Objective: Relatively few studies have evaluated the clinical implications of lifetime attention-deficit/hyperactivity disorder (ADHD) in adults with bipolar disorder or major depressive disorder (MDD). Herein, we sought to determine the prevalence as well as the demographic and clinical correlates of lifetime ADHD in persons with a mood disorder.
Method: The first 399 patients enrolled in the International Mood Disorders Collaborative Project (IMDCP) were evaluated for lifetime ADHD using the Mini-International Neuropsychiatric Interview-Plus (MINI-Plus) as the primary instrument to derive current and lifetime DSM-IV diagnoses. All analyses of variables of interest were conducted utilizing the MINI-Plus, the Adult ADHD Self-Report Scale-v1.1, and the Wender Utah Rating Scale-Short Form. The effect of ADHD on clinical presentation, course of illness variables, comorbidity, anamnesis, treatment, and outcome are reported. The IMDCP is a joint initiative of the Mood Disorders Psychopharmacology Unit at the University Health Network, University of Toronto, Toronto, Ontario, Canada, and the Cleveland Clinic Center for Mood Disorders Treatment and Research at Lutheran Hospital, Cleveland, Ohio. All data for this study were procured between January 2008 and January 2009.
Results: The percentages of subjects with MDD or bipolar disorder meeting the DSM-IV criteria for lifetime adult ADHD were 5.4% and 17.6% (P < .001), respectively. Lifetime comorbid ADHD in both mood disorder populations was associated with earlier age at illness onset (MDD, P = .049; bipolar disorder, P = .005), a higher number of psychiatric comorbidities (eg, MDD and current panic disorder with agoraphobia [P = .002]; bipolar disorder and social phobia [P = .012]), and decreased quality of life (MDD, P = .018).
Conclusions: The overarching findings herein are that the adult ADHD phenotype is commonly reported by individuals with MDD or bipolar disorder and is associated with a greater illness burden and complexity.
Prim Care Companion J Clin Psychiatry 2010;12(3):e1-e7
© Copyright 2010 Physicians Postgraduate Press, Inc.
Submitted: July 9, 2009; accepted September 19, 2009.
Published online: May 27, 2010 (doi:10.4088/PCC.09m00861gry).
Corresponding author: Roger S. McIntyre, MD, FRCPC, Departments of Psychiatry and Pharmacology, University of Toronto, Mood Disorders Psychopharmacology Unit, University Health Network, 399 Bathurst St, Toronto, Ontario, Canada M5T 2S8 ([email protected]).
During the past decade, a similar composite has emerged for mood disorders and adult attention-deficit/hyperactivity disorder (ADHD).1-4 Both conditions have a relatively high prevalence, low case detection, protracted illness course, high rate of comorbidity, multifactorial etiology, substantial heritability of liability, substantial illness burden and economic cost, and significant interpersonal and vocational maladjustment. Moreover, results from neuroimaging investigations implicate common regions and neural circuits subserving essential features for both conditions.5-7
Clinical Points
- Attention-deficit/hyperactivity disorder (ADHD) is a common comorbidity in adults with mood disorders, with a higher prevalence in bipolar disorder compared to major depressive disorder.
- ADHD in the adult mood disorder population is associated with a more severe mood disorder course and presentation.
- All adults with mood disorder should be screened for features suggestive of ADHD.
Several epidemiologic and clinical studies have documented a high rate of lifetime ADHD in pediatric bipolar samples.8-11 Comorbid ADHD is associated with a more complex illness presentation and decreased response to lithium in young populations with bipolar disorder.12 Features of ADHD often persist into adulthood, implying homotypic continuity with the pediatric phenotype.13 Nevertheless, relatively few systematic studies of adults have evaluated the diagnostic and clinical implications of lifetime ADHD comorbidity in adults with bipolar disorder.14 Moreover, managing ADHD in the bipolar disorder population with conventional treatment (eg, psychostimulants) poses a hazard for destabilization of bipolar disorder.
To our knowledge, the only large systematic evaluation of the bipolar disorder-ADHD phenotype was conducted by the National Institute of Mental Health’s Systematic Treatment Enhancement Program for Bipolar Disorder (STEP-BD).14 The overall lifetime prevalence of comorbid ADHD in their cohort (N = 1,000) was 9.5% (14.7% for men; 5.8% for women). Individuals with comorbid bipolar disorder and ADHD had an earlier age at onset, shorter “well” intervals, a greater burden of depression, and higher rates of psychiatric comorbidity.
The primary aims of this initiative were to report on the prevalence and clinical implications of lifetime comorbid ADHD in individuals with either bipolar disorder or major depressive disorder (MDD). Our sample comprised the first consecutive 399 patients enrolled in the International Mood Disorders Collaborative Project (IMDCP) between the Mood Disorders Psychopharmacology Unit at the University Health Network, University of Toronto, Toronto, Ontario, Canada, and the Cleveland Clinic, Cleveland, Ohio.
METHOD
The IMDCP is a joint initiative of the Mood Disorders Psychopharmacology Unit at the University Health Network, University of Toronto, Toronto, Ontario, Canada, and the Cleveland Clinic Center for Mood Disorders Treatment and Research at Lutheran Hospital, Cleveland, Ohio. Both the Mood Disorders Psychopharmacology Unit and the Cleveland Clinic Center for Mood Disorders Treatment and Research are academic specialty research programs providing clinical service to adults (aged 18-65 years at the Toronto site and ≥ 18 years at the Cleveland site) seeking evaluation and treatment for MDD or bipolar disorder. The Mood Disorders Psychopharmacology Unit is exclusively an outpatient program while the Cleveland Clinic Center for Mood Disorders Treatment and Research offers both outpatient and inpatient services.
