Psychiatric Treatment Needs Among the Medically Underserved: A Study of Black and White Primary Care Patients Residing in a Racial Minority Neighborhood
Objective: Racial disparities in psychiatric treatment are well documented. A growing body of research demonstrates that residing in a racial minority neighborhood adversely affects access to health care and may in part account for psychiatric treatment disparities. The study objective is to determine the role of race in psychiatric treatment disparities among blacks and whites residing in a racial minority neighborhood.
Method: A systematic sample of black (n = 345) and white (n = 57) patients from a primary care clinic in a racial minority neighborhood in northern Manhattan, New York, was analyzed. Logistic regression models were utilized to assess the effect of race on psychiatric treatment. The study was conducted during 1998-1999 and 2001-2003.
Results: Blacks were less likely than whites to have a lifetime psychiatric disorder (OR = 0.17; 95% CI, 0.06-0.53). Among patients with a current psychiatric disorder, there were no significant black-white differences in psychiatric treatment (OR = 0.72; 95% CI, 0.21-2.49). Yet, there were significant and substantial differences among patients without a current psychiatric disorder, with blacks less likely to receive psychiatric treatment than whites (OR = 0.09; 95% CI, 0.04-0.21).
Conclusions: The study findings suggest that neighborhood residence moderates the relationship between race and psychiatric treatment. Black and white primary care patients with a current disorder residing in this racial minority neighborhood had similar rates of psychiatric treatment. Yet, whites, who were the minority in the clinic and the neighborhood from which the clinic draws patients, appear to have more chronic psychiatric problems for which they are receiving treatment. Primary care clinics can serve as a vital tool in addressing the persistent disparities in psychiatric treatment and the psychiatric conditions among whites residing in racial minority neighborhoods.
Prim Care Companion J Clin Psychiatry 2010;12(6):e1-e7
© Copyright 2010 Physicians Postgraduate Press, Inc.
Submitted: March 2, 2009; accepted February 10, 2010.
Published online: November 11, 2010 (doi:10.4088/PCC.09m00804whi).
Corresponding author: Azure B. Thompson, DrPH, Rutgers, The State University of New Jersey, Institute for Health, Health Care Policy and Aging Research, 30 College Ave, New Brunswick, NJ 10010 ([email protected]).
In 2001, the US Surgeon General published a detailed account of the persistently lower rate of detection and treatment of psychiatric disorders among racial minority groups compared to whites.1 A growing body of research suggests that neighborhood environment plays a vital role in these types of disparate health outcomes.2,3 Historically, racial discrimination in the United States has led many racial minority groups to live in neighborhoods segregated from whites; these neighborhoods differ in ways that can negatively affect health.3,4 For example, racial minority neighborhoods are likely to be high-poverty areas that suffer from a historical lack of health care investment.3,5-10 Moreover, these communities have a relatively high rate of residents who are uninsured.3 The lower rate of detection and psychiatric treatment among racial minority groups compared to whites might be due in part to residence in neighborhoods with inadequate access to medical care, including health services to detect and treat psychiatric disorders.
Clinical Points
- Screening for psychiatric disorders in primary care should include inquiry about past history and not focus only on the patient’s current state.
- Community health center physicians should be aware of demographic shifts in the community and pay particular attention to the psychiatric needs of patients who are “aging in place.”
The disparate health outcomes associated with residing in a racial minority neighborhood are not limited to racial minority residents; whites who reside in racial minority neighborhoods experience adverse health outcomes as well. In general, whites residing in racial minority neighborhoods have higher rates of mortality than whites who reside in predominantly white neighborhoods, and, in some cases, higher than their black residential counterparts.4,11 For example, Fang et al11 examined racial segregation and mortality rates in New York City and found that white people living in black areas had higher mortality rates than those living in white areas. Moreover, white women in black areas had mortality rates higher than black women.11 Poor health outcomes among whites in primarily black areas may also be due in part to residence in neighborhoods with inadequate access to health care and to other factors related to their minority status in the community.2
Over the past couple of decades, a growing number of individuals have received treatment for their psychiatric problems within primary care practices. Moreover, a relatively higher proportion of low socioeconomic and racial minority groups receive treatment in these settings.12,13 Few studies have examined patterns of psychiatric disorders and treatment among blacks and whites who access medical care in a racial minority neighborhood. An understanding of psychiatric needs and patterns of treatment within this setting can aid in the development of services that correspond to the diverse needs of all residents of medically underserved neighborhoods. The purpose of this article is to describe the rates of psychiatric disorders and treatment among black and white low-income patients attending a general medical practice serving a racial minority neighborhood. Within this neighborhood, whites represent a racial minority group. The aims of this study are to determine black and white (1) rates of current and lifetime psychiatric disorders, (2) levels of mental health-related functional impairment, and (3) treatment received for psychiatric disorders.
