Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
Cannabinoid hyperemesis syndrome (CHS) is a relatively new phenomenon first described in 2004, wherein chronic cannabis users presented with vomiting refractory to antiemetics that resolved with cannabis abstinence, with the peculiar observation that they were compulsive hot water bathers. CHS has since been described in a variety of contexts with a variety of complications.
Presently, 22 million Americans report current cannabis usage, a number that will most likely increase as legal prohibitions on cannabis decrease.

Cannabinoid Hyperemesis Syndrome Presenting With Spontaneous Pneumomediastinum
Cannabinoid hyperemesis syndrome (CHS) is a relatively new phenomenon first described in 2004, wherein chronic cannabis users presented with vomiting refractory to antiemetics that resolved with cannabis abstinence, with the peculiar observation that they were compulsive hot water bathers.1 CHS has since been described in a variety of contexts with a variety of complications.2-4
Presently, 22 million Americans report current cannabis usage, a number that will most likely increase as legal prohibitions on cannabis decrease.5 Similarly, the frequency of emergency department visits for cyclic vomiting of any etiology has doubled since marijuana legalization in Colorado, with the proportion of patients presenting with cyclic vomiting and reporting marijuana usage tripling.6
As such, it is imperative that we gain a greater understanding of CHS and its complications. Here, we report a case of CHS wherein the presenting symptom was spontaneous pneumomediastinum, which to our knowledge is the first of its kind.
Case Report
A 19-year-old man was transferred to our hospital for escalation of care. He presented to an outside hospital with a 4-day history of intractable emesis, with an acute onset of diffuse abdominal pain and constipation. The patient noted partial relief of nausea and vomiting with hot water showers. He had never experienced similar episodes. At the outside hospital, he was noted to have pneumomediastinum, precipitating his transfer.
The patient revealed daily marijuana usage since the age of 12 years, with a 1-year cessation at the age of 16 years. He had a 6-year history of alcohol use, ranging from 1 beer to 375 mL of liquor a week, with the most recent use 5 days prior to admission. He denied use of other drugs. A urine drug screen was obtained at the outside hospital, but the patient refused retrieval of documentation from the transferring hospital. His family history was unremarkable.
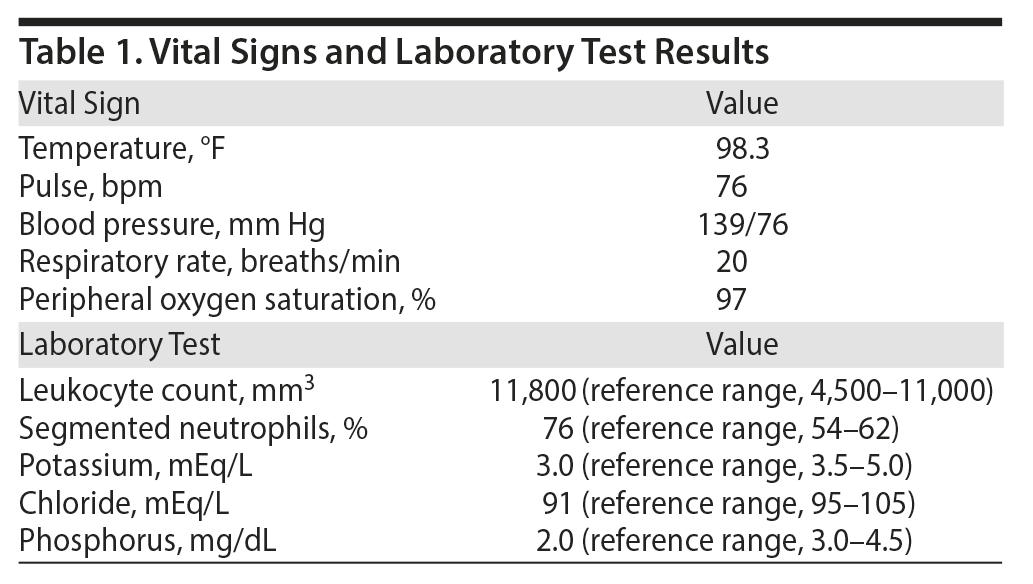
Physical examination revealed the patient to be in mild distress. The patient had crepitus of his neck on palpation and a nondistended abdomen with mild epigastric tenderness. He displayed a flat affect. Vital signs and laboratory test results are presented in Table 1.
A computed tomography scan of the chest demonstrated air tracking into the soft tissue of the neck and supraclavicular region, consistent with posterior pneumomediastinum. A barium swallow study demonstrated no esophageal extravasation. The patient’s pneumomediastinum was thus attributed to spontaneous pneumomediastinum, precluding surgical intervention. While his differential diagnosis at the outside hospital included pressure-induced esophageal rupture, known as Boerhaave syndrome, precipitated by cyclical vomiting syndrome, he was ultimately diagnosed with spontaneous pneumomediastinum secondary to CHS.
