Anxiety complaints are common among older people. Specific phobia is characterized by exaggerated fear to a specific object or situation. Fear of falling is one example and occurs in about 50% of older persons who have fallen recently. Polypharmacy heightens fall risks. Generalized anxiety disorder is characterized by chronic uncontrollable worry that interferes with functioning and is accompanied by restlessness and disturbed sleep. Panic disorder refers to recurrent, unexpected surges of intense fear that evidence physical and cognitive dysfunction. Cognitive behavior therapy has efficacy among psychotherapies for older anxious adults. In treating anxiety, medications that might be anxiogenic are reduced in dosage or discontinued. It is essential to monitor for suicidal ideation and symptom change. The first-selected pharmacotherapy for people with most anxiety disorders is selective serotonin reuptake inhibitors or serotonin-norepinephrine reuptake inhibitors. The risk-benefit ratio of benzodiazepine pharmacotherapy in elderly patients is not favorable.

ABSTRACT
Anxiety complaints are common among older people. Specific phobia is characterized by exaggerated fear to a specific object or situation. Fear of falling is one example and occurs in about 50% of older persons who have fallen recently. Polypharmacy heightens fall risks. Generalized anxiety disorder is characterized by chronic uncontrollable worry that interferes with functioning and is accompanied by restlessness and disturbed sleep. Panic disorder refers to recurrent, unexpected surges of intense fear that evidence physical and cognitive dysfunction. Cognitive behavior therapy has efficacy among psychotherapies for older anxious adults. In treating anxiety, medications that might be anxiogenic are reduced in dosage or discontinued. It is essential to monitor for suicidal ideation and symptom change. The first-selected pharmacotherapy for people with most anxiety disorders is selective serotonin reuptake inhibitors or serotonin-norepinephrine reuptake inhibitors. The risk-benefit ratio of benzodiazepine pharmacotherapy in elderly patients is not favorable.
Prim Care Companion CNS Disord 2019;21(1):18nr02335
To cite: Pary R, Sarai SK, Micchelli A, et al. Anxiety disorders in older patients. Prim Care Companion CNS Disord. 2019;21(1):18nr02335.
To share: https://doi.org/10.4088/PCC.18nr02335
© Copyright 2019 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Veterans Administration Medical Center, Louisville, Kentucky
bDepartment of Psychiatry, University of Louisville School of Medicine, Louisville, Kentucky
cMedical Library, Veterans Administration Medical Center, Louisville, Kentucky
*Corresponding author: Steven Lippmann, MD, 410 East Chestnut St , Ste 610, Louisville, KY 40202 ([email protected]).
Anxiety is a mood state oriented toward a future concern associated with preparation for a possible negative event.1 In contrast, fear is an alarm response to present or imminent danger. The objective of this narrative review is to acquaint readers with the characteristics of common anxiety disorders among older people. Treatment guidelines are also provided.
METHODS
A search with no date restrictions was conducted in early 2018 for English-language articles in PubMed, Psychiatry Online, UpToDate, and OvidMD. MeSH terms used in the search included benzodiazepines, anxiety, anxiety disorders, phobic disorders, psychiatry, adult, aged, complementary therapies, phobia, social, anti-anxiety agents, tai chi, psychotherapy, accidental falls, pulmonary disease, chronic obstructive, and drug therapy. The search strategy is included in the Supplementary Appendix.
Google Scholar was used to check article citations, author affiliations, and journal impact factor. The articles1-64 chosen were frequently cited in journals, with randomized controlled trials preferred.
