Accuracy of Self-Reported Weight and Height and Resulting Body Mass Index Among Obese Binge Eaters in Primary Care: Relationship With Eating Disorder and Associated Psychopathology
Objective: This study assessed the accuracy of self-reported weight, height, and body mass index in obese patients with binge-eating disorder (DSM-IV-TR criteria) presenting at primary care clinics and tested whether the degree of inaccuracy was associated with demographic factors or eating disorder and depressive features.
Method: Sixty-six participants were interviewed using the Eating Disorder Examination interview, completed the Eating Disorder Examination Questionnaire and the Beck Depression Inventory, and had their height and weight measured between November 2007 and May 2009.
Results: Self-reported and measured weight did not differ significantly, but participants significantly overestimated their height (P < .01), and this discrepancy resulted in a significantly lower self-reported than measured body mass index (P < .05). Discrepancy scores did not differ by eating disorder or depressive symptoms, sex, or ethnicity, although increasing age was associated with overestimation of height and underestimation of body mass index.
Conclusions: The findings suggest that obese patients with binge-eating disorder in primary care settings are reasonably accurate reporters of weight and height and that the degree of inaccuracy does not appear to be systematically related to eating disorder psychopathology or depressive features.
Prim Care Companion J Clin Psychiatry 2010;12(4):e1-e6
© Copyright 2010 Physicians Postgraduate Press, Inc.
Submitted: August 6, 2009; accepted October 26, 2009.
Published online: July 1, 2010 (doi:10.4088/PCC.09m00868blu).
Corresponding author: Rachel D. Barnes, PhD, Program for Obesity, Weight, and Eating Research, Yale University School of Medicine, PO Box 208098, New Haven, CT 06520-8098 ([email protected]).
Research with eating and weight disorders sometimes requires reliance upon self-reported weight and height data because of the impracticality of obtaining actual measurements. This practice is supported by well-known findings that, in general, self-reported weight is highly correlated with measured weight.1 Although individuals report their weight reasonably accurately, research has found that there tends to be bias toward underreporting weight and overreporting height.2 Underreporting weight tends to increase with increasing overweight, and the degree of inaccuracy of self-reported weight and height varies with a number of characteristics, including age, sex, ethnicity, and education.2,3 The degree of weight underestimation tends to vary across patient groups, with obese persons showing greater inaccuracy.3-6 Interestingly, the few studies that have examined this issue in persons with eating disorders have found that these patient groups tend to be more accurate than other groups,7,8 including patients with binge-eating disorder (BED) who were also obese.9 Systematic biases such as these can have substantial implication for research findings as well as perceptions regarding obesity.3,10
Obese patients with BED represent an important group for studying systematic biases in weight and height reporting, given that eating disorders have been associated with greater accuracy and obesity has been associated with greater inaccuracy. Masheb and Grilo9 found that, among a clinical sample of patients with comorbid obesity and BED, the degree of weight discrepancy was not related to eating disorder psychopathology, depression, or self-esteem.
The lack of relationship between self-report discrepancy and psychopathology has also been found in several studies with obese women5,9,11 and, most recently, in a large epidemiologic study with a wide range of body mass indices (BMIs).12 In contrast, Meyer and colleagues13 recently reported that high eating concerns predicted weight overestimation and high weight concerns predicted weight underestimation in a nonclinical sample of female college students.
Binge-eating disorder is a common clinical problem in primary care settings, but—despite its association with increased health service utilization, health problems, and psychosocial impairment14,15—it is frequently overlooked by health care providers in these settings.14-17 Obese persons with BED who present to general medical settings may differ in important ways from obese persons with BED who seek psychological or behavioral treatments at specialty clinics.9 For example, it is possible that treatment seeking at specialty psychiatry clinics may be associated with distress related to weight, eating, or body image,18,19 whereas obese persons who present to primary care facilities may have different priorities (eg, heightened medical concerns). Thus, the present study aimed to examine the accuracy of self-reported weight and height among obese binge eaters in primary care settings and to explore possible relationships with demographic and clinical variables, including eating disorder and associated psychological features.
