Role of the General Practitioner in the Care of Patients Recently Discharged From the Hospital After a First Psychotic Episode: Influence of Length of Stay
Objective: It is unclear to what extent general practitioners are involved in the postdischarge care of patients hospitalized for a first psychotic episode and whether this involvement is influenced by length of stay in the hospital. The objectives of this study were to describe the role of the general practitioner in providing postdischarge care to patients with first-episode psychosis in terms of frequency and type of consultation and the extent of collaboration with hospital-based specialist services and to determine whether decreasing length of stay was accompanied by a modification in this role.
Method: Six months after hospital discharge, a postal questionnaire was sent to the general practitioners of patients recruited to the French STEP cohort (Schizophrenie et son Traitement: une Evaluation de la Prize en charge), a prospective study of the clinical and social determinants of care pathways and prognosis for patients hospitalized for a first psychotic episode (DSM-IV criteria) in 5 services of the La Colombiרre Psychiatric Hospital, Montpellier, France. Length of stay in the hospital was dichotomized according to the median value of 35 days. Data collection took place from February 2008 to March 2009.
Results: Of the 121 STEP patients, 65% (n = 79) had a regular general practitioner. The general practitioners had been informed by the hospital of the admission of their patient in only 17.9% (7/39) of cases. Of the general practitioners, 78.3% (47/60) had seen the patient at least once since discharge, with a median number of visits standardized over 6 months of 0.86 (range, 0-8.6). General practitioners were better informed with regard to diagnosis, date of discharge, name of psychiatrist, treatment, and community follow-up at discharge for patients with a short length of stay in the hospital, who were also more likely than those with a long length of stay to be consulting for mental health problems.
Conclusions: Our findings suggest a low level of implication of general practitioners in providing postdischarge care to first-episode psychotic patients, irrespective of their length of hospital stay. Yet, the general practitioner has a role to play in coordinating and providing care for somatic health problems as well as psychiatric symptoms, specifically in the case of early discharge.
Prim Care Companion CNS Disord 2011;13(5):doi:10.4088/PCC.11m01180
© Copyright 2011 Physicians Postgraduate Press, Inc.
Submitted: March 14, 2011; accepted April 13, 2011.
Published online: September 29, 2011.
Corresponding author: Joanna L. Norton, PhD, INSERM, U1061, Neuropsychiatry: Epidemiological and Clinical Research, La Colombiרre Hospital, 39 avenue Charles Flahault, BP 34493, 34093 Montpellier Cedex 5, France ([email protected]).
Since the middle of the last century, there has been a transition in almost all Western countries toward a policy of reduced periods of hospitalization for patients with severe mental illness. While initially not evidence based, a number of observational studies have suggested that patients returning to the community show better quality of life and have larger friendship networks, lower mortality rates, and reduced dependence on pharmacotherapies than those remaining in institutions.1 This policy assumes, however, that community care is well organized and places increasing burden in particular on primary caregivers. While there has been considerable research on community mental health care in general in preventing relapse, relatively little attention has been paid to the interface with general practitioners, although it is estimated that 25% of patients with psychosis lose all contact with mental health services and are followed and cared for entirely within general practice.2,3 Patients discharged from the hospital following a psychotic episode frequently discontinue medication and often have multiple pathologies as well as social and professional difficulties. Antipsychotic medication also has numerous side effects that require monitoring. Adequate medical follow-up therefore assumes not only knowledge of these disorders on the part of primary care practitioners, but also an efficient interface between hospital practitioners and primary caregivers at discharge. There are many studies on pathways to care in first-episode psychosis4-7 and general practitioner management of early psychosis.8-12 Few studies, however, have examined care pathways of specific patients13 and particularly the influence of length of hospital stay on postdischarge community care.
Clinical Points
- There is a need for greater recognition of the role of the general practitioner in managing first-episode psychotic patients after hospital discharge, specifically for the management of psychiatric symptoms in the case of early discharge.
- Communication between general practitioners and psychiatrists needs to be improved.
