Objective: This retrospective study assessed the cost of illness and medical and psychiatric comorbidities in adults with attention-deficit/hyperactivity disorder (ADHD) compared with adults without ADHD (matched 1:3) and adults with depression (1:1). Individuals with depression were included as a benchmark against which the burden of ADHD could be measured.
Method: Measures of health care and employment-related costs were compared to generate estimates of medical expenditures, workplace absences, and comorbidities in adults with ADHD (using ICD-9-CM codes) who were enrolled in employer-sponsored health plans throughout 2006. Individuals with ADHD (31,752) were matched with 95,256 non-ADHD controls. The majority of individuals with ADHD (n = 29,965) were also matched with an equal number of individuals with a depression diagnosis (using ICD-9-CM codes).
Results: In this adult population with ADHD enrolled in an employer-sponsored health plan, medical and psychiatric comorbidities were the primary drivers of health care utilization and cost. Of note, depression was significantly prevalent among those with ADHD compared to matched non-ADHD controls (14% vs 3.2%; P ≤ .0001). Subgroup analysis demonstrated that ADHD patients with depression had a significantly higher number of medical and other psychiatric comorbid illnesses including diabetes, hypertension, asthma, irritable bowel syndrome, bipolar disorder, anxiety, alcohol abuse, and substance abuse compared to those with ADHD alone (P ≤ .0001). Patients with ADHD incurred higher total annual health care expenditures than control subjects ($4,306 vs $2,418); approximately 15% of costs were paid by the patient. The total annual costs associated with productivity losses were also higher (driven by differences in short-term disability costs) in the ADHD group compared with controls ($4,403 vs $4,209).
Conclusions: Medical and psychiatric comorbidities were primary drivers of the direct health care cost associated with ADHD in adult patients. The present study demonstrated that the total costs of ADHD among adults are doubled when indirect costs associated with workplace productivity losses are included.
Prim Care Companion CNS Disord 2011;13(2):e1-e12
© Copyright 2011 Physicians Postgraduate Press, Inc.
Submitted: May 28, 2010; accepted October 21, 2010.
Published online: April 14, 2011 (doi:10.4088/PCC.10m01030).
Corresponding author: Paul Hodgkins, PhD, Global Health Economics and Outcomes Research, Shire Development Inc, 725 Chesterbrook Blvd, Wayne, PA 19087 ([email protected]).
Cost of Illness and Comorbidities in Adults Diagnosed
With Attention-Deficit/Hyperactivity Disorder:
A Retrospective Analysis
Objective: This retrospective study assessed the cost of illness and medical and psychiatric comorbidities in adults with attention-deficit/hyperactivity disorder (ADHD) compared with adults without ADHD (matched 1:3) and adults with depression (1:1). Individuals with depression were included as a benchmark against which the burden of ADHD could be measured.
Method: Measures of health care and employment–related costs were compared to generate estimates of medical expenditures, workplace absences, and comorbidities in adults with ADHD (using ICD-9-CM codes) who were enrolled in employer-sponsored health plans throughout 2006. Individuals with ADHD (31,752) were matched with 95,256 non-ADHD controls. The majority of individuals with ADHD (n = 29,965) were also matched with an equal number of individuals with a depression diagnosis (using ICD-9-CM codes).
Results: In this adult population with ADHD enrolled in an employer-sponsored health plan, medical and psychiatric comorbidities were the primary drivers of health care utilization and cost. Of note, depression was significantly prevalent among those with ADHD compared to matched non-ADHD controls (14% vs 3.2%; P ≤ .0001). Subgroup analysis demonstrated that ADHD patients with depression had a significantly higher number of medical and other psychiatric comorbid illnesses including diabetes, hypertension, asthma, irritable bowel syndrome, bipolar disorder, anxiety, alcohol abuse, and substance abuse compared to those with ADHD alone (P ≤ .0001). Patients with ADHD incurred higher total annual health care expenditures than control subjects ($4,306 vs $2,418); approximately 15% of costs were paid by the patient. The total annual costs associated with productivity losses were also higher (driven by differences in short-term disability costs) in the ADHD group compared with controls ($4,403 vs $4,209).
Conclusions: Medical and psychiatric comorbidities were primary drivers of the direct health care cost associated with ADHD in adult patients. The present study demonstrated that the total costs of ADHD among adults are doubled when indirect costs associated with workplace productivity losses are included.
Prim Care Companion CNS Disord 2011;13(2):e1–e12
© Copyright 2011 Physicians Postgraduate Press, Inc.
Submitted: May 28, 2010; accepted October 21, 2010.
Published online: April 14, 2011 (doi:10.4088/PCC.10m01030).
Corresponding author: Paul Hodgkins, PhD, Global Health Economics and Outcomes Research, Shire Development Inc, 725 Chesterbrook Blvd, Wayne, PA 19087 ([email protected]).
Attention-deficit/hyperactivity disorder (ADHD) is a neurobehavioral condition characterized by core symptoms of inattentiveness, hyperactivity, and impulsivity that can manifest as disruptions in the academic, social, and home settings.1 Although once considered to be a childhood disorder, there is a growing recognition of the persistence of ADHD into adulthood and the need for treatment.2–10 The 12-month prevalence of adults with ADHD in the United States has been estimated to be 4.4%,11 making it one of the most common psychiatric disorders of adulthood. A recent meta-analysis of studies of ADHD among adults from a number of countries reported a pooled prevalence of 2.5%.12
In the workplace, ADHD places a potentially large economic burden on employers, who incur direct and indirect health care costs associated with ADHD and comorbid illnesses, resulting in significant loss in productivity.13,14 Accordingly, a 2006 study estimated the loss of ADHD-related economic productivity to be between $67 billion and $116 billion.14 In comparison, the economic burden of asthma has been estimated to be $20 billion.15 In a 2005 study of ADHD in an employed population,16 individuals with ADHD had more comorbidities (including anxiety, bipolar disorder, depression, drug or alcohol abuse, antisocial disorder, and oppositional defiant disorder), lost more work time, and utilized more health care resources than those who sought professional care for other medical problems. The same study showed that total medical costs for adults with ADHD were almost twice those of individuals without ADHD ($5,651 vs $2,771, respectively). Another study showed that each year employees with ADHD have a mean excess of 8.4 days of absence from work, 21.7 days with reduced work quantity, and 13.6 days with reduced work quality compared with employees without the condition.17 These workplace-related performance issues associated with ADHD accounted for an estimated 143.8 million days of lost productivity in the 10 countries studied.17 In the United States in 2000, work loss accounted for 12% of the estimated $31.6 billion cost of adults with ADHD or $3.7 billion.18
The objective of this study was to determine the burden of adults with ADHD in an employed population by measuring the prevalence of comorbidities and the cost of illness associated with health care utilization and workplace productivity loss comparisons in 2 groups (non-ADHD control and depression). To compare the health care utilization and annual cost of ADHD, the present study used depression as a benchmark, as depression is one of the most prevalent psychiatric conditions. It is a leading cause of social and economic burdens, costing an estimated $26.1 billion annually in medical care and up to $51.5 billion in lost productivity.19,20
METHOD
Data Source
This was a retrospective analysis of health care claims and employer-reported productivity data for calendar year 2006 taken from the MarketScan Commercial Claims and Encounters (commercial) and the Health and Productivity Management (HPM) databases. The commercial database contained inpatient, outpatient, and outpatient prescription details of employees and their dependents from more than 100 self-insured large employers located throughout all 50 states. However, members from the North Central and South census regions were overrepresented compared to the US Census 2000 population distribution data (36% vs 23% and 48% vs 36%, respectively), whereas the Northeast was underrepresented (9% vs 19%). The number of adults included in the commercial database was between 5.7 million and 9.6 million in each calendar year from 2002 to 2007. The HPM database contained workplace absence, short-term disability, and worker’s compensation data for a subset of individuals in the larger commercial database. Confidentiality and anonymity of person-level data were maintained in accordance with the guidelines of the Health Insurance Portability and Accountability Act.
Study Population
ADHD group. Adults 18 years of age or older on November 30, 2006, meeting the following criteria were included: have at least 1 evaluation and management or psychiatry claim carrying a diagnosis of ADHD in the period 2002 to 2007; at least 1 confirmatory ADHD diagnosis within 12 months of the first diagnosis; evidence of continuing treatment for ADHD in 2006, if the initial diagnosis predated 2006; and continuous enrollment in a health plan with pharmacy benefits in 2006. A diagnosis of attention-deficit disorder was defined as a claim carrying an International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) code of 314.0, 314.00 (attention-deficit disorder without mention of hyperactivity), or 314.01 (attention-deficit disorder with mention of hyperactivity). One or more claims with an ADHD diagnosis or drug claims for an ADHD-related medication were regarded as evidence of continuing treatment.
