Prim Care Companion CNS Disord 2022;24(1):21cr02932
To cite: Shad MU. Acute aggression after progesterone discontinuation in a young woman. Prim Care Companion CNS Disord. 2022;24(1):21cr02932.
To share: https://doi.org/10.4088/PCC.21cr02932
© Copyright 2022 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, University of Nevada, Las Vegas, Nevada
bDepartment of Psychiatry, Touro University Nevada College of Osteopathic Medicine, Las Vegas, Nevada
cDepartment of Psychiatry, Valley Health Services, Las Vegas, Nevada
*Corresponding author: Mujeeb U. Shad, MD, MSCS, Valley Health System, Spring Mountain Hospital and Medical Center, 5400 South Rainbow Blvd, Las Vegas, NV 89118 ([email protected]).
The psychiatric effects of progesterone and its primary metabolite allopregnanolone are well-documented in anxiety,1 premenstrual syndrome, dysmenorrhea,2 and postpartum depression.3,4 However, the clinical evidence for progesterone’s role in behavioral aggression is scarce. This report describes the first case of acute aggression in a young woman after the discontinuation of a subdermal etonogestrel implant and resolution of aggression after the initiation of depot medroxyprogesterone acetate (DMPA).
Case Report
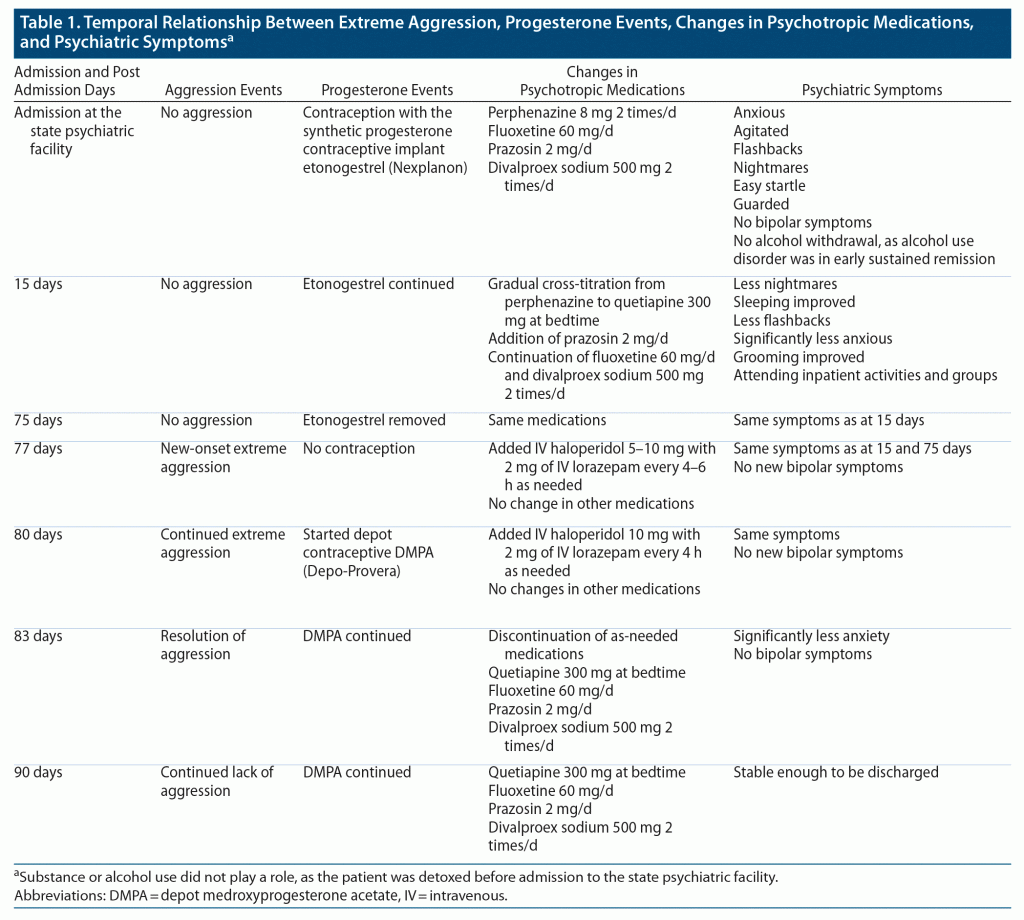
The patient, a 23-year old black woman with severe posttraumatic stress disorder (PTSD), unspecified bipolar disorder, and a history of alcohol use disorder, was admitted to a psychiatric facility to manage extreme agitation and suicidal thoughts precipitated by excessive alcohol intake. Medications at admission included fluoxetine 60 mg/d, prazosin 2 mg/d, perphenazine 8 mg 2 times/d, and divalproex sodium 500 mg 2 times/d with therapeutic levels (ie, 91 mcg/mL). Since the patient developed significant extrapyramidal symptoms and hyperprolactinemia, she was gradually cross-titrated from perphenazine to quetiapine 300 mg at bedtime with resolution of both adverse effects as well as symptom stabilization. However, a couple of weeks before the patient’s discharge, the progesterone contraceptive implant, etonogestrel (Nexplanon), was secretly removed by the patient so that she could become pregnant despite cautions against teratogenic effects of divalproex sodium. Within 2 days, the patient became extremely aggressive toward staff and peers for 3 days despite the frequent use of as-needed antipsychotics and sedatives (Table 1). But, the patient did not exhibit pressured speech, increase in goal-directed activity, grandiosity, decreased sleep, or flight of ideas. After discovering the implant removal, the patient was started on DMPA (Depo-Provera) to prevent future nonadherence. She stabilized within 3 days and was discharged from the state psychiatric facility a week later after a 3-month hospitalization (Table 1).
Discussion
