Objective: To determine the pattern of care sought in cases of psychiatric emergency before presentation to a tertiary health care center.
Method: Consecutive recruitment of 180 emergency psychiatric cases, which comprised a total of 156 patients, presenting to the accident and emergency unit of the University of Benin Teaching Hospital (UBTH), Edo State, Nigeria, was conducted from June 2008 to January 2009. A structured instrument was used to gather the patients’ information including their sociodemographic characteristics, their care before presentation, and the relations accompanying them to the hospital.
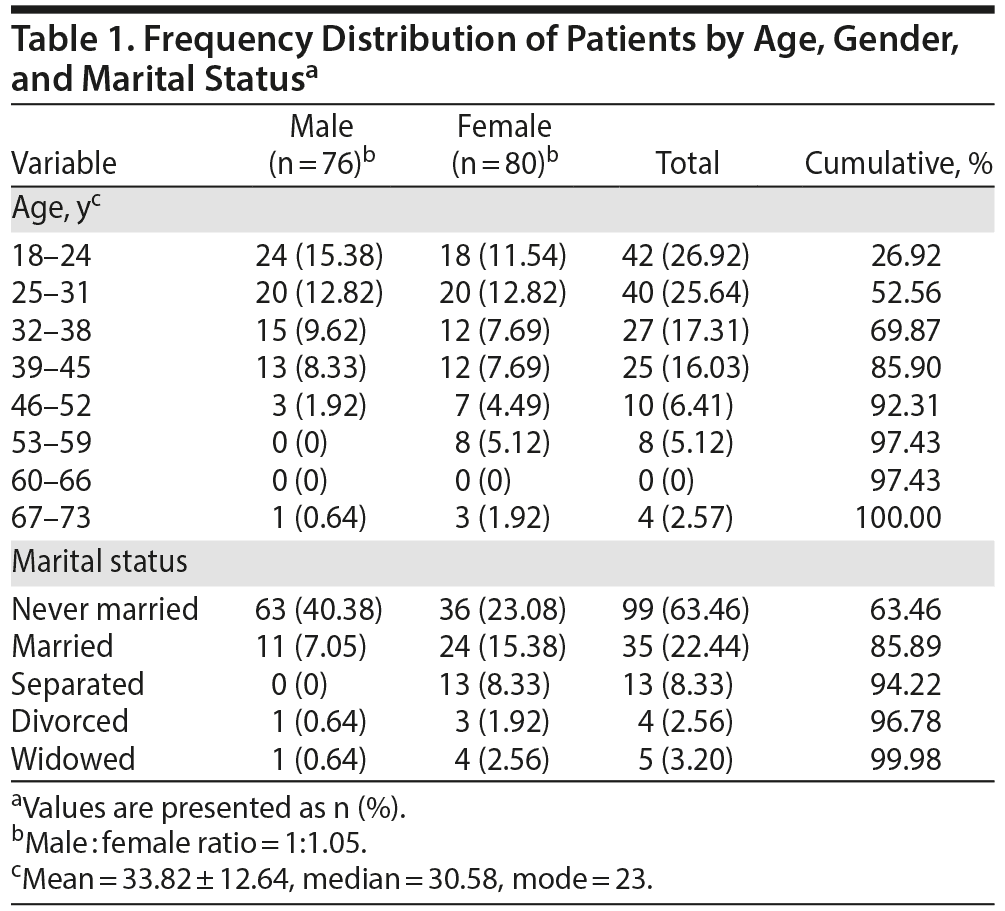
Results: The mean ± SD patient age was 33.82 ± 12.64 years, with an age range of 18-73 years and a modal age of 23 years. The male to female ratio was 1:1.05. Of the patients, 121 (77.6%) were not married, while 35 (22.4%) were married. Most identified as Christian (96.2%). The majority of the patients (70.0%) presented to the hospital through self-referral. Eighty (44.4%) of the patients had not sought any treatment before coming to UBTH. Forty-seven patients (26.1%) had sought care in churches, 39 (21.7%) had sought treatment in other hospitals, and 12 (6.7%) had sought traditional care before presenting to UBTH. Seventy-four patients (41.1%) were accompanied by parents and 44 (24.4%) were accompanied by siblings, while the spouse accompanied 23 (12.8%) patients.
Conclusions: Most patients with psychiatric emergencies at UBTH prefer to present directly to the tertiary health care center in Benin City, and they are usually supported by their immediate family members.
Pattern of Care Before Presentation Among the Psychiatric Emergency Cases at a Tertiary Health Care Center in Nigeria

ABSTRACT
Objective: To determine the pattern of care sought in cases of psychiatric emergency before presentation to a tertiary health care center.
