lifetime. Sudden death of a loved one was the most frequently endorsed PTE (61.3%), and sexual abuse in adulthood had the highest conditional probability of PTSD (37.3%). PTSD was associated with increased odds of mood, anxiety, and substance use disorders (odds ratios [ORs] = 2.2-19.1, P values < .001); suicidal ideation (OR = 9.7, P < .001); and suicide attempts (OR = 11.8, P < .001). Psychosocial factors, including resilience, community integration, and secure attachment, were associated with decreased odds of PTSD (ORs = 0.5-0.7, P values < .05).
Conclusions: In a nationally representative sample of US veterans, the prevalence of lifetime and current PTSD was 8.0% and 4.8%, respectively, and PTSD was associated with elevated risk for several psychiatric conditions and suicidality. Veterans reported exposure to many PTE types in addition to combat, and conditional risk for PTSD was high for noncombat-related trauma. Prevention and treatment efforts designed to bolster protective psychosocial factors may help mitigate PTSD risk in this population.
J Clin Psychiatry 2014;75(12):1338-1346
© Copyright 2014 Physicians Postgraduate Press, Inc.
Submitted: June 18, 2014; accepted August 18, 2014 (doi:10.4088/JCP.14m09328).
Corresponding author: Robert H. Pietrzak, PhD, MPH, National Center for Posttraumatic Stress Disorder, VA Connecticut Healthcare System, Department of Psychiatry, Yale School of Medicine, 950 Campbell Ave/151E, West Haven, CT 06516 ([email protected]).
Posttraumatic stress disorder (PTSD) is one of the most prevalent mental disorders among US veterans.1,2 Recent studies using nationally representative samples of the general US population have estimated lifetime prevalence of PTSD to be 6.4%-6.8%.3,4 Although informative, such estimates are unlikely to generalize to US veterans, who differ from the general US adult population.5 For example, prevalence estimates in US veterans will most likely be influenced by the different demographic composition of this population, which contains a much larger proportion of older men, a group at decreased risk of PTSD relative to younger individuals6,7 and to women.8 Further, estimates of the lifetime prevalence of PTSD among US veterans, specifically, have ranged widely (5%-32%),1,9-11 as these studies have typically assessed the prevalence of PTSD in specific cohorts of veterans, such as Vietnam-era veterans or veterans deployed to Iraq or Afghanistan, who are not representative of the entire US veteran population. Notably, to date, a precise estimate of the prevalence of PTSD in the current population of US veterans has yet to be established, even though such information can be useful in informing public policy and health care planning.
Data from contemporary, nationally representative US veteran samples regarding nonmilitary-related trauma exposure and the associated conditional risk of PTSD given exposure to different trauma types are also lacking. Such data are important to ascertain, as US veterans frequently report exposure to both military and nonmilitary traumas, and nonmilitary traumas experienced prior to deployment have been related to increased risk for postdeployment PTSD.12-14 Prior research has also found that PTSD is associated with increased risk for psychiatric comorbidity,4,10,15,16 as well as suicidality.4,17-20 Elucidation of common comorbidities associated with PTSD can help facilitate understanding of the population-based comorbidity burden associated with this disorder.
Although epidemiologic studies have identified risk factors besides combat exposure for PTSD, including younger age, female sex, racial/ethnic minority status, low socioeconomic status and education level, unmarried marital status, and serving in the Army relative to other military branches,10,16,21-23 these findings may not be applicable to the broader US veteran population. While a substantial body of research has focused on risk factors for PTSD, few studies have assessed potentially modifiable factors that may help mitigate PTSD risk, such as social support, optimism, gratitude, purpose in life, and community integration.22,24-26
In the current study, we analyzed data from a contemporary, nationally representative sample of US veterans to address 3 aims: (1) to describe the prevalence of probable PTSD, trauma exposure, and comorbid psychiatric conditions; (2) to evaluate the conditional probability of PTSD given exposure to different potentially traumatic events; and (3) to identify risk and protective factors associated with probable PTSD.

- The prevalence of posttraumatic stress disorder (PTSD) in US veterans is slightly higher compared with the general US adult population, and veterans with PTSD have higher rates of other psychiatric disorders and suicidal behaviors relative to veterans without PTSD.
- Both combat- and noncombat-related traumas are common in this population and are differentially associated with PTSD risk, suggesting the importance of comprehensive assessment of trauma histories in veterans.
- US veterans with PTSD may benefit from interventions designed to bolster social connectedness and protective psychosocial characteristics, such as resilience and community integration.
METHOD
Participants and Procedure
We analyzed data from Wave 1 of the National Health and Resilience in Veterans Study (NHRVS), which surveyed a nationally representative sample of 3,157 US Veterans.27 The NHRVS sample was recruited between October and December 2011 from a research panel of over 80,000 households that was developed and maintained by GfK Knowledge Networks, Inc, Palo Alto, California. Panel members were recruited through national random samples using a sampling procedure that includes listed and unlisted phone numbers; telephone, nontelephone, and cellphone-only households; and households with or without Internet access, offering coverage of approximately 98% of US households. To promote generalizability of results to the entire population of US veterans, we applied poststratification weights based on demographic distributions of US veterans from concurrent US Census data (October 2010 Current Population Survey28). Of the 4,750 veterans who were in the GfK Knowledge Networks survey panel at the time the NHRVS was fielded (veteran status was assessed using a general demographic questionnaire), 3,408 (71.7%) responded to an invitation to participate and completed a screening question to confirm their study eligibility (current or past active military status). Of these respondents, 3,188 (93.5%) confirmed their current or past active military status, and 3,157 (92.6%) completed a confidential, 60-minute online survey. The main outcome measure, probable lifetime PTSD status, was unavailable for 27 participants (< 1%); these participants were excluded from analyses. Probable current PTSD status was unavailable for an additional 199 participants (6.4%); these participants were excluded from analyses examining probable current PTSD. All participants provided informed consent; the Human Subjects Subcommittee of the Veterans Affairs (VA) Connecticut Healthcare System and VA Office of Research and Development approved the study procedures.
Assessments
Demographic variables included age, gender, race/ethnicity, annual household income, and current marital and employment status. Military variables included military branch and enlistment status (enlisted versus drafted into military service). Participants were also asked whether the VA health care system was their primary source of health care.
Trauma exposure. The Trauma History Screen29 is a self-report measure that assesses the occurrence of 13 potentially traumatic life events. Potential traumas across the lifespan, such as physical or sexual assault during childhood or adulthood, traumatic events during military service, accidents, and unexpected loss of a loved one were assessed. An additional potentially traumatic event—life-threatening illness or injury—was added to the NHRVS.
Combat exposure. A single item, “Did you ever serve in a combat or war zone?” was used to assess whether veterans had experienced any combat exposure. All veterans who answered yes to this item were classified as “combat veterans” for the purpose of analyses. Because not all combat veterans experience potentially traumatic events, combat veterans were classified as having “traumatic combat exposure” if they also endorsed the item “During military service-saw something horrible or was badly scared” on the Trauma History Screen. Combat veterans were also administered the Combat Exposure Scale,30 which was used to classify veterans into levels of combat exposure from “light” to “heavy” using standard cut scores.