INCIDENCE AND PREVALENCE
Anxiety is the most prevalent psychiatric disorder, with a lifetime prevalence of approximately 29%.2 Potential predictors for persistent anxiety include poor overall quality of life and comorbid personality or mood disorders.3
Incidence of newly emerging anxiety disorders in late life is low, as they typically do not newly emerge in older people. Anxiety complaints have usually already been present in 99% of anxious individuals who are over age 65 years.2
Anxiety among chronically ill older adults is disabling.4 Elderly outpatients with high anxiety frequently visit doctors but receive relatively few mental health services.4 Among nursing home residents, pain, pharmacotherapies for depression, and suboptimal quality of life are consistently associated with anxiety.5
ANXIETY SYNDROMES
Specific phobia is an anxiety disorder that represents exaggerated or irrational fear related to a specific object or situation6 (Table 1). A study7 of the prevalence and course of specific phobia in a population of 70-year-old individuals revealed a declining frequency from 10% at age 70 to 4% at age 79. The lifetime occurrence of anxiety disorders in noninstitutionalized persons over age 65 years is 30%, with a prevalence rate of 14% among those with anxiety and a rate of 11% for those with phobias8 (Table 2).
A fear of falling is one example of a specific phobia that is especially common among older individuals and occurs in up to 50% of those in long-term facilities.9 As people age, confidence in and ability to balance may impair performance, which over time can result in isolation. Those with significant mobility limitations, but without fear of an unstable gait, are most likely to fall; thus, fear of falling may act as a protective buffer.10 In a review11 of 28 studies of elderly people, the prevalence range for fear of falling was between 3% and 85%. Fear of falling occurs in about 50% of older persons who have fallen in the previous year.12 Some factors associated with fear of falling include female sex, impaired mobility, and the need for gait assistance devices.13

- Anxiety is a common emotion that can become chronic and yield considerable dysfunction.
- Intervention includes various psychotherapies, pharmacotherapies, and stress reduction techniques.
- When prescribing, it is especially important to consider geriatric patient problems such as unstable gait, reduced metabolism, and medicinal interactions.
Anxiety and especially depression are associated with fear of falling, with mood disorders being the most strongly connected.12 Detection and effective treatment of people with depression and anxiety are protective factors.
Polypharmacy, such as with coprescribed antidepressant and antianxiety drugs, heightens fall risks, especially among demented nursing home patients.14 People appear to fall more often when selective serotonin reuptake inhibitor (SSRI) dosages are high; however, this contention is controversial.15 With no known randomized controlled trials on this topic, there is insufficient evidence to recommend avoidance of SSRIs in older people based only on risk for falling.16
Social phobia is characterized by marked anxiety about 1 or more social situations in which the individual is exposed to possible scrutiny by others17 such as social interactions or being observed while eating or performing in public.17 There are several core symptoms of social phobia across the adult lifespan.18 These symptoms include anxiety associated with thinking about social situations, being in the social situation, remaining in the social situation too long, and avoiding such occasions.18 Additional concerns involve self-evaluations of being more nervous than others and having greater fear or avoidance than is reasonable.18 About 3% of adults experienced some social phobia in the prior year and 5% have during their lifetimes.19 People 65 years and older experience less social phobia than those who are younger.
