Objective: To describe the effect of a multimodal intervention targeting chronic benzodiazepine and sedative-hypnotic prescriptions in a large behavioral health system.
Methods: This retrospective study analyzed chronic sedative-hypnotic prescription rates in patients seeking mental health services in a large behavioral health system. The multimodal intervention consisted of provider education, coordination of care with all providers involved in patient care, and guideline development and implementation for safe prescribing of sedative-hypnotics. Three time periods were analyzed: preintervention (October 2013-December 2013), 12-month assessment (October 2014-December 2014), and 24-month assessment (October 2015-December 2015). The primary outcome of the study was the change in frequency of chronic (≥ 60 days) sedative-hypnotic prescriptions received before and after the multimodal intervention. The secondary outcome included the change in prescription rates in a priori-defined cohorts: patients on methadone maintenance therapy and patients ≥ 60 years of age.
Results: There were 32,944 prescriptions during the study period. The rate of chronic sedative-hypnotic prescriptions decreased from 1,764 (15.3%) to 1,634 (14.9%) to 1,018 (9.8%) between the 3 assessment periods, respectively. A significant decrease occurred between the preintervention period and 24-month assessment (5.5%, P < .0001) and between the 12-month assessment and the 24-month assessment (5.1%, P < .0001). In the elderly, prescription rates decreased significantly between the preintervention period and the 24-month assessment (3.6%, P < .0001) and the 12-month and 24-month assessments (3.2%, P = .0001). In patients in methadone maintenance programs, rates of concomitant chronic sedative-hypnotic prescriptions decreased significantly between all assessment periods: preintervention and 12-month assessment (8.2%, P = .001), 12-month and 24-month assessment (6.3%, P = .002), and preintervention and 24-month assessment (14.5%, P < .0001). Additionally, prescription rates increased significantly for antidepressants (4.1%, P < .05), hydroxyzine (1.1%, P = .01), buspirone (2.1%, P < .05), gabapentin (6.3%, P < .05), and melatonin agonists (0.3%, P < .05) between the preintervention and 24-month assessment periods.
Conclusions: Implementation of a multimodal intervention led to a significant decrease in rates of chronic sedative-hypnotic prescriptions in a large behavioral health system.
Evaluation of the Impact of a Multimodel Intervention on Prescribing Patterns of Sedative-Hypnotics in a Behavioral Health System

ABSTRACT
Objective: To describe the effect of a multimodal intervention targeting chronic benzodiazepine and sedative-hypnotic prescriptions in a large behavioral health system.
Methods: This retrospective study analyzed chronic sedative-hypnotic prescription rates in patients seeking mental health services in a large behavioral health system. The multimodal intervention consisted of provider education, coordination of care with all providers involved in patient care, and guideline development and implementation for safe prescribing of sedative-hypnotics. Three time periods were analyzed: preintervention (October 2013-December 2013), 12-month assessment (October 2014-December 2014), and 24-month assessment (October 2015-December 2015). The primary outcome of the study was the change in frequency of chronic (≥ 60 days) sedative-hypnotic prescriptions received before and after the multimodal intervention. The secondary outcome included the change in prescription rates in a priori-defined cohorts: patients on methadone maintenance therapy and patients ≥ 60 years of age.
Results: There were 32,944 prescriptions during the study period. The rate of chronic sedative-hypnotic prescriptions decreased from 1,764 (15.3%) to 1,634 (14.9%) to 1,018 (9.8%) between the 3 assessment periods, respectively. A significant decrease occurred between the preintervention period and 24-month assessment (5.5%, P < .0001) and between the 12-month assessment and the 24-month assessment (5.1%, P < .0001). In the elderly, prescription rates decreased significantly between the preintervention period and the 24-month assessment (3.6%, P < .0001) and the 12-month and 24-month assessments (3.2%, P = .0001). In patients in methadone maintenance programs, rates of concomitant chronic sedative-hypnotic prescriptions decreased significantly between all assessment periods: preintervention and 12-month assessment (8.2%, P = .001), 12-month and 24-month assessment (6.3%, P = .002), and preintervention and 24-month assessment (14.5%, P < .0001). Additionally, prescription rates increased significantly for antidepressants (4.1%, P < .05), hydroxyzine (1.1%, P = .01), buspirone (2.1%, P < .05), gabapentin (6.3%, P < .05), and melatonin agonists (0.3%, P < .05) between the preintervention and 24-month assessment periods.
