Suicide After Release From Prison:
A Population-Based Cohort Study From Sweden
ABSTRACT
Objective: Released prisoners have high suicide rates compared with the general population, but little is known about risk factors and possible causal pathways. We conducted a population-based cohort study to investigate rates and risk factors for suicide in people previously imprisoned.
Method: We identified individuals released from prison in Sweden between January 1, 2005, and December 31, 2009, through linkage of national population-based registers. Released prisoners were followed from the day of release until death, emigration, new incarceration, or December 31, 2009. Survival analyses were conducted to compare incidence rates and psychiatric morbidity with nonconvicted population controls matched on gender and year of birth.
Results: We identified 38,995 releases among 26,985 prisoners (7.6% female) during 2005–2009. Overall, 127 suicides occurred, accounting for 14% of all deaths after release (n = 920). The mean suicide rate was 204 per 100,000 person-years, yielding an incidence rate ratio of 18.2 (95% CI, 13.9–23.8) compared with general population controls. Previous substance use disorder (hazard ratio [HR] = 2.1; 95% CI, 1.4–3.2), suicide attempt (HR = 2.5; 95% CI, 1.7–3.7), and being born in Sweden versus abroad (HR = 2.1; 95% CI, 1.2–3.6) were independent risk factors for suicide after release.
Conclusions: Released prisoners are at high suicide risk and have a slightly different pattern of psychiatric risk factors for suicide compared with the general population. Results suggest appropriate allocation of resources to facilitate transition to life outside prison and increased attention to prisoners with both a previous suicide attempt and substance use disorder.
J Clin Psychiatry 2014;75(10):1047–1053
© Copyright 2014 Physicians Postgraduate Press, Inc.
Submitted: December 23, 2013; accepted April 7, 2014
(doi:10.4088/JCP.13m08967).
Corresponding author: Axel Haglund, MD, Centre for Psychiatry Research and Education, Stockholm County Council & Karolinska Institutet, St Görans Hospital, Vårdvägen 1, 112 81 Stockholm, Sweden ([email protected]).
Although 10 million people are currently held in prison worldwide,1 considerably larger numbers of ex-prisoners are living in society.2 Since most prison sentences are short, the annual prevalence of people imprisoned is 2–3 times the total number of prisoners at any 1 time point. Rates of suicide within prison are high,3 as are mortality rates from all causes after release.4 Psychiatric disorders, especially affective, psychotic, and personality disorders, are well-known risk factors for suicide in the general population.5–7 Further, psychosis and depression are consistently overrepresented among prisoners,8 and substance use disorders are highly prevalent upon arrival to prison.9 A systematic review10 of suicide in prison suggested that current psychiatric disorder or alcohol problems were associated with completed suicide; this link was also shown in ex-prisoners.11,12 However, previous research on psychiatric risk factors has been limited by incomplete information on psychiatric morbidity, follow-up time no longer than 1 year, and an absence of investigated personality disorders.
A recent systematic review13 of suicide after release from prison found that all existing studies reported standardized mortality ratios above 1, varying between 3 and 6 in England and Wales,14 the United States,15 Australia,11 and the Netherlands.16 Two of these studies demonstrated particularly high suicide rates during the first weeks after release, suggesting that this is a high-risk period.11,17 Hence, suicide in recently released prisoners has become a part of national suicide prevention strategies in many countries. For example, England’s 2012 National Suicide Prevention strategy targets high-risk groups and specifically mentions recently released prisoners.3
More than 10,000 persons (7% women) started serving their prison sentences in Sweden each year during 2005–2009.18 The prison population rate in Sweden is 78 per 100,000 of the national population.1 This is lower than both the world average (148) and that in Australia (133), Netherlands (94), England and Wales (153), and the United States (743), where previous studies of suicides in released prisoners have been conducted,11,14–16 but similar to other Scandinavian countries. Previous studies show that a lifetime history of self-harm is prevalent among Swedish prisoners (reported by 17.9%)19 and that the suicide rates inside Swedish prisons are similar to other Scandinavian countries.3 Further, suicide rates have been shown to be elevated among Swedish ex-prisoners with substance use problems.20 However, no previous studies have investigated suicide rates and risk factors after release from prison on a population-based level in Sweden or in any other country with similar incarceration rates.
On the basis of current uncertainties in the literature, we addressed 3 main questions: (1) Are the first 28 days after release from prison the period of highest risk for suicide? (2) What psychiatric risk factors are linked to suicide after release from prison? and (3) Is there a difference in risk factors for suicide between released prisoners and general population individuals?
METHOD
Study Design
By linking longitudinal national registers, we conducted a cohort study including all releases from prison in Sweden between January 1, 2005, and December 31, 2009. People released from remand prisons (which house prisoners awaiting trial) without a subsequent conviction to imprisonment were excluded. The cohort was followed from the day of release until death, emigration, new incarceration, or end of the study period (December 31, 2009). The focus in this design was on time after release, so that a unique person could reappear in the cohort (be released) several times during the study period.
To compare prevalence of psychiatric morbidity and to calculate incidence rate ratios, we used a control group. Each released prisoner in the cohort was matched on gender and year of birth with 10 general population controls who had never been convicted to imprisonment by the date of the corresponding cohort member’s release (labeled index date). If a control individual was convicted to a prison sentence during the study period, that person ceased to be a control, and—if released within the study period—reappeared as a member of the studied cohort.
Sources of Data
Using personal identification numbers as key, we linked several nationwide population-based registries in Sweden. The studied outcome was suicide and the information about causes of death was obtained from the Cause of Death Register, held by the National Board of Health and Welfare. To avoid underestimation of suicide rates21 and be consistent with recent suicide research in prisoners and other contexts,22–25 we included both certain suicide and unnatural death with undetermined intent (ICD-8 and ICD-9: E950–9, E980–9; ICD-10: X60–84, Y10–34) in our definition of suicide.