METHOD
Protocol and Patient Recruitment
The study was conducted in an integrated faculty and resident internal medicine group practice of an urban academic health center. The clinic provides approximately 74,000 medical outpatient visits annually to residents of the Washington Heights and Harlem communities of northern Manhattan, New York. Both neighborhoods are designated as health professional shortage areas. Non-Hispanic whites are a minority of the population within both neighborhoods (2% and 13%, respectively).14,15
The sample was assessed in 2 waves. The first sample was interviewed during 1998-1999, and the second sample was interviewed during 2001-2003. No patient was included twice in the analysis, and there were no significant demographic differences between samples. During both data collection periods, patients were systematically approached on the basis of the position of the seat they freely selected in the waiting room. Starting from the back of the room, every consecutive patient was screened for eligibility. Eligible patients were between 18 and 70 years of age, had made at least 1 prior visit, could speak and understand English or Spanish, and were waiting for scheduled face-to-face contact with their primary care physician.
A total of 3,807 patients were approached, of whom 169 (4.4%) refused to participate. Of the 3,638 who were prescreened, 2,291 (63.0%) were not eligible to participate. Common criteria for exclusion were (1) not being scheduled for face-to-face contact with a primary care physician (eg, walk-in visits, scheduled nurse visits, escorting patients with a scheduled visit to the clinic, filling prescriptions) (56.5%), (2) not being between 18 and 70 years of age (33.5%), and (3) not having made a previous visit to the practice (16.7%). Less commonly, patients were excluded because of poor physical health (3.3%) or cognitive impairment (1.6%). Of the 1,347 who met eligibility criteria, 1,157 (85.9%) consented to participate. A total of 1,146 patients (99.0%) completed the survey. The overall sample was of low-income status (51% with annual household income below $6,000); 29% were non-Hispanic black and 5% were non-Hispanic white. The remainder of the sample identified as Hispanic (ie, black, white, or other). On the basis of the preponderance of literature examining the effects of race on health among blacks and whites, we limited our analysis to these racially classified groups. Therefore, a total of 402 respondents not of Hispanic ancestry and who described their racial background as black or white were included in the sample. The analysis included 345 blacks and 57 whites.
Demographic and Clinical Assessment
All data were collected through a survey read to the patient by a research assistant. A demographic history form assessed sex, age, annual household income, race, ethnicity, marital status, educational achievement, and occupational status. The National Institutes of Health guidelines for classification of race and ethnicity were used.14 Current psychiatric disorders were assessed with selected modules of the Primary Care Evaluation of Mental Disorders (PRIME-MD) Patient Health Questionnaire.16 The survey included modules to assess current symptoms of major depressive disorder, panic disorder, generalized anxiety disorder, and alcohol use disorder.15 A drug use disorder module patterned after the PRIME-MD alcohol use module was developed by the study team. Patients who entered the study after 2001 were also assessed for lifetime psychiatric disorders by completing a checklist of specific psychiatric disorders that had ever been diagnosed by a health care provider. The psychiatric conditions included anxiety, bipolar disorder, depression, and alcohol or drug use problems.
Impairment in mental functioning was assessed with the 10-point self-rated social life and family life/home responsibilities subscales of the Sheehan Disability Scale17 (0, none; 1-3, mild; 4-6, moderate; 7-9, marked; 10, extreme) and a measure of self-perceived emotional health that asked respondents to rate their emotional health on a 5-point Likert scale (excellent, very good, good, fair, and poor). Mental health treatment was assessed by a self-report measure that asked about the presence or absence of past-year and past-month treatment by a health care provider for an emotional problem. The questionnaire also included 2 items asking if the respondent had ever been prescribed a medication by a health care provider for an emotional problem (past year and past month) or had ever been hospitalized for an emotional problem.
Statistical Methods
Self-reported race (non-Hispanic black or non-Hispanic white) was the independent variable. The dependent variables were (1) presence of a current or past psychiatric disorder, (2) mental health-related functional impairment, and (3) receipt of treatment for a psychiatric disorder. Chi-square tests were used for racial group comparisons of categorical variables such as sex and marital status, and a Student t test was used to compare groups on age. Logistic regression models were used to examine the independent association between race and having any psychiatric disorder, any mental health-related functional impairment, and any psychiatric treatment, after controlling for income, education, and marital status. Odds ratios (ORs) adjusted for covariates and the corresponding 95% confidence intervals (CIs) are reported.
