Objective: The negative impact of weight gain is a common problem facing all patients, but it is especially concerning in the seriously mentally ill population. The literature is replete with interventions to mitigate weight gain in this population; however, most focus on outpatient settings. This study was undertaken to quantify weight gain in an inpatient setting and to assess whether instituted interventions to reduce weight gain were effective.
Methods: This retrospective study analyzed weight changes in adult psychiatric inpatients with length of stay of 30 days or more. Data regarding weight changes were collected from records before (July 2005 to June 2006) a hospital-wide policy change to combat weight gain and after (July 2013 to June 2014) the changes were instituted. A total of 537 charts were reviewed.
Results: Male inpatients gained a mean of 7.61 lb and females gained 6.02 lb. The mean weight change increased for the pre and post policy change periods: 6.08 lb and 7.85 lb, respectively, a 29% increase in mean weight.
Conclusion: This study demonstrates that weight in psychiatric inpatients hospitalized for 30 days or longer increased despite widespread changes in the hospital setting implemented to limit weight gain.
Weight Gain in Psychiatric Inpatients:
Are Interventions Making a Positive Impact?

ABSTRACT
Objective: The negative impact of weight gain is a common problem facing all patients, but it is especially concerning in the seriously mentally ill population. The literature is replete with interventions to mitigate weight gain in this population; however, most focus on outpatient settings. This study was undertaken to quantify weight gain in an inpatient setting and to assess whether instituted interventions to reduce weight gain were effective.
Methods: This retrospective study analyzed weight changes in adult psychiatric inpatients with length of stay of 30 days or more. Data regarding weight changes were collected from records before (July 2005 to June 2006) a hospital-wide policy change to combat weight gain and after (July 2013 to June 2014) the changes were instituted. A total of 537 charts were reviewed.
Results: Male inpatients gained a mean of 7.61 lb and females gained 6.02 lb. The mean weight change increased for the pre and post policy change periods: 6.08 lb and 7.85 lb, respectively, a 29% increase in mean weight.
Conclusion: This study demonstrates that weight in psychiatric inpatients hospitalized for 30 days or longer increased despite widespread changes in the hospital setting implemented to limit weight gain.
Prim Care Companion CNS Disord 2017;19(4):17m02111
https://doi.org/10.4088/PCC.17m02111
© Copyright 2017 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry District Medical Group, University of Arizona College of Medicine, Maricopa Integrated Health System Behavioral Health Annex, Phoenix, Arizona
*Corresponding author: Gwen A. Levitt, DO, MIHS-BHA-Unit 9, 2619 East Pierce St, Phoenix, AZ 85008 ([email protected]).
The population of seriously mentally ill (SMI) patients has a life span that is approximately 25 years shorter than the general population.1 Many SMI patients do not seek routine medical care and lack the ability or motivation to maintain a healthy lifestyle.2 These individuals are susceptible to metabolic syndromes as a sequelae of psychotropic medications. It is estimated that as many as 80% of SMI patients battle medication-induced weight gain.3 Use of psychotropic medications poses treatment dilemmas, given that patients typically require them to adequately address their psychiatric symptoms. It is problematic that these necessary medications may contribute to a patient’s risk of medical comorbidities, which impact the higher mortality rates seen in this population.
WEIGHT GAIN INTERVENTIONS
Various strategies are useful, both alone and in combination, to address weight gain for individuals taking psychotropic medications. These strategies include calorie-restricted diets, nutritional education and consultation, exercise, support groups, and the use of reminders and electronic applications. Meta-analyses4,5 indicate efficacy in utilizing preventative nonpharmacologic approaches such as patient education, exercise, and cognitive-behavioral interventions to mitigate weight gain. These interventions show short-term benefits when promoted and supervised. Antiobesity pharmacotherapy such as sibutramine and orlistat have shown some benefit for addressing weight gain as well.6-8 Changing or avoiding medications that promote weight gain can be an option for some patients.
The majority of studies focusing on controlling weight gain in SMI individuals are conducted on outpatients. Jacobowitz et al9 published results of a calorie-restricted diet among inpatients, concluding that this intervention was helpful only for those prescribed olanzapine, a second-generation antipsychotic. To date, few studies have been conducted on weight gain among inpatients, especially those with longer hospital stays.