Non-ADHD control group (comparator). Any adult member in the commercial database with continuous enrollment in a health plan in 2006 and with no claims for a diagnosis of 314.0x in 2002–2007 met the inclusion criteria. The control group was not limited to those who utilized health care services in 2006 and thus included patients with zero costs. Controls were matched 3:1 to ADHD patients on the basis of gender, 5-year age bands (based on age as of January 1, 2006), geographical region, and the presence of capitated services in 2006. The control to test group match ratio was optimized to 3:1 to yield increased statistical power relative to a 1:1 match.21
Depression group (comparator). A similar methodology to the selection of the ADHD sample was adopted to identify members with depression. Briefly, adult members with no claims for ADHD but evidence of depression on the basis of ICD-9-CM codes 296.2x (major depressive disorder, single episode), 296.3x (major depressive disorder, recurrent episode), 300.4 (neurotic depression, dysthymic disorder), or 311 (depressive disorder, not otherwise classified) with at least 1 additional claim for confirmatory diagnosis within 12 months were identified from the commercial database. The depression group was matched 1:1 to the ADHD sample on the basis of gender, 5-year age bands, region, and the presence of capitated services in 2006. Patients with ADHD who could not be matched to the depression group were not included in the comparative analysis.
Individuals with capitated services were excluded from expenditure analyses because records for health care services under capitated plans usually exclude cost data. Nevertheless, matching on capitated services allowed matched samples to remain intact after individuals with capitated services were dropped. In the HPM database, individuals were matched by employer between cohorts when possible in an attempt to ensure that matches had similar paid time-off benefits. If no match could be made by employer, individuals were matched on the availability of data on absences, short-term disability, and worker’s compensation.
Variables
Comorbid burden. The comorbid burden was assessed using individuals’ scores on the Charlson Comorbidity Index (CCI).22 This measure assigns a weight from 1 (least severe) to 6 (most severe) to 17 medical conditions; the only conditions given a weighting of 6 were metastatic solid tumor and human immunodeficiency virus. A summed score (0 to 33) was then assigned to each individual as a composite indicator of comorbid burden on the basis of the presence of these diagnoses. Comorbid burden was also assessed independently by the presence of at least 1 nondiagnostic claim during 2006 for each of the following specific medical and psychiatric comorbidities that were considered to be of interest due to their association with ADHD in the literature: obesity, diabetes, hypothyroidism, hypertension, other cardiovascular disease, asthma, enuresis, irritable bowel syndrome, injuries, insomnia, depression, bipolar disorder, anxiety, social phobia, antisocial disorder, oppositional defiant disorder, obsessive-compulsive disorder, alcohol abuse, substance abuse, and eating disorders.16
Health care utilization and expenditure analyses. The annual direct health care costs incurred were assessed by the utilization and expenditure data, which were categorized by type of service (inpatient, emergency department visit, outpatient visit, other outpatient services, and outpatient prescriptions) and diagnosis (psychiatric and nonpsychiatric). Health care expenditures (total, psychiatric, and nonpsychiatric) were calculated as the sum of the costs paid by the individual (patient responsibility portion) and the health plan (health plan portion) in 2006 US dollars.
Productivity measures. To assess the indirect costs of ADHD, workplace productivity loss was compared between the ADHD and comparator groups. The measures that were used were absences (the number of days of absence and associated cost estimated using the US Bureau of Labor Statistics Current Population Survey data for the same age, gender, and region), short-term disability (number of days and associated cost, calculated as 70% of the costs from the US Bureau of Labor Statistics data), and workers’ compensation (number of claims and associated cost taken from information provided by the employer). The 70% value used to calculate short-term disability costs approximates the proportion of total wages and benefits paid by employers in the HPM database, as reported in previous studies on the basis of the MarketScan databases.23,24 Each productivity measure was evaluated separately, as not all employers reported all 3 types of data. Costs resulting from lost productivity were compared between matched groups (ie, ADHD vs non-ADHD controls and ADHD vs depression).
Statistical Analysis
Descriptive statistics were used to compare the 2 pairs of matched groups (ADHD vs non-ADHD controls, ADHD vs depression). Chi-square tests were used to test significance for categorical variables, and t tests were used for continuous variables. P values less than .05 were considered statistically significant.
Multivariate analyses of expenditure were conducted to control for treatment differences within the ADHD sample and differences between the ADHD and non-ADHD control or depression samples that remained after matching. The cost models estimated the burden of ADHD in terms of health care expenditures and costs related to productivity loss (absenteeism, short-term disability, and worker’s compensation) using individuals’ demographic variables and comorbidity as independent variables. General linear models, which are commonly employed when analyzing skewed data like health care costs, were run for each cost model using the γ distribution function and log link. The Park test was used to check the selection of variance and link functions.25,26
RESULTS
Between 2002 and 2007, the commercial database contained 342,284 individuals with at least 1 ADHD claim, including 150,936 adults. Of this sample population, 31,752 adults met the inclusion criteria for the ADHD group. These individuals were matched in a 1:3 ratio with non-ADHD controls (n = 95,256), and 29,965 were matched to an equal number of individuals with depression. Depression matches could not be found for all of the individuals with ADHD because the depression sample yielded older individuals compared with the ADHD sample. Spouses and dependents of employed members constituted approximately 60% of the sample population.
Baseline Demographics
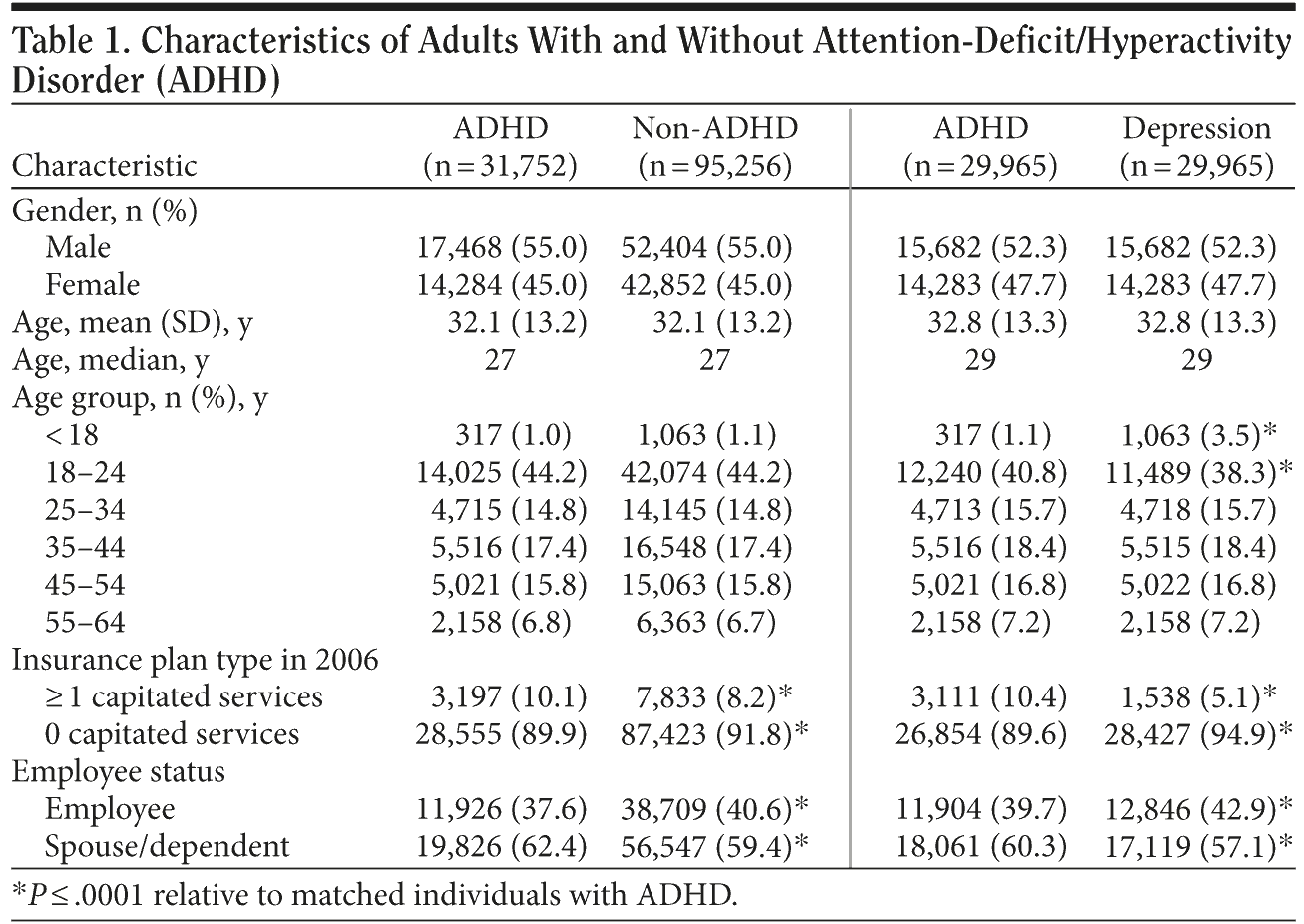
The proportion of males in the ADHD and non-ADHD control groups was the same (55.0%), as was the proportion of males in the ADHD and depression groups (52.3%; Table 1), due to matching. There was no significant difference in mean age between the ADHD and non-ADHD control groups, or between the ADHD and depression groups (Table 1). In this nationwide sample, the geographic distribution of patients in the different groups (ADHD vs non-ADHD control, ADHD vs depression) ranged from 11.0% to 12.6% in the Northeast, 27.3% to 32.8% in the North Central region, 38.3% to 47.3% in the South, and 15.5% to 17.6% in the West on the basis of known/nonmissing data, thus reflecting the overall regional population distribution of the commercial database.