The Prison Register (held by the Prison and Probation Services) provided data on exact dates of release from prison between January 1, 2005, and December 31, 2009. To avoid selection bias, we limited the inclusion period to 5 years since Swedish law requires that individual data should be removed from the Prison Register if no new criminal convictions involving prison and probation have occurred within this period.
Through the National Crime Register (since 1973, held by the National Council of Crime Prevention), we obtained information about previous prison sentences. Information about psychiatric (including abuse or dependence) disorders was obtained from the National Patient Register (National Board of Health and Welfare), including all psychiatric hospitalizations since 1973 and outpatient, non–general practitioner physician specialist diagnoses since 2001. The diagnostic categories used were psychotic disorder (ICD-8: 295, 297, 298.2–9, 299; ICD-9: 295, 297, 298.2–9; ICD-10: F20–29), affective disorder (ICD-8: 296.0–3, 296.8–9, 298.0–1, 300.4, 301.1; ICD-9: 296.0–9, 298.0–1, 300.4, 311; ICD-10: F30–33), personality disorder (ICD-8: 301.1–9; ICD-9: 301.0, 301.2–9; ICD-10: F60–61), substance use disorder (ICD-8: 291, 303, 304; ICD-9: 291, 292, 303, 304, 305.0–9; ICD-10: F10–19), any psychiatric disorder (ICD-8: 290–315; ICD-9: 290–319; ICD-10: F00–F99), and any psychiatric disorder excluding substance disorder (as defined above). At least 1 main diagnosis was required for inclusion in psychotic disorder or affective disorder categories, whereas for personality and substance use disorders, a secondary diagnosis sufficed for inclusion. Further, for the category of any psychiatric diagnosis, at least 1 main or secondary diagnosis was required for inclusion. Information about previous suicide attempts was also obtained from the National Patient Register and was defined as a definite or an uncertain suicide attempt (ICD-8 and ICD-9: E950–9 and E980–9; ICD-10: X60–84 and Y10–34), as registered in outpatient or inpatient services.
We used a definition of violent crime previously used in epidemiologic research. It includes homicide, assault, robbery, threats and violence against an officer, gross violation of a person’s integrity, unlawful coercion, unlawful threats, kidnapping, illegal confinement, arson, and intimidation.26 Attempted and aggravated versions of these offenses were included. Sexual crimes were not included in our definition of violent crime.
Statistical Analyses
Absolute suicide rates and incidence rate ratios were calculated by using data from released prisoners and matched controls. Prevalence of psychiatric morbidity among released prisoners was obtained, and prevalence ratios were calculated for comparisons with controls. We used Fisher exact tests and Cox proportional hazards regression modeling to compare psychiatric morbidity among released prisoners who committed suicide and nonprisoner suicide controls. Relative risks were expressed as hazard ratios (HRs) with 95% confidence intervals (CIs). Statistical analyses were undertaken with SPSS 20 (SPSS Inc).
RESULTS
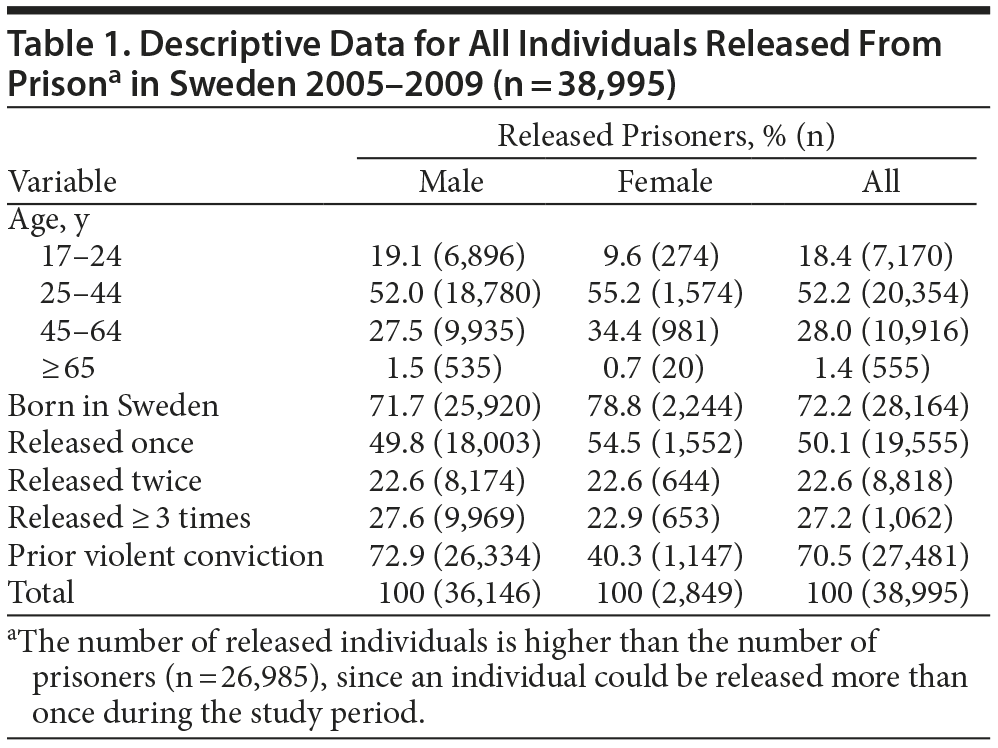
We observed 38,995 releases among 26,985 prisoners (7.6% female) during the study period. At the date of release, the mean ± SD age was 37.8 ± 12.1 years (range, 18–84). In total, 27.8% of the released prisoners were born outside of Sweden (Table 1). The number of releases per prisoner varied from 1 to 9 during the study period, with a mean of 1.5 releases per prisoner (median = 1). The median follow-up time per release was 451 days.
