Background: It has been proposed that relapse rates after antipsychotic discontinuation may be artificially inflated and that some of these symptom recurrences may be due to rebound or withdrawal phenomena rather than due to illness recurrence.
Methods: Post hoc analysis of data from a relapse-prevention study (conducted from March 2005 to February 2007) of paliperidone palmitate once-monthly (PP1M) versus placebo was conducted to compare the nature of operationally defined relapse events in schizophrenia patients (diagnosed by DSM-IV criteria) experiencing relapses after randomization to placebo (n = 97) with those in patients receiving maintenance PP1M treatment (n = 36). These 2 groups were compared for onset and severity of recurrence symptoms, symptom profiles at relapse, and postrelapse treatment response. Psychological and physiological signs of discontinuation and signs of antipsychotic tolerance, dyskinesia, and prolactin elevation that might indicate dopamine receptor supersensitivity were compared.
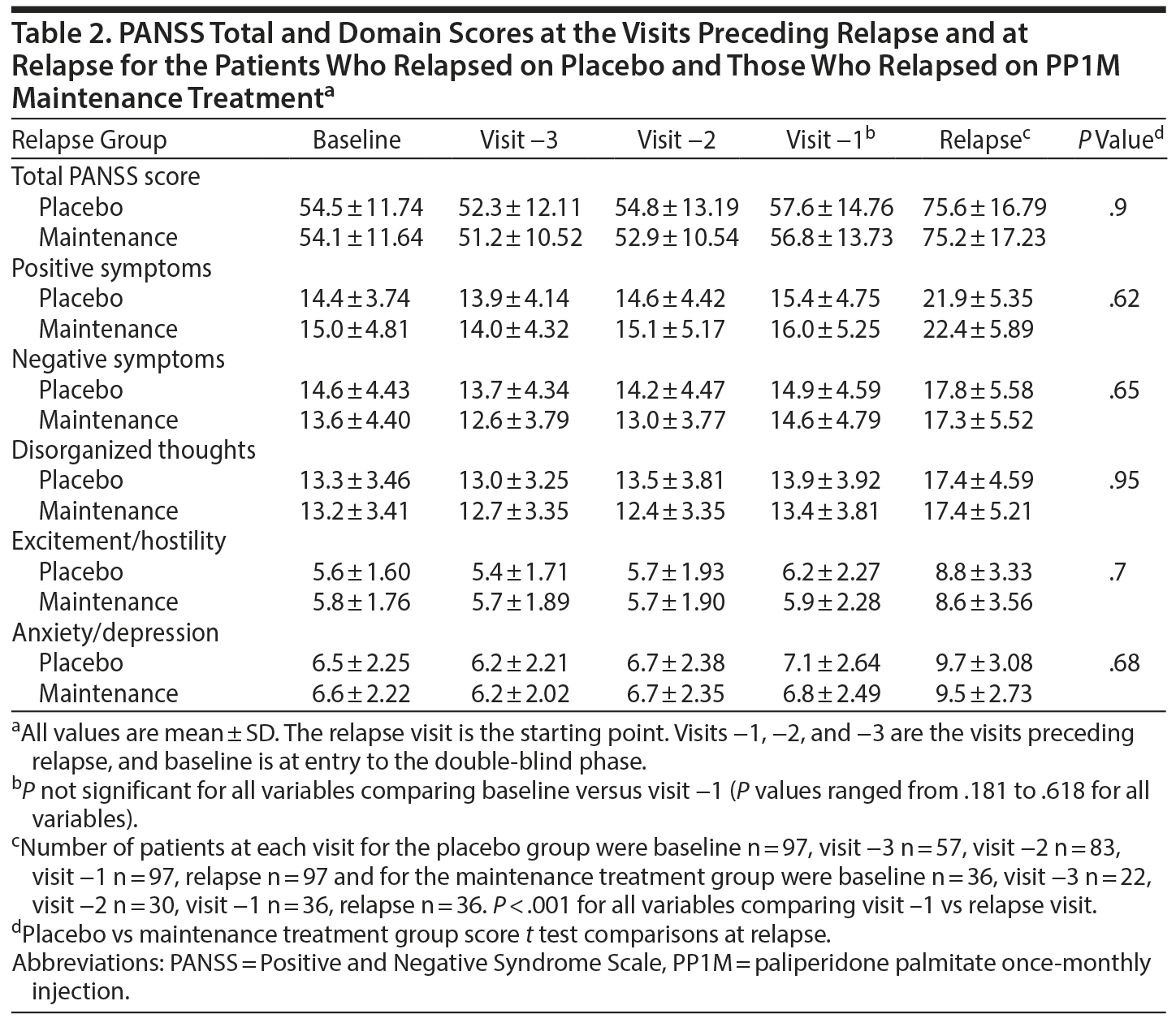
Results: Both groups were similar in terms of relapse symptom profiles, onset and severity of relapse symptoms, and postrelapse treatment response. The Positive and Negative Syndrome Scale total score (mean ± SD) for placebo versus maintenance treatment group at baseline was 54.5 ± 11.74 vs 54.1 ± 11.64 and at relapse was 75.6 ± 16.79 vs 75.2 ± 17.23 (P = .9). No elevated blood pressure or heart rate, dyskinesia, antipsychotic tolerance, or elevated prolactin in the patients relapsing after antipsychotic discontinuation was noted.
Conclusions: Findings suggest that relapses after treatment discontinuation reflect recurrence of the underlying illness and may be consistent with a hypothesis of direct relationship between dopamine and psychosis. No evidence was obtained for withdrawal-related phenomena contributing to the high relapse rates after treatment discontinuation.
Trial Registration: ClinicalTrials.gov identifier: NCT00111189
Relapse After Antipsychotic Discontinuation in Schizophrenia
as a Withdrawal Phenomenon vs Illness Recurrence:
A Post Hoc Analysis of a Randomized Placebo-Controlled Study
ABSTRACT
Background: It has been proposed that relapse rates after antipsychotic discontinuation may be artificially inflated and that some of these symptom recurrences may be due to rebound or withdrawal phenomena rather than due to illness recurrence.
Methods: Post hoc analysis of data from a relapse-prevention study (conducted from March 2005 to February 2007) of paliperidone palmitate once-monthly (PP1M) versus placebo was conducted to compare the nature of operationally defined relapse events in schizophrenia patients (diagnosed by DSM-IV criteria) experiencing relapses after randomization to placebo (n = 97) with those in patients receiving maintenance PP1M treatment (n = 36). These 2 groups were compared for onset and severity of recurrence symptoms, symptom profiles at relapse, and postrelapse treatment response. Psychological and physiological signs of discontinuation and signs of antipsychotic tolerance, dyskinesia, and prolactin elevation that might indicate dopamine receptor supersensitivity were compared.