In France, public psychiatric care is organized into sectors that cover well-defined geographical areas of approximately 70,000 inhabitants.14 Each sector is responsible for providing inpatient and outpatient care. Care is largely hospital based, the amount provided at a community level being limited overall, although it varies widely from one sector to another depending on the care organization and internal policy. Psychiatrists have few guidelines and protocols to follow with managerial targets to meet, resulting in different care models working alongside. There are long appointment delays for consulting private psychiatrists, many of whom offer psychoanalytic therapy only.15-17
Although general practitioners are the main primary care providers, they are not actively integrated into the community mental health team and seldom receive referrals from psychiatric services. General practitioners work mainly alone with no ancillary staff and limited collaboration with specialists, especially hospital psychiatrists.18 Changes were introduced in 2004, with patients strongly encouraged to register with a general practitioner of their choice whose role it is to coordinate care and refer patients if necessary to specialists (all except ophthalmologists, gynecologists, pediatricians, and psychiatrists for those patients under 26 years old). Those who bypass general practitioner referral can be financially sanctioned with lower reimbursements.19,20
In France there is still considerable variation in length of stay; our previous findings (D.C., unpublished data, 2011) confirm this, with length of stay varying from 4 to 371 days for first-episode psychotic patients within the same hospital. Our results suggest that this variation is not determined by clinical differences in patients at admission but rather by changes in medication during hospitalization, symptomatology at discharge (less negative but more positive symptoms for short-stay patients), and ward policy (length of stay being significantly shorter in services where the head psychiatrist declared being in priori more in favor of shorter [≤ 30 days] than longer stays [> 30 days]). With regard to care plans at discharge, one-third (32.5%) of patients with a short length of stay were “referred” to care by a private psychiatrist compared to 12.5% of long length of stay patients; the remaining patients received community care or day hospital care (52.5% and 15%, respectively, for short length of stay patients; 44.4% and 43.1%, respectively, for long length of stay patients). Length of stay may also have an impact on the role of the general practitioner in providing postdischarge care and on the collaboration between general practitioners and specialists. However, there are to our knowledge no studies specifically on this topic. Furthermore, findings on service use specific to one health care organization are difficult to extrapolate to other settings.
The aim of the present study was thus to describe the role of the general practitioner in providing postdischarge care to patients with first-episode psychosis in terms of frequency and type of consultation and the extent of collaboration with hospital-based specialist services. We then sought to determine whether decreasing length of stay was accompanied by a modification in this role. Although community psychiatric care remains largely underdeveloped and hospital based in France,14 it was hypothesized that short-stay patients would be more likely to consult their general practitioner after discharge than long-stay patients, most of whom stay “within” the system.
METHOD
The STEP Project
The STEP (Schizophrenie et son Traitement: une Evaluation de la Prize en charge) cohort includes consecutive admissions to 5 services of the La Colombiרre Psychiatric Hospital, Montpellier, France. The inclusion criteria were being between 15 and 60 years of age and hospitalized for a first episode of psychosis. Psychotic symptoms were determined by the International Classification of Diseases, Tenth Edition21: hallucinations, delusions, marked thought disorders, and marked psychomotor disorders including mutism, stupor, catatonia, and grossly disorganized behavior. Subjects were excluded if they had a confusional state, psychosis of organic origin, or did not speak French. Patients were included from January 2007 to March 2008. Among questionnaires completed at admission and discharge, information was collected on sociodemographics, use of health care services during the past year, duration of untreated psychosis, and planned care at discharge. For each patient, a diagnosis was established after admission by the study psychiatrist using DSM-IV criteria.
All subjects (or parents in the case of minors) were asked to sign a consent form. Authorization for the STEP cohort study was obtained from the Computerised Personal Information Protection Committee and from the regional ethics committee.