METHOD
Participants
Participants were a consecutive series of 66 (16 men and 50 women) obese (BMI ≥ 30 kg/m2) patients with subthreshold BED (≥ 1 binge weekly, n = 17) or full BED (≥ 2 binges weekly, n = 49) from primary care facilities in a large university-based medical center in an urban setting. Participants with subthreshold BED were included because research has found that they generally do not differ significantly from individuals with full BED.20,21 Overall, participants had a mean age of 44.1 (SD = 11.3) years and a mean BMI of 38.1 (SD = 5.2) kg/m2. Ethnicity was as follows: 47.0% (n = 31) white, 33.3% (n = 22) African American, 13.6% (n = 9) Hispanic, 3.0% (n = 2) Asian, 1.5% (n = 1) Native American, and 1.5% (n = 1) multiethnic. Educationally, 9.1% (n = 6) had some high school education, 15.2% (n = 10) had a high school degree or general equivalency diploma, 36.4% (n = 24) had some college or an Associate degree, and 39.4% (n = 26) had a college degree. Three participants’ data were removed. One participant’s weight discrepancy score was more than 3 standard deviations below the mean, and 2 participants did not include either a self-reported height or weight.
Clinical Points
- Binge-eating disorder is a common clinical problem associated with obesity in primary care settings but may be frequently overlooked by health care providers.
- Obese patients with binge-eating disorder in primary care settings are reasonably accurate reporters of their weight, but they may modestly overestimate their height, which leads to underestimations of their resulting body mass index.
- The degree of self-reported height and weight inaccuracy in obese patients with binge-eating disorder does not appear to be systematically related to eating disorder psychopathology or depressive features.
Procedures
Participants were a consecutive series of respondents for a treatment study being performed in primary care for obese persons who binge eat at least once weekly. Participants were recruited via mailings from primary care providers to their patients, placement of flyers and posters in the primary care settings, and direct referrals from primary care providers. Primary care patients who were potentially interested in the treatment study called the investigative team and were screened by phone by research staff to determine potential eligibility. Potentially eligible participants were then scheduled for in-person assessments that were performed by research staff at the investigators’ research facility and not at the primary care facility. Thus, participants were not assessed during or soon after a primary care office appointment during which their weights may have been measured. Study procedures were institutional review board-approved, and all participants provided written informed consent. The study was conducted between November 2007 and May 2009.
During the assessment procedures performed at the research facility (ie, not at the primary care settings), participants completed a battery of self-report questionnaires, which included items for self-reported weight and height, and were subsequently measured and interviewed by doctoral-level research clinicians who were trained in the administration of all of the study’s interviews and measures. Actual measurements of weight and height were obtained after the self-report was completed and during the initial meeting using a calibrated medical balance beam scale.
Diagnoses (subthreshold and full BED diagnoses based on Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision [DSM-IV-TR] criteria) were determined using the Structured Clinical Interview for DSM-IV Axis I Disorders22 and the Eating Disorder Examination (EDE) interview.23 The self-reported and measured weight and height values were used to calculate self-reported BMI and actual BMI, and discrepancy values were generated as the difference between self-reported and actual measurements.