RESULTS
Demographic Characteristics of the Study Sample
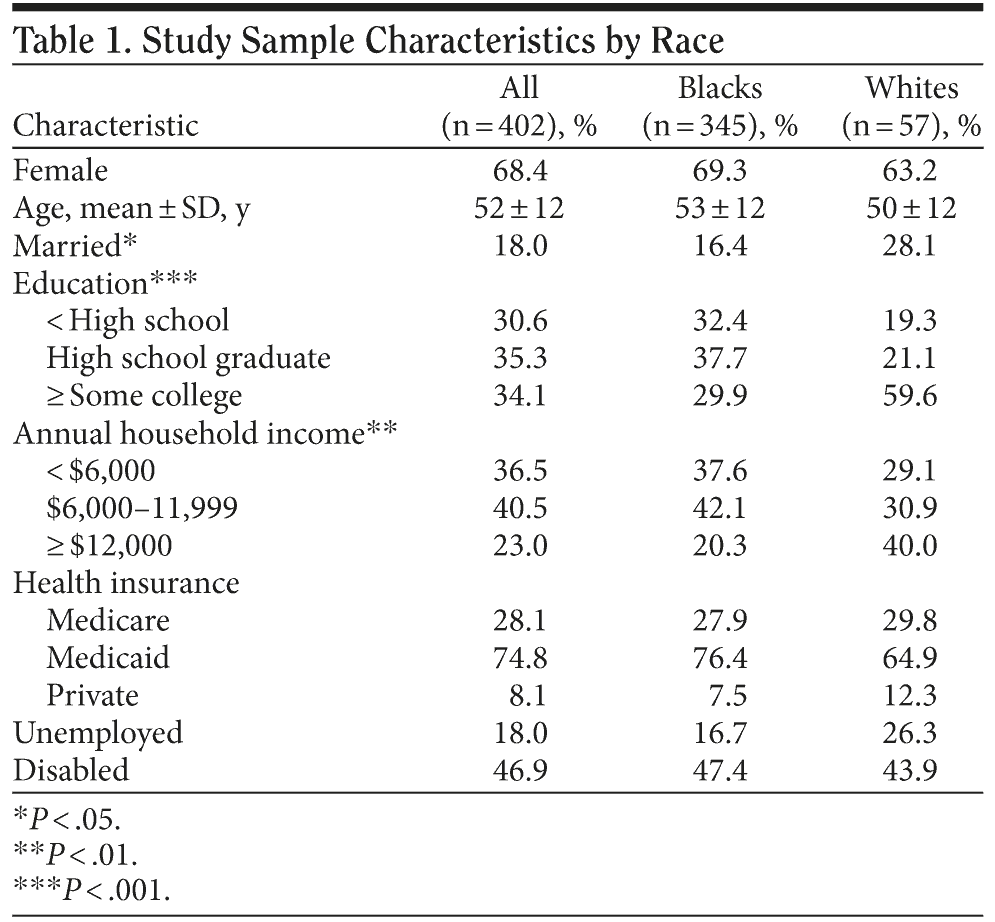
The distribution of demographic characteristics in the total sample, and among the black and white subgroups, is shown in Table 1. The combined sample was composed primarily of women (68%), and the mean age was 52 years (SD = 12). Three-quarters of the patients were on Medicaid and nearly half were disabled. Whites were more likely than blacks to report being married/cohabiting (28% vs 16%, P < .05) and having attended college (60% vs 30%, P < .001). Although blacks were more likely to have an annual household income below $12,000 (80% vs 60%, P < .01), more than 75% of the entire sample was living below or near the 2003 Federal Poverty Level for a household of 1 person, which is $8,980.16 In order to control for possible confounding, racial comparisons on psychiatric-related outcomes were adjusted for education, income, and marital status.
Overall Rates of Current and Lifetime Psychiatric Disorders and Impairment
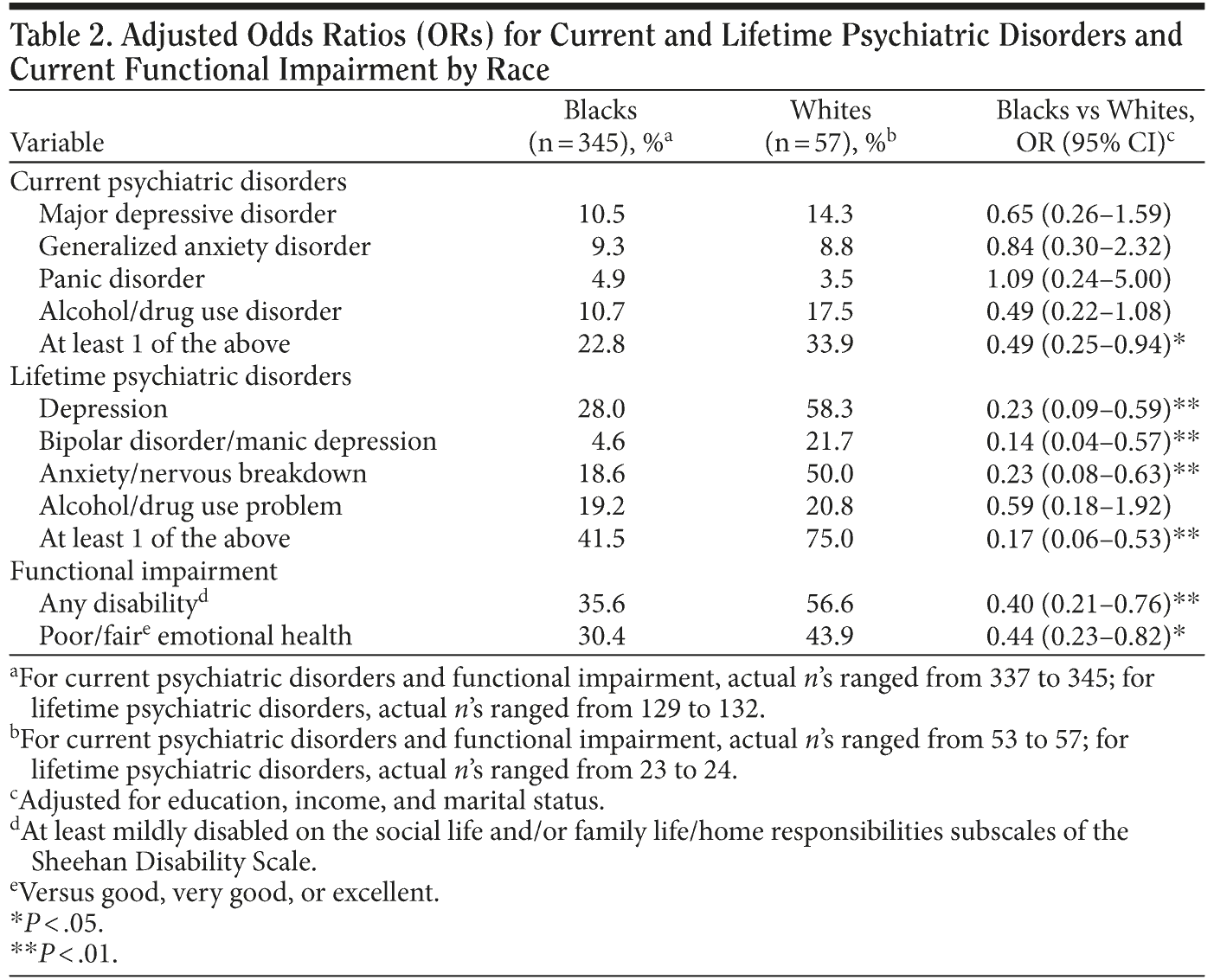
Blacks were significantly less likely than whites to reach the criteria for a current psychiatric disorder when screened (22.8% vs 33.9%; OR = 0.49; 95% CI, 0.25-0.94) (Table 2). These differences were also reflected in lifetime rates (41.5% among blacks vs 75.0% among whites; OR = 0.17; 95% CI, 0.06-0.53). Blacks had significantly less lifetime anxiety (18.6% vs 50.0%; OR = 0.23; 95% CI, 0.08-0.63), bipolar disorder (4.6% vs 21.7%; OR = 0.14; 95% CI, 0.04-0.57), and depression (28.0% vs 58.3%; OR = 0.23; 95% CI, 0.09-0.59). Blacks were also less likely than whites to report any disability on the Sheehan Disability Scale or to report fair/poor emotional health (Table 2).
Psychiatric History and Treatment Utilization
Analyses showed that the effects of race on the receipt of psychiatric treatment depended on the presence rather than the absence of a current psychiatric disorder. The interaction of race and presence of a current psychiatric disorder was statistically significant in the prediction of lifetime psychiatric hospitalization (P = .03), past-year mental health treatment (P = .009), receipt of medication (P = .04), and past-month mental health treatment (P = .02) as well as receipt of medication (P = .03). Therefore, we stratified our race comparisons of treatment by the presence of a psychiatric disorder at screening, while also examining psychiatric history.
