A Case of Autoimmune Encephalitis in a Patient With Alcohol Use Disorder
We present a case of a patient with alcohol use disorder (AUD) and new-onset mental status changes due to anti-N-methyl-d-aspartate (NMDA) receptor (anti-NMDAR) encephalitis. AUD was a confounding factor, and accurate diagnosis and treatment were found at the crossroads of addiction psychiatry and neurology. The patient returned to baseline cognition after 5 days of intravenous immunoglobulin (IVIG).
Description of Case
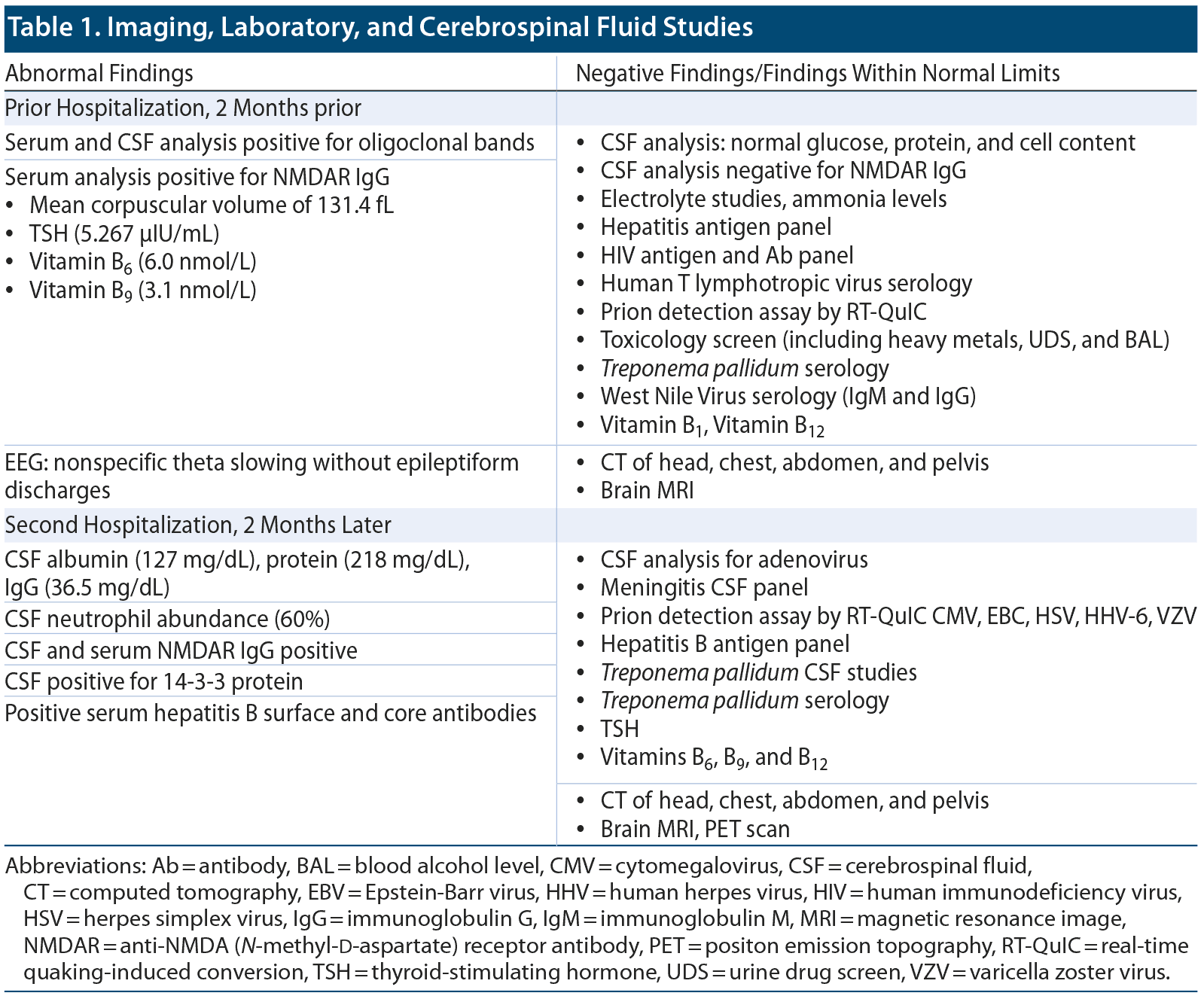
A 37-year-old Black woman was brought to the hospital after her partner found her at home, awake and seemingly alert but nonverbal except for bursts of profanity. He noted that onset of these behaviors had followed an episode of drinking. The patient took no medications and had no significant medical problems apart from AUD (per DSM-5 criteria). She was admitted to the general hospital service with amnesia, lethargy, psychomotor retardation, and flattened affect. Consults were ordered for addiction psychiatry and neurology, and the patient received an extensive neurologic workup including imaging and laboratory studies. Findings of urine drug screen (UDS) and blood alcohol level (BAL) testing were negative. Imaging was unremarkable, and electroencephalogram showed nonspecific theta slowing. A list of pertinent diagnostic study findings is reported in Table 1.
