ABSTRACT
Objective: Patients with schizophrenia may exhibit symptoms of hostility. HP-3070 is the first antipsychotic patch approved by the US Food and Drug Administration (FDA) for adults with schizophrenia. Its efficacy was demonstrated in a phase 3 study. This post hoc analysis assessed the efficacy of HP-3070 in treating hostility in schizophrenia.
Methods: In the pivotal phase 3 study, conducted between August 2016 and November 2017, adults with schizophrenia (per DSM-5 criteria) were randomized to HP-3070 3.8 mg/24 h, HP-3070 7.6 mg/24 h, or placebo. Least-squares mean (LSM) changes in Positive and Negative Syndrome Scale (PANSS) hostility item and PANSS–Excited Component (PANSS-EC) scores from baseline to week 6 were assessed post hoc using a mixed-effects model for repeated measures adjusted for selected PANSS-Positive symptoms and presence of somnolence or akathisia.
Results: Among 442 patients with baseline PANSS hostility item score > 1 (n = 151, HP-3070 7.6 mg/24 h; n = 147, 3.8 mg/24 h; n = 144, placebo), week 6 LSM (95% CI) change from baseline (CFB) in hostility score was superior with HP-3070 versus placebo for 7.6 mg/24 h (−0.4 [−0.6 to −0.2]; P < .001) and 3.8 mg/24 h (−0.3 [−0.6 to −0.1]; P < .01), with similar results for 7.6 mg/24 h after adjusting for covariates (P < .05). For all patients regardless of baseline PANSS hostility item score, PANSS-EC week 6 LSM CFB was greater for HP-3070 7.6 mg/24 h (−1.1 [−1.9 to −0.4]; n = 203; P < .01) and 3.8 mg/24 h (−1.3 [−2.0 to −0.6]; n = 201; P < .001) than for placebo (n = 203), with similar results observed in patients with baseline hostility item score > 1.
Conclusions: In this post hoc analysis, HP-3070 was superior to placebo in reducing schizophrenia-associated hostility, even after adjusting for covariates, suggesting these effects are at least partially independent of general antipsychotic effects or effects on sedation or akathisia. These findings suggest HP-3070 has a specific antihostility effect in patients with schizophrenia.
Clinical Trials Registration: ClinicalTrials.gov identifier: NCT02876900; EudraCT number: 2015–005134-21
J Clin Psychiatry 2022;83(4):21m14355
To cite: Citrome L, Komaroff M, Starling B, et al. Efficacy of HP-3070, an asenapine transdermal system, on symptoms of hostility in adults with schizophrenia: a post hoc analysis of a 6-week phase 3 study. J Clin Psychiatry. 2022;83(4):21m14355.
To share: https://doi.org/10.4088/JCP.21m14355
© 2022 Physicians Postgraduate Press, Inc.
aPsychiatry and Behavioral Sciences, New York Medical College, Valhalla, New York
bResearch and Development, Noven Pharmaceuticals, Inc., Jersey City, New Jersey
cHisamitsu Pharmaceutical Co, Inc., Chiyoda-ku, Tokyo, Japan
*Corresponding author: Leslie Citrome, MD, MPH, Clinical Professor, Department of Psychiatry and Behavioral Sciences, New York Medical College, 40 Sunshine Cottage Rd, Valhalla, NY 10595 ([email protected]).
See letter by El-Mallakh
Patients with schizophrenia are known to potentially exhibit aggressive, hostile behavior, especially during the acute phase of the illness, and this can present a danger to the patient and others, thus making effective management critical.1–4 The general topic of hostility, agitation, and aggression is of special relevance to inpatient and acute psychiatric services and to providers who are caring for patients with ongoing risk for such behaviors in outpatient settings, as in, for example, Assertive Community Treatment (ACT) programs. Of note are new workplace violence prevention standards directing hospitals to take actions to mitigate or resolve workplace violence risks.5
Hostility can be assessed using the Positive and Negative Syndrome Scale (PANSS),6 which defines it as “verbal and non-verbal expressions of anger and resentment, including sarcasm, passive-aggressive behavior, verbal abuse, and assaultiveness”(p50) and rates the hostility item on a scale of 1 (absent) to 7 (extreme). Clozapine was the first of the atypical antipsychotics to be identified as having a specific antihostility effect,7–9 and similar effects have been observed in other second-generation antipsychotics, including aripiprazole, risperidone, and lurasidone,10–12 as also reviewed by Citrome and Volavka.2 Specific antihostility effects of asenapine in the treatment of schizophrenia have not been reported in the published literature, although a poster has been presented of a post hoc analysis in which the effects of sublingual asenapine on hostility remained significant after adjustment for positive symptoms and sedation at some visits but not at the study endpoint.13
HP-3070 (asenapine) is the first transdermal system (patch) approved by the US Food and Drug Administration (FDA) for use in adults with schizophrenia.14,15 In a phase 3 randomized controlled trial,16 once-daily applications of HP-3070 7.6 mg/24 h and 3.8 mg/24 h were found to demonstrate significant improvement versus placebo in PANSS total scores after 2–3 weeks of treatment, continuing through week 6 of treatment. HP-3070 was well-tolerated, with a systemic safety profile similar to that of sublingual asenapine.16 A post hoc analysis of this trial was performed to investigate the specific effect of the HP-3070 asenapine transdermal system on the symptoms of hostility and agitation in adults with schizophrenia.