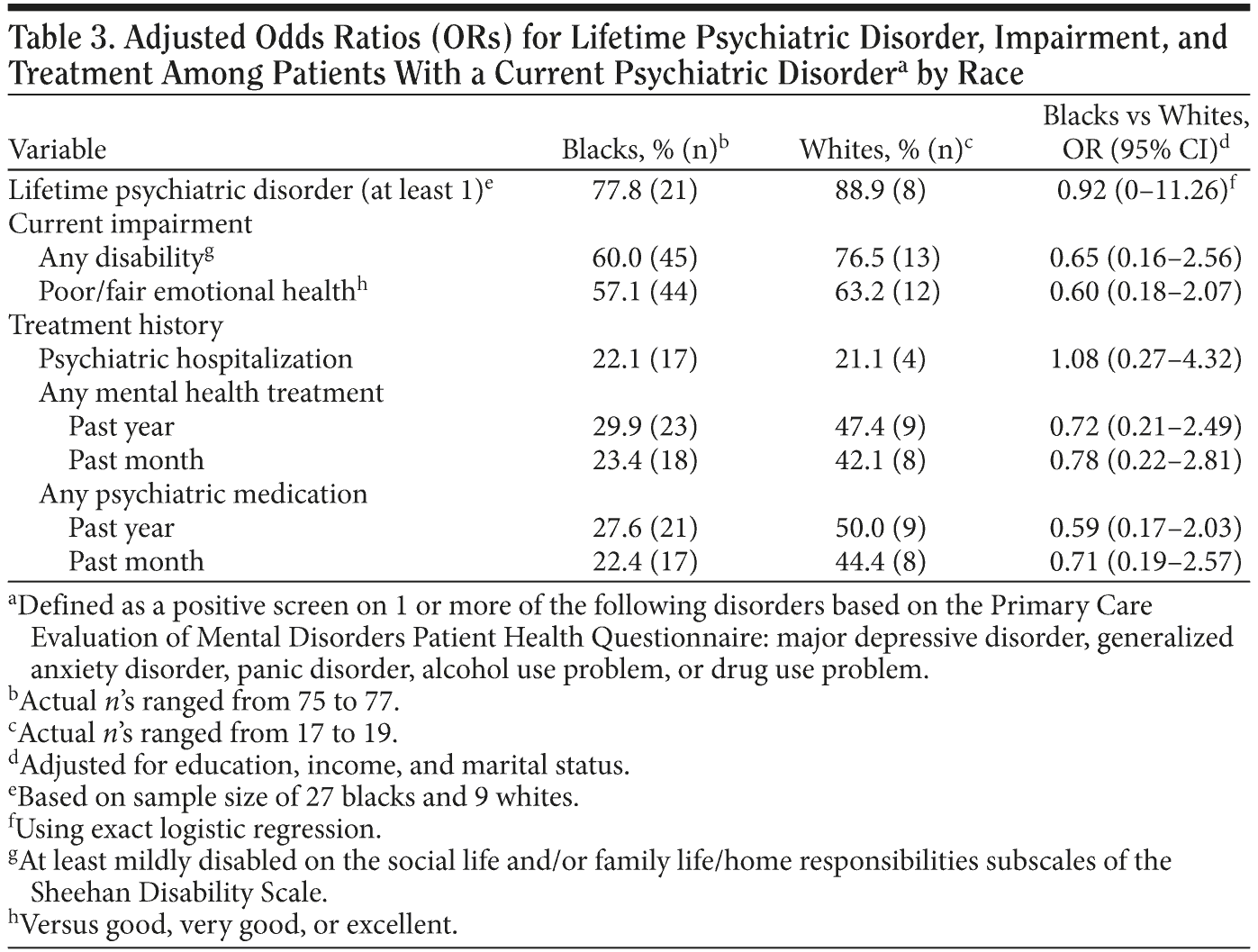
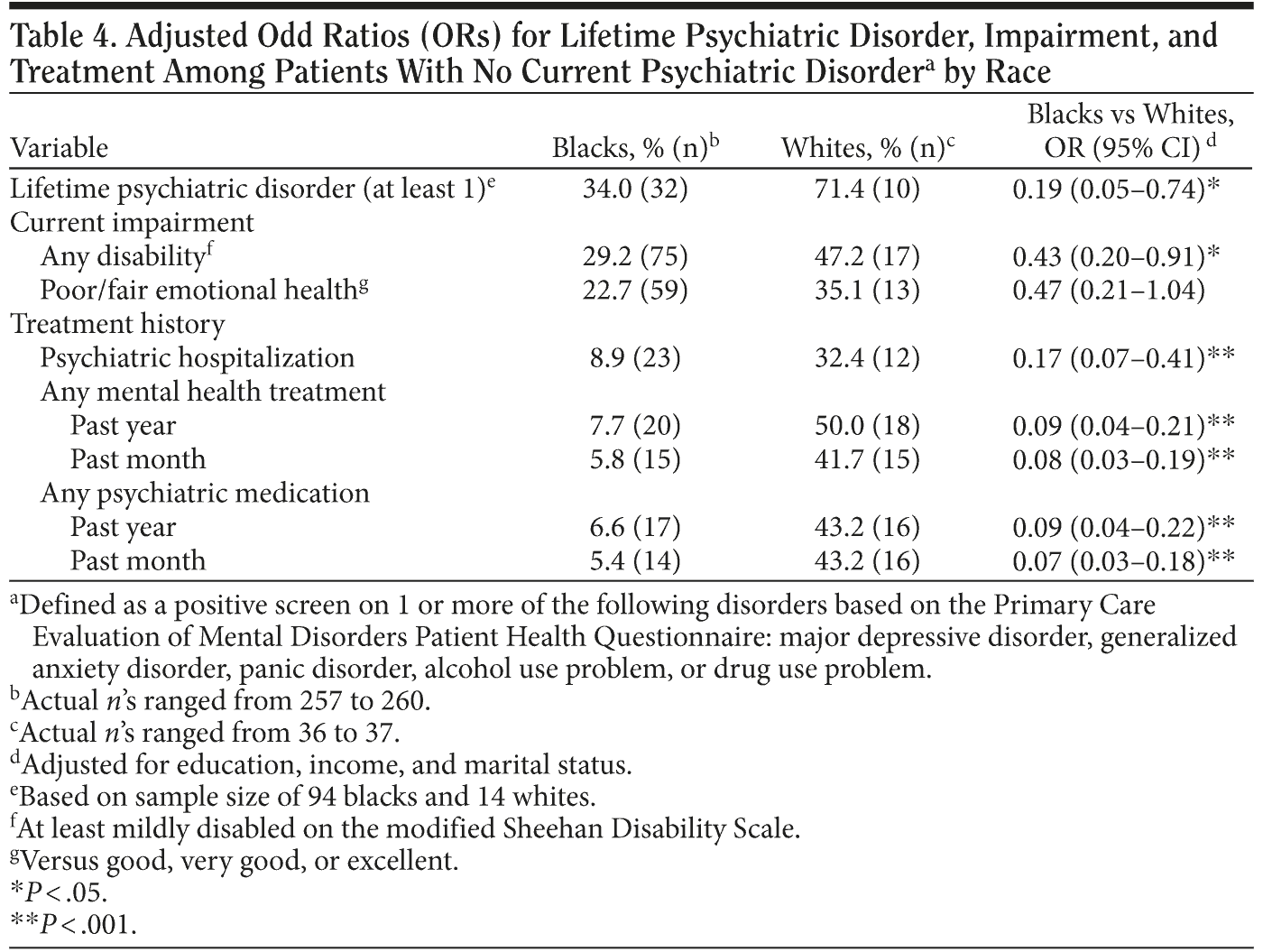
For patients with at least 1 current psychiatric disorder at the time of screening, there were no significant racial differences in rates of past history of a psychiatric disorder, current impairment, lifetime psychiatric hospitalization, and history of mental health treatment or medication use (Table 3). However, significant racial differences emerged among patients with no current psychiatric disorders (Table 4). Blacks in comparison to whites with no current psychiatric disorder less often reported a past history of psychiatric disorder or impairment, and, consistent with their less serious history of psychiatric disorders, also received less psychiatric treatment. Blacks additionally had less lifetime psychiatric hospitalization (8.9% vs 32.4%; OR = 0.17; 95% CI, 0.07-0.41), less past-year mental health treatment (7.7% vs 50.0%; OR = 0.09; 95% CI, 0.04-0.21) and past-month mental health treatment (5.8% vs 41.7%; OR = 0.08; 95% CI, 0.03-0.19), and less often received medication for a mental health problem in the past year (6.6% vs 43.2%, OR = 0.09; 95% CI, 0.04-0.22) and the past month (5.4% vs 43.2%; OR = 0.07; 95% CI, 0.03-0.18) (Table 4). These findings suggest that the past chronic history of psychiatric disorders among whites as compared to blacks was likely to account for whites’ greater use of mental health services in the absence of a current psychiatric disorder.
DISCUSSION
Our findings highlight the complexity of racial disparities in psychiatric treatment. Black and white primary care patients residing in racial minority neighborhoods present unique psychiatric profiles that reflect a variation in treatment needs. In a systematic sample from a primary care clinic whose patient population is drawn from a racial minority neighborhood, we found that whites as compared to blacks (1) had higher rates of any current and lifetime psychiatric disorder, (2) more often reported