Measures
The EDE23 is a semistructured investigator-based interview that assesses the specific features of eating disorders. The EDE focuses on the previous 28 days, except for the diagnostic items that are rated per the durations stipulated in the DSM-IV-TR.24 The EDE assesses the frequency of different forms of overeating, including objective bulimic episodes (ie, binge eating defined as unusually large quantities of food with a subjective sense of loss of control). The EDE also comprises 4 subscales (dietary restraint, eating concern, weight concern, and shape concern) and an overall global score. The items assessing the features of eating disorders for the 4 EDE subscales are rated on a 7-point forced-choice format (0-6), with higher scores reflecting greater severity or frequency. The EDE has demonstrated good interrater and test-retest reliability in diverse patient groups,25,26 including BED.27
The Eating Disorder Examination Questionnaire (EDE-Q)28 is the self-report version of the EDE. The EDE-Q focuses on the previous 28 days and assesses the same eating disorder features as does the EDE and generates the same 4 subscales and overall global score. The EDE-Q has received psychometric support, including adequate test-retest reliability29 and good convergence with the EDE in studies of BED performed in specialty clinics, although the EDE-Q tends to result in higher subscale scores than the EDE interview.30,31 The present study used the EDE-Q version with instructions; this version includes added written definitions and examples of binge eating that have been found to improve the performance of the self-report questionnaire in 2 studies with BED performed in specialty clinics.32,33
The 21-item Beck Depression Inventory34 assesses current depression level and symptoms of depression. It is a widely used and well-established measure with excellent reliability and validity.35 Higher scores reflect higher levels of depression and, more broadly, negative affect and are an efficient marker for broad psychopathology.36
Data Analyses
Participants’ measured weight, height, and resulting BMI were subtracted from their self-reported measurements to create discrepancy scores. Positive scores denote participants’ overestimating their weight, height, or BMI, while negative scores indicate underestimation. Pearson r, independent samples t test, Student paired t test, and 1-way between-groups analyses of variances were used for the normally distributed data. Kendall Ï„b, Mann-Whitney U test, Wilcoxon matched-pairs signed rank test, and Kruskal-Wallis test were used for the nonnormally distributed data. Participants’ height discrepancy scores were normally distributed, whereas their weight and BMI discrepancy scores were nonnormally distributed. The discrepancy scores were examined in relation to both the EDE interview and the self-report EDE-Q. These “parallel” analyses explored whether the discrepancy scores for weight and height might be differentially associated with the 2 different assessment methods in light of established findings that the EDE-Q tends to produce higher subscale scores than the interview.30
RESULTS
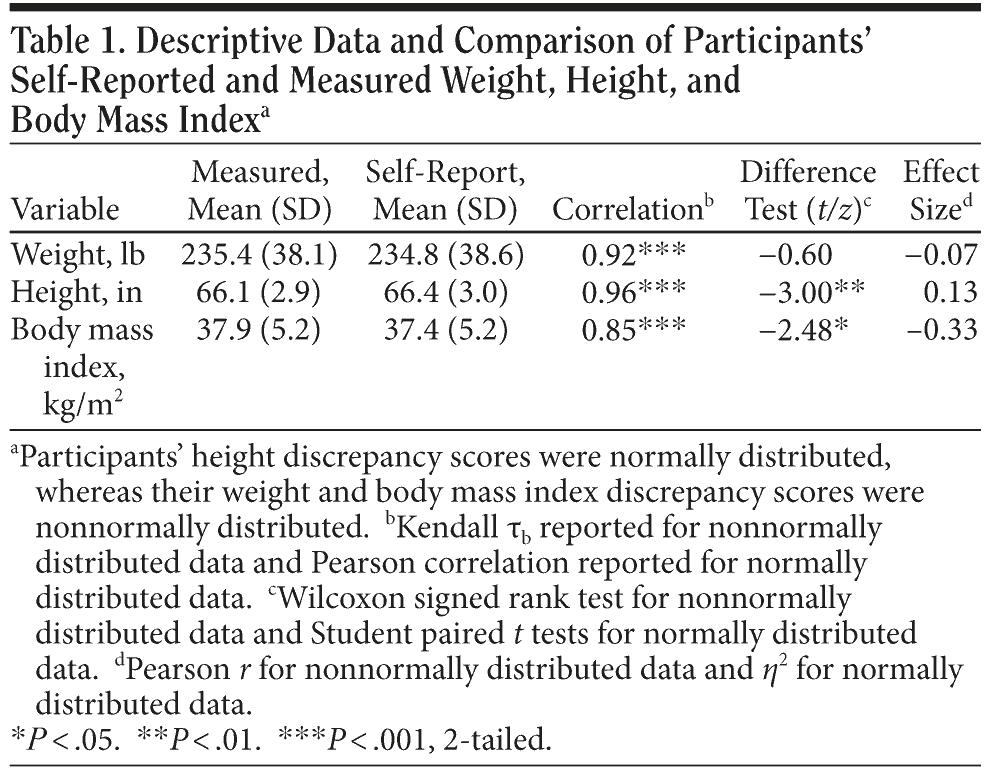
Table 1 summarizes self-reported and actual measured weight, height, and BMI data and statistical analyses of the degree of association and the magnitude of differences. Self-reported weight, height, and BMI were significantly correlated with the measured scores. Comparisons between self-reported and measured indices, based on Wilcoxon signed rank tests and Student paired t tests, found that participants accurately reported their weight (effect size for difference, r = −0.07, small) but significantly overestimated their height (effect size for difference, Å‹2 = 0.13, small), and the resulting self-report BMI was significantly lower than the measured BMI (effect size r = −0.33, medium). On average, participants underestimated their weight by a mean of 0.6 (SD = 5.9) lb and overestimated their height by a mean of 0.3 (SD = 0.9) inches, and these self-reported data resulted in a BMI underestimation of a mean of 0.4 (SD = 1.30) kg/m2.