PTSD. The PTSD Checklist-Specific Stressor version (PCL-S)31 is a 17-item self-report measure for assessing PTSD according to criteria in the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV)32 criteria for PTSD. The Specific Stressor version of the PCL asks about PTSD symptoms in the past month related to an individual’s “worst” stressful experience. We modified the PCL-S for this study to include both lifetime and past-month ratings. Participants rated how much they have been bothered by each of the 17 symptoms ever in their lifetime (lifetime PTSD) and in the past month (current PTSD) on a scale from 1 (not at all) to 5 (extremely). Following recommendations for veteran samples,31 we used a cut score ≥ 50 to determine presence of probable lifetime and current PTSD.
Psychiatric comorbidity. Lifetime history of major depressive disorder, social phobia, alcohol abuse/dependence, and drug abuse/dependence were assessed by using items derived from the relevant modules of the Mini-International Neuropsychiatric Interview.33 Current depression and anxiety symptoms were assessed with the Patient Health Questionnaire-4 (PHQ-4),34 a commonly used 4-item screening instrument for depression and generalized anxiety. Current suicidal ideation was assessed by using question 9 from the PHQ-9,35 and lifetime suicide attempt was assessed by using the question “Have you ever tried to kill yourself?” with the response options no and yes.
Psychosocial factors. As described in detail elsewhere,25 exploratory factor analysis was used to reduce a number of scales from the NHRVS survey into 2 factors assessing relatively stable psychosocial characteristics. The protective psychosocial characteristics factor includes individual measures/questions that assess characteristics associated with positive mental health outcomes, including resilience (score on the Connor-Davidson Resilience Scale-1036), dispositional optimism (score on single-item measure of optimism from Life Orientation Test-Revised37: “In uncertain times, I usually expect the best” [rating 1 = strongly disagree to 7 = strongly agree]), gratitude (score on single-item measure from the Gratitude Questionnaire38: “I have so much in life to be thankful for” [rating 1 = strongly disagree to 7 = strongly agree]), curiosity (score on single-item measure of curiosity/exploration from Curiosity and Exploration Inventory-II39: “I frequently find myself looking for new opportunities to grow as a person [eg, information, people, resources]” [rating 1 = strongly disagree to 7 = strongly agree]), purpose in life (score on the Purpose in Life Test-Short Form40), and community integration (score on the item “I feel well integrated in my community [eg, regularly participate in community activities]” [rating 1 = strongly disagree to 7 = strongly agree]).
The social connectedness factor includes individual measures/questions that assess adaptive interpersonal factors, including number of close friends and relatives (response to question: “About how many close friends and relatives do you have [people you feel at ease with and can talk to about what is on your mind]?”), secure attachment style (endorsement of secure attachment [response a] to the following question: “Please select the statement below that best describes your feelings and attitudes in relationships: [a] feeling that it is easy to get close to others and feeling comfortable with them [secure], [b] feeling uncomfortable being close to others [avoidant], or [c] feeling that others are reluctant to get close [anxious/ambivalent]”),41 and perceived social support (score on abbreviated 5-item measure of the Medical Outcomes Study Social Support Scale42). Factor scores were used for all analyses.
Data Analysis
First, we computed the prevalence of probable lifetime and current PTSD in the overall sample and by sex and by age groups. Second, we computed the prevalence of exposure to different types of potential traumas and the conditional probability of PTSD given exposure to different trauma types; conditional probabilities of PTSD were calculated based on any exposure to that trauma type, whether or not that trauma was endorsed as the worst trauma. Third, we conducted χ2 analyses to examine psychiatric comorbidities associated with probable lifetime PTSD and to compare proportions of possible risk and protective factors among veterans with and without probable current PTSD. Probable current PTSD was used as the outcome variable for tests of risk and protective factors to help ensure that PTSD symptoms did not temporally precede any of the predictor variables. Fourth, we conducted a multivariable logistic regression including all theoretically derived risk and protective factors that we hypothesized would be associated with probable current PTSD. Bonferroni corrections were applied to control for familywise error in multivariable analyses. All raw frequencies reported are unweighted; all means, percentages, and inferential statistics are weighted to reflect the general population of US veterans.
RESULTS
The demographic composition of participants in the NHRVS survey was highly comparable to that of US veterans in the concurrent US Census data (2010 American Community Survey 1-Year Estimates).28 Specifically, our sample was predominantly male (89.8% unweighted vs 92.8% in Census) and white (83.6% unweighted vs 84.3% in Census), and it comprised a comparable percentage of veterans aged 65 years or older (46.4% unweighted vs 41.9% in Census). In our sample, 4.8% (unweighted) of veterans were Hispanic (compared to 5.3% in Census), and, excluding veterans who were retired, 74.1% (unweighted) were currently employed/working (compared to 75.5% in Census).
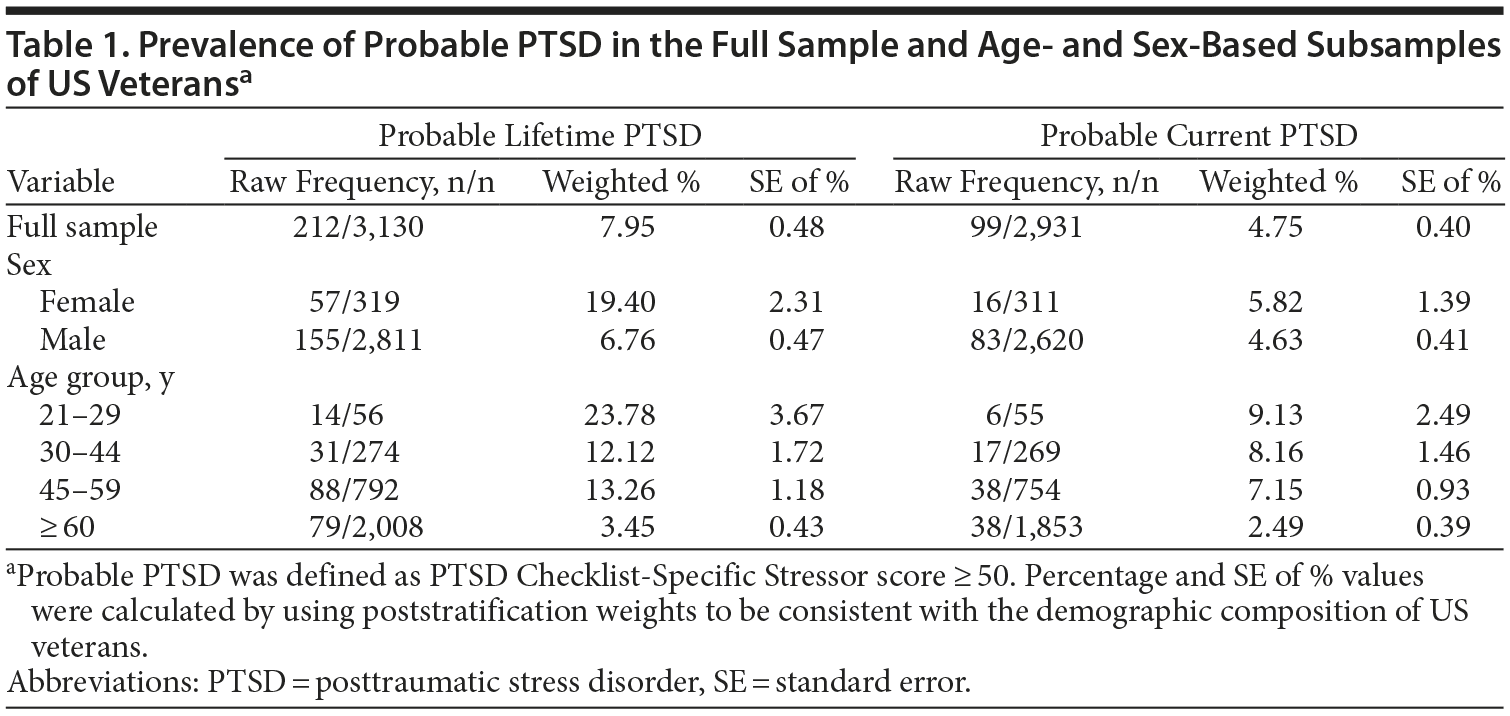
Table 1 displays the prevalence of probable PTSD for the full sample, and sex- and age-group-based subsamples of veterans. The lifetime prevalence of probable PTSD was 8.0% (standard error [SE] = 0.48), with 4.8% (SE = 0.40) screening positive for probable current PTSD. Lifetime prevalence was significantly higher among female than male veterans (OR = 3.32; 95% CI, 2.40-4.59) and among younger veterans than older veterans (aged ≥ 60 years) (aged 21-29 years: OR = 3.94; 95% CI, 2.03-7.66; aged 30-44 years: OR = 3.48; 95% CI, 2.13-5.71; and aged 45-59 years: OR = 3.02; 95% CI, 1.99-4.59).