The General Practitioner Study
During their hospital stay, patients (or parents in the case of minors) were asked to indicate the name of their usual general practitioner or the general practitioner they registered with within the 2004 physician registration framework. At least 6 months after hospital discharge, a questionnaire was sent to the general practitioner, with a section specifically about the patient (referred to as STEP-GP patient) who had indicated the general practitioner as his/her usual physician, as well as questions on the physician’s sociodemographic and practice characteristics and training received in mental health during the past 3 years.
An accompanying letter was sent to the general practitioner giving the name of the patient. For confidentiality purposes, only the initials and the STEP study identification number were reported on the questionnaire. Nonrespondents received a follow-up questionnaire a month later, followed by a phone call and 2 more follow-up questionnaires. Data collection took place from February 2008 to March 2009.
Statistics
Descriptive statistics are shown with percentages for categorical variables and medians and ranges for skewed continuous variables. Normality was tested using the Shapiro-Wilks test. As length of time between hospital discharge and the general practitioner questionnaire varied, the number of general practitioner consultations was standardized over 6 months, which is the minimum time span between discharge and the general practitioner survey. For the study of factors associated with length of stay, values were classified into 2 groups according to the median length of stay of 35 days. Comparisons were made using the χ2 test and, when appropriate, the Fisher exact test for categorical variables and the Wilcoxon approximation of the normal distribution for continuous variables. Significance was set at P < .05. Statistical analyses were carried out using SAS version 9.1 (SAS Institute, Inc, Cary, North Carolina).
RESULTS
Of the 121 first-episode psychotic patients (86 men and 35 women) admitted to the hospital during the recruitment period who met inclusion criteria and consented to take part in the study, 79 (65%) gave the name of a general practitioner that they had previously visited, that they considered as their usual general practitioner, or had registered with.
Comparison of Patients According to Whether They Did or Did Not Give the Name of a General Practitioner
There were no significant differences between the 79 patients who gave the name of a usual general practitioner and the 42 patients who did not regarding age, sex, education level, duration of untreated psychosis, and diagnosis. There was no significant difference in length of stay, with medians of 36 (range, 6-270) and 40.5 (range, 4-371) among those with and without a usual general practitioner, respectively (P = .85). However, those declaring a usual general practitioner were significantly more likely to be living with their family (66.7% versus 46.5%, P = .03) and to have consulted any general practitioner at least once during the year preceding their hospital stay (78.2% versus 60.5%, P = .04).
General Practitioner Descriptions and Response Rates
Of the 79 general practitioners who received a questionnaire about their patient, 64 were returned (81% response rate). There were no significant differences in age and sex between respondents and nonrespondents. Mean age of the respondents was 51.7 years (SD = 7.4) and half were male (32/64). Of the general practitioners, 88.7% (55/62) had been practicing for 10 years or more and 61.3% (38/62) had followed a training course in mental health in the past 3 years, of which 68.4% (26/38) were evening training seminars. Also, 90.6% (58/64) practiced in an urban area and 48.4% (31/64) within 3 miles of La Colombiרre Hospital.
Description of the STEP-GP Patients
The 64 patients for whom the general practitioners returned the questionnaire were mainly male (75%, 48/64), with a mean age of 25.0 years (SD = 5.8). Forty-six patients had been hospitalized in services with a policy of short length of stay (preference of head psychiatrist) and 18 in a service with a policy of long length of stay. The median length of hospital stay was 35 days, ranging from 8 to 259 days. The main diagnosis was brief psychotic disorder (50.0%, 32/64), followed by schizophrenia (40.6%, 26/64), bipolar disorder (7.9%, 5/64), and 1 case of schizoaffective disorder (1.5%, 4/64). Duration of untreated psychosis, estimated as the delay between first psychotic symptoms according to the patient, family, or clinician, and date of hospital admission ranged from 0 to 17 years (median = 2.5). In the year preceding their admission, 20.3% (13/64) had not visited a general practitioner, 53.1% (34/64) had made 1 to 3 visits to any general practitioner, and 26.6% (17/64) had made 4 visits or more. Overall, 79.7% (51/64) of the patients had seen a general practitioner at least once. Of those visiting a general practitioner, 17.6% (9/51) had visited 2 or more different physicians.