Men and women did not differ significantly in their tendency to underestimate their weight (Mann-Whitney U = 258.5, z = −1.40, P = .16) or to overestimate their height (t61 = 0.95, P = .35); the degree of discrepancy in resulting BMI also did not differ significantly by sex (Mann-Whitney U = 241, z = −1.69, P = .09). Patients who met BED criteria at full threshold versus at subthreshold criteria did not differ significantly in their tendency to underestimate their weight (Mann-Whitney U = 376, z = −1.20, P = .23) or to overestimate their height (t61 = 0.38, P = .70); the degree of discrepancy in resulting BMI also did not differ significantly (Mann-Whitney U = 441, z = −0.27, P = .79).
There was no significant relationship between age and weight discrepancy (r63 = −0.06, P = .53), but age was positively and significantly correlated with height discrepancy (r63 = 0.28, P = .03), and this correlation resulted in a negative and significant correlation with BMI discrepancy (r63 = −0.19, P = .03). Analyses comparing white, African American, and Hispanic participants revealed no significant differences between these ethnic groups for weight (Kruskal-Wallis χ22 [n = 59] = 2.84, P = .24), height (F2,56 = 0.56, P = .58), or BMI (Kruskal-Wallis χ22 [n = 59] = 3.60, P = .17) discrepancy scores.
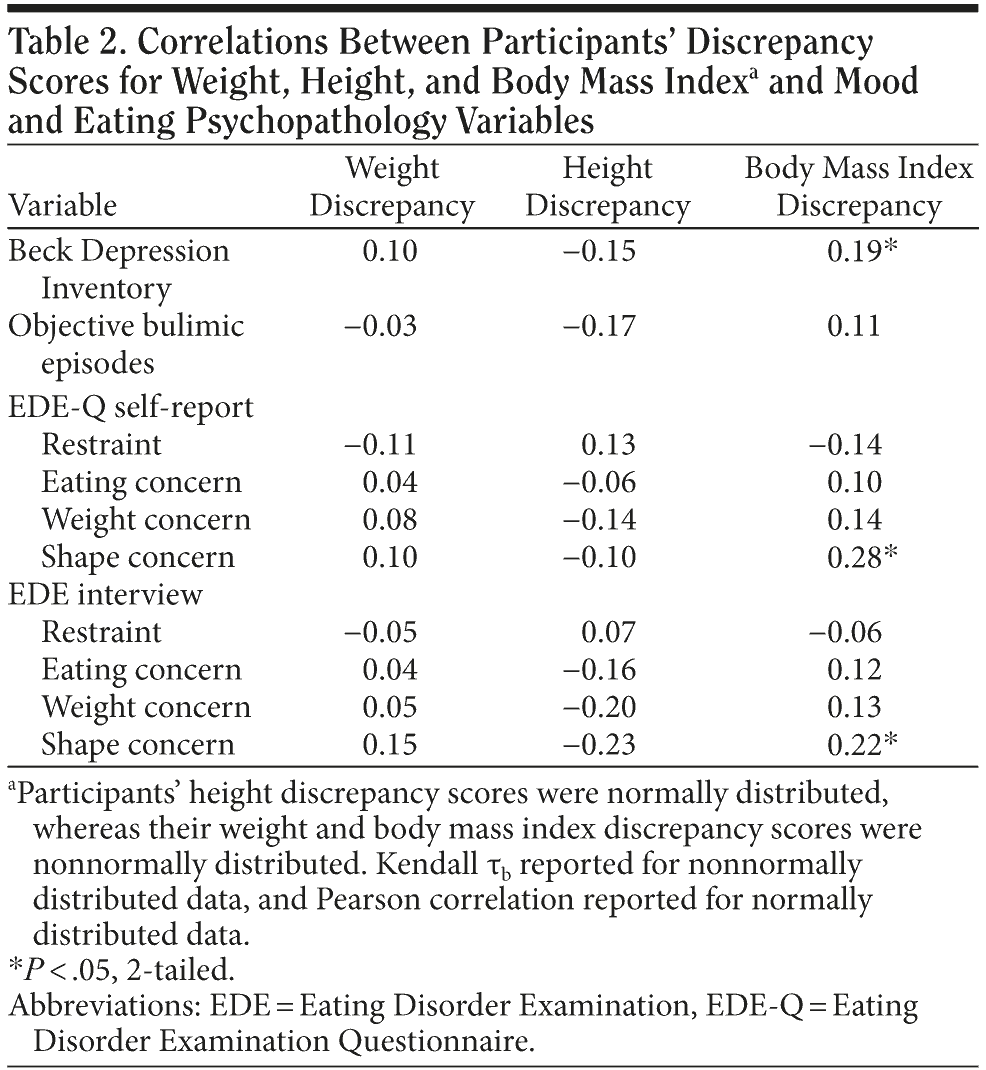
Table 2 summarizes the correlations between participants’ discrepancy scores for weight, height, and BMI and the depressive and eating disorder psychopathology variables. The Beck Depression Inventory scores, objective bulimic episode frequency, and the 4 EDE scales (both the interview and the self-report measures) were not significantly associated with weight discrepancy or with height discrepancy scores. Similarly, only 2 (Beck Depression Inventory and shape concern) of the 6 correlations between these variables and BMI discrepancy scores were statistically significant at the P < .05 level; Bonferroni correction for multiple comparisons yields all nonsignificant findings.
DISCUSSION
This study assessed patients with BED who presented at primary care clinics to examine the accuracy of self-report versus measured weight, height, and resulting BMI. Consistent with previous reports for diverse groups, in this consecutive series of obese individuals with binge-eating problems, correlations between self-reported and measured values for weight and height exceeded 0.90. The amount of discrepancy between self-report and actual was quite small for weight and very modest for height. Participants significantly overestimated their height, and this self-reported height discrepancy resulted in a significantly lower self-reported BMI.