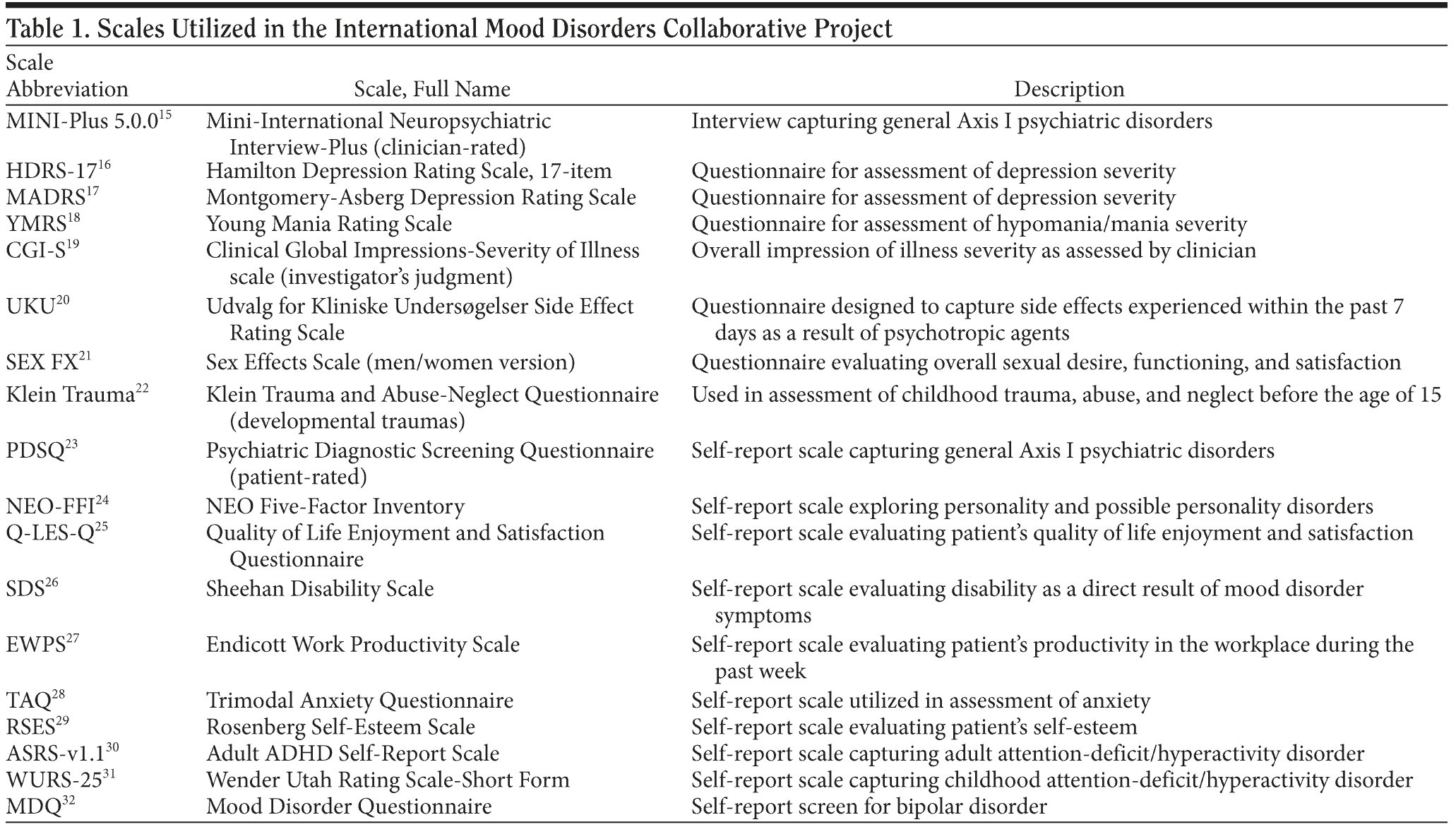
Both the Mood Disorders Psychopharmacology Unit and the Cleveland Clinic Center for Mood Disorders Treatment and Research have an established research platform in order to foster a structured approach to patient evaluation and initiation of standardized treatment protocols. Both centers share a battery of common assessments listed in Table 1. Exclusion criteria for entry into the IMDCP are unwillingness or inability to provide informed consent or to comply with study assessment.
The Mini-International Neuropsychiatric Interview-Plus (MINI-Plus) was the primary instrument used to derive DSM-IV diagnoses (current and lifetime). In the case of ADHD, this instrument does not differentiate between inattentive and hyperactive subtypes. The MINI-Plus-derived lifetime ADHD diagnosis is established if, prior to the age of 7, a subject meets 6 of 10 criteria for ADHD and, during adult years, a subject meets 9 of 14 criteria. The Adult ADHD Self-Report Scale (ASRS-v1.1) and the Wender Utah Rating Scale-Short Form (WURS-25) screen for adult and childhood ADHD, respectively. All analyses of variables of interest were conducted utilizing the MINI-Plus, the ASRS-v1.1, and the WURS-25. Our primary data analysis was based on the MINI-Plus lifetime ADHD diagnosis and provides data for ASRS-v1.1 and WURS-25 only when the respective results are discrepant from the MINI-Plus. Statistical correction for multiple comparisons was conducted.
