Objective: Many forms of synthetic marijuana are available in the United States for recreational use. Although the composition of these synthetic forms is unclear, consumption has been on the rise among adolescents. The objective of this study is to understand the usage rates and identify the reasons and risk factors for synthetic cannabinoid use.
Methods: We recruited 637 adolescents (aged 13 to 17 years) admitted to the Children’s Recovery Center, Norman, Oklahoma, from August 11, 2014, to March 30, 2016, for the study. Descriptive statistics and Pearson χ2 test were used to analyze the data. Logistic regression and adjusted odds ratio (OR) were performed to determine the risk factors for synthetic marijuana use.
Results: The mean age of synthetic cannabinoid users was 16 years. Increased prevalence of synthetic marijuana use was observed in 16- to 17-year-old adolescent males, in the white population, and in individuals living in urban areas. Synthetic marijuana was preferred by subjects over the regular form, as it is less expensive, produces a better high, is undetectable on drug tests, and is perceived as legal. Male sex (OR = 2.63, P < .0001), aged 16 to 17 years (OR = 1.99, P < .0001), and residing in an urban locality (OR = 1.57, P = .05) were identified as risk factors for consuming synthetic marijuana. Adolescents who use synthetic marijuana are more at risk of having substance use disorder (OR = 11.87, P < .0001) than those who do not.
Conclusions: Synthetic marijuana use is increasing in the adolescent age group and could potentially have a negative impact on the health of teenagers. Hence, enforcing strict laws against synthetic marijuana use and promoting awareness programs targeting adolescents would be beneficial.’ ‹
CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer the questions in the Posttest, and complete the Evaluation.
CME Objective
After studying this article, you should be able to:
• Educate adolescent patients about the risks associated with use of synthetic cannabinoids
Accreditation Statement
The CME Institute of Physicians
Postgraduate Press, Inc., is
accredited by the Accreditation
Council for Continuing Medical
Education to provide continuing
medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1.0 AMA PRA Category 1 Credit™. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Academy of Physician Assistants (AAPA) accepts certificates of participation for educational activities certified for AMA PRA Category 1 Credit™ from organizations accredited by ACCME or a recognized state medical society. Physician assistants may receive a maximum of 1.0 hour of Category I credit for completing this program.
Release, Expiration, and Review Dates
This educational activity was published in September 2018 and is eligible for AMA PRA Category 1 Credit™ through October 31, 2020. The latest review of this material was August 2018.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Larry Culpepper, MD, MPH, Editor in Chief, has been a consultant for Alkermes, Jazz, Lundbeck, Merck, and Sunovion; has been a stock shareholder of M-3 Information; and has received royalties from UpToDate and Oxford University Press. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
Rates of Synthetic Cannabinoid Use in Adolescents Admitted to
a Treatment Facility
ABSTRACT
Objective: Many forms of synthetic marijuana are available in the United States for recreational use. Although the composition of these synthetic forms is unclear, consumption has been on the rise among adolescents. The objective of this study is to understand the usage rates and identify the reasons and risk factors for synthetic cannabinoid use.
Methods: We recruited 637 adolescents (aged 13 to 17 years) admitted to the Children’s Recovery Center, Norman, Oklahoma, from August 11, 2014, to March 30, 2016, for the study. Descriptive statistics and Pearson χ2 test were used to analyze the data. Logistic regression and adjusted odds ratio (OR) were performed to determine the risk factors for synthetic marijuana use.
Results: The mean age of synthetic cannabinoid users was 16 years. Increased prevalence of synthetic marijuana use was observed in 16- to 17-year-old adolescent males, in the white population, and in individuals living in urban areas. Synthetic marijuana was preferred by subjects over the regular form, as it is less expensive, produces a better high, is undetectable on drug tests, and is perceived as legal. Male sex (OR = 2.63, P < .0001), aged 16 to 17 years (OR = 1.99, P < .0001), and residing in an urban locality (OR = 1.57, P = .05) were identified as risk factors for consuming synthetic marijuana. Adolescents who use synthetic marijuana are more at risk of having substance use disorder (OR = 11.87, P < .0001) than those who do not.
Conclusions: Synthetic marijuana use is increasing in the adolescent age group and could potentially have a negative impact on the health of teenagers. Hence, enforcing strict laws against synthetic marijuana use and promoting awareness programs targeting adolescents would be beneficial.
Prim Care Companion CNS Disord 2018;20(5):17m02265
To cite: Martz G, Tankersley W, Mekala HM, et al. Rates of synthetic cannabinoid use in adolescents admitted to a treatment facility. Prim Care Companion CNS Disord. 2018;20(5):17m02265.
To share: https://doi.org/10.4088/PCC.17m02265
© Copyright 2018 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Griffin Memorial Hospital, Norman, Oklahoma
bDepartment of Psychiatry, Child and Adolescent Psychiatry, University of Oklahoma, Tulsa, Oklahoma
*Corresponding author: Hema Madhuri Mekala, MD, Department of Psychiatry, Griffin Memorial Hospital, 900 E Main St, Norman, OK 73071 ([email protected]).
Illicit drug abuse has become a significant public health concern worldwide.1 Marijuana is now the most abused substance after alcohol and tobacco.2 Since 2009, there has been an increased availability of synthetic cannabinoids in the United States.3 Although synthetic marijuana is considered to be an analog of conventional marijuana, it is man-made and contains a mixture of unknown chemicals.4 These synthetic cannabinoid products are often marketed as designer drugs or herbal preparations.5,6 As of 2016, more than 170 types of synthetic marijuana products were manufactured in the United States.7 They are available under various brand names such as AK-47, Black Magic, Chill Out, Crazy Monkey, Diablo, Get Real, K2, Kush, Mr Happy, Mr Nice Guy, Scooby Snax, and Spice.8–11 The US Drug Enforcement Administration categorized synthetic marijuana under Schedule 1, as it has no indications for medical use and has a high abuse potential and safety concerns.12 Young individuals are at an increased risk for using synthetic cannabinoid products, as they are relatively inexpensive, easily available, known to produce higher subjective effects, and difficult to detect on drug tests.13–16
When compared to the conventional forms, synthetic marijuana is known to be more potent and cause many life-threatening complications.17 This potent effect is attributed to its action on several different receptors like serotonin and N-methyl-d-aspartate and interaction with other neurotransmitters like γ-aminobutyric acid, opioids, and monoamines, along with cannabinoid receptors CB1 and CB2.18 Reported side effects due to synthetic marijuana use are conjunctival injection, tachycardia, slurred sleep, delirium, hallucinations, psychosis, and seizures.7,14,19,20 Intoxication from synthetic cannabinoid use can cause renal failure, myocardial ischemia, pneumothorax, and stroke.13,21 Chronic marijuana use could lead to addiction, cognitive impairment, and withdrawal symptoms.22,23
It can be difficult to predict the diverse adverse effects of synthetic marijuana, as they depend on dosage, route of intake, combination with other illicit substances, and individual vulnerability to drugs.24 Also, screening for synthetic marijuana use can be a challenge, as the manufacturers alter the composition of these products by combining them with various herbal preparations and other supplements like vitamin E, fatty acids, aminoalkylindoles, and preservatives.25 Although specific tests such as gas chromatography and mass spectrometry of blood and urine samples are available, it might take several days to weeks to receive the results. All of these factors further complicate the early detection of drug intoxication and treatment.26 The increasing number of people using synthetic cannabinoid products and the availability of new formulations of these drugs on the market might pose a serious threat to public health.27
Though many studies1,10,13,14 have reported the side effects and negative impact that synthetic marijuana could have on the adolescent age group, there is a limited literature explaining why teenagers prefer to use these products. The objective of our study is to understand the usage rates and identify the reasons and risk factors for synthetic cannabinoid use.