Method: Consecutive recruitment of 180 emergency psychiatric cases, which comprised a total of 156 patients, presenting to the accident and emergency unit of the University of Benin Teaching Hospital (UBTH), Edo State, Nigeria, was conducted from June 2008 to January 2009. A structured instrument was used to gather the patients’ information including their sociodemographic characteristics, their care before presentation, and the relations accompanying them to the hospital.
Results: The mean ± SD patient age was 33.82 ± 12.64 years, with an age range of 18-73 years and a modal age of 23 years. The male to female ratio was 1:1.05. Of the patients, 121 (77.6%) were not married, while 35 (22.4%) were married. Most identified as Christian (96.2%). The majority of the patients (70.0%) presented to the hospital through self-referral. Eighty (44.4%) of the patients had not sought any treatment before coming to UBTH. Forty-seven patients (26.1%) had sought care in churches, 39 (21.7%) had sought treatment in other hospitals, and 12 (6.7%) had sought traditional care before presenting to UBTH. Seventy-four patients (41.1%) were accompanied by parents and 44 (24.4%) were accompanied by siblings, while the spouse accompanied 23 (12.8%) patients.
Conclusions: Most patients with psychiatric emergencies at UBTH prefer to present directly to the tertiary health care center in Benin City, and they are usually supported by their immediate family members.
Prim Care Companion CNS Disord 2016;18(2):doi:10.4088/PCC.15m01817
© Copyright 2016 Physicians Postgraduate Press, Inc.
aDepartment of Mental Health, University of Benin Teaching Hospital, Benin City, Nigeria
bDepartment of Child Health, University of Benin Teaching Hospital, Benin City, Nigeria
*Corresponding author: Israel Odunmayowa Aina, FWACP, Department of Mental Health, PMB 1111, Benin City, Edo State, Nigeria ([email protected]).
Psychiatric emergencies are common in health care facilities that provide mental health services. These psychiatric emergencies are cases of acute disturbance of thought, mood, behavior, and social relationship that require an immediate intervention as defined by the patient, family, or community.1 Thus, the patient and his or her significant others determine what constitutes an emergency, as well as the amount and type of attention to be given to the patient before presenting to the hospital. If the required medical attention is not provided, the patient as well as those close to the patient, including the surrounding property, may be endangered.2 The reason for selecting a particular kind of care has been attributed to the concept and attitude related to the cause of the illness by the patient and family members.3 It has been documented that when orthodox mental health services are available to manage psychiatric emergencies, they are underutilized due to several constraints such as being distantly located or attached with stigma.4 Hence, many people with mental illness may seek other forms of care before presenting to the hospital. Thus, it is important to understand what forms of treatment patients with psychiatric emergencies access before presentation to the hospital and to identify the significant others (eg, relatives, friends) who might have contributed to this decision.
METHOD
This study was carried out in the accident and emergency unit of the University of Benin Teaching Hospital, Benin City, Edo State, Nigeria (UBTH). The patients were selected consecutively as they presented to the unit over a period of 8 months (June 2008 to January 2009). The unit takes care of all medical and surgical emergencies from Benin City and the surrounding area. The hospital has a 20-bed capacity and provides emergency care 24 hours per day. Ethical approval for this study was obtained from the research and ethics committee of the hospital. Informed verbal consent was obtained from each patient or the relatives who accompanied the patient to the hospital when he or she was too ill to give consent.
A structured mental health instrument was used by the resident doctor on call to gather the relevant information. Training sessions were held to familiarize the residents with the use of the instrument. The information obtained comprised the sociodemographic characteristics of the patient, the alternative sources of care sought before hospital presentation, and the name of the person who accompanied the patient to the hospital. The data obtained were analyzed using the Statistical Package for Social Sciences version 13 (SPSS Inc, Chicago, Illinois).
RESULTS
A total of 156 patients accounted for 180 cases of psychiatric emergencies seen over the 8-month study period. Of the 156 patients, 137 made single presentations, 14 presented twice, and 5 presented 3 times. The mean ± SD age of the patients was 33.82 ± 12.64 years (range, 18-73 years, with a modal age of 23 years). Of the patients, 52.6% were aged ≤ 31 years, while 69.9% were aged ≤ 38 years (Table 1). The patients included 76 (48.7%) men and 80 (51.3%) women. The male:female ratio was 1:1.05. There was no statistically significant difference between the number of men and women presenting to UBTH with psychiatric emergencies (χ21=0.103, P = .749).

- Over time, more patients are becoming aware of the availability of medical care for psychiatric emergencies at tertiary health care centers; thus, patients are starting to present directly to tertiary care rather than primary care.
- There is a need to strengthen primary health care services in the environments in which they have not been effective to avoid overburdening the tertiary health care centers.