The data for this analysis were procured from patients assessed at the mood disorder clinics located at the University Health Network and Lutheran Hospital between January 2008 and January 2009. All data were initially captured with paper versions of all scales and then either manually entered or scanned with automated capture software (TeleForm, Version 8; Syscom Services, Inc; Silver Spring, Maryland) prior to statistical analysis. Statistical analysis was conducted using SPSS for Windows, Versions 13.0 and 16.0 (SPSS Inc, Chicago, Illinois). The χ2 statistic was utilized for prevalence rates of nominal and ordinal variables. Independent-samples t tests were utilized for continuous dependent variables and dichotomous variables. All tests were 2-tailed, with statistical significance set at P < .05.
The Mood Disorders Psychopharmacology Unit research platforms at both centers were approved by the Research Ethics Board of the University Health Network, University of Toronto, and the Institutional Review Board of the Cleveland Clinic Foundation at Lutheran Hospital, respectively, and written informed consent was obtained from all subjects enrolled in the IMDCP.
RESULTS
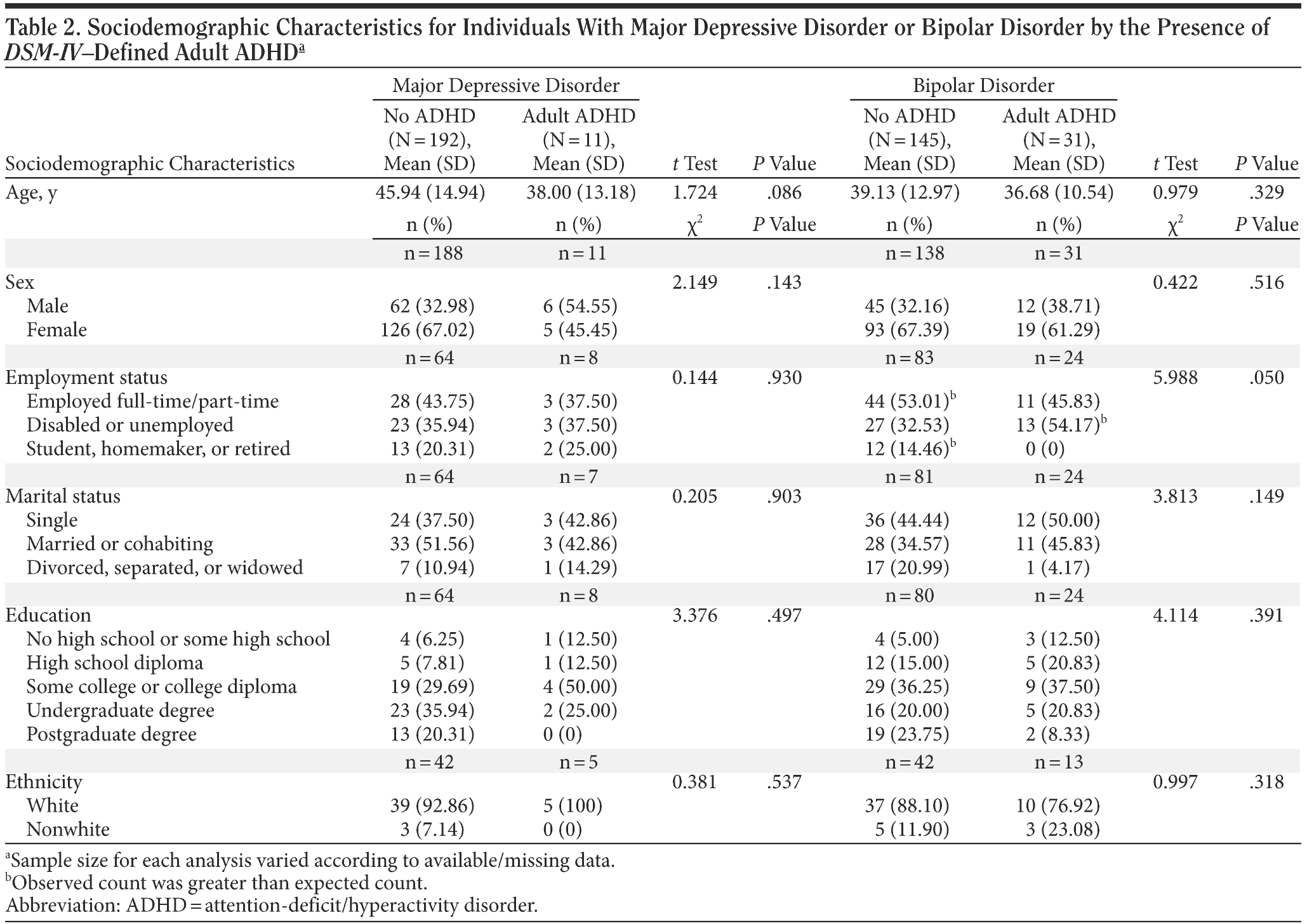
Demographic and clinical characteristics are presented in Table 2. The mean (SD) age of the cohort presenting with MDD or bipolar disorder with comorbid ADHD was 38.0 (13.2) years and 36.7 (10.5) years, respectively. The number (%) of subjects diagnosed with MDD, bipolar I, and bipolar II were 203 (50.9), 119 (29.8), and 56 (14.0), respectively. The predominant symptomatic presentation at entry and during assessment was depression. To our knowledge, no patients in the cohort were being actively treated for ADHD. Of the 399 patients, 20 were excluded from the analysis because of incomplete diagnostic data, resulting in a sample size of 379.