METHODS
Setting and Participants
A total of 654 adolescents were eligible for the study. Of them, 637 participants aged 13 to 17 years admitted to the Children’s Recovery Center (CRC), Norman, Oklahoma, from August 11, 2014, to March 30, 2016, were included in the study. The CRC is a 55-bed, inpatient, state adolescent mental health and substance abuse treatment facility. Following admission to CRC, patients are sent initially to crisis services for 5 to 7 days. If further care is required, they are transferred to residential services for mental health problems or residential services for substance use disorders for 2 to 3 weeks. Informed consent was obtained from the participants and their parents or legal guardians. The Oklahoma Department of Mental Health and Substance Abuse Services Institutional Review Board approved this study.
Data
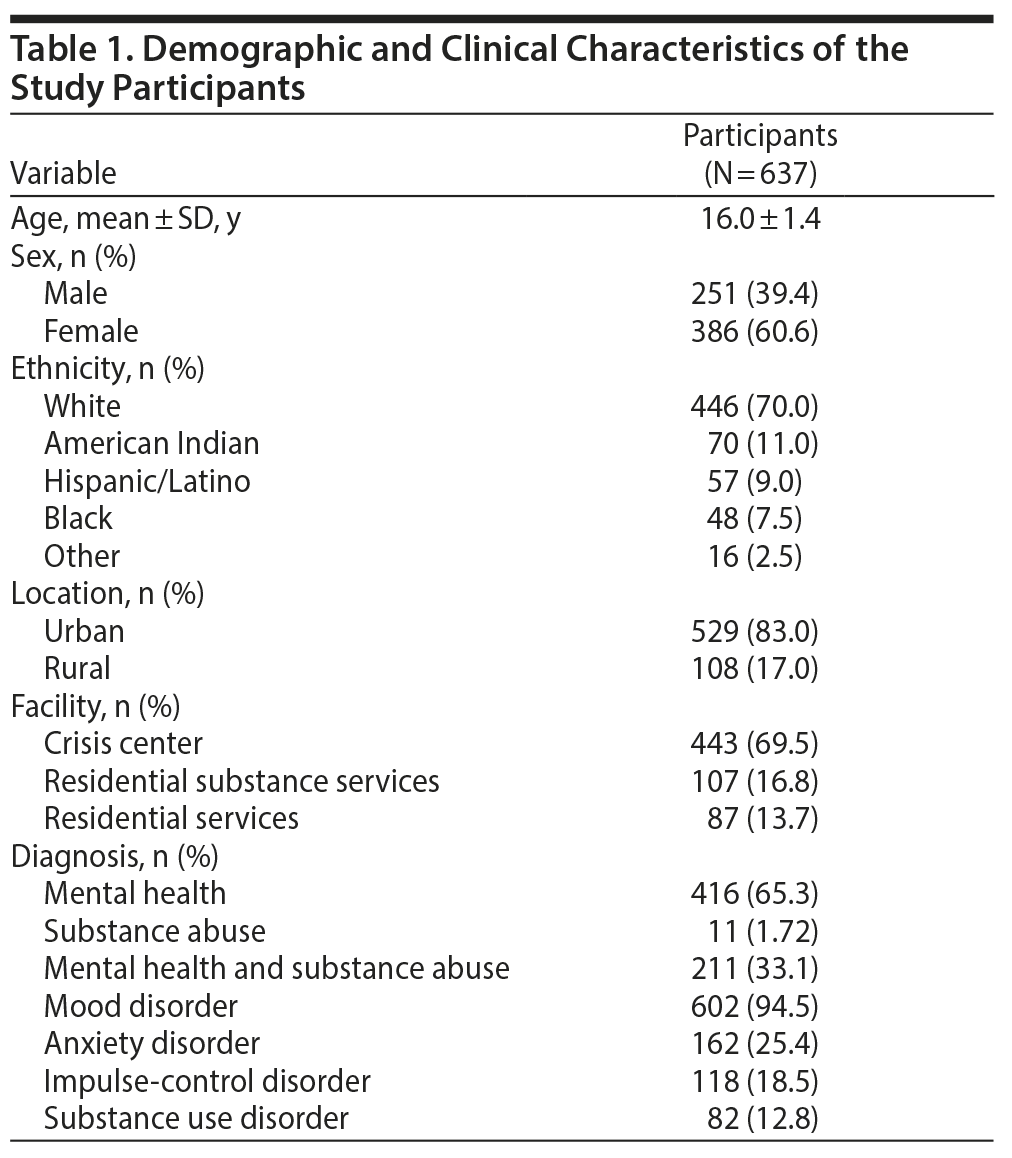
All of the data were collected during the participants’ hospital admission. Demographic data comprised age, sex, race, and locality (urban or rural classification). Other variables included type of service the adolescents were admitted to within the facility and their diagnosis. Diagnosis data included 1 variable measuring the type of diagnosis, ie, mental health and substance abuse, and 4 dichotomous variables measuring the presence or absence of mood, anxiety, impulse-control, and substance use disorders.
All of the participants were asked questions about their synthetic marijuana lifetime use, age at first use, type, and frequency. The survey for synthetic marijuana use evolved over the study period. Beginning January 1, 2015, we expanded the survey, and 455 participants responded to the new questionnaire that included the following:
(1) Reason for synthetic marijuana use
(2) How the experiences differ between synthetic and conventional marijuana use
(3) Source of synthetic marijuana
(4) Perception of the relative danger of synthetic and conventional marijuana
(5) If the patient or anyone he or she knows had any adverse reaction to synthetic marijuana use
(6) Lifetime use of any other illicit synthetic substances.
All information obtained from the participants was documented for analysis.