Proposed Care Plan at Discharge for the STEP-GP Patients
The proposed care plan at hospital discharge was outpatient psychiatric care for 31 patients (51.7%), follow-up by private psychiatrist for 14 patients (23.3%), and day hospital for 15 patients (25.0%). Forty-eight (77.4%) patients left the hospital with an appointment. Only 1 patient was advised to visit a general practitioner.
STEP-GP Patient Follow-Up and Influence of Length of Hospitalization
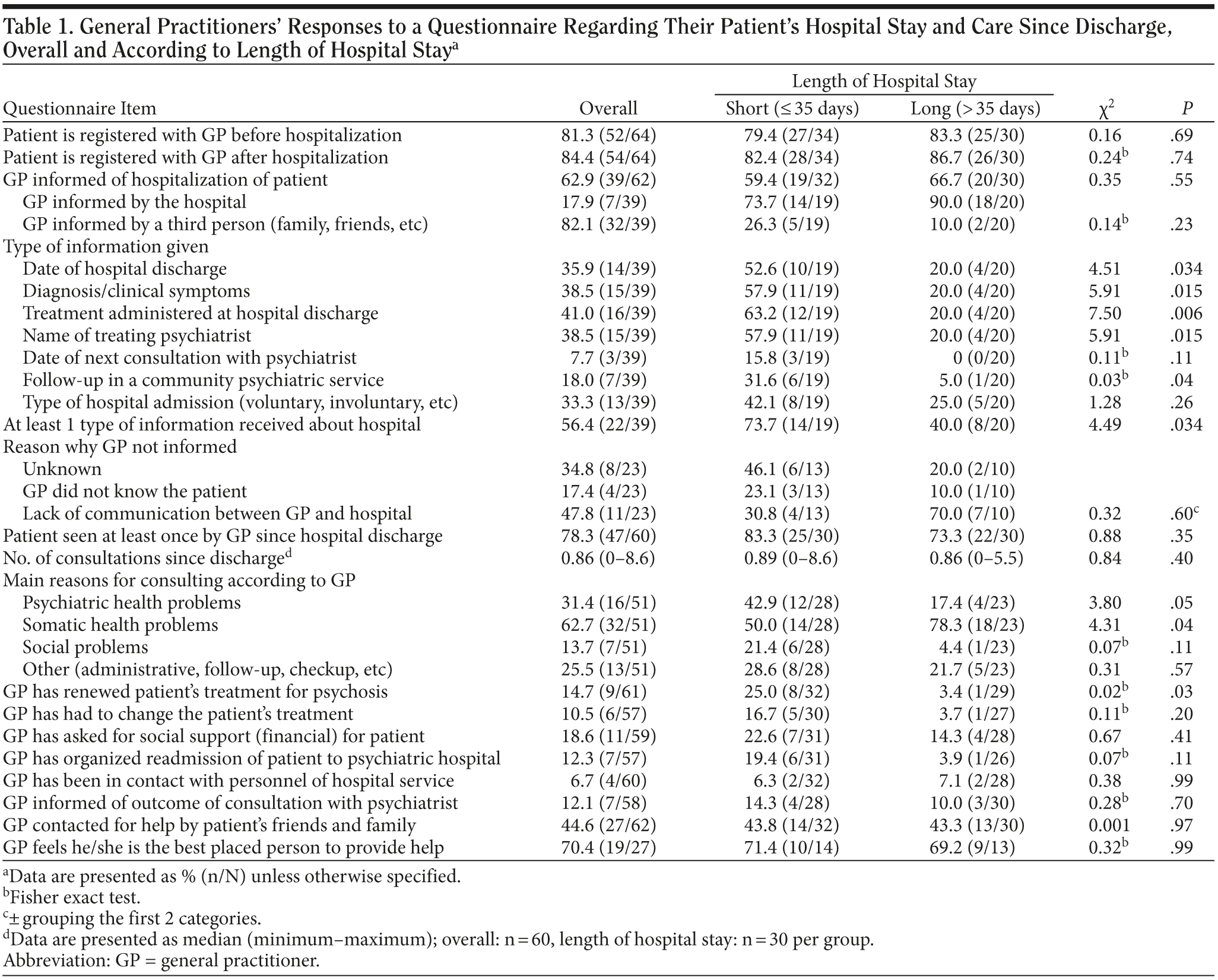
General practitioner responses for the management of these 64 patients are given in Table 1. Of the general practitioners, 84.4% declared that the patient had registered with them as their physician. At completion of the questionnaire, the median length of time since hospital discharge was 11.7 months, ranging from 6.0 to 23.7 months. The median number of general practitioner visits standardized over a 6-month period was 0.86, ranging from 0 to 8.6. The main reason for consulting the general practitioner was somatic health problems (62.7%, 32/51), followed by psychiatric problems (31.4%, 16/51). The general practitioner had renewed (14.7%, 9/61) and/or modified (10.5%, 6/57) the patient’s treatment in 18.5% of cases.