Results: Both groups were similar in terms of relapse symptom profiles, onset and severity of relapse symptoms, and postrelapse treatment response. The Positive and Negative Syndrome Scale total score (mean ± SD) for placebo versus maintenance treatment group at baseline was 54.5 ± 11.74 vs 54.1 ± 11.64 and at relapse was 75.6 ± 16.79 vs 75.2 ± 17.23 (P = .9). No elevated blood pressure or heart rate, dyskinesia, antipsychotic tolerance, or elevated prolactin in the patients relapsing after antipsychotic discontinuation was noted.
Conclusions: Findings suggest that relapses after treatment discontinuation reflect recurrence of the underlying illness and may be consistent with a hypothesis of direct relationship between dopamine and psychosis. No evidence was obtained for withdrawal-related phenomena contributing to the high relapse rates after treatment discontinuation.
Trial Registration: ClinicalTrials.gov identifier: NCT00111189
J Clin Psychiatry 2018;79(4):17m11874
To cite: Emsley R, Nuamah I, Gopal S, et al. Relapse after antipsychotic discontinuation in schizophrenia as a withdrawal phenomenon vs illness recurrence: a post hoc analysis of a randomized placebo-controlled study. J Clin Psychiatry. 2018;79(4):17m11874.
To share: https://doi.org/10.4088/JCP.17m11874
© Copyright 2018 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Faculty of Medicine and Health Sciences, Stellenbosch University, Cape Town, South Africa
bJanssen Research & Development, LLC, Titusville, New Jersey
cDepartment of Psychiatry and Psychotherapy, Medical University Innsbruck, Innsbruck, Austria
*Corresponding author: Prof. Robin Emsley, DMed, DSc, Faculty of Medicine and Health Sciences, Stellenbosch University, PO Box 241, Tygerberg Campus 8000, Cape Town, South Africa ([email protected]).
The effectiveness of maintenance antipsychotic medication for preventing relapse in schizophrenia has been extensively documented,1 and treatment discontinuation studies report very high rates of relapse, even after a single episode of psychosis.2 For these reasons, long-term antipsychotic treatment has been the mainstay of treatment for schizophrenia.3 However, concerns have been raised recently about possible harmful effects of long-term antipsychotic treatment.4 In addition to studies citing the well-recognized side-effect burden accompanying antipsychotic treatment, a few studies5,6 suggest poorer outcome for patients who have had greater exposure to antipsychotic medication. These findings, together with those of a recent long-term study7 suggesting that a substantial number of patients stabilize and remain free of symptoms of psychosis without ongoing antipsychotic treatment, have reopened the debate on maintenance antipsychotic treatment in schizophrenia.8,9 Indeed, it has been proposed that the need for long-term antipsychotic maintenance treatment in schizophrenia should be reconsidered.4 One of the arguments put forth is that antipsychotic withdrawal studies are fundamentally flawed—that relapse rates may be artificially inflated and symptom exacerbation after treatment discontinuation may be caused by the process of drug withdrawal itself, rather than representing reemergence of symptoms of the underlying illness.10 Because many withdrawal studies do not define relapse precisely or they use a low threshold, it has been suggested that physiological discontinuation symptoms or the psychological reaction to treatment discontinuation could be mistaken for relapse.11 A more specific concern is that chronic administration of dopamine antagonists is in itself psychotogenic. Relapse risk after antipsychotic discontinuation is nonlinearly distributed over time with a large excess of risk within the first 3 months, thus suggesting the possibility of a withdrawal-related phenomenon.12
The concept of neuroleptic-induced supersensitivity psychosis (SSP) was originally introduced by Chouinard et al.13 According to the hypothesis, SSP is caused by alteration of mesolimbic or mesocortical dopamine receptors secondary to prolonged neuroleptic blockade, similar to the proposed mechanism of tardive dyskinesia involving changes in the neostriatum.14 Although the validity of SSP as a diagnostic entity has not been established,15 several studies have been conducted using the proposed SSP criteria of Chouinard.16 For example, 39% (16/41) of patients experiencing a psychotic relapse were regarded as having SSP,17 and an association between abnormal involuntary movements and psychotic relapse was reported in patients meeting SSP criteria.18 Also, SSP is proposed to be one cause of treatment-resistant schizophrenia.19,20
According to Chouinard and colleagues13 there are 2 proposed subtypes of SSP: (1) withdrawal type, characterized by rapid emergence of psychotic symptoms shortly after antipsychotic dose-reduction or discontinuation (oral antipsychotics: within 6 weeks; long-acting injectable (LAI) antipsychotics: 12 weeks), and (2) tardive type, with features including tolerance to antipsychotics and emergent refractoriness. Additional proposed withdrawal and tardive SSP features include the presence of tardive dyskinesia, rapid improvement in psychosis when antipsychotics are reintroduced, exacerbation of symptoms by stress, and high levels of prolactin. Some researchers4,17 propose that if symptom recurrence is related to the process of drug withdrawal itself, the psychosis should have its own distinct symptom profile. In particular, symptoms should be more severe, and symptoms associated with discontinuation syndromes such as anxiety and excitement could be expected.
Determining whether some relapses are due to withdrawal-related symptom exacerbation rather than illness recurrence has major implications for the maintenance treatment of patients with antipsychotics. However, research involving antipsychotic discontinuation is challenging, and ethical considerations preclude conducting well-designed prospective studies with sufficiently large samples. We investigated the topic by using existing data from a randomized, placebo-controlled, relapse-prevention study comparing paliperidone palmitate once-monthly (PP1M) injection with placebo.21,22 This dataset was particularly suitable for the following reasons: the sample was large, operationally defined relapse criteria were used, regular assessments were conducted both prior to and subsequent to relapse, and the use of an LAI antipsychotic formulation provided assured medication delivery and removed the possible confounding factor that relapses in the maintenance treatment group were due to nonadherence. We were able to compare the symptom profiles of relapses occurring after antipsychotic discontinuation (ie, those occurring in patients randomized to placebo) with relapses occurring in patients receiving assured maintenance antipsychotic treatment. We were also able to compare antecedents to relapse and the postrelapse treatment response between patients who relapsed on placebo with those who relapsed on maintenance treatment.
