Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
Serotonin syndrome is a potentially life-threatening condition that is particularly relevant to both primary care and psychiatric clinical practice. Serotonin syndrome has been documented with increasing frequency in recent years, in part due to the increased use of selective serotonin reuptake inhibitors, serotonin-norepinephrine reuptake inhibitors, and other serotonergic medications. However, it is still relatively underdiagnosed and underreported.

A Case of Serotonin Syndrome in the Setting of Dextromethorphan-Based Cough Medicine, Tramadol, and Multiple Antidepressants
Serotonin syndrome is a potentially life-threatening condition that is particularly relevant to both primary care and psychiatric clinical practice. Serotonin syndrome has been documented with increasing frequency in recent years, in part due to the increased use of selective serotonin reuptake inhibitors, serotonin-norepinephrine reuptake inhibitors, and other serotonergic medications.1-3 However, it is still relatively underdiagnosed and underreported.1,4 We present a case of serotonin syndrome resulting from the use of dextromethorphan-based cough medicine in addition to multiple antidepressant and pain medications.
Case Report
Ms A, a 68-year-old woman with past psychiatric history of bipolar II disorder and past medical history of poorly controlled diabetes, hypertension, and hypothyroidism, presented to the emergency department of a large teaching hospital complaining of weakness and difficulty walking. She also reported recent nausea, vomiting, and diarrhea. She was found to have tachycardia, diaphoresis, dry mucous membranes, abdominal tenderness, and tremor but was afebrile, alert, and oriented. Initial laboratory studies were notable for elevated white blood cells (14 ×—109/L), anion gap metabolic acidosis (gap 21, HCO3 16 mmol/L), and elevated blood glucose (322 mg/dL). Computed tomography scans of the head and abdomen/pelvis revealed no acute abnormalities. Initially, emergency department staff were concerned for sepsis or diabetic ketoacidosis and treated her symptoms with intravenous ondansetron and normal saline before admitting her to the internal medicine service.
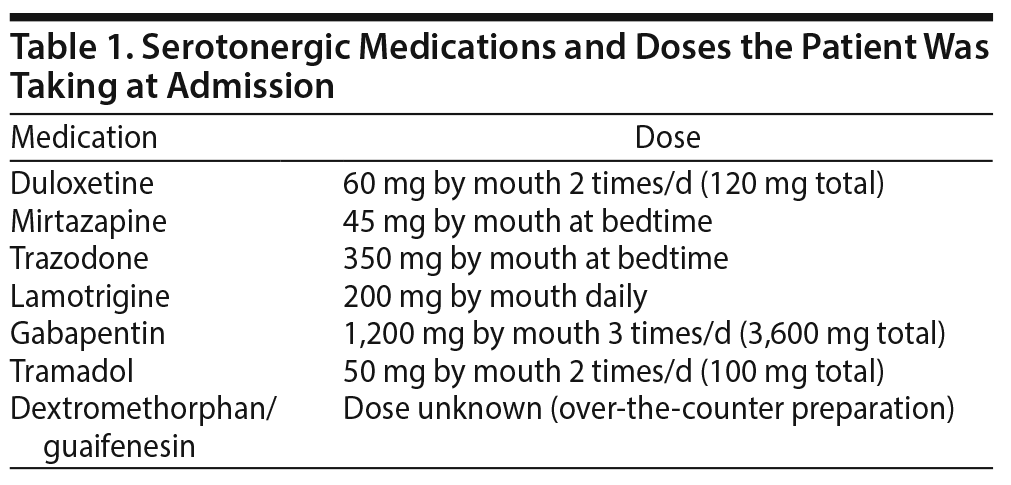
Further review of the patient’s medical record revealed that she was being prescribed high doses of duloxetine, mirtazapine, trazodone, lamotrigine, gabapentin, and tramadol (Table 1). She had been stable on this regimen for several weeks. However, she had recently started taking over-the-counter dextromethorphan/guaifenesin for an upper respiratory infection. A thorough neurologic examination demonstrated bilateral fine tremors in hands, stiffness in elbows/wrists, inducible ankle clonus, lower extremity hypertonia, and diffuse hyperreflexia. A diagnosis of serotonin syndrome was made using the Hunter diagnostic criteria.5 All serotonergic medications were held. She rapidly improved over the following 48 hours and was discharged home on a significantly simplified medication regimen.