METHODS
Trial Design and Participants
This study was a post hoc analysis of data from the HP-3070 phase 3 randomized, double-blind, placebo-controlled trial (ClinicalTrials.gov identifier: NCT02876900) conducted between August 2016 and November 2017.16 The analyses included data from the full analysis set of study participants and from the subset of participants with evidence of hostility at baseline (PANSS hostility item score > 1 at baseline).
Detailed methods of the phase 3 trial have been previously published.16 Briefly, study participants were adults with schizophrenia (Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition [DSM-5] criteria) experiencing acute exacerbations at the time of screening. Eligible patients had a Clinical Global Impressions–Severity of Illness scale (CGI-S) score of ≥ 4 and PANSS total score of ≥ 80, with scores of ≥ 4 in ≥ 2 of the PANSS items for conceptual disorganization, delusions, hallucinatory behavior, and unusual thought content at screening and baseline. Exclusion criteria included schizophrenia diagnosis < 6 months prior to screening or a current DSM-5 diagnosis other than schizophrenia. Patients were also excluded if they were known to be resistant/refractory to antipsychotic treatment, including asenapine. No other antipsychotics, antidepressants, mood stabilizers, stimulants, or non-psychopharmacologic medications with psychotropic properties were permitted, with the exception of a limited number of psychotropic medications for specific conditions: lorazepam (for insomnia, agitation, or anxiety only; if lorazepam was not available, another available benzodiazepine may have been approved), benztropine (for treatment-emergent extrapyramidal symptoms), zolpidem (for insomnia), and propranolol (for akathisia). Medications used for chronic non-psychiatric medical conditions were allowed if the condition and treatment regimen were stable before screening.
After a 3- to 14-day screening/run-in period, eligible patients were randomized to HP-3070 7.6 mg/24 h, HP-3070 3.8 mg/24 h, or placebo in the form of patches applied daily for 6 weeks. Patches were applied by study personnel, and application sites (abdomen, hip, upper arm, upper back, and upper chest) were rotated daily.
The study protocol was approved by an independent ethics committee or review board at each study center. Written informed consent was obtained from all participants.
Study Endpoints
Least-squares mean (LSM) changes from baseline to week 6 in the PANSS hostility item score (P7, 1 = absent to 7 = extreme) were assessed post hoc in patients with hostility item score > 1 at baseline.6,10 LSM changes from baseline to week 6 in the PANSS–Excited Component (PANSS-EC; the sum of items P4 [excitement], P7 [hostility], G4 [tension], G8 [uncooperativeness], and G14 [poor impulse control]) were assessed post hoc in all patients and in patients with hostility item score > 1 at baseline. The PANSS-EC is an accepted outcome measure for agitation.6,10,17,18
Statistical Methods
Reductions in PANSS hostility item score and PANSS-EC score were evaluated using a mixed-effects model for repeated-measures (MMRM) analysis with treatment group, visit, treatment by visit, country, and baseline hostility item (P7) score as fixed effects.2,10 Additional analyses were performed to adjust for select covariates in the model, including both PANSS-Positive symptoms of schizophrenia, calculated as a sum of the P1 [delusions], P2 [conceptual disorganization], P3 [hallucinatory behavior], P5 [grandiosity], P6 [suspiciousness/persecution], and G9 [unusual thought content] items, and presence of somnolence, including hypersomnia, hypersomnolence, and sedation, or akathisia reported as adverse events.10
Change in hostility status over time was also analyzed using generalized estimating equations (GEE).19 GEE can be used to analyze categorical data (binary or polychotomous). In this analysis, hostility item was a polychotomous categorical variable. Treatment group was the between-subject variable, and time was the within-subject (repeated-measures) factor. Time (overall change over time) and the interaction effect between group and time (group difference in change over time) were the effects of interest in this analysis.