The general practitioners were informed of the hospitalization of their patient in 62.9% (39/62) of cases and for half of the 12 patients not registered with the general practitioner prior to hospitalization. No difference was found in terms of length of stay. When informed of the hospitalization, the information was given by family and friends in 82.1% (32/39) of cases and by the hospital in 17.9% (7/39) of cases. Of the general practitioners, 78.3% (47/60) declared having seen the patient at least once since hospital discharge. In the case of shorter length of stay, however, the general practitioner had more often been given information on date of discharge (52.6% [10/19] versus 20.0% [4/20], P = .034), symptoms and diagnosis (57.9% [11/19] versus 20.0% [4/20], P = .015), treatment administered at discharge (63.2% [12/19] versus 20.0% [4/20], P = .006), name of treating psychiatrist (57.9% [11/19] versus 20.0% [4/20], P = .015), and follow-up by community mental health services (31.6% [6/19] versus 5.0% [1/20], P = .04). Those with a short length of stay consulted more often for psychiatric health problems compared to long length of stay patients (42.9% [12/28] versus 17.4% [4/23], P = .05). The opposite was found for somatic health problems, with figures of 50.0% (14/28) and 78.3% (18/23) for short and long lengths of stay, respectively (P = .04).
DISCUSSION
The main limitation of this article is the small sample size and the nature of the sample, including only general practitioners identified as the personal physicians of first-episode psychotic patients hospitalized in the public sector. This is likely to represent “best practice” in so far as the general practitioner is responding to a real case. This study has a high response rate (81%) compared to other general practitioner studies,22 no doubt because the main part of the questionnaire concerned a patient known to the physician.23
The proportion of STEP patients with a regular general practitioner at discharge is lower (65%) than the 2007 national adult rate in France (80%)24 and is no higher in short-stay patients. This difference is clearly a reflection of the age and sex structure of the study sample (mainly young males), as physician registration rates are higher in women and increase with age.24 This lower rate can also be explained by the type of patient recruited into the study (severe mental illness, geographically and professionally unstable population, experiencing many social and personal problems, etc). Patients in over two-thirds of cases stay “within” the psychiatric system with outpatient psychiatric care (visits or day hospital) as the proposed care plan at discharge. Although visiting a general practitioner for their psychiatric disorder may not be necessary, the general practitioner would still have a role to play in coordinating overall health and dealing with somatic health problems. Yet, general practitioners report that one-third of patients and nearly half (42.9%) of short length of stay patients actually consulted for psychiatric symptoms, suggesting unmet need with respect to care that was planned to be provided by specialist services.