disability, and (3) more often reported poor/fair emotional health. Among patients with current disorders, there were no racial differences in psychiatric history, functional impairment, psychiatric hospitalization, mental health treatment, or medication received. However, there were significant and substantial racial differences in treatment among patients with no current disorder. Whites with no current disorder at screening were more likely to have a psychiatric history, to be more disabled, and to be receiving psychiatric treatment.
Whites more than blacks in our sample seemed to have more chronic psychiatric conditions for which they were receiving treatment. While blacks had a rate of lifetime disorders only 3% higher than those among a national sample of blacks, rates of lifetime disorders among whites were nearly 30% higher than those found among a national sample of whites.18,19 The findings on rates of psychiatric disorders among whites are consistent with previous research showing that whites who reside in racial minority neighborhoods have poorer health outcomes than whites residing in majority white neighborhoods and blacks residing in majority black neighborhoods.11,20
Research on processes of neighborhood demographic change reveals insights into the characteristics of whites in our sample that would seem to increase their risk for poor psychiatric outcomes. Notably, the primary care clinic examined in this study is located in a neighborhood that has experienced significant shifts in its ethnic and racial demographics. Since the 1980s, the neighborhood began a shift from predominantly white and middle class to nonwhite and low income.21-23 Whites who remain in racially and ethnically shifting neighborhoods are usually poorer and older than whites who leave. Sampson and Sharkey’s work24 on neighborhood out-migration showed that whites who remain are more likely to be poor than whites who move. Moreover, whites in the current study may be aging-in-place, a preference among the elderly to remain living in their homes for as long as they are physically able.25 The elderly who age-in-place also likely outlive or become estranged from their social networks.26