Statistical Analysis
Data were analyzed using SPSS version 23 software (IBM, Armonk, New York). The descriptive statistical analysis was performed for most variables. Demographic characteristics such as age, sex, race, and urban or rural classification were considered to analyze the rates of synthetic marijuana use. Pearson χ2 test was used to compare marijuana users with nonusers. Logistic regression analysis and adjusted odds ratio (OR) were performed to identify the potential risk factors for synthetic marijuana use. A P value ≤ .05 was considered statistically significant.
RESULTS
The demographic characteristics for the entire study population are summarized in Table 1.
Marijuana Use Among the Study Population
Of 637 adolescents, 429 (67.3%) reported using marijuana at least once in their lifetime. The mean age at first use of marijuana was 13 years, and the mean age for synthetic marijuana users was 16 years. The distribution of marijuana use in the study population is tabulated in Table 2.
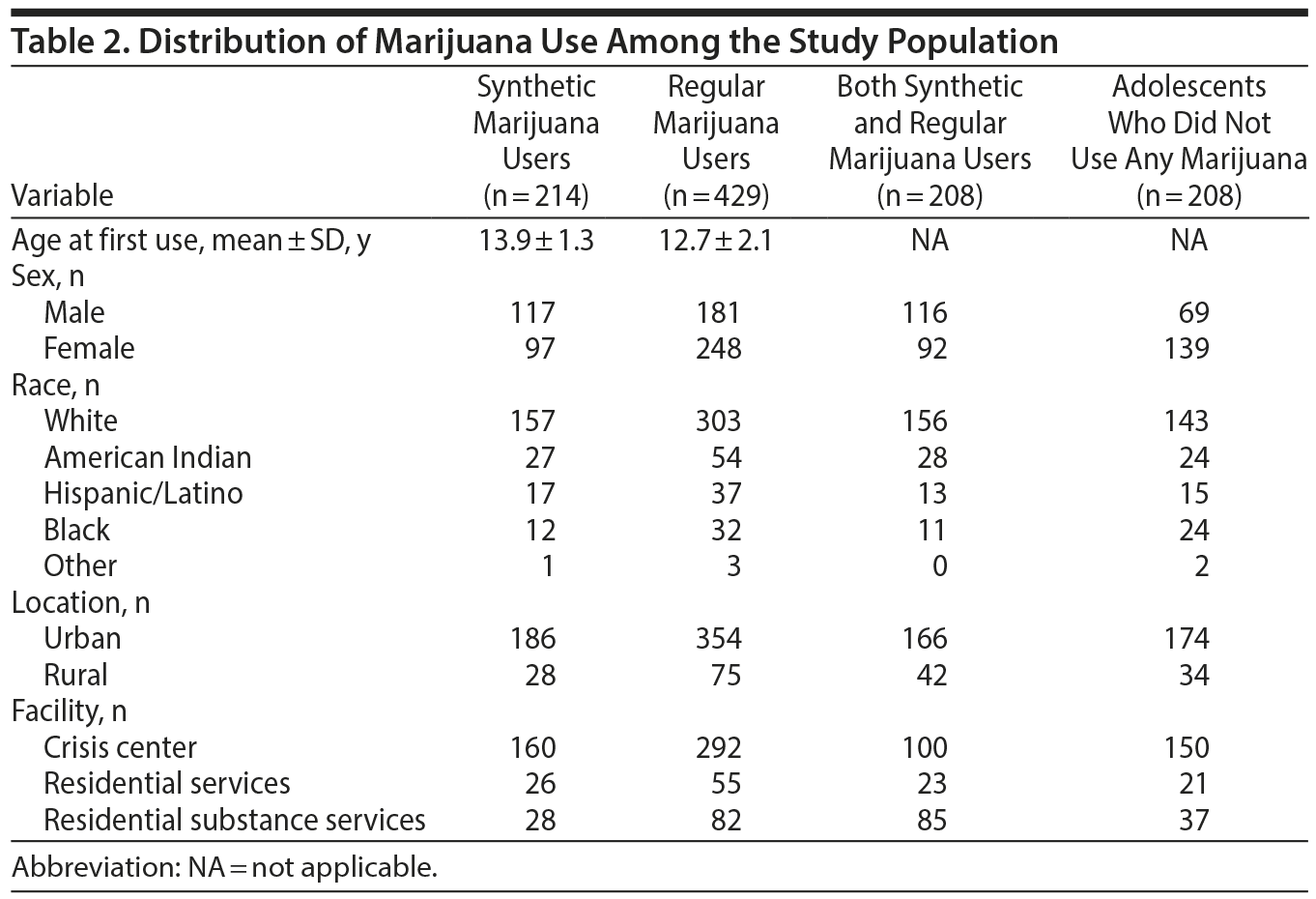
Synthetic Marijuana Use Among the Study Population
Among 429 adolescents using marijuana, 214 (49.8%) admitted using synthetic marijuana. Of them, 71 (33.1%) reported using at least once, and 48 (22.4%) were daily users. The demographic characteristics of adolescents using synthetic marijuana are included in Table 3.

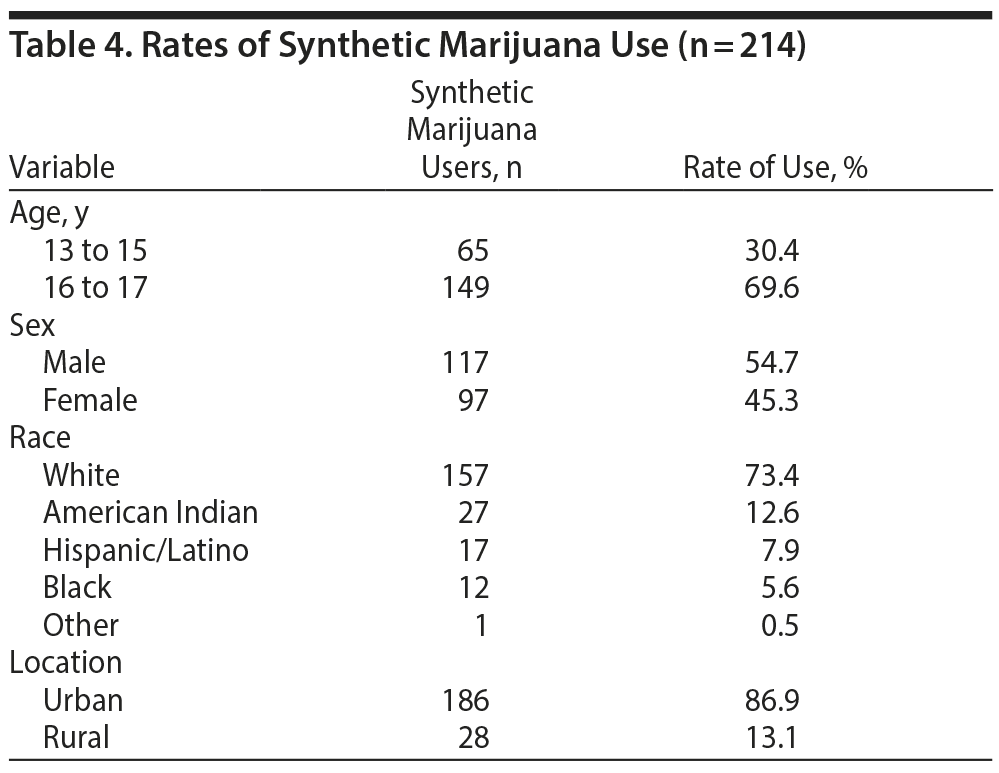
Rates of synthetic cannabinoid use. We used age, sex, race, and location to calculate rates of synthetic cannabinoid use (Table 4). Increased prevalence of synthetic cannabinoid consumption was observed in 16- to 17-year-old adolescent white males from urban communities. The types of synthetic cannabinoid products used by the study population include K2: 84 (39.2%), Diablo: 15 (7%), Mr Nice Guy: 7 (3.2%), Get Real: 5 (2.3%), Spice: 4 (1.8%), Fake Bake: 3 (1.4%), and unknown: 9 (4.2%).