The patient was given intravenous normal saline and symptomatic management. He continued taking hot showers throughout his hospital stay. His pneumomediastinum, laboratory abnormalities, and symptoms improved on the fourth day of hospitalization, and he was discharged.
Conclusion
Spontaneous pneumomediastinum is well understood to be a consequence of alveolar rupture following an acute rise in intra-alveolar pressure.7 Vomiting precipitates up to 36%8 of cases, producing concern for the often lethal Boerhaave syndrome. Those with spontaneous pneumomediastinum are typically much younger than those with Boerhaave syndrome and appear well, unlike their toxic-appearing counterparts.7 It has been suggested that in young, otherwise healthy, and well-appearing patients, a full workup for Boerhaave syndrome is likely unnecessary.9
Although this is the first reported instance, to our knowledge, of CHS presenting with spontaneous pneumomediastinum, we suspect that it occurs somewhat frequently. And, considering the anticipated rise in prevalence of CHS, it stands to reason that an increase in spontaneous pneumomediastinum will be observed. As such, recognizing a potential relationship between CHS and spontaneous pneumomediastinum may allow the clinician to make a more expedient diagnosis with no extensive esophageal perforation workup.
Published online: March 26, 2020.
Potential conflicts of interest: None.
Funding/support: None.
Previous presentation: This work was previously presented at the Colloquium of Scholars Annual Update in Psychiatry; March 30, 2019; Philadelphia, Pennsylvania and the Camden Scholars’ Forum; April 15, 2019; Camden, New Jersey.
Additional information: Information has been de-identified to protect anonymity.
REFERENCES
1.Allen JH, de Moore GM, Heddle R, et al. Cannabinoid hyperemesis: cyclical hyperemesis in association with chronic cannabis abuse. Gut. 2004;53(11):1566-1570. PubMed CrossRef
2.Argamany JR, Reveles KR, Duhon B. Synthetic cannabinoid hyperemesis resulting in rhabdomyolysis and acute renal failure. Am J Emerg Med. 2016; 34: 765 e1-e2.
3.Bonnet U. An Overlooked Victim of Cannabis: Losing Several Years of Well-being and Inches of Jejunum on the Way to Unravel Her Hyperemesis Enigma. Clin Neuropharmacol. 2016;39(1):53-54. PubMed CrossRef
4.Nourbakhsh M, Miller A, Gofton J, et al. Cannabinoid Hyperemesis Syndrome: Reports of Fatal Cases. J Forensic Sci. 2019;64(1):270-274. PubMed CrossRef
5.Lapoint J, Meyer S, Yu CK, et al. Cannabinoid hyperemesis syndrome: public health implications and a novel model treatment guideline. West J Emerg Med. 2018;19(2):380-386. PubMed CrossRef
6.Kim HS, Anderson JD, Saghafi O, et al. Cyclic vomiting presentations following marijuana liberalization in Colorado. Acad Emerg Med. 2015;22(6):694-699. PubMed CrossRef
7.Forshaw MJ, Khan AZ, Strauss DC, et al. Vomiting-induced pneumomediastinum and subcutaneous emphysema does not always indicate Boerhaave’s syndrome: report of six cases. Surg Today. 2007;37(10):888-892. PubMed CrossRef
8.Caceres M, Ali SZ, Braud R, et al. Spontaneous pneumomediastinum: a comparative study and review of the literature. Ann Thorac Surg. 2008;86(3):962-966. PubMed CrossRef
9.Bakhos CT, Pupovac SS, Ata A, et al. Spontaneous pneumomediastinum: an extensive workup is not required. J Am Coll Surg. 2014;219(4):713-717. PubMed CrossRef
aCooper Medical School of Rowan University, Camden, New Jersey
bDepartment of Psychiatry, Cooper University Hospital, Camden, New Jersey
cChildren’s Hospital of Philadelphia, Philadelphia, Pennsylvania
‘ ¡These authors contributed equally to this report.
*Corresponding author: Consuelo Cagande, MD, Children’s Hospital of Philadelphia, 3440 Market St, Ste 410, Philadelphia, PA 19104 ([email protected]).
Prim Care Companion CNS Disord 2020;22(2):19l02509
To cite: Davis W, Frye K, Shah D, et al. Cannabinoid hyperemesis syndrome presenting with spontaneous pneumomediastinum. Prim Care Companion CNS Disord. 2020;22(2):19l02509.
To share: https://doi.org/10.4088/PCC.19l02509
© Copyright 2020 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!