Bipolar Disorder Comorbid With Attention-Deficit/Hyperactivity Disorder in Adult Inpatients With Acute Relapse

ABSTRACT
Objective: The aim of this prospective, observational study was to detect the rate of comorbid attention-deficit/hyperactivity disorder (ADHD) in a sample of inpatients diagnosed with bipolar disorder, and to identify differences between patients with bipolar disorder with concomitant ADHD and those without concomitant ADHD.
Method: Fifty subjects with bipolar disorder (DSM-IV-TR criteria) aged 18 to 65 years were enrolled in the study in Kingston, Ontario, from October 2008 to April 2010, following their admission to an adult inpatient psychiatric unit during an acute relapse. The Mini-International Neuropsychiatric Interview (MINI) and the ADHD Rating Scale were used to screen the subjects for ADHD and bipolar disorder, while the Hamilton Depression Rating Scale, the Young Mania Rating Scale, and the Global Assessment of Function were used to assess clinical severity at baseline and at 8 weeks.
Results: Thirteen (26%) of the enrolled patients rated positive for ADHD on both the MINI and the ADHD Rating Scale. At baseline, no differences were found between the patients with ADHD and those without ADHD with regard to gender, age, length of hospitalization, and severity of clinical and functional deterioration. At 8 weeks, patients with ADHD had lower general scores for depression (P = .025) than those without ADHD.
Conclusions: In a psychiatric inpatient sample, patients with bipolar disorder and ADHD were not more severely ill in the acute phase and did not have a poorer outcome at 8 weeks.
Prim Care Companion CNS Disord 2013;15(4):doi:10.4088/PCC.12m01495
© Copyright 2013 Physicians Postgraduate Press, Inc.
Submitted: November 23, 2012; accepted February 18, 2013.
Published online: July 4, 2013.
Corresponding author: Alina Marin, MD, PhD, Department of Psychiatry, Queen’s University, 166 Brock St, Room J5-008, Kingston, Ontario, K7L 5G2, Canada ([email protected]).
The diagnostic category of attention-deficit/hyperactivity disorder (ADHD) in adults has recently received increased consideration. Although it has been independently validated,1 adult ADHD has been found to be comorbid with a considerable number of other disorders.2-4 The concomitance of ADHD with bipolar disorder deserves special attention, as both clinical entities affect a large proportion of the population and have a significant impact on the patients’ functionality. Results of prospective, longitudinal studies of high-risk youth have shown that, early in the development and clinical course of bipolar disorder, symptoms appear to be nonspecific and often overlap with those of ADHD.5 There is a pressing need to further elucidate the exact nature of the clinical overlaps in these diagnosis categories and their implication for clinical outcomes.6 Among the adult population, previous research has reported that roughly 9% to 21% of adults are diagnosed as having both ADHD and bipolar disorder, depending on the study methodology and diagnosis process involved.7-9
Earlier studies with children and adolescents have documented a strong association between ADHD and bipolar disorder, with a recent meta-analysis supporting the idea that the age at onset, the response to treatment, and the outcome of bipolar disorder are all influenced by the co-occurrence of ADHD. Strong associations between early onset of bipolar disorder and rates of lifetime ADHD have been suggested, with patients who have a history of ADHD also reporting a more chronic and disabling course of bipolar disorder.7
The association between ADHD and bipolar disorder is a serious public health issue. Patients with both ADHD and bipolar disorder often lead high-risk lives, as they may be chronically impulsive or subject to dangerous behavior. During the course of their illness, these individuals may become suicidal, or they may lose cognitive control over their actions and concomitantly engage in dangerous behaviors. Unfortunately, this clinical association is often overlooked due in part to the fact that most of these individuals lose the full syndromatic presentation of ADHD when they reach adulthood, which increases the risk of the disease being underdiagnosed.1,10 Furthermore, considerable symptom overlap of the 2 clinical entities during acute episodes of bipolar disorder hinders the accurate diagnosis of the comorbidity. The diagnosis of ADHD in adults also requires a childhood history of the disorder, which is sometimes difficult to confirm.