Our participants’ accuracy of self-reported weight is similar to that of individuals with BED presenting to specialty clinics9 and to the accuracy observed among patients with other eating disorders7,8; however, their accuracy is unlike that of nonclinical obese individuals who tend to underestimate their weight.3-6 Nearly all of the literature on the accuracy of self-reported weight and height comes from studies that relied on different recruitment methods and with study groups that differ from our participant group, which was recruited from primary care settings. Despite some important differences, the closest relevant study11 recruited non-BED (BMI > 28 kg/m2) participants via the media to an outpatient hospital setting. Overweight and obese participants in that study significantly underestimated their weight to a larger degree than our BED participants; that study failed to assess either height or BMI discrepancies, thus precluding further comparison. Our findings for BED participants are similar to the relevant literature indicating that individuals tend to overestimate their height.2,13
This study also examined whether the discrepancy in self-reported values was related to demographic factors, eating disorder psychopathology, or depressive features. In this study group of obese binge eaters, we found that men and women did not differ significantly in their accuracy of self-report, which is at odds with some studies that men tend to be more likely than women to overestimate their weight and height.37,38 Moreover, we observed no differences between subthreshold and full BED participants in their height and weight discrepancies, which is consistent with the broader literature revealing few differences in eating-related features based on once-weekly versus twice-weekly binge frequency criteria.20,21 We found that the degree of discrepancy between self-reported and actual values did not differ significantly by ethnicity in this study group, which is at odds with some previous reports.6,38 It is possible that the homogeneity of shared clinical characteristics of having an eating disorder, such as BED9 or bulimia nervosa,7 may supersede reporting inaccuracies about height and weight or further biases due to sex and ethnicity observed for other study groups.