Comorbidities
The mean CCI scores were low in all cohorts; however, the scores were significantly lower in the ADHD group than in the non-ADHD control group (0.15 vs 0.18, respectively; P < .0001), although the absolute difference between these groups was very small and not considered clinically relevant (data not shown). Among the medical/physical comorbidities, 8 of the 11 conditions were more prevalent in the ADHD group than in the non-ADHD control group (Figure 1A). Although there were no significant differences between groups in the proportion of individuals reporting hypertension or other cardiovascular diseases, there were significantly more individuals with diabetes in the non-ADHD control group. By contrast, a number of psychiatric conditions, including depression, bipolar disorder, anxiety, alcohol abuse, and substance abuse, were more prevalent in the ADHD group than in the non-ADHD control group (Figure 1A). Of significance was the high prevalence of depression in the ADHD group compared with the non-ADHD control group (14.0% vs 3.2%; P ≤ .0001). The next 2 most commonly observed psychiatric comorbidities in the ADHD group, anxiety and bipolar disorder, occurred at a rate 3 to 6 times higher than in the non-ADHD control group (P ≤ .0001).
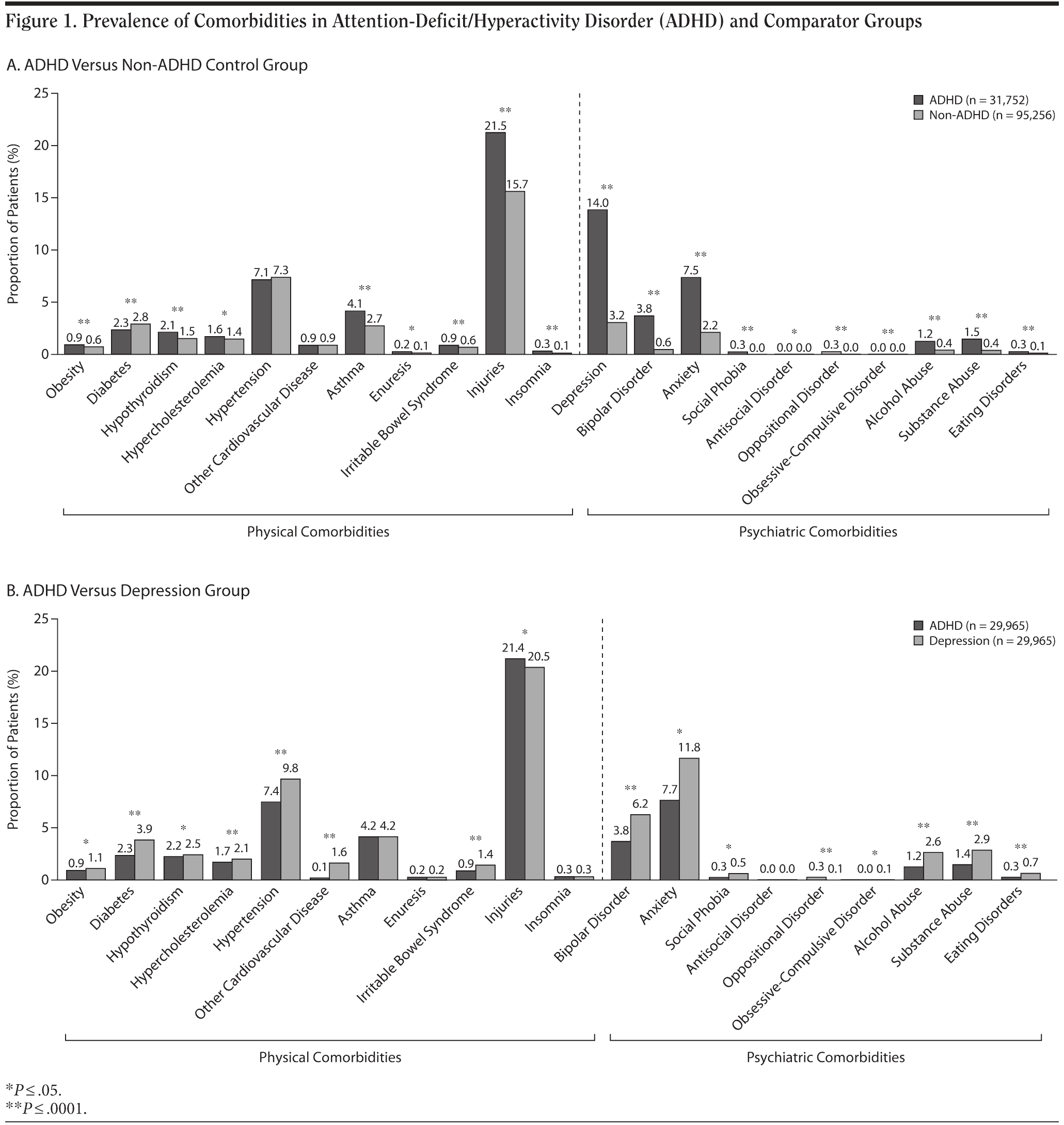
Comparison of the ADHD group with the depression comparator group showed that the mean CCI score was significantly lower in the ADHD group than in the depression group (0.16 vs 0.25, respectively; P < .0001), although the absolute difference was again very small (data not shown). Notably, physical comorbidities such as injuries were more common in the ADHD group (21.4 vs 20.5; P < .05), whereas most medical comorbidities were significantly more prevalent in the depression group (Figure 1B). Most psychiatric comorbidities, including bipolar disorder, anxiety, alcohol abuse, substance abuse, and eating disorders, occurred in approximately twice as many individuals in the depression group as in the ADHD group (P ≤ .0001; P ≤ .05 for anxiety only; Figure 1B).