Generalized anxiety disorder (GAD) is characterized by chronic, uncontrollable worry that interferes with function and is accompanied by restlessness, muscle tension, impaired concentration, and disturbed sleep.20 Such worries in older individuals often focus on concerns about health, finances, or disability of self or spouse.21 The prevalence of generalized anxiety without comorbidity is 1%, but up to 4% when associated with another psychiatric condition.22 The prevalence of GAD in persons over 65 years of age is lower than in younger adults, with a range in elderly people of 1%-2%.22
Panic disorder refers to recurrent, unexpected panic attacks. These emotions are surges of intense fear that peak within minutes and evidence numerous physical and cognitive symptoms.17 First-onset panic attacks occurring after age 55 are usually less severe than those starting earlier in life.23 The rate of panic disorder among those over age 55 is 1%, with a lifetime occurrence of nearly 4%.24 This condition is more common among patients reporting recent stress, poor health-related quality of life, tachycardia, or gastric ulcers.24 It is also associated with depression and being in lower socioeconomic groups. Since panic among older people has origins earlier in life, new cases are less likely over time.24 Yet, medical illnesses, use of stimulants, and drug withdrawal syndromes may contribute to panic symptoms and should remain in the differential diagnosis.25
COMORBIDITY
Anxiety and depression share some symptoms in common.1 Shared manifestations typically include a generalized distress factor. Anhedonia is specific to depression, whereas hyperarousal is related to persons with anxiety.1
Older persons experience comorbidities to a similar extent as younger adults; depressive and anxiety disorders frequently coexist across the lifespan.26 In a study by Lenze and colleagues,27 approximately 35% of older subjects with depression had at least 1 lifetime anxiety disorder, and 23% had a current diagnosis. The most common anxiety disorder diagnoses were panic disorder, specific phobia, and social phobia.27
Anxiety has links to coronary artery disease, but disparate findings are cited regarding postmyocardial infarction anxiety.28 Older adults who experienced a heart attack and are also anxious have more adverse cardiac events.29,30 Postmyocardial infarct anxiety-induced complications exist beyond the effects of depression31; yet, the validity of such contentions are not universally confirmed. An analysis of people after an infarct revealed that anxiety assessments were affected by the severity of heart disease, physical inactivity, and depression.31 Yet, postinfarction anxiety was not associated with more cardiovascular events or death.31
Patients with chronic obstructive pulmonary disease (COPD) are more likely to develop anxiety disorders compared with healthy controls.32 The development of anxiety among patients with COPD results in a compromised prognosis.32 Anxiety disorders are disabling in this population and without intervention can become chronic, thereby lowering self-esteem, predisposing to suicidal ideation, and increasing hospitalization rates.33 Both patients and caregivers may become overwhelmed and find it difficult to cope with such difficulties.
Patients with COPD also have a high prevalence of social and specific phobia.34 Socially phobic persons with COPD often are embarrassed by breathlessness, sweating, and urinary incontinence.34 Those with specific phobia fear certain circumstances or the idea of being without medication.34 Such patients frequently avoid leaving the house without their medication and minimize activities likely to cause breathlessness.34