In this study group of obese binge eaters, the degree of inaccuracy or discrepancy between self-reported and actual measurements for weight and height were not significantly related to measures of depression or eating disorder psychopathology (assessed with either interview or self-report methods). Similarly, only 2 (Beck Depression Inventory and shape concern) of the 6 correlations between the clinical variables and the degree of discrepancy for BMI were statistically significant, and these modest correlations were not significant after a Bonferroni correction for multiple comparisons. This general lack of significant association between eating disorder psychopathology and degree of accuracy for self-reported weight and height was observed for both self-report and interview assessment methods. Our use of both self-report and interview methods suggests that our findings, which differ from those recently reported by Meyer and colleagues13 for a nonclinical sample, are not attributable to measurement differences. Our observed nonsignificant relationships, however, are consistent with those reported by Masheb and Grilo9 for a treatment-seeking sample of BED patients who presented to a specialty clinic. Similarly, White et al5 found no relationship between self-report accuracy and variables of eating pathology or psychological variables in a sample of severely obese bariatric surgery candidates.
Strengths of this study include an ethnically diverse sample and utilization of well-validated measures to examine eating disorder psychopathology and depressive symptoms. Limitations include the small number of men and fairly limited age range (20 to 65 years) in comparison to other investigations of age-related differences39 (ie, 20 to 80 + years). Lastly, while the primary care sampling may improve generalizability, when compared to specialty care clinics, these individuals self-selected to participate in a research study and, therefore, may differ from those patients in primary care settings who do not. Similarly, the current study does not include a matched sample of obese participants who do not binge eat recruited from primary care. Future studies would benefit from including a direct comparison of a non-BED sample and examining larger samples of men to determine if the lack of sex differences is consistent with this population or due to the lack of statistical power.
Bearing in mind the strengths and weaknesses of this study, findings suggest that overweight patients with binge-eating problems in primary care settings are reasonably accurate reporters of weight and height and that the degree of inaccuracy does not appear to be systematically related to eating disorder psychopathology or depressive features. These findings suggest that research with such patients that has relied on self-report may not necessarily be systematically skewed, as recently suggested by Meyer et al13 for nonclinical samples. This is not to suggest, however, that it is unimportant to carefully obtain measured weights and especially heights whenever possible. Overestimating heights may lead to biased estimates of BMI, and these biased estimates may lead patients and professionals to underestimate risk for associated health problems.3,38
Author affiliation: Department of Psychiatry, Yale University School of Medicine (all authors); Department of Psychology, Yale University (Dr Grilo), New Haven, Connecticut.
Potential conflicts of interest: None reported.
Funding/support: This research was supported by grants from the National Institutes of Health (R01 DK073542, K24 DK070052, and K23 DK071646).
REFERENCES
1. Stunkard AJ, Albaum JM. The accuracy of self-reported weights. Am J Clin Nutr. 1981;34(8):1593-1599. PubMed
2. Gorber SC, Tremblay M, Moher D, et al. A comparison of direct vs self-report measures for assessing height, weight and body mass index: a systematic review. Obes Rev. 2007;8(4):307-326. PubMed doi:10.1111/j.1467-789X.2007.00347.x
3. Gregory CO, Blanck HM, Gillespie C, et al. Health perceptions and demographic characteristics associated with underassessment of body weight. Obesity (Silver Spring). 2008;16(5):979-986. PubMed doi:10.1038/oby.2008.22