OVERVIEW OF WEIGHT GAIN IN A PSYCHIATRIC POPULATION
It is well recognized in the literature that medications such as antipsychotics, mood stabilizers, and antidepressants can promote weight gain. Predictors of medication-induced weight gain include elevated premorbid body mass index (BMI), female sex, and younger age.10 Weight gain tends to occur during the acute phase of treatment.10 There is evidence11 to suggest that weight increases are dose-dependent with some antipsychotics. Specific diagnoses, such as depression and bipolar disorder, may be associated with being overweight, an independent factor from the weight gain caused by psychiatric medications.11

- Despite interventions to mitigate weight gain, mentally ill inpatients are still at high risk to rapidly gain weight, even in as little as 30 days.
- Clinicians must remain vigilant about monitoring weight gain in an inpatient setting and not assume that hospital interventions will suffice to alleviate the problem.
- Weight gain in inpatient settings is not consistent for all patients; age, sex, body mass index, length of stay, and repeated hospitalizations are only a few of the factors that may impact hospital-related weight changes.
Food intake is under the control of an outpatient. Many SMI patients have a limited income, which hampers their ability to purchase healthier, often more expensive, foods, and the indigent may not have regular access to meals. In contrast, inpatients are guaranteed well-balanced meals and snacks. Family members may bring in high-calorie "comfort" or fast food. (It is interesting to note that fast food restaurants are often located near hospitals.) Vending machines are commonplace in hospitals as well. Opportunities to exercise can be limited in the hospital setting. Outpatients have greater access to exercise options and activities.
STUDY BACKGROUND
In 2006, a large, urban, involuntary psychiatric hospital began a quality improvement project to assess weight gain in their population, and records of 65 inpatients were retrospectively reviewed. Twenty-seven patients (42%) showed a 5% or greater increase in weight during their admission. As a result of these findings, the hospital instituted a number of changes to combat weight gain that included changes to meal plans and snacks, eliminating access to vending machines, promotion of exercise, nutritional consults on all admissions, educational groups, and improving nursing protocols that related to meals and monitoring weight.
In 2014, a follow-up study on weight gain in the same population was performed by the dietitian. She reviewed 160 inpatient records. Forty patients (25%) gained weight from admission to the time of the dietitian’s chart review. The mean weight increase was 0.46 lb per day (based on a 14-day length of stay). This limited sampling indicated that the above-described interventions had not been effective. In fact, it suggested that patient weights were increasing more than before the 2006 changes.
The primary interest of the current study was to compare weight gain prior to and after the aforementioned institutional changes. The null hypothesis was that there would be no significant improvement in weight gain despite the interventions.
METHODS
The present study is a retrospective analysis of weight change for 2 groups of adult psychiatric inpatients before and after institutional changes related to mitigating weight gain in the facility.
The study included 2 inpatient facilities. Site 1 includes a medical-geriatric unit and an outdoor area for exercise (although access is limited in the summer), has a general population with more comorbid medical concerns, and serves all meals on premeasured trays. Site 2 has an indoor gymnasium and an outdoor patio, has a medically healthier population, and provides meals in a cafeteria-style setting. The study facilities are providing a diet of 1,800 calorie a day. (The US Department of Agriculture recommends 1,200 to 1,400 calories a day for sedentary adults.12) "Healthy" snacks are provided, which include saltines (25 calories), graham crackers (60 calories), peanut butter packages (165 calories), baked potato chips (120 calories), and juice cups (50-60 calories).
Sample
The sampling method included medical records for psychiatric inpatients over 2 time periods: July 2005 to June 2006 (prior to the implementation of the aforementioned changes or "pre") and July 2013 to June 2014 (after the changes were in place or "post"). Data were extracted from records for patients with a length of stay of 30 days or longer. The 30-day inclusion criterion was considered a suitable duration for the weight changes to be related to factors other than regular, biologic weight fluctuations. Patients were excluded who had a BMI < 17 or pregnancy, as weight gain would be promoted or expected; or a BMI > 40, since weight loss is recommended. Records that had missing measurements of weight or height were excluded. The final sample included 270 patient records from 2005 and 2006 and 267 records from 2013 and 2014.