Several studies have been conducted on adult patients with concomitant bipolar disorder and ADHD. In some of these studies, the diagnosis of ADHD was based solely on patient self-report, which raises serious methodological concerns regarding the accuracy of the retrospective presence of the childhood symptoms.6 It has been hypothesized that concomitance of ADHD aggravates the mood symptoms and the outcome of bipolar disorder. To our knowledge, no research has yet been conducted on acutely ill patients, and no study has taken into consideration variation in severity of bipolar symptomatology. More information regarding the impact of comorbid ADHD and the relapse severity in bipolar disorder, as well as the recovery rates, may be crucial for improving the care and the outcomes in bipolar disorder.
The purpose of this study was to detect the rate of comorbid ADHD in a sample of inpatients diagnosed with bipolar disorder and to compare the clinical and functional outcomes in adult patients with bipolar disorder to those with bipolar disorder and concomitant ADHD within the acute inpatient population. We hypothesized that individuals diagnosed with bipolar disorder and comorbid ADHD are more likely to undergo severe deterioration during their acute phases and have poorer outcomes with regard to their bipolar episodes as compared to those individuals without this comorbid burden.

- Inpatient treatment during acute relapses can result in better outcomes for patients with bipolar disorder and attention-deficit/hyperactivity disorder (ADHD).
- Systematic ratings of the mood symptoms and functional impairment in patients with coexisting ADHD and bipolar disorder can help provide a better understanding of the long-term course of this comorbid condition.
METHOD
This was a prospective, observational study. The study population consisted entirely of patients diagnosed with bipolar disorder who were admitted to an acute care hospital in Kingston, Ontario, Canada. All individuals, both male and female ranging between the ages of 18 and 65 years, who met the DSM-IV-TR criteria for bipolar disorder and were admitted to our adult psychiatric inpatient unit over the 18-month recruitment period (from October 2008 to April 2010) were considered for inclusion. Patients with severe comorbid medical disorders, possibly impinging on patients’ functioning, or those declared incompetent upon admission and whose issues of competence had not resolved after 17 days of admission were excluded. People living too far away and thus unable to return for the follow-up were also excluded.
Diagnoses of bipolar disorder and ADHD were confirmed with a structured diagnostic interview. Baseline clinical assessments were conducted with standardized, internationally validated clinical and functional rating scales. A follow-up visit was completed at 8 weeks after baseline using the same rating instruments.
Ethical Considerations
This study was approved by Queen’s University Health Sciences Research Ethics Board, Kingston, Ontario, Canada, prior to commencement, and all of the patients provided informed consent before being enrolled in the study. Funding for this study was provided by Queen’s University grant 383277. The study design was subject of the Queen’s University Research Ethics Board review in 2008. Queen’s University had no further role in the collection, analysis, and interpretation of the data; in the writing of the report; or in the decision to submit the paper for publication.
Instruments Used
In order to ensure that the recruited patients consistently met the DSM-IV-TR diagnostic criteria, we chose to screen all of the participants with the Mini-International Neuropsychiatric Interview Plus, version 5.0.0 (MINI). The MINI is a structured diagnostic interview developed for DSM-IV and ICD-10 psychiatric disorders.11,12 The version we used was updated with a section validated for the screening of adult ADHD.