Contrary to what was expected, patients with a short length of stay in the hospital were no more likely than others to have registered with a general practitioner or to have consulted this physician after discharge. In the current study, patients who declared having registered with a personal general practitioner actually seldom consulted this physician (less than twice a year), irrespective of their length of stay in the hospital. There are to our knowledge no comparative data for general practitioner consultation rates after hospital discharge for a first psychotic episode. With regard to all psychotic patients, studies report median numbers of yearly contacts of 6.425 and 8.0,2 with a mean of 4.4 psychotic patients per general practitioner for the United Kingdom10 and 5% of psychotic patients per practice for France.26 It has been shown that psychotic patients in the United Kingdom consult physicians more frequently than others.27 In a French primary care study, a median of 3 consultations (range, 1-30) per patient over a 6-month period was found in a subsample of 18 to 30-year-old consecutive attenders.28
The low postdischarge general practitioner consultation rate in our study could partly be explained by patients having direct access to private psychiatrists. The 2004 physician registration scheme allows patients under age 26 years to consult psychiatrists without being referred by their general practitioner. This means that most patients referred to a private psychiatrist after hospital discharge would no doubt have bypassed the general practitioner, especially if not advised by the hospital team to contact a general practitioner as their care coordinator and in the absence of somatic complaints. However, only a minority of patients will be followed at discharge by a private psychiatrist, and the higher rate of short length of stay patients with this care plan is not reflected in a lower general practitioner contact rate.
As found elsewhere,23,27 the general practitioner was consulted for somatic health problems more often than for mental health problems. Compared to patients with a long length of stay, those with a shorter length of stay were significantly more likely to consult the general practitioner for psychiatric problems. This may be because they were more likely to have positive symptoms at discharge and may have had difficulty in rapidly accessing a private psychiatrist. This finding underlines the importance of the general practitioner in providing follow-up care for psychotic patients for both somatic and psychiatric health problems. Furthermore, general practitioners were involved in renewing (14.7%) and changing (10.5%) patients’ treatment for psychosis in spite of a lack of communication at and after discharge (general practitioners were informed of the outcome of specialized consultations in only 12% of cases). The lack of transfer of information is in keeping with the general practitioners’ high level of dissatisfaction concerning collaboration with psychiatrists.18
According to a 2003 decree (article R1112-2 of the public health code in France), specialized services are supposed to inform the general practitioner by letter of the hospitalization and treatment plan at discharge. We observed that this was the case for only 17.9% of the patients. Moreover, the rate was not improved for patients discharged after a short stay. Information about hospital admission was mainly given to the general practitioner by family and friends. We did note that although few general practitioners were contacted, better information was given with regard to diagnosis, treatment, name of psychiatrist, and follow-up by community mental health services for patients with a short length of stay. This finding suggests that, although there is no difference in contact rate between hospital specialists and general practitioners when patients are discharged earlier, the contact information when it occurs is improved.
In many countries, including France, there has been a reduction in the number of psychiatric hospital beds and duration of stay over the past years, which is forecasted to continue, accompanied by a reduction in the number of psychiatrists.29 This suggests that general practitioners, whose numbers will also drop, are going to be increasingly involved in managing mental illness, including severe mental disorders. In the current study, the general practitioners were not actively implicated by the psychiatrists in providing postdischarge care for first-episode psychotic patients, irrespective of patients’ length of stay in the hospital. Yet, it has been shown elsewhere that the follow-up of psychotic patients in general practice leads to more rapid social integration.30 The current study also shows that general practitioners have a role to play in dealing with both psychiatric and somatic health problems and in renewing and changing antipsychotic medication for those patients who do contact them. Better recognition of this role and a closer collaboration between general practitioners and psychiatrists, enhanced by interventions such as “collaborative care” for depression,31-33 are needed to support general practitioners in caring for psychotic patients.
Author affiliations: INSERM, U1061, University of Montpellier 1 (Drs Norton, Boulenger, Ritchie, and Capdevielle and Mss Jaussent and Prudhomme); Department of General Practice, University of Montpellier (Drs Rivoiron-Besset and David); and Department of Adult Psychiatry, La Colombiרre Hospital, University of Montpellier (Drs Boulenger and Capdevielle), Montpellier, France; and Faculty of Medicine, Imperial College, Saint Mary’s Hospital (Dr Ritchie) and Institute of Psychiatry (Dr Mann), London, United Kingdom.