Subgroup Analysis of ADHD Group: Comorbidities
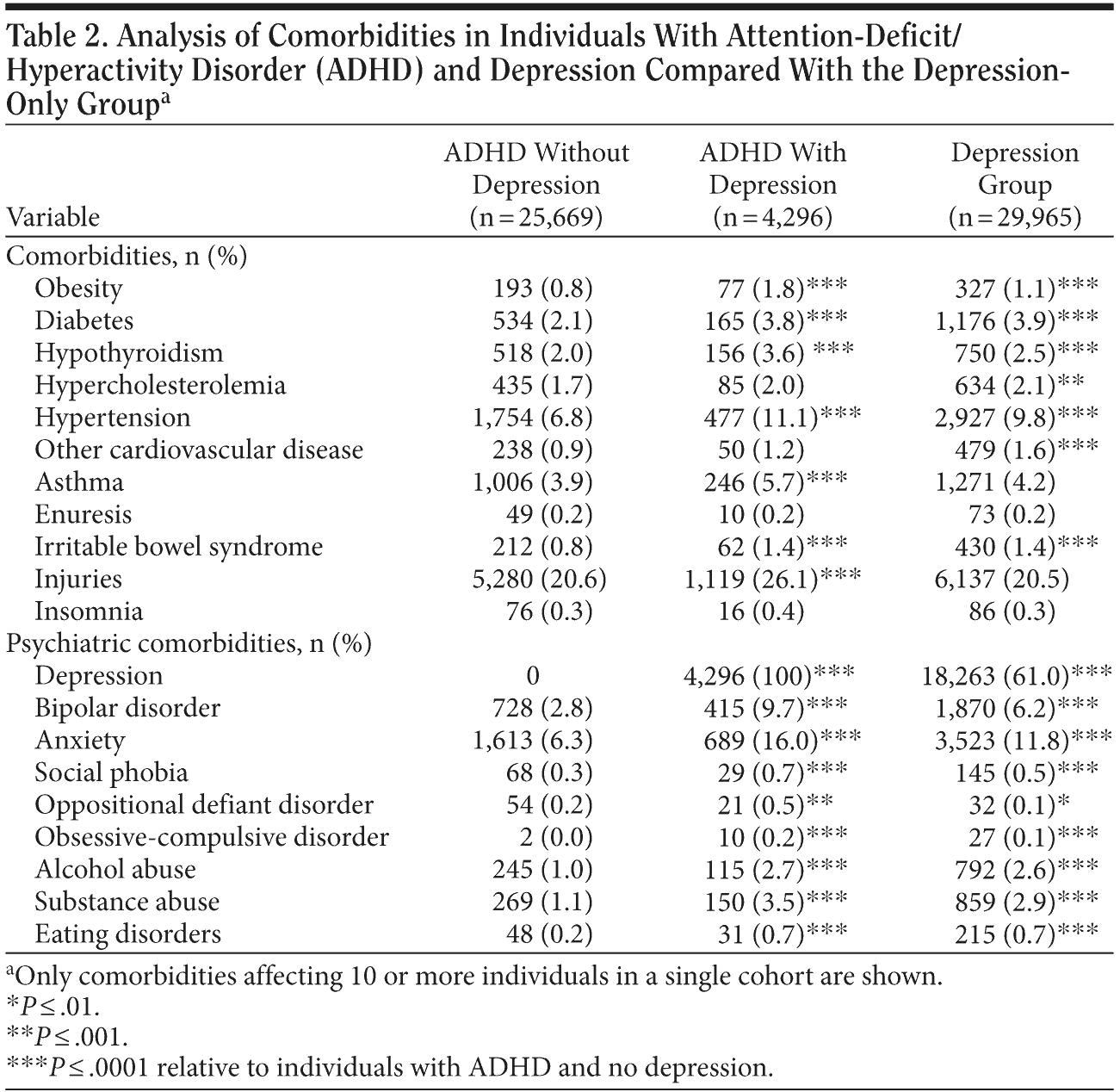
Because depression was prevalent in patients with ADHD, a subgroup analysis was performed to assess the impact of depression on the incidence of medical and other psychiatric comorbidities that may drive health care utilization and cost. The analysis showed that ADHD patients with depression also had significantly more medical comorbidities, including obesity, diabetes, hypothyroidism, hypertension, asthma, and irritable bowel syndrome, compared to those individuals with ADHD alone (Table 2). Similarly, a higher prevalence of psychiatric comorbidities was evident in patients with ADHD and depression than in those with ADHD alone. Notably, the extent of medical and psychiatric comorbidities in ADHD patients with depression was comparable to those patients in the depression comparator group (Table 2).
Health Care Utilization and Annual Total Cost
Psychiatric health care services. Compared with non-ADHD controls, ADHD patients utilized more psychiatric services and were approximately 3 times more likely to have inpatient admissions or emergency department visits, approximately 10 times more likely to have outpatient visits or use other outpatient services, and approximately 5 times more likely to claim for outpatient prescriptions (P < .0001 for all comparisons; Figure 2A).
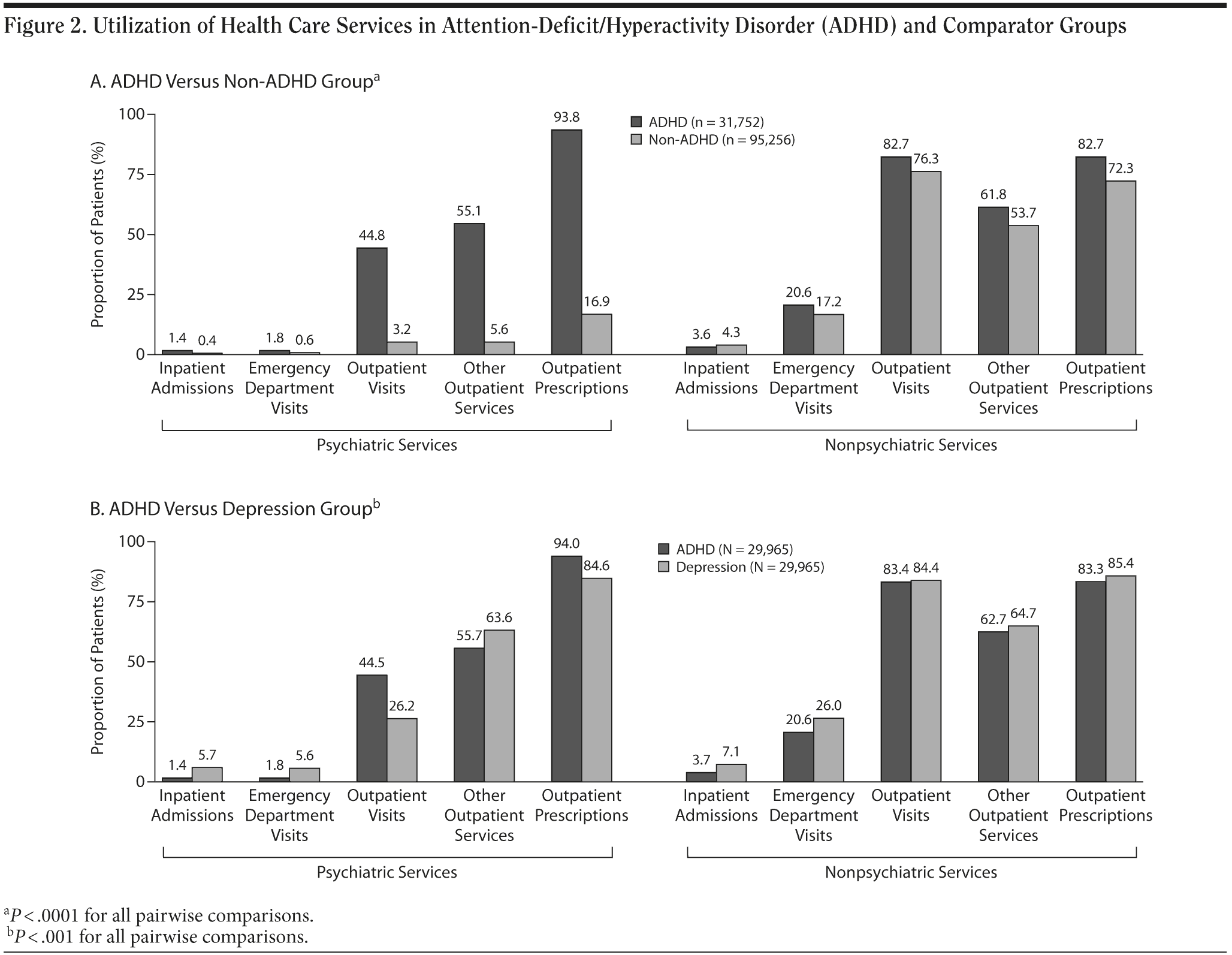
Compared with individuals in the depression comparator group, those with ADHD were 3 times less likely to have psychiatric inpatient admissions and emergency department visits (P < .001; Figure 2B). However, psychiatric outpatient visits and prescriptions were more common in the ADHD group than in those with depression (44.5% vs 26.2% and 94.0% vs 84.6%, respectively; P < .001 for both comparisons).
Nonpsychiatric health care services. Individuals with ADHD were more likely to use most categories of nonpsychiatric health care than non-ADHD controls (P < .0001), with the exception of nonpsychiatric inpatient admissions. The use of this service was significantly higher among non-ADHD controls (3.6% ADHD group vs 4.3% non-ADHD controls; P < .0001; Figure 2A). Compared with individuals with depression, individuals with ADHD were less likely to use all of the nonpsychiatric health care services categories examined in this study (P < .001; Figure 2B).
