Olanzapine-Induced Weight Gain in Patients With Bipolar I Disorder: A Meta-Analysis

ABSTRACT
Objective: The weight impact produced by the atypical antipsychotic olanzapine has been explored in meta-analyses focusing on patients with schizophrenia. However, outcomes identified for schizophrenia patients cannot always be generalized to patients with bipolar disorder. This study aims to quantitatively estimate the impact of olanzapine on the weight of patients with bipolar disorder.
Data Sources: EMBASE, Medline, and PsycINFO were searched using the keywords olanzapine AND (bipolar OR acute mania) in conjunction with (weight gain OR weight increase) (last search: October 2010, with no restrictions on dates of publication). English language was used as a restriction.
Study Selection: The search identified 110 articles for review. The inclusion criteria for the chosen studies were a diagnosis of bipolar disorder, the presence of an olanzapine monotherapy group, a comparator placebo or monotherapy group, and mean weight gain and/or incidences of weight gain data. This process identified 13 studies for inclusion.
Data Extraction: The primary outcome measure was the mean weight change between olanzapine monotherapy and comparator monotherapy, reported in kilograms. Standard deviation was extracted directly from studies when possible and imputed for 3 studies. The secondary outcome measure was the reported incidences of ≥ 7% weight gain.
Data Synthesis: The mean difference in weight gain was calculated for the continuous data of the primary outcome. Olanzapine monotherapy was associated with more weight gain when compared to placebo (mean difference = 2.10 kg; 95% CI, 1.16-3.05; P < .001) and other bipolar monotherapy (mean difference = 1.34 kg; 95% CI, 0.95-1.72; P < .001). Odds ratio analysis of the dichotomous secondary outcome also showed more weight gain with olanzapine monotherapy compared to placebo (odds ratio [OR] = 10.12; 95% CI, 1.93-53.14; P = .006) and other bipolar monotherapy (OR = 2.09; 95% CI, 1.27-3.44; P = .004).
Conclusions: Currently available data suggest that olanzapine is associated with significant weight gain in bipolar patients. Issues related to side effect profiles and their impact on treatment compliance and physical health outcomes need to be considered when selecting pharmacotherapy.
Prim Care Companion CNS Disord 2011;13(6):doi:10.4088/PCC.11r01174
© Copyright 2011 Physicians Postgraduate Press, Inc.
Submitted: February 25, 2011; accepted June 13, 2011.
Published online: November 10, 2011.
Corresponding author: Valerie H. Taylor, MD, PhD, FRCPC, Department of Psychiatry, University of Toronto, Women’s College Hospital, 76 Grenville St, Toronto, Ontario, M5S 1B2 Canada ([email protected]).
Bipolar disorder, a chronic mental illness that impacts 1% of the population, is defined clinically by a wide range of symptoms: a depressed or euphoric mood, lack of activity paralleled at times with energized behavior, and a decreased need for sleep and social interaction that can manifest as either the desire for complete isolation or extreme extroversion that can become problematic.1 To further complicate the picture, individuals in either the manic or depressed phases of bipolar disorder can experience psychotic symptoms as well.1 As a consequence, the pharmacologic management of bipolar disorder involves a myriad of options from a variety of drug categories; mood stabilizers, antidepressants, and atypical antipsychotics are all recommended as first-line agents, either as monotherapy or in combination.1 Of these options, the most recent class of medications to become first line for acute and maintenance treatment of bipolar disorder is the second-generation atypical antipsychotics (SGAs). While these agents are heterogeneous in their efficacy and tolerability, studies suggest that SGAs, either alone or in combination with mood stabilizers, are currently an efficacious treatment strategy in the management of both the depressive and manic stages of bipolar disorder.2 Added benefits in favor of the use of SGAs include reduced extrapyramidal side effects and the absence of depressive symptom exacerbation.3 There are concerns associated with the use of this medication class, however, and the adverse metabolic profile associated with SGAs needs to be considered when making treatment recommendations.
In terms of market share, the most commonly prescribed atypical antipsychotic worldwide is olanzapine.4 In 2003, olanzapine was approved for the treatment of bipolar depressive episodes in combination with fluoxetine,5 and in 2004 it was approved for long-term maintenance treatment of bipolar disorder.6 Since then, olanzapine has become the best-studied SGA in this patient population, but while significant weight gain has been consistently reported with the use of olanzapine in the treatment of bipolar disorder, there has not been a meta-analysis to comprehensively investigate the problem in this population. The bulk of work examining the weight gain side effects associated with olanzapine has focused on schizophrenia, and a 2009 meta-analysis by Leucht et al7 concluded that olanzapine was associated with 3.3-kg more weight gain when compared with haloperidol monotherapy (95% CI, 2.2-4.4, P < .001) in 9 studies on patients with schizophrenia. In 2 other meta-analyses, olanzapine was shown to cause more weight gain than any other SGA, with the exception of clozapine, in patients in schizophrenia.8,9
Results from schizophrenia studies are not always generalizable to other patient populations; therefore, a meta-analysis on the weight gain effects of olanzapine on patients with bipolar disorder is warranted. The aim of this study was to compare weight gain outcomes of olanzapine monotherapy to placebo and other monotherapies in patients with bipolar disorder.