Conclusions: Implementation of a multimodal intervention led to a significant decrease in rates of chronic sedative-hypnotic prescriptions in a large behavioral health system.
Prim Care Companion CNS Disord 2018;20(3):18m02269
To cite: Avdagic K, Geier M, Coralic Z, et al. Evaluation of the impact of a multimodel intervention on prescribing patterns of sedative-hypnotics in a behavioral health system. Prim Care Companion CNS Disord. 2018;20(3):18m02269.
To share: https://doi.org/10.4088/PCC.18m02269
© Copyright 2018 Physicians Postgraduate Press, Inc.
aDepartment of Pharmacy, University of California San Francisco, San Francisco, California
bSan Francisco Department of Public Health, San Francisco, California
cDepartment of Clinical Pharmacy, University of California San Francisco, San Francisco, California
*Corresponding author: Korana Avdagic, PharmD, Department of Pharmacy, University of California San Francisco, 505 Parnassus, San Francisco, CA 94147 ([email protected]).
The Centers for Disease Control (CDC) reports that the majority of drug overdose deaths are related to prescription medications.1 In the United States, drug overdose deaths have surpassed motor vehicle accidents as the leading cause of unintentional death. Opioids are the most common medication class involved; however, sedative-hypnotics are the most frequent concomitant medications found among opioid overdose deaths.2 In the United States, benzodiazepines were involved in 6,497 fatal overdoses in a 2010 report.3 In addition to increased risk of death, the sedative-hypnotics (including the "Z" drugs such as zolpidem and zaleplon) may increase the risk of motor vehicle collisions by up to 60%.4-6 Additionally, in methadone maintenance programs, patients who are chronic users of benzodiazepines are more likely to overdose, to start prescription opioids, and to test positive for cocaine or other opioids on drug urine screens than occasional and nonusers.7 In patients over 65 years of age, sedative-hypnotic use is associated with a high risk of fractures and falls.8 Patients taking sedative-hypnotics are 4.5 times more likely to die of any cause compared to those not taking a sedative-hypnotic.9
Sedative-hypnotics are frequently used in treatment of anxiety and insomnia, which are common and often chronic disorders. Insomnia is strongly associated with major depressive disorder and anxiety disorders in adults.10,11 Experts generally advise against long-term sedative-hypnotic use due to concerns of side effects including residual sedative effects, memory impairment, decreased cognitive functioning, respiratory depression, rebound insomnia, falls, medication abuse, dependency, withdrawal, and potentially increased risk of death.12
Currently, there are no comprehensive guidelines for sedative-hypnotic use in patients with mental illness. The fifth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5)13 allows for a diagnosis of insomnia disorder independent of, or in addition to, concomitant psychiatric or medical disorders.
In January 2014, recognizing the risk of chronic sedative-hypnotic use, the San Francisco Department of Public Health Community Behavioral Health Services (CBHS) decided to implement a multimodal intervention to decrease chronic sedative-hypnotic prescriptions. This study will analyze the impact of the multimodal intervention on CBHS sedative-hypnotic prescribing practices.
METHODS
Design
This was a retrospective cohort study designed to evaluate the impact of a multimodal intervention14 on prescribing patterns of chronic sedative-hypnotic medications in the CBHS general patient population. The chronic sedative-hypnotic medications included benzodiazepines and Z-drugs (Table 1). The primary outcome of the study was the change in frequency of chronic (≥ 60 days) sedative-hypnotic prescriptions received before and after the multimodal intervention. Two high-risk patient populations were identified a priori for subanalysis: the elderly (≥ 60 years) and patients on methadone maintenance. Additionally, we collected data on sex, race, mental health diagnoses, and alternative medications (antidepressants, diphenhydramine, hydroxyzine, buspirone, gabapentin, and melatonin agonists). The study was classified exempt by the University of California San Francisco Committee on Human Research.
Setting
CBHS provides community behavioral health services in San Francisco County. CBHS is supported by the San Francisco Department of Public Health and consists of clinics with 1,706 providers covering a wide array of mental health services. The providers include psychiatrists, therapists, pharmacists, case managers, and other health care providers. As of 2016, CBHS consists of 202 clinics or programs providing mental health services to 19,090 patients annually. CBHS is the only system providing comprehensive mental health services to the underserved and underinsured population in the county of San Francisco.