Effect size for change in hostility status over time was estimated using the odds ratios (ORs) derived from the GEE.19 ORs indicate the odds of shifting 1 point down on the hostility item in the HP-3070 group versus the placebo group, with OR > 1 indicating superiority for HP-3070.
All statistical tests of treatment effects were performed at a 2-sided significance level of .05. Confidence intervals (CIs) were reported at 95%. No formal power analysis was conducted. All results presented here are considered descriptive.
RESULTS
Baseline Characteristics
In total, 616 eligible patients provided informed consent and were randomized into HP-3070 7.6 mg/24 h, HP-3070 3.8 mg/24 h, and placebo treatment groups (intent-to-treat [ITT] analysis set). Of these patients, 614 received ≥ 1 dose of study medication, forming the safety analysis set (SAS), and 607 had ≥ 1 additional post-baseline assessment of PANSS total score (full analysis set [FAS]).16
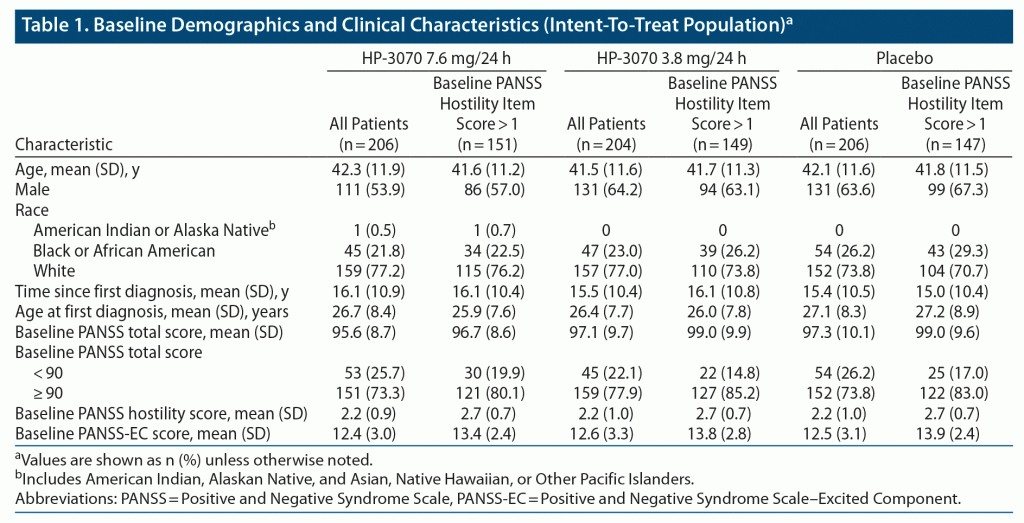
Detailed baseline characteristics for this study population have already been reported.16 Demographics and baseline disease characteristics were balanced between the HP-3070 and placebo treatment groups in the ITT analysis set, as previously reported (Table 1). Slightly more than half of the patients were male, and three-fourths were White. The mean age was 42 years. More than half of the patients received an initial schizophrenia diagnosis ≥ 10 years prior, and the mean time since initial diagnosis was 15.7 years.
Among the subset of patients with PANSS hostility item score > 1 at baseline (n = 447), demographic characteristics were similarly balanced (Table 1). Mean age and demographic background were similar to those in the ITT population. Age at initial schizophrenia diagnosis was similar between treatment groups and similar to that in the full population. Baseline PANSS total scores, PANSS hostility scores, and PANSS-EC scores were also similar between treatment groups.
Concomitant Medications
There were no marked differences in the use of permitted psychoactive concomitant medications across the treatment groups.