Anxiety is associated with cognitive impairment and dementia.35 Depression and anxiety disorders in midlife are risk factors for dementia.36 Within this population, anxiety has a moderate incidence and persistence.37 Chronic anxiety is associated with reduced cortical brain thickness; yet, in a Mayo Clinic study38 after adjusting for comorbid depression, only the association between anxiety and reduced insular thickness was significant. The prevalence of anxiety in patients with Parkinson’s disease is higher than in healthy and comparably disabled elderly subjects.39
TREATMENT
Management
The elderly patient and family should be informed that treatment of anxiety is important to improve health and quality of life.40 Collateral information from family and caretakers is helpful for a complete history. Physicians should to be aware of prior therapies for anxiety and response. All medications that might be anxiogenic such as anticholinergic agents, antihistamines, steroids, sympathomimetic compounds, stimulants, and dopaminergic drugs should be reviewed.41 Ingestion of coffee, tea, and other caffeine sources and illicit stimulant drugs should be avoided.41 Coexistent anxiety and depression is frequent and requires treatment.40 Close follow-up with discussion of possible medication side effects enhances compliance.40 It is essential to monitor for suicidal ideation and symptom change, and symptom decline indicates clinical improvement.40
Psychotherapy
Cognitive behavioral therapy (CBT) benefits older patients with GAD.42 CBT has been shown to diminish worry and depressive symptoms, with improved mental health among older persons with GAD; however, that is not always consistently so.43
Exposure therapy is recommended for patients with specific phobias.44 Phobic severity, anxiety, and avoidance can be lessened when applied in combination with other psychotherapies.44 Treatment gains are maintained for 1 year, but exposure therapy yields high dropout rates and low treatment acceptance.45
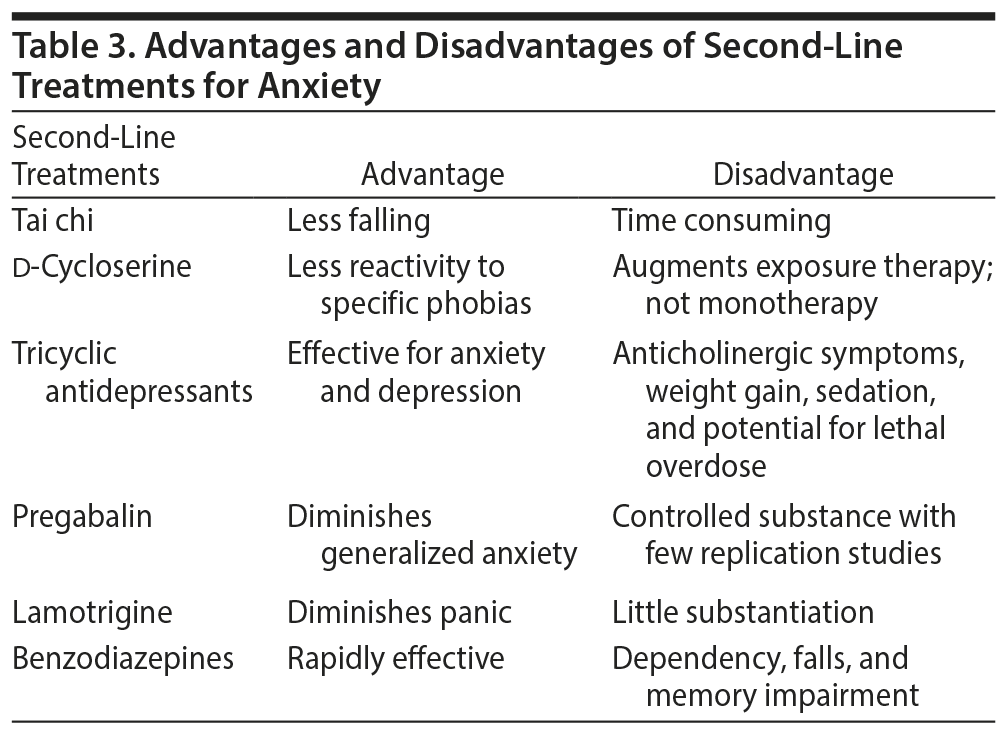
Tai chi is effective in reducing falls and fear of falling in older adults (Table 3).46 Its greatest benefit is enhancement of balance confidence.46 Tai chi is a system of gentle physical exercise and stretching that develops flexibility and coordination.47 Individuals are challenged to move through positions with a reduced base of support—standing on 1 leg is an example.48 Tai chi also promotes relaxation, awareness, and focus and is a form of physical therapy.47
Psychological interventions reduce anxiety and depression in demented patients by helping them learn better ways to cope with these symptoms.48 Psychotherapies compare favorably with pharmacologic treatments.49
Pharmacotherapy
Drug treatment often has better efficacy than psychotherapy in people with late-life anxiety.50 The usual first-selected treatment for anxiety disorders, with the exception of specific phobias, are the SSRI or serotonin-norepinephrine reuptake inhibitor (SNRI) drugs.51 Escitalopram and paroxetine are effective for specific phobias.52-54 Tricyclic antidepressant drugs are usually a second-choice option because of anticholinergic side effects, weight gain, sedation, and potential for lethal overdose.51 Other pharmacotherapies not approved for anxiety disorder management include monoamine oxidase inhibitors, mirtazapine, gabapentin, pregabalin, hydroxyzine, and antipsychotic drugs.
Pregabalin has efficacy for patients with GAD.51 Pregabalin acts on the α2δ subunit of calcium channels to reduce neurotransmitter release.51 Gabapentin has a similar mechanism in off-label prescribing.51 Lamotrigine may inhibit voltage-dependent sodium channels to decrease glutamate release. Lamotrigine can diminish panic in some people.55 All 3 of these drugs are anticonvulsant medications.