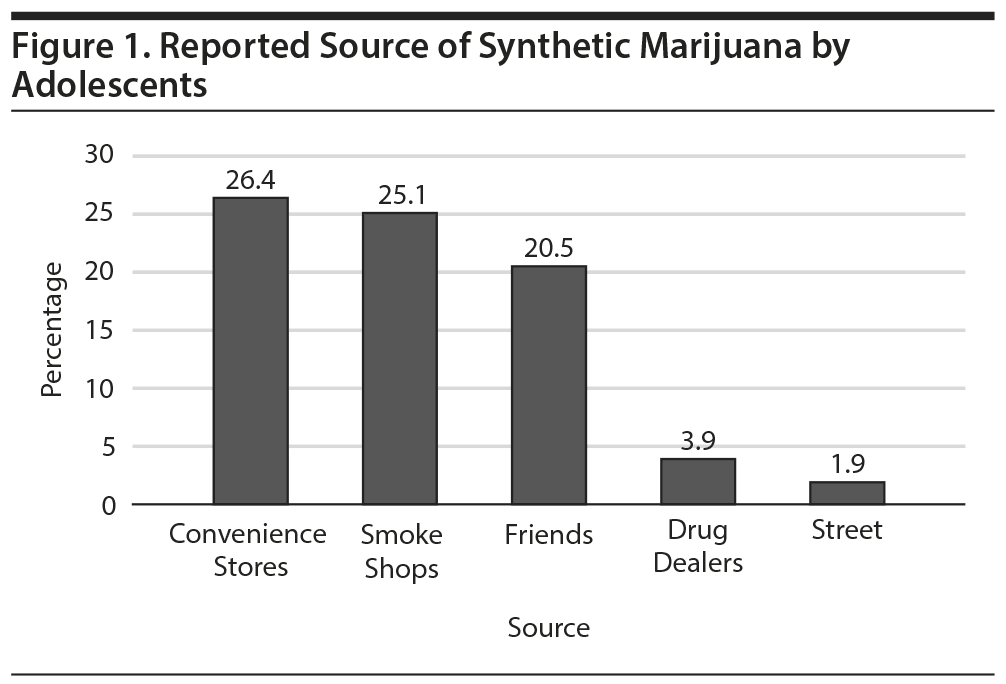
Source of synthetic marijuana. Among 214 adolescents, 151 (70.5%) reported their source of synthetic cannabinoid products as convenience stores: 40 (26.4%), smoke or head shops: 38 (25.1%), friends: 31 (20.5%), drug dealers: 6 (3.9%), and random people on the street: 3 (1.9%) (Figure 1).
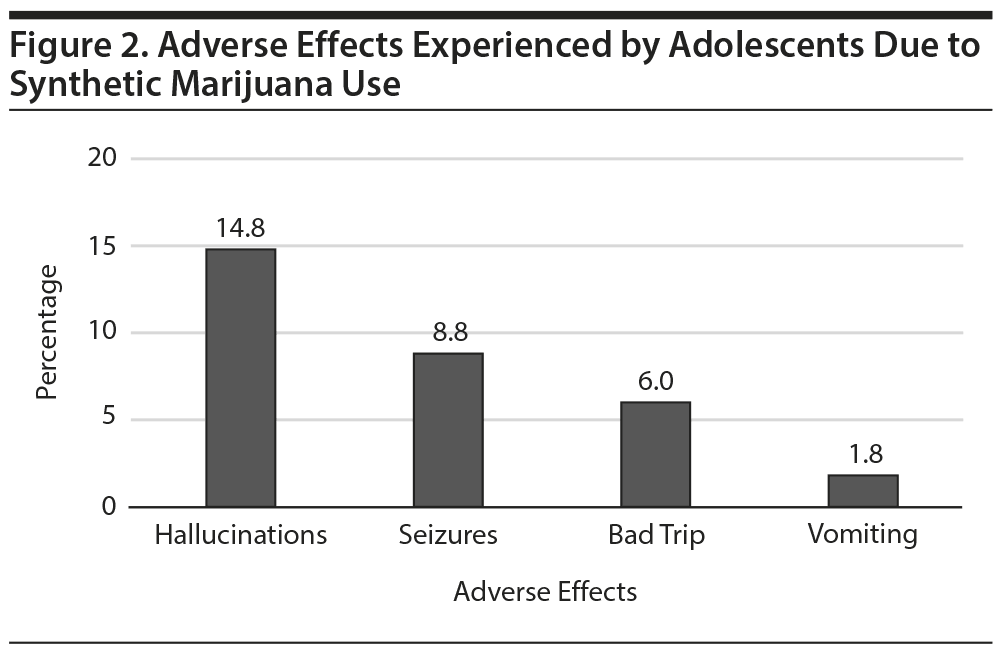
Perception of danger among adolescents regarding synthetic marijuana use. Of 455 study participants, 376 (82.6%) reported that they perceive synthetic marijuana to be more dangerous than regular marijuana. A total of 216 (47.4%) of 455 adolescents described experiencing or witnessing an adverse reaction due to synthetic cannabinoid use. Of them, 19 (8.8%) reported having seizures, while 27 (12.5%) stated that they witnessed their friends or a family member having a seizure. Thirty-two (14.8%) indicated having hallucinations, 13 (6%) experienced a bad “trip,” and 4 (1.8%) vomited after the use of synthetic marijuana (Figure 2). Seven (3.2%) participants reported that they were aware of the harmful side effects caused by synthetic marijuana products.
