Conservative physicians were about five times more likely than their liberal and moderate colleagues to say that they would treat a hypothetical COVID-19 patient with hydroxychloroquine.
The authors of a new study suggest that this willingness to prescribe controversial pandemic drugs shows just how much political ideology shapes a physician’s attitudes towards scientific evidence.
Published in Proceedings of the National Academy of Sciences, the study found that participants with conservative political beliefs were more inclined to view hydroxychloroquine favorably and vaccination unfavorably, and that this was true of laypeople and physicians alike. Conservative ideology was also linked with favorable beliefs about ivermectin among laypeople, though not necessarily physicians.
Telepsychiatry in Flux Due to Shifting Pandemic-Era Rules
New Findings Help Make Sense of Brain Fog From Long COVID
COVID-19–Associated Benzodiazepine-Resistant Catatonia Responds to Amantadine
“In the United States, conservatives and liberals disagree about the facts,” University of Pittsburgh scientists wrote in their paper.
To test this theory, the researchers surveyed nearly 600 board certified critical care physicians and 900 average Americans. They chose the critical care specialty because they are on the frontlines of COVID care yet less involved in patient preferences than most other specialties, the authors explained.
In a series of questionnaires, physicians were asked to evaluate a clinical vignette about a severely ill COVID patient and then decide on the best course of action. They were also asked to assess all of the available treatment options based on their perception of the data’s scientific rigor. The average joes filled out the same assessment minus the treatment recommendations and both groups were surveyed for their thoughts on COVID vaccines.
On average, physicians’ beliefs were less polarized than laypeoples’ but their political leanings did influence their opinions about vaccination and hydroxychloroquine, with liberal docs polling more pro vaccine and anti hydroxychloroquine than their conservative counterparts.
When ivermectin wasn’t identified, liberals and conservatives drew largely similar conclusions about the drug’s benefits. But when they were told the drug given was ivermectin, conservatives expressed more skepticism than liberals about any information that questioned its effectiveness. This doesn’t necessarily mean that physicians evaluate evidence about ivermectin with a political spin, the scientists said.
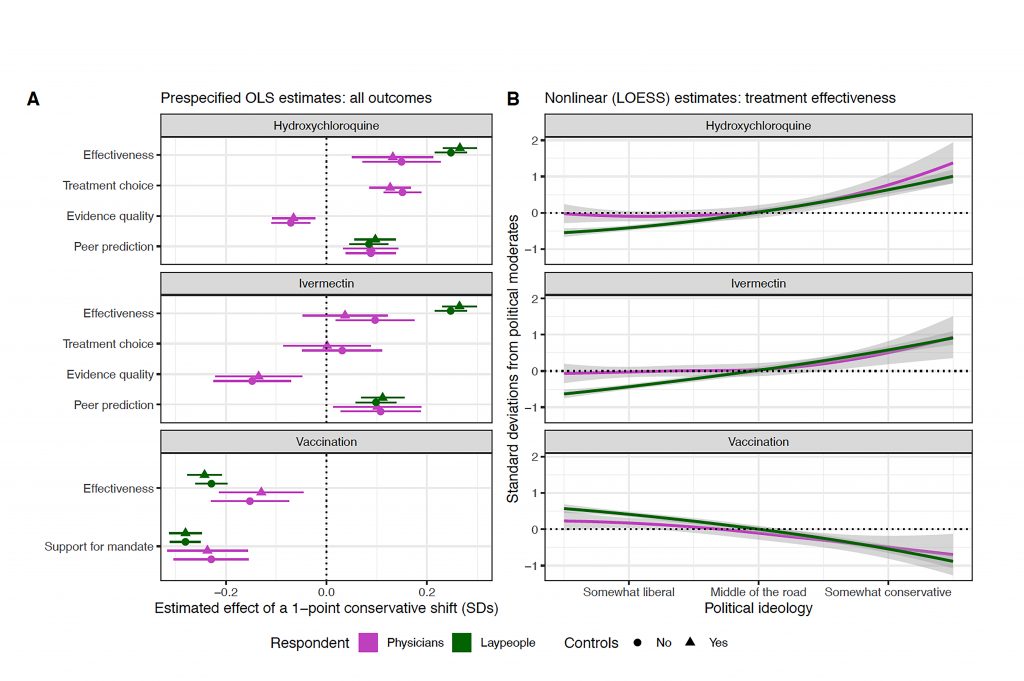
“What our study does show is that people evaluate scientific evidence about ivermectin in a biased way,” explained senior author Jeremy Kahn, M.D., professor of critical care medicine at Pitt’s School of Medicine and health policy and management at Pitt’s School of Public Health.