4. Jansen W, van de Looij-Jansen PM, Ferreira I, et al. Differences in measured and self-reported height and weight in Dutch adolescents. Ann Nutr Metab. 2006;50(4):339-346. PubMed doi:10.1159/000094297
5. White MA, Masheb RM, Burke-Martindale C, et al. Accuracy of self-reported weight among bariatric surgery candidates: the influence of race and weight cycling. Obesity (Silver Spring). 2007;15(11):2761-2768. PubMed doi:10.1038/oby.2007.328
6. Ziebland S, Thorogood M, Fuller A, et al. Desire for the body normal: body image and discrepancies between self reported and measured height and weight in a British population. J Epidemiol Community Health. 1996;50(1):105-106. PubMed doi:10.1136/jech.50.1.105
7. Doll HA, Fairburn CG. Heightened accuracy of self-reported weight in bulimia nervosa: a useful cognitive “distortion.” Int J Eat Disord. 1998;24(3):267-273. PubMed doi:10.1002/(SICI)1098-108X(199811)24:3<267::AID-EAT4>3.0.CO;2-K
8. Smith GT, Hohlstein LA, Atlas JG. Accuracy of self-reported weight: covariation with binger or restrainer status and eating disorder symptomatology. Addict Behav. 1992;17(1):1-8. PubMed doi:10.1016/0306-4603(92)90047-Y
9. Masheb RM, Grilo CM. Accuracy of self-reported weight in patients with binge eating disorder. Int J Eat Disord. 2001;29(1):29-36. PubMed doi:10.1002/1098-108X(200101)29:1<29::AID-EAT5>3.0.CO;2-E
10. Kuchler F, Variyam JN. Mistakes were made: misperception as a barrier to reducing overweight. Int J Obes Relat Metab Disord. 2003;27(7):856-861. PubMed doi:10.1038/sj.ijo.0802293
11. Rossouw K, Senekal M, Stander I. The accuracy of self-reported weight by overweight and obese women in an outpatient setting. Public Health Nutr. 2001;4(1):19-26. PubMed doi:10.1079/PHN200051
12. Atlantis E, Ball K. Association between weight perception and psychological distress. Int J Obes (Lond). 2008;32(4):715-721. PubMed doi:10.1038/sj.ijo.0803762
13. Meyer C, McPartlan L, Sines J, et al. Accuracy of self-reported weight and height: relationship with eating psychopathology among young women. Int J Eat Disord. 2009;42(4):379-381. PubMed doi:10.1002/eat.20618
14. Cummins LH, Dunn EC, Rabin L, et al. Primary care provider familiarity with binge eating disorder and implications for obesity management: a preliminary survey. J Clin Psychol Med Settings. 2003;10(1):51-56. doi:10.1023/A:1022857830793
15. Striegel-Moore RH, Dohm FA, Wilfley DE, et al. Toward an understanding of health services use in women with binge eating disorder. Obes Res. 2004;12(5):799-806. PubMed doi:10.1038/oby.2004.96
16. Crow SJ, Peterson CB, Levine AS, et al. A survey of binge eating and obesity treatment practices among primary care providers. Int J Eat Disord. 2004;35(3):348-353. PubMed doi:10.1002/eat.10266
17. Johnson JG, Spitzer RL, Williams JBW. Health problems, impairment and illnesses associated with bulimia nervosa and binge eating disorder among primary care and obstetric gynaecology patients. Psychol Med. 2001;31(8):1455-1466. PubMed doi:10.1017/S0033291701004640
18. Grilo CM, Lozano C, Masheb RM. Ethnicity and sampling bias in binge eating disorder: black women who seek treatment have different characteristics than those who do not. Int J Eat Disord. 2005;38(3):257-262. PubMed doi:10.1002/eat.20183
19. Wilfley DE, Pike KM, Dohm FA, et al. Bias in binge eating disorder: how representative are recruited clinic samples? J Consult Clin Psychol. 2001;69(3):383-388. PubMed doi:10.1037/0022-006X.69.3.383
20. Crow SJ, Stewart Agras W, Halmi K, et al. Full syndromal versus subthreshold anorexia nervosa, bulimia nervosa, and binge eating disorder: a multicenter study. Int J Eat Disord. 2002;32(3):309-318. PubMed doi:10.1002/eat.10088
21. Striegel-Moore RH, Dohm FA, Solomon EE, et al. Subthreshold binge eating disorder. Int J Eat Disord. 2000;27(3):270-278. PubMed doi:10.1002/(SICI)1098-108X(200004)27:3<270::AID-EAT3>3.0.CO;2-1
22. First MB, Spitzer RL, Gibbon M, et al. Structured Clinical Interview for DSM-IV Axis I Disorders, Patient Edition (SCID-I/P, Version 2.0). New York, NY: New York State Psychiatric Institute; 1996.