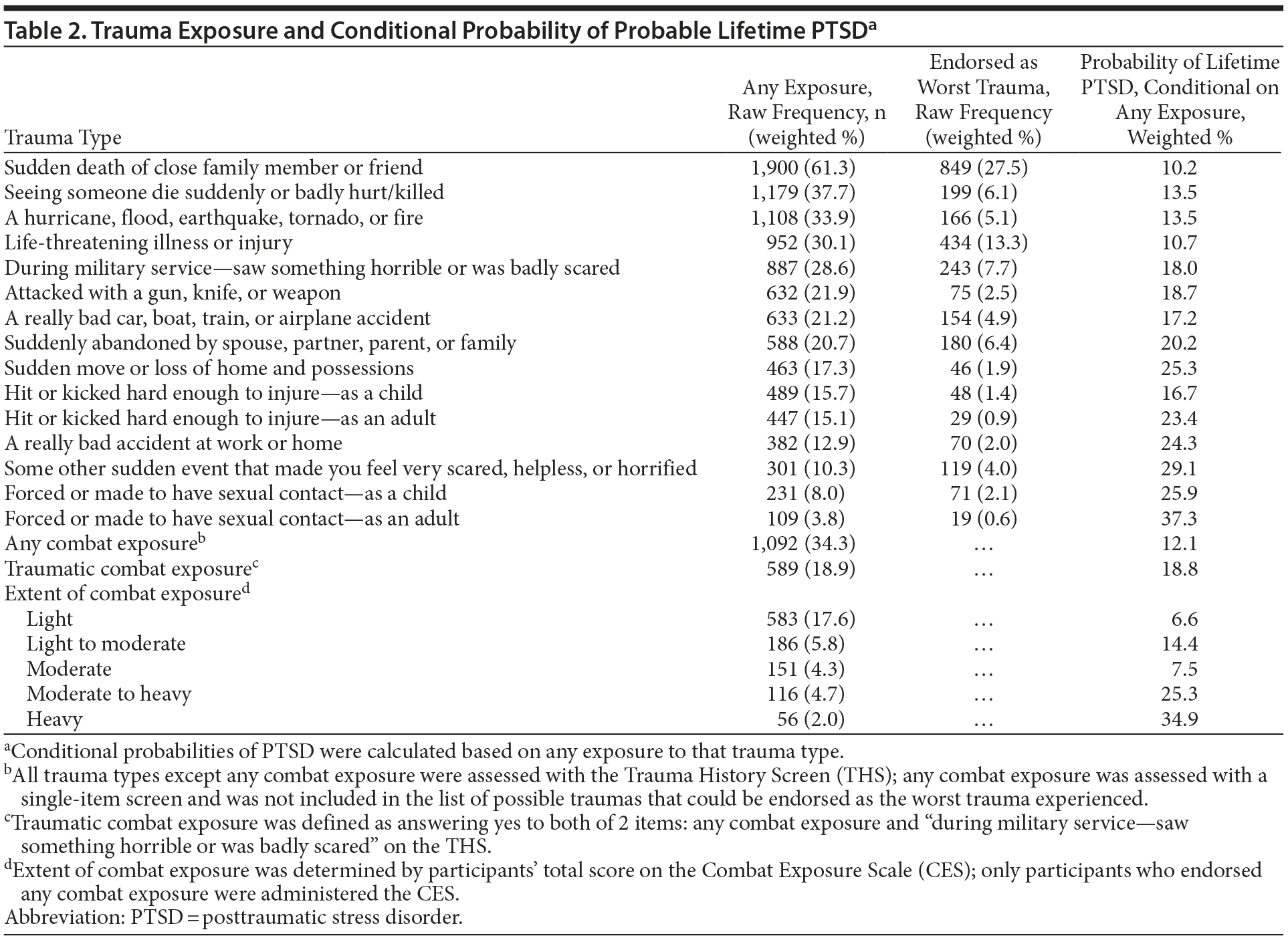
Table 2 displays estimates of the prevalence of potentially traumatic exposures and the probability of lifetime PTSD conditional on exposure to each trauma type. Veterans reported exposure to a mean of 3.38 (SD = 2.80) potentially traumatic event types in their lifetime, with the majority (n = 2,719, 87.0%) reporting exposure to at least 1 event. Sudden death of a close family member or friend was the most frequently endorsed trauma type (61.3%), followed by witnessing death or injury (seeing someone die suddenly or get badly hurt or killed; 37.7%), combat (34.3%), natural disasters (hurricane, flood, earthquake, tornado, or fire; 33.9%), and life-threatening illness or injury (30.1%). Sexual abuse in childhood and sexual abuse in adulthood were the least frequently endorsed trauma types (8.0% and 3.8%, respectively) but were associated with some of the highest conditional probabilities of PTSD (25.9% and 37.3%). Conditional probability of PTSD was 12.1% among veterans exposed to any combat and 18.8% among veterans exposed to traumatic combat. Risk of PTSD varied based on extent of combat exposure, with moderate-to-heavy and heavy combat exposure associated with particularly elevated PTSD risk (25.3% and 34.9%, respectively).