In this post hoc analysis, we investigated whether withdrawal-related phenomena, including SSP, could contribute to the high rates of symptom recurrence after antipsychotic treatment discontinuation. We aimed to compare the nature of relapse events after antipsychotic discontinuation with those in patients receiving ongoing antipsychotic. We hypothesized that if a withdrawal psychosis exists, it would be phenomenologically distinct. Symptoms would be more severe and anxiety/depression and excitement/hostility levels would be higher, whereas illness recurrence would be characterized by prominent core symptoms of schizophrenia, ie, positive, negative, and disorganized symptoms. Also, withdrawal psychosis would differ from illness recurrence insofar as it would be characterized by a more abrupt onset of symptoms and rapid resolution once antipsychotic treatment was reinstated.4 Finally, withdrawal psychosis would also have physiological features associated with discontinuation syndromes, ie, elevated blood pressure, increased heart rate, and other proposed features of SSP such as antipsychotic tolerance, tardive dyskinesia, and elevated prolactin.
METHODS
We performed an analysis of a multicenter, multinational, randomized, placebo-controlled study conducted at 56 centers in 9 countries from March 2005 to February 2007. Detailed findings of the original study21,22 have been published elsewhere (ClinicalTrials.gov identifier: NCT00111189).
Patients
Patients were considered for inclusion if they were aged 18–65 years; met Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV), diagnosis of schizophrenia of ≥ 1 year duration; and had a Positive and Negative Syndrome Scale (PANSS)23 score < 120. Exclusion criteria were other major DSM-IV Axis I diagnosis, significant suicidality or aggression, substance dependence in the previous 3 months, significant general medical condition, treatment refractoriness (ie, failure to respond to 2 prior adequate antipsychotic medications of ≥ 4 weeks), and use of an LAI antipsychotic within the previous 4 weeks.
Ethics approval was obtained from independent ethics committees or institutional review boards at each study site. The study was conducted according to the ethical principles as outlined in the Declaration of Helsinki and was consistent with Good Clinical Practices. All patients provided informed, written consent.
Study Design
The study comprised the following 5 phases: (1) a screening and oral tolerability phase of up to 7 days; (2) an open-label (OL) transition phase of 9 weeks during which patients were switched from their previous antipsychotic to flexible doses of PP1M (25, 50, or 100 mEq once monthly) after an initial regimen of PP1M 50 mEq on days 1 and 8; (3) an OL maintenance phase of 24 weeks during which patients with PANSS total score ≤ 75 at week 9 of the transition phase received flexible doses of PP1M (25, 50, or 100 mEq once monthly) for 12 weeks, followed by 12 weeks on the maintenance dose; (4) a double-blind phase in which stable patients (defined as maintaining PANSS total score ≤ 75 and ≤ 4 on PANSS items P1 [delusions], P2 [conceptual disorganization], P3 [hallucinatory behavior], P6 [suspiciousness/persecution], P7 [hostility], G8 [uncooperativeness], and G14 [poor impulse control] for 12 weeks) were randomized 1:1 to receive either PP1M at the previously stabilized dose or placebo, and (5) an optional 52-week OL extension phase. Patients remained in the double-blind phase until relapse, study withdrawal, or study completion. After the confirmation of a relapse, patients were offered entry into the OL treatment extension phase with PP1M. A preplanned interim analysis was conducted after 68 relapse events. Relapse was operationally defined as: (1) hospitalization for symptoms of schizophrenia; (2) ≥ 25% increase in PANSS total score for 2 consecutive assessments if PANSS total was > 40 at randomization or ≥ 10-point PANSS total score increase for those with ≤ 40 at randomization; (3) deliberate self-harm or significant aggression; suicidality or homicidality; (4) increase in PANSS items P1, P2, P3, P6, P7, and G8 to ≥ 5 for those whose score was ≤ 3 at randomization, or to ≥ 6 for those whose score was 4 at randomization.
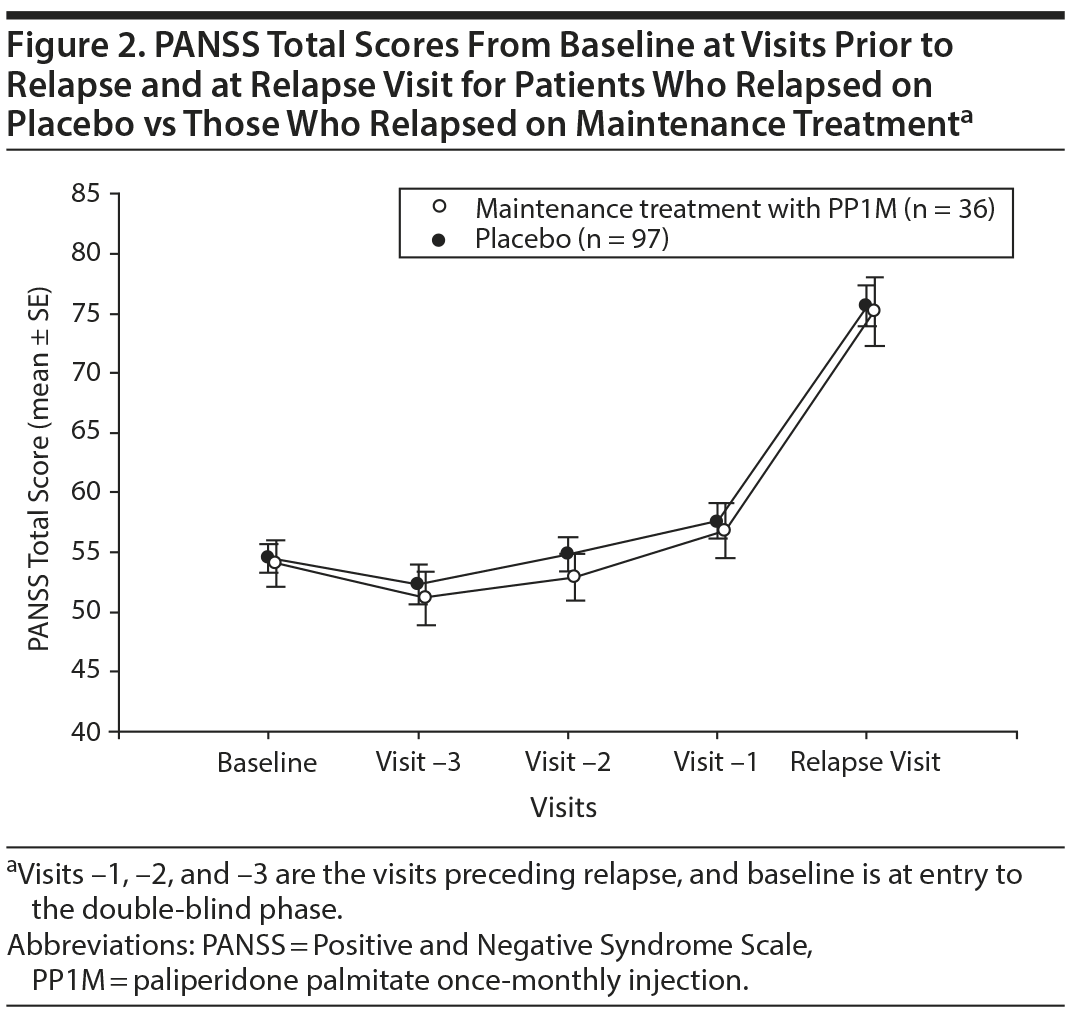
Psychopathology by PANSS total scores and 5 factor-analysis–derived24 domain scores (positive, negative, disorganized, anxiety/depression, and excitement/hostility) were assessed. To assess the course of symptom recurrence prior to relapse, PANSS total and domain24 scores for the visits preceding relapse were calculated. With the relapse visit as the starting point, the data for the 3 visits before relapse were grouped as visit –1 (ie, 1 visit prior to relapse), visit –2 (ie, 2 visits prior), and visit –3 (ie, 3 visits prior). The baseline visit refers to the first visit in the double-blind maintenance phase.