The childhood onset of ADHD symptoms was verified through retrospective administration of the ADHD Rating Scale.13 This scale appeared to be the most reliable and adequate for the prediction of the clinical diagnosis of the disorder and has been documented to have the best psychometric properties in diagnosing adult ADHD subjects when the DSM-IV criteria were taken into consideration.14 The ADHD Rating Scale was given to a relative of the patient, most often to a parent, who was asked to consider the patient’s history before age 12 years when responding. We considered the ADHD childhood symptoms to be confirmed if 6 or more symptoms were rated as "often" or "very often" by the relative. We preferred this instrument over the Wender Utah Rating Scale,15 as it more accurately reflects the DSM-IV-TR diagnostic requirements. Although the Wender Utah Rating Scale is the only assessment instrument for ADHD that was explicitly conceived for retrospective assessment of childhood symptoms of ADHD in adults, it includes additional symptoms of affective lability that are not inherent to the DSM-IV-TR concept of ADHD, and, thus, the ratings may be misleading.16
For a positive diagnosis of ADHD, we required both a positive screening on the MINI and confirmation of childhood ADHD symptoms via the ADHD Rating Scale. At baseline, we assessed the clinical severity of the affective episode with clinical observer rating scales: the 21-item Hamilton Depression Rating Scale (HDRS-21)17 and the Young Mania Rating Scale (YMRS).18
Although adult ADHD self-report rating scales appear to be reliable in distinguishing ADHD from normal controls, this assumption may not necessarily be true for patients with additional psychiatric disorders.14 As we assumed that acute bipolar episodes may impact on the reliability of self-administered clinical instruments, we avoided applying any ADHD self-report instruments at baseline.
In addition, the subjects’ functional levels were assessed with the Global Assessment of Functioning (GAF) observer-based rating scale.19 The same rating instruments were also used for the follow-up assessments at 8 weeks.
Data Analysis
All data were analyzed using the SPSS/PASW Statistics 18.0 computer program (SPSS Inc, Chicago, Illinois). Descriptive, univariate statistics (mean, standard deviation, frequency, and percentage) were used to describe the populations and the instrument scores at the different time periods and for the different groups. Comparative statistics aimed to detect differences between the groups (positive vs negative MINI screenings for ADHD and positive versus negative confirmation of childhood symptoms of ADHD) were computed by means of the χ2 test for categorical variables and Student t test for continuous variables. Agreement between the MINI and the ADHD Rating Scale was measured using the κ statistic. The significance limit for all the tests was set at 5%.
RESULTS
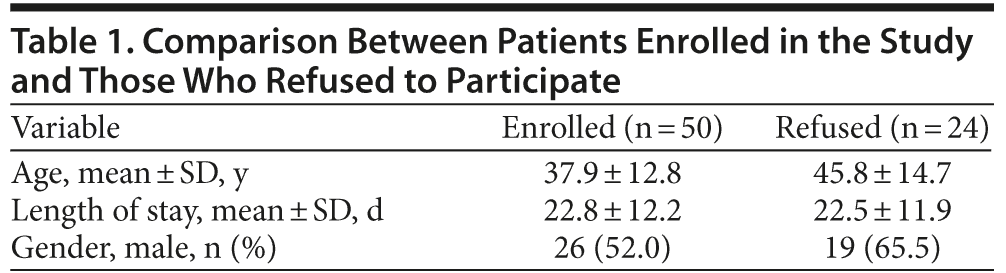
A total of 74 consecutive inpatients diagnosed with bipolar disorder type I or II who did not meet the exclusion criteria were taken into consideration for enrollment. Among the patients invited to participate in the study, 24 refused, resulting in 50 patients in total who consented to participate.
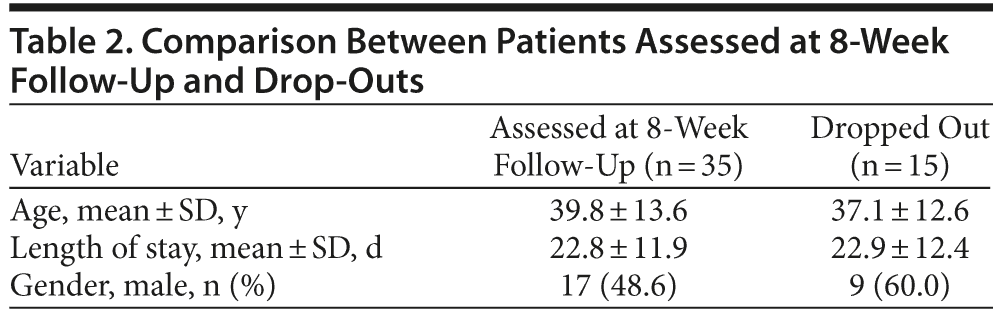
Among these consenting patients, 15 dropped out after the initial visit, and only 35 of the initially recruited patients participated in the follow-up visit. We did not find significant differences in age, gender, and length of stay in the hospital between enrolled patients and those who refused to participate or between study participants who attended the follow-up visit and dropouts (Tables 1 and 2).