PANSS Hostility Item Score
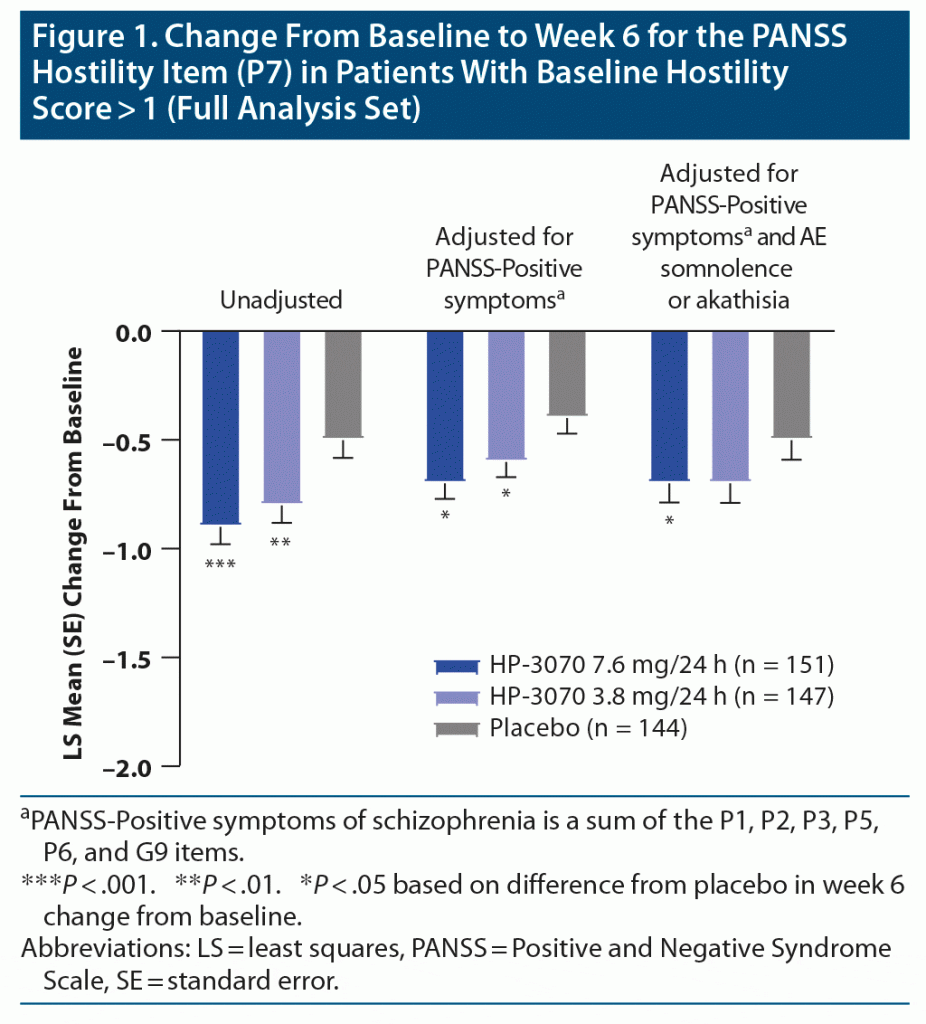
Among the 607 patients in the FAS, 442 had a PANSS hostility item score > 1 at baseline. In patients with evidence of hostility at baseline, a statistically significant improvement from baseline to week 6 in the PANSS hostility item score was observed for both HP-3070 doses compared to placebo (Figure 1 and Supplementary Table 1). The LS mean difference (95% CI) in change from baseline was −0.4 (−0.6 to −0.2; P < .001) for HP-3070 7.6 mg/24 h versus placebo. For HP-3070 3.8 mg/24 h, the LS mean difference from placebo in change from baseline to week 6 was −0.3 (−0.6 to −0.1; P < .01).
The improvements from baseline to week 6 compared to placebo remained significant when PANSS-Positive symptoms and somnolence or akathisia were included as additional covariates (Figure 1 and Supplementary Table 1). After adjusting for PANSS-Positive symptoms of schizophrenia, LS mean difference from placebo in change from baseline to week 6 was −0.3 (−0.4 to −0.1; P < .05) for HP-3070 7.6 mg/24 h and −0.2 (−0.4 to 0; P < .05) for HP-3070 3.8 mg/24 h. After adjusting for PANSS-Positive symptoms of schizophrenia and for the presence of adverse events of somnolence or akathisia, LS mean difference from placebo in change from baseline to week 6 was −0.2 (−0.4 to −0.1; P < .05) for HP-3070 7.6 mg/24 h and −0.2 (−0.4 to 0; P = .052) for HP-3070 3.8 mg/24 h.