Statistical Analyses
A post hoc analysis was performed to compare the 2 groups of patients who relapsed during the double-blind phase (those on placebo at time of relapse and those who relapsed while receiving maintenance therapy with PP1M). Differences between the 2 groups at baseline and at the relapse visit were assessed using χ2 tests for categorical variables and 2-sample t test for continuous variables. To assess whether there were differences after relapse, we compared postrelapse treatment response between the 2 groups. We also assessed the differences in postrelapse endpoint antipsychotic dose between the 2 groups. Incidence of tardive dyskinesia between the 2 groups was assessed using the Schooler-Kane criteria.25 Finally, given that one of the criteria for the proposed supersensitivity psychosis is that psychotic symptoms reappear shortly after treatment discontinuation (within 3 months in the case of LAI antipsychotics), we conducted an additional analysis by dividing the patients who relapsed on placebo (n = 97) into those occurring before 3 months (n = 62) and those occurring after 3 months (n = 35) of placebo treatment. These groups were compared in terms of symptom domain profile at relapse, blood pressure, heart rate, dyskinesia score, antipsychotic dose (to investigate whether tolerance had occurred), and prolactin levels.
RESULTS
Of the 849 patients enrolled, 410 (placebo = 204 and PP1M = 206) were randomized to the double-blind phase and 352 completed the double-blind phase of this study. Full study flow and patient disposition are described elsewhere.21,22 Demographics and baseline characteristics such as age, sex, duration of illness, and baseline PANSS scores were similar between the 2 groups.21,22 A total of 97 of 204 patients (47.5%) randomized to placebo and 36 of 206 (17.5%) randomized to ongoing maintenance treatment with PP1M relapsed in the double-blind phase before termination of the study (hazard ratio [placebo/PP1M] = 3.60 [95% CI, 