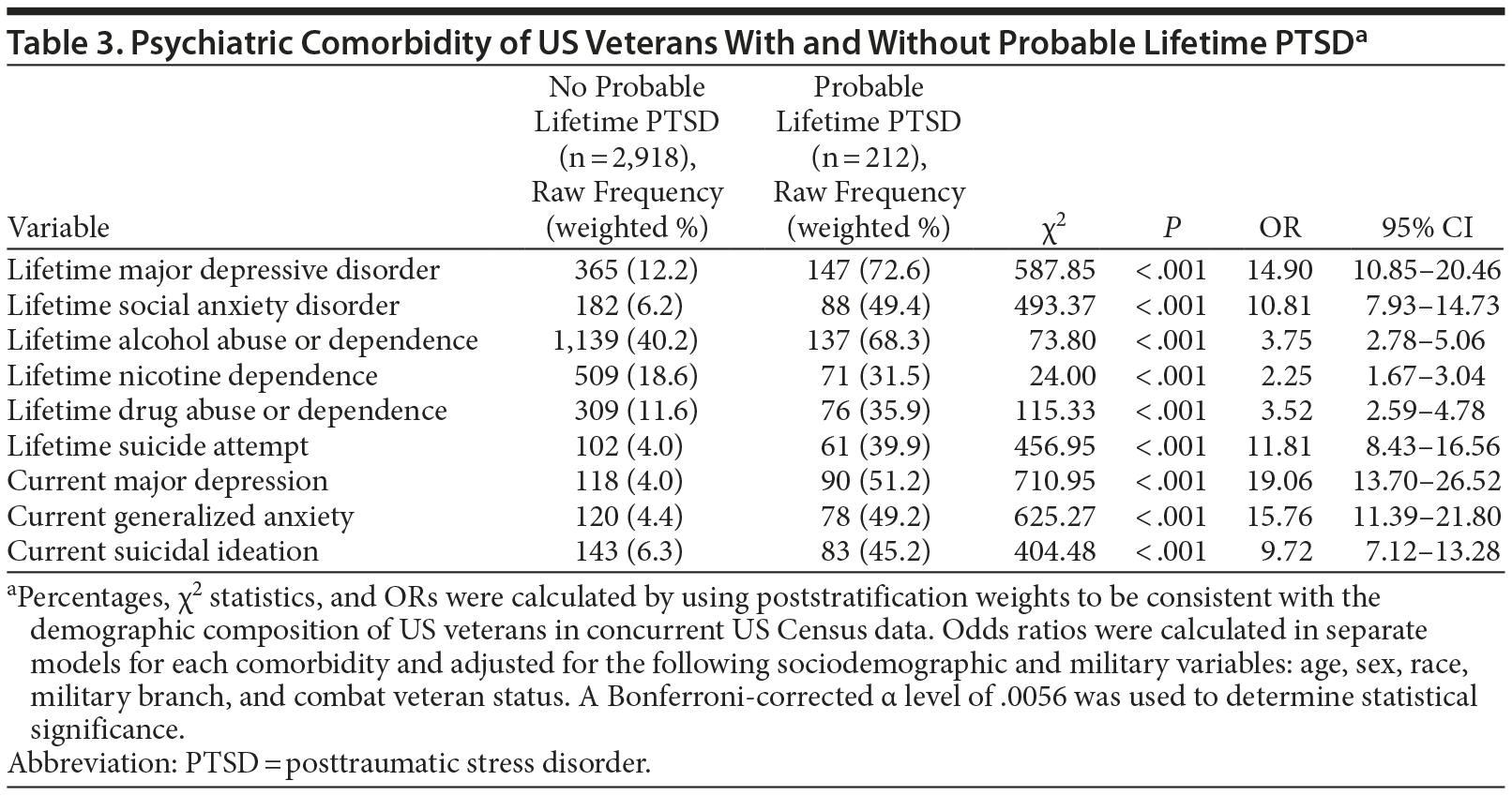
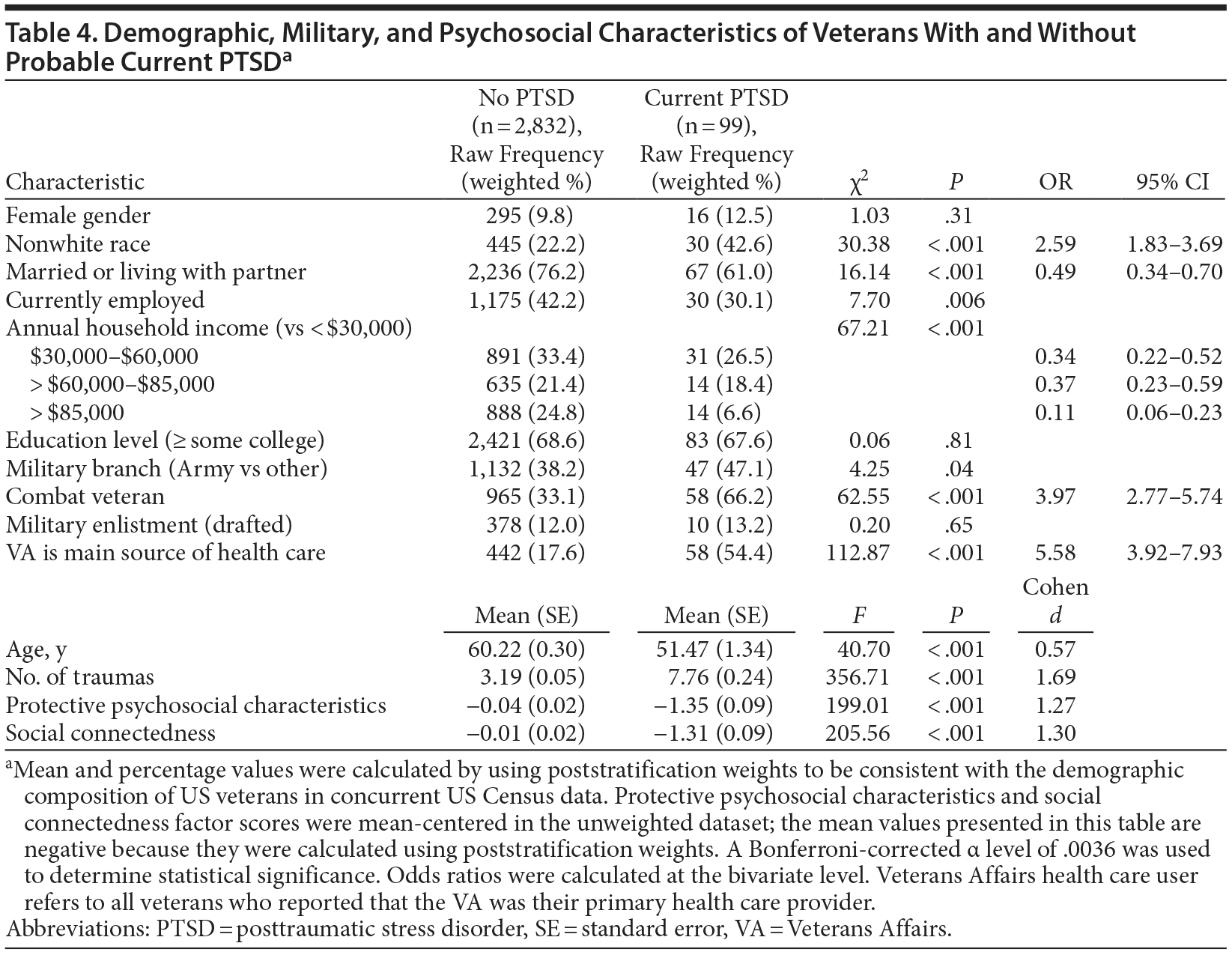
As shown in Table 3, after adjustment for sociodemographic and military characteristics, probable lifetime PTSD was associated with elevated odds of lifetime major depressive disorder, social anxiety disorder, alcohol abuse/dependence, drug abuse/dependence, nicotine dependence, and suicide attempt, as well as current depression, generalized anxiety, and suicidal ideation. Relative to veterans without probable current PTSD, veterans with probable current PTSD were more likely to be nonwhite and less likely to be married and have high household income (Table 4). Veterans with probable current PTSD were also younger and more likely to be combat veterans and to report the VA as their main source of health care; they also reported more potentially traumatic events in their lifetime and scored lower on measures of protective psychosocial characteristics and social connectedness.