METHOD
Database Search
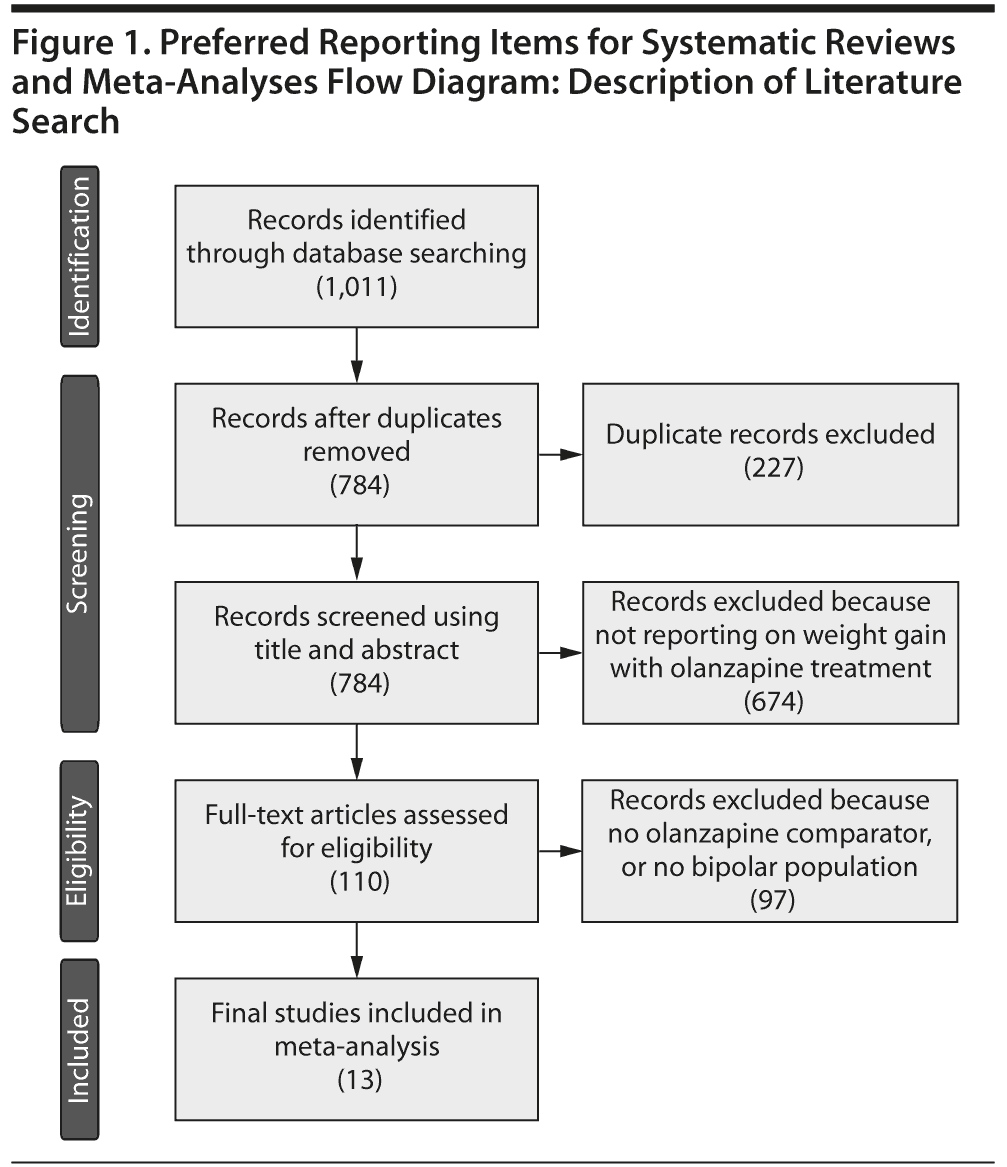
The OVID search engine was used to perform a combined search of 3 databases: EMBASE, MEDLINE, and PsycINFO. The last search was conducted in October of 2010, and there were no restrictions on date of publication. English language was used as a restriction. Abstracts, titles, and indexed terms of studies were searched using the keywords olanzapine AND (bipolar OR acute mania) in conjunction with (weight gain OR weight increase). After duplicates and articles with no abstracts were filtered out, 784 results remained (Figure 1). Studies that did not investigate weight gain with olanzapine monotherapy were excluded. This process identified 110 articles for full-text investigation. Of these, studies that did not include at least 1 comparator to olanzapine monotherapy were excluded, along with studies that did not investigate bipolar patients. Studies on adolescent bipolar patients were not included in the analysis due to limitations in comparing weight gain between adults and adolescents. Open-label and naturalistic studies were included since physical measures, such as weight gain, are not susceptible to placebo effect.
Further screening of the 110 retrieved articles and their references identified 12 double-blind, randomized, controlled studies and 1 naturalistic observational study to be included in this analysis. Four of the total 13 studies were placebo controlled, and the remaining tested olanzapine monotherapy against an alternative monotherapy. The coauthors of the present analysis (M.G.N. and M.R.R.) performed the search and extracted data from the studies independently, and disagreements were discussed until a consensus was reached. The inclusion criteria for the final studies were a diagnosis of bipolar disorder, the presence of an olanzapine monotherapy group, a comparator placebo or monotherapy group, and mean weight gain and/or incidences of weight gain data.
It is worth noting that 2 studies that initially passed all phases of screening were later excluded. The first is a maintenance study by Tohen et al10 in which subjects were randomized to receive either olanzapine or lithium after 6 to 12 weeks of open-label cotherapy. Consequently, the subjects were not olanzapine naive at randomization, having gained a mean of 2.7 kg during cotherapy. The second study was also a maintenance study by Tohen et al,11 and, similarly, this study randomized subjects to receive either olanzapine or placebo after 6 to 12 weeks of open-label olanzapine treatment. Thus, the placebo group had gained weight due to olanzapine treatment prior to randomization. Both studies show significantly more weight gain with olanzapine monotherapy at endpoint but were excluded from the present analysis due to their experimental design.

- Olanzapine monotherapy is associated with significantly more weight gain than placebo and other bipolar disorder medications that are known to cause moderate weight gain.
- Weight gain may exacerbate other health risks associated with bipolar disorder, such as compromised neurocognitive function.
- Clinician awareness regarding the adverse metabolic side effects of antipsychotics, such as olanzapine, will ensure that patients are able to safely choose the best medication to manage their complicated illness and improve medication compliance.
The clinical trials registry clinicaltrials.gov was searched for unpublished results using the keywords olanzapine AND bipolar AND weight. This search yielded 30 trials, of which 2 were completed with results. Of these, 1 compared placebo to olanzapine combination therapy with divalproex and was therefore excluded on the basis of not having an olanzapine monotherapy group. The other study included schizophrenia and schizoaffective subjects, along with bipolar subjects, and reported the weight gain results for all subjects combined. The investigators of this trial were contacted via e-mail, requesting the separate weight gain results of the bipolar subject, but no response was obtained.
Outcome Parameters and Data Extraction
The primary outcome of interest for this analysis was the mean weight gain in the olanzapine monotherapy and comparator monotherapy groups. For the primary outcome, we needed to extract mean weight gain, standard deviation (SD), and sample size from each study. When reported, the last observation carried forward (LOCF) was used as the sample size in the analysis. For studies that did not report a LOCF, the randomized sample size was used. For 10 of the 13 articles, the SDs were extracted directly from the article, and for the remaining 3 studies that did not disclose SDs, the SDs were imputed using the pooled SDs from all the other articles matched appropriately for intervention group. This method was used because borrowing SDs from other studies to impute data has been empirically shown to be an appropriate remedy for missing SDs in meta-analyses.12
The secondary outcome of interest was the incidence of weight gain, that is, the number of patients in each group who gained weight during the intervention. Clinically significant weight gain was defined as 7% or more of initial body weight. While it would have been preferable to use body mass index or waist circumference as a surrogate marker of weight gain, only 4 of the 13 studies included in this meta-analysis had information on body mass index and of these 4 studies, 3 reported baseline body mass index but not change over time. No data on change in waist circumference were available.
Analytic Methods
The meta-analysis was conducted using the software Review Manager Version 5.0 (Clicktime.com, Inc, San Francisco, California), with statistical significance set at P < .05. As the primary outcome examined continuous data, the mean difference in weight gain (change in kilograms) was calculated with a 95% confidence interval (CI). For the dichotomous data of the secondary measure incidence of weight gain, an odds ratio (OR) analysis was performed. This method allows for the inclusion of more types of studies and is less prone to outliers than relative risk analysis.13,14
A random-effects model was used in both primary and secondary outcome analyses, with heterogeneity among studies investigated using both χ2 (P < . 01) and I2 tests.