Data
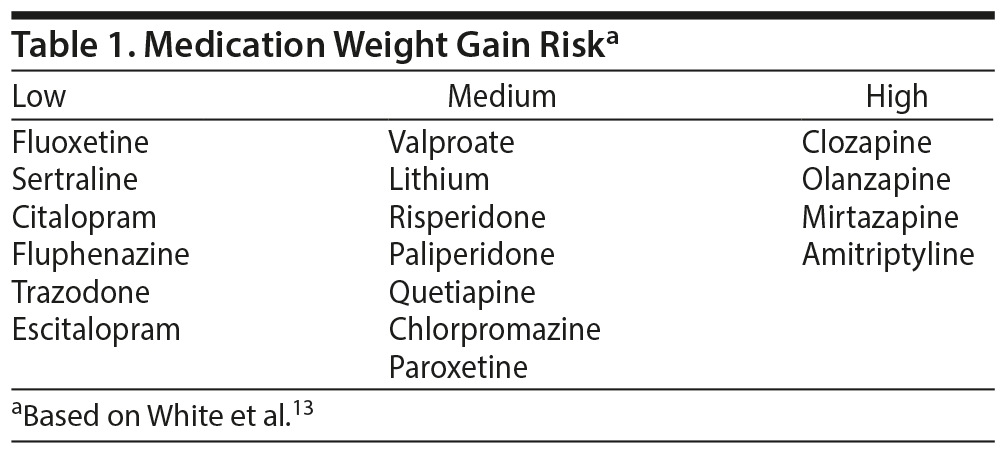
Weights and BMIs were collected at admission and then at the thirtieth day of stay (± 5 days). Other data collected included length of stay, sex, age, treatment site, and prescribed psychiatric medications. Some patients had repeated hospitalizations within the research time frame. In these cases, each admission was considered a separate subject. Patients who were hospitalized for longer durations allowed for the analysis of weight change over time. In these patients, weights were measured at 60 and 90 days of hospitalization (± 5 days). A subsample of 350 patient charts was reviewed for medications, which were categorized by the relative incidence of weight gain into low-, moderate-, and high-risk groups as described in the literature (Table 1).13
Analyses
All analyses were performed using SPSS 21 with α of .05 corrected for multiple comparisons. After obtaining the final sample, outliers were compared against original records to verify and correct errors. A random sample of remaining data was examined to ensure accuracy of the extracted dataset. Frequency counts and percentages were calculated for all discrete data; continuous data were examined for central tendencies. Repeat hospitalizations, older age, and medication type were examined descriptively to fully assess the nature of the sample. Univariate analyses were conducted on those with longer hospitalization stays and by sex. A multivariate analysis was used to test the primary hypothesis, while also examining the effects of obesity status and inpatient site.
RESULTS
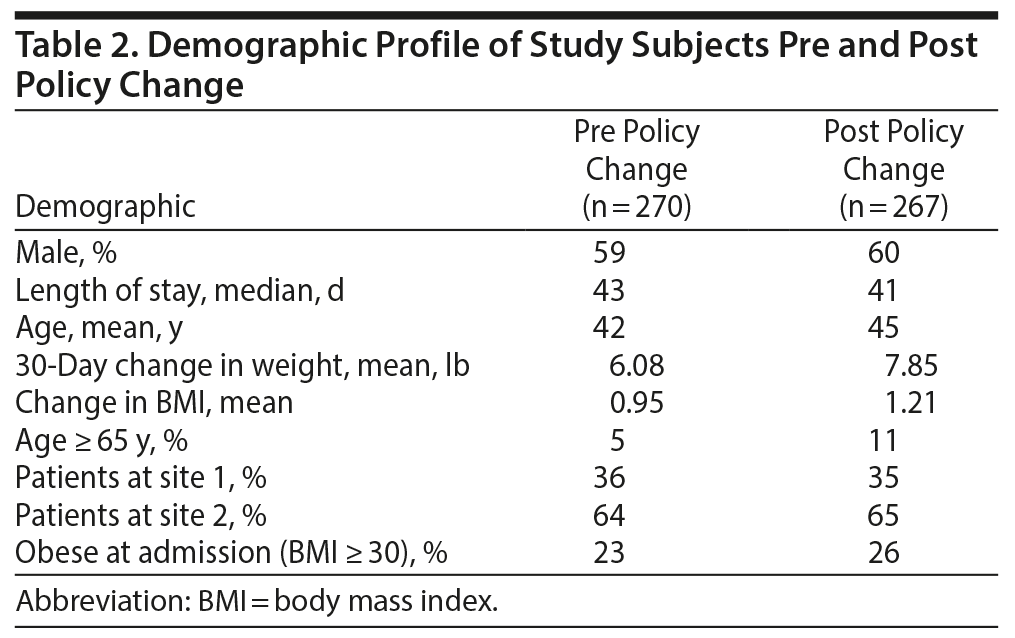
A total of 537 charts were reviewed. The mean age of the patients was 43 years. Patients aged 65 years and older comprised 8% of the total sample. The median length of stay for all subjects was 42 days. Patients with valid weight measurements for hospitalizations over 90 days comprised 8% of the total sample. Eight percent had another hospitalization. The patient sex distribution was 59% male and 41% female. The proportions for sex and treatment site were similar between the pre and post time periods. The mean weight change during hospitalization increased for the pre and post periods: 6.08 lb and 7.85 lb, respectively. This change represents a 29% increase in mean weight from pre to post time periods. BMI similarly increased between the time periods from 0.95 to 1.21 (Table 2).