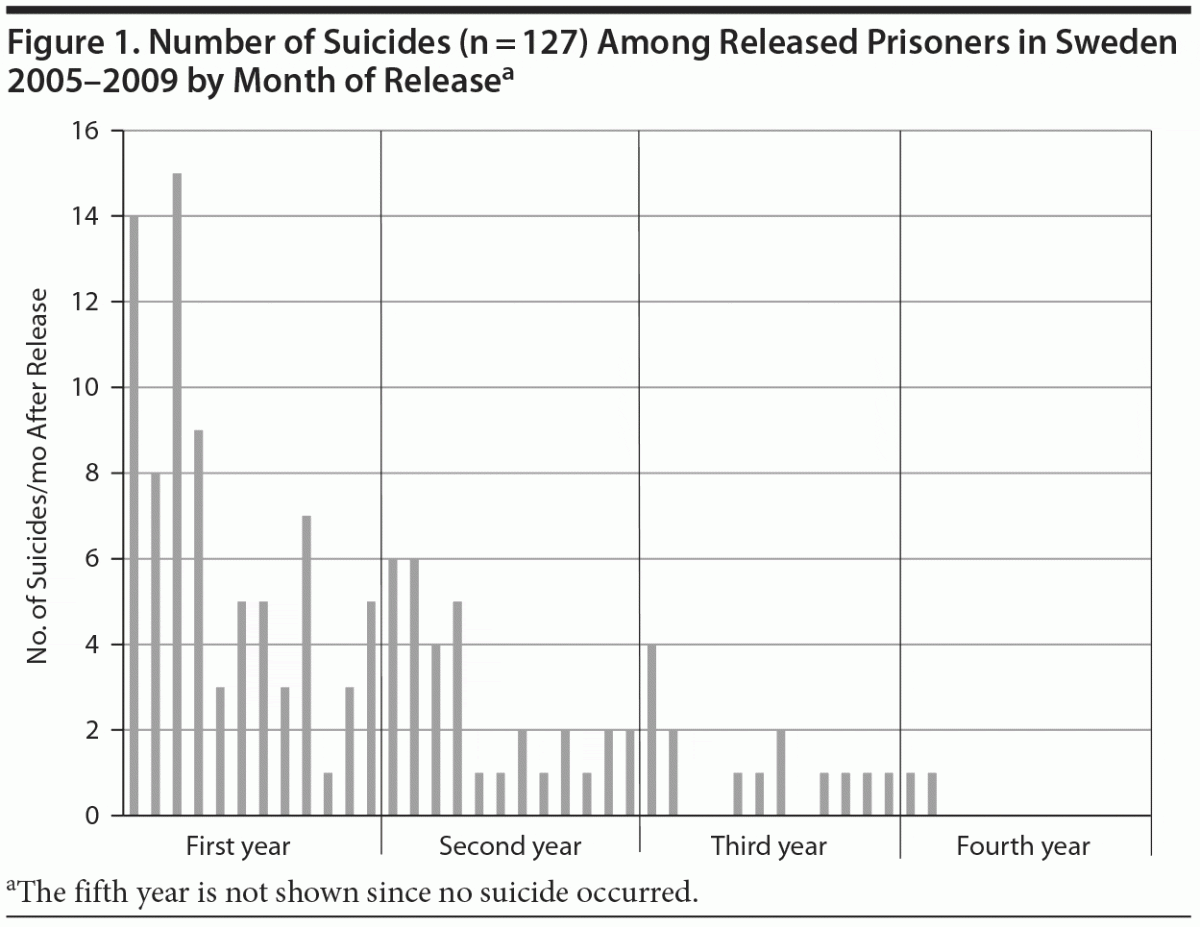
We found 920 deaths, of which 127 (14%) were from suicide. Most suicides were identified during the first year after release (Figure 1). Naturally, the numbers of person-years at risk were also falling for each year of the study period. Nevertheless, with 12 observed suicides, the incidence rate for suicide was highest during the first 28 days (408 per 100,000 person-years; 95% CI, 211–712), and the suicide incidence rate ratio was 58 (95% CI, 13–534) compared to controls. The mean suicide rate during the whole study period was 204 per 100,000 person-years (95% CI, 170–243), yielding an incidence rate ratio of 18.2 (95% CI, 13.9–23.8).
Prevalence of Psychiatric History
in Prisoners and General Population Controls
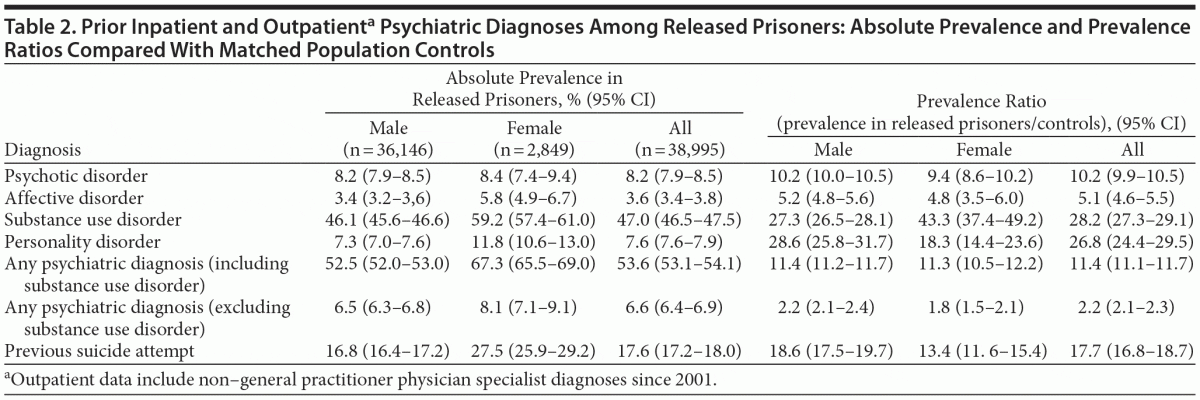
More than half of all released prisoners (53.6%) had been diagnosed with a psychiatric disorder at some point, with substance use disorder as the predominant category (47.0%). Altogether, 17.6% had made a previous suicide attempt that became known to health care. A previous psychiatric diagnosis was more common among released prisoners than controls. The difference was seen across all diagnostic categories, with the highest prevalence ratios in substance use disorder and personality disorder. Except for psychotic disorder, the prevalence was significantly higher for released female prisoners compared with released male prisoners across all diagnostic categories (Table 2).