Research suggests that the integration of socially isolated groups might improve health outcomes.2 For example, significant efforts have been made to insure integration into the community among persons with psychiatric disabilities transitioning from institutionalized to community settings.27 Similar efforts may be effective in addressing psychiatric conditions among whites residing in racial minority neighborhoods.
Our findings on psychiatric treatment rates also reveal important insights into the psychiatric conditions of blacks and whites residing in neighborhoods with a high proportion of racial minorities. Foremost, our finding of no significant racial difference in psychiatric treatment rates among patients with a current psychiatric disorder suggests the potential role of primary care in the reduction of racial disparities in psychiatric treatment.20 Yet, our findings on treatment rates among whites without a current disorder highlight the importance of continued outreach to socially marginalized groups regardless of race. Among patients without a current psychiatric disorder, whites were significantly more likely than blacks to receive treatment and to report a psychiatric disorder in their lifetime. Notably, treatment rates among whites in our sample without a current disorder were more than twice as high as a national sample of individuals without current disorders.28 This finding suggests that treatment is being sought to address past psychiatric conditions. After their initial diagnosis, whites in our sample might be receiving care that is effective in treating their symptoms so that they no longer screen positive for a current disorder.
The implication of this finding suggests that studies looking at racial/ethnic differences in treatment utilization need to take into account psychiatric severity, inclusive of ascertaining both current and past history of psychiatric disorders. Psychiatric screening instruments in primary care settings, for the most part, focus only on current status. A previous psychiatric history among currently asymptomatic patients can have an impact on current disability and treatment needs, which may account for the relatively higher rates of treatment among whites.