This is the first case, to my knowledge, of acute aggression after 2 days of discontinuing an etonogestrel implant followed by aggression resolution within 3 days of starting DMPA. This onset of action is consistent with the time DMPA requires for its peripheral effects5 (Table 1). Since progesterone can easily cross the blood-brain barrier, the appearance of peripheral effects in 2 days may coincide with the central effects. The half-life of etonogestrel is 25 hours,6 which means that the etonogestrel levels may decline more than 50% in 2 days, further explaining peripheral changes within 2 days of progesterone discontinuation.5 Of note, the implant’s removal did not result in menstruation, which rules out behavioral dysregulation due to hormonal changes other than progesterone.7,8
Although the mechanisms underlying aggression are not clear, progesterone’s discontinuation may have resulted in behavioral dysregulation due to loss of positive allosteric modulation of inhibitory γ-aminobutyric acid-A (GABA-A) receptors, which has been reported with progesterone’s primary metabolite, allopregnanolone.3,4 An increase in GABA activity dampens the glutamate excitotoxicity associated with behavioral aggression,9 postpartum depression,10,11 and psychosis.12 Despite underlying bipolarity, therapeutic levels of divalproex sodium did not prevent the sudden onset of behavioral aggression in this patient, suggesting that allosteric modulation may differ from valproic acid’s direct GABAergic effects. Thus, it is plausible that loss of potential mood stabilization with the contraceptive13,14 may have precipitated aggression in this patient. A decrease in progesterone levels has also been associated with posttraumatic symptomatology and heightened intensity, as well as the duration of adrenergic response,15 which may be relevant in this patient diagnosed with PTSD. Also, individuals with low plasma GABA levels are prone to develop PTSD after a traumatic experience.16 Unfortunately, the progesterone level was not measured to support the findings in this case, which also could have helped to rule out any drug interactions. Etonogestrel is metabolized by the cytochrome P450 (CYP) enzyme system,17 which does not metabolize any of the psychotropic medications prescribed to this patient except quetiapine.18 However, it is counterintuitive to think that a potential increase in etonogestrel levels due to competitive inhibition by quetiapine contributed to behavioral dysregulation in this patient. A similar argument can be made with high-dose use of fluoxetine (ie, 60 mg/d) that can also inhibit CYP3A419 and may increase etonogestrel levels. In addition, during a 3-month hospitalization, sobriety makes alcohol a less likely contributor to aggression in this patient. Although the findings from this report are based on a single case and should be interpreted cautiously, clinicians should consider progesterone’s psychiatric effects beyond contraception, especially in patients with complex psychiatric comorbidities.
Published online: January 27, 2022.
Potential conflicts of interest: None.
Funding/support: None.
Patient consent: Verbal consent was received from the patient to publish this case report, and information has been de-identified to protect anonymity.