Annual Health Care Costs
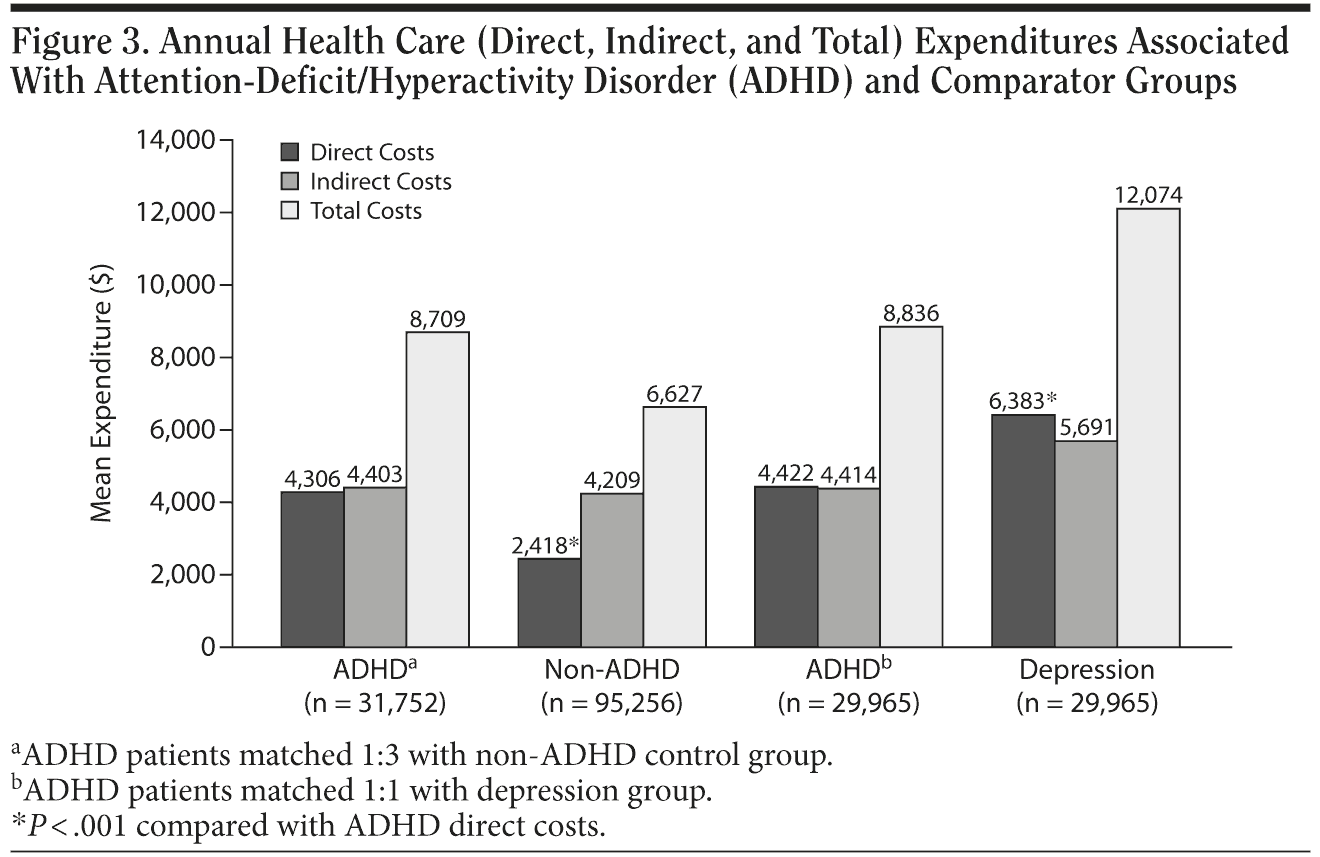
Total direct costs. Individuals with ADHD incurred higher total health care expenditures than non-ADHD controls; mean total expenditures were $4,306 and $2,418 (P < .001; Figure 3), with median values of $2,270 and $606, respectively. The health plan–paid and patient-paid portions for direct costs were higher in the ADHD group (mean costs of $3,586 [median of $1,712] and $720 [median of $480], respectively) than in the non-ADHD control group ($2,058 [median of $395] and $360 [median of $193], respectively; P < .001 for the difference between mean values; Figure 3). In comparisons between ADHD and depression groups, however, the reverse was observed; the ADHD group incurred significantly lower direct costs (mean of $4,422 [median of $902] vs $6,383 [median of $1,219]; P < .001; Figure 3).
Psychiatric health care expenditures. Individuals with ADHD incurred higher total psychiatric health care expenditures than non-ADHD controls. Total mean psychiatric health care costs (annual) were $1,675 and $183 (P < .001; Figure 4), with median values of $1,053 and $0, respectively. Although individuals with depression had significantly higher mean psychiatric health care expenditures than individuals with ADHD ($1,943 vs $1,704; P < .001; Figure 4), median costs were lower than in individuals with ADHD ($879 vs $1,075). The health plan–paid and patient-paid portions for total psychiatric and nonpsychiatric expenditures were also lower in the ADHD group than in the depression group (plan-paid and patient-paid mean costs for total psychiatric expenditure: $1,359 and $345 vs $1,566 and $377 for ADHD vs depression groups, respectively; for nonpsychiatric expenditures: $2,327 and 391 vs $3,894 and 551 for ADHD vs depression groups, respectively; Figure 4).
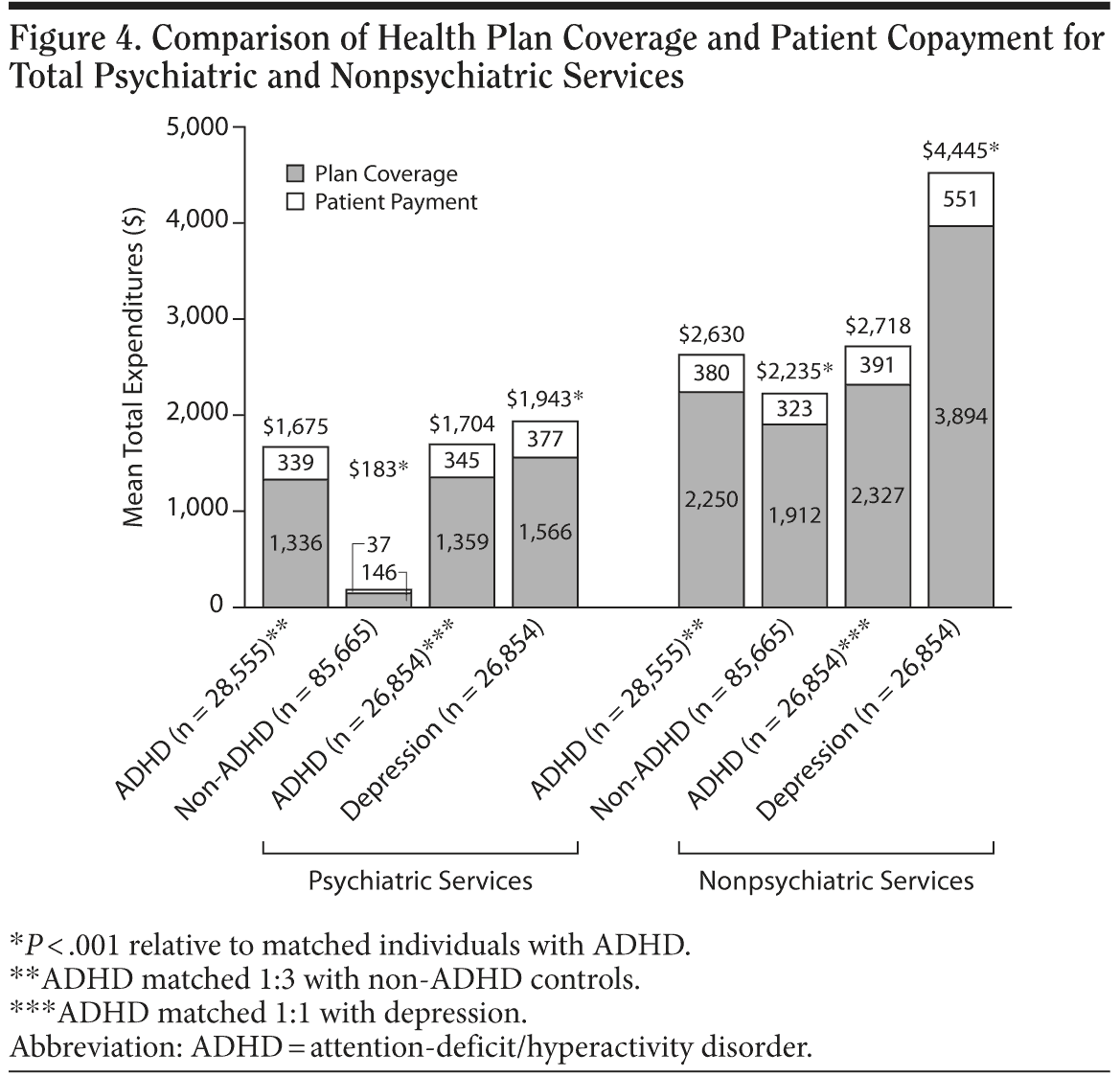
Nonpsychiatric health care expenditures. Nonpsychiatric health care expenditures followed similar trends to those observed for psychiatric health care expenditures (Figure 4). Mean nonpsychiatric costs for individuals with ADHD were $2,630 (median of $857) compared with $2,235 (median of $544) for non-ADHD controls (P < .001) and $2,718 (median of $902) compared with $4,445 (median of $1,219) for individuals with depression (P < .001; Figure 4). Of note, mean nonpsychiatric expenditures accounted for a larger proportion of total expenditure among individuals with depression ($4,445/$6,388; 70%) than among those with ADHD ($2,718/$4,422; 61%).