d-Cycloserine is an N-methyl-d-aspartate (NMDA) partial agonist prescribed off-label to augment exposure therapy.51 Although not effective in monotherapy, it can facilitate fear extinction.56 Additionally, d-cycloserine reduces reactivity to phobic stimuli in subjects with a specific phobia, as documented by functional magnetic resonance imaging.57 d-Cycloserine combined with exposure therapy can lead to sustained changes in the ventromedial and prefrontal cortex response to phobic stimuli.57
Benzodiazepines are often prescribed to older patients with anxiety. However, they are usually indicated only for short-term applications, as when adults experience infrequent anxiety symptoms, eg, flight phobia.58 Close physician monitoring is required when prescribing benzodiazepines, as anxiety in older people tends to become a chronic condition.4 Among sustained benzodiazepine users, only a small proportion use higher doses than recommended.59 Favorable features of benzodiazepines include a lack of metabolic or sexual side effects and quick alleviation of anxiety.60 These drugs are well tolerated and safe in oral monotherapy. When used on an as-needed basis, however, they might reinforce maladaptive behavior.40 The practice of prescribing anxiety medication for immediate relief may prolong anxiety for an extended period of time.40 There is greater dependence potential with short versus long half-life benzodiazepines.61 Physicians should use caution to avoid drug dependence. The risk-to-benefit ratio of this pharmacotherapy in older people is generally less favorable.61
Benzodiazepines induce a heightened risk for falls and hip fracture—dosages greater than 3 mg/d of diazepam equivalent increased the risk of hip fracture by 50%. Such injuries usually occur shortly after initiating therapy.62 Large dosages should be avoided. Short half-life benzodiazepine versions may not be safer than the long half-life versions; yet, falls occur more often with long elimination half-life benzodiazepines, especially when prescribed in combination with other drugs.63
Since benzodiazepines are eliminated slowly from the body, prolonged treatment with repeated doses often results in adipose tissue accumulation, dependence, and potential drug withdrawal.64 Impaired cognition can also occur. Thus, when benzodiazepines are utilized in older people, those with a short elimination half-life are usually preferred.63 Nevertheless, many people have been safely prescribed these medications for decades with no misuse or clinical concerns.
CONCLUSION
CBT has the best efficacy among the psychotherapies in treating elderly people with anxiety. Among pharmacotherapies, SSRI and SNRI drugs provide the greatest benefit in these patients.
Submitted: May 31, 2018; accepted September 17, 2018.
Published online: January 31, 2019.
Potential conflicts of interest: None.
Funding/support: None.
Supplementary material: See accompanying pages.
REFERENCES
1. Craske MG, Rauch SL, Ursano R, et al. What is an anxiety disorder? Focus. 2011;9(3):369-388. CrossRef
2. Kessler RC, Berglund P, Demler O, et al. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2005;62(6):593-602. PubMed CrossRef
3. Mackenzie CS, El-Gabalawy R, Chou K-L, et al. Prevalence and predictors of persistent versus remitting mood, anxiety, and substance disorders in a national sample of older adults. Am J Geriatr Psychiatry. 2014;22(9):854-865. PubMed CrossRef
4. Schuurmans J, van Balkom A. Late-life anxiety disorders: a review. Curr Psychiatry Rep. 2011;13(4):267-273. PubMed CrossRef