Potential conflicts of interest: None reported.
Funding/support: The study was supported by a university hospital research grant from the Centre Hospital, University of Montpellier, Montpellier, France.
Acknowledgments: The authors would like to thank the staff of the La Colombiרre Psychiatric Hospital for their participation in the project and the general practitioners who took the time to complete and return the questionnaire.
REFERENCES
1. Ryu Y, Mizuno M, Sakuma K, et al. Deinstitutionalization of long-stay patients with schizophrenia: the 2-year social and clinical outcome of a comprehensive intervention program in Japan. Aust N Z J Psychiatry. 2006;40(5):462-470. PubMed
2. Kendrick T, Burns T, Freeling P, et al. Provision of care to general practice patients with disabling long-term mental illness: a survey in 16 practices. Br J Gen Pract. 1994;44(384):301-305. PubMed
3. Kendrick T, Burns T, Garland C, et al. Are specialist mental health services being targeted on the most needy patients? the effects of setting up special services in general practice. Br J Gen Pract. 2000;50(451):121-126. PubMed
4. Cole E, Leavey G, King M, et al. Pathways to care for patients with a first episode of psychosis: a comparison of ethnic groups. Br J Psychiatry. 1995;167(6):770-776. PubMed doi:10.1192/bjp.167.6.770
5. Platz C, Umbricht DS, Cattapan-Ludewig K, et al. Help-seeking pathways in early psychosis. Soc Psychiatry Psychiatr Epidemiol. 2006;41(12):967-974. PubMed doi:10.1007/s00127-006-0117-4
6. Shiers D, Lester H. Early intervention for first episode psychosis. BMJ. 2004;328(7454):1451-1452. PubMed doi:10.1136/bmj.328.7454.1451
7. Skeate A, Jackson C, Birchwood M, et al. Duration of untreated psychosis and pathways to care in first-episode psychosis: investigation of help-seeking behaviour in primary care. Br J Psychiatry Suppl. 2002;181(43):s73-s77. PubMed doi:10.1192/bjp.181.43.s73
8. Oud MJ, Schuling J, Slooff CJ, et al. Care for patients with severe mental illness: the general practitioner’s role perspective. BMC Fam Pract. 2009;10(1):29. PubMed doi:10.1186/1471-2296-10-29
9. Simon AE, Lauber C, Ludewig K, et al; Swiss Early Psychosis Project. General practitioners and schizophrenia: results from a Swiss survey. Br J Psychiatry. 2005;187(3):274-281. PubMed doi:10.1192/bjp.187.3.274
10. Simon AE, Lester H, Tait L, et al. The International Study on General Practitioners and Early Psychosis (IGPS). Schizophr Res. 2009;108(1-3):182-190. PubMed doi:10.1016/j.schres.2008.11.004
11. Verdoux H, Cougnard A, Grolleau S, et al. How do general practitioners manage subjects with early schizophrenia and collaborate with mental health professionals? a postal survey in south-western France. Soc Psychiatry Psychiatr Epidemiol. 2005;40(11):892-898. PubMed doi:10.1007/s00127-005-0975-1
12. Verdoux H, Cougnard A, Grolleau S, et al. A survey of general practitioners’ knowledge of symptoms and epidemiology of schizophrenia. Eur Psychiatry. 2006;21(4):238-244. PubMed doi:10.1016/j.eurpsy.2005.05.013
13. Cougnard A, Kalmi E, Desage A, et al. Pathways to care of first-admitted subjects with psychosis in south-western France. Psychol Med. 2004;34(2):267-276. PubMed doi:10.1017/S003329170300120X
14. Verdoux H, Tignol J. Focus on psychiatry in France. Br J Psychiatry. 2003;183(5):466-471. PubMed doi:10.1192/bjp.183.5.466
15. Chapireau F. Les recours aux soins spécialisés en santé mentale. DREES: Direction de la Recherche, des Etudes, de l’ Evaluation et des Statistiques. Etudes et Résultats. 2006;533:1-8.