A few limitations should be noted. Although the study found lower rates of psychiatric disorders in blacks as compared to whites, research suggests that this may be due to racial differences in reporting psychiatric symptoms. Some cultural groups find it more appropriate to report mental health problems to a family member, elder, spiritual or community leader, or someone familiar with their social ties.29 Whites may be more likely than blacks to report their emotional problems to their physician and thus be diagnosed and referred to treatment. Another possible limitation is the assessment of psychiatric disorders. The PRIME-MD has been validated primarily in white middle-class populations. The sample used to validate the PRIME-MD included 79% whites and 13% blacks16; however, these screening tools may not be sensitive enough to detect psychiatric disorders effectively among blacks, particularly when considering the potential for racial differences in reporting of psychiatric symptoms.
Although there was a relatively large sample of blacks within this primary care clinic, the sample of whites was small and the statistical power for our comparisons, particularly the analysis of treatment among patients with a current disorder, was limited. For this reason, some of the racial differences in treatment observed in our study did not meet the criterion for statistical significance. Although we conclude that there are no differences in treatment among black and white patients with a current disorder, we cannot make this conclusion with confidence because of the limited power. However, the treatment findings were highly significant for patients with no current disorder in which the sample size was also limited.
Despite these limitations, our findings suggest that access to psychiatric treatment can be improved through primary care service provision in resource-poor settings. The primary care clinic described in this study was created to provide services for the medically underserved in impoverished communities. Findings suggest that these services may be effective in reducing disparities in treatment between blacks and whites. Results further indicate that whites living in a racial minority neighborhood have a higher rate of chronic psychiatric conditions relative to blacks and appear to be receiving treatment for those conditions through primary care services. Yet, given the high burden of chronic psychiatric conditions among this group, further outreach efforts may be needed to ensure that these individuals receive appropriate psychiatric treatment and become better integrated into their neighborhood community.
Author affiliations: Department of Sociomedical Sciences, Mailman School of Public Health (Dr Thompson); Division of Internal Medicine, College of Physicians and Surgeons (Dr Carrasquillo); Division of Epidemiology, New York State Psychiatric Institute (Drs Gameroff and Weissman); and Department of Epidemiology, Mailman School of Public Health (Dr Weissman), Columbia University, New York, New York. Dr Thompson is currently with the Institute for Health, Health Care Policy, and Aging Research at Rutgers, The State University of New Jersey, Institute for Health, New Brunswick. Dr Carrasquillo is currently with the Division of General Internal Medicine, Miller School of Medicine, University of Miami, Florida.
Potential conflicts of interest: In the past 5 years, Dr Weissman has received investigator-initiated grants, which are no longer active, from GlaxoSmithKline, Eli Lilly, and the Josiah Macy Foundation. Dr Weissman currently receives research funding from the National Institute of Mental Health, the National Institute on Drug Abuse, the National Alliance for Research on Schizophrenia and Depression, and the Sackler Foundation; and receives royalties from the Oxford University Press, Perseus Press, the American Psychiatric Association Press, and MultiHealth Systems. Drs Thompson, Carrasquillo, and Gameroff report no financial or other conflicts of interest.
Funding/support: This article was funded by the Columbia Center for the Health of Urban Minorities (NCMHHD MD000206-019006) (Drs Thompson, Carrasquillo, and Weissman) and an unrestricted grant from Eli Lilly (Dr Weissman). Dr Thompson was funded by the W.K. Kellogg Fellowship in Health Policy Research; a predoctoral fellowship in the Behavioral Sciences Training in Drug Abuse Research, a program sponsored by Public Health Solutions and the National Development and Research Institutes (NDRI); and by the National Institute on Drug Abuse (5T32 DA07233).
Disclaimer: The points of view, opinions, and conclusions in this article do not necessarily represent the official position of the US government, Public Health Solutions, or NDRI.
Previous presentation: Thompson A, Carrasquillo O, Gameroff M, et al. Psychiatric disorders and treatment among black and white patients in an urban primary care setting [poster]. Presented at the 29th Annual Meeting of the Society for General Internal Medicine; April 26-29, 2006; Los Angeles, California.
REFERENCES
1. US Department of Health and Human Services. Mental Health: Culture, Race and Ethnicity—A Supplement to Mental Health: A Report of the Surgeon General. Rockville, Maryland: US Department of Health and Human Services Substance Abuse and Mental Health Services Administration, Center for Mental Health Services; 2001.
2. Pickett KE, Wilkinson RG. People like us: ethnic group density effects on health. Ethn Health. 2008;13(4):321-334.PubMed doi:10.1080/13557850701882928
3. UN Committee on the End of Racial Discrimination Working Group on Health and Environmental Health. Unequal Health Outcomes in the United States: Racial and Ethnic Disparities in Health Care Treatment and Access, the Role of Social and Environmental Determinants of Health, and the Responsibility of the State. http://www.prrac.org/pdf/CERDhealthEnvironmentReport.pdf. Published January 2008. Accessed July 29, 2010.