Lifetime use of any other synthetic substances. Of 455 adolescents, 27 (5.9%) admitted using other synthetic substances. The most commonly reported are bath salts (33.3%), Ecstasy (14.8%), N-Bomb (7.4%), bird eggs (3.7%), and Krokodil (3.7%).
Synthetic Versus Regular Marijuana
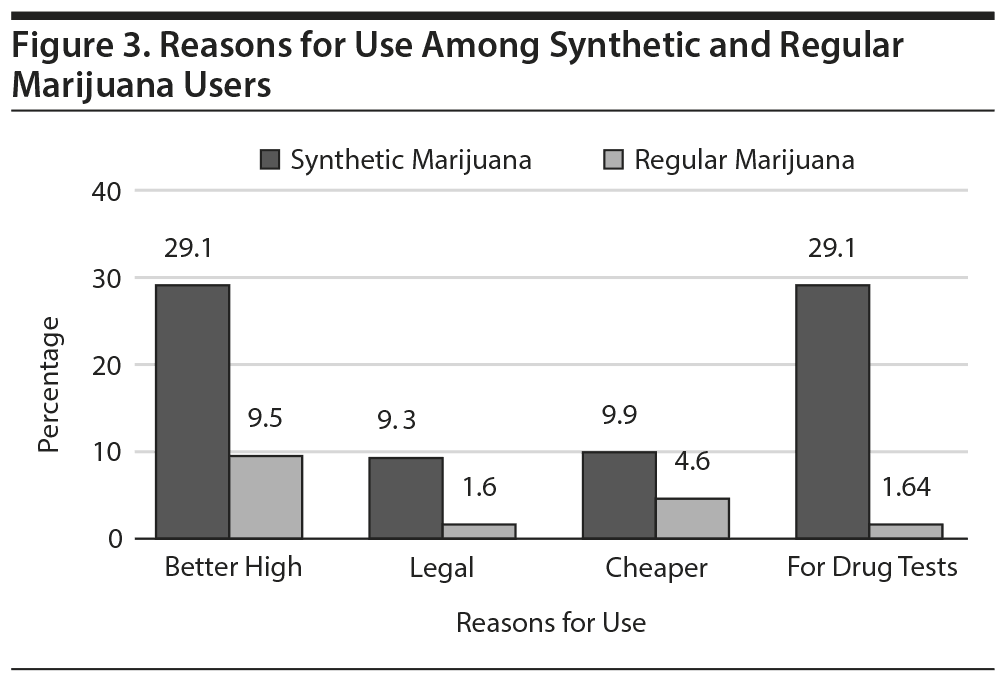
Reasons for synthetic marijuana use. After expanding the questionnaire, 455 adolescents completed the survey. The determining factors for adolescents using synthetic over regular marijuana are shown in Figure 3. Adolescents preferred synthetic marijuana, as it is a cheaper alternative to conventional marijuana, produces a better high, is undetectable on drug testing, and is perceived as legal.
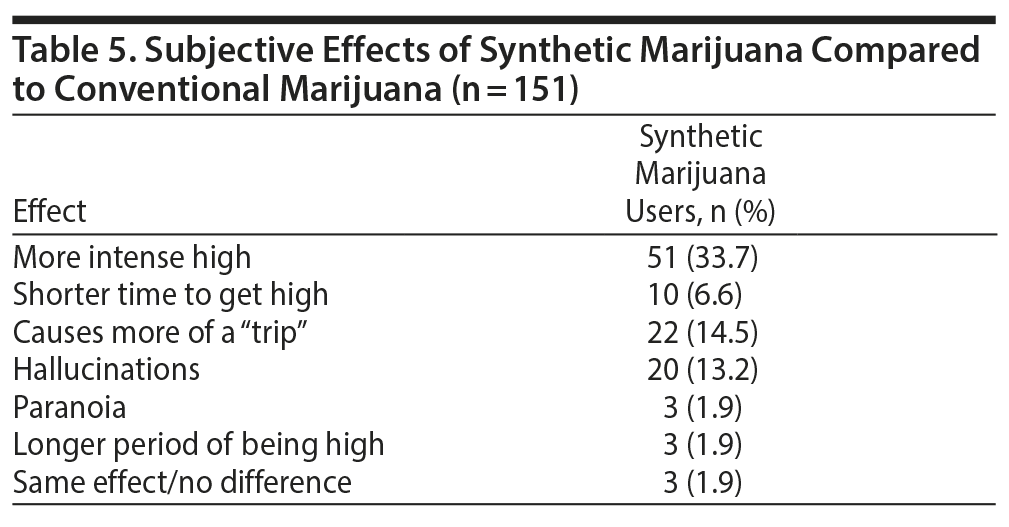
Subjective effects of synthetic marijuana use compared to conventional marijuana. Of 214 synthetic cannabinoid users, 151 (70.5%) adolescents described experiencing a high in a shorter period of time, longer lasting effects, more trips, hallucinations, and paranoia with synthetic marijuana compared to regular marijuana (Table 5).
Comparison Between
Synthetic Marijuana Users and Nonusers
To compare synthetic marijuana use, we divided our study population into 2 groups (Table 6). The first group included adolescents who used synthetic marijuana versus those who did not use marijuana, and the second group comprised adolescents who used synthetic marijuana versus those who used regular marijuana. The mean age for all of the participants was 16 years.