Risk Factors for Suicide After Release From Prison
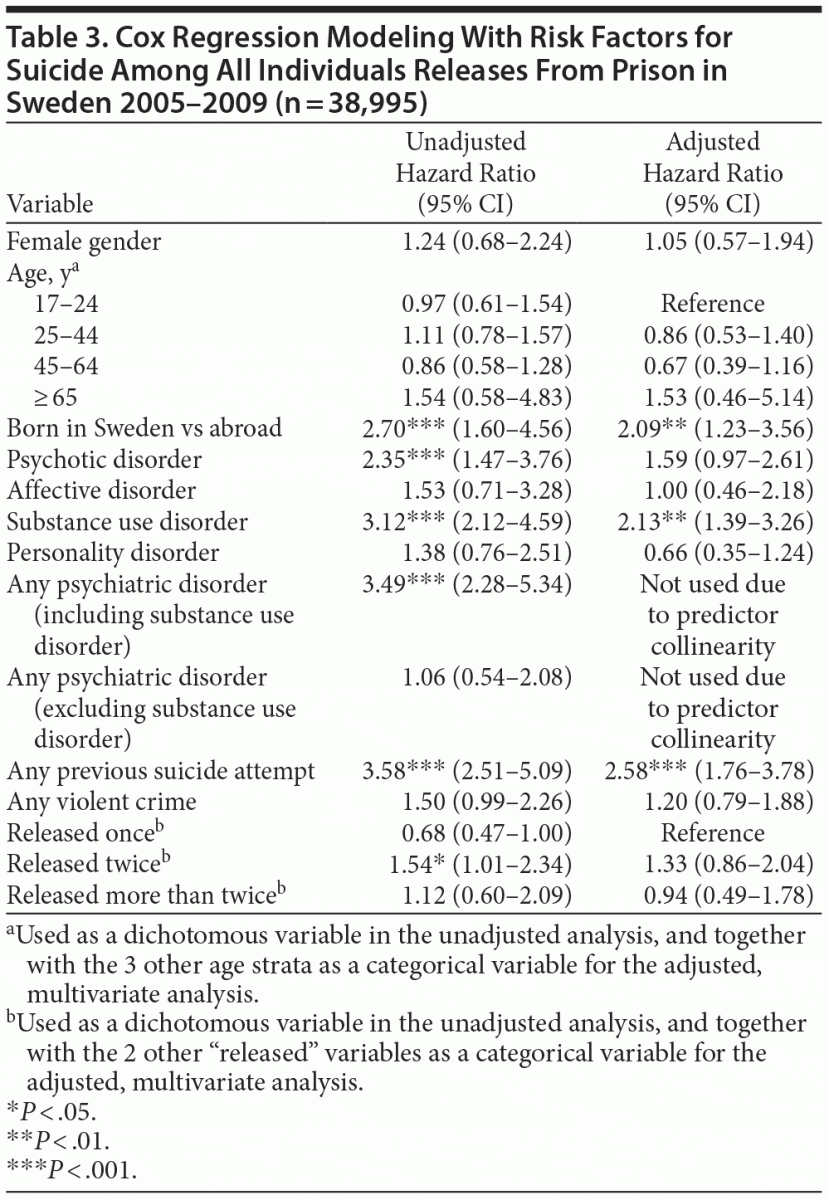
A univariate Cox regression analysis of risk factors for suicide (Table 3) among released prisoners found significantly increased risk in prisoners with any previous psychiatric history (HR = 3.5; 95% CI, 2.3–5.3). However, when substance use disorder was excluded from this category, the increase disappeared (HR = 1.1; 95% CI, 0.5–2.1). Other factors related to increased suicide risk were previous suicide attempt (HR = 3.6; 95% CI, 2.5–5.1), being released twice during the study period (HR = 1.6; 95% CI, 1.0–2.4), and being born in Sweden compared with abroad (HR = 2.7; 95% CI, 1.6–4.6). Specific diagnostic categories associated with increased suicide risk were psychotic disorder (HR = 2.4; 95% CI, 1.5–3.8) and substance use disorder (HR = 3.1; 95% CI, 2.1–4.6). We found no significant increase of risk by gender, age band, or history of violent crime. In the multivariate Cox regression model, including nonoverlapping predictors, the findings remained significant for substance use disorder (HR = 2.1; 95% CI, 1.4–3.2), previous suicide attempt (HR = 2.5; 95% CI, 1.7–3.7), and being born in Sweden (HR = 2.1; 95% CI, 1.2–3.6) (Table 3).