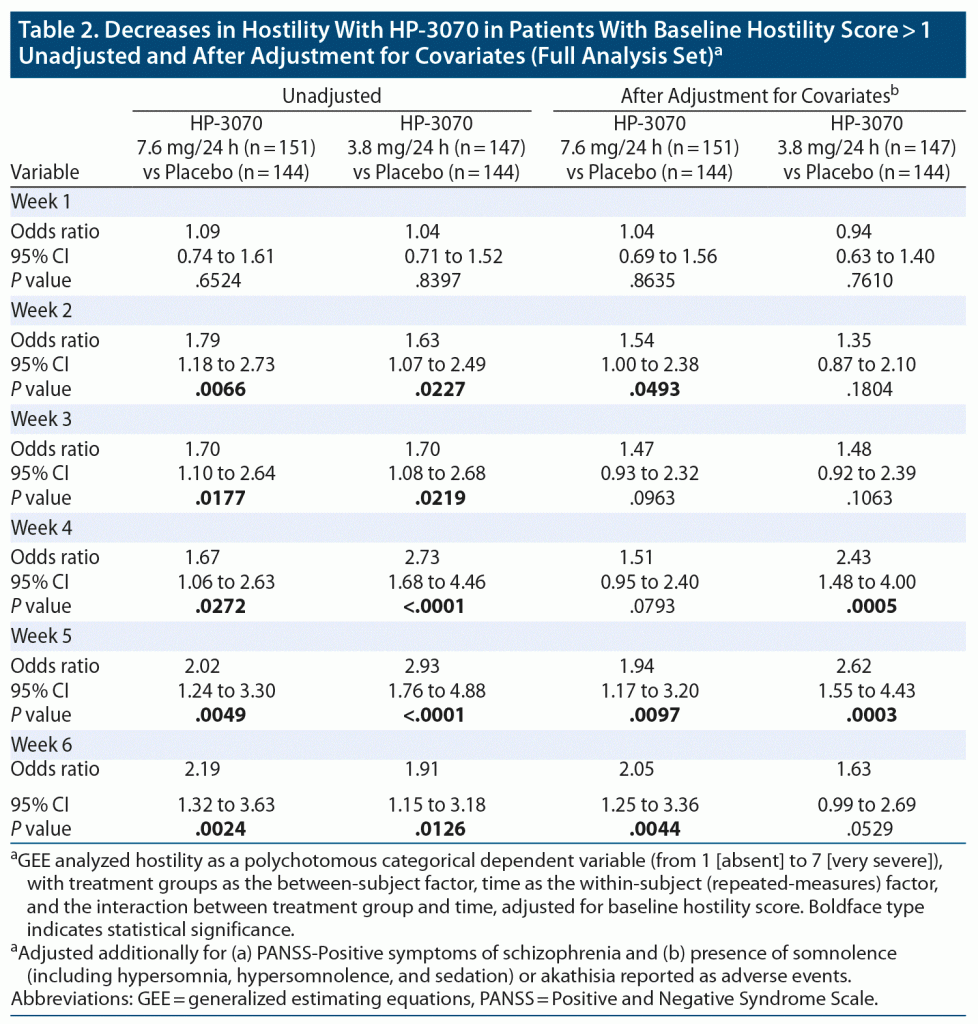
When examining downward shifts in hostility item scores among patients in whom hostility was present at baseline (hostility item score > 1), both HP-3070 7.6 mg/24 h and 3.8 mg/24 h treatments were superior to placebo in the likelihood of reduction in hostility, shown as OR > 1 for effect of treatment and time, starting at week 2 of treatment and continuing through week 6 (Table 2).
When PANSS-Positive symptoms of schizophrenia and presence of somnolence or akathisia were added as covariates, HP-3070 7.6 mg/24 h was found to be superior to placebo in reducing hostility at weeks 2, 5, and 6, and HP-3070 3.8 mg/24 h was superior to placebo at weeks 4 and 5 (Table 2).
PANSS–Excited Component
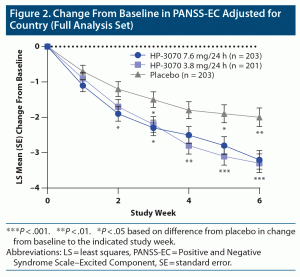
In the overall population, a significant improvement in the LS mean change from baseline for PANSS-EC was observed for both HP-3070 doses compared to placebo (Figure 2 and Supplementary Table 2). For HP-3070 7.6 mg/24 h, a significant improvement from baseline compared with placebo was observed at weeks 2, 3, 5, and 6. At week 6, the LS mean (95% CI) change from baseline compared to placebo was −1.1 (−1.9 to −0.4; P < .01). For HP-3070 3.8 mg/24 h, significant improvement from baseline compared with placebo was observed from week 3 and continued through week 6. The week 6 LS mean change from baseline versus placebo was −1.3 (−2.0 to −0.6; P < .001).