Older Patients
Weight gain in older inpatients (defined as age ≥ 65 years) showed a different pattern than what was seen in younger individuals. Younger patients gained a mean of 3 lb more than patients aged 65 and older. In the older patients, those who were not obese gained a mean of 5.51 lb over 30 days, while those who were obese at admission lost a mean of 2 lb. In addition, older patients stayed a mean of 10 days longer than younger patients.
Repeat Admission
Forty-four patients had more than 1 admission during the time frames reviewed. Fourteen had weight changes ± 4 lb and were removed from the dataset, as this change could be accounted for by natural monthly weight fluctuations. Of the remaining patients, 15 (50%) had sustained their weight gain from the first admission to the second with a range of 5 to 35 lb, a mean increase of 12.6 lb. Of those who lost weight, the range was from 6 to 35 lb, a mean loss of 14.5 lb.
Prescribed Medication
Thirty-four percent of patients were on high-risk medications (see Table 1). Forty-two percent of the subjects were prescribed risperidone as their sole medication. These patients gained a mean of 7 lb. Valproic acid as monotherapy was prescribed in 13% of the subjects, and these patients had a weight increase of 6.3 lb on average. Thirty-two percent of the sample was prescribed both risperidone and valproic acid, which was the most common medication combination identified in the study, and gained a mean of 7.6 lb. Patients taking clozapine gained an mean of 3 lb. Older patients were less likely than younger patients to be prescribed high-risk medications (74% vs 59%) and more likely to be prescribed risperidone monotherapy (56% vs 40%).
Univariate Analyses
Sex. Males gained a mean of 7.61 lb (SD = 9.96 lb) and females gained 6.02 lb (SD = 8.07 lb) (t521.07 = 2.03, P = .04) in 30 days.
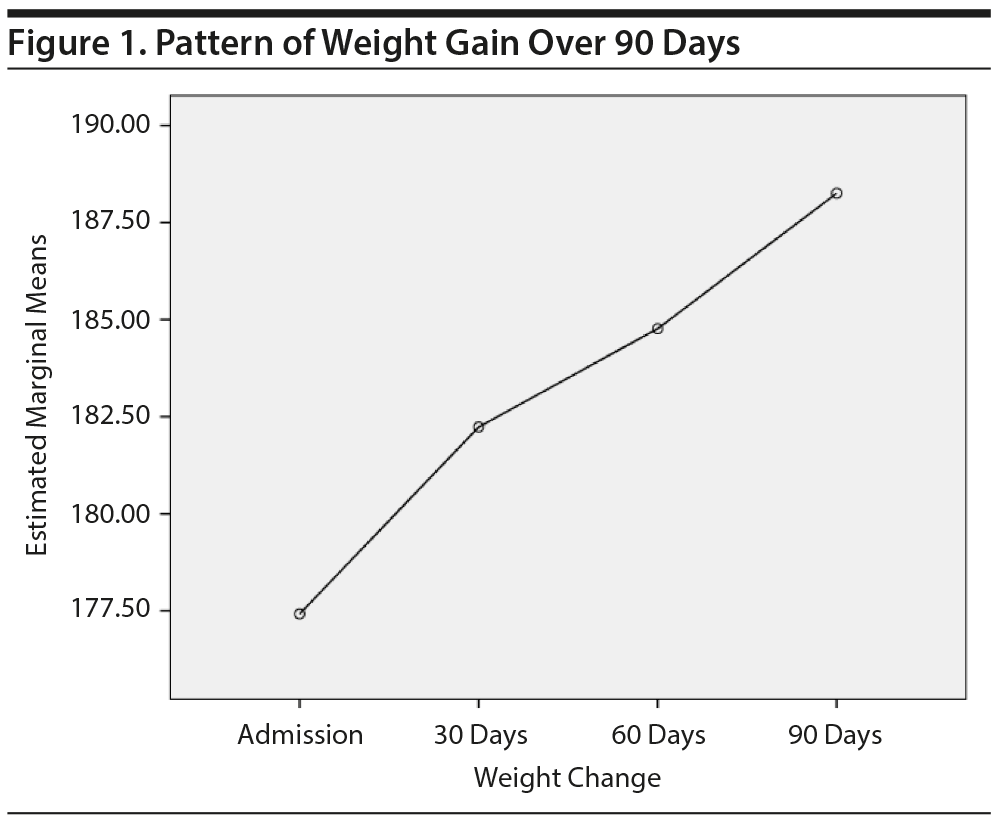
Longer inpatient stays. In the 43 patients who were hospitalized up to 90 days, a repeated-measures analysis of variance (ANOVA) was used to determine if mean weight gain continued to increase over time (Figure 1). Mean weight continued to increase throughout the hospitalization in the following pattern: admission weight (mean = 177.42, SE = 5.46 lb), 30 days (mean = 182.23, SE = 5.38 lb), 60 days (mean = 184.77, SE = 5.32 lb), and 90 days (mean = 188.26, SE = 5.30 lb). The effect of time was significant (F1.63, 68.43 = 14.63, P < .01), with the greatest increase occurring within 30 days.
Multivariate Analysis