Multimodal Intervention
The study consisted of 3 time periods: October 2013-December 2013 (preintervention period), October 2014-December 2014 (12-month assessment period), and October 2015-December 2015 (24-month assessment period). Briefly, the multimodal intervention consisted of provider education, coordination of care with all providers involved in patient care, and guideline development and implementation for safe prescribing of sedative-hypnotics. The implementation timeline and details of the multimodal intervention are shown in Table 2.

- Currently, there are no comprehensive guidelines for sedative-hypnotic use in patients with mental illness.
- Patients taking sedative-hypnotics are more likely to suffer from adverse drug events, including death, compared to patients not taking sedative-hypnotics.
- A simple low-cost educational intervention may significantly reduce overall prescription rates of sedative-hypnotics in a large behavioral health system.
Participants
The study population consisted of all active adult patients (≥ 18 years of age) with diagnosed mental illness who had billed services in the CBHS electronic health record during the preintervention and assessment periods. The exclusion criteria included patients using private provider networks or crisis stabilization services, hospitalization, and patients in long-term care facilities. At CBHS, patients < 18 years of age account for < 1% of total prescriptions and thus were excluded from the study.
Data Analysis
CBHS utilizes e-prescribing software, Infoscriber, which enables tracking of the prevalence of prescriptions. The data on eligible active patients receiving mental health services billed in the electronic health record were extracted from the Avatar Data Warehouse system. For the primary outcome, we calculated the data on chronic sedative-hypnotic prescribing percentages (number of patients with sedative-hypnotic prescriptions for ≥ 60 days in a 90-day quarter divided by number of patients with a mental health service billed within a 90-day quarter). The descriptive statistics were calculated using proportions, means or medians, interquartile ranges, and pairwise tests as appropriate. The change in prescribing frequency was analyzed using the χ2 test.
RESULTS
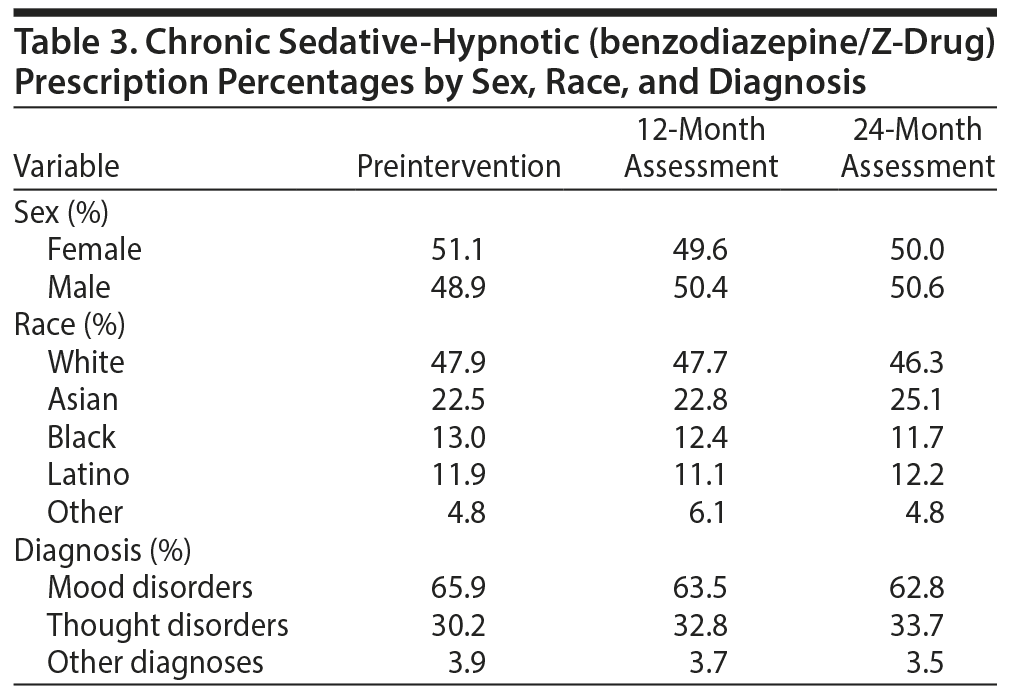
A total of 32,944 prescriptions were analyzed (11,512 in the preintervention period, 11,003 in the 12-month assessment, and 10,429 in the 24-month assessment). There was no difference in the rate of chronic sedative-hypnotic prescriptions between patients’ sex, race, or mental health diagnoses across the 3 assessment periods (Table 3).