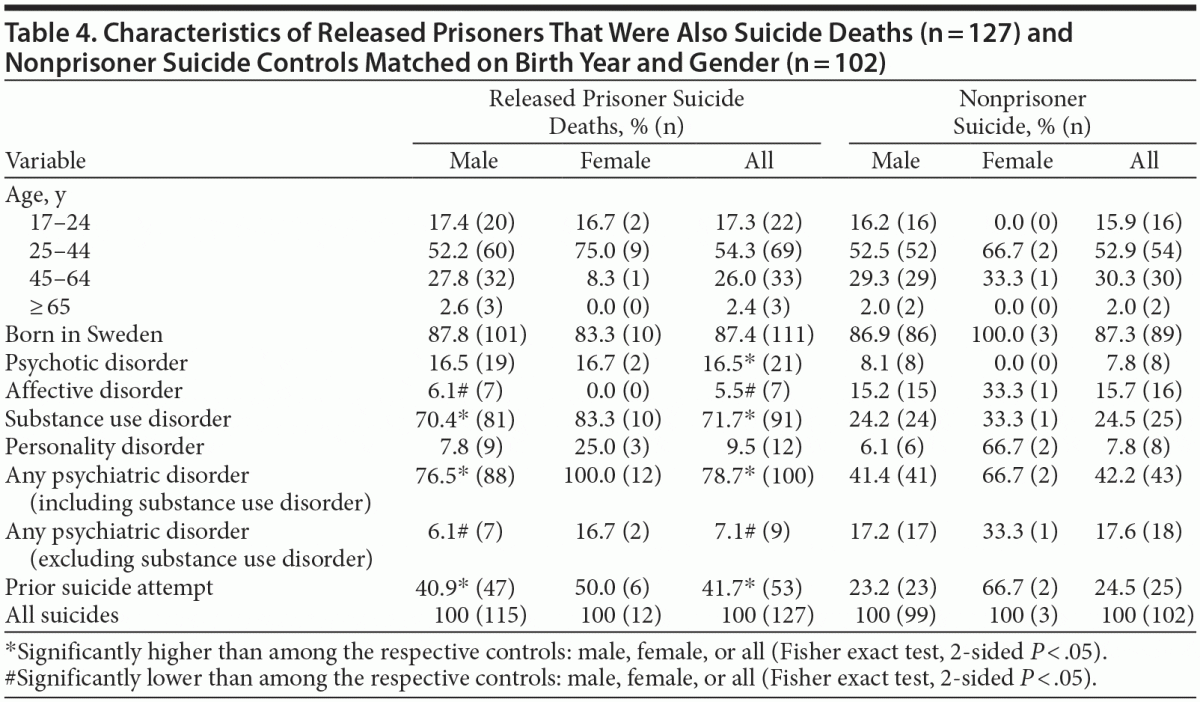
Comparisons of psychiatric morbidity among all suicide victims (Table 4) suggested higher prevalence of substance use disorder and prior suicide attempts among male prisoner suicide completers compared to male nonprisoner suicides. In contrast, a history of affective disorders was less common among released male prisoners who committed suicide than among male suicide victims in the control group of nonprisoners.
DISCUSSION
In this study of almost 40,000 releases of nearly 27,000 prisoners over 5 years, we identified 127 suicides. There were 3 main findings. First, the overall suicide risk among released prisoners was 18 times higher compared to the nonconvicted general population. The risk increase was even more pronounced during the first months after release, suggesting that this is a particularly vulnerable period. Second, the strongest independent risk factors for suicide among released prisoners were substance use disorder, previous suicide attempt, and being born in Sweden. Third, the prevalence of risk factors for completed suicide differed between released prisoners and general population controls.
Suicide Rates After Release From Prison
The high overall suicide rate supported the idea that transition to life outside prison is a period with substantially increased risk for premature death. Previous research has also suggested increased risks for relapse in alcohol and drug misuse, unemployment, and homelessness.27 Programs designed to facilitate the transition from prison to the general community differ among countries; this observation could partly explain differences between studies in suicide rates immediately after release. The different ways in which pathologists label cases of drug overdoses with unknown intent might also explain some differences.28
The generalizability of previous research on suicide rates and risk factors in ex-prisoners has been uncertain because prison systems differ across countries. Previous research has been conducted in nations with large prison populations. However, despite this important difference, suicide rates in this study were similar to (or slightly higher) than those in prior research.3 Interestingly, the study with the most similar suicide rates to the current investigation was from England and Wales,14 where the prison population rate is almost twice that in Sweden.
The particularly high suicide rate ratios in this study should be interpreted with caution because of the large confidence intervals. The use of nonconvicted general population controls enabled us to show the difference in suicide risk between ex-prisoners and individuals who have never been sentenced. Our choice of controls can partly explain the prominent figures in this study. In some earlier work in the field, researchers have tried to adjust for social class and others have used suicide rates in drug-addicted persons,29 with lower suicide rate ratios subsequently reported.
Risk Factors for Suicide After Release From Prison
We identified several risk factors for suicide among prisoners following release. Substance use disorder and psychotic disorder were strong risk factors in unadjusted analyses. However, when combined in a multivariate Cox regression model, psychotic disorder was of borderline significance. This result is probably a type II error, but it could also suggest that psychosis often coexists with substance use disorder in offender populations. The latter interpretation is supported by the fact that the combination of these disorders has a strong association with criminal behavior.30,31 Importantly, a previous suicide attempt, an established risk factor for suicide among psychiatric patients6 and incarcerated prisoners,10 remained a moderately strong independent risk factor in the multivariate model. Previous research in this field has not been able to compare the impact of psychiatric morbidity, including personality disorder, with the same detail as in the present study. Our novel findings underline the relevance of identifying substance use disorder and prior suicidal behavior when assessing suicide risk in released prisoners.