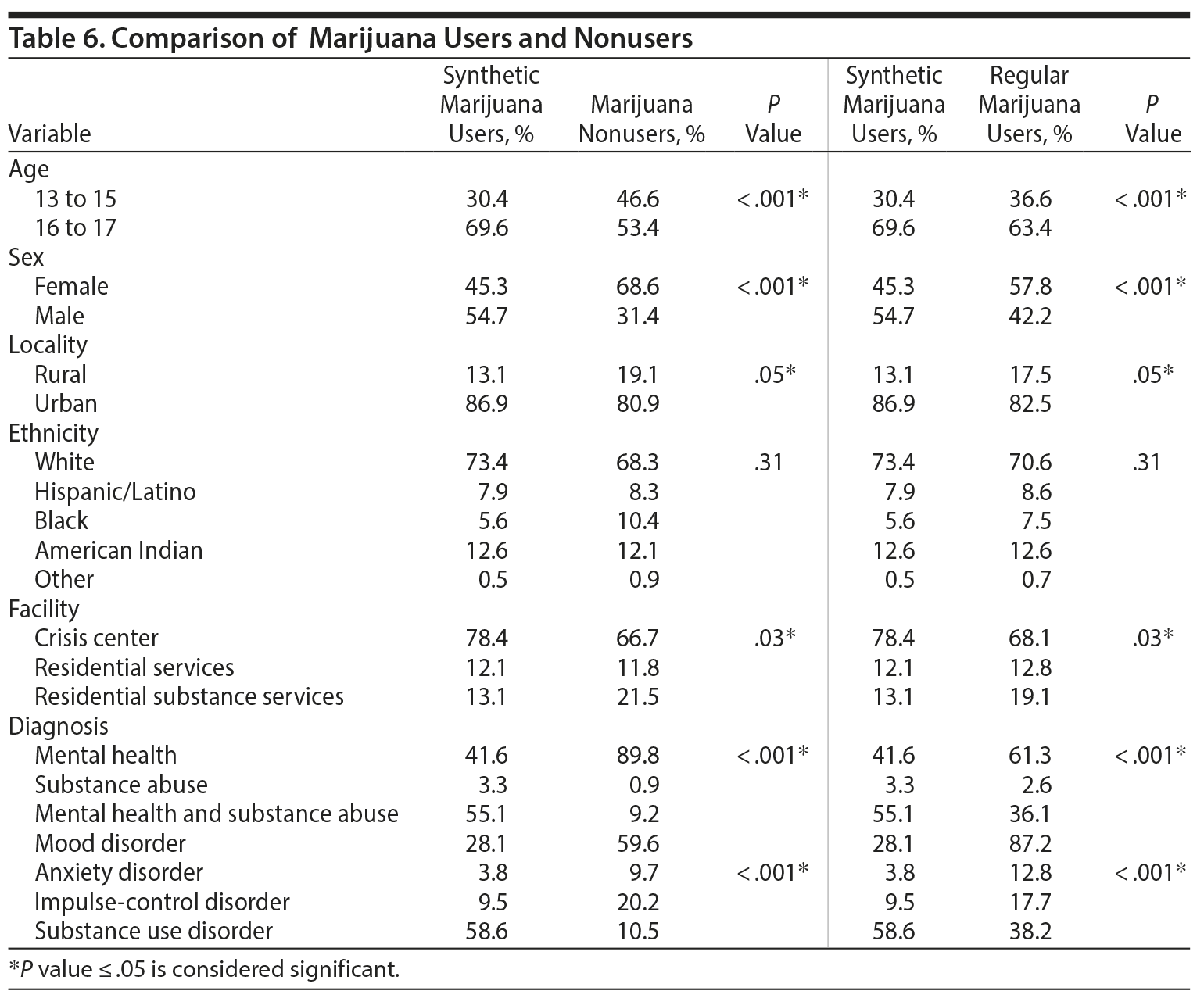
Synthetic marijuana users versus marijuana nonusers. More adolescents using synthetic marijuana were male (54.7%) than female, whereas the group that did not use marijuana comprised more females (68.6%, P < .001). In both groups, more adolescents were aged 16 to 17 years (69.6% vs 53.4%, P < .001). Both the synthetic marijuana users and marijuana nonusers were mainly living in urban areas (86.9% vs 80.9%, P = .05). Additionally, the prevalence of substance use disorder was higher in the adolescents using synthetic marijuana compared to marijuana nonusers (58.6% vs 10.5%, P < .001).
Synthetic marijuana users versus regular marijuana users. When synthetic and regular marijuana users were compared, more adolescents were aged 16 to 17 years in both groups (69.6% vs 63.4%, P < .001). More males were synthetic marijuana users (54.7%), and more females were using regular marijuana (57.8%, P < .001). Both synthetic and regular marijuana users were from urban areas (86.5% vs 82.5%, P = .05). Regular marijuana users were having more mental health problems than synthetic marijuana users (61.3% vs 41.6%, P < .001), whereas synthetic marijuana users had more diagnoses of substance use disorder compared to regular marijuana users (58.6% vs 38.2%, P < .001).
Risk Factors Associated With Synthetic Marijuana Use
To identify the risk factors for synthetic marijuana use, we considered age, sex, race, locality, type of service the adolescents were admitted to within CRC, and their diagnosis. We performed binary logistic regression, and the outcomes are included in Table 7. When subjects who used synthetic marijuana were compared with those who did not use marijuana, 16- to 17-year-old adolescents were found to be more at risk of using synthetic marijuana, and for every 1-year increase in age, the risk increased by 99% (OR = 1.99; 95% CI, 1.41–2.83; P < .001). The odds of using synthetic marijuana were 2.63 times higher for males than females (OR = 2.63; 95% CI, 1.87–3.68; P < .001). Also, for each study participant living in an urban area, the odds of using synthetic marijuana increased by 57% (OR = 1.57; 95% CI, 0.98–2.50; P = .05). Synthetic marijuana users were also 11.8 times more at risk of having substance use disorder than those who did not use marijuana (OR = 11.87; 95% CI, 7.58–18.60; P < .001).