“Physicians are human, and they have biases that are driven by their political ideology. I think there’s a notion among the public that decision makers and experts arrive at their viewpoints through analysis of empirical data and base their decisions on the best available evidence, but this study suggests that this is not the whole story,” he added.
All the physicians in the study were highly trained and had access to the same information, so the contrasting opinions weren’t for lack of knowledge or motivation, the scientists noted.
The one big difference between the two groups? Fox News.
A dramatic preference for Fox News by conservative docs suggests that polarization was driven by their taste for partisan cable news but not by exposure to scientific research – and that exposure to different information could contribute to polarized beliefs, the researchers wrote. And, as the findings also suggest, this variation is driven in part, by the beliefs of physicians rather than by patient preferences alone.
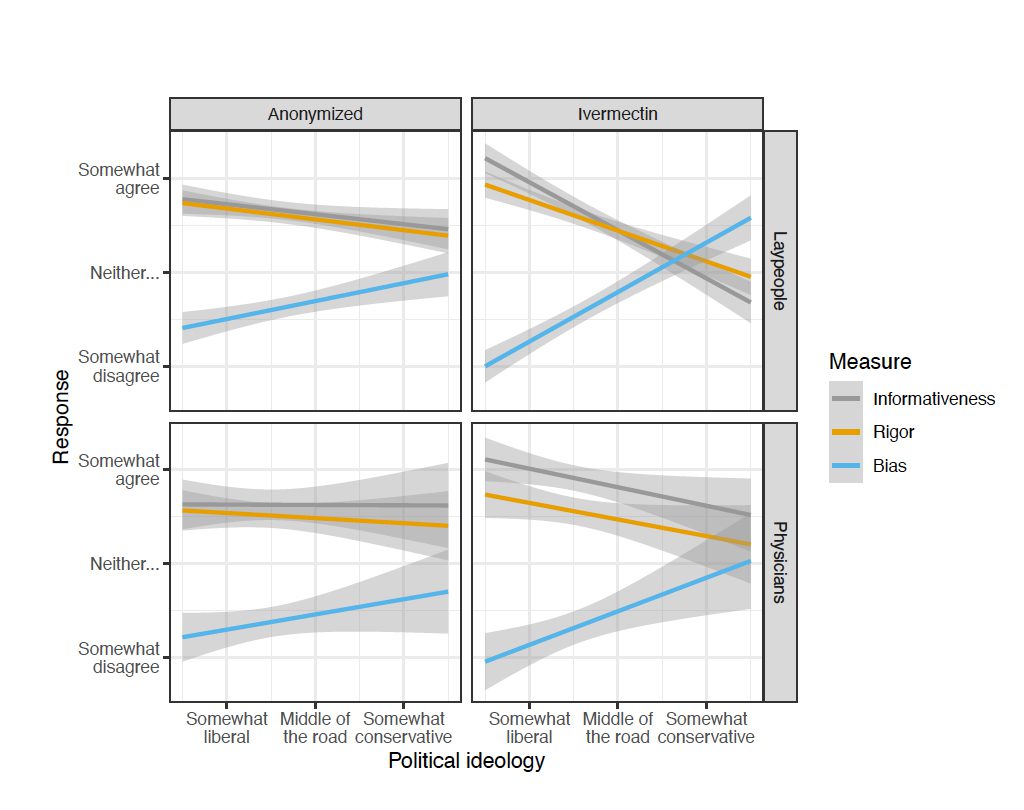
These results underscore the extent to which political ideology is increasingly relevant for understanding beliefs, even among expert decision makers like physicians. Education alone is likely not enough to combat polarization in the medical profession.
“The challenge now is thinking about how we can achieve consensus among physicians around the best available evidence to treat patients to achieve the best possible outcomes,” Kahn said.