2.45–5.28]. Patients randomized to continue on PP1M experienced a significant delay in time-to-relapse compared with placebo-assigned patients. The median time-to-relapse (the estimated time point where 50% of patients have experienced relapse) in the placebo group was 163 days and not estimable for PP1M (P < .0001).22 The mean ± SD age of patients relapsing on placebo was slightly higher than those of patients who relapsed on PP1M maintenance treatment (40.5 ± 10.71 years vs 36.3 ± 11.37 years). The proportion of women and men in the placebo group was similar (49.5% vs 50.5%), while in the PP1M maintenance treatment group, there was a higher proportion of men (63.9%) compared with women (36.1%) (Table 1).
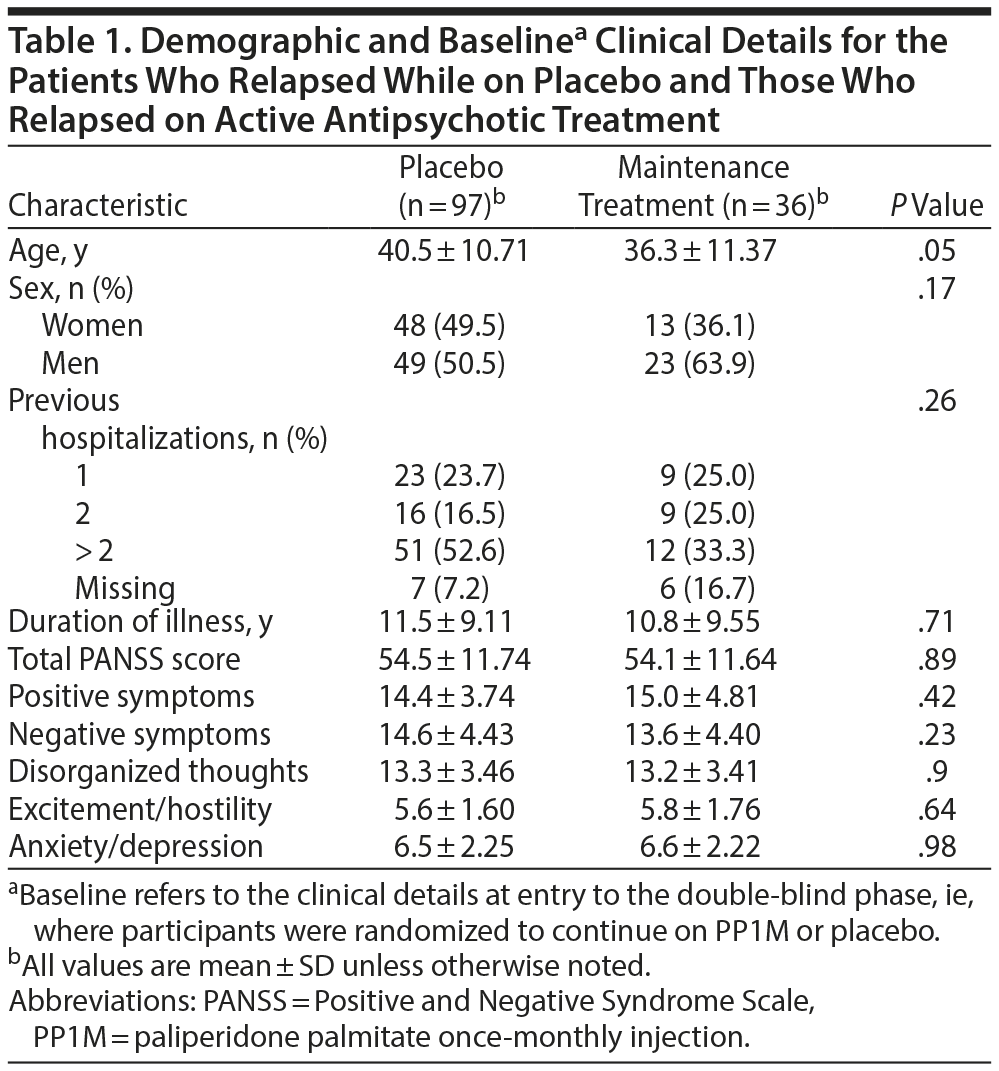
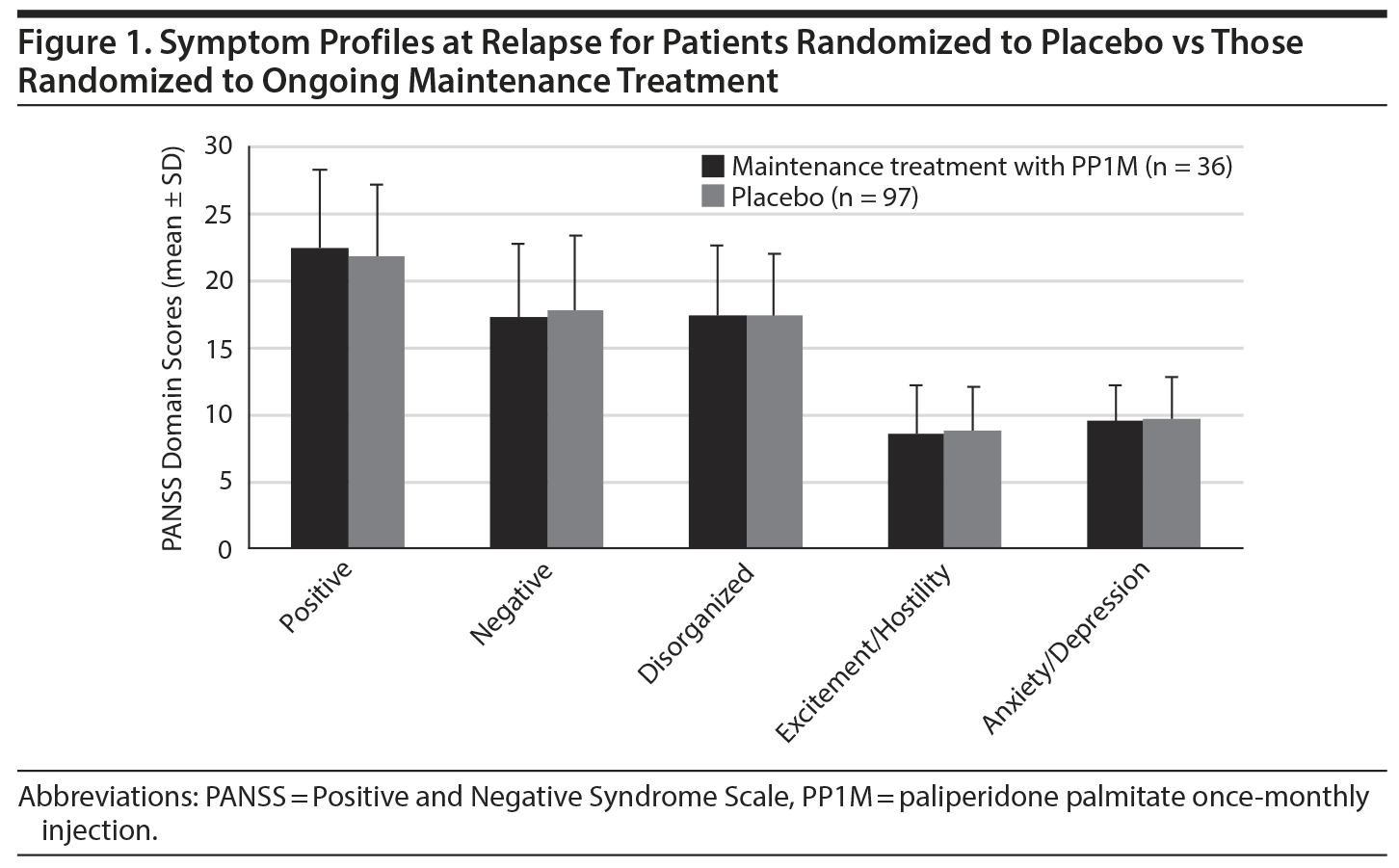
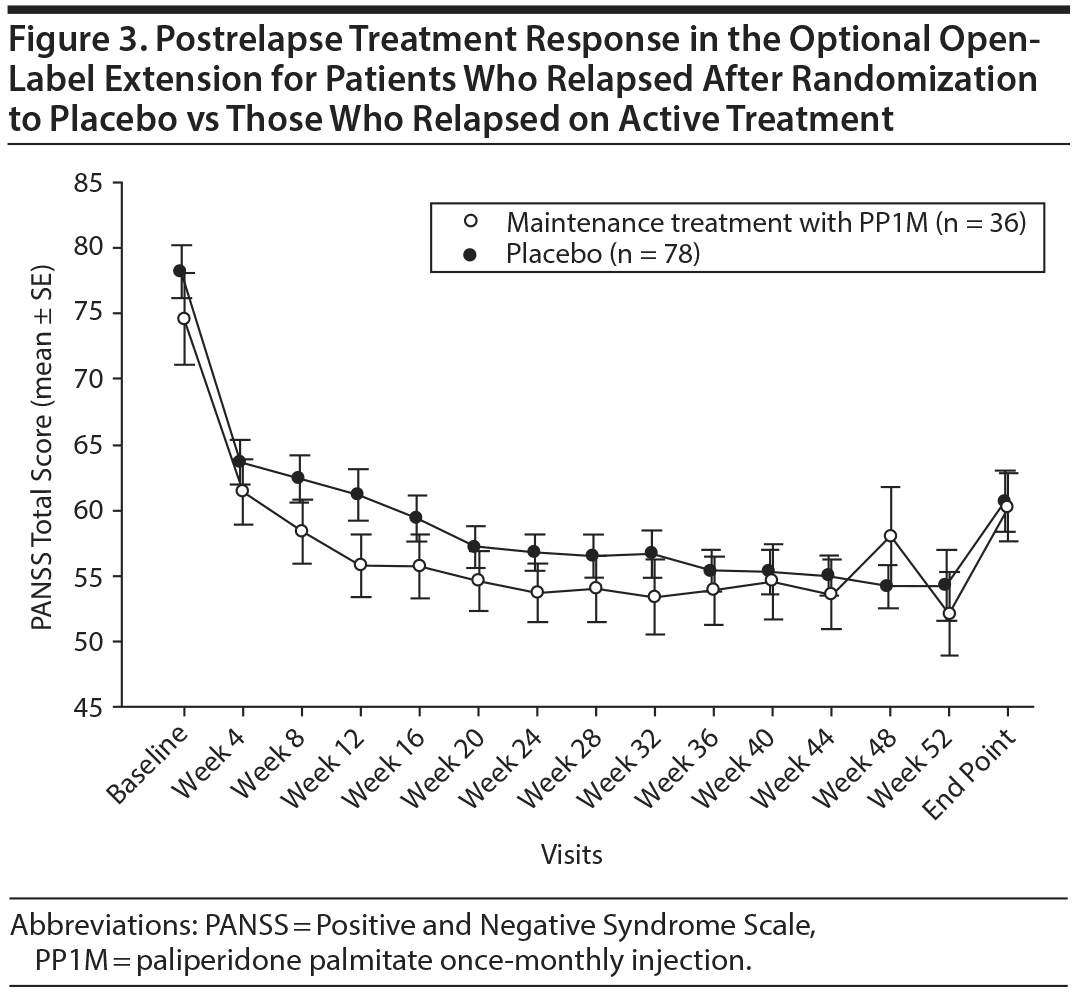
Mean scores for each of the PANSS domains at time of relapse were similar in both placebo and PP1M maintenance groups (Figure 1). The PANSS total and domain scores at relapse were much higher than at baseline and for the 3 visits prior to relapse for both placebo and PP1M maintenance treatment groups; no significant difference was noted between the groups (Table 2). Both groups showed a similar pattern of symptom recurrence. There were no significant differences (P > .18) in PANSS scores between baseline and the visit immediately prior to the relapse episode (Figure 2) for all variables in Table 2. However, when we compared the visit preceding relapse with data from the relapse visit, there was statistically significant evidence of abrupt deterioration (P < .001) for all variables presented in Table 2. The PANSS total scores improved similarly in both groups in the postrelapse treatment phase (Figure 3). From these results, it is apparent that the placebo and PP1M maintenance treatment groups were similar in terms of the rate of reemergence of symptoms, the symptom profile of the relapse event, and the postrelapse treatment response.