In terms of marital status, 99 patients (63.5%) who were never married constituted the largest group. There were 35 (22.4%) married patients. The patients who were not married (n = 121, 77.6%) included those who were never married and those who were separated, widowed, or divorced. There was a statistically significant difference between the number of emergency consultations for married patients compared to those who were not married (χ21=47.410, P = .000).
The marital status of patients matched by gender is shown in Table 1. The never-married group consisted of 63.6% men and 36.6% women. The married patients comprised 31.4% men and 68.6% women. Thirteen women were separated compared to none of the men. Of the divorced patients, 25.0% were men compared to 75.0% women. The male patients made up 20.0% of the widowed patients, while women made up 80.0%.
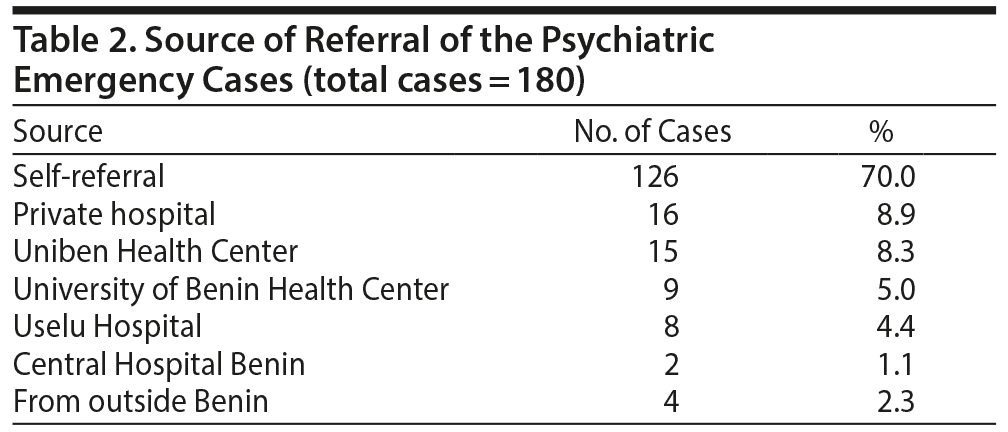
The majority of the psychiatric emergency cases were self-referral (126 accounting for 70.0% of the cases). Private hospitals were the sources of referral for 16 cases (8.9%). These private hospitals are smaller hospitals within an hour’s drive of UBTH. Of note is that 8.3% of the referrals were from the University of Benin Health Center, which is the school health center for the University of Benin. It is within a 10-minute drive from UBTH and can also be considered a smaller urban health care center. Other units of UBTH, such as the general practice clinic, accounted for 5% of the referrals. The general practice clinic is located within UBTH and takes care of all nonemergency cases that do not require emergency or specialist care. However, when the attending physician at the general practice clinic comes across a psychiatric case that requires urgent attention, such a patient is referred immediately to the psychiatric emergency unit of the hospital. Other referral centers such as the Uselu Hospital and the Central Hospital are urban hospitals that are within an hour’s drive of UBTH (Table 2).
Eighty patients (44.4%) had not sought care at any other place before presenting to UBTH. The next largest group of patients, 47 (26.1%), had sought care in a church before presentation, and 6.7% had sought traditional care (eg, traditional healing homes where herbs are used for treatment) before presentation (Table 3).
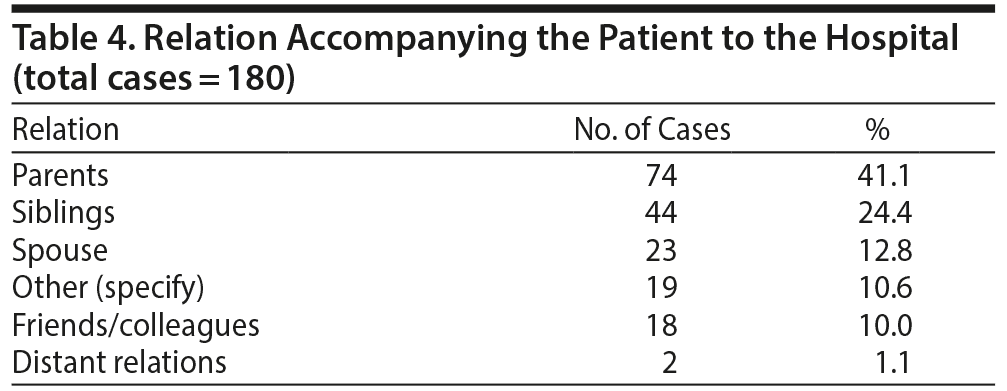
The study showed that 74 (41.1%) of the patients were accompanied by parents, while 24.4% were accompanied by siblings. A spouse accompanied the patient in 12.8% of the cases (Table 4). These immediate family members (parents, siblings, and spouses) accounted for 78.3% of the relations accompanying the patient to the hospital in the cases of psychiatric emergency.