Symptom-triggered benzodiazepine treatment was initiated for suspected alcohol withdrawal. The patient showed no autonomic signs of alcohol withdrawal and became increasingly confused while receiving benzodiazepines, leading to their being discontinued on hospital day 9. Despite thiamine levels within normal limits, the patient received parenteral supplementation for the duration of her hospital stay, along with daily multivitamin and folic acid.
Addiction psychiatry specialists believed the patient’s presentation was not consistent with alcohol withdrawal. Her unexplained fluctuating mentation in the setting of primarily unremarkable laboratory and imaging findings thus led to considering cerebrospinal fluid (CSF) studies. The CSF encephalitis panel included NMDAR antibodies, oligoclonal bands, and other markers seen in a variety of neurologic diseases. The patient’s results returned shortly prior to discharge and showed oligoclonal bands in the serum and the CSF and anti-NMDAR antibodies (NMDAR IgG) in the serum but not the CSF.
On hospital day 20, the patient’s mentation spontaneously recovered to its baseline level. She was discharged in stable condition without a clear etiology for her presenting symptoms. Wernicke encephalopathy was considered earlier in the hospitalization, but was later deemed unlikely given the spontaneous remission of altered mentation and thiamine levels within normal limits. The official diagnoses at the time of discharge were altered mentation, AUD, and vitamin deficiencies (vitamins B3, B6, and D).
One month later, the patient’s sister found her disrobed in her neighborhood in the snowy winter weather. The patient was incoherent and non-redirectable; her sister brought her to the hospital with concerns about recent alcohol use. Onset was preceded by 1 week of irritability, fatigue, decreased appetite, and auditory and visual hallucinations. Notable findings on the second admission were a reduction in body mass index from 26.37 to 19.03 kg/m2, persecutory and grandiose delusions, ideas of reference, agitation, and social disinhibition. Findings of BAL testing and UDS were again negative, although collateral information from family suggested recent alcohol use. Over several days, the patient grew progressively more agitated, requiring a bedside sitter to prevent elopement. Benzodiazepines were used as needed for recurrent episodes of acute agitation and disorientation for the first 7 days of the hospitalization with minimal improvement of mental status. Addiction psychiatry specialists were consulted to help with management of agitation and psychosis; benzodiazepines were discontinued, and olanzapine 10 mg was initiated at bedtime with an additional 5 mg of olanzapine as needed for agitation on hospital days 8-13, resulting in significant reduction in agitation and psychotic symptoms.
Neurology workup from the first admission was reviewed and partially repeated due to unusual findings of negative CSF markers in the setting of positive serum markers. (Table 1). This time, NMDAR IgG was positive in the CSF and the serum. Malignancy screen using positron emission tomography scan was unrevealing. A 5-day course of IVIG treatment was initiated, and the patient’s mentation improved dramatically, returning to its baseline level by day 5. Olanzapine was discontinued on the last day of IVIG treatment.
The patient expressed a desire for sobriety from alcohol but an unwillingness to pursue formal treatment. She was amenable to a trial of naltrexone 50 mg daily and committed to following up with her primary care physician for ongoing management. Outpatient neurology follow-up was also scheduled. The patient was discharged without the need for antipsychotics or ongoing psychiatric care.