There were no significant differences in blood pressure or heart rate between the groups at baseline and at relapse. The mean ± SD systolic blood pressure for patients relapsing on placebo and those relapsing on PP1M maintenance treatment, respectively, was 122 ± 14.7 and 119 ± 10.1 mm Hg (P = .17) at baseline and 122 ± 13.0 and 123 ± 15.6 mm Hg (P = .85) at the relapse visit; diastolic blood pressure values were 76.7 ± 10.0 and 77.6 ± 7.7 mm Hg (P = .65) at baseline and 79.1 ± 12.9 and 77.8 ± 10.3 mm Hg (P = .57) at the relapse visit. Heart rates for patients relapsing on placebo and those relapsing on PP1M maintenance treatment, respectively, were 79.9 ± 10.29 and 76.1 ± 10.31/min (P = .06) at baseline and 80.5 ± 11.75 and 80.4 ± 11.98/min (P = .97) at the relapse visit. Similarly, there were no significant differences in dyskinesia scores between the placebo and PP1M maintenance groups. Total Abnormal Involuntary Movement Scale26 scores for patients relapsing on placebo and PP1M maintenance treatment respectively were 0.5 ± 1.98 and 0.1 ± 0.42 (P = .30) at baseline and 0.6 ± 1.67 and 0.4 ± 1.57 (P = .66) at the relapse visit. There was 1 case of probable tardive dyskinesia and no cases of definitive tardive dyskinesia in the group of patients relapsing on placebo, and no cases of probable or definitive dyskinesia in the group of patients relapsing on PP1M maintenance treatment. The endpoint PP1M dose was not significantly different for the 2 groups (81.0 ± 29.73 mEq and 77.9 ± 29.3 mEq for the 2 groups, P = .63). Prolactin levels were similar in the 2 groups at baseline (47.8 ± 38.6 and 46.8 ± 34.8 ng/mL, P = .89) and lower in the placebo group at week 12 of the double-blind phase (38.5 ± 37.4 and 49.9 ± 33.8 ng/mL, P = .28) as well as at the postrelapse treatment phase endpoint (41.7 ± 27.8 and 57.1 ± 54.2 ng/mL, P = .06).
The results of the comparison between the patients who relapsed before 3 months (n = 62) and those who relapsed after 3 months (n = 35) of placebo are provided in Supplementary Table 1. There were no differences between the early relapsers versus the late relapsers in terms of symptom domain profile at relapse, heart rate, diastolic blood pressure, dyskinesia score, antipsychotic dose, and prolactin levels, while systolic blood pressure was higher in the late relapsers (P < .05).
DISCUSSION
To the best of our knowledge, this post hoc analysis is the first study to investigate in a controlled setting whether symptom recurrence after treatment discontinuation in schizophrenia is due to withdrawal-related phenomena or to illness recurrence. Our findings demonstrate that relapses in the placebo group were similar to those that occurred in patients on active treatment, with respect to the following aspects: First, the symptom profiles at relapse were similar for both groups. Relapse after antipsychotic discontinuation was not characterized by higher levels of psychological symptoms associated with discontinuation, ie, anxiety/depression or excitement/hostility. Also, severity levels for core positive, negative, and disorganized symptoms were similar, which is consistent with illness recurrence rather than a withdrawal-related phenomenon. Second, the pattern of recurrence of symptoms was similar in PP1M maintenance and placebo groups—symptom levels remained fairly consistent in the visits preceding relapse, with an abrupt return of symptoms to levels of similar severity between the groups at the relapse visit. This was the case for all of the PANSS symptom domains. While this pattern differs from the onset of a first psychotic episode where prodromal and subsyndromal symptoms frequently predate the onset of frank psychosis by months and even years,27 it is consistent with previous work indicating an abrupt return of symptoms and absence of reliable early warning signs for recurrent episodes.28,29 Third, when examining the postrelapse treatment response between the 2 groups, the patients who relapsed after treatment discontinuation did not show a more rapid resolution of symptoms with reintroduction of treatment, as was proposed by Chouinard as a criterion for SSP.13 (Although, given the open nature of the extension phase, these results need to be interpreted with caution.) Fourth, no evidence of physiological signs was noted that could be related to discontinuation syndromes insofar as blood pressure and heart rates were similar between the groups. Fifth, evidence of antipsychotic tolerance or tardive dyskinesia was not observed in the patients who relapsed after treatment discontinuation. Sixth, the finding that prolactin levels were similar at baseline and nonsignificantly lower after 12 weeks of placebo treatment and at the postrelapse treatment phase endpoint in the patients who relapsed after treatment discontinuation is contrary to the proposed elevated prolactin levels characterizing SSP.13 Finally, the patients who relapsed within 3 months of placebo treatment did not display any of the proposed features of SSP or physiological discontinuation symptoms when compared with the patients who relapsed after 3 months of placebo treatment. Thus, our analysis does not support the existence of a withdrawal-related psychosis or evidence that physiological or psychological discontinuation symptoms could contribute to the high rates of relapse after treatment discontinuation. Rather, our analysis indicates that the relapse episodes occurring after treatment discontinuation represent illness recurrence.