4. Inagami S, Borrell LN, Wong MD, et al. Residential segregation and Latino, black and white mortality in New York City. J Urban Health. 2006;83(3):406-420.PubMed doi:10.1007/s11524-006-9035-8
5. Smith DB, Feng ZL, Fennell ML, et al. Separate and unequal: racial segregation and disparities in quality across US nursing homes. Health Aff (Millwood). 2007;26(5):1448-1458.PubMed doi:10.1377/hlthaff.26.5.1448
6. Williams DR, Collins C. Racial residential segregation: a fundamental cause of racial disparities in health. Public Health Rep. 2001;116(5):404-416. PubMed
7. Haas JS, Earle CC, Orav JE, et al. Racial segregation and disparities in cancer stage for seniors. J Gen Intern Med. 2008;23(5):699-705.PubMed doi:10.1007/s11606-008-0545-9
8. McLafferty S. Neighborhood characteristics and hospital closures: a comparison of the public private and voluntary hospital systems. Soc Sci Med. 1982;16(19):1667-1674.PubMed doi:10.1016/0277-9536(82)90091-0
9. Rice MF. Inner-city hospital closures/relocations: race, income status, and legal issues. Soc Sci Med. 1987;24(11):889-896.PubMed doi:10.1016/0277-9536(87)90282-6
10. Almgren G, Ferguson M. The urban ecology of hospital failure: hospital closures in the city of Chicago, 1970-1991. J Sociol Soc Welf. 1999;26(4):5-25.
11. Fang J, Madhavan S, Bosworth W, et al. Residential segregation and mortality in New York City. Soc Sci Med. 1998;47(4):469-476.PubMed doi:10.1016/S0277-9536(98)00128-2
12. Snowden LR, Pingitore D. Frequency and scope of mental health service delivery to African Americans in primary care. Ment Health Serv Res. 2002;4(3):123-130.PubMed doi:10.1023/A:1019709728333
13. Kessler RC, Demler O, Frank RG, et al. Prevalence and treatment of mental disorders, 1990 to 2003. N Engl J Med. 2005;352(24):2515-2523.PubMed doi:10.1056/NEJMsa043266
14. New York City Department of Planning. Manhattan Community District 10. Community District Information. http://nyc.gov/html/dcp/pdf/lucds/mn10profile.pdf#profile. Accessed February 1, 2009.
15. New York City Department of Planning. Manhattan Community District 12. Community District Information. http://nyc.gov/html/dcp/pdf/lucds/mn12profile.pdf#profile. Accessed February 1, 2009.
16. Spitzer RL, Williams JB, Kroenke K, et al. Utility of a new procedure for diagnosing mental disorders in primary care: the PRIME-MD 1,000 study. JAMA. 1994;272(22):1749-1756.PubMed doi:10.1001/jama.272.22.1749
17. Sheehan DV. The Anxiety Disease. New York, NY: Scribner’s ; 1983.
18. Breslau J, Kendler KS, Su M, et al. Lifetime risk and persistence of psychiatric disorders across ethnic groups in the United States. Psychol Med. 2005;35(3):317-327.PubMed doi:10.1017/S0033291704003514
19. Breslau J, Aguilar-Gaxiola S, Kendler KS, et al. Specifying race-ethnic differences in risk for psychiatric disorder in a USA national sample. Psychol Med. 2006;36(1):57-68.PubMed doi:10.1017/S0033291705006161
20. Chow JCC, Jaffee K, Snowden L. Racial/ethnic disparities in the use of mental health services in poverty areas. Am J Public Health. 2003;93(5):792-797.PubMed doi:10.2105/AJPH.93.5.792
21. Limonic L. The Latino Population of New York City. New York, NY: New York Center for Latino American, Caribbean and Latino Studies; 2008.
22. Fernandez M. New winds at an island outpost. The New York Times. March 4, 2007;The City:14.
23. Bader DP. Northern Manhattan gentrifying? study says no. The Manhattan Times. December 11, 2008; Community section:1.
24. Sampson RJ, Sharkey P. Neighborhood selection and the social reproduction of concentrated racial inequality. Demography. 2008;45(1):1-29.PubMed doi:10.1353/dem.2008.0012
25. Sabia JJ. There’s no place like home: a hazard model analysis of aging in place among older homeowners in the PSID. Res Aging. 2008;30(1):3-35. doi:10.1177/0164027507307919
26. Klinenberg E. Dying alone: the social production of urban isolation. Ethnography. 2001;2(4):501-531. doi:10.1177/14661380122231019
27. Metraux S, Caplan JM, Klugman D, et al. Assessing residential segregation among Medicaid recipients with psychiatric disability in Philadelphia. J Community Psychol. 2007;35(2):239-255. doi:10.1002/jcop.20145
28. Druss BG, Wang PS, Sampson NA, et al. Understanding mental health treatment in persons without mental diagnoses: results from the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2007;64(10):1196-1203.PubMed doi:10.1001/archpsyc.64.10.1196
29. Kirmayer LJ. Cultural variations in the clinical presentation of depression and anxiety: implications for diagnosis and treatment. J Clin Psychiatry. 2001;62(suppl 13):22-28, discussion 29-30. PubMed