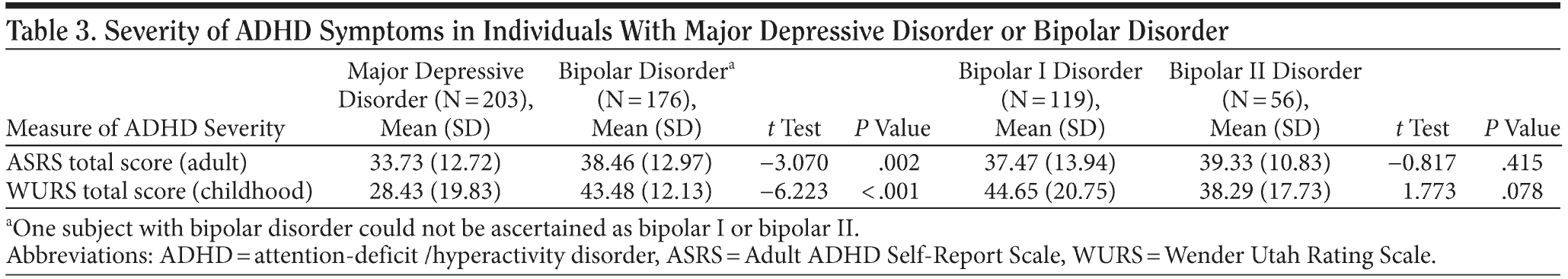
The percentages of subjects with MDD or bipolar disorder meeting criteria for a lifetime diagnosis of comorbid ADHD were 5.4% and 17.6% (P < .001), respectively. The prevalence of ADHD was significantly higher in bipolar disorder than in MDD, as evaluated using the MINI-Plus and the WURS-25, but not the ASRS-v1.1. We did not find a significant difference between the mood disorder groups in the rate of lifetime ADHD as a function of sex. Moreover, we did not find a significant difference between subpopulations with bipolar I or bipolar II disorder in the rate of lifetime ADHD.
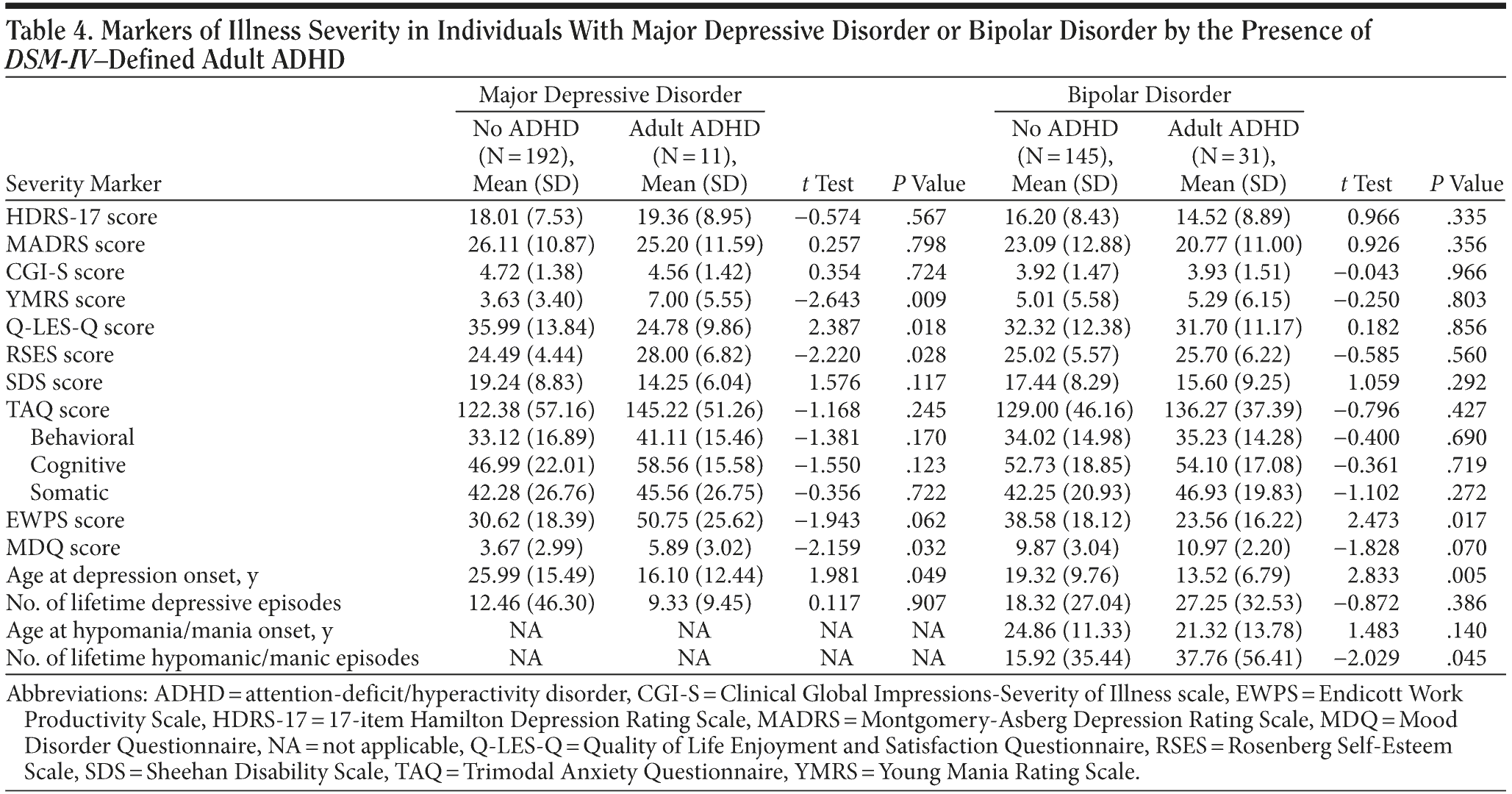
Baseline depression severity, as measured by the total Montgomery-Asberg Depression Rating Scale (MADRS) score, as well as the Clinical Global Impressions-Severity of Illness score, was not significantly different between groups. Individuals with MDD meeting ASRS-v1.1 criteria for ADHD had higher levels of depression severity as evaluated by both the MADRS and the Hamilton Depression Rating Scale, a difference not observed in the bipolar sample (Tables 3 and 4). Individuals meeting criteria for MDD and lifetime ADHD had lower quality of life ratings, as measured by the Quality of Life Enjoyment and Satisfaction Questionnaire, when compared to those with MDD but without ADHD. Quality of life ratings in individuals with bipolar disorder did not differ as a function of ADHD comorbidity.