5. Creighton AS, Davison TE, Kissane DW. The correlates of anxiety among older adults in nursing homes and other residential aged care facilities: a systematic review. Int J Geriatr Psychiatry. 2017;32(2):141-154. PubMed CrossRef
6. Le Beau RT, Glenn D, Liao B, et al. A review of specific phobia and preliminary recommendations for DSM-V. Depress Anxiety. 2010;27(2):148-167. PubMed CrossRef
7. Sigström R, Skoog I, Karlsson B, et al. Nine-year follow up of specific phobia in a population sample of older people. Depress Anxiety. 2016;33(4):339-346. PubMed CrossRef
8. Ritchie K, Artero S, Beluche I, et al. Prevalence of DSM-IV psychiatric disorder in the French elderly population. Br J Psychiatry. 2004;184:147-152. PubMed
9. Lach HW, Parsons JL. Impact of fear of falling in long term care: an integrative review. J Am Med Dir Assoc. 2013;14(8):573-577. PubMed
10. Litwin H, Erlich B, Dunsky A. The complex association between fear of falling and mobility limitations in relation to late-life falls: a SHARE-based analysis. J Aging Health. 2018;30(6):987-1008. PubMed CrossRef
11. Scheffer AC, Schuurmans MJ, van Dijk N, et al. Fear of falling: measurement strategy, prevalence, risk factors and consequences among older persons. Age Ageing. 2008;37(1):19-24. PubMed CrossRef
12. Gagnon N, Flint AJ, Naglie G, et al. Affective correlates of fear of falling in elderly persons. Am J Geriatr Psychiatry. 2005;13(1):7-14. PubMed CrossRef
13. Denkinger MD, Lukas A, Nikolaus T, et al. Factors associated with fear of falling and associated activity restriction in community-dwelling older adults: a systematic review. Am J Geriatr Psychiatry. 2015;23(1):72-86. PubMed CrossRef
14. Sterke CS, Verhagen AP, van Beeck EF, et al. The influence of drug use on fall incidents among nursing home residents: a systematic review. Int Psychogeriatr. 2008;20(5):890-910. PubMed CrossRef
15. Sterke CS, Ziere G, van Beeck EF, et al. Dose-response relationship between selective serotonin reuptake inhibitors and injurious falls: a study in nursing home residents with dementia. Br J Clin Pharmacol. 2012;73(5):812-820. PubMed CrossRef
16. Gebara MA, Lipsey KL, Karp JF, et al. Cause or effect? Selective serotonin reuptake inhibitors and falls in older adults: a systematic review. Am J Geriatr Psychiatry. 2015;23(10):1016-1028. PubMed CrossRef
17. Black DW, Grant JE. Anxiety disorders. In: Black DW, Grant JE, eds. DSM-5 Guidebook: The Essential Companion to the Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Washington, DC: American Psychiatric Publishing; 2014:131-135.
18. Miloyan B, Bulley A, Pachana NA, et al. Social phobia symptoms across the adult lifespan. J Affect Disord. 2014;168:86-90. PubMed CrossRef
19. Grant BF, Hasin DS, Blanco C, et al. The epidemiology of social anxiety disorder in the United States: results from the National Epidemiologic Survey on Alcohol and Related Conditions. J Clin Psychiatry. 2005;66(11):1351-1361. PubMed CrossRef
20. Huge EA, Oppenheimer JE, Simmons NM. Generalized anxiety disorder. Focus. 2004;2(3):346-359.
21. Diefenbach GJ, Stanley MA, Beck JG. Worry content reported by older adults with and without generalized anxiety disorder. Aging Ment Health. 2001;5(3):269-274. PubMed CrossRef
22. Flint AJ. Generalised anxiety disorder in elderly patients: epidemiology, diagnosis and treatment options. Drugs Aging. 2005;22(2):101-114. PubMed CrossRef
23. Sheikh JI, Swales PJ, Carlson EB, et al. Aging and panic disorder: phenomenology, comorbidity, and risk factors. Am J Geriatr Psychiatry. 2004;12(1):102-109. PubMed CrossRef
24. Chou KL. Panic disorder in older adults: evidence from the national epidemiologic survey on alcohol and related conditions. Int J Geriatr Psychiatry. 2010;25(8):822-832. PubMed CrossRef
