Patients with posttraumatic stress disorder (PTSD) often experience symptoms of psychological distress, including flashbacks and nightmares.1 Prazosin, an α-1 adrenergic receptor antagonist, is used off label for PTSD symptoms.2 The purported mechanism of action is that prazosin crosses the blood-brain barrier to reduce the fear response associated with increased adrenergic activity.3 Prazosin is dosed 3 times daily for hypertension, while in PTSD, it is typically given once daily at bedtime.4 There is potential that more frequent administration may be beneficial for PTSD-induced psychological distress; however, this is limited by side effects, particularly hypotension. This case report discusses our experience utilizing a 3-times daily dosing scheme during a hospital admission for a patient experiencing severe nightmares and daytime flashbacks associated with PTSD.
Case Report
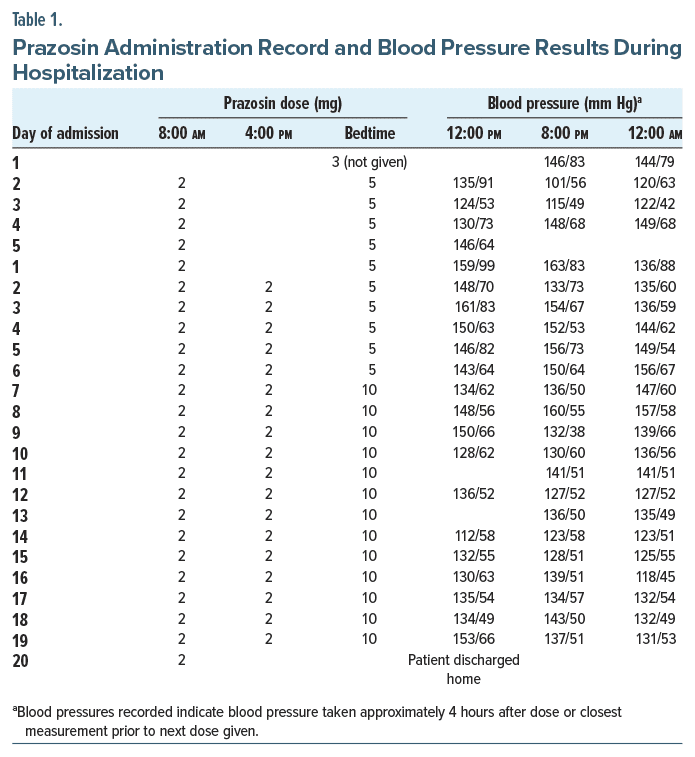
A 53-year-old man presented to the emergency department (ED) with complaints of fatigue following 3 missed hemodialysis sessions. The patient reported recurrent, terrifying flashbacks from past military service, which interrupted his sleep and disrupted his ability to attend hemodialysis. His psychiatric history included PTSD, chronic suicidal ideation, and depression. Psychiatric medications prescribed included hydroxyzine, prazosin, sertraline, and quetiapine. Current medical comorbidities included end-stage renal disease, heart failure, atrial fibrillation, cirrhosis, history of myocardial infarction, and hypertension. Prior to admission, the patient’s prazosin dose was increased to 3 mg once daily for worsening symptoms, which were reported as flashbacks causing severe insomnia. The patient felt that medications were helping; however, he endorsed continued, frequent awakenings and daytime flashbacks of wartime experiences, which continued to trouble him during his hospital admission. We titrated the prazosin dose as reported in Table 1. The patient was discharged on twice-daily prazosin, which was reported to decrease intensity and frequency of symptoms.
Six days later, the patient was readmitted to the ED with complaints of abdominal swelling and was found to have methicillin-resistant Staphylococcus aureus bacteremia. He continued to take prazosin twice daily, which he reported to be more helpful for symptoms, but still endorsed breakthrough flashbacks. Prazosin was increased to 3 times daily: 2 mg in the morning, 2 mg at 4:00 pm, and 5 mg at bedtime. On day 7 of admission, the bedtime dosing was increased to 10 mg, while the other doses remained at 2 mg. Blood pressures remained stable throughout admission (Table 1). The patient reported subjective improvement in sleep and anxiety levels with the increased prazosin dose. No additional changes were made to the regimen, and the patient was ultimately discharged home on day 20.