The mean (SD) age at onset for the initial affective episode was earlier in individuals with MDD with comorbid ADHD (16.10 [12.44] years vs 25.99 [15.49] years) and in bipolar individuals with comorbid ADHD (13.52 [6.79] years vs 19.32 [9.76] years) compared to those without lifetime ADHD. The mean (SD) age at hypomania/mania onset in the bipolar population was also earlier in the comorbid subgroup (21.32 [13.78] years) than in those without lifetime ADHD comorbidity (24.86 [11.33] years).
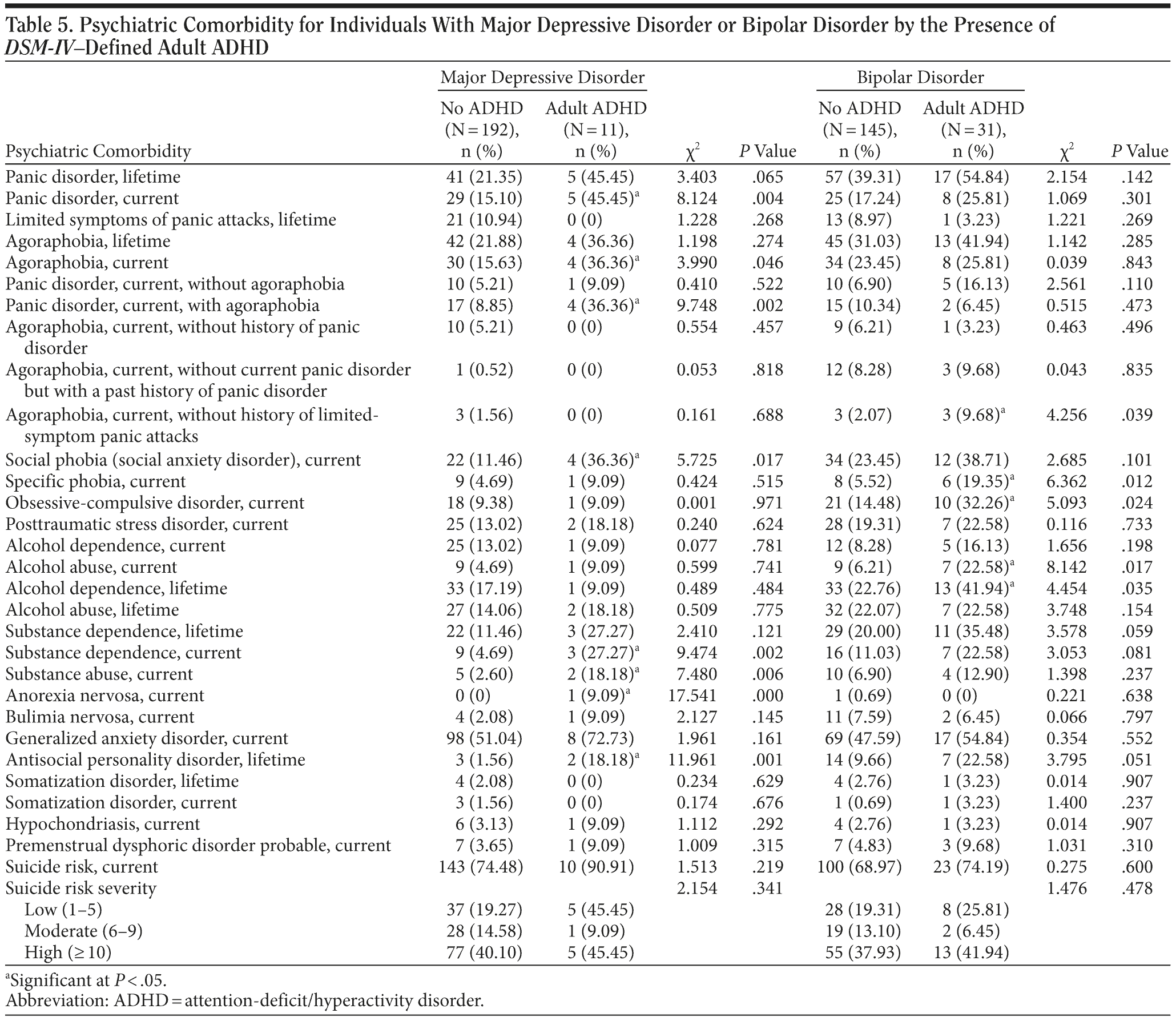
There were no differences in the frequency of affective episodes in either the MDD or bipolar disorder groups as a function of lifetime ADHD (Table 5). Moreover, individuals with lifetime comorbid ADHD were similar to those without comorbid ADHD in their MINI-Plus suicide risk severity score and current suicide risk. Lifetime ADHD was associated with a higher rate of antisocial personality disorder in both MDD and bipolar disorder.