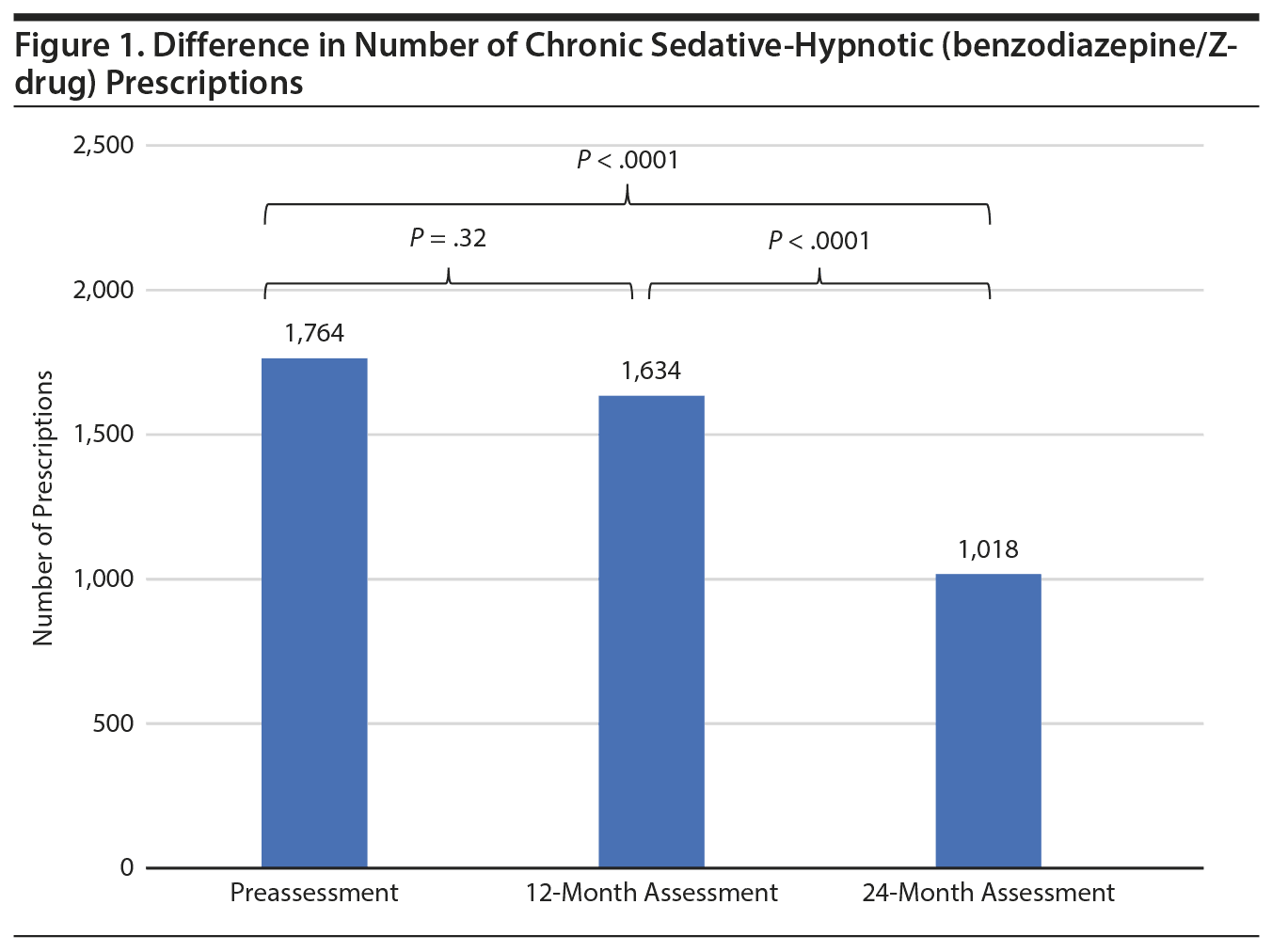
For the primary outcome, the rate of chronic sedative-hypnotic prescriptions decreased from 1,764 (15.3%) to 1,634 (14.9%) to 1,018 (9.8%) between the assessment periods, respectively. The difference between the preintervention period and the 12-month assessment was not statistically significant (absolute decrease of 0.4%, P = .32). However, there were significant decreases between the preintervention period and 24-month assessment (absolute decrease of 5.5%, P < .0001) and between the 12-month assessment and the 24-month assessment (absolute decrease of 5.1%, P < .0001) (Figure 1).