Previous studies12,32,33 have suggested that violent crime predicts subsequent suicide among released prisoners. However, our results agree with another recent population study34 of suicide risk among criminal offenders in Denmark; these authors reported that the suicide risk seen among violent offenders was substantially lowered when psychiatric and social risk factors were accounted for.
We found that being born in Sweden versus abroad was associated with higher suicide risk among the released prisoners. This finding is in line with a recent Swedish cohort study35 in which being born in Sweden was compared with being born in a non-Nordic country. In general, the suicide rates among first-generation immigrants reflect the suicide rates in the countries of birth.36 A national Swedish report37 from 2005 showed that more than 60% of the immigrants who were suspected of crime between 1997 and 2001 were from outside the European Union. However, since we lack more detailed data on specific country, further analysis on this issue is beyond the scope of our present study.
Psychiatric History Among Prisoners
and General Population Controls
As expected, lifetime psychiatric morbidity was common among released prisoners, especially substance use, psychotic, and personality disorders. Substance use disorder strongly correlates with criminal behavior,38,39 and the high prevalence seen in our study is in line with previous work based on screening at incarceration.9 Psychotic disorder is a heterogeneous diagnostic category including schizophrenia but also, for instance, acute and psychotic states that may be induced by substance abuse. Since substance abuse is common among prisoners, prevalence patterns of psychotic disorder could differ between prisoners and the general population. In addition, since people with a severe psychotic disorder (excluding alcohol-induced psychoses) while committing a crime are normally diverted away from prison sentences in Sweden, this group was not included in our study. The prevalence of personality disorder in this cohort of released prisoners is most likely underestimated, since personality disorders are seldom the primary reason for inpatient psychiatric care. Hence, several studies based on structured interviews have shown much higher figures among prisoners.40
Interestingly, a history of substance use disorder was more common among released male prisoners who committed suicide than among matched population, nonprisoner suicides. This finding suggests that substance use disorder may play a more important role in suicides among released prisoners. Further, released prisoners who committed suicide more often had previous suicide attempts compared to general population suicide victims. The relatively low prevalence of affective disorder and personality disorder among released prisoners who committed suicide is somewhat surprising.
Previous studies have shown that risk factors for suicide appear to be different for suicide in custody (eg, marital status)10 and for those with any psychiatric diagnosis (eg, marital status and socioeconomic status)41 when compared with the general population. The findings in our present study support the hypothesis that suicide among released prisoners is less related to affective disorder than is suicide in the general population and that other markers of psychopathology are more prominent. One explanation could be higher prevalence of impulsive and/or aggressive personality traits that predispose to both criminal and suicidal behavior among criminal offenders, as well as the development of substance use disorders.42 It is also possible that the observed difference indicates specific health care–seeking behaviors among prisoners or tendencies in the health care system to underdiagnose affective disorders when they coexist with substance use disorders. Our results also suggest that more research is needed to further investigate specific risk factors for suicide and all-cause mortality in recently released prisoners. This could include the effect of imprisonment, psychosocial factors, and the role of treatment after release.
Strengths and Limitations
To date, this is the largest study on suicide following release from prison. Further, compared to previous studies, our study was able to delineate the psychiatric morbidity that affects suicide risk and how the suicide risk factor pattern differs from that in the general population. Complete coverage of the studied population is another strength. Although our data collection was prospective and preceded the suicide death, register-based studies rely on collection of data from many different clinics and hospitals and the validity of the diagnoses may thus vary. Still, previous studies of the Swedish Patient Register indicate good to excellent validity for schizophrenia and bipolar disorder diagnoses.43,44 The particularly high suicide rate ratios in this study should be interpreted with some caution because of the large confidence intervals. Further, the use of nonconvicted general population controls without adjusting for possible social risk factors could partly explain the prominent elevation of suicide risk.
However, a limitation of our study was that we could only include psychiatric morbidity and suicide attempts that led to an episode of inpatient care if it occurred before 2001 and inpatient or outpatient care after 2001. People with psychiatric problems who never sought help and who never were referred to psychiatric care were therefore not included. Further, because of a lack of statistical power, we did not study the contribution of length of sentence, physical illness, family history of suicide, and work status, to name a few potentially important factors, that could be considered in future research.
CONCLUSION
In summary, we found that suicide among released prisoners was 18 times more common than in the general population, with particularly high risks during the first 4 weeks. A previous suicide attempt; previous psychiatric disorder, particularly substance abuse; and being born in Sweden were important, independent risk factors. We found a different pattern of psychiatric risk factors for suicide among released prisoners compared with suicide in the general population.
Our findings are consistent with those from other high-income countries with different prison systems than Sweden, such as the United States, England, and Australia, suggesting some generalizability of previous results in this field. Further, our study advances knowledge on suicide risk factors among ex-prisoners, which should inform suicide risk assessment following release from prison. Future research in this field is needed, for example, to investigate the role of risk assessment, psychiatric treatment, and efforts aimed to facilitate transition to life outside prison.
The elevated suicide rates in this study underline the need for selective preventive efforts for this high-risk group. Hence, prison and probation services, mental health care, and social services may need to collaborate to develop evidence-based prevention strategies for this population. Other implications arising from our findings include allocating appropriate resources to facilitate transition to life outside prison, as well as increased clinical monitoring during the first 4 weeks after release for ex-prisoners with a history of both previous suicide attempts and substance abuse. In addition, consideration should be given to involving community mental health services before release from prison in those at high risk. Finally, the risk of suicide after release from prison should be highlighted. National suicide prevention strategies should include recently released prisoners as a high-risk group.
Author affiliations: Departments of Clinical Neuroscience (Drs Haglund, Tidemalm, Jokinen, and Runeson) and Medical Epidemiology and Biostatistics (Drs Långström and Lichtenstein), Karolinska Institutet, Stockholm, Sweden; and Department of Psychiatry, University of Oxford, United Kingdom (Dr Fazel).