At the initial visit, 41 of 50 patients who participated in the study (82%) were found to be positive for ADHD on the MINI. Retrospective observer ratings for childhood symptoms, on the other hand, were obtained for only 39 of 50 participants. These ratings supported the diagnosis of ADHD in 26% (n = 13) of the patients enrolled on the study. All patients with positive screenings on the ADHD Rating Scale also rated positive for ADHD on the MINI. The calculated Spearman’s Ï for the overall agreement between the MINI and the retrospective ratings with the ADHD Rating Scale was 0.319 (P = .048).
The patients with positive screenings for ADHD did not differ significantly in age and in length of stay in the hospital from those for whom ADHD was not confirmed. The patients with ADHD also did not significantly differ at baseline from those without ADHD with regard to clinical global scores (HDRS-21 and YMRS) and functional severity (GAF). Furthermore, no significant differences between the groups were found when individual clinical items were considered.
Among the 50 patients who participated in the initial visit, 35 took part in the follow-up visit at 8 weeks, with 15 of the enrolled patients having dropped out. Only 27 of the 35 patients had retrospective ratings of childhood ADHD symptoms, thereby meeting the requirements for the diagnosis of ADHD. Among these 27 patients, there was a significant difference (P = .025) in the clinical ratings for depression (HDRS-21) at 8-week follow-up between those with ADHD and those without ADHD, with those patients with the disorder presenting lower scores. However, at 8-week follow-up, there was no difference seen in the YMRS and GAF scores between the patients with ADHD and those without ADHD. When single symptom ratings of the applied assessment instruments were considered, no significant differences between patients with or without ADHD were found at 8-week follow-up.
DISCUSSION
Previous studies addressing the complex ADHD/bipolar disorder comorbidity have not quantified the clinical severity of the concomitant conditions. Such a limitation may significantly impact the homogeneity of the samples and limit the reproducibility of the results. The methodology applied in this study offers the advantage of quantitatively assessing the severity of the bipolar relapse at the moment of the dual diagnostic screening.
In this study, the majority (82%) of the patients diagnosed with an acute episode of bipolar disorder did screen positive for ADHD when the MINI was used. These results support the difficulty of recognizing comorbid ADHD in acute patients with bipolar disorder. When the diagnosis is based on information provided by the patient, mood-induced cognitive impairments may affect the accuracy with regard to the lifetime history and the evaluation of functional impairment. The confirmation of childhood-onset ADHD symptoms reduced the rate of patients diagnosed with ADHD comorbidity to 26%, which is closer to the rate previously found in the community in other studies. We attribute the higher rate of comorbidity found in our study to possible higher sensitivity of the retrospective ratings and to biases related to the sample selection (admitted patients). Unexpectedly, the study results do not support our presumption that patients with ADHD have more severe, acute clinical presentations than those without this comorbid burden.
At 8 weeks, the patients with ADHD actually rated lower on the depression scale compared to those without ADHD. This finding is not likely due to the possibility that the ADHD presentation could be masking the depressive symptoms, as the YMRS scores did not differ between the 2 groups of patients. It remains to be confirmed through further research whether ADHD, as a result of its pervasiveness and impact on functionality, would influence the long-term well-being or the risk of relapse among patients with bipolar disorder.