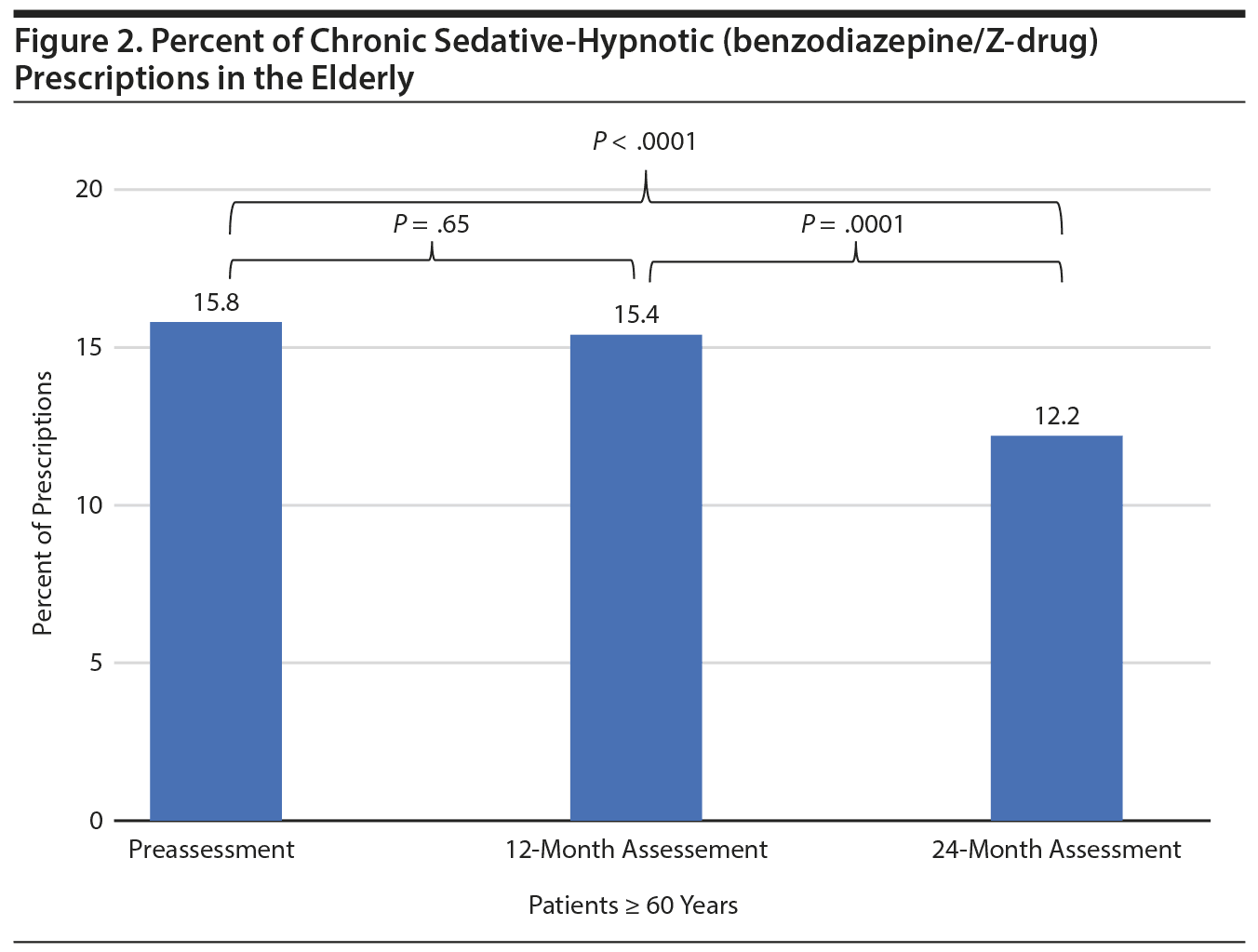
Similar decreases of rates of chronic sedative-hypnotic prescriptions were also seen in the 2 high-risk patient cohorts. There were a total of 8,643 prescriptions for patients who were ≥ 60 years of age (2,818, 2,989, and 2,836 in the assessment periods, respectively). In the elderly, prescription rates decreased significantly between the preintervention period and the 24-month assessment (absolute decrease of 3.6%, P < .0001) and between the 12-month and 24-month assessments (absolute decrease of 3.2%, P = .0001). A trend toward decreasing prescriptions was seen between the preintervention period and the 12-month assessment; however, the difference remained nonsignificant (Figure 2).