Discussion
Serotonin syndrome can be challenging to recognize, given its often nuanced presentation and overlap with other clinical syndromes. The classic triad of autonomic instability (hypertension, tachycardia, diaphoresis), altered mental status (delirium, agitation), and neuromuscular findings (tremors, clonus, hyperreflexia) is often not present, particularly in mild or moderate cases.1,6,7 Laboratory findings, such as metabolic acidosis and elevated white blood cell count, are nonspecific and may detract from the correct diagnosis.2 Delays in diagnosis can result in inappropriate treatment that may prolong or even worsen serotonin syndrome. In the present case, the patient was initially administered another serotoninergic agent, ondansetron. Neuromuscular symptoms appear to be the most specific finding in serotonin syndrome.7 Thus, the diagnosis is most accurately made through a thorough neurologic examination, as this case demonstrates. According to the Hunter diagnostic criteria, patients must have been exposed to 1 or more serotonergic agents and have at least 1 of the following findings: (1) spontaneous clonus, (2) inducible clonus plus agitation or diaphoresis, (3) ocular clonus plus agitation or diaphoresis, (4) tremor plus hyperreflexia, or (5) hypertonia plus temperature above 38°C plus ocular clonus or inducible clonus. These criteria are 84% sensitive and 97% specific to the diagnosis of serotonin syndrome.5
Psychiatrists and primary care physicians should be able to recognize and diagnose the syndrome early, given that the cause is often iatrogenic and the most commonly prescribed psychiatric medications are serotonergic.3 In this patient’s case, it was the additional use of a seemingly benign cough medicine containing dextromethorphan (which has been linked to serotonin syndrome8) that appears to have precipitated the syndrome. Thus, providers should also be closely aware of all medications, both psychiatric and nonpsychiatric and over-the-counter or prescribed, that their patients are taking.3,4,9 They should especially seek to avoid situations of hazardous polypharmacy.
Published online: March 5, 2020.
Potential conflicts of interest: None.
Funding/support: None.
Patient consent: Informed consent was obtained from the patient to publish this case report, and information was de-identified to protect anonymity.
REFERENCES
1.Boyer EW, Shannon M. The serotonin syndrome. N Engl J Med. 2005;352(11):1112-1120. PubMed CrossRef
2.Mason PJ, Morris VA, Balcezak TJ. Serotonin syndrome: presentation of 2 cases and review of the literature. Medicine (Baltimore). 2000;79(4):201-209. PubMed CrossRef
3.Ables AZ, Nagubilli R. Prevention, recognition, and management of serotonin syndrome. Am Fam Physician. 2010;81(9):1139-1142. PubMed
4.Wang RZ, Vashistha V, Kaur S, et al. Serotonin syndrome: preventing, recognizing, and treating it. Cleve Clin J Med. 2016;83(11):810-817. PubMed CrossRef
5.Dunkley EJC, Isbister GK, Sibbritt D, et al. The Hunter Serotonin Toxicity Criteria: simple and accurate diagnostic decision rules for serotonin toxicity. QJM. 2003;96(9):635-642. PubMed CrossRef
6.Buckley NA, Dawson AH, Isbister GK. Serotonin syndrome. BMJ. 2014;348:g1626. PubMed
7.Werneke U, Jamshidi F, Taylor DM, et al. Conundrums in neurology: diagnosing serotonin syndrome: a meta-analysis of cases. BMC Neurol. 2016;16(97):97. PubMed
8.Schwartz AR, Pizon AF, Brooks DE. Dextromethorphan-induced serotonin syndrome. Clin Toxicol (Phila). 2008;46(8):771-773. PubMed CrossRef
9.Dvir Y, Smallwood P. Serotonin syndrome: a complex but easily avoidable condition. Gen Hosp Psychiatry. 2008;30(3):284-287. PubMed CrossRef
aUnited States Air Force, Medical Corps, 59th Medical Wing, Joint Base-San Antonio, San Antonio, Texas
bDepartment of Psychiatry, University of Texas Health San Antonio, San Antonio, Texas
cUnited States Army, Medical Corps, Joint Base-San Antonio, San Antonio, Texas
dDepartment of Psychiatry, Uniformed Services University, Bethesda, Maryland
eDepartment of Psychiatry, New York University Langone Health, New York, New York
*Corresponding author: Morgan Hardy, MD, MPH, Department of Psychiatry, University of Texas Health San Antonio, 7703 Floyd Curl Drive, San Antonio, TX 78210 ([email protected]).
Prim Care Companion CNS Disord 2020;22(2):19l02518
To cite: Hardy M, Panikkar G. A case of serotonin syndrome in the setting of dextromethorphan-based cough medicine, tramadol, and multiple antidepressants. Prim Care Companion CNS Disord. 2020;22(2):19l02518.
To share: https://doi.org/10.4088/PCC.19l02518
© Copyright 2020 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!