Death From COVID-19 in a Patient Receiving Clozapine:
Factors Involved and Prevention Strategies to Consider
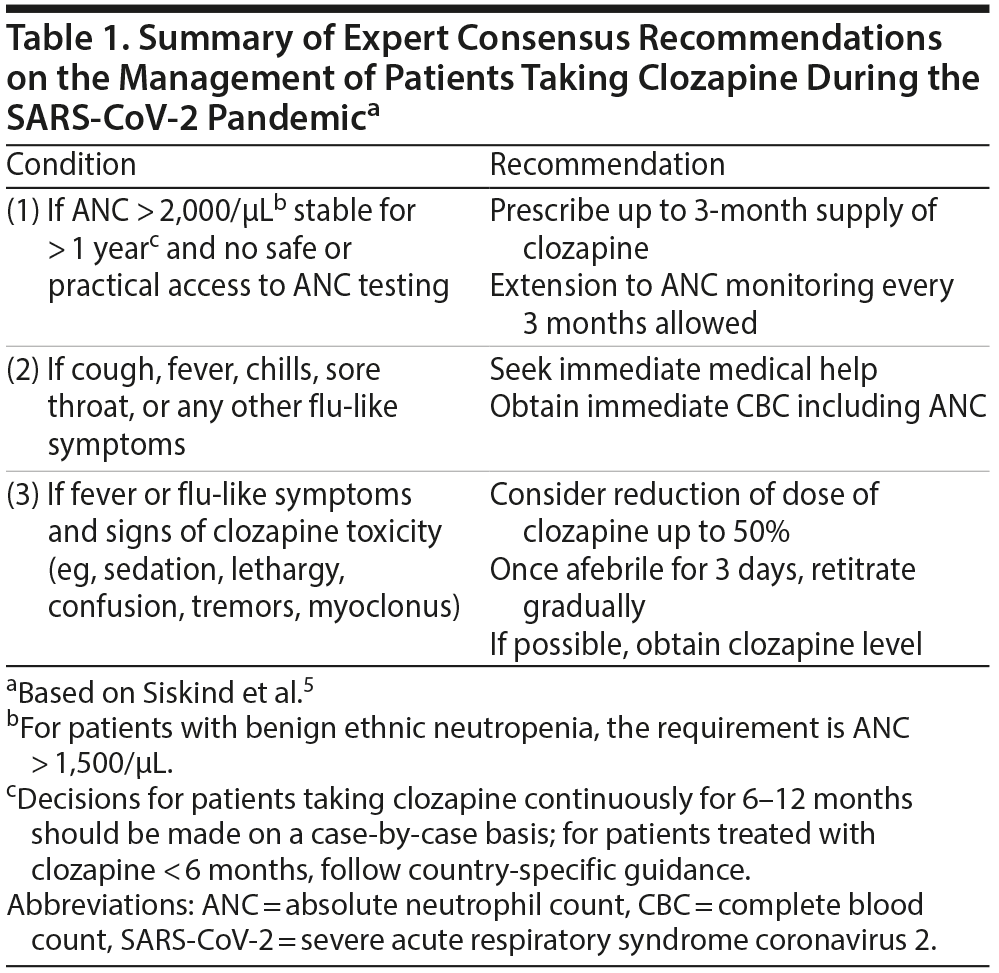
Care of vulnerable patients with severe and persistent mental illness during the current severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) pandemic requires special considerations, particularly for those taking clozapine. Patients with schizophrenia tend to have poor cardiovascular health and difficulty engaging in care and are likely to be active cigarette smokers, which are linked to increased mortality risk from coronavirus disease 2019 (COVID-19).1,2 Patients taking clozapine also have increased incidence of pneumonia most likely due to sialorrhea, immunomodulation properties, and anticholinergic effects.3,4 Moreover, pneumonia appears to be more frequent and to carry higher mortality risk than agranulocytosis or myocarditis in these patients.4 To provide guidance in caring for patients taking clozapine during the COVID-19 pandemic, expert consensus recommendations5 have been published and are summarized in Table 1. Here, we present the case of a patient taking clozapine who died of COVID-19 and discuss the role that psychiatric providers have in reducing mortality risk for these patients.