25. Krasucki C, Howard R, Mann A. The relationship between anxiety disorders and age. Int J Geriatr Psychiatry. 1998;13(2):79-99. PubMed CrossRef
26. King-Kallimanis B, Gum AM, Kohn R. Comorbidity of depressive and anxiety disorders for older Americans in the national comorbidity survey-replication. Am J Geriatr Psychiatry. 2009;17(9):782-792. PubMed CrossRef
27. Lenze EJ, Mulsant BH, Shear MK, et al. Comorbid anxiety disorders in depressed elderly patients. Am J Psychiatry. 2000;157(5):722-728. PubMed CrossRef
28. Sheps DS, Sheffield D. Depression, anxiety, and the cardiovascular system: the cardiologist’s perspective. J Clin Psychiatry. 2001;62(suppl 8):12-16, discussion 17-18. PubMed
29. Tully PJ, Cosh SM, Baumeister H. The anxious heart in whose mind? a systematic review and meta-regression of factors associated with anxiety disorder diagnosis, treatment and morbidity risk in coronary heart disease. J Psychosom Res. 2014;77(6):439-448. PubMed CrossRef
30. Huffman JC, Smith FA, Blais MA, et al. Anxiety, independent of depressive symptoms, is associated with in-hospital cardiac complications after acute myocardial infarction. J Psychosom Res. 2008;65(6):557-563. PubMed CrossRef
31. Larsen KK, Christensen B, Nielsen TJ, et al. Post-myocardial infarction anxiety or depressive symptoms and risk of new cardiovascular events or death: a population-based longitudinal study. Psychosom Med. 2014;76(9):739-746. PubMed CrossRef
32. Eisner MD, Blanc PD, Yelin EH, et al. Influence of anxiety on health outcomes in COPD. Thorax. 2010;65(3):229-234. PubMed CrossRef
33. Yohannes AM, Alexopoulos GS. Depression and anxiety in patients with COPD. Eur Respir Rev. 2014;23(133):345-349. PubMed CrossRef
34. Willgoss TG, Yohannes AM. Anxiety disorders in patients with COPD: a systematic review. Respir Care. 2013;58(5):858-866. PubMed
35. Gulpers B, Ramakers I, Hamel R, et al. Anxiety as a predictor for cognitive decline and dementia: a systematic review and meta-analysis. Am J Geriatr Psychiatry. 2016;24(10):823-842. PubMed CrossRef
36. Zilkens RR, Bruce DG, Duke J, et al. Severe psychiatric disorders in mid-life and risk of dementia in late-life (age 65-84 years): a population based case-control study. Curr Alzheimer Res. 2014;11(7):681-693. PubMed CrossRef
37. van der Linde RM, Dening T, Stephan BC, et al. Longitudinal course of behavioural and psychological symptoms of dementia: systematic review. Br J Psychiatry. 2016;209(5):366-377. PubMed CrossRef
38. Pink A, Przybelski SA, Krell-Roesch J, et al. Cortical thickness and anxiety symptoms among cognitively normal elderly persons: the Mayo Clinic Study of Aging. J Neuropsychiatry Clin Neurosci. 2017;29(1):60-66. PubMed CrossRef
39. Pontone GM, Palanci J, Bienvenu OJ, et al. Familial aggregation of panic disturbances in Parkinson’s disease. J Neuropsychiatry Clin Neurosci. 2011;23(4):417-424. PubMed CrossRef
40. Bower ES, Wetherell JL, Mon T, et al. Treating anxiety disorders in older adults: current treatments and future directions. Harv Rev Psychiatry. 2015;23(5):329-342. PubMed CrossRef
41. Aggarwal R, Kunik M, Asghar-Ali A, et al. Anxiety in later life. Focus. 2017;15(2):157-161. CrossRef
42. Cuijpers P, Sijbrandij M, Koole S, et al. Psychological treatment of generalized anxiety disorder: a meta-analysis. Clin Psychol Rev. 2014;34(2):130-140. PubMed CrossRef
43. Stanley MA, Wilson NL, Novy DM, et al. Cognitive behavior therapy for generalized anxiety disorder among older adults in primary care: a randomized clinical trial. JAMA. 2009;301(14):1460-1467. PubMed CrossRef
44. Pachana NA, Woodward RM, Byrne GJ. Treatment of specific phobia in older adults. Clin Interv Aging. 2007;2(3):469-476. PubMed