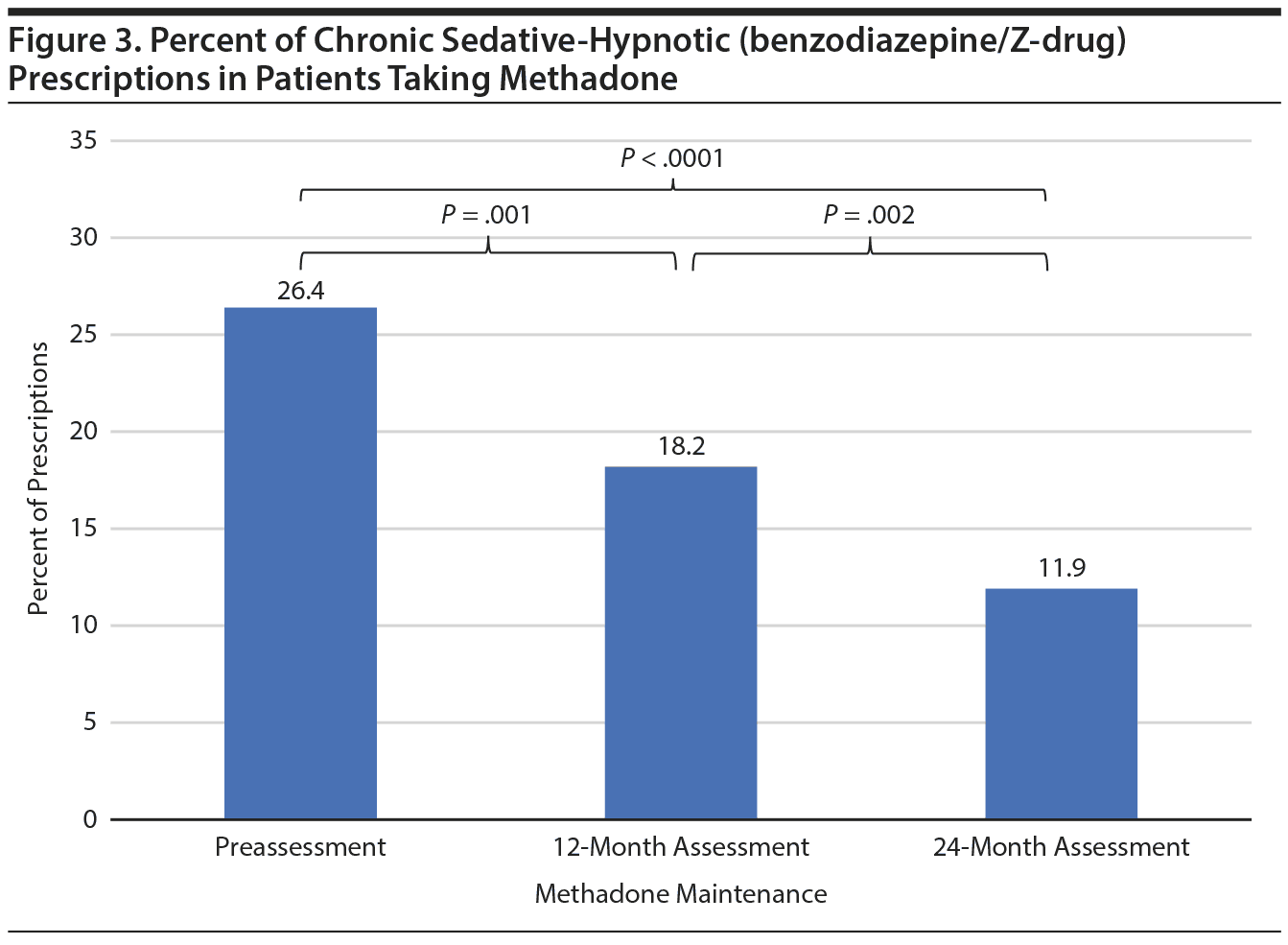
Further, there were a total of 1,732 prescriptions for methadone (531, 628, and 573 in the assessment periods, respectively). There was a significant decrease in the rates of concomitant chronic sedative-hypnotic prescriptions between all assessment periods: preintervention and 12-month assessment (absolute decrease of 8.2%, P = .001), 12-month and 24-month assessment (absolute decrease of 6.3%, P = .002), and preintervention and 24-month assessment (absolute decrease of 14.5%, P < .0001) (Figure 3).