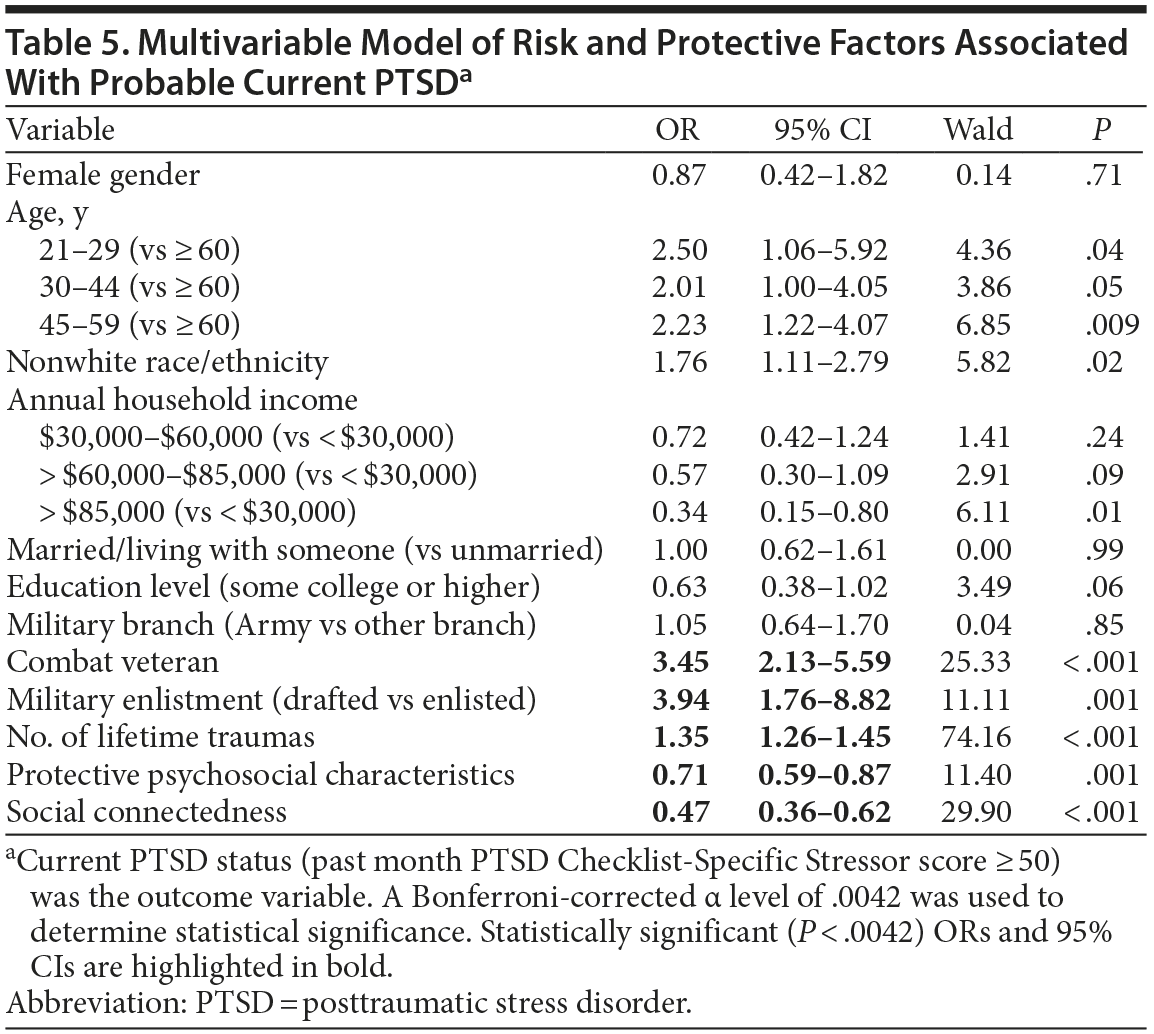
As shown in Table 5, results of a multivariable logistic regression that examined possible risk and protective factors associated with probable current PTSD revealed that, combat exposure, exposure to a greater number of traumas, and being drafted into the military were associated with increased odds of probable current PTSD. Protective psychosocial characteristics and social connectedness were associated with decreased odds of probable current PTSD. Exploratory post hoc analyses revealed that, of the psychosocial characteristic items, resilience (OR = 0.95; 95% CI, 0.92-0.99) and community integration (OR = 0.72; 95% CI, 0.61-0.85) were the only significant predictors of probable current PTSD after adjustment for covariates; of the social connectedness items, secure attachment emerged as the sole significant predictor (OR = 0.20; 95% CI, 0.10-0.38).
DISCUSSION
Overall, the estimated prevalence of probable lifetime PTSD (8.0%) among US veterans was at the lower end of ranges previously reported (eg, 5%-32%).9-11 Notably, the lifetime prevalence of PTSD was slightly higher than that observed in large epidemiologic studies of the general US adult population (6.4%-6.8%).3,4 Analyses stratified by sex and by age, however, revealed lifetime prevalence estimates higher than those found in the general US adult population among all subgroups.3 Specifically, the prevalence of lifetime probable PTSD was particularly high among female veterans (19.4% vs 9.7%) and veterans aged 21-29 years (23.8% vs 6.3%) compared with the general US adult population.3
The high prevalence of trauma exposure among our sample (87.0% exposed to at least 1 potentially traumatic event) was comparable with estimates in prior studies of combat veterans (90%)12 and the general adult samples (81.7%-89.6%).21,43 Consistent with findings in community adult samples,4,21,44 the most frequently experienced trauma type among US veterans was sudden death of a close family member or friend. Sexual abuse in childhood and sexual abuse in adulthood were the least frequently experienced trauma types but were also associated with high conditional probabilities of PTSD. This finding aligns with prior findings that sexual assault is associated with high conditional risk of developing PTSD.21 Among combat veterans, light-to-moderate levels of combat exposure were associated with relatively low conditional probability of PTSD, whereas moderate-to-heavy and heavy levels of combat exposure were associated with high conditional probabilities of PTSD. This finding highlights the importance of considering the extent of combat exposure when screening for PTSD in combat veterans. Taken together, these findings underscore high rates of trauma exposure among US veterans and the importance of examining PTSD resulting from a broad range of military and nonmilitary traumatic events in this population.