Individuals with MDD and lifetime comorbid ADHD had a significantly higher rate for panic disorder-current, agoraphobia-current, social anxiety disorder-current, substance abuse and dependence-current, and antisocial personality disorder-lifetime. Individuals with bipolar disorder meeting criteria for ADHD were also more likely to meet criteria for agoraphobia-current, alcohol abuse-current, alcohol dependence-lifetime, and antisocial personality disorder-lifetime (Table 5).
Patients meeting criteria for both bipolar disorder and lifetime ADHD, but not patients with comorbid MDD and ADHD, had lower work productivity scores as measured by the Endicott Work Productivity Scale. Also, individuals with comorbid bipolar disorder and ADHD were relatively more likely to be currently unemployed or receiving disability.
DISCUSSION
The overarching findings of our analysis are that the ADHD phenotype is commonly reported in adult individuals with a mood disorder. Individuals with bipolar disorder are approximately 3 to 4 times more likely to receive a comorbid ADHD diagnosis than are those individuals with MDD. Notwithstanding the fact that our sample was numerically modest when compared to the STEP-BD cohort, the rate of comorbid ADHD in our bipolar subsample was similar to their observations. Moreover, a separate Turkish study with a bipolar sample (N = 159) similar to ours reported a 16.3% prevalence rate of adult ADHD.33,34
The STEP-BD group14 reported that individuals with bipolar I disorder were differentially affected by lifetime comorbid ADHD when compared to individuals with bipolar II disorder. We also observed a higher percentage of bipolar I individuals versus bipolar II individuals affected by lifetime ADHD. Admittedly, the population sample in our group of individuals with bipolar disorder in general, and more specifically, bipolar II disorder, was considerably smaller than in the STEP-BD group.
Among individuals with MDD, the presence of comorbid lifetime ADHD was associated with an age at mood disorder onset approximately 10 years earlier when compared to those without ADHD. For individuals with bipolar disorder, those with lifetime ADHD had a mood disorder age at onset approximately 6 years earlier than those without ADHD. The STEP-BD group14 reported that the age at bipolar disorder onset in individuals with ADHD was approximately 5 years earlier than in those without ADHD. The pertinacity of these collective observations relates to the question of whether or not the “comorbidity” of ADHD and bipolar disorder in younger populations reflects distinct comorbidity, overlapping syndromes, or heterotypic continuity.35
Converging with results from both epidemiologic and clinical studies, individuals in the IMDCP with MDD or bipolar disorder and lifetime comorbid ADHD were differentially affected by anxiety disorder as well as substance use disorders.4 Moreover, the subjects with comorbid ADHD were more likely to meet criteria for antisocial personality disorder. The STEP-BD group14 reported that individuals with bipolar disorder and ADHD had a greater frequency and earlier age at onset of violence and legal problems.
There are several methodological limitations that affect inferences and interpretation of our results. Most subjects were experiencing symptoms related to a mood disorder; as such, there is no definitive mechanism to assure that overdiagnosis (or underreporting) of ADHD did not occur.14 A second limitation relates to the representativeness of individuals utilizing university-based mood clinics, as well as Berkson’s bias.36 Third, our attempt to look at both MDD and bipolar disorder subpopulations as a function of ADHD comorbidity resulted in a relatively small sample size. A separate limitation relates to interrater reliability between sites. Both the Toronto and Cleveland sites have demonstrated interrater reliability at each respective center; at the time of data-capture analysis herein, both centers had not demonstrated interrater concordance with respect to MINI-Plus-derived diagnosis. Notwithstanding this latter limitation, both centers have extensive experience in clinical trials utilizing the MINI-Plus as well as other diagnostic and rating instruments.
In addition, our dataset was missing a significant number of data points across several variables. The primary reason for missing data relates to the time-consuming nature of the data-gathering process (eg, up to 2 hours in duration) that was unacceptable to many individuals utilizing services at both centers. Moreover, although we corrected for multiple comparisons, we conducted a large number of statistical tests on a relatively small subsample size, thereby introducing a risk for type 1 error. Finally, most individuals with comorbid ADHD were not receiving guideline-concordant care for that condition, raising the possibility that the increased severity in the mood disorder-ADHD group was in part due to insufficient treatment of ADHD.
Taken together, the IMDCP results represent a partial replication of several findings previously reported by the STEP-BD group.14 Our results extend the observations further by separately reporting on similar variables in individuals with MDD. The greater burden associated with the ADHD phenotype in mood disorder populations invites the need for adequately designed clinical trials aiming to establish safe and effective pharmacologic and psychosocial approaches in individuals meeting criteria for both conditions.
Drug name: lithium (Lithobid and others).