A fixed-effect, 3-way factorial ANOVA model was used to test the differences in mean weight gain by site, obesity status, and across pre and post periods. The total sample size for the analysis was 494 subjects, excluding older subjects. The ANOVA yielded no main effect for time (F1,490 = 3.25, not significant); the mean change in weight was not significantly higher post changes (mean = 6.24, SE = 0.63 lb) than in the prechange period (mean = 4.80, SE = 0.62 lb). There was a significant difference in weight gain by hospital site (F1, 490 = 26.60, P < .01). Patients at site 2 gained significantly more weight (mean = 7.72, SE = 0.53 lb) than did patients at site 1 (mean = 3.32, SE = 0.74 lb). There was a significant difference in weight gain by obesity status (F1,490 = 15.04, P < .01). Patients who were not obese at admission, both pre and post changes, gained significantly more weight (mean = 7.30, SE = 0.49 lb) than did patients who were already obese (BMI between 30 and 40) (mean = 3.74, SE = 0.81 lb).
DISCUSSION
This study demonstrated that weight in psychiatric inpatients hospitalized for 30 days or longer increased despite widespread changes implemented to limit weight gain. There was no statistically relevant difference in the mean amount of weight gained in the pre and post policy change groups. Half of the patients who had readmissions during the time frame studied sustained their weight gain. Because weight gain was not impacted, this study suggests that the interventions used by the hospital to address the problem were ineffective.
Several areas were identified as possibly contributing to the weight increases seen in the study. Behavioral health technicians may have limited knowledge of healthy eating and portion control and were the primary providers of meals and snacks. They inadvertently promoted weight gain by, for example, giving patients several snack items during snack times (3 times a day). Staff often "bent the rules" about snacks, using them as a behavioral modification or distraction tool. Juice cups were given throughout the day when requested, rather than water, which was available at all times. Few patients attended the dietary class or were invested in exercising. Staff did not actively encourage exercise or engage patients in attending recreational activities. In reviewing the patient problem lists at admission and discharge, providers did not appear to recognize a patient’s weight issue because "overweight or obesity" was not listed as a hospital problem.
The difference in weight gained at each site was a curious finding. Site 2 had improved access to exercising and a generally healthier population than site 1. These factors would suggest that weight gain would be less problematic. Site 2 served cafeteria-style meals, whereas site 1 had premeasured trays. Researchers suspect that cafeteria-style meals impacted the weight gain most significantly, because although cafeteria staff limit portions by using a scoop, food portions vary from one staff member to another, and patients were allowed 1 serving of each item but often took as many items as are available.