Consistent with findings in the general US adult population,3,4 PTSD was associated with high rates of psychiatric comorbidity, with probable lifetime PTSD associated with increased odds of every other psychiatric disorder assessed. Probable lifetime PTSD was associated with particularly high odds of mood and anxiety disorders (adjusted ORs ranged from 10.8 to 19.1). Probable lifetime PTSD was also associated with increased odds of alcohol and drug use disorders, although these effect sizes were smaller (adjusted ORs = 2.2-3.7). These findings accord with a large literature documenting high co-occurrence of PTSD and mood, anxiety, and substance use disorders, which may reflect shared risk factors, diagnostic overlap, and/or causal associations, such as “self-medication” of PTSD with alcohol or drugs.4,45 Importantly, probable lifetime PTSD was also associated with highly elevated odds of current suicidal ideation and lifetime history of suicide attempts (adjusted ORs = 9.7 and 11.8, respectively). These findings are consistent with prior research demonstrating that veterans with PTSD are at increased risk for suicidality.18-20,46 They further suggest that veterans with PTSD may be an appropriate target for suicide prevention efforts. Across all psychiatric comorbidities, effect sizes observed in this study were larger than those observed in large epidemiologic studies of the general US population.3,4 It is possible that rates of co-occurring disorders are higher among US veterans relative to civilians. However, our estimates of comorbidity may have been inflated by our use of self-report questionnaires, rather than diagnostic interviews, to assess psychiatric conditions.47,48 We also limited our covariates to key demographic and military variables; adjusting for a wider array of covariates might reduce magnitudes of comorbidity estimates.
Specific demographic and military characteristics were identified as robust correlates of current PTSD. After adjustment for other covariates, younger age, combat exposure, cumulative lifetime trauma burden, and enlistment status remained significantly associated with increased odds of probable current PTSD. These findings are generally consistent with prior findings of PTSD risk and resilience correlates in veterans.16,21,22,45 Protective psychosocial characteristics, such as resilience and community integration, and social connectedness were associated with decreased odds of PTSD. Importantly, these factors remained significant predictors even after we adjusted for a number of possible PTSD risk factors, indicating that they offer additional explanatory power in predicting PTSD risk. Because some aspects of these psychosocial correlates are potentially modifiable (eg, resilience, community integration),49,50 they may represent possible targets for PTSD prevention and early intervention efforts.51,52
Limitations of this study include the fact that PTSD and other psychiatric disorders were assessed with self-report questionnaires rather than diagnostic interviews. Although we used well-validated questionnaires, it is difficult to compare prevalence obtained in this study to prevalence obtained using structured interviews.3,4 Additionally, the use of the PCL-S to assess prevalence of PTSD has been criticized because there is considerable variation across populations in recommended cut scores.53 Although a PCL cut score ≥ 50 is generally recommended among veterans,31,53,54 no study of which we are aware has validated optimal PCL cut scores in a nationally representative sample of veterans, and some evidence suggests that even higher cut scores (eg, 55-60) may be appropriate when the true population prevalence of PTSD is less than 15%.55 Second, the Trauma History Screen and the version of the PCL administered in this study (PCL-S) were based on DSM-IV criteria, which have now been replaced with DSM-5 criteria.56 Consequently, different prevalence estimates might have been obtained with DSM-5-based instruments. Third, the cross-sectional and retrospective nature of our data is another limitation. Finally, our measures of trauma history did not clearly distinguish between combat- and noncombat-related trauma and did not assess whether traumatic events occurred before, during, or after veterans’ military service; more precise data would have allowed us to better distinguish military- from nonmilitary-related trauma.
Notwithstanding these limitations, this study extends prior research by examining the prevalence and correlates of PTSD in a large, contemporary, and nationally representative sample of US veterans, thereby allowing generalizability of these findings to the entire US veteran population. Our results indicate that US veterans show a slightly higher prevalence of probable lifetime PTSD compared with the general US population. They further indicate that US veterans report exposure to a wide range of potentially traumatic events, including both military- and nonmilitary-related events, and that veterans with probable PTSD have increased odds of mood, anxiety, and substance use disorders, as well as suicidal ideation and suicide attempts. After adjustment for possible risk factors for PTSD, protective psychosocial characteristics and social connectedness (most notably resilience, community integration, and secure attachment style) were associated with decreased risk for PTSD, thereby suggesting the importance of potentially targeting these factors in prevention and treatment efforts. Further research is needed to examine the policy implications of the relatively high rates of PTSD among certain subgroups of US veterans, particularly younger female veterans and veterans who rely on VA health care services; to distinguish the relative burden of military versus nonmilitary trauma on PTSD risk; and to examine the implications of the high levels of psychiatric comorbidity and suicidality for health care planning. Additional research will also be useful in evaluating whether the PTSD risk factors identified in this study may be used to refine PTSD screening instruments and to examine the efficacy of PTSD prevention and treatment efforts focused on bolstering protective psychosocial factors.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Author affiliations: Department of Psychology, University of North Carolina at Greensboro (Dr Wisco); National Center for PTSD, US Department of Veterans Affairs (VA) Boston Healthcare System and Department of Psychiatry, Boston University School of Medicine, Boston, Massachusetts (Drs Marx, Wolf, and Miller); and National Center for PTSD, VA Connecticut Healthcare System, and Department of Psychiatry, Yale University School of Medicine, New Haven, Connecticut (Drs Southwick and Pietrzak).
Author contributions: Dr Wisco had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. All authors contributed to the study concept and design and revised the manuscript for important intellectual content. Drs Southwick and Pietrzak acquired the data, Drs Pietrzak and Wisco contributed to the statistical analyses, and Dr Wisco drafted the manuscript.
Financial disclosure: Dr Pietrzak is a scientific consultant to Cogstate, Ltd for work that bears no relationship to the present study. Drs Wisco, Marx, Wolf, Miller, and Southwick have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: This study was funded by the VA National Center for Posttraumatic Stress Disorder and a private donation. Dr Marx was supported by funding from the National Institute of Mental Health (1R01MH095737-01A1), Department of Defense (W81XWH-10-2-0181, W81XWH-12-2-0117-PTSD-IIRA-INT), Defense Advanced Research Programs Agency (N66001-11-C-4006), and the VA (Cooperative Studies Program #591). This work was supported by a Career Development Award to Dr Wolf from the VA Clinical Science Research and Development Program. Dr Miller’s contribution was supported by a VA Clinical Science Research and Development Merit Review Award.