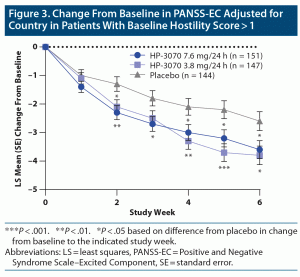
Among patients in whom hostility was present at baseline (baseline hostility item score > 1), significant improvement in PANSS-EC LS mean change from baseline was also observed for both HP-3070 doses compared to placebo (Figure 3 and Supplementary Table 3). Treatment with HP-3070 7.6 mg/24 h resulted in significant improvement from baseline compared with placebo from week 2 continuing through week 6. At week 6, the LS mean (95% CI) change from baseline compared with placebo was −1.0 (−1.9 to −0.1; P < .05). For HP-3070 3.8 mg/24 h, significant improvement from baseline compared with placebo was observed at week 2 and then from weeks 4 through 6. The week 6 LS mean change from baseline versus placebo was −1.2 (−2.1 to −0.3; P < .05).
DISCUSSION
Once-daily treatment with the HP-3070 transdermal system at both 7.6- and 3.8-mg/24 h doses has been shown to be effective and well-tolerated for treatment of schizophrenia in adults.16 Managing hostile behavior remains a significant treatment challenge among some patients with schizophrenia. Hostility can be defined as an underlying negative attitude toward situations and other people.2 Although not all people with measurable hostility are agitated, aggressive, or violent, their interpersonal interactions can be strained because of hostility.2 In other instances, individuals who have a hostile attitude can become agitated, and subsequently this agitation can escalate into aggression. A national US study of violence in schizophrenia found that “for each unit increase on the 7-point rating of hostility [PANSS hostility item score], the odds of serious violence increased by a factor of 1.65 (P < .001).”20(p493)
In this post hoc analysis of the phase 3 trial, treatment with HP-3070 led to significant improvement in the PANSS hostility item among adults with schizophrenia. After 6 weeks of treatment with HP-3070 7.6 mg/24 h or 3.8 mg/24 h, significant improvement from baseline in PANSS hostility item scores was observed relative to placebo among patients with a hostility score > 1 at baseline. This observation was supported by the significant improvement in agitation as measured by the PANSS-EC, both among the overall study population and in patients in whom hostility was present at baseline.
These effects of HP-3070 treatment on the PANSS hostility item score remained even after adjustment for confounding variables, suggesting that the effect of HP-3070 on reducing symptoms of hostility may be at least partially independent of general antipsychotic effects on hallucinations or delusions or the presence or absence of relevant medication-induced adverse effects such as sedation or akathisia.
Effects on hostility in patients with schizophrenia have been observed for several other atypical antipsychotics, as reviewed by Citrome and Volavka,2 who concluded that clozapine and olanzapine had the strongest clinical evidence for a specific effect on symptoms of hostility, based on the availability of specifically designed randomized controlled studies. To date, only a single post hoc study of pooled data from phase 3 randomized controlled trials, presented as a poster,13 has addressed the effect of asenapine on hostility symptoms in patients with schizophrenia. Findings were comparable to those obtained in this post hoc analysis: improvement in PANSS hostility item score was observed after 6 weeks of twice-daily treatment with sublingual asenapine compared to placebo treatment.13,21,22 However, the statistically significant difference between asenapine and placebo treatment was lost by the end of the study after adjusting for PANSS-Positive symptoms and sedation.13
A limitation of this study is that it was conducted post hoc, limiting the strength of the conclusions. In addition, the mean baseline PANSS hostility score was low, even among patients with a hostility score > 1 at baseline, translating to a severity level of minimal to mild. This limits the generalizability of the results of this analysis. Randomized controlled trials that include pre-specified analyses addressing hostility and that are conducted in a population of patients selected for their hostile and aggressive behavior would provide additional confidence in these findings.
As a treatment for schizophrenia, HP-3070 demonstrated a consistent effect on both hostility and the Excited Component of the PANSS, providing good control over this constellation of symptoms, which can be of considerable concern in the treatment of individuals with schizophrenia. The once-daily transdermal formulation may address some of the challenges associated with sublingual asenapine or other oral treatments that are administered twice daily, such as low adherence, as well as providing an alternative for those individuals who would like to avoid oral medications and are reluctant to accept an injectable formulation.