Discussion
Data regarding the overall effectiveness of prazosin for PTSD have been inconsistent.5–7 While prazosin is typically dosed at night for PTSD, the medication only has a 2 to 3–hour half life, and the peak effect only lasts for 2–4 hours, suggesting it may not be as effective at controlling PTSD-induced symptoms throughout the day.4,8 We identified only 1 other case report that utilized a 3-times-daily dosing scheme.9 The authors9 found that the more frequent dosing scheme was effective at reducing their patient’s subjective PTSD-induced symptoms without substantially impacting blood pressure. Nevertheless, the patient in their study was seen in the clinic,9 and concerns of prazosin-induced hypotension may limit inpatient initiation of more frequent dosing schemes.2,4 We collected blood pressures throughout the day over a period of 5 weeks with no evidence of prazosin-induced hypotension. The patient was discharged on a total daily prazosin dose of 14 mg in divided doses of 2 mg, 2 mg, and 10 mg. The goal of reporting our experience is to raise awareness of this dosing scheme as an option for in hospital use in patients experiencing severe PTSD symptoms, especially given ability to monitor hemodynamic responses more closely during an inpatient admission. We found that initiation of a 3-times-daily regimen of prazosin significantly improved the patient’s symptoms without evidence of harm.
Article Information
Published Online: June 25, 2024.
https://doi.org/10.4088/PCC.23cr03696
© 2024 Physicians Postgraduate Press, Inc.
Prim Care Companion CNS Disord 2024;26(3):23cr03696
Submitted: January 2, 2024; accepted March 11, 2024.
To Cite: Tucker KJ, Villanueva TT, Fletcher M, et al. A 3- times-daily dosing scheme of prazosin to treat posttraumatic stress disorder–induced psychological distress in the hospital. Prim Care Companion CNS Disord. 2024;26(3):23cr03696.
Author Affiliations: Department of Pharmacy Practice, College of Pharmacy, Oregon State University, Portland, Oregon (Tucker, Villanueva, Herink); Department of Family Medicine, Oregon Health & Science University, Portland, Oregon (Fletcher, Putnam).
Corresponding Author: Kendall J. Tucker, PharmD, MS, Department of Pharmacy Practice, College of Pharmacy, Oregon State University, 2730 S Moody Ave, CL5CP, Portland, OR 97201 ([email protected]).
Relevant Financial Relationships: None.
Funding/Support: None.
Additional Information: Patient information has been de-identified to protect anonymity.
ORCID: Kendall J. Tucker: https://orcid.org/0000-0001-5868-0449; Trisha T. Villanueva: https://orcid.org/0009-0007-3257-2918; Megan C. Herink: https://orcid.org/0000-0001-6402-0260; Miles Fletcher: https://orcid.org/0000-0001-8666-1261
References (9)

- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th edition, Text Revision. American Psychiatric Association; 2022.
- Hudson SM, Whiteside TE, Lorenz RA, et al. Prazosin for the treatment of nightmares related to posttraumatic stress disorder: a review of the literature. Prim Care Companion CNS Disord. 2012;14(2):11r01222. PubMed CrossRef
- Do Monte FH, Souza RR, Wong TT, et al. Systemic or intra-prelimbic cortex infusion of prazosin impairs fear memory reconsolidation. Behav Brain Res. 2013;244:137–141. PubMed CrossRef
- Basquez R, Pippin MM. Prazosin. In: StatPearls [Internet]. StatPearls Publishing; 2023. Accessed October 3, 2023. https://www.ncbi.nlm.nih.gov/books/NBK555959/
- Raskind MA, Peskind ER, Chow B, et al. Trial of prazosin for post-traumatic stress disorder in military veterans. N Engl J Med. 2018;378(6):507–517. PubMed CrossRef
- Singh B, Hughes AJ, Mehta G, et al. Efficacy of prazosin in posttraumatic stress disorder: a systematic review and meta-analysis. Prim Care Companion CNS Disord. 2016;18(4):16r01943
- Khachatryan D, Groll D, Booij L, et al. Prazosin for treating sleep disturbances in adults with posttraumatic stress disorder: a systematic review and meta-analysis of randomized controlled trials. Gen Hosp Psychiatry. 2016;39:46–52. PubMed CrossRef
- Prazosin (minipress) [Package Insert]. Pfizer Labs; 2009.
- Richardson C, Swartz A, Forsberg M. Prazosin dosed 3 times a day to treat flashbacks related to PTSD: a case report. Ment Health Clin:12(4):267–269. PubMed
Enjoy this premium PDF as part of your membership benefits!