There were significant differences in the rate of prescriptions in the alternative medications across the 3 assessment periods. In general, there was a statistically significant increase between the preintervention and 24-month assessment period in prescriptions for antidepressants (absolute increase of 4.1%, P < .05), hydroxyzine (absolute increase of 1.1%, P = .01), buspirone (absolute increase of 2.1%, P < .05), gabapentin (absolute increase of 6.3%, P < .05), and melatonin agonists (absolute increase of 0.3%, P < .05). There was no significant difference in diphenhydramine prescriptions (absolute difference of 0.5%, P = .27)
DISCUSSION
The implementation of a multimodal intervention at CBHS was associated with a statistically significant decrease in prescription rates of chronic sedative-hypnotics. Our study is unique, as we show a relatively simple low-cost educational intervention resulting in a significant positive practice change on a health system level. Although this study was not designed to assess adverse drug events and mortality reduction, we believe that a more conscientious approach to sedative-hypnotic prescribing, especially in high-risk patients, may result in overall harm reduction.
A systemic change in practice is a difficult challenge. Our intervention was multimodal and rolled out with sequential interventions. Correlatively, our results show that the impact of the intervention was not immediate and that the greatest results were seen between the preintervention and 24-month assessments. The 12-month assessment showed a trend in the decrease of sedative-hypnotic prescriptions but did not reach statistical significance. We speculate that this finding may reflect a "learning curve" and a gradual acceptance of the intervention by prescribers. Another explanation may be that, initially, patients and prescribers may be reluctant to discontinue chronic medications for which patients have no complaints.
Our subanalysis shows that the frequency of prescribing sedative-hypnotics was reduced in the elderly. The elderly are more sensitive to the effects of sedative-hypnotics than younger adults. Sedative-hypnotics should be generally avoided in older patients due to the increased risk of adverse effects such as delirium, cognitive impairment, falls, and hip fractures. The American Geriatrics Society 2015 Beers Criteria15 for potentially inappropriate medication use in older adults discourages the use of sedative-hypnotics in this patient population.
The most dramatic effect on prescribing of chronic sedative-hypnotics was seen in patients on methadone maintenance therapy. These results are encouraging, as use of sedative-hypnotics in patients taking methadone is associated with poorer treatment outcomes and a potential for significant drug-drug interactions.16,17 One part of the multimodal intervention was presentation of mortality data to prescribers. Of CBHS patients who died between 2010 and 2011, 25% were in a methadone maintenance program. In addition, a number of patient suicides were noted in our patients taking methadone and benzodiazepines. In 14 of the 55 reported deaths, accidental overdose with methadone was the cause or contributing factor to death. Of this group, 8 used methadone long term and had sedative-hypnotics present during postmortem toxicologic screening. Knowledge of mortality data by prescribers may have had a large impact in changing prescribing practices.
Our results indicate that there was an increase in prescription rates for antidepressants, hydroxyzine, buspirone, gabapentin, and melatonin agonists. This increase is most likely a result of providers attempting to treat patients with alternatives to sedative-hypnotics. In general practice, anxiety and insomnia disorders are commonly treated with benzodiazepines and sedative-hypnotics. However, selective serotonin reuptake inhibitors and serotonin-norepinephrine reuptake inhibitors are considered first-line pharmacologic treatment for anxiety disorders.18 For insomnia, current guidelines19 recommend nonpharmacologic measures, such as improved sleep hygiene or psychotherapy, as first-line therapy. Practice changes after the multimodal intervention are more consistent with evidence-based approaches to insomnia and anxiety.
There are limitations to our study. We were unable to follow the same cohort of patients in the preintervention and postintervention periods and relied on total prescriptions rather than individual patient practices. We were unable to assess patients’ adherence to medications, only that they were prescribed a sedative-hypnotic and received the dispensed medication. Also, since our data are derived from the electronic health record unique to CBHS, we are unable to say if a client was prescribed a sedative-hypnotic from another provider (eg, primary care). We also did not evaluate the trend in dosage, which might reveal if patients were tapered from the medications during the assessment periods. We are unable to differentiate if the increase in alternate medications is a result of direct substitution for sedative-hypnotics (eg, hydroxyzine replacing zolpidem) or a cross-taper to switch patients to a nonsedative-hypnotic agent. We are unsure of the impact of each part of the multimodal intervention, and it is very likely that the sum of all the parts of the intervention led to the decrease in inappropriate prescribing. Finally, a common criticism of pre- and poststudies is uncertainty of sustainability of the studied intervention; however, our study covers 3 years of data and shows a consistent reduction of prescriptions for sedative-hypnotics. Additionally, continued compliance will be addressed with future studies and quality improvement initiatives. Our patient cohort represents a large number of underserved or underinsured patients from a single county, and generalization of our results should be done with caution.