Multivariate analysis. Multivariate analysis confirmed that individuals with ADHD incurred higher annual health care expenditures than non-ADHD controls (general linear model coefficient = 0.57; standard error = 0.03; P ≤ .01). Although the rates of comorbidities were generally low overall, multivariate analysis revealed that each of the comorbidities examined was associated with higher health care expenditures in individuals with ADHD compared with non-ADHD controls (P ≤ .05), with the exception of asthma and insomnia (P = not significant).
Individuals with ADHD incurred lower expenditures than individuals with depression (general linear model coefficient = 0.05; standard error = 0.02; P ≤ .05). The prevalence of comorbidities was higher in the depression group than in the ADHD group, which may contribute to the higher expenditures observed in the depression group relative to the ADHD group.
Productivity loss and associated (indirect) annual costs. In the ADHD versus non-ADHD control comparison, total annual costs associated with productivity losses (absences, short-term disability leave, and worker’s compensation claims) were $4,403 and $4,209. In the ADHD versus depression comparison, these costs were $4,414 and $5,691, respectively (Figure 3).
There were no significant differences between the ADHD and non-ADHD control groups in terms of the proportion of individuals with absence days (and related costs) or in the likelihood of incurring a worker’s compensation claim (and related costs) (Table 3). However, compared with non-ADHD controls, more individuals with ADHD were out on short-term disability (10.8% vs 7.6% of individuals; P < .0001). Individuals with ADHD also had approximately 50% longer mean ± SD periods of short-term disability (6.8 ± 0.6 days vs 4.1 ± 0.3 days; P < .0001) and incurred higher mean short-term disability-related costs ($743 vs $424; P < .0001; Table 3).
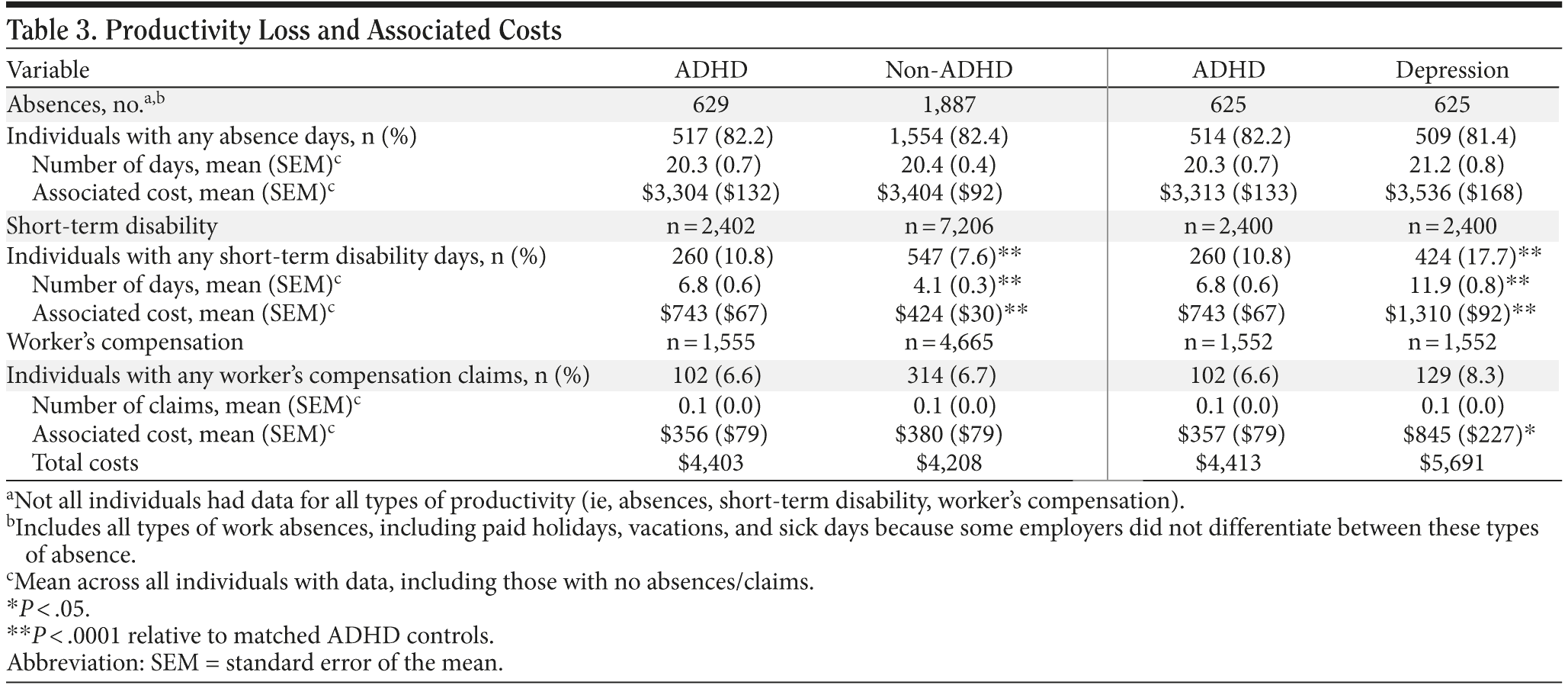
Both ADHD and depression groups were not significantly different in terms of workplace absence and associated indirect costs, or in the likelihood of having a worker’s compensation claim, although mean worker’s compensation costs were significantly lower in the ADHD group ($357 vs $845; P < .05; Table 3). Individuals with ADHD were approximately 60% less likely to report short-term disability and incurred approximately 73% lower costs related to short-term disability than individuals with depression (10.8% vs 17.7%; $743 vs $1,310; P < .0001 for both; Table 3).
Subgroup Analysis: Productivity Loss
Patients with ADHD and depression were more likely to incur productivity loss from short-term disability compared to those patients with ADHD or depression alone. Accordingly, costs associated with short-term disability in individuals with ADHD and depression were approximately 3 times higher than in individuals with ADHD alone ($1,748 vs $574, respectively; P = .0000) but not significantly different from those in the depression comparator group ($1,748 vs $1,310, respectively; P = .0934). There was no significant difference among ADHD, depression, and ADHD with depression cohorts in the proportion of individuals with worker’s compensation claims or costs associated with worker’s compensation.
DISCUSSION
This study demonstrated that adults with ADHD have more medical/physical and psychiatric comorbidities than matched non-ADHD controls and incur higher health care utilization and cost. The comorbidities with the largest significant differences between ADHD and non-ADHD controls included depression, anxiety, asthma, and bipolar disorder.
In a survey of adults with mental health and substance abuse disorders treated in community hospitals in the United States in 2004,27 more than 90% of individuals with ADHD presented with an additional mental health and substance abuse disorder compared with 71% of those with depressive disorders. It should be noted that alcohol/substance abuse rates were very low (≤ 5%) in the present study, but many of the comorbidities examined were reported by more individuals with depression than by those with ADHD. The only 2 comorbidities that were reported by more individuals with ADHD than individuals with depression were injuries and oppositional defiant disorder. Oppositional defiant disorder is one of the most frequent psychiatric comorbidities in children with ADHD,28 and although it was significantly more common among individuals with ADHD than among those with depression in this study, the number of individuals with this comorbidity was very small, probably due to their age.
After controlling for differences between groups, individuals with ADHD had higher health care expenditures than non-ADHD controls. These findings are broadly consistent with studies based on previous data.4,29 Our results can also be compared with those from an earlier study that estimated the 6-month cost of treating ADHD in adults to be between $2,000 and $2,500.30 However, there are a number of differences that should be considered when comparing cost data. Although both studies were based on claims data, the present study included both direct and indirect (productivity-related) costs based on total billed charges; in contrast, the Wu et al30 study included only direct costs paid by the health plan, excluding patient copayments and deductibles. Furthermore, the MarketScan data presented here were drawn from 2002 to 2007 (with a focus on 2006) and were based on prescriptions for any ADHD medications, while the study by Wu et al30 was based on data from 1999 to 2004 and looked specifically at osmotic-release oral system methylphenidate, mixed amphetamine salts extended release, and atomoxetine.