Potential conflicts of interest: Dr Långström has received one speaker honorarium from Lundbeck in the past year. Dr Runeson has received honoraria from AstraZeneca AB, Lundbeck Foundation, and Lilly in the past year. Drs Haglund, Tidemalm, Jokinen, Lichtenstein, and Fazel report no conflicts of interest.
Funding/support: Dr Haglund received financial support for this research project from the Swedish Prison and Probation Administration. Dr Jokinen received support from the Swedish Research Council (K2009-61P-21304-04-4). Dr Långström received support from the Swedish Prison and Probation Administration. Dr Fazel received support from the Wellcome Trust.
Role of the sponsors: The sponsors had no role in the design and conduct of the study; in collection, management, analysis, and interpretation of the data; and in preparation, review, or approval of the manuscript.
Previous presentation: Preliminary data from this study were presented in an oral presentation at the International Association for Suicide Prevention’s World Congress; September 24–28, 2013; Oslo, Norway.
Additional information: Ethics approval was obtained from the Stockholm’s Regional Ethics Committee (protocol 2010/5:7)
REFERENCES
1. Walmsley R. World Prison Population List, 9th edition. London, UK: Kings College London International Centre for Prison Studies; 2012. http://www.scribd.com/doc/77097293/World-Prison-Population-List-9th-edition. Accessed June 25, 2014.
2. Schmitt J, Warner K. Ex-offenders and the Labor Market. Center for Economic and Policy Research. http://www.cepr.net/documents/publications/ex-offenders-2010-11.pdf. Updated November 2010. Accessed June 25, 2014.
3. Fazel S, Grann M, Kling B, et al. Prison suicide in 12 countries: an ecological study of 861 suicides during 2003–2007. Soc Psychiatry Psychiatr Epidemiol. 2011;46(3):191–195. doi:10.1007/s00127-010-0184-4 PubMed
4. Fazel S, Baillargeon J. The health of prisoners. Lancet. 2011;377(9769):956–965. doi:10.1016/S0140-6736(10)61053-7 PubMed
5. Harris EC, Barraclough B. Suicide as an outcome for mental disorders. a meta-analysis. Br J Psychiatry. 1997;170(3):205–228. doi:10.1192/bjp.170.3.205 PubMed
6. Tidemalm D, Långström N, Lichtenstein P, et al. Risk of suicide after suicide attempt according to coexisting psychiatric disorder: Swedish cohort study with long term follow-up. BMJ. 2008;337:a2205. doi:10.1136/bmj.a2205 PubMed
7. Hawton K, van Heeringen K. Suicide. Lancet. 2009;373(9672):1372–1381. doi:10.1016/S0140-6736(09)60372-X PubMed
8. Fazel S, Seewald K. Severe mental illness in 33,588 prisoners worldwide: systematic review and meta-regression analysis. Br J Psychiatry. 2012;200(5):364–373. doi:10.1192/bjp.bp.111.096370 PubMed
9. Fazel S, Bains P, Doll H. Substance abuse and dependence in prisoners: a systematic review. Addiction. 2006;101(2):181–191. doi:10.1111/j.1360-0443.2006.01316.x PubMed
10. Fazel S, Cartwright J, Norman-Nott A, et al. Suicide in prisoners: a systematic review of risk factors. J Clin Psychiatry. 2008;69(11):1721–1731. doi:10.4088/JCP.v69n1107 PubMed
11. Kariminia A, Law MG, Butler TG, et al. Suicide risk among recently released prisoners in New South Wales, Australia. Med J Aust. 2007;187(7):387–390. PubMed
12. Pratt D, Appleby L, Piper M, et al. Suicide in recently released prisoners: a case-control study. Psychol Med. 2010;40(5):827–835. doi:10.1017/S0033291709991048 PubMed
13. Zlodre J, Fazel S. All-cause and external mortality in released prisoners: systematic review and meta-analysis. Am J Public Health. 2012;102(12):e67–e75. doi:10.2105/AJPH.2012.300764 PubMed
14. Pratt D, Piper M, Appleby L, et al. Suicide in recently released prisoners: a population-based cohort study. Lancet. 2006;368(9530):119–123. doi:10.1016/S0140-6736(06)69002-8 PubMed
15. Binswanger IA, Stern MF, Deyo RA, et al. Release from prison—a high risk of death for former inmates. N Engl J Med. 2007;356(2):157–165. doi:10.1056/NEJMsa064115 PubMed
16. Dirkzwager A, Nieuwbeerta P, Blokland A. Effects of first-time imprisonment on postprison mortality: a 25-year follow-up study with a matched control group. J Res Crime Delinq. 2012;49(3):383–419. doi:10.1177/0022427811415534
17. Binswanger IA, Blatchford PJ, Lindsay RG, et al. Risk factors for all-cause, overdose and early deaths after release from prison in Washington state. Drug Alcohol Depend. 2011;117(1):1–6. doi:10.1016/j.drugalcdep.2010.11.029 PubMed
18. Swedish Prison and Probation Services. Official Statistics. http://www.kriminalvarden.se/sv/Statistik/. Updated 2012. Accessed June 25, 2014.