Role of the sponsors: The study sponsors had no role in the study design, collection, analysis, or interpretation of data; writing of the report; or the decision to submit the report for publication.
Disclaimer: The views and opinions expressed in this report are those of the authors and should not be construed to represent the views of sponsoring organizations, agencies, or the US government.
Acknowledgment: The authors thank Annie LeDoux, BA, VA Boston Healthcare System, who assisted with formatting of this article. Ms LeDoux has no conflicts of interest to disclose.
Additional information: The VA National Center for PTSD funded data collection for the National Health and Resilience in Veterans Study (NHRVS). Individuals interested in collaborating on NHRVS-related projects should contact Dr Pietrzak ([email protected]).
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Richardson LK, Frueh BC, Acierno R. Prevalence estimates of combat-related post-traumatic stress disorder: critical review. Aust N Z J Psychiatry. 2010;44(1):4-19. PubMed doi:10.3109/00048670903393597
2. Seal KH, Bertenthal D, Miner CR, et al. Bringing the war back home: mental health disorders among 103,788 US veterans returning from Iraq and Afghanistan seen at Department of Veterans Affairs facilities. Arch Intern Med. 2007;167(5):476-482. PubMed doi:10.1001/archinte.167.5.476
3. Kessler RC, Berglund P, Demler O, et al. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2005;62(6):593-602. PubMed doi:10.1001/archpsyc.62.6.593
4. Pietrzak RH, Goldstein RB, Southwick SM, et al. Prevalence and Axis I comorbidity of full and partial posttraumatic stress disorder in the United States: results from Wave 2 of the National Epidemiologic Survey on Alcohol and Related Conditions. J Anxiety Disord. 2011;25(3):456-465. PubMed doi:10.1016/j.janxdis.2010.11.010
5. United States Department of Veterans Affairs; Westat. National Survey of Veterans, Active Duty Service Members, Demobilized National Guard and Reserve Members, Family Members, and Surviving Spouses: Final report, deliverable 27. http://www.va.gov/SURVIVORS/docs/NVSSurveyFinalWeightedReport.pdf. Updated October 18, 2010. Accessed September 22, 2014.
6. Böttche M, Kuwert P, Knaevelsrud C. Posttraumatic stress disorder in older adults: an overview of characteristics and treatment approaches. Int J Geriatr Psychiatry. 2012;27(3):230-239. PubMed doi:10.1002/gps.2725
7. Lapp LK, Agbokou C, Ferreri F. PTSD in the elderly: the interaction between trauma and aging. Int Psychogeriatr. 2011;23(6):858-868. PubMed doi:10.1017/S1041610211000366
8. Tolin DF, Foa EB. Sex differences in trauma and posttraumatic stress disorder: a quantitative review of 25 years of research. Psychol Bull. 2006;132(6):959-992. PubMed doi:10.1037/0033-2909.132.6.959
9. Dohrenwend BP, Turner JB, Turse NA, et al. The psychological risks of Vietnam for US veterans: a revisit with new data and methods. Science. 2006;313(5789):979-982. PubMed doi:10.1126/science.1128944
10. Kulka RA, Schlenger WE, Fairbank JA, et al. Trauma and the Vietnam War Generation: Report of Findings From the National Vietnam Veterans Readjustment Study. New York, NY: Brunner/Mazel;1990
11. Kang HK, Natelson BH, Mahan CM, et al. Post-traumatic stress disorder and chronic fatigue syndrome-like illness among Gulf War veterans: a population-based survey of 30,000 veterans. Am J Epidemiol. 2003;157(2):141-148. PubMed doi:10.1093/aje/kwf187
12. Clancy CP, Graybeal A, Tompson WP, et al. Lifetime trauma exposure in veterans with military-related posttraumatic stress disorder: association with current symptomatology. J Clin Psychiatry. 2006;67(9):1346-1353. PubMed doi:10.4088/JCP.v67n0904
13. Dedert EA, Green KT, Calhoun PS, et al. Association of trauma exposure with psychiatric morbidity in military veterans who have served since September 11, 2001. J Psychiatr Res. 2009;43(9):830-836. PubMed doi:10.1016/j.jpsychires.2009.01.004
14. Van Voorhees EE, Dedert EA, Calhoun PS, et al; VA Mid-Atlantic MIRECC Workgroup. Childhood trauma exposure in Iraq and Afghanistan war era veterans: implications for posttraumatic stress disorder symptoms and adult functional social support. Child Abuse Negl. 2012;36(5):423-432. PubMed doi:10.1016/j.chiabu.2012.03.004
15. Keane TM, Wolfe J. Comorbidity in post-traumatic stress disorder: an analysis of community and clinical studies. J Appl Soc Psychol. 1990;20(21):1776-1788. doi:10.1111/j.1559-1816.1990.tb01511.x
16. Kessler RC, Sonnega A, Bromet E, et al. Posttraumatic stress disorder in the National Comorbidity Survey. Arch Gen Psychiatry. 1995;52(12):1048-1060. PubMed doi:10.1001/archpsyc.1995.03950240066012
17. Cougle JR, Keough ME, Riccardi CJ, et al. Anxiety disorders and suicidality in the National Comorbidity Survey-Replication. J Psychiatr Res. 2009;43(9):825-829. PubMed doi:10.1016/j.jpsychires.2008.12.004
18. Jakupcak M, Cook J, Imel Z, et al. Posttraumatic stress disorder as a risk factor for suicidal ideation in Iraq and Afghanistan War veterans. J Trauma Stress. 2009;22(4):303-306. PubMed doi:10.1002/jts.20423
19. Pietrzak RH, Goldstein MB, Malley JC, et al. Risk and protective factors associated with suicidal ideation in veterans of Operations Enduring Freedom and Iraqi Freedom. J Affect Disord. 2010;123(1-3):102-107. PubMed doi:10.1016/j.jad.2009.08.001
20. Wisco BE, Marx BP, Holowka DW, et al. Traumatic brain injury, PTSD, and current suicidal ideation among Iraq and Afghanistan US veterans. J Trauma Stress. 2014;27(2):244-248. PubMed doi:10.1002/jts.21900
21. Breslau N, Kessler RC, Chilcoat HD, et al. Trauma and posttraumatic stress disorder in the community: the 1996 Detroit Area Survey of Trauma. Arch Gen Psychiatry. 1998;55(7):626-632. PubMed doi:10.1001/archpsyc.55.7.626
22. Ozer EJ, Best SR, Lipsey TL, et al. Predictors of posttraumatic stress disorder and symptoms in adults: a meta-analysis. Psychol Bull. 2003;129(1):52-73. PubMed doi:10.1037/0033-2909.129.1.52
23. Barrett DH, Doebbeling CC, Schwartz DA, et al. Posttraumatic stress disorder and self-reported physical health status among US military personnel serving during the Gulf War period: a population-based study. Psychosomatics. 2002;43(3):195-205. PubMed doi:10.1176/appi.psy.43.3.195
24. Charuvastra A, Cloitre M. Social bonds and posttraumatic stress disorder. Annu Rev Psychol. 2008;59(1):301-328. PubMed doi:10.1146/annurev.psych.58.110405.085650
25. Pietrzak RH, Cook JM. Psychological resilience in older US veterans: results from the national health and resilience in veterans study. Depress Anxiety. 2013;30(5):432-443. PubMed doi:10.1002/da.22083
26. Vahia IV, Chattillion E, Kavirajan H, et al. Psychological protective factors across the lifespan: implications for psychiatry. Psychiatr Clin North Am. 2011;34(1):231-248. PubMed doi:10.1016/j.psc.2010.11.011
27. Pietrzak RH, Tsai J, Kirwin PD, et al. Successful aging among older veterans in the United States. Am J Geriatr Psychiatry. 2014;22(6):551-563. PubMed doi:10.1016/j.jagp.2012.11.018
28. United States Census Bureau. American Community Survey website. 2010. http://factfinder2.census.gov/faces/tableservices/jsf/pages/productview.xhtml?pid=ACS_10_1YR_S2101&prodType=table. Accessed July 28, 2014.