Limitations
From a methodological perspective, the retrospective screening of childhood symptoms may limit the validity of the study results. Childhood diagnosis of ADHD has been set according to retrospective recall in several past studies20 using different methodologies. There are no data to confirm the superiority of any one structured instrument over another or of unstructured approaches. Overall, recall biases may impinge on accurate remembrance of childhood behavior. In our study, we attempted to minimize this effect by asking a close relative to complete the screening for childhood symptoms rather than asking the patient. However, both aging of the relative and contamination with overlapping present behaviors may have influenced their recollections. Nonetheless, previous studies have shown that a reliable and valid retrospective diagnosis of childhood-onset ADHD can be made.1
Another significant limitation of our study is the relatively small number of patients who completed 2 visits and who also had childhood symptom ratings. Although we were able to recruit 50 patients for the study, retrospective assessments were obtained for only 39 of the 50 patients, with only 27 of them completing the follow-up visit. However, this sample is fairly representative, since participants did not significantly differ from the dropouts with regard to age, gender, and clinical severity.
CONCLUSIONS
The present study does not support the notion that comorbid ADHD has a negative impact on the recovery from an acute relapse of bipolar disorder in patients who have been admitted to an acute inpatient unit. These results may not generalize to all ambulatory patients with ADHD/bipolar disorder comorbidity. Long-term follow-up studies of community samples demonstrate poorer outcomes for adult patients with bipolar disorder and ADHD than for those with bipolar disorder without concomitant ADHD.7 Hence, further research is needed to help better comprehend the lasting complex relationship between bipolar disorder and ADHD. Systematic ratings of the severity of the mood symptoms and of the functional impairment in patients with comorbid ADHD and bipolar disorder, in both the clinical and research settings, would be helpful to better understand factors influencing outcomes.
Although the validation of the MINI was not an objective of this study, we found that the use of the MINI in adult patients with an acute episode of bipolar disorder may lead to the overdiagnosis of comorbid ADHD. Our results confirm that the MINI is a highly sensitive instrument for the detection of ADHD in patients with bipolar disorder, but we also advise that a systematic retrospective assessment of childhood ADHD symptoms be conducted in order to increase the accuracy of the diagnosis.
Author affiliations: Department of Psychiatry, Queen’s University, Kingston, Ontario, Canada (Drs Marin, Scott, and Groll).
Potential conflicts of interest: None reported.
Funding/support: Funding for this study was provided by Queen’s University grant 383277, Kingston, Ontario, Canada. The study design was subject of the Queen’s University Research Ethics Board Review in 2008, and the study itself was approved by the Queen’s University Health Sciences Research Ethics Board prior to commencement.
Acknowledgments: The authors thank Clarene Ho, BScPharm, Victoria, British Columbia, for her important contribution to the literature searches; Diane Hannah, RN, Kingston General Hospital, Kingston, Ontario, Canada, who kindly provided support with data collection in the study; and Nicole Rodrigues, BA(H)Psychology, Brockville Mental Health, Brockville, Ontario, Canada, for data entry. Mss Ho, Hannah, and Rodrigues report no conflicts of interest related to the subject of this article.