23. Fairburn CG, Cooper Z. The Eating Disorder Examination. In: Fairburn CG, Wilson GT, eds. Binge Eating: Nature, Assessment, and Treatment. 12th ed. New York, NY: Guilford Press; 1993:317-360.
24. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
25. Grilo CM, Lozano C, Elder KA. Inter-rater and test-retest reliability of the Spanish language version of the Eating Disorder Examination interview: clinical and research implications. J Psychiatr Pract. 2005;11(4):231-240. PubMed doi:10.1097/00131746-200507000-00003
26. Rizvi SL, Peterson CB, Crow SJ, et al. Test-retest reliability of the Eating Disorder Examination. Int J Eat Disord. 2000;28(3):311-316. PubMed doi:10.1002/1098-108X(200011)28:3<311::AID-EAT8>3.0.CO;2-K
27. Grilo CM, Masheb RM, Lozano-Blanco C, et al. Reliability of the Eating Disorder Examination in patients with binge eating disorder. Int J Eat Disord. 2004;35(1):80-85. PubMed doi:10.1002/eat.10238
28. Fairburn CG, Beglin SJ. Assessment of eating disorders: interview or self-report questionnaire? Int J Eat Disord. 1994;16(4):363-370. PubMed
29. Reas DL, Grilo CM, Masheb RM. Reliability of the Eating Disorder Examination-Questionnaire in patients with binge eating disorder. Behav Res Ther. 2006;44(1):43-51. PubMed doi:10.1016/j.brat.2005.01.004
30. Grilo CM, Masheb RM, Wilson GT. A comparison of different methods for assessing the features of eating disorders in patients with binge eating disorder. J Consult Clin Psychol. 2001;69(2):317-322. PubMed doi:10.1037/0022-006X.69.2.317
31. Grilo CM, Masheb RM, Wilson GT. Different methods for assessing the features of eating disorders in patients with binge eating disorder: a replication. Obes Res. 2001;9(7):418-422. PubMed doi:10.1038/oby.2001.55
32. Celio AA, Wilfley DE, Crow SJ, et al. A comparison of the Binge Eating Scale, Questionnaire for Eating and Weight Patterns-revised, and Eating Disorder Examination Questionnaire with instructions with the Eating Disorder Examination in the assessment of binge eating disorder and its symptoms. Int J Eat Disord. 2004;36(4):434-444. PubMed doi:10.1002/eat.20057
33. Goldfein J, Devlin M, Kamenetz C, et al. EDE-Q with and without instruction to assess binge eating in patients with binge eating disorder. Poster presented at the Annual Meeting of the Academy of Eating Disorders; Boston, MA; April 25-28, 2002.
34. Beck AT, Steer R. Manual for Revised Beck Depression Inventory. New York, NY: Psychological Corporation; 1987.
35. Beck AT, Steer R, Garbin MG. Psychometric properties of the Beck Depression Inventory: 25 years of evaluation. Clin Psychol Rev. 1988;8(1):77-100. doi:10.1016/0272-7358(88)90050-5
36. Grilo CM, Masheb RM, Wilson GT. Subtyping binge eating disorder. J Consult Clin Psychol. 2001;69(6):1066-1072. PubMed doi:10.1037/0022-006X.69.6.1066
37. DelPrete LR, Caldwell M, English C, et al. Self-reported and measured weights and heights of participants in community-based weight loss programs. J Am Diet Assoc. 1992;92(12):1483-1486. PubMed
38. Okosun IS, Bhatt DV, Boltri JM, et al. Self-reported and measured height and weight: impact on racial/ethnic differences in hypertension. Ethn Dis. 2008;18(4):415-420. PubMed
39. Kuczmarski MF, Kuczmarski RJ, Najjar M. Effects of age on validity of self-reported height, weight, and body mass index: findings from the Third National Health and Nutrition Examination Survey, 1988-1994. J Am Diet Assoc. 2001;101(1):28-34. PubMed doi:10.1016/S0002-8223(01)00008-6