References (19)

- Reynolds TA, Makhanova A, Marcinkowska UM, et al. Progesterone and women’s anxiety across the menstrual cycle. Horm Behav. 2018;102:34–40. PubMed CrossRef
- Glick ID, Bennett SE. Psychiatric complications of progesterone and oral contraceptives. J Clin Psychopharmacol. 1981;1(6):350–367. PubMed CrossRef
- Kanes SJ, Colquhoun H, Doherty J, et al. Open-label, proof-of-concept study of brexanolone in the treatment of severe postpartum depression. Hum Psychopharmacol. 2017;32(2):e2576. PubMed CrossRef
- Meltzer-Brody S, Colquhoun H, Riesenberg R, et al. Brexanolone injection in post-partum depression: two multicentre, double-blind, randomised, placebo-controlled, phase 3 trials. Lancet. 2018;392(10152):1058–1070. PubMed CrossRef
- Petta CA, Faúndes A, Dunson TR, et al. Timing of onset of contraceptive effectiveness in Depo-Provera users. II. effects on ovarian function. Fertil Steril. 1998;70(5):817–820. PubMed CrossRef
- Wenzl R, van Beek A, Schnabel P, et al. Pharmacokinetics of etonogestrel released from the contraceptive implant Implanon. Contraception. 1998;58(5):283–288. PubMed CrossRef
- Brambilla F, Speca A, Pacchiarotti I, et al. Hormonal background of physiological aggressiveness in psychologically healthy women. Int J Psychophysiol. 2010;75(3):291–294. PubMed CrossRef
- Ziomkiewicz A, Pawlowski B, Ellison PT, et al. Higher luteal progesterone is associated with low levels of premenstrual aggressive behavior and fatigue. Biol Psychol. 2012;91(3):376–382. PubMed CrossRef
- Craig MC, Mulder LM, Zwiers MP, et al. Distinct associations between fronto-striatal glutamate concentrations and callous-unemotional traits and proactive aggression in disruptive behavior. Cortex. 2019;121:135–146. PubMed CrossRef
- Gerhard DM, Pothula S, Liu RJ, et al. GABA interneurons are the cellular trigger for ketamine’s rapid antidepressant actions. J Clin Invest. 2020;130(3):1336–1349. PubMed CrossRef
- Li YF. A hypothesis of monoamine (5-HT) - Glutamate/GABA long neural circuit: aiming for fast-onset antidepressant discovery. Pharmacol Ther. 2020;208:107494. PubMed CrossRef
- Lieberman JA, Girgis RR, Brucato G, et al. Hippocampal dysfunction in the pathophysiology of schizophrenia: a selective review and hypothesis for early detection and intervention. Mol Psychiatry. 2018;23(8):1764–1772. PubMed CrossRef
- Belelli D, Bolger MB, Gee KW. Anticonvulsant profile of the progesterone metabolite 5 alpha-pregnan-3 alpha-ol-20-one. Eur J Pharmacol. 1989;166(2):325–329. PubMed CrossRef
- Brown ES, Park J, Marx CE, et al. A randomized, double-blind, placebo-controlled trial of pregnenolone for bipolar depression. Neuropsychopharmacology. 2014;39(12):2867–2873. PubMed CrossRef
- Garcia NM, Walker RS, Zoellner LA. Estrogen, progesterone, and the menstrual cycle: a systematic review of fear learning, intrusive memories, and PTSD. Clin Psychol Rev. 2018;66:80–96. PubMed CrossRef
- Vaiva G, Thomas P, Ducrocq F, et al. Low posttrauma GABA plasma levels as a predictive factor in the development of acute posttraumatic stress disorder. Biol Psychiatry. 2004;55(3):250–254. PubMed CrossRef
- Sunaga T, Cicali B, Schmidt S, et al. Comparison of contraceptive failures associated with CYP3A4-inducing drug-drug interactions by route of hormonal contraceptive in an adverse event reporting system. Contraception. 2021;103(4):222–224. PubMed CrossRef
- Bakken GV, Rudberg I, Christensen H, et al. Metabolism of quetiapine by CYP3A4 and CYP3A5 in presence or absence of cytochrome B5. Drug Metab Dispos. 2009;37(2):254–258. PubMed CrossRef
- Lutz JD, VandenBrink BM, Babu KN, et al. Stereoselective inhibition of CYP2C19 and CYP3A4 by fluoxetine and its metabolite: implications for risk assessment of multiple time-dependent inhibitor systems. Drug Metab Dispos. 2013;41(12):2056–2065. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!