Submitted: January 4, 2018; accepted March 13, 2018.
Published online: May 31, 2018.
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1. Deaths From Prescription Opioid Overdose. CDC.gov website. http://www.cdc.gov/drugoverdose/data/overdose.html. Accessed May 7, 2018.
2. Hall AJ, Logan JE, Toblin RL, et al. Patterns of abuse among unintentional pharmaceutical overdose fatalities. JAMA. 2008;300(22):2613-2620. PubMed CrossRef
3. Jones CM, Mack KA, Paulozzi LJ. Pharmaceutical overdose deaths, United States, 2010. JAMA. 2013;309(7):657-659. PubMed CrossRef
4. Ravera S, van Rein N, de Gier JJ, et al. Road traffic accidents and psychotropic medication use in The Netherlands: a case-control study. Br J Clin Pharmacol. 2011;72(3):505-513. PubMed CrossRef
5. Orriols L, Philip P, Moore N, et al. Benzodiazepine-like hypnotics and the associated risk of road traffic accidents. Clin Pharmacol Ther. 2011;89(4):595-601. PubMed CrossRef
6. Gustavsen I, Bramness JG, Skurtveit S, et al. Road traffic accident risk related to prescriptions of the hypnotics zopiclone, zolpidem, flunitrazepam and nitrazepam. Sleep Med. 2008;9(8):818-822. PubMed CrossRef
7. Brands B, Blake J, Marsh DC, et al. The impact of benzodiazepine use on methadone maintenance treatment outcomes. J Addict Dis. 2008;27(3):37-48. PubMed CrossRef
8. Nurminen J, Puustinen J, Piirtola M, et al. Opioids, antiepileptic and anticholinergic drugs and the risk of fractures in patients 65 years of age and older: a prospective population-based study. Age Ageing. 2013;42(3):318-324. PubMed CrossRef
9. Weich S, Pearce HL, Croft P, et al. Effect of anxiolytic and hypnotic drug prescriptions on mortality hazards: retrospective cohort study. BMJ. 2014;348:g1996. PubMed CrossRef
10. Ford DE, Kamerow DB. Epidemiologic study of sleep disturbances and psychiatric disorders. an opportunity for prevention? JAMA. 1989;262(11):1479-1484. PubMed CrossRef
11. Mellinger GD, Balter MB, Uhlenhuth EH. Insomnia and its treatment. Prevalence and correlates. Arch Gen Psychiatry. 1985;42(3):225-232. PubMed CrossRef
12. Kramer M. Hypnotic medication in the treatment of chronic insomnia: non nocere! doesn’ t anyone care? Sleep Med Rev. 2000;4(6):529-541. PubMed CrossRef
13. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
14. Guideline to Promote Prescription Safety of Sedative-Hypnotics for CBHS Clients. 2014. San Francisco Department of Health website. https://www.sfdph.org/dph/files/CBHSdocs/Sedative-Hypnotic-Guideline.pdf. Accessed May 7, 2018.
15. American Geriatrics Society Beers Criteria Update Expert Panel. American Geriatrics Society 2015 Updated Beers Criteria for potentially inappropriate medication use in older adults. J Am Geriatr Soc. 2015;63(11):2227-2246. PubMed CrossRef
16. Backmund M, Meyer K, Henkel C, et al. Co-consumption of benzodiazepines in heroin users, methadone-substituted and codeine-substituted patients. J Addict Dis. 2005;24(4):17-29. PubMed CrossRef
17. Brands B, Blake J, Marsh D. Impact of methadone program philosophy changes on early treatment outcomes. J Addict Dis. 2003;22(3):19-38. PubMed CrossRef
18. Bandelow B, Sher L, Bunevicius R, et al. Guidelines for the pharmacological treatment of anxiety disorders, obsessive-compulsive disorder and posttraumatic stress disorder in primary care. Int J Psychiatry Clin Pract. 2012;16(2):77-84. PubMed CrossRef
19. Schutte-Rodin S, Broch L, Buysse D, et al. Clinical guideline for the evaluation and management of chronic insomnia in adults. J Clin Sleep Med. 2008;4(5):487-504. PubMed
Enjoy this premium PDF as part of your membership benefits!