The high relapse rates and abrupt reemergence of psychotic symptoms after treatment discontinuation suggest a reduced threshold for psychotic decompensation once a first psychotic episode has occurred.30 Our findings are also consistent with current thinking regarding the dopamine hypothesis, where a direct relationship between dopamine dysregulation and psychosis is proposed. According to Howes et al,31,32 elevated striatal presynaptic dopamine synthesis is linked to the acute psychotic symptoms characterizing relapse, and psychosis represents a state of aberrant salience due to this dopamine dysregulation.33 Supporting evidence for a direct relationship between dopamine and psychosis is provided by the observation that the onset of antipsychotic action is rapid, contrary to a previous hypothesis.33 Antipsychotics dampen the symptoms of psychosis rather than eradicating them. Therefore, when treatment is discontinued, there is a resurgence of dopamine with symptoms being reinvested with aberrant salience.35 Just as symptoms resolve rapidly with antipsychotic treatment, it should not be surprising that symptoms frequently reemerge shortly after treatment discontinuation.
There are several limitations in this study. First, because patients were treated with an LAI antipsychotic, withdrawal from antipsychotic treatment was gradual, potentially protecting patients from developing withdrawal or discontinuation symptoms. Indeed, “dopamine rebound/withdrawal syndromes” are said to occur when antipsychotics are abruptly discontinued.36 On the other hand, relapse rates after discontinuation of LAI antipsychotics are very high37,38 and in this study were similar to those reported in other discontinuation studies using oral antipsychotics.39 Nevertheless, studies investigating the nature of relapse after oral antipsychotic discontinuation are indicated. Second, it could be argued that some of the relapses that occurred in patients while on active treatment were also due to SSP, as it has been speculated that SSP may occur as a “breakthrough” phenomenon in the course of active treatment.16 However, this is unlikely as the additional features of this proposed condition such as tardive dyskinesia, elevated prolactin, and antipsychotic tolerance were not observed in patients who relapsed while on active treatment. Our findings may not necessarily be generalizable to patients treated with other antipsychotics, as rebound or withdrawal phenomena have been linked to specific receptor-binding profiles including muscarinic and histaminergic receptors.36
In conclusion, our findings suggest that relapse episodes after treatment discontinuation denote recurrence of underlying illness and may be consistent with a direct relationship between dopamine and psychosis. No evidence was found from this study to suggest that the high rates of relapse after antipsychotic discontinuation can be attributed beyond mere symptom recurrence to the process of drug withdrawal itself or to the existence of SSP. Further studies including patients discontinued from oral antipsychotics and from antipsychotics with different receptor binding profiles are indicated.
Submitted: August 18, 2017; accepted December 20, 2017.
Published online: June 19, 2018.
Author contributions: All authors met International Committee of Medical Journal Editors criteria, and all those who fulfilled those criteria are listed as authors. All authors had access to the study data, provided direction and comments on the manuscript, made the final decision about where to publish these data, and approved the final draft submission to the journal.
Potential conflicts of interest: Drs Nuamah, Gopal, and Hough are employees of Janssen Research & Development, LLC. Dr Emsley has been a speaker and has participated in advisory boards for, and received honoraria from, Janssen, Lundbeck, Servier, and Otsuka, and has received research funding from Janssen and Lundbeck. Dr Fleischhacker has received research grants from Boehringer Ingelheim, Janssen-Cilag, Otsuka, and Lundbeck and has received speaking fees and advisory board honoraria from AOP Orphan, Boehringer Ingelheim, Janssen, Richter, Roche, Lundbeck, Otsuka, Takeda, Amgen, Allergan, Teva, and Sumitomo Dainippon.
Funding/support: This study was funded by Janssen Research & Development, LLC, USA.
Role of sponsor: The clinical team from Janssen Research & Development, LLC, reviewed the manuscript; however, the final approval for the decision to submit the manuscript was the sole decision of the authors.
Previous presentation: This post hoc analysis was submitted as an abstract for a poster presentation at the 6th Schizophrenia International Research Society (SIRS) conference; April 4–8, 2018; Florence, Italy.
Acknowledgments: The authors thank Ramji Narayanan, MPharm, ISMPP CMPP, and Wendy P. Battisti, PhD, for writing assistance and Ellen Baum, PhD, for additional editorial assistance. Dr Battisti was and Dr Baum is a full-time employee of Janssen Research & Development, LLC, USA. Mr Narayanan is a full-time employee of SIRO Clinpharm Pvt. Ltd, Thane, India.
Supplementary material: Available at PSYCHIATRIST.COM.