REFERENCES
1. Spencer T, Biederman J, Wilens T, et al. Is attention-deficit hyperactivity disorder in adults a valid disorder? Harv Rev Psychiatry. 1994;1(6):326-335. PubMed doi:10.3109/10673229409017099
2. Hornig M. Addressing comorbidity in adults with attention-deficit/hyperactivity disorder. J Clin Psychiatry. 1998;59(suppl 7):69-75. PubMed
3. Biederman J, Faraone SV, Spencer T, et al. Patterns of psychiatric comorbidity, cognition, and psychosocial functioning in adults with attention deficit hyperactivity disorder. Am J Psychiatry. 1993;150(12):1792-1798. PubMed
4. Milberger S, Biederman J, Faraone SV, et al. Attention deficit hyperactivity disorder and comorbid disorders: issues of overlapping symptoms. Am J Psychiatry. 1995;152(12):1793-1799. PubMed
5. Duffy A. The nature of the association between childhood ADHD and the development of bipolar disorder: a review of prospective high-risk studies. Am J Psychiatry. 2012;169(12):1247-1255. PubMed doi:10.1176/appi.ajp.2012.11111725
6. Klassen LJ, Katzman MA, Chokka P. Adult ADHD and its comorbidities, with a focus on bipolar disorder. J Affect Disord. 2010;124(1-2):1-8. PubMed doi:10.1016/j.jad.2009.06.036
7. Nierenberg AA, Miyahara S, Spencer T, et al; STEP-BD Investigators. Clinical and diagnostic implications of lifetime attention-deficit/hyperactivity disorder comorbidity in adults with bipolar disorder: data from the first 1000 STEP-BD participants. Biol Psychiatry. 2005;57(11):1467-1473. PubMed doi:10.1016/j.biopsych.2005.01.036
8. Kessler RC, Adler L, Barkley R, et al. The prevalence and correlates of adult ADHD in the United States: results from the National Comorbidity Survey Replication. Am J Psychiatry. 2006;163(4):716-723. PubMed doi:10.1176/appi.ajp.163.4.716
9. Wingo AP, Ghaemi SN. A systematic review of rates and diagnostic validity of comorbid adult attention-deficit/hyperactivity disorder and bipolar disorder. J Clin Psychiatry. 2007;68(11):1776-1784. PubMed doi:10.4088/JCP.v68n1118
10. Murphy KR, Barkley RA. Attention deficit hyperactivity disorder adults: comorbidities and adaptive impairments. Compr Psychiatry. 1996;37(6):393-401. PubMed doi:10.1016/S0010-440X(96)90022-X
11. Sheehan DV, Lecrubier Y, Harnett Sheehan K, et al. The validity of the Mini International Neuropsychiatric Interview (MINI) according to the SCID-P and its reliability. Eur Psychiatry. 1997;12:232-241. doi:10.1016/S0924-9338(97)83297-X
12. Sheehan DV, Lecrubier Y, Sheehan KH, et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry. 1998;59(suppl 20):22-33, quiz 34-57. PubMed
13. DuPaul GJ, Power TJ, Anastopoulos AD, et al. ADHD Rating Scale IV: Checklists, Norms, and Clinical Interpretation. New York, NY: The Guilford Press; 1998.
14. Sandra Kooij JJ, Marije Boonstra A, Swinkels SH, et al. Reliability, validity, and utility of instruments for self-report and informant report concerning symptoms of ADHD in adult patients. J Atten Disord. 2008;11(4):445-458. PubMed doi:10.1177/1087054707299367
15. Ward MF, Wender PH, Reimherr FW. The Wender Utah Rating Scale: an aid in the retrospective diagnosis of childhood attention deficit hyperactivity disorder. Am J Psychiatry. 1993;150(6):885-890. PubMed
16. McCann BS, Scheele L, Ward N, et al. Discriminant validity of the Wender Utah Rating Scale for attention-deficit/hyperactivity disorder in adults. J Neuropsychiatry Clin Neurosci. 2000;12(2):240-245. PubMed doi:10.1176/appi.neuropsych.12.2.240
17. Hamilton MA. A rating scale for depression. J Neurol Neurosurg Psychiatry. 1960;23(1):56-62. doi:10.1136/jnnp.23.1.56 PubMed >
18. Young RC, Biggs JT, Ziegler VE, et al. A rating scale for mania: reliability, validity and sensitivity. Br J Psychiatry. 1978;133:429-435. doi:10.1192/bjp.133.5.429 PubMed >
19. Hurtig T, Ebeling H, Taanila A, et al. ADHD symptoms and subtypes: relationship between childhood and adolescent symptoms. J Am Acad Child Adolesc Psychiatry. 2007;46(12):1605-1613. PubMed doi:10.1097/chi.0b013e318157517a
20. Guy W. ECDEU Assessment Manual for Psychopharmacology. US Department of Health, Education, and Welfare publication (ADM) 76-338. Rockville, MD: National Institute of Mental Health; 1976:218-222.