16. Lafitte C, Martin C, Grabot D, et al. A survey of private practice psychiatrist’s training and activity in activity in Aquitaine, France, in 1993 [Article in French]. Encephale. 1996;22(6):417-421. PubMed
17. Réseau de Promotion pour la Santé Mentale. 78. Rapport de l’ enquête 2000 du Réseau de Promotion pour la Santé Mentale dans les Yvelines Sud. La Lettre de Promotion Santé Mentale Yvelines Sud. 2003:4.
18. Younes N, Gasquet I, Gaudebout P, et al. General Practitioners’ opinions on their practice in mental health and their collaboration with mental health professionals. BMC Fam Pract. 2005;6(1):18. PubMed doi:10.1186/1471-2296-6-18
19. Bourgueil Y, Marek A, Mousques J. Trois modרles types d’ organisation des soins primaires en Europe, au Canada, en Australie et en Nouvelle-Zélande. Quest Eco Santé. 2009:141.
20. Dourgnon P, Guillaume S, Naiditch M, et al. Les assurés et le médecin traitant: premier bilan aprרs la réforme. Quest Eco Santé. 2007:124.
21. World Health Organization. The ICD-10 Classification of Mental and Behavioral Disorders-Diagnostic Criteria for Research. Geneva, Switzerland: World Health Organization; 1993.
22. Deehan A, Templeton L, Taylor C, et al. The effect of cash and other financial inducements on the response rate of general practitioners in a national postal study. Br J Gen Pract. 1997;47(415):87-90. PubMed
23. Lang FH, Forbes JF, Murray GD, et al. Service provision for people with schizophrenia, 1: clinical and economic perspective. Br J Psychiatry. 1997;171(2):159-164. PubMed doi:10.1192/bjp.171.2.159
24. CNAMTS. Le médecin traitant, adopté par la majorité des Français, favorise la prévention. Communique. 2009;22:2009.
25. Nazareth I, King M, Davies S. Care of schizophrenia in general practice: the general practitioner and the patient. Br J Gen Pract. 1995;45(396):343-347. PubMed
26. Younרs N, Hardy-Bayle MC, Falissard B, et al. Differing mental health practice among general practitioners, private psychiatrists and public psychiatrists. BMC Public Health. 2005;5(1):104. PubMed doi:10.1186/1471-2458-5-104
27. Nazareth I, King M, Haines A, et al. Care of schizophrenia in general practice. BMJ. 1993;307(6909):910. PubMed doi:10.1136/bmj.307.6909.910
28. Norton J, De Roquefeuil G, David M, et al. The mental health of doctor-shoppers: experience from a patient-led fee-for-service primary care setting. J Affect Disord. 2011;131(1):428-432. doi:10.1016/j.jad.2010.12.009 PubMed
29. Norton J, David M, Boulenger JP. General practitioners are bearing an increasing burden of the care of common mental disorders in France. Eur J Psychiatry. 2007;21(1):63-70.
30. Capdevielle D, Ritchie K. The long and the short of it: are shorter periods of hospitalisation beneficial? Br J Psychiatry. 2008;192(3):164-165. PubMed doi:10.1192/bjp.bp.107.044719
31. Dietrich AJ, Oxman TE, Williams JW Jr, et al. Re-engineering systems for the treatment of depression in primary care: cluster randomised controlled trial. BMJ. 2004;329(7466):602. PubMed doi:10.1136/bmj.38219.481250.55
32. Gilbody S, Whitty P, Grimshaw J, et al. Educational and organizational interventions to improve the management of depression in primary care: a systematic review. JAMA. 2003;289(23):3145-3151. PubMed doi:10.1001/jama.289.23.3145
33. Upshur C, Weinreb L. A survey of primary care provider attitudes and behaviors regarding treatment of adult depression: what changes after a collaborative care intervention? Prim Care Companion J Clin Psychiatry. 2008;10(3):182-186. PubMed doi:10.4088/PCC.v10n0301