Submitted: December 10, 2021; accepted April 19, 2022.
Published online: June 6, 2022.
Relevant financial relationships: Dr Citrome received non-financial support from Hisamitsu Pharmaceutical Co, Inc., and personal fees from Noven Pharmaceuticals, Inc., during the conduct of the study; personal fees from AbbVie/Allergan, Acadia, Adamas, Alkermes, Angelini, Astellas, Avanir, Axsome, BioXcel, Boehringer Ingelheim, Cadent Therapeutics, Eisai, Enteris BioPharma, HLS Therapeutics, Impel, Intra-Cellular Therapies, Janssen, Karuna, Lundbeck, Lyndra, MedAvante-ProPhase, Merck, Neurocrine, Novartis, Noven, Otsuka, Ovid, Relmada, Reviva, Sage, Sunovion, Takeda, Teva, and University of Arizona and for one-off ad hoc consulting for individuals/entities conducting marketing, commercial or scientific scoping research and CME activities organized by medical education companies such as Medscape, NACCME, NEI, and Vindico and universities and professional organizations/societies, outside the submitted work. He has stocks (small number of shares of common stock) in Bristol-Myers Squibb, Eli Lilly, Johnson & Johnson, Merck, and Pfizer purchased > 10 years ago and has received royalties from Springer Healthcare (book), UpToDate (reviewer), Wiley (Editor-in-Chief, International Journal of Clinical Practice, through end of 2019), and Elsevier (Topic Editor, Psychiatry, Clinical Therapeutics). Drs Komaroff and Starling and Mr Byreddy received non-financial support from Hisamitsu Pharmaceutical Co, Inc., during the conduct of the study and have received personal fees from Noven Pharmaceuticals, Inc., outside the submitted work. Dr Terahara and Ms Hasebe received non-financial support from Hisamitsu Pharmaceutical Co, Inc.; personal fees from Hisamitsu Pharmaceutical Co, Inc., outside the submitted work.
Funding/support: This study was funded by Hisamitsu Pharmaceutical Co, Inc.
Role of the sponsor: Although personnel at Hisamitsu Pharmaceutical Co, Inc., reviewed the manuscript, final approval for the decision to submit the manuscript was the sole decision of the authors.
Previous presentations: Presented as a poster at the Psych Congress; October 29–November 1, 2021; San Antonio, Texas; and the Neuroscience Education Institute (NEI) 2021 Congress; November 4–7, 2021; Colorado Springs, Colorado.
Acknowledgements: Medical writing and editorial assistance were provided by Michelle L. Jones, PhD, MWC, and Anthony DiLauro, PhD, of PharmaWrite, LLC, and were funded by Hisamitsu Pharmaceutical Co, Inc. This manuscript was prepared according to the International Society for Medical Publication Professionals’ “Good Publication Practice for Communicating Company-Sponsored Medical Research: The GPP3 Guidelines.”
Supplementary material: Available at Psychiatrist.com.
CLINICAL POINTS
- Patients with schizophrenia may exhibit aggressive, hostile behavior, which is important to effectively manage. Specific antihostility effects of some second-generation antipsychotics have been described, although they are not extensively reported for asenapine.
- Once-daily treatment with the asenapine transdermal system (HP-3070) at both 7.6- and 3.8-mg/24 h doses has been shown to be effective and well-tolerated for treatment of schizophrenia in adults.
- In this post hoc analysis of the pivotal study, HP-3070 was superior to placebo in reducing hostility in patients with schizophrenia, as measured by Positive and Negative Syndrome Scale (PANSS) hostility item and PANSS–Excited Component (PANSS-EC) scores, even after adjusting for covariates, suggesting a specific antihostility effect for HP-3070.
References (22)

- Citrome L, Volavka J. Pharmacological management of acute and persistent aggression in forensic psychiatry settings. CNS Drugs. 2011;25(12):1009–1021. PubMed CrossRef
- Citrome L, Volavka J. Specific anti-hostility effects of atypical antipsychotics in persons with schizophrenia: from clozapine to cariprazine. Harv Rev Psychiatry. 2021;29(1):20–34. PubMed CrossRef
- Volavka J, Citrome L. Pathways to aggression in schizophrenia affect results of treatment. Schizophr Bull. 2011;37(5):921–929. PubMed CrossRef
- Citrome L, Volavka J. The psychopharmacology of violence: making sensible decisions. CNS Spectr. 2014;19(5):411–418. PubMed CrossRef
- The Joint Commission. R3 report issue 30: workplace violence prevention standards. June 18, 2021. The Joint Commission website. https://www.jointcommission.org/-/media/tjc/documents/standards/r3-reports/wpvp-r3-30_revised_06302021.pdf. Accessed February 11, 2022.