Case Report
The patient was a 50-year-old domiciled woman with schizophrenia stabilized on clozapine 300 mg and quetiapine 100 mg daily who had a medical history significant for diabetes, obesity, and active cigarette use. She was hospitalized in April 2020 with 2 weeks of fever, cough, and worsening shortness of breath. Her last clozapine level was 296 ng/mL on October 2019 while taking 175 mg daily, and her monthly absolute neutrophil counts were within normal limits. In the emergency department, she was febrile to 101.3° F, in respiratory distress with oxygen saturation of 92%, and had a chest X-ray showing bilateral opacities. Laboratories at admission were notable for positive SARS-CoV-2 polymerase chain reaction, C-reactive protein of 330.4 mg/L, lymphopenia to 900/μL, and hemoglobin A1c of 8%. She was intubated for hypoxic respiratory failure and admitted to the intensive care unit. She developed worsening hypoxemia, vaginal bleeding, and hypotension. On hospital day 6, she had evidence of pulmonary embolus, was started on tissue plasminogen activator with no improvement, and died. Both clozapine and quetiapine were held during the hospitalization.
Discussion
Our case highlights how psychiatric providers have a role in helping monitor patients for COVID-19 symptoms, taking action to engage patients in care when ill and adjusting clozapine prescribing to mitigate risks of COVID-19. Many patients are unaware of the risks of pneumonia, fear isolation from family members or hospitalization after reporting symptoms of COVID-19, and may subsequently underreport symptoms. Importantly, studies6 have found that some medical interventions, when applied early in the course of the disease, could decrease mortality from COVID-19. Our patient developed COVID-19 symptoms 2 weeks prior to admission and did not seek medical treatment during this period. We recommend that clinicians should proactively counsel their patients and caregivers to seek urgent psychiatric and medical evaluation in the presence of fever or flu-like symptoms to rule out clozapine toxicity and to consider further medical interventions. Clinicians should have risk-benefit discussions with their patients taking clozapine, weighing increased risks of pneumonia with the medication’s many clinical benefits.7 Studies8 in schizophrenia show how such discussions can help prevent nonadherence to medications.
Finally, clinicians should be aware that clozapine toxicity may occur during infections due to inhibition of cytochrome P450 1A2 liver enzymes by cytokines.9 Although it is unclear whether toxicity contributed to our patient’s death since clozapine level was not obtained during her illness course, early medical and psychiatric assessment can help mitigate the dangerous combination of pneumonia and clozapine intoxication by adjusting clozapine dose if needed. Of note, the risk of pneumonia is much higher when clozapine is administered with some antipsychotics including quetiapine.3 Therefore, clinicians should also consider the preventive discontinuation of adjunctive antipsychotics. As the SARS-CoV-2 pandemic continues to evolve, clinicians caring for patients taking clozapine have an important role in helping reduce the risks of COVID-19.
Received: May 29, 2020.
Published online: July 23, 2020.
Potential conflicts of interest: None.
Funding/support: None.
Additional information: Information has been de-identified to protect patient anonymity.
REFERENCES
1.CDC COVID-19 Response Team. Preliminary estimates of the prevalence of selected underlying health conditions among patients with coronavirus disease 2019 – United States, February 12-March 28, 2020. MMWR Morb Mortal Wkly Rep. 2020;69(13):382-386. PubMed CrossRef
2.Kozloff N, Mulsant BH, Stergiopoulos V, et al. The COVID-19 global pandemic: implications for people with schizophrenia and related disorders [published online ahead of print April 28, 2020]. Schizophr Bull. PubMed CrossRef
3.Kuo C-J, Yang S-Y, Liao Y-T, et al. Second-generation antipsychotic medications and risk of pneumonia in schizophrenia. Schizophr Bull. 2013;39(3):648-657. PubMed CrossRef
4.de Leon J, Sanz EJ, Norén GN, et al. Pneumonia may be more frequent and have more fatal outcomes with clozapine than with other second-generation antipsychotics. World Psychiatry. 2020;19(1):120-121. PubMed