29. Carlson EB, Smith SR, Palmieri PA, et al. Development and validation of a brief self-report measure of trauma exposure: the Trauma History Screen. Psychol Assess. 2011;23(2):463-477. PubMed doi:10.1037/a0022294
30. Keane TM, Fairbank JA, Caddell JM, et al. Clinical evaluation of a measure to assess combat exposure. Psychol Assess. 1989;1(1):53-55. doi:10.1037/1040-3590.1.1.53
31. Weathers FW, Litz BT, Herman DS, et al. The PTSD Checklist (PCL): reliability, validity, and diagnostic utility. Presented at the Annual Meeting of the International Society for Traumatic Stress Studies, Vol 141; October 1993; San Antonio, TX.
32. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
33. Sheehan DV, Lecrubier Y, Sheehan KH, et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry. 1998;59(suppl 20):22-33, quiz 34-57. PubMed
34. Kroenke K, Spitzer RL, Williams JBW, et al. An ultra-brief screening scale for anxiety and depression: the PHQ-4. Psychosomatics. 2009;50(6):613-621. PubMed
35. Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16(9):606-613. PubMed doi:10.1046/j.1525-1497.2001.016009606.x
36. Campbell-Sills L, Stein MB. Psychometric analysis and refinement of the Connor-Davidson Resilience Scale (CD-RISC): Validation of a 10-item measure of resilience. J Trauma Stress. 2007;20(6):1019-1028. PubMed doi:10.1002/jts.20271
37. Scheier MF, Carver CS, Bridges MW. Distinguishing optimism from neuroticism (and trait anxiety, self-mastery, and self-esteem): a reevaluation of the Life Orientation Test. J Pers Soc Psychol. 1994;67(6):1063-1078. PubMed doi:10.1037/0022-3514.67.6.1063
38. Mccullough ME, Emmons RA, Tsang J-A. The grateful disposition: a conceptual and empirical topography. J Pers Soc Psychol. 2002;82(1):112-127. PubMed doi:10.1037/0022-3514.82.1.112
39. Kashdan TB, Gallagher MW, Silvia PJ, et al. The Curiosity and Exploration Inventory-2: development, factor structure, and psychometrics. J Res Pers. 2009;43(6):987-998. PubMed doi:10.1016/j.jrp.2009.04.011
40. Schulenberg SE, Schnetzer LW, Buchanan EM. The Purpose in Life Test-Short Form: development and psychometric support. J Happiness Stud. 2011;12(5):861-876. doi:10.1007/s10902-010-9231-9
41. Hazan C, Shaver PR. Love and work: an attachment-theoretical perspective. J Pers Soc Psychol. 1990;59(2):270-280. doi:10.1037/0022-3514.59.2.270
42. Sherbourne CD, Stewart AL. The MOS social support survey. Soc Sci Med. 1991;32(6):705-714. PubMed doi:10.1016/0277-9536(91)90150-B
43. Sledjeski EM, Speisman B, Dierker LC. Does number of lifetime traumas explain the relationship between PTSD and chronic medical conditions? Answers from the National Comorbidity Survey-Replication (NCS-R). J Behav Med. 2008;31(4):341-349. PubMed doi:10.1007/s10865-008-9158-3
44. Stein MB, Walker JR, Hazen AL, et al. Full and partial posttraumatic stress disorder: findings from a community survey. Am J Psychiatry. 1997;154(8):1114-1119. PubMed
45. Breslau N. The epidemiology of trauma, PTSD, and other posttrauma disorders. Trauma Violence Abuse. 2009;10(3):198-210. PubMed doi:10.1177/1524838009334448
46. LeardMann CA, Powell TM, Smith TC, et al. Risk factors associated with suicide in current and former US military personnel. JAMA. 2013;310(5):496-506. PubMed doi:10.1001/jama.2013.65164
47. Frueh BC, Hamner MB, Cahill SP, et al. Apparent symptom overreporting in combat veterans evaluated for PTSD. Clin Psychol Rev. 2000;20(7):853-885. PubMed doi:10.1016/S0272-7358(99)00015-X
48. Rogers R. Clinical Assessment of Malingering and Deception. New York, NY: Guilford Press; 2008.
49. Thoits PA, Hewitt LN. Volunteer work and well-being. J Health Soc Behav. 2001;42(2):115-131. PubMed doi:10.2307/3090173
50. Penner LA, Dovidio JF, Piliavin JA, et al. Prosocial behavior: multilevel perspectives. Annu Rev Psychol. 2005;56(1):365-392. PubMed doi:10.1146/annurev.psych.56.091103.070141
51. Cloitre M, Koenen KC, Cohen LR, et al. Skills training in affective and interpersonal regulation followed by exposure: a phase-based treatment for PTSD related to childhood abuse. J Consult Clin Psychol. 2002;70(5):1067-1074. PubMed doi:10.1037/0022-006X.70.5.1067
52. Bleiberg KL, Markowitz JC. A pilot study of interpersonal psychotherapy for posttraumatic stress disorder. Am J Psychiatry. 2005;162(1):181-183. PubMed doi:10.1176/appi.ajp.162.1.181
53. McDonald SD, Calhoun PS. The diagnostic accuracy of the PTSD checklist: a critical review. Clin Psychol Rev. 2010;30(8):976-987. PubMed doi:10.1016/j.cpr.2010.06.012
54. Forbes D, Creamer M, Biddle D. The validity of the PTSD checklist as a measure of symptomatic change in combat-related PTSD. Behav Res Ther. 2001;39(8):977-986. PubMed doi:10.1016/S0005-7967(00)00084-X
55. Terhakopian A, Sinaii N, Engel CC, et al. Estimating population prevalence of posttraumatic stress disorder: an example using the PTSD checklist. J Trauma Stress. 2008;21(3):290-300. PubMed doi:10.1002/jts.20341
56. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition. Washington, DC: American Psychiatric Association; 2013.