Despite these differences, the study by Wu et al30 still provides an interesting benchmark for the present analysis. To compare the 2 studies, the direct costs of ADHD treatment in our study could be recalculated to more closely mimic those reported by Wu et al30 (ie, costs for 6 months of therapy rather than 1 year and including only costs paid by health plans, rather than those paid by the health plans and the patient). Despite the methodological differences between studies, the approximate mean 6-month direct costs paid by the health plan in the present study ($1,793 for the adults with ADHD who were compared with non-ADHD controls; $1,843 for those compared with individuals with depression) are broadly similar to those reported by Wu et al30 ($2,008 to $2,540, dependent on the ADHD medication prescribed).
Our study adds important information to the results reported by Wu et al.30 Most significantly, the present study shows the total costs of ADHD in adults are doubled when indirect costs (those associated with productivity losses) are included. Mean direct treatment costs were $4,306 and $4,422 in the ADHD cohorts included in our study, while mean indirect costs were $4,403 and $4,414. Our study also shows that patient copayments add considerably to the costs paid by the health plan, accounting for approximately 15% of the total direct health care expenditure for individuals with ADHD ($720 from a total cost of $4,306). For payers trying to calculate the total economic burden of ADHD in adults, it is important that indirect costs and patient copayments are included. In the present study, the total annual cost of ADHD was over $8,500 ($3,586 direct costs paid by the health plan, $720 direct costs paid by the patient, and $4,403 in indirect costs), which is approximately double the direct costs paid by the health plan, as reported previously.
In addition to the direct (treatment) and indirect (productivity) costs for adults with ADHD, there is evidence that health care–related costs for relatives of individuals with the disorder are also increased. More recently, Kleinman et al31 have reported health benefit costs and absenteeism data for employees with ADHD and for employees with children with the disorder. Compared with individuals without ADHD, those with ADHD had significantly higher annual health benefit costs ($6,885 vs $4,242; P < .0001) and significantly more days of health-related absence (8.9 vs 7.2 days per year; P = .0044).31 Absence days in the present study were considerably higher than those reported by Kleinman et al,31 and there was no significant difference between the ADHD and non-ADHD control groups (> 20 days in each group). This difference between the studies was probably due to the definition of absences. While Kleinman et al31 used only health-related absences, the present study grouped all absences (including paid holidays, vacations, and sick leave) because some employers in the database did not differentiate between the different types of absence. Absences specifically due to ill health were captured in the short-term disability data in the present study, which indicated significantly more (approximately 50%) days of lost productivity for employees with ADHD than among those without the disorder, which is consistent with the absence data reported by Kleinman et al.31
Data from 2000 indicated the total economic burden of depression in the United States to be more than $83 billion, with 43.6% of this due to absenteeism, 18.4% to presenteeism, and 12.5% to pharmaceutical costs.32 It is not possible to directly compare these cost estimates with the costs reported in the present analysis, which were based on a subset of all individuals with depression in the MarketScan databases (selected on the basis of matched characteristics with individuals with ADHD). Nevertheless, it is interesting to note the broad similarity between the economic burden associated with depression in the present study with the estimates of between $4,590 and $10,516 based on national data.
In the present study, the total mean annual cost burden (calculated as the sum of direct and indirect costs) was approximately 37% higher for individuals with depression than for those with ADHD. It should be noted that there was a larger difference for direct costs (depression costs were 44% higher than ADHD costs) than for indirect costs (depression costs were 29% higher than ADHD costs). As indirect and direct costs did not contribute equally to the difference in total costs between the ADHD and depression groups, it is important that both direct and indirect costs are considered when assessing the total economic burden of these disorders. Furthermore, indirect costs accounted for a slightly higher proportion of total costs for individuals with ADHD (50%) than for those with depression (47%), suggesting that it is particularly important to include indirect costs when assessing the total cost of ADHD.
One of the strengths of the present study was the reduction in bias in individual selection. In many ADHD studies, individuals are commonly referred from tertiary referral centers.12 Inclusion of these individuals may introduce bias, as they may be more difficult to treat. Individuals in the present study were not clinically referred but were drawn from a population with access to employer-sponsored health insurance and may therefore be more representative of the larger population overall, and certainly more representative of the working population. Interestingly, the male:female ratio in the present study was almost 1:1, while previous research based on clinical data11 has shown that adult ADHD is significantly more prevalent among men than women. It is not possible to determine whether the high proportion of women in the present study is due to the help seeking or recognition bias, which has been reported previously.11,33
Limitations
It is important to note that the present study has a number of limitations. First, the severity of the symptoms of ADHD, and the personal and social impairments that they cause, varies among individuals.34 The degree to which symptom severity impacted the variables examined in the present study was not examined, so this may have confounded our results. Second, although workplace absences were recorded in this study, costs incurred as a result of underperformance at work (presenteeism) due to ADHD were not measured. Previous research has shown that underperformance at work led to more days of lost productivity than workplace absences in adults with ADHD (21.6 days/year vs 13.6 days/year),13 so productivity losses reported here are probably underestimates. Third, ADHD is associated with decreased occupational stability and job termination,34,35 and only 34% of adults with ADHD were employed versus 59% of adults without ADHD in 1 study (P < .001).14 Adults with ADHD were included in the present study because either they or a family member had employer-sponsored health insurance. Employment data for the individuals who were included because a family member had insurance (> 60% of the total number of individuals with ADHD) were not recorded, so it is not possible to calculate the proportion of individuals in the database who were employed or unemployed. To generalize our findings to the larger population of adults with ADHD, studies of unemployed adults with ADHD using the variables in this study are needed. Until then, the findings presented here may not be reliably extrapolated to the population of adults with ADHD.
Fourth, employment termination rates have been shown to be significantly higher among adults with ADHD than among those without the disorder (9.0% vs 5.3% in a 12- to 18-month period; P = .0003).31 Individuals in the present study were required to have continuous enrollment in an employer-sponsored health plan throughout 2006, so many individuals whose employment was terminated during the study period would have been excluded from the analysis. Fifth, individuals who sought medical attention for ADHD may have been more likely to be diagnosed with or treated for another medical condition compared with individuals who did not seek medical attention, thus introducing a selection bias. Sixth, the geographic distribution of individuals in the MarketScan database was not identical to national census data. Although this means that the database was not completely representative of the general population, the large sample size and broad geographical coverage are still important characteristics of the database.
Seventh, previous research has indicated that parents of children with ADHD have significantly increased health benefit costs, health-related absence days, and employment termination rates compared with parents whose children are not affected by the disorder.31 The present study included employees and their dependents with access to employer-sponsored health plans but did not include children or attempt to distinguish between parents with children affected by ADHD and those whose children did not have ADHD. Finally, the inclusion criterion on employment is likely to contribute to an underestimate of the true economic burden of ADHD.
CONCLUSIONS
This large-scale study provides further information on the clinical and economic burden of ADHD in adults and shows that individuals with ADHD have more comorbidities, greater health care utilization, and greater health care expenditures than those without ADHD. This study also shows that adults with ADHD had fewer comorbidities and reduced health care utilization and expenditures compared with adults with depression. However, indirect costs accounted for a slightly higher proportion of total costs for adults with ADHD than for those with depression, suggesting that ADHD has a particularly significant impact in the workplace. Given the potentially large incremental costs and clinical burden associated with ADHD, the findings in this study have significant implications for insurers and policy decision makers who must make cost-effective choices for health plan enrollees.
Drug names: atomoxetine (Strattera), methylphenidate (Focalin, Daytrana, and others).
Author affiliations: Global Health Economics and Outcomes Research, Shire Development Inc, Wayne, Pennsylvania (Drs Hodgkins and Sasané); and Thomson Reuters, Cambridge, Massachusetts (Ms Montejano and Mr Huse). Dr Sasané is now an employee of Bayer.
Potential conflicts of interest: Dr Hodgkins is an employee of and stock shareholder in Shire. Dr Sasané was an employee of and stock shareholder in Shire at the time of the study. Ms Montejano and Mr Huse are employees of Thomson Reuters.
Funding/support: This study was conducted by Thomson Reuters (Healthcare) Inc (Cambridge, Massachusetts) and funded by Shire Development Inc (Wayne, Pennsylvania).
Disclaimer: MarketScan is a registered trademark of Thomson Reuters (Healthcare) Inc.
Previous presentation: Parts of this analysis were presented at the American Psychiatric Association 162nd Annual Meeting; May 16–21, 2009; San Francisco, California (Abstract NR6-095).