Discussion
Patients that present to the health care system with predominantly psychiatric symptoms can have an underlying medical disease. Determining whether symptoms are from a primary psychiatric disorder or secondary to another medical condition can pose a diagnostic dilemma. Psychiatric diagnostic criteria are rarely pathognomonic and often overlap with symptoms of medical illness.1 When features of an illness are atypical of any suspected psychiatric disease, alternative medical etiologies should be considered.2 Although substance use disorder has significant comorbidity with psychotic disorders,3 primary psychiatric and addiction etiology are diagnoses of exclusion, particularly if the alternative diagnosis is a potentially treatable autoimmune disease.4
A conclusive diagnosis of anti-NMDAR encephalitis requires positive NMDAR IgG in both the serum and the CSF.5,6 It is atypical for anti-NMDAR encephalitis to present with positive serum but not matching positive CSF NMDAR IgG,5,6 as was the case in our patient’s first hospitalization, although matching positive oligobands are found in only about 60% of cases.7 Because onset of symptoms and positive laboratory markers may not strictly coincide, careful consideration of all potential causes is critical.
In times of diagnostic uncertainty, attributing seemingly unexplained symptoms to a patient’s history of substance use disorder, such as Wernicke encephalopathy, may seem appealing. In our patient’s case, thiamine levels within normal limits and spontaneous resolution of symptoms during the first hospitalization, in conjunction with positive NMDAR IgG in both the serum and CSF on the second admission, ruled out this diagnosis.
Conclusion
In this case report, we present the onset and course of anti-NMDAR encephalitis in a patient with alcohol use disorder. Determining the diagnosis was complicated by suspected alcohol withdrawal, and evaluation by addiction psychiatry specialists helped prompt workup for other medical etiologies. Our patient returned to baseline cognition after a course of IVIG and was discharged without the need for psychotropic medications.
Published online: December 10, 2020.
Potential conflicts of interest: Dr Balasanova and Mr Valquier report no conflicts of interest.
Funding/support: There were no sources of financial or material support. There were no sources of external funding.
Patient consent: The patient has provided permission to publish these features of her case, and the identity of the patient has been protected.
REFERENCES
1.McKee J, Brahm N. Medical mimics: differential diagnostic considerations for psychiatric symptoms. Ment Health Clin. 2016;6(6):289-296. PubMed CrossRef
2.Freudenreich O. Differential diagnosis of psychotic symptoms: medical mimics. Psychiatr Times. 2010;27(12):56-61.
3.Caton CLM, Drake RE, Hasin DS, et al. Differences between early-phase primary psychotic disorders with concurrent substance use and substance-induced psychoses. Arch Gen Psychiatry. 2005;62(2):137-145. PubMed CrossRef
4.Davies G, Irani SR, Coltart C, et al. Anti-N-methyl-d-aspartate receptor antibodies: a potentially treatable cause of encephalitis in the intensive care unit. Crit Care Med. 2010;38(2):679-682. PubMed CrossRef
5.Graus F, Titulaer MJ, Balu R, et al. A clinical approach to diagnosis of autoimmune encephalitis. Lancet Neurol. 2016;15(4):391-404. PubMed CrossRef
6.Kayser MS, Dalmau J. Anti-NMDA receptor encephalitis in psychiatry. Curr Psychiatry Rev. 2011;7(3):189-193. PubMed CrossRef
7.Dalmau J, Lancaster E, Martinez-Hernandez E, et al. Clinical experience and laboratory investigations in patients with anti-NMDAR encephalitis. Lancet Neurol. 2011;10(1):63-74. PubMed CrossRef
aCollege of Medicine, University of Nebraska Medical Center, Omaha, Nebraska
bDepartment of Psychiatry, College of Medicine, University of Nebraska Medical Center, Omaha, Nebraska
*Corresponding author: Alëna A. Balasanova, MD, Department of Psychiatry, Poynter Hall 5th Floor, University of Nebraska Medical Center, 985578 Nebraska Medical Center, Omaha, NE 68198-5578 ([email protected]).
Prim Care Companion CNS Disord 2020;22(6):20l02606
To cite: Valquier CL, Balasanova AA. A case of autoimmune encephalitis in a patient with alcohol use disorder. Prim Care Companion CNS Disord. 2020;22(6):20l02606.
To share: https://doi.org/10.4088/PCC.20l02606
© Copyright 2020 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!