It is estimated that 80% of the SMI population are overweight or obese.2 One study14 documented an average weight increase of 5.41 lb in a population of patients admitted into a public hospital setting. This weight increase is less than the amount gained in this study. Overall, weight gain may be expected, given the well-recognized increases in population obesity in the United States over time. According to the Centers for Disease Control study,15 the BMI of average Americans from 1960 to 2002 rose 3 units (which equates to an average of approximately 24 lb). Population-based increases, however, do not account for the rapid weight increases found in the current study population who had normal weight and BMI, nor would this finding account for the differences in weight gain seen between hospital sites.
Unlike previously described statistics in the literature,18 this study showed that male patients gained more weight than female patients. Patients on clozapine gained half the weight of those on other antipsychotics despite clozapine being one of the medications known to cause the most weight gain. It is possible the patients on clozapine have a greater level of psychiatric impairment, extensive treatment history, or longer overall duration of antipsychotic use, which may impact their weight differently than those who are prescribed other medications in this study. However, it is unclear why the data from this study vary from commonly known statistics in regard to these 2 areas.
Even with extensive interventions, as was undertaken at the study facility, the amount of weight gained by inpatients is very concerning. Some patients not only maintain the weight gained between admissions, but also are at risk for subsequent weight gain at future admissions. The Harvard Medical School Special Report16 concluded that just 22 lb of excess weight can increase systolic and diastolic blood pressure, cardiac disease, and stroke risk and decrease life span. Excess weight gain is linked to a higher risk of cancer and cancer-related deaths. There is a lack of literature that addresses the health risks specific to rapid weight gain.
Several limitations should be noted. Complete accuracy of weight-related data could not be assured for various reasons. As these variations were system-wide, they were expected to affect all data similarly. Visitors were allowed to bring in food and snacks for patients, so patients do obtain extra food. These factors affected patients at both sites equally as well.
This study did not evaluate the duration, combinations, or doses of medications used. The majority of patients were prescribed multiple medications during their stay, making the comparison of isolated effects impossible. There was no statistical difference found in the types of medications and combinations prescribed pre or post policy change, between sites, or in the patient population in general. Second-generation antipsychotics, used to treat psychotic symptoms, such as risperidone, olanzapine, and quetiapine can cause about a 7% increase in weight from baseline.17 Clozapine, another antipsychotic, has the most significant impact, with up to a 20% increase in patients’ pretreatment weight.18 Valproic acid, a mood stabilizer used to treat conditions such as bipolar disorder, is estimated to cause between 3 kg to 20 kg of weight gain.18 Lithium, another mood stabilizer, has been estimated to increase weight by between 4.5 to 12 kg.19 Patients prescribed mirtazapine, an antidepressant, gained 1.74 kg to 2.59 kg in weight.19 The mechanisms of action that cause weight gain are related to receptor activity in the brain, and this varies with each medication. We cannot conclude whether the weight gain seen in the research population was solely or in part due to medication or failure of the aforementioned interventions.
It is difficult to change people’s eating habits under the best of circumstances. Only so much can be done to limit calorie intake in the hospital without compromising the strived-for therapeutic environment of an inpatient setting. Friction already exists in a hospital setting, especially an involuntary one, for patient autonomy, and the battle over what one can eat is a day-to-day issue. This study demonstrates that more needs to be done to address weight gain in an inpatient setting. Further research on ways to combat weight gain must be undertaken to address this problem.
Submitted: February 8, 2017; accepted May 10, 2017.
Published online: July 13, 2017.
Potential conflicts of interest: None.
Funding/support: None
Acknowledgment: The research team thanks Fay Pezely, RD, clinical nutrition manager at Maricopa Integrated Health System, Phoenix, Arizona, for her invaluable insights and information about nutrition and the hospital’s dietary policy and reviews of patient data. Ms Pezely has no conflicts of interest to declare.
REFERENCES
1. National Alliance on Mental Illness website. http://www.nami.org/Learn-More/Mental-Health-By-the-Numbers. Accessed January 11, 2017.