Acknowledgment: The authors would like to acknowledge the writing assistance of Andy Brown, PhD (PAREXEL, Worthing, West Sussex, United Kingdom). Financial support for this assistance was provided by Shire Development Inc. Dr Brown reports no financial or other affiliations related to the subject of this article.
REFERENCES
1. Harpin VA. The effect of ADHD on the life of an individual, their family, and community from preschool to adult life. Arch Dis Child. 2005;90(suppl 1):i2–i7. doi:10.1136/adc.2004.059006 PubMed
2. Wood DR, Reimherr FW, Wender PH, et al. Diagnosis and treatment of minimal brain dysfunction in adults: a preliminary report. Arch Gen Psychiatry. 1976;33(12):1453–1460. PubMed
3. Wender PH, Reimherr FW, Wood DR. Attention deficit disorder (‘minimal brain dysfunction’) in adults: a replication study of diagnosis and drug treatment. Arch Gen Psychiatry. 1981;38(4):449–456. PubMed
4. Biederman J, Faraone SV, Spencer T, et al. Patterns of psychiatric comorbidity, cognition, and psychosocial functioning in adults with attention deficit hyperactivity disorder. Am J Psychiatry. 1993;150(12):1792–1798. PubMed
5. Biederman J, Faraone SV, Spencer T, et al. Gender differences in a sample of adults with attention deficit hyperactivity disorder. Psychiatry Res. 1994;53(1):13–29. doi:10.1016/0165-1781(94)90092-2 PubMed
6. Hammerness P, Surman C, Miller K. Update on adult attention-deficit/hyperactivity disorder. Curr Neurol Neurosci Rep. 2008;8(6):484–489. doi:10.1007/s11910-008-0077-z PubMed
7. Mannuzza S, Klein RG, Bessler A, et al. Adult psychiatric status of hyperactive boys grown up. Am J Psychiatry. 1998;155(4):493–498. PubMed
8. Banaschewski T, Coghill D, Santosh P, et al. Long-acting medications for the hyperkinetic disorders: a systematic review and European treatment guideline. Eur Child Adolesc Psychiatry. 2006;15(8):476–495. doi:10.1007/s00787-006-0549-0 PubMed
9. Asherson P. Clinical assessment and treatment of attention deficit hyperactivity disorder in adults. Expert Rev Neurother. 2005;5(4):525–539. doi:10.1586/14737175.5.4.525 PubMed
10. National Institute for Health and Clinical Excellence. Attention deficit hyperactivity disorder: diagnosis and management of ADHD in children, young people and adults. Clinical guideline 72. http://www.nice.org.uk/nicemedia/pdf/ADHDFullGuideline.pdf. Accessed February 7, 2011.
11. Kessler RC, Adler L, Barkley R, et al. The prevalence and correlates of adult ADHD in the United States: results from the National Comorbidity Survey Replication. Am J Psychiatry. 2006;163(4):716–723. doi:10.1176/appi.ajp.163.4.716 PubMed
12. Simon V, Czobor P, Bálint S, et al. Prevalence and correlates of adult attention-deficit hyperactivity disorder: meta-analysis. Br J Psychiatry. 2009;194(3):204–211. doi:10.1192/bjp.bp.107.048827 PubMed
13. Kessler RC, Adler L, Ames M, et al. The prevalence and effects of adult attention deficit/hyperactivity disorder on work performance in a nationally representative sample of workers. J Occup Environ Med. 2005;47(6):565–572. doi:10.1097/01.jom.0000166863.33541.39 PubMed
14. Biederman J, Faraone SV. The effects of attention-deficit/hyperactivity disorder on employment and household income. MedGenMed. 2006;8(3):12. PubMed
15. American Lung Association. Asthma in adults fact sheet. http://www.lungusa.org/lung-disease/asthma/resources/facts-and-figures/asthma-in-adults.html. Accessed February 7, 2011.
16. Secnik K, Swensen A, Lage MJ. Comorbidities and costs of adult patients diagnosed with attention-deficit hyperactivity disorder. Pharmacoeconomics. 2005;23(1):93–102. doi:10.2165/00019053-200523010-00008 PubMed
17. de Graaf R, Kessler RC, Fayyad J, et al. The prevalence and effects of adult attention-deficit/hyperactivity disorder (ADHD) on the performance of workers: results from the WHO World Mental Health Survey Initiative. Occup Environ Med. 2008;65(12):835–842. doi:10.1136/oem.2007.038448 PubMed
18. Birnbaum HG, Kessler RC, Lowe SW, et al. Costs of attention deficit-hyperactivity disorder (ADHD) in the US: excess costs of persons with ADHD and their family members in 2000. Curr Med Res Opin. 2005;21(2):195–206. doi:10.1185/030079904X20303 PubMed
19. Lerner D, Adler DA, Chang H, et al. Unemployment, job retention, and productivity loss among employees with depression. Psychiatr Serv. 2004;55(12):1371–1378. doi:10.1176/appi.ps.55.12.1371 PubMed
20. Murray CJL, Lopez AD. The Global Burden of Disease. A Comprehensive Assessment of Mortality and Disability From Diseases, Injuries, and Risk Factors in 1990 and Projected to 2020. Boston, MA: Harvard School of Public Health on behalf of World Bank, World Health Organization; 1996. The Global Burden of Disease and Injury Series; vol I.
21. Mandrekar JN, Mandrekar SJ. An Introduction to matching and its application using SAS. http://www2.sas.com/proceedings/sugi29/208-29.pdf. Accessed February 7, 2011.
22. Deyo RA, Cherkin DC, Ciol MA. Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol. 1992;45(6):613–619. doi:10.1016/0895-4356(92)90133-8 PubMed
23. Hawkins K, Wang S, Rupnow MF. Indirect cost burden of migraine in the United States. J Occup Environ Med. 2007;49(4):368–374. doi:10.1097/JOM.0b013e31803b9510 PubMed
24. Lee DW, Ozminkowski RJ, Carls GS, et al. The direct and indirect cost burden of clinically significant and symptomatic uterine fibroids. J Occup Environ Med. 2007;49(5):493–506. doi:10.1097/JOM.0b013e31805f6cf2 PubMed
25. Park R. Estimation with heteroscedastic error terms. Econometrica. 1966;34(4):888. doi:10.2307/1910108
26. Manning WG, Mullahy J. Estimating log models: to transform or not to transform? J Health Econ. 2001;20(4):461–494. doi:10.1016/S0167-6296(01)00086-8 PubMed
27. Owens P, Myers M, Elixhauser A, et al. Care of adults with mental health and substance abuse disorders in US community hospitals, 2004. Agency for Healthcare Research and Quality, Department of Health and Human Services. AHRQ Publication No. 07-0008 (2007). http://www.ahrq.gov. Accessed January 28, 2010.
28. Wigal SB. Efficacy and safety limitations of attention-deficit hyperactivity disorder pharmacotherapy in children and adults. CNS Drugs. 2009;23(suppl 1):21–31. doi:10.2165/00023210-200923000-00004 PubMed
29. Shekim WO, Asarnow RF, Hess E, et al. A clinical and demographic profile of a sample of adults with attention deficit hyperactivity disorder, residual state. Compr Psychiatry. 1990;31(5):416–425. doi:10.1016/0010-440X(90)90026-O PubMed
30. Wu EQ, Birnbaum HG, Zhang HF, et al. Health care costs of adults treated for attention-deficit/hyperactivity disorder who received alternative drug therapies. J Manag Care Pharm. 2007;13(7):561–569. PubMed
31. Kleinman NL, Durkin M, Melkonian A, et al. Incremental employee health benefit costs, absence days, and turnover among employees with ADHD and among employees with children with ADHD. J Occup Environ Med. 2009;51(11):1247–1255. doi:10.1097/JOM.0b013e3181bca68c PubMed
32. Greenberg PE, Kessler RC, Birnbaum HG, et al. The economic burden of depression in the United States: how did it change between 1990 and 2000? J Clin Psychiatry. 2003;64(12):1465–1475. doi:10.4088/JCP.v64n1211 PubMed
33. Arcia E, Conners CK. Gender differences in ADHD? J Dev Behav Pediatr. 1998;19(2):77–83. doi:10.1097/00004703-199804000-00002 PubMed
34. Barkley RA. Major life activity and health outcomes associated with attention-deficit/hyperactivity disorder. J Clin Psychiatry. 2002;63(suppl 12):10–15. PubMed
35. Mannuzza S, Klein RG. Long-term prognosis in attention-deficit/hyperactivity disorder. Child Adolesc Psychiatr Clin N Am. 2000;9(3):711–726. PubMed
Enjoy this premium PDF as part of your membership benefits!