Author affiliations: Department of Psychiatry (Drs McIntyre and Kennedy), Department of Pharmacology (Dr McIntyre), and Institute of Medical Science (Drs McIntyre and Kennedy and Ms Soczynska), University of Toronto, Toronto, Ontario, Canada; Mood Disorders Psychopharmacology Unit, University Health Network, Toronto, Ontario, Canada (Drs McIntyre, Kennedy, and Nathanson and Mss Soczynska, Nguyen, Woldeyohannes, Joshi, and Cheng); Bilkey Clinic, Barrie, Ontario, Canada (Dr Bilkey); and Center for Mood Disorders Treatment and Research, Cleveland Clinic, Cleveland, Ohio (Ms Benson and Dr Muzina).
Potential conflicts of interest: Dr McIntyre has received research grants from Stanley Medical Research Institute, NARSAD, and Eli Lilly; has been a member of the advisory boards of AstraZeneca, Bristol-Myers Squibb, France Foundation, GlaxoSmithKline, Janssen-Ortho, Solvay/Wyeth, Eli Lilly, Organon, Lundbeck, Biovail, Pfizer, and Shire; has served on speakers bureaus for Janssen-Ortho, AstraZeneca, Eli Lilly, Lundbeck, and Biovail; and has performed continuing medical education activities for AstraZeneca, Bristol-Myers Squibb, France Foundation, 13CME, Solvay/Wyeth, and Physicians Postgraduate Press. Dr Kennedy has been a consultant for St Jude Medical, Biovail, Eli Lilly, GlaxoSmithKline, Janssen-Ortho, Lundbeck, Servier, Wyeth, and AstraZeneca; has received grant/research support from St Jude Medical, AstraZeneca, BrainCells, Eli Lilly, GlaxoSmithKline, Janssen-Ortho, Lundbeck, and Merck Frosst; and has received honoraria from and served on speakers or advisory boards for AstraZeneca, Biovail, Eli Lilly, GlaxoSmithKline, Janssen-Ortho, Lundbeck, Servier, and Wyeth. Dr Bilkey has received honoraria or other fees for presentations from Janssen-Ortho, Shire BioChem, Lundbeck, Eli Lilly, and Biovail; has participated in advisory boards or similar committees for Janssen-Ortho, Shire BioChem, Eli Lilly, and Biovail; and has participated in or continues to participate in clinical trials for Shire BioChem and Eli Lilly. Dr Muzina has received grant/research support from Repligen and has received honoraria from AstraZeneca, Pfizer, and Wyeth. Dr Nathanson and Mss Soczynska, Nguyen, Woldeyohannes, Joshi, Cheng, and Benson report no financial or other relationships relevant to the subject of this article.
Funding/support: This research project was supported by an unrestricted grant from Shire Canada Inc.
REFERENCES
1. Faraone SV. ADHD in adults—a familiar disease with unfamiliar challenges. CNS Spectr. 2007;12(suppl 23):14-17. PubMed
2. Biederman J. Attention-deficit/hyperactivity disorder: a selective overview. Biol Psychiatry. 2005;57(11):1215-1220. PubMed doi:10.1016/j.biopsych.2004.10.020
3. McIntyre RS, Konarski JZ. Bipolar disorder: a national health concern. CNS Spectr. 2004;9(suppl 12):6-15. PubMed
4. Kessler RC, Adler L, Barkley R, et al. The prevalence and correlates of adult ADHD in the United States: results from the National Comorbidity Survey Replication. Am J Psychiatry. 2006;163(4):716-723. PubMed doi:10.1176/appi.ajp.163.4.716
5. Spencer TJ, Biederman J, Wilens TE, et al. Overview and neurobiology of attention-deficit/hyperactivity disorder. J Clin Psychiatry. 2002;63(suppl 12):3-9. PubMed
6. Konarski JZ, McIntyre RS, Kennedy SH, et al. Volumetric neuroimaging investigations in mood disorders: bipolar disorder versus major depressive disorder. Bipolar Disord. 2008;10(1):1-37. PubMed
7. Seidman LJ, Valera EM, Makris N. Structural brain imaging of attention-deficit/hyperactivity disorder. Biol Psychiatry. 2005;57(11):1263-1272. PubMed doi:10.1016/j.biopsych.2004.11.019
8. Wozniak J, Biederman J, Mundy E, et al. A pilot family study of childhood-onset mania. J Am Acad Child Adolesc Psychiatry. 1995;34(12):1577-1583. PubMed doi:10.1097/00004583-199512000-00007
9. West SA, McElroy SL, Strakowski SM, et al. Attention deficit hyperactivity disorder in adolescent mania. Am J Psychiatry. 1995;152(2):271-273. PubMed
10. Geller B, Zimerman B, Williams M, et al. Diagnostic characteristics of 93 cases of a prepubertal and early adolescent bipolar disorder phenotype by gender, puberty and comorbid attention deficit hyperactivity disorder. J Child Adolesc Psychopharmacol. 2000;10(3):157-164. PubMed doi:10.1089/10445460050167269
11. Borchardt CM, Bernstein GA. Comorbid disorders in hospitalized bipolar adolescents compared with unipolar depressed adolescents. Child Psychiatry Hum Dev. 1995;26(1):11-18. PubMed doi:10.1007/BF02353226
12. Strober M, DeAntonio M, Schmidt-Lackner S, et al. Early childhood attention deficit hyperactivity disorder predicts poorer response to acute lithium therapy in adolescent mania. J Affect Disord. 1998;51(2):145-151. PubMed doi:10.1016/S0165-0327(98)00213-4