REFERENCES
1. Leucht S, Tardy M, Komossa K, et al. Maintenance treatment with antipsychotic drugs for schizophrenia. Cochrane Database Syst Rev. 2012;(5):CD008016. PubMed CrossRef
2. Zipursky RB, Menezes NM, Streiner DL. Risk of symptom recurrence with medication discontinuation in first-episode psychosis: a systematic review. Schizophr Res. 2014;152(2–3):408–414. PubMed CrossRef
3. Citrome L. Oral antipsychotic update: a brief review of new and investigational agents for the treatment of schizophrenia. CNS Spectr. 2012;17(suppl 1):1–9. PubMed CrossRef
4. Moncrieff J. Antipsychotic maintenance treatment: time to rethink? PLoS Med. 2015;12(8):e1001861. PubMed CrossRef
5. Harrow M, Jobe TH, Faull RN. Do all schizophrenia patients need antipsychotic treatment continuously throughout their lifetime? a 20-year longitudinal study. Psychol Med. 2012;42(10):2145–2155. PubMed CrossRef
6. Wunderink L, Nieboer RM, Wiersma D, et al. Recovery in remitted first-episode psychosis at 7 years of follow-up of an early dose reduction/discontinuation or maintenance treatment strategy: long-term follow-up of a 2-year randomized clinical trial. JAMA Psychiatry. 2013;70(9):913–920. PubMed CrossRef
7. Morgan C, Lappin J, Heslin M, et al. Reappraising the long-term course and outcome of psychotic disorders: the AESOP-10 study. Psychol Med. 2014;44(13):2713–2726. PubMed CrossRef
8. Murray RM, Quattrone D, Natesan S, et al. Should psychiatrists be more cautious about the long-term prophylactic use of antipsychotics? Br J Psychiatry. 2016;209(5):361–365. PubMed CrossRef
9. Goff DC, Falkai P, Fleischhacker WW, et al. The long-term effects of antipsychotic medication on clinical course in schizophrenia. Am J Psychiatry. 2017;174(9):840–849. PubMed CrossRef
10. Moncrieff J. Why is it so difficult to stop psychiatric drug treatment? it may be nothing to do with the original problem. Med Hypotheses. 2006;67(3):517–523. PubMed CrossRef
11. Moncrieff J. Does antipsychotic withdrawal provoke psychosis? review of the literature on rapid onset psychosis (supersensitivity psychosis) and withdrawal-related relapse. Acta Psychiatr Scand. 2006;114(1):3–13. PubMed CrossRef
12. Baldessarini RJ, Viguera AC. Neuroleptic withdrawal in schizophrenic patients. Arch Gen Psychiatry. 1995;52(3):189–192. PubMed CrossRef
13. Chouinard G, Jones BD, Annable L. Neuroleptic-induced supersensitivity psychosis. Am J Psychiatry. 1978;135(11):1409–1410. PubMed CrossRef
14. Davis KL, Rosenberg GS. Is there a limbic system equivalent of tardive dyskinesia? Biol Psychiatry. 1979;14(4):699–703. PubMed
15. Kirkpatrick B, Alphs L, Buchanan RW. The concept of supersensitivity psychosis. J Nerv Ment Dis. 1992;180(4):265–270. PubMed CrossRef
16. Chouinard G. Severe cases of neuroleptic-induced supersensitivity psychosis: diagnostic criteria for the disorder and its treatment. Schizophr Res. 1991;5(1):21–33. PubMed CrossRef
17. Fallon P, Dursun S, Deakin B. Drug-induced supersensitivity psychosis revisited: characteristics of relapse in treatment-compliant patients. Ther Adv Psychopharmacol. 2012;2(1):13–22. PubMed CrossRef
18. Fallon P, Dursun SM. A naturalistic controlled study of relapsing schizophrenic patients with tardive dyskinesia and supersensitivity psychosis. J Psychopharmacol. 2011;25(6):755–762. PubMed CrossRef
19. Kimura H, Kanahara N, Komatsu N, et al. A prospective comparative study of risperidone long-acting injectable for treatment-resistant schizophrenia with dopamine supersensitivity psychosis. Schizophr Res. 2014;155(1–3):52–58. PubMed CrossRef
20. Suzuki T, Kanahara N, Yamanaka H, et al. Dopamine supersensitivity psychosis as a pivotal factor in treatment-resistant schizophrenia. Psychiatry Res. 2015;227(2–3):278–282. PubMed CrossRef
21. Gopal S, Vijapurkar U, Lim P, et al. A 52-week open-label study of the safety and tolerability of paliperidone palmitate in patients with schizophrenia. J Psychopharmacol. 2011;25(5):685–697. PubMed CrossRef
22. Hough D, Gopal S, Vijapurkar U, et al. Paliperidone palmitate maintenance treatment in delaying the time-to-relapse in patients with schizophrenia: a randomized, double-blind, placebo-controlled study. Schizophr Res. 2010;116(2–3):107–117. PubMed CrossRef
23. Kay SR, Fiszbein A, Opler LA. The Positive and Negative Syndrome Scale (PANSS) for schizophrenia. Schizophr Bull. 1987;13(2):261–276. PubMed CrossRef
24. Marder SR, Davis JM, Chouinard G. The effects of risperidone on the five dimensions of schizophrenia derived by factor analysis: combined results of the North American trials. J Clin Psychiatry. 1997;58(12):538–546. PubMed CrossRef
25. Schooler NR, Kane JM. Research diagnoses for tardive dyskinesia. Arch Gen Psychiatry. 1982;39(4):486–487. PubMed CrossRef
26. Guy W. ECDEU Assessment Manual for Psychopharmacology, Revised. Rockville, MD: US Dept of Health, Education, and Welfare (ADM 76-338); 1976:534–537.
27. Yung AR, McGorry PD. The prodromal phase of first-episode psychosis: past and current conceptualizations. Schizophr Bull. 1996;22(2):353–370. PubMed CrossRef
28. Emsley R, Nuamah I, Hough D, et al. Treatment response after relapse in a placebo-controlled maintenance trial in schizophrenia. Schizophr Res. 2012;138(1):29–34. PubMed CrossRef
29. Emsley R, Oosthuizen P, Koen L, et al. Comparison of treatment response in second-episode versus first-episode schizophrenia. J Clin Psychopharmacol. 2013;33(1):80–83. PubMed CrossRef
30. Birchwood M, Smith J, Macmillan F, et al. Predicting relapse in schizophrenia: the development and implementation of an early signs monitoring system using patients and families as observers, a preliminary investigation. Psychol Med. 1989;19(3):649–656. PubMed CrossRef
31. Howes OD, Kambeitz J, Kim E, et al. The nature of dopamine dysfunction in schizophrenia and what this means for treatment. Arch Gen Psychiatry. 2012;69(8):776–786. PubMed CrossRef
32. Howes OD, Kapur S. The dopamine hypothesis of schizophrenia: version III—the final common pathway. Schizophr Bull. 2009;35(3):549–562. PubMed CrossRef
33. Kapur S. Psychosis as a state of aberrant salience: a framework linking biology, phenomenology, and pharmacology in schizophrenia. Am J Psychiatry. 2003;160(1):13–23. PubMed CrossRef
34. Agid O, Siu CO, Potkin SG, et al. Meta-regression analysis of placebo response in antipsychotic trials, 1970–2010. Am J Psychiatry. 2013;170(11):1335–1344. PubMed CrossRef
35. Kapur S, Agid O, Mizrahi R, et al. How antipsychotics work-from receptors to reality. NeuroRx. 2006;3(1):10–21. PubMed CrossRef
36. Correll CU. Antipsychotic use in children and adolescents: minimizing adverse effects to maximize outcomes. J Am Acad Child Adolesc Psychiatry. 2008;47(1):9–20. PubMed CrossRef
37. Emsley R, Oosthuizen PP, Koen L, et al. Symptom recurrence following intermittent treatment in first-episode schizophrenia successfully treated for 2 years: a 3-year open-label clinical study. J Clin Psychiatry. 2012;73(4):e541–e547. PubMed CrossRef
38. Gitlin M, Nuechterlein K, Subotnik KL, et al. Clinical outcome following neuroleptic discontinuation in patients with remitted recent-onset schizophrenia. Am J Psychiatry. 2001;158(11):1835–1842. PubMed CrossRef
39. Gilbert PL, Harris MJ, McAdams LA, et al. Neuroleptic withdrawal in schizophrenic patients. A review of the literature. Arch Gen Psychiatry. 1995;52(3):173–188. PubMed CrossRef
This PDF is free for all visitors!