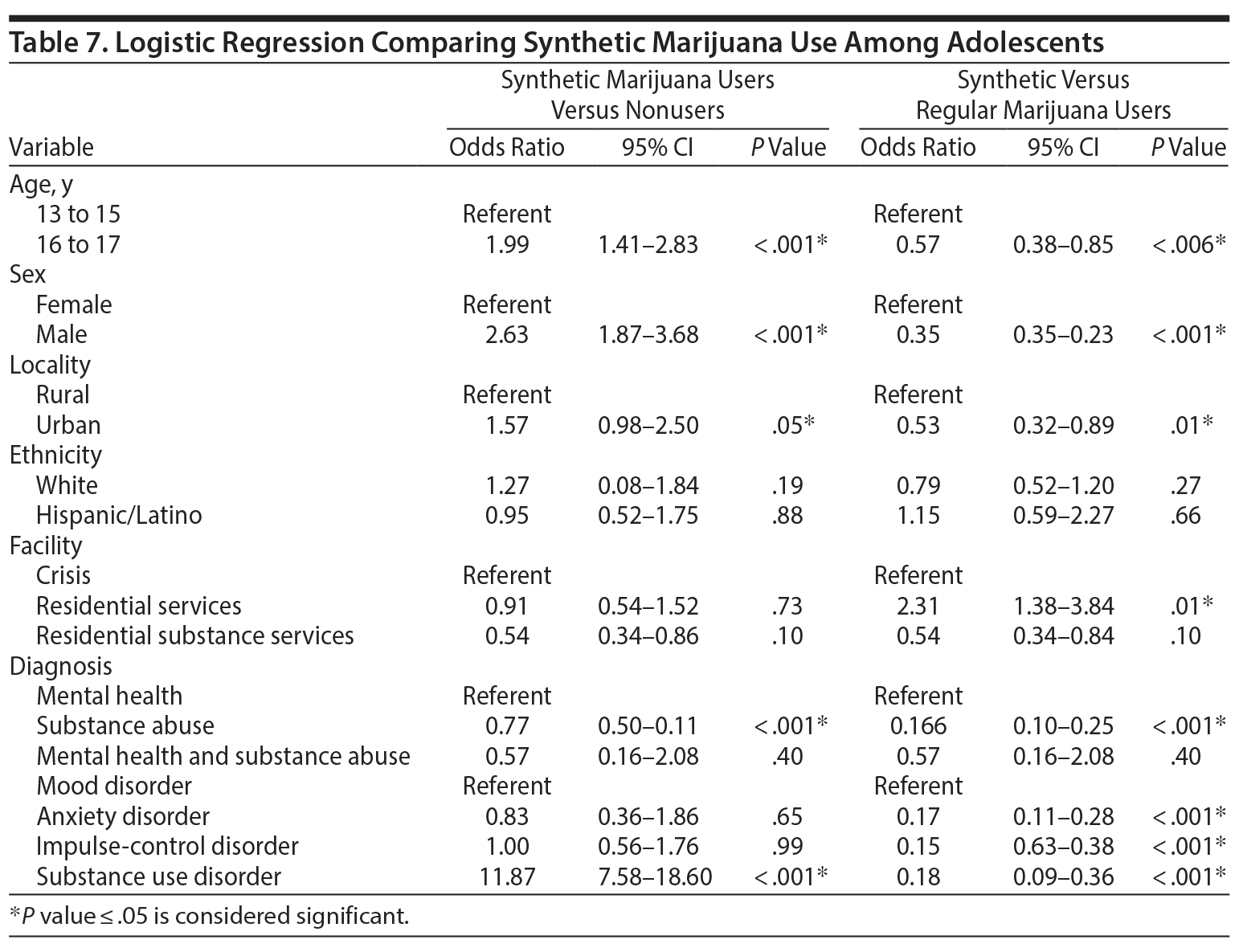
When we compared the demographic variables for synthetic and regular marijuana users, there was a minimal difference between both groups. Adolescents who consume synthetic marijuana have a 2.3 times higher risk of being admitted to long-term residential services within CRC than regular marijuana users (OR = 2.31; 95% CI, 1.38–3.84; P = .01).
DISCUSSION
Our study provides insight into synthetic marijuana use by adolescents admitted to our treatment facility. Although there are studies1,10,13,14,21,22 on synthetic marijuana use by adolescents, to our knowledge, this is the first to report the reasons, source, perception of use, and adverse effects with regard to consumption among this age group. The strength of our study also lies in using the comparison groups and analyzing the differences between the demographic and clinical characteristics of synthetic marijuana users versus marijuana nonusers and synthetic and regular marijuana users.
This study analysis showed that about 67% of the adolescents used marijuana at least once. Among them, 50% used synthetic marijuana. Our results support evidence from previous studies28 that the prevalence of synthetic marijuana consumption is higher in adolescent males. As per our study results, adolescent perception of synthetic cannabinoid products compared to regular marijuana included gives better high, perceive them as legal, less expensive, and cannot be detected on drug tests. Adolescent males aged 16 to 17 years living in urban areas are more at risk of consuming synthetic marijuana and having substance use disorder compared to those who use regular marijuana.
Additionally, this study revealed that most of the teenagers obtained synthetic marijuana from convenience stores and smoke shops, followed by friends, drug dealers, and street vendors. Approximately 82.6% of adolescents reported that synthetic marijuana is more dangerous than conventional marijuana. Of those, 47.4% mentioned having or witnessing a seizure, hallucinations, bad trip, and vomiting after synthetic marijuana consumption. About 70.5% of the adolescents reported experiencing a high in a shorter time that lasted for a longer duration, more trips, hallucinations, and paranoia with synthetic marijuana than with regular marijuana.
Since the last decade, several studies3,29 have focused on adolescents’ risk perception for substance use. The National Survey on Drug Use and Health29 reported that among adolescents, the perception of risk was high for drugs like cocaine, heroin, and lysergic acid diethylamide (LSD) but varies for cannabis. For instance, in a study3 conducted from 2012 to 2014, teenagers reported that consuming synthetic marijuana is dangerous, and a subsequent decline was noticed in the rate of use. However, another study29 revealed that youngsters who use synthetic marijuana do not perceive it to be dangerous and believe that they can quit using the drug at any time. Contrarily, our study indicates that despite the perception of harm and significant rates of either experiencing or witnessing an adverse event, adolescents still used synthetic cannabinoid products.
Synthetic marijuana use could potentially increase the risk of acute inpatient care and the length of stay in the hospital, causing a health care burden.28,30 A study31 revealed that synthetic marijuana was the cause of death when patients were investigated for a drug overdose, driving under the influence, suicide, or homicide. As new forms of synthetic marijuana continue to become available with different formulations, it may be beneficial to screen all patients, especially adolescents, for intoxication and withdrawal symptoms and develop innovative procedures to detect these drugs.3,32 Clinical trials33 have emphasized that along with pharmacologic treatment, psychosocial interventions involving cognitive-behavioral therapy, motivational enhancement therapy, or a combination of both for cannabis use disorder might be effective.
Our study has a few limitations. As we expanded our survey during the study, we were unable to obtain information from all our participants regarding synthetic marijuana use. Since our research comprised only a high-risk population, we cannot extrapolate these results to the general population. From the researcher’s clinical experiences, it was also evidenced that working with this population historically had a “canary in the coal mine” effect, which might increase the new substance trends and rate spikes in the general population and also the Substance Abuse and Mental Health Services Administration data by 1 or 2 years. Hence, further research is required to identify the rates of synthetic cannabinoid use in the general population.
CONCLUSION
As synthetic marijuana use among adolescents is increasing, educating teenagers at school regarding the adverse effects caused by consuming the drug could create awareness to an extent. A collaborative approach involving health care workers, research scientists, jurisdictive bodies, and citizens at all levels of society to enforce firm regulations and implement new policies against synthetic marijuana use would be beneficial. Further research is also needed to identify the potential consequences that could occur with long-term synthetic marijuana use.
Submitted: December 27, 2017; accepted May 9, 2018.
Published online: September 6, 2018.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration–approved labeling has been presented in this article.
Financial disclosure: Drs Martz, Tankersley, Mekala, and Motiwala have no personal affiliations or financial relationships with any commercial interest to disclose relative to this article.
Funding/support: None.
REFERENCES
1. Hermanns-Clausen M, Kneisel S, Hutter M, et al. Acute intoxication by synthetic cannabinoids—four case reports. Drug Test Anal. 2013;5(9–10):790–794. PubMed CrossRef
2. Volkow N. Principles of Adolescent Substance Use Disorder Treatment: A Research-Based Guide. Bethesda, MD: National Institutes of Health; 2014:1–42.