- Kay SR, Opler LA, Fiszbein A, et al. Positive and Negative Syndrome Scale (PANSS) - Technical Manual. North Tonawanda, NY: Multi-Health Systems Inc; 2010.
- Volavka J, Zito JM, Vitrai J, et al. Clozapine effects on hostility and aggression in schizophrenia. J Clin Psychopharmacol. 1993;13(4):287–289. PubMed CrossRef
- Buckley P, Bartell J, Donenwirth K, et al. Violence and schizophrenia: clozapine as a specific antiaggressive agent. Bull Am Acad Psychiatry Law. 1995;23(4):607–611. PubMed
- Rabinowitz J, Avnon M, Rosenberg V. Effect of clozapine on physical and verbal aggression. Schizophr Res. 1996;22(3):249–255. PubMed CrossRef
- Citrome L, Du Y, Risinger R, et al. Effect of aripiprazole lauroxil on agitation and hostility in patients with schizophrenia. Int Clin Psychopharmacol. 2016;31(2):69–75. PubMed CrossRef
- Czobor P, Volavka J, Meibach RC. Effect of risperidone on hostility in schizophrenia. J Clin Psychopharmacol. 1995;15(4):243–249. PubMed CrossRef
- Citrome L, Pikalov A, Tocco M, et al. Effects of lurasidone on hostility in patients with an acute exacerbation of schizophrenia: a pooled post hoc analysis of 5 short-term studies. Eur Psychiatry. 2015;30(S1):249. CrossRef
- Citrome L, Landbloom R, Wu X, et al. Effect of asenapine on measures of hostility in adults with bipolar I disorder or schizophrenia [poster]. Presented at Annual Meeting of the American Society of Clinical Psychopharmacology (ASCP). May 30–June 3, 2016; Scottsdale, AZ.
- Secuado (asenapine) transdermal system [package insert]. Tosu, Japan: Hisamitsu Pharmaceutical Co, Inc; 2019.
- Noven Pharmaceuticals, Inc. US FDA approves SECUADO (asenapine) transdermal system, the first-and-only transdermal patch for the treatment of adults with schizophrenia [press release]. October 15, 2019. Noven website. http://www.noven.com/wp-content/uploads/2020/02/PR101519-1.pdf. Accessed October 23, 2019.
- Citrome L, Walling DP, Zeni CM, et al. Efficacy and safety of HP-3070, an asenapine transdermal system, in patients with schizophrenia: a phase 3, randomized, placebo-controlled study. J Clin Psychiatry. 2020;82(1):20m13602. PubMed
- Lindenmayer JP, Brown E, Baker RW, et al. An excitement subscale of the positive and negative syndrome scale. Schizophr Res. 2004;68(2–3):331–337. PubMed CrossRef
- Montoya A, Valladares A, Lizán L, et al. Validation of the Excited Component of the Positive and Negative Syndrome Scale (PANSS-EC) in a naturalistic sample of 278 patients with acute psychosis and agitation in a psychiatric emergency room. Health Qual Life Outcomes. 2011;9(1):18. PubMed CrossRef
- Citrome L, Volavka J, Czobor P, et al. Efficacy of ziprasidone against hostility in schizophrenia: post hoc analysis of randomized, open-label study data. J Clin Psychiatry. 2006;67(4):638–642. PubMed CrossRef
- Swanson JW, Swartz MS, Van Dorn RA, et al. A national study of violent behavior in persons with schizophrenia. Arch Gen Psychiatry. 2006;63(5):490–499. PubMed CrossRef
- Kane JM, Cohen M, Zhao J, et al. Efficacy and safety of asenapine in a placebo- and haloperidol-controlled trial in patients with acute exacerbation of schizophrenia. J Clin Psychopharmacol. 2010;30(2):106–115. PubMed CrossRef
- Potkin SG, Cohen M, Panagides J. Efficacy and tolerability of asenapine in acute schizophrenia: a placebo- and risperidone-controlled trial. J Clin Psychiatry. 2007;68(10):1492–1500. PubMed CrossRef
This PDF is free for all visitors!