DISCUSSION
This study revealed that, among the various forms of alternative treatment sought before presentation at UBTH, the group of patients who had not obtained any other form of treatment was the largest (44.4%). This finding is different from a study5 in Eastern Europe, which found that only 16% of patients presented directly to the psychiatric service. Gater et al5 noted that in another part of Eastern Europe, 38% of patients presented directly to the psychiatric service.
Our study also revealed that 21.7% of the patients came from other hospitals (including general practitioners in clinics or primary care offices). However, in the study by Gater et al,5 the larger group of patients (62%) were referred by general practitioners.
Most studies have quoted a relatively lower percentage of patients presenting directly to the psychiatric service.6,7 Most of the patients presented first to a general practitioner. In a study6 from the United Kingdom, 60% of the patients were referred by general practitioners, while self-referral was found in only 4% of the patients. In a community-based mental health system in South Verona, Italy, it was reported that the most common route to mental health service is via a general practitioner (40%), followed by a referral from a hospital doctor (26%) and self-referral (23%).7
The UBTH experience showed that the larger group of patients (44.4%) had not obtained any form of treatment before presentation to the emergency unit. This finding may be accounted for by the fact that UBTH also serves as a primary health care provider under the national health insurance scheme. Thus, the psychiatric emergency unit of the hospital becomes a major entry point for patients seeking mental health services.8
The churches were the alternative source of care sought before hospital presentation at UBTH in 26.1% of cases in this study. This finding reflects the predominant religion in this region. Christianity was the predominant religion found in 96.2% of the patients in this study. The common belief that mental illness has some spiritual causation also may explain why some of the patients tend to visit the churches before coming to the hospital.
The larger group of patients had parents accompanying them to the hospital to seek treatment. This finding may be a reflection of the predominance of young adults among the patients presenting with psychiatric emergencies. Patients aged ≤ 38 years made up a cumulative total of 69.9%. Another reason for this finding could be that most psychiatric conditions have their onset in the young adult age group. On the whole, the immediate family members were more represented as the relations accompanying the patients to the hospital. This finding may be a reflection of the possible cohesive and caring nature of the family unit of the mentally ill presenting in an emergency to this unit.
CONCLUSION
The majority of the patients had not received any form of care before presentation to UBTH. This finding suggests that there is a good level of awareness among the general population in Benin City and the surrounding area of the availability of medical treatment for psychiatric emergencies. The immediate family members of the patients demonstrated a good level of support by accompanying the patients in the majority of cases.
Submitted: April 2, 2015; accepted August 6, 2015.
Published online: April 21, 2016.
Potential conflicts of interest: None.
Funding/support: None.
Acknowledgment: The assistance of the resident doctors in the Department of Mental Health, University of Benin Teaching Hospital, Benin City, Nigeria, is acknowledged in the data-gathering process.
REFERENCES
1. Allen MH, Carpenter D, Sheets JL, et al. What do consumers say they want and need during a psychiatric emergency? J Psychiatr Pract. 2003;9(1):39-58. PubMed doi:10.1097/00131746-200301000-00005
2. Shakya DR, Shyangwa PM, Shakya R. Psychiatric emergencies in a tertiary care hospital. JNMA J Nepal Med Assoc. 2008;47(169):28-33. PubMed
3. Kessler RC, Olfson M, Berglund PA. Patterns and predictors of treatment contact after first onset of psychiatric disorders. Am J Psychiatry. 1998;155(1):62-69. PubMed doi:10.1176/ajp.155.1.62
4. Banerjee G. Help-seeking behavior and belief system. Indian J Soc Psychiatry. 1997;13:61-64.
5. Gater R, Jordanova V, Maric N, et al. Pathways to psychiatric care in Eastern Europe. Br J Psychiatry. 2005;186(6):529-535. PubMed doi:10.1192/bjp.186.6.529
6. Harrison J, Kisely SR, Jones JA, et al. Access to psychiatric care: the results of the Pathways to Care Study in Preston. J Public Health Med. 1997;19(1):69-75. PubMed doi:10.1093/oxfordjournals.pubmed.a024592
7. Amaddeo F, Zambello F, Tansella M, et al. Accessibility and pathways to psychiatric care in a community-based mental health system. Soc Psychiatry Psychiatr Epidemiol. 2001;36(10):500-507. PubMed doi:10.1007/s001270170015
8. Apsler R, Bassuk E. Differences among clinicians in the decision to admit. Arch Gen Psychiatry. 1983;40(10):1133-1137. PubMed doi:10.1001/archpsyc.1983.01790090095015
Enjoy this premium PDF as part of your membership benefits!