3. Weinstein AM, Rosca P, Fattore L, et al. Synthetic cathinone and cannabinoid designer drugs pose a major risk for public health. Front Psychiatry. 2017;8:156. PubMed CrossRef
4. Wood KE. Exposure to bath salts and synthetic tetrahydrocannabinol from 2009 to 2012 in the United States. J Pediatr. 2013;163(1):213–216. PubMed CrossRef
5. Musselman ME, Hampton JP. “Not for human consumption”: a review of emerging designer drugs. Pharmacotherapy. 2014;34(7):745–757. PubMed CrossRef
6. Vandrey R, Dunn KE, Fry JA, et al. A survey study to characterize use of Spice products (synthetic cannabinoids). Drug Alcohol Depend. 2012;120(1–3):238–241. PubMed CrossRef
7. Dresen S, Ferreirós N, Pütz M, et al. Monitoring of herbal mixtures potentially containing synthetic cannabinoids as psychoactive compounds. J Mass Spectrom. 2010;45(10):1186–1194. PubMed CrossRef
8. Nelson ME, Bryant SM, Aks SE. Emerging drugs of abuse. Dis Mon. 2014;60(3):110–132. PubMed CrossRef
9. Rosenbaum CD, Carreiro SP, Babu KM. Here today, gone tomorrow…and back again? a review of herbal marijuana alternatives (K2, Spice), synthetic cathinones (bath salts), kratom, Salvia divinorum, methoxetamine, and piperazines. J Med Toxicol. 2012;8(1):15–32. PubMed CrossRef
10. Wells DL, Ott CA. The “new” marijuana. Ann Pharmacother. 2011;45(3):414–417. PubMed CrossRef
11. Ashton JC. Synthetic cannabinoids as drugs of abuse. Curr Drug Abuse Rev. 2012;5(2):158–168. PubMed CrossRef
12. Drug Enforcement Administration, Department of Justice. Schedules of controlled substances: temporary placement of four synthetic cannabinoids into Schedule I: final order. Fed Regist. 2014;79(27):7577–7582. PubMed
13. Riederer AM, Campleman SL, Carlson RG, et al; Toxicology Investigators Consortium (ToxIC). Acute poisonings from synthetic cannabinoids—50 US toxicology investigators consortium registry sites, 2010–2015. MMWR Morb Mortal Wkly Rep. 2016;65(27):692–695. PubMed CrossRef
14. Adams AJ, Banister SD, Irizarry L, et al. “Zombie” outbreak caused by the synthetic cannabinoid AMB-FUBINACA in New York. N Engl J Med. 2017;376(3):235–242. PubMed CrossRef
15. Kemp AM, Clark MS, Dobbs T, et al. Top 10 facts you need to know about synthetic cannabinoids: not so nice Spice. Am J Med. 2016;129(3):240–244.e1. PubMed CrossRef
16. Fattore L, Fratta W. Beyond THC: the new generation of cannabinoid designer drugs. Front Behav Neurosci. 2011;5:60. PubMed CrossRef
17. Labay LM, Caruso JL, Gilson TP, et al. Synthetic cannabinoid drug use as a cause or contributory cause of death. Forensic Sci Int. 2016;260:31–39. PubMed CrossRef
18. Fattore L. Synthetic cannabinoids—further evidence supporting the relationship between cannabinoids and psychosis. Biol Psychiatry. 2016;79(7):539–548. PubMed CrossRef
19. Adams IB, Martin BR. Cannabis: pharmacology and toxicology in animals and humans. Addiction. 1996;91(11):1585–1614. PubMed CrossRef
20. Ashton CH. Pharmacology and effects of cannabis: a brief review. Br J Psychiatry. 2001;178(2):101–106. PubMed CrossRef
21. Tashkin DP. Effects of marijuana smoking on the lung. Ann Am Thorac Soc. 2013;10(3):239–247. PubMed CrossRef
22. Solowij N, Stephens RS, Roffman RA, et al; Marijuana Treatment Project Research Group. Cognitive functioning of long-term heavy cannabis users seeking treatment. JAMA. 2002;287(9):1123–1131. PubMed CrossRef
23. Goldstein RZ, Volkow ND. Dysfunction of the prefrontal cortex in addiction: neuroimaging findings and clinical implications. Nat Rev Neurosci. 2011;12(11):652–669. PubMed CrossRef
24. Pintori N, Loi B, Mereu M. Synthetic cannabinoids: the hidden side of Spice drugs. Behav Pharmacol. 2017;28(6):409–419. PubMed CrossRef
25. Zuba D, Byrska B, Maciow M. Comparison of “herbal highs” composition. Anal Bioanal Chem. 2011;400(1):119–126. PubMed CrossRef
26. Gwak S, Arroyo-Mora LE, Almirall JR. Qualitative analysis of seized synthetic cannabinoids and synthetic cathinones by gas chromatography triple quadrupole tandem mass spectrometry. Drug Test Anal. 2015;7(2):121–130. PubMed CrossRef
27. Davidson C, Opacka-Juffry J, Arevalo-Martin A, et al. Spicing up pharmacology: a review of synthetic cannabinoids from structure to adverse events. Adv Pharmacol. 2017;80:135–168. PubMed CrossRef
28. Shalit N, Barzilay R, Shoval G, et al. Characteristics of synthetic cannabinoid and cannabis users admitted to a psychiatric hospital: a comparative study. J Clin Psychiatry. 2016;77(8):e989–e995. PubMed CrossRef
29. Azofeifa A, Mattson ME, Schauer G, et al. National estimates of marijuana use and related indicators—National Survey on Drug Use and Health, United States, 2002–2014. MMWR Surveill Summ. 2016;65(11):1–28. PubMed CrossRef
30. Patel RS, Patel P, Shah K, et al. Is cannabis use associated with worst inpatient outcomes in attention deficit hyperactivity disorder adolescents? Cureus. 2018;10(1):e2033. PubMed CrossRef
31. Marinetti LJ, Antonides HM. Analysis of synthetic cathinones commonly found in bath salts in human performance and postmortem toxicology: method development, drug distribution and interpretation of results. J Anal Toxicol. 2013;37(3):135–146. PubMed CrossRef
32. Wintermeyer A, Möller I, Thevis M, et al. In vitro phase I metabolism of the synthetic cannabimimetic JWH-018. Anal Bioanal Chem. 2010;398(5):2141–2153. PubMed CrossRef
33. Gates PJ, Sabioni P, Copeland J, et al. Psychosocial interventions for cannabis use disorder. Cochrane Database Syst Rev. 2016;(5):CD005336. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!