19. Carli V, Mandelli L, Poštuvan V, et al. Self-harm in prisoners. CNS Spectr. 2011;16(3):75–81. doi:10.1017/S1092852912000211 PubMed
20. Hakansson A, Berglund M. All-cause mortality in criminal justice clients with substance use problems—a prospective follow-up study. Drug Alcohol Depend. 2013;132(3):499–504. doi:10.1016/j.drugalcdep.2013.03.014 PubMed
21. Neeleman J, Wessely S. Changes in classification of suicide in England and Wales: time trends and associations with coroners’ professional backgrounds. Psychol Med. 1997;27(2):467–472. doi:10.1017/S0033291796004631 PubMed
22. Runeson B, Tidemalm D, Dahlin M, et al. Method of attempted suicide as predictor of subsequent successful suicide: national long term cohort study. BMJ. 2010;341(1):c3222. doi:10.1136/bmj.c3222 PubMed
23. Webb RT, Kontopantelis E, Doran T, et al. Suicide risk in primary care patients with major physical diseases: a case-control study. Arch Gen Psychiatry. 2012;69(3):256–264. doi:10.1001/archgenpsychiatry.2011.1561 PubMed
24. Hawton K, Bergen H, Simkin S, et al. Long term effect of reduced pack sizes of paracetamol on poisoning deaths and liver transplant activity in England and Wales: interrupted time series analyses. BMJ. 2013;346(1):f403. doi:10.1136/bmj.f403 PubMed
25. Björkenstam E, Björkenstam C, Vinnerljung B, et al. Juvenile delinquency, social background and suicide—a Swedish national cohort study of 992,881 young adults. Int J Epidemiol. 2011;40(6):1585–1592. doi:10.1093/ije/dyr127 PubMed
26. Frisell T, Lichtenstein P, Långström N. Violent crime runs in families: a total population study of 12.5 million individuals. Psychol Med. 2011;41(1):97–105. PubMed
27. Binswanger IA, Nowels C, Corsi KF, et al. Return to drug use and overdose after release from prison: a qualitative study of risk and protective factors. Addict Sci Clin Pract. 2012;7(1):3. doi:10.1186/1940-0640-7-3 PubMed
28. Bohnert AS, Ilgen MA, Ignacio RV, et al. Risk of death from accidental overdose associated with psychiatric and substance use disorders. Am J Psychiatry. 2012;169(1):64–70. doi:10.1176/appi.ajp.2011.10101476 PubMed
29. Fazel S, Benning R. Suicides in female prisoners in England and Wales, 1978–2004. Br J Psychiatry. 2009;194(2):183–184. doi:10.1192/bjp.bp.107.046490 PubMed
30. Fazel S, Långström N, Hjern A, et al. Schizophrenia, substance abuse, and violent crime. JAMA. 2009;301(19):2016–2023. doi:10.1001/jama.2009.675 PubMed
31. Van Dorn R, Volavka J, Johnson N. Mental disorder and violence: is there a relationship beyond substance use? Soc Psychiatry Psychiatr Epidemiol. 2012;47(3):487–503. doi:10.1007/s00127-011-0356-x PubMed
32. Stenbacka M, Moberg T, Romelsjö A, et al. Mortality and causes of death among violent offenders and victims—a Swedish population based longitudinal study. BMC Public Health. 2012;12(1):38. doi:10.1186/1471-2458-12-38 PubMed
33. Joukamaa M. The mortality of released Finnish prisoners; a 7 year follow-up study of the WATTU project. Forensic Sci Int. 1998;96(1):11–19. doi:10.1016/S0379-0738(98)00098-X PubMed
34. Webb RT, Qin P, Stevens H, et al. National study of suicide in all people with a criminal justice history. Arch Gen Psychiatry. 2011;68(6):591–599. doi:10.1001/archgenpsychiatry.2011.7 PubMed
35. Crump C, Sundquist K, Sundquist J, et al. Sociodemographic, psychiatric and somatic risk factors for suicide: a Swedish national cohort study. Psychol Med. 2014;44(2):279–289. PubMed
36. Ferrada-Noli M. A cross-cultural breakdown of Swedish suicide. Acta Psychiatr Scand. 1997;96(2):108–116. doi:10.1111/j.1600-0447.1997.tb09914.x PubMed
37. Martens P, Holmberg S. Crime Among Persons Born in Sweden and Other Countries. Stockholm, Sweden: National Council for Crime Prevention; 2005.
38. Grann M, Danesh J, Fazel S. The association between psychiatric diagnosis and violent re-offending in adult offenders in the community. BMC Psychiatry. 2008;8(1):92. doi:10.1186/1471-244X-8-92 PubMed
39. Lundholm L, Haggård U, Möller J, et al. The triggering effect of alcohol and illicit drugs on violent crime in a remand prison population: a case crossover study. Drug Alcohol Depend. 2013;129(1–2):110–115. doi:10.1016/j.drugalcdep.2012.09.019 PubMed
40. Fazel S, Danesh J. Serious mental disorder in 23000 prisoners: a systematic review of 62 surveys. Lancet. 2002;359(9306):545–550. doi:10.1016/S0140-6736(02)07740-1 PubMed
41. Agerbo E. High income, employment, postgraduate education, and marriage: a suicidal cocktail among psychiatric patients. Arch Gen Psychiatry. 2007;64(12):1377–1384. doi:10.1001/archpsyc.64.12.1377 PubMed
42. Gvion Y, Apter A. Aggression, impulsivity, and suicide behavior: a review of the literature. Arch Suicide Res. 2011;15(2):93–112. doi:10.1080/13811118.2011.565265 PubMed
43. Dalman Ch, Broms J, Cullberg J, et al. Young cases of schizophrenia identified in a national inpatient register—are the diagnoses valid? Soc Psychiatry Psychiatr Epidemiol. 2002;37(11):527–531. doi:10.1007/s00127-002-0582-3 PubMed
44. Sellgren C, Landén M, Lichtenstein P, et al. Validity of bipolar disorder hospital discharge diagnoses: file review and multiple register linkage in Sweden. Acta Psychiatr Scand. 2011;124(6):447–453. doi:10.1111/j.1600-0447.2011.01747.x PubMed