2. Daumit GL, Dickerson FB, Wang NY, et al. A behavioral weight-loss intervention in persons with serious mental illness. N Engl J Med. 2013;368(17):1594-1602. PubMed doi:10.1056/NEJMoa1214530
3. Alvarez-Jiménez M, Hetrick SE, Gonzסlez-Blanch C, et al. Non-pharmacological management of antipsychotic-induced weight gain: systematic review and meta-analysis of randomised controlled trials. Br J Psychiatry. 2008;193(2):101-107. PubMed doi:10.1192/bjp.bp.107.042853
4. Shrivastava A, Johnston ME. Weight-gain in psychiatric treatment: risks, implications, and strategies for prevention and management. Mens Sana Monogr. 2010;8(1):53-68. PubMed doi:10.4103/0973-1229.58819
5. Bonfioli E, Berti L, Goss C, et al. Health promotion lifestyle interventions for weight management in psychosis: a systematic review and meta-analysis of randomised controlled trials. BMC Psychiatry. 2012;12:78. PubMed doi:10.1186/1471-244X-12-78
6. Apfelbaum M, Vague P, Ziegler O, et al. Long-term maintenance of weight loss after a very-low-calorie diet: a randomized blinded trial of the efficacy and tolerability of sibutramine. Am J Med. 1999;106(2):179-184. PubMed doi:10.1016/S0002-9343(98)00411-2
7. Finer N, James WP, Kopelman PG, et al. One-year treatment of obesity: a randomized, double-blind, placebo-controlled, multicentre study of orlistat, a gastrointestinal lipase inhibitor. Int J Obes Relat Metab Disord. 2000;24(3):306-313. PubMed doi:10.1038/sj.ijo.0801128
8. Faulkner G, Soundy AA, Lloyd K. Schizophrenia and weight management: a systematic review of interventions to control weight. Acta Psychiatr Scand. 2003;108(5):324-332. PubMed doi:10.1034/j.1600-0447.2003.00218.x
9. Jacobowitz W, Derbabian B, Saunders A. The effect of a calorie-restricted diet on weight gain in short-term psychiatric inpatients receiving atypical antipsychotic medications. J Psychosoc Nurs Ment Health Serv. 2014;52(7):30-37. PubMed doi:10.3928/02793695-20140421-01
10. Simon V, van Winkel R, De Hert M. Are weight gain and metabolic side effects of atypical antipsychotics dose dependent? a literature review. J Clin Psychiatry. 2009;70(7):1041-1050. PubMed doi:10.4088/JCP.08r04392
11. Fagiolini A, Frank E, Houck PR, et al. Prevalence of obesity and weight change during treatment in patients with bipolar I disorder. J Clin Psychiatry. 2002;63(6):528-533. PubMed doi:10.4088/JCP.v63n0611
12. Dietary Guidelines for Americans. 2010. Office of Disease Prevention and Health Promotion website. http://www.dietaryguidelines.gov. Accessed December 9, 2016.
13. White W, Elmore L, Luthin DR, et al. Psychotropic induced weight gain: a review of management strategies. Consultant. 2013;53(3):153-160.
14. Shin JK, Barron CT, Chiu YL, et al. Weight changes and characteristics of patients associated with weight gain during inpatient psychiatric treatment. Issues Ment Health Nurs. 2012;33(8):505-512. PubMed doi:10.3109/01612840.2012.683931
15. Four-Decade Study: Americans Taller, Fatter. http://www.livescience.com/49-decade-study-americans-taller-fatter.html. Accessed on April 5, 2017.
16. Alonso-Alonso M, McManus K. Healthy solutions to lose weight and keep it off. Harvard Medical School Health Publication series, Harvard Medical School Special Health Report, Harvard Health Publications website. http://www.Health.harvard.edu/special-health-reports/lose-weight-and-keep-it-off. Accessed January 2017.
17. Lieberman JA, Stroup TS, McEvoy JP, et al; Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) Investigators. Effectiveness of antipsychotic drugs in patients with chronic schizophrenia. N Engl J Med. 2005;353(12):1209-1223. PubMed doi:10.1056/NEJMoa051688
18. Umbricht DS, Pollack S, Kane JM. Clozapine and weight gain. J Clin Psychiatry. 1994;55(suppl B):157-160. PubMed
19. Torrent C, Amann B, Sסnchez-Moreno J, et al. Weight gain in bipolar disorder: pharmacological treatment as a contributing factor. Acta Psychiatr Scand. 2008;118(1):4-18. PubMed doi:10.1111/j.1600-0447.2008.01204.x