13. Wilens TE, Biederman J, Wozniak J, et al. Can adults with attention-deficit/hyperactivity disorder be distinguished from those with comorbid bipolar disorder? findings from a sample of clinically referred adults. Biol Psychiatry. 2003;54(1):1-8. PubMed doi:10.1016/S0006-3223(02)01666-9
14. Nierenberg AA, Miyahara S, Spencer T, et al. STEP-BD Investigators. Clinical and diagnostic implications of lifetime attention-deficit/hyperactivity disorder comorbidity in adults with bipolar disorder: data from the first 1000 STEP-BD participants. Biol Psychiatry. 2005;57(11):1467-1473. PubMed doi:10.1016/j.biopsych.2005.01.036
15. Sheehan DV, Lecrubier Y, Sheehan KH, et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry. 1998;59(suppl 20):22-33. PubMed
16. Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry. 1960;23(1):56-62. PubMed doi:10.1136/jnnp.23.1.56
17. Montgomery SA, Asberg M. A new depression scale designed to be sensitive to change. Br J Psychiatry. 1979;134(4):382-389. PubMed doi:10.1192/bjp.134.4.382
18. Young RC, Biggs JT, Ziegler VE, et al. A rating scale for mania: reliability, validity and sensitivity. Br J Psychiatry. 1978;133(5):429-435. PubMed doi:10.1192/bjp.133.5.429
19. Kadouri A, Corruble E, Falissard B. The improved Clinical Global Impression Scale (iCGI): development and validation in depression. BMC Psychiatry. 2007;7(1):7. PubMed doi:10.1186/1471-244X-7-7
20. Lingjærde O, Ahlfors UG, Bech P, et al. The UKU side effect rating scale. A new comprehensive rating scale for psychotropic drugs and a cross-sectional study of side effects in neuroleptic-treated patients. Acta Psychiatr Scand Suppl. 1987;76(s334):1-100. PubMed doi:10.1111/j.1600-0447.1987.tb10566.x
21. Kennedy SH, Fulton KA, Bagby RM, et al. Sexual function during bupropion or paroxetine treatment of major depressive disorder. Can J Psychiatry. 2006;51(4):234-242. PubMed
22. Lizardi H, Klein DN, Ouimette PC, et al. Reports of the childhood home environment in early-onset dysthymia and episodic major depression. J Abnorm Psychol. 1995;104(1):132-139. PubMed doi:10.1037/0021-843X.104.1.132
23. Zimmerman M, Mattia JI. The reliability and validity of a screening Questionnaire for 13 DSM-IV Axis I disorders (the Psychiatric Diagnostic Screening Questionnaire) in psychiatric outpatients. J Clin Psychiatry. 1999;60(10):677-683. PubMed
24. McCrae RR, Costa PT Jr. A contemplated revision of the NEO Five-Factor Inventory. Pers Individ Dif. 2004;36(3):587-596. doi:10.1016/S0191-8869(03)00118-1
25. Ritsner M, Kurs R, Gibel A, et al. Validity of an abbreviated quality of life enjoyment and satisfaction questionnaire (Q-LES-Q-18) for schizophrenia, schizoaffective, and mood disorder patients. Qual Life Res. 2005;14(7):1693-1703. PubMed doi:10.1007/s11136-005-2816-9
26. Leon AC, Olfson M, Portera L, et al. Assessing psychiatric impairment in primary care with the Sheehan Disability Scale. Int J Psychiatry Med. 1997;27(2):93-105. PubMed
27. Endicott J, Nee J. Endicott Work Productivity Scale (EWPS): a new measure to assess treatment effects. Psychopharmacol Bull. 1997;33(1):13-16. PubMed
28. Lehrer PM, Woolfolk RL. Self-report assessment of anxiety: somatic, cognitive, and behavioral modalities. Behav Assess. 1982;4(2):167-177.
29. Rosenberg M. Conceiving the Self. New York, NY: Basic Books; 1979.
30. Kessler RC, Adler L, Ames M, et al. The World Health Organization Adult ADHD Self-Report Scale (ASRS): a short screening scale for use in the general population. Psychol Med. 2005;35(2):245-256. PubMed doi:10.1017/S0033291704002892
31. Ward MF, Wender PH, Reimherr FW. The Wender Utah Rating Scale: an aid in the retrospective diagnosis of childhood attention deficit hyperactivity disorder. Am J Psychiatry. 1993;150(6):885-890. PubMed
32. Hirschfeld RM, Williams JB, Spitzer RL, et al. Development and validation of a screening instrument for bipolar spectrum disorder: the Mood Disorder Questionnaire. Am J Psychiatry. 2000;157(11):1873-1875. PubMed doi:10.1176/appi.ajp.157.11.1873
33. Tamam L, Karakus G, Ozpoyraz N. Comorbidity of adult attention-deficit hyperactivity disorder and bipolar disorder: prevalence and clinical correlates. Eur Arch Psychiatry Clin Neurosci. 2008;258(7):385-393. PubMed doi:10.1007/s00406-008-0807-x
34. Alpert JE, Maddocks A, Nierenberg AA, et al. Attention deficit hyperactivity disorder in childhood among adults with major depression. Psychiatry Res. 1996;62(3):213-219. PubMed doi:10.1016/0165-1781(96)02912-5
35. McIntyre RS, Keck PE Jr. Comorbidity in bipolar disorder: clinical and research opportunities. Bipolar Disord. 2006;8(6):645-647. PubMed doi:10.1111/j.1399-5618.2006.00409.x
36. Feinstein AR, Walter SD, Horwitz RI. An analysis of Berkson’s bias in case-control studies. J Chronic Dis. 1986;39(7):495-504. PubMed doi:10.1016/0021-9681(86)90194-3