45. Choy Y, Fyer AJ, Lipsitz JD. Treatment of specific phobia in adults. Clin Psychol Rev. 2007;27(3):266-286. PubMed CrossRef
46. Hackney ME, Wolf SL. Impact of Tai Chi Chu’ an practice on balance and mobility in older adults: an integrative review of 20 years of research. J Geriatr Phys Ther. 2014;37(3):127-135. PubMed CrossRef
47. Rand D, Miller WC, Yiu J, et al. Interventions for addressing low balance confidence in older adults: a systematic review and meta-analysis. Age Ageing. 2011;40(3):297-306. PubMed CrossRef
48. Orgeta V, Qazi A, Spector AE, et al. Psychological treatments for depression and anxiety in dementia and mild cognitive impairment. Cochrane Database Syst Rev. 2014;1(1):CD009125. PubMed
49. Bains J, Birks J, Dening T. Antidepressants for treating depression in dementia. Cochrane Database Syst Rev. 2002;(4):CD003944. PubMed
50. Gonçalves DC, Byrne GJ. Interventions for generalized anxiety disorder in older adults: systematic review and meta-analysis. J Anxiety Disord. 2012;26(1):1-11. PubMed CrossRef
51. Garakani A, Murrough J, Iosifescu DV. Advances in psychopharmacology for anxiety disorders. Focus. 2014;14(2):152-162. CrossRef
52. Alamy S, Wei Zhang, Varia I, et al. Escitalopram in specific phobia: results of a placebo-controlled pilot trial. J Psychopharmacol. 2008;22(2):157-161. PubMed CrossRef
53. Baldwin D, Bobes J, Stein DJ, et al; Paroxetine Study Group. Paroxetine in social phobia/social anxiety disorder: randomised, double-blind, placebo-controlled study. Br J Psychiatry. 1999;175(02):120-126. PubMed CrossRef
54. Benjamin J, Ben-Zion IZ, Karbofsky E, et al. Double-blind placebo-controlled pilot study of paroxetine for specific phobia. Psychopharmacology (Berl). 2000;149(2):194-196. PubMed CrossRef
55. Masdrakis VG, Papadimitriou GN, Oulis P. Lamotrigine administration in panic disorder with agoraphobia. Clin Neuropharmacol. 2010;33(3):126-128. PubMed CrossRef
56. Davis M, Ressler K, Rothbaum BO, et al. Effects of D-cycloserine on extinction: translation from preclinical to clinical work. Biol Psychiatry. 2006;60(4):369-375. PubMed CrossRef
57. Nave AM, Tolin DF, Stevens MC. Exposure therapy, D-cycloserine, and functional magnetic resonance imaging in patients with snake phobia: a randomized pilot study. J Clin Psychiatry. 2012;73(9):1179-1186. PubMed CrossRef
58. Wilhelm FH, Roth WT. Acute and delayedeffects of alprazolam on flight phobics during exposure. Behav Res Ther. 1997;35(9):831-841. PubMed CrossRef
59. Alessi-Severini S, Bolton JM, Enns MW, et al. Sustained use of benzodiazepines and escalation to high doses in a Canadian population. Psychiatr Serv. 2016;67(9):1012-1018. PubMed CrossRef
60. Dunlop BW, Davis PG. Combination treatment with benzodiazepines and SSRIs for comorbid anxiety and depression: a review. Prim Care Companion J Clin Psychiatry. 2008;10(3):222-228. PubMed CrossRef
61. Hallfors DD, Saxe L. The dependence potential of short half-life benzodiazepines: a meta-analysis. Am J Public Health. 1993;83(9):1300-1304. PubMed CrossRef
62. Wang PS, Bohn RL, Glynn RJ, et al. Hazardous benzodiazepine regimens in the elderly: effects of half-life, dosage, and duration on risk of hip fracture. Am J Psychiatry. 2001;158(6):892-898. PubMed CrossRef
63. D×az-Gutiérrez MJ, Mart×nez-Cengotitabengoa M, Sáez de Adana E, et al. Relationship between the use of benzodiazepines and falls in older adults: a systematic review. Maturitas. 2017;101:17-22. PubMed CrossRef
64. Griffin CE 3rd, Kaye AM, Bueno FR, et al. Benzodiazepine pharmacology and central nervous system-mediated effects. Ochsner J. 2013;13(2):214-223. PubMed
Enjoy this premium PDF as part of your membership benefits!