RESULTS
Study Characteristics
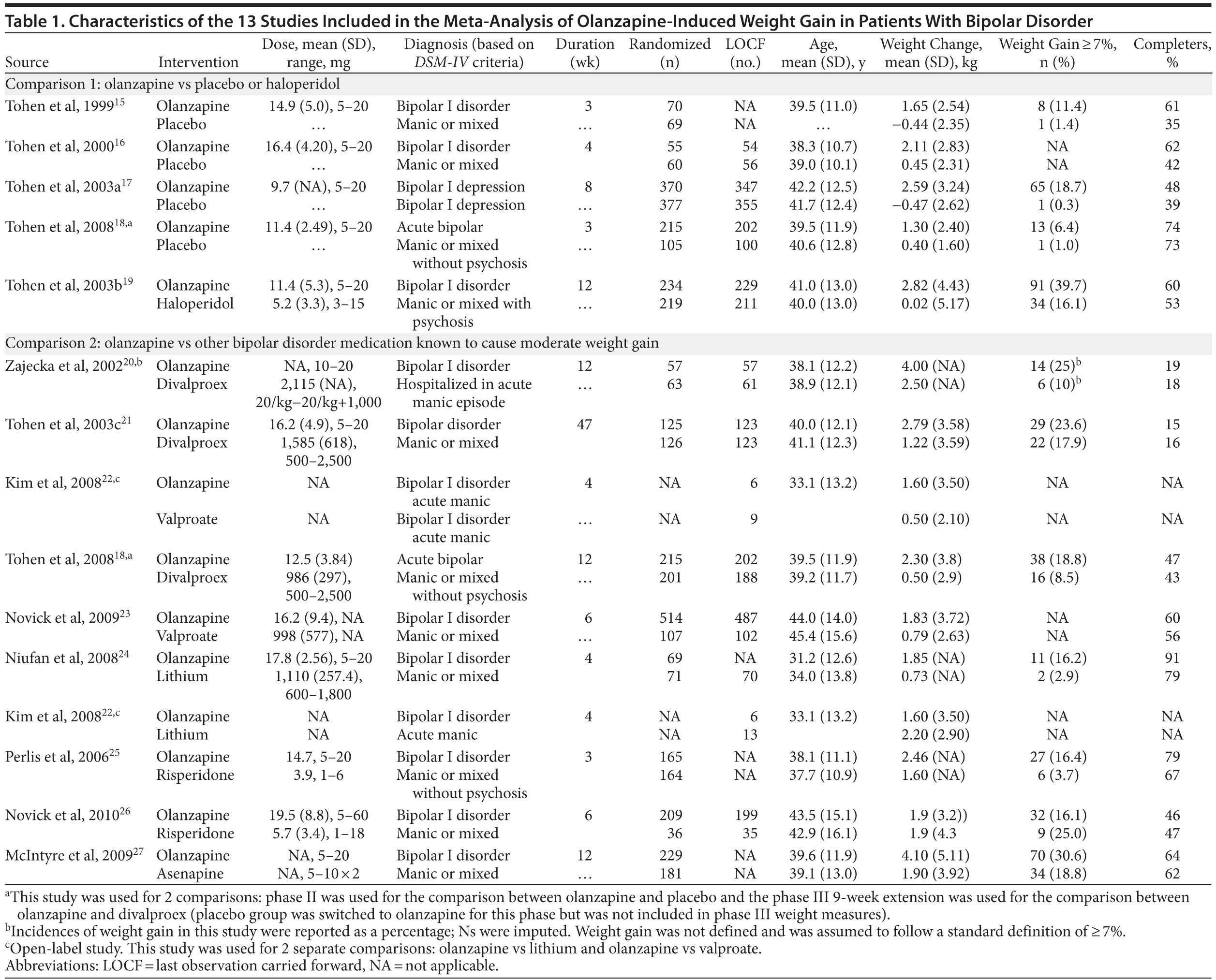
Table 1 summarizes the characteristics of the 13 studies included in the meta-analysis.15-27 The duration for most of the studies was between 3 and 12 weeks, with 3 studies each investigating 3-week and 4-week intervals,15,16,18,22,24,25 2 studies investigating a 6-week period,23,26 1 study investigating an 8-week follow-up,17 and 4 studies investigating weight gain over 12 weeks.18-20,27 The remaining study looked at side effects over a longer maintenance phase of 47 weeks.21

With respect to study type, 4 of the 13 studies in the present analysis were placebo controlled,15-18 while the remaining studies compared olanzapine monotherapy to various comparators, namely haloperidol,19 divalproex/valproate,18,20-23 lithium,22,24 risperidone,25,26 and asenapine.27 Tohen et al18 conducted a 3-branch examination on olanzapine monotherapy versus placebo versus divalproex monotherapy, while Kim et al22 conducted a 3-branch monotherapy examination of olanzapine versus lithium versus valproate, so data from both studies were included in 2 comparisons. The study comparing olanzapine monotherapy with haloperidol monotherapy19 was grouped with the placebo-controlled studies, as haloperidol has not been associated with significant weight gain and for the purpose of the present analysis behaves as a placebo.28,29 Thus, “olanzapine monotherapy versus placebo or haloperidol” constituted the first comparison. Studies with other comparators were grouped together under the second comparison, “olanzapine versus other bipolar disorder medication known to cause moderate weight gain.” As this comparison suggests, studies with nonplacebo, nonhaloperidol comparators were grouped together due to their documented comparable effects on weight gain. On the basis of the literature, divalproex, lithium, risperidone, and asenapine have all been associated with weight gain that is significantly greater than placebo, but less than olanzapine.28,30,31
Primary Outcome: Mean Weight Gain
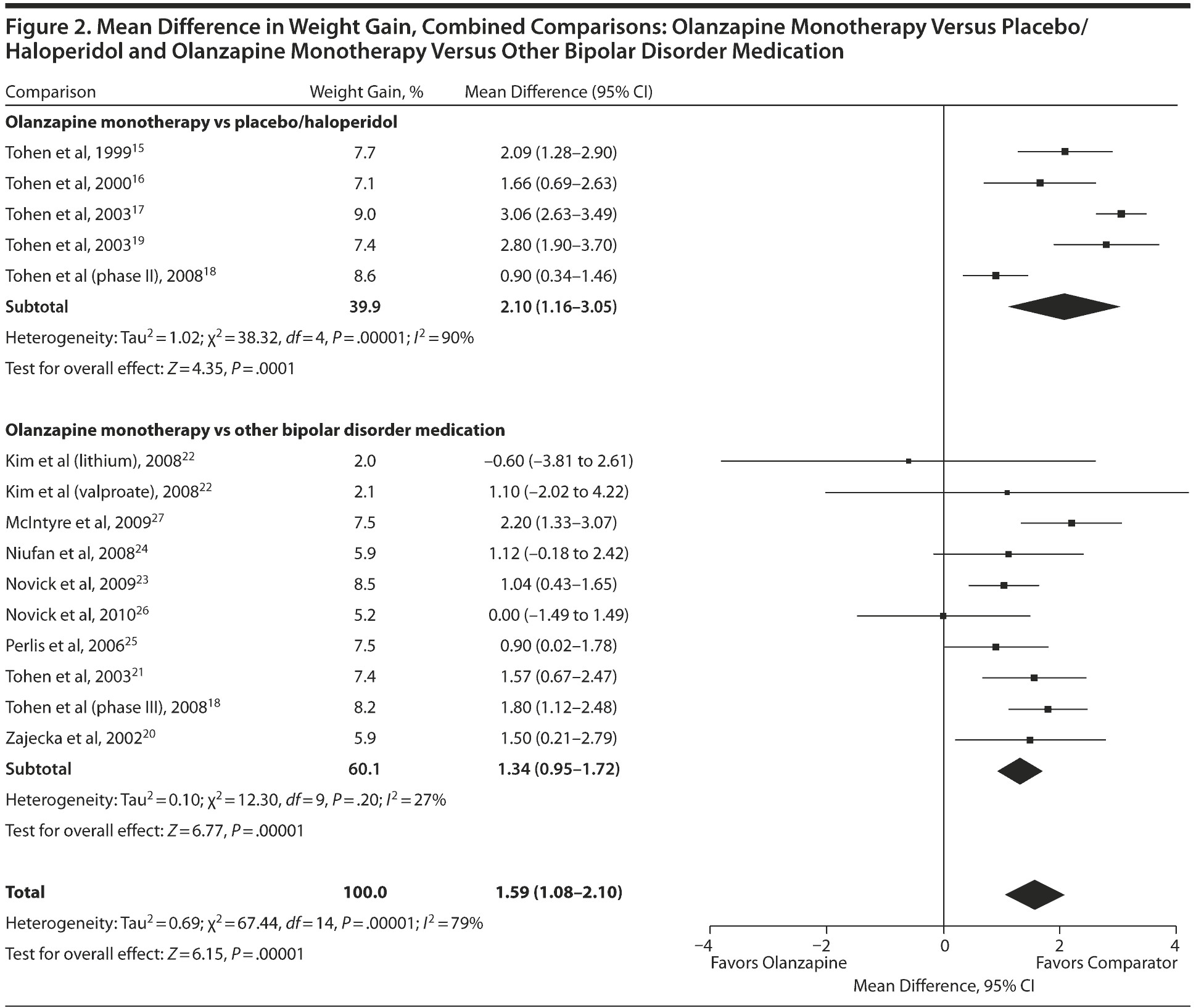
Olanzapine versus placebo/haloperidol. The 5 studies in the first analysis compared olanzapine monotherapy versus placebo or haloperidol. In this comparison, olanzapine was associated with significantly more weight gain than placebo or haloperidol (Figure 2). The pooled mean difference of this comparison was 2.10 kg (95% CI, 1.16-3.05; P < .001). The results showed significant heterogeneity among the 5 studies (I2 = 90%, χ2 = 38.32, P < .001). Sequential removal of single studies from the analysis was performed to test for a possible outlier, but no single removal was found to render heterogeneity nonsignificant.
Olanzapine versus other bipolar disorder medication. The 10 studies in the second comparison investigated olanzapine monotherapy versus other bipolar disorder medications that are known to cause moderate weight gain. The outcome of this comparison showed greater weight gain associated with olanzapine versus other bipolar disorder medication. As expected, the effect size was smaller than that observed in the first comparison. The pooled mean difference of this comparison was 1.34 kg (95% CI, 0.95-1.72; P < .001). The heterogeneity of the 10 studies was not significant (I2 = 27%, χ2 = 12.30, P = .20).
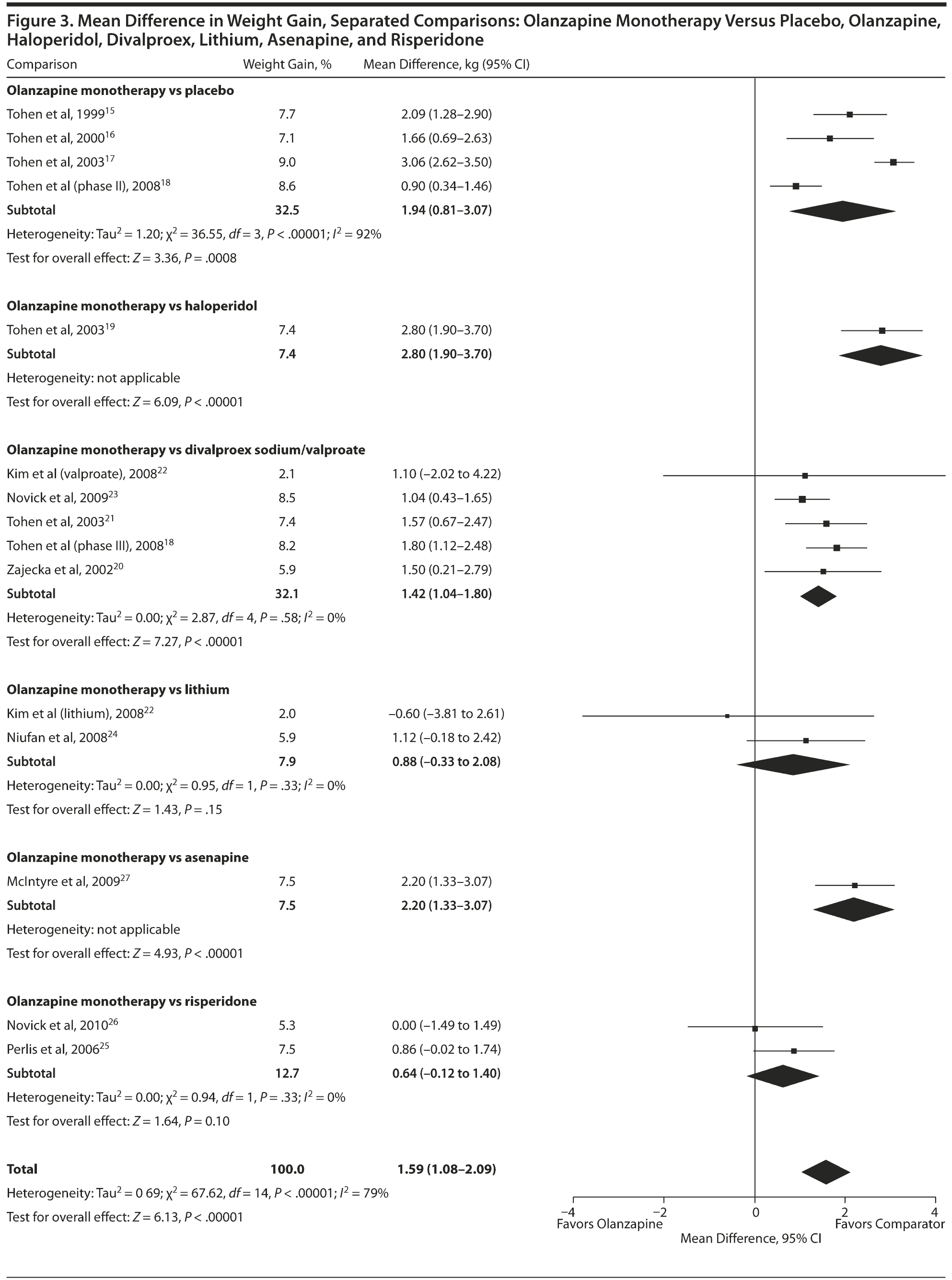
Separated analyses. To test the belief that the divalproex, lithium, risperidone, and asenapine trials can justifiably be combined into 1 comparison and that the haloperidol trial can be combined with the placebo-controlled comparison, a second analysis was performed with all comparators separated (Figure 3). Results from this analysis showed little change in the placebo group’s pooled effect size and heterogeneity when the haloperidol trial19 was separated, and, so, this combination may be justifiable.
Effect sizes from the lithium and risperidone groups were similar (mean differences of 0.88 to 0.64 kg, respectively), suggesting justifiable combination. However, the divalproex and asenapine groups showed varied effect sizes (mean differences of 1.42 and 2.20 kg, respectively). Only the divalproex mean difference of 1.42 kg was similar to the combined mean difference of 1.34 kg. Furthermore, all groups in the separated analysis showed less heterogeneity, when applicable, than the combined analysis. On the basis of these results, it is unclear whether the combined analyses are justifiable; therefore, both the combined and separated analyses are presented.
Secondary Outcome: Incidence of Weight Gain
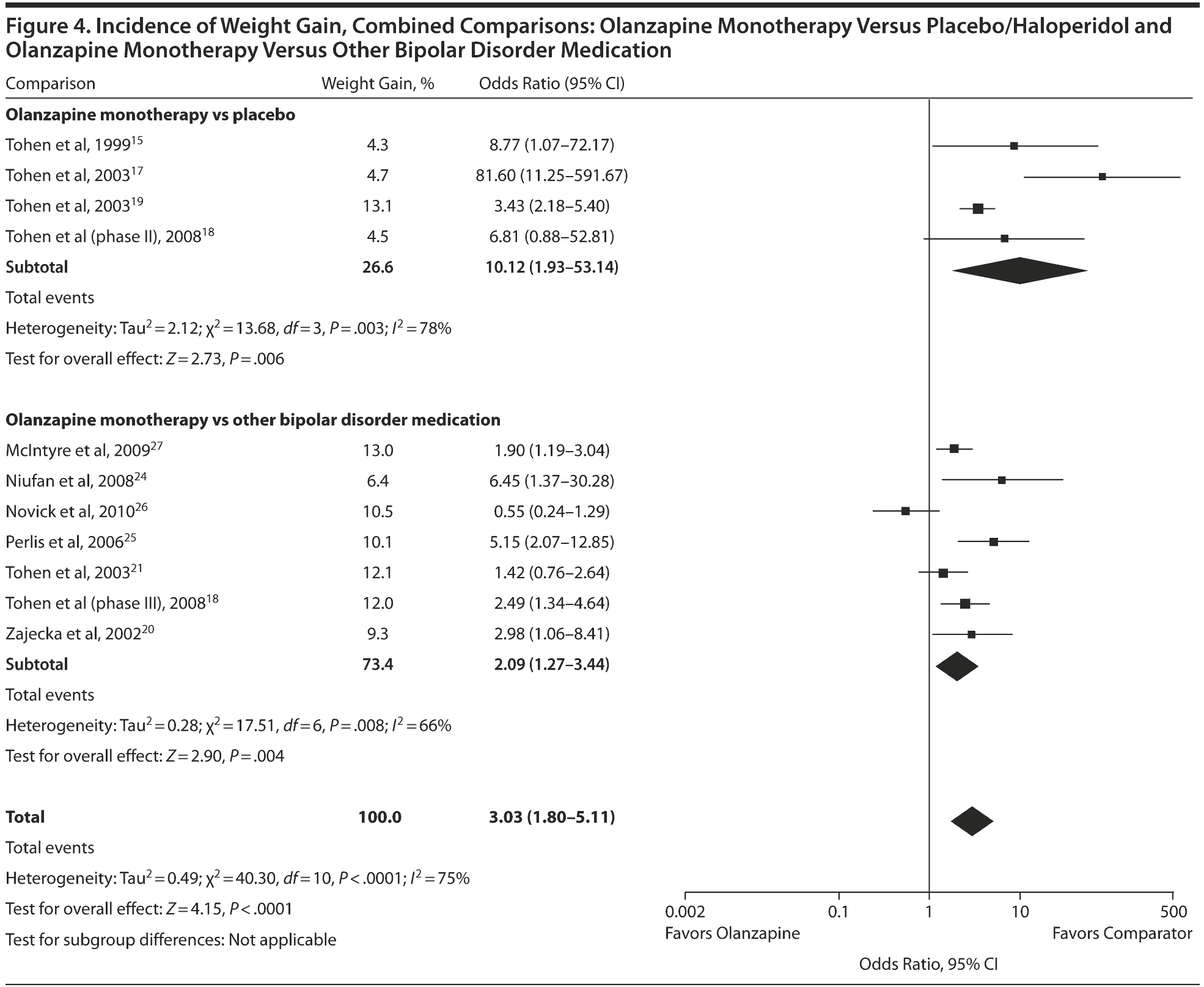
Olanzapine versus placebo/haloperidol. When incidences of reported weight gain were investigated, olanzapine was again associated with significantly more weight gain than was placebo or haloperidol (Figure 4). The pooled OR of this comparison was 10.12 (95% CI, 1.93-53.14; P = .006). The results for these trials were heterogeneous (I2 = 78%, χ2 = 13.68, P = .003). The heterogeneity was rendered nonsignificant with the removal of 2 studies by Tohen et al: Tohen et al17 (I2 = 0%, χ2 = 1.12, P = .57) and Tohen et al19 (I2 = 51%, χ2 = 4.10, P = .13), and it is possible that at least 1 of these studies is an outlier. It is worth noting that exclusion of the Tohen et al study19 increased the pooled OR to 17.35 (95% CI, 3.20-94.01), and exclusion of the Tohen et al study17 decreased the OR to 3.68 (95% CI, 2.39-5.67). However, exclusion of these studies did not affect the conclusion of the results, as they remained significant in all cases.
Second comparison: olanzapine versus other bipolar disorder medication. Analysis on incidences of weight gain for the second comparison showed more people gaining weight with olanzapine versus other bipolar disorder medication, with an effect size smaller than that observed in the first comparison. The pooled OR of this comparison was 2.09 (95% CI, 1.27-3.44; P = .004). The results for these trials were heterogeneous (I2 = 66%, χ2 = 17.51, P = .008), but heterogeneity was rendered nonsignificant with the removal of the study by Novick et al26 (I2 = 38%, χ2 = 8.00, P = .16), indicating that it may be an outlier. Removal of this study had little effect on the pooled OR, however, and did not affect the conclusion of the analysis.
Separated analyses. As with the primary outcome, a second analysis was performed with all comparators separated (Figure 5). For this outcome, separation of the haloperidol study from the placebo-controlled group caused an increase in the pooled OR of the placebo group (from 10.12 to 17.42). In addition, heterogeneity of the results decreased, indicating the combined analysis may not be justifiable.
Effect sizes from the divalproex, lithium, asenapine, and risperidone groups were relatively similar (ORs ranging from 1.68 to 6.45). Individually, the divalproex group showed less heterogeneity (I2 = 11%) when separated, whereas the risperidone group showed more heterogeneity (I2 = 92%), possibly owing to the previously discussed outlier effect of the study by Novick et al.26 As with the primary outcome, it is unclear whether a combined analysis is justifiable; therefore, both the combined and separated analyses are presented.
Possible covariates. Linear regression analysis failed to show a significant relationship between study duration and mean weight gain when all of the studies were included (R = 0.39; F1,12 = 2.10; P = .17). However, when the maintenance study by Tohen et al21 was removed from the analysis, a significant relationship was observed between study duration and mean weight gain (R = 0.78; F1,11 = 17.42; P = .0015). The same pattern with nearly identical statistics was observed when incidences of weight gain were used in place of mean weight gain, suggesting a possible plateau effect on weight gain between 12 and 47 weeks. A second linear regression was performed to assess the effect of mean olanzapine dosage on mean weight gain. This analysis found no significant effect (R = −0.25; F1,10 = 0.62; P = .45). Additionally, no significant effect of mean olanzapine dosage on incidences of weight gain was found (R = −0.18; F1,7 = 0.24; P = .64).
DISCUSSION
To our knowledge, this is the first meta-analysis investigating the extent of weight gain associated with olanzapine monotherapy in the treatment of patients with bipolar disorder. The results clearly show that olanzapine monotherapy is associated with significantly more weight gain than placebo and other bipolar disorder medications that are known to cause moderate weight gain. These medications include other SGAs (risperidone and asenapine), a first-generation antipsychotic (haloperidol), a mood stabilizer (lithium), and an anticonvulsant (divalproex/valproate). These results held when investigating mean weight gained during monotherapy, as well as incidences of reported weight gain.
Our results are consistent with meta-analyses investigating the weight gain effects of olanzapine on schizophrenia subjects that have also focused on comparisons between different SGAs. In an analysis of 16 studies by Rummel-Kluge et al,9 for example, the mean difference in weight gain between olanzapine and risperidone was 2.44 kg (95% CI, 1.61-3.27) in favor of risperidone, while in a 13-study analysis by Komossa et al,8 the mean difference between olanzapine and risperidone was 2.61 kg (95% CI, 1.48-3.74) in favor of risperidone. The results from the present analysis, in comparison, show a mean difference of 0.64 kg (95% CI, -0.12 to 1.40) in favor of risperidone, although the results are based on only 2 studies. A 9-study meta-analysis by Leucht et al7 investigated the weight gain effects of olanzapine versus haloperidol on schizophrenia subjects and suggests a mean difference of 3.3 kg (95% CI, 2.2-4.4) in favor of haloperidol, similar to the present analysis that suggests a mean difference of 2.80 kg (95% CI, 1.90-3.70) in favor of haloperidol the basis of 1 study only. Due to the low power of the olanzapine versus risperidone and olanzapine versus haloperidol comparisons in this analysis, it is still difficult to draw strong conclusions. Our findings are supported by a study by Treuer et al32 in which olanzapine monotherapy was examined in both schizophrenia and bipolar subgroups. In this study, both groups gained weight, with the schizophrenia patients gaining a larger proportion of weight earlier than the bipolar subgroup (25% vs 11%, respectively).
A limitation of this analysis is the small number of studies available. Without active exclusion of possible outliers, the combined analyses for both outcomes showed significant heterogeneity, with the exception of the combined mean differences for bipolar disorder medications known to cause moderate weight gain (primary outcome, second comparison). Performing separate analyses (with all comparators separated) helped remedy this problem in most cases but also decreased the number of trials and total number of subjects in each comparison, resulting in a decrease in the power of the individual analyses.
Another point of caution stems from the conclusions of the individual studies. While all placebo/haloperidol trials reported more weight gain in their olanzapine monotherapy group, this was not the case for the other comparators. The naturalistic study by Kim et al22 reported greater mean weight gain with lithium monotherapy when compared to olanzapine monotherapy, while a study by Novick et al26 found no difference in the mean weight gain between the olanzapine group and the risperidone group, but reported more incidences of weight gain in the risperidone group. This trial, however, was targeted as a possible outlier in our analysis. Another limitation of our results is a confounder that impacts many reviews on medication use: only 2 trials in our analysis22,27 did not receive funding from Eli Lilly, the maker of olanzapine. Weight gain was not the primary endpoint of the trials included, however, and weight gain was reported in all studies.
The results of this analysis highlight the significant weight gain associated with olanzapine in the treatment of bipolar disorder and illustrate the need to focus on this side effect. Olanzapine was the most effective SGA in the Clinical Antipsychotic Trials of Intervention Effectiveness schizophrenia trial33 and has proven effectiveness in bipolar disorder as well.1 Issues related to weight gain have a significant impact on treatment compliance, and a consensus statement by clinical and research experts lists SGA-associated weight gain as 1 of the main risk factors for medication adherence in both patients with bipolar disorder and patients with schizophrenia,34 putting patients at risk for relapse.35
Weight gain may also exacerbate other health risks associated with bipolar disorder, as both obesity and mood disorders are chronic low-grade proinflammatory states, and the 2 conditions existing together may be associated with problems such as compromised neurocognitive function.36 Rates of obesity-related medical illness, such as cardiovascular disease, type 2 diabetes, and metabolic syndrome are also increased in patients with bipolar disorder and may increase the risk of premature mortality in this population.36,37 Therefore, continued research on the metabolically adverse effects of SGAs is warranted in order to counter these effects, increase treatment compliance, and confer better patient care to individuals with bipolar disorder.
Side effect profiles of medications need to be considered when making treatment decisions, as does the use of interventions to counteract these side effects. Current literature suggests that most of the weight gain associated with olanzapine occurs within the first 12 weeks of treatment,38 with a plateau usually reached between 36 and 39 weeks.38,39 These results may have little to do with the pharmacologic properties of the medication, however, and instead may be related to interventions and lifestyle changes that are put in place once weight changes are observed. A number of trials examining the effects of medication,40,41 cognitive-behavioral therapy,42 and lifestyle43 changes have been able to successfully impact weight gain and cause weight loss in patients taking olanzapine. As clinicians, we need to be more aware of medication side effects and better able to educate patients on how to minimize these outcomes. This awareness will ensure that patients are able to safely choose the best medication to manage their complicated illness.
Drug names: asenapine (Saphris), clozapine (Clozaril, FazaClo, and others), divalproex sodium (Depakote and others), fluoxetine (Prozac and others), haloperidol (Haldol and others), lithium (Lithobid and others), olanzapine (Zyprexa), risperidone (Risperdal and others).
Author affiliations: MiNDS Neuroscience Graduate Program, McMaster University, Hamilton (Mr Nashed and Ms Restivo); and Women’s College Hospital, Department of Psychiatry, University of Toronto (Dr Taylor), Ontario, Canada.
Potential conflicts of interest: None reported.
Funding/support: None reported.
Acknowledgments: The authors would like to thank David Streiner, PhD (Department of Psychiatry and Behavioural Neurosciences, McMaster University, Hamilton, and Department of Psychiatry, University of Toronto, Ontario, Canada), for his help and direction regarding the meta-analytical techniques. Dr Streiner reports no conflicts of interest related to the subject of this article.
REFERENCES
1. Yatham LN, Kennedy SH, Schaffer A, et al. Canadian Network for Mood and Anxiety Treatments (CANMAT) and International Society for Bipolar Disorders (ISBD) collaborative update of CANMAT guidelines for the management of patients with bipolar disorder: update 2009. Bipolar Disord. 2009;11(3):225-255. PubMed doi:10.1111/j.1399-5618.2009.00672.x
2. Scherk H, Pajonk FG, Leucht S. Second-generation antipsychotic agents in the treatment of acute mania: a systematic review and meta-analysis of randomized controlled trials. Arch Gen Psychiatry. 2007;64(4):442-455. PubMed doi:10.1001/archpsyc.64.4.442
3. Liauw SS, McIntyre RS. Atypical antipsychotic tolerability and switching strategies in bipolar disorder. Expert Opin Pharmacother. 2010;11(17):2827-2837. PubMed doi:10.1517/14656566.2010.510835
4. Cascade EF, Kalali AH, Lieberman J, et al. Use of antipsychotics pre- and post-dissemination of CATIE data. Psychiatry (Edgmont). 2007;4(5):21-23. PubMed
5. Symbyax Approval Letter. (NDA 21-520), Department of Health and Human Services. Food and Drug Administration, 12-24-2003. www.accessdata.fda.gov/drugsatfda_docs/appletter/2003/21520ltr.pdf. Accessed October 3, 2011.
6. Zyprexa Approval Letter. (NDA 20-592/S-019), Department of Health and Human Services. Food and Drug Administration, 01-14-2004. www.accessdata.fda.gov/drugsatfda_docs/appletter/2004/20592se1-019ltr.pdf. Accessed October 3, 2011.
7. Leucht S, Corves C, Arbter D, et al. Second-generation versus first-generation antipsychotic drugs for schizophrenia: a meta-analysis. Lancet. 2009;373(9657):31-41. PubMed doi:10.1016/S0140-6736(08)61764-X
8. Komossa K, Rummel-Kluge C, Hunger H, et al. Olanzapine versus other atypical antipsychotics for schizophrenia. Cochrane Database Syst Rev. 2010;(3):CD006654. PubMed
9. Rummel-Kluge C, Komossa K, Schwarz S, et al. Head-to-head comparisons of metabolic side effects of second generation antipsychotics in the treatment of schizophrenia: a systematic review and meta-analysis. Schizophr Res. 2010;123(2-3):225-233. PubMed doi:10.1016/j.schres.2010.07.012
10. Tohen M, Greil W, Calabrese JR, et al. Olanzapine versus lithium in the maintenance treatment of bipolar disorder: a 12-month, randomized, double-blind, controlled clinical trial. Am J Psychiatry. 2005;162(7):1281-1290. PubMed doi:10.1176/appi.ajp.162.7.1281
11. Tohen M, Calabrese JR, Sachs GS, et al. Randomized, placebo-controlled trial of olanzapine as maintenance therapy in patients with bipolar I disorder responding to acute treatment with olanzapine. Am J Psychiatry. 2006;163(2):247-256. PubMed doi:10.1176/appi.ajp.163.2.247
12. Furukawa TA, Barbui C, Cipriani A, et al. Imputing missing standard deviations in meta-analyses can provide accurate results. J Clin Epidemiol. 2006;59(1):7-10. PubMed doi:10.1016/j.jclinepi.2005.06.006
13. Higgins JPT, Green S, eds. Cochrane Handbook for Systematic Reviews of Interventions: Version 5.1.0. The Cochrane Collaboration, 2011. www.cochrane-handbook.org. Accessed October 3, 2011.
14. Streiner DL. Meta-analysis. PowerPoint presentation presented at the Department of Psychiatry, University of Toronto; September 21, 2010; Toronto, Ontario, Canada.
15. Tohen M, Sanger TM, McElroy SL, et al; Olanzapine HGEH Study Group. Olanzapine versus placebo in the treatment of acute mania. Am J Psychiatry. 1999;156(5):702-709. PubMed
16. Tohen M, Jacobs TG, Grundy SL, et al; The Olanzipine HGGW Study Group. Efficacy of olanzapine in acute bipolar mania: a double-blind, placebo-controlled study. Arch Gen Psychiatry. 2000;57(9):841-849. PubMed doi:10.1001/archpsyc.57.9.841
17. Tohen M, Vieta E, Calabrese J, et al. Efficacy of olanzapine and olanzapine-fluoxetine combination in the treatment of bipolar I depression. Arch Gen Psychiatry. 2003;60(11):1079-1088. PubMed doi:10.1001/archpsyc.60.11.1079
18. Tohen M, Vieta E, Goodwin GM, et al. Olanzapine versus divalproex versus placebo in the treatment of mild to moderate mania: a randomized, 12-week, double-blind study. J Clin Psychiatry. 2008;69(11):1776-1789. PubMed doi:10.4088/JCP.v69n1113
19. Tohen M, Goldberg JF, Gonzalez-Pinto Arrillaga AM, et al. A 12-week, double-blind comparison of olanzapine vs haloperidol in the treatment of acute mania. Arch Gen Psychiatry. 2003;60(12):1218-1226. PubMed doi:10.1001/archpsyc.60.12.1218
20. Zajecka JM, Weisler R, Sachs G, et al. A comparison of the efficacy, safety, and tolerability of divalproex sodium and olanzapine in the treatment of bipolar disorder. J Clin Psychiatry. 2002;63(12):1148-1155. PubMed doi:10.4088/JCP.v63n1210
21. Tohen M, Ketter TA, Zarate CA, et al. Olanzapine versus divalproex sodium for the treatment of acute mania and maintenance of remission: a 47-week study. Am J Psychiatry. 2003c;160(7):1263-1271. PubMed doi:10.1176/appi.ajp.160.7.1263
22. Kim B, Kim SJ, Son JI, et al. Weight change in the acute treatment of bipolar I disorder: a naturalistic observational study of psychiatric inpatients. J Affect Disord. 2008;105(1-3):45-52. PubMed doi:10.1016/j.jad.2007.04.006
23. Novick D, Gonzalez-Pinto A, Haro JM, et al; EMBLEM Advisory Board. Translation of randomised controlled trial findings into clinical practice: comparison of olanzapine and valproate in the EMBLEM study. Pharmacopsychiatry. 2009;42(4):145-152. PubMed doi:10.1055/s-0028-1128115
24. Niufan G, Tohen M, Qiuqing A, et al. Olanzapine versus lithium in the acute treatment of bipolar mania: a double-blind, randomized, controlled trial. J Affect Disord. 2008;105(1-3):101-108. PubMed doi:10.1016/j.jad.2007.04.020
25. Perlis RH, Baker RW, Zarate CA Jr, et al. Olanzapine versus risperidone in the treatment of manic or mixed states in bipolar I disorder: a randomized, double-blind trial. J Clin Psychiatry. 2006;67(11):1747-1753. PubMed doi:10.4088/JCP.v67n1112
26. Novick D, Reed C, Haro JM, et al. Comparison of olanzapine and risperidone in the EMBLEM study: translation of randomized controlled trial findings into clinical practice. Int Clin Psychopharmacol. 2010;25(5):257-263. PubMed doi:10.1097/YIC.0b013e32833b8fe4
27. McIntyre RS, Cohen M, Zhao J, et al. Asenapine versus olanzapine in acute mania: a double-blind extension study. Bipolar Disord. 2009;11(8):815-826. PubMed doi:10.1111/j.1399-5618.2009.00749.x
28. Citrome L. Asenapine for schizophrenia and bipolar disorder: a review of the efficacy and safety profile for this newly approved sublingually absorbed second-generation antipsychotic. Int J Clin Pract. 2009;63(12):1762-1784. PubMed doi:10.1111/j.1742-1241.2009.02228.x
29. Vieta E, Bourin M, Sanchez R, et al; Aripiprazole Study Group. Effectiveness of aripiprazole v haloperidol in acute bipolar mania: double-blind, randomised, comparative 12-week trial. Br J Psychiatry. 2005;187(3):235-242. PubMed doi:10.1192/bjp.187.3.235
30. Keck PE, McElroy SL. Bipolar disorder, obesity, and pharmacotherapy-associated weight gain. J Clin Psychiatry. 2003;64(12):1426-1435. PubMed doi:10.4088/JCP.v64n1205
31. Torrent C, Amann B, Sסnchez-Moreno J, et al. Weight gain in bipolar disorder: pharmacological treatment as a contributing factor. Acta Psychiatr Scand. 2008;118(1):4-18. PubMed doi:10.1111/j.1600-0447.2008.01204.x
32. Treuer T, Hoffmann VP, Chen AK, et al. Factors associated with weight gain during olanzapine treatment in patients with schizophrenia or bipolar disorder: results from a six-month prospective, multinational, observational study. World J Biol Psychiatry. 2009;10(4, Pt 3):729-740. PubMed doi:10.1080/15622970903079507
33. Lieberman JA, Stroup TS, McEvoy JP, et al; Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) Investigators. Effectiveness of antipsychotic drugs in patients with chronic schizophrenia. N Engl J Med. 2005;353(12):1209-1223. PubMed doi:10.1056/NEJMoa051688
34. Velligan DI, Weiden PJ, Sajatovic M, et al; Expert Consensus Panel on Adherence Problems in Serious and Persistent Mental Illness. The Expert Consensus Guideline Series: Adherence Problems in Patients With Serious and Persistent Mental Illness. J Clin Psychiatry. 2009;70(suppl 4):1-46, quiz 47-48. PubMed
35. Newcomer JW, Haupt DW. The metabolic effects of antipsychotic medications. Can J Psychiatry. 2006;51(8):480-491. PubMed
36. Soczynska JK, Kennedy SH, Woldeyohannes HO, et al. Mood disorders and obesity: understanding inflammation as a pathophysiological nexus. Neuromolecular Med. 2011;13(2):93-116. PubMed doi:10.1007/s12017-010-8140-8
37. McIntyre RS, Konarski JZ, Soczynska JK, et al. Medical comorbidity in bipolar disorder: implications for functional outcomes and health service utilization. Psychiatr Serv. 2006;57(8):1140-1144. PubMed doi:10.1176/appi.ps.57.8.1140
38. Kinon BJ, Basson BR, Gilmore JA, et al. Long-term olanzapine treatment: weight change and weight-related health factors in schizophrenia. J Clin Psychiatry. 2001;62(2):92-100. PubMed doi:10.4088/JCP.v62n0204
39. Jones B, Basson BR, Walker DJ, et al. Weight change and atypical antipsychotic treatment in patients with schizophrenia. J Clin Psychiatry. 2001;62(suppl 2):41-44. PubMed
40. Praharaj SK, Jana AK, Goyal N, et al. Metformin for olanzapine-induced weight gain: a systematic review and meta-analysis. Br J Clin Pharmacol. 2011;71(3):377-382. PubMed doi:10.1111/j.1365-2125.2010.03783.x
41. Narula PK, Rehan HS, Unni KE, et al. Topiramate for prevention of olanzapine associated weight gain and metabolic dysfunction in schizophrenia: a double-blind, placebo-controlled trial. Schizophr Res. 2010;118(1-3):218-223. PubMed doi:10.1016/j.schres.2010.02.001
42. Khazaal Y, Fresard E, Rabia S, et al. Cognitive behavioural therapy for weight gain associated with antipsychotic drugs. Schizophr Res. 2007;91(1-3):169-177. PubMed doi:10.1016/j.schres.2006.12.025
43. Kwon JS, Choi JS, Bahk WM, et al. Weight management program for treatment-emergent weight gain in olanzapine-treated patients with schizophrenia or schizoaffective disorder: a 12-week randomized controlled clinical trial. J Clin Psychiatry. 2006;67(4):547-553. PubMed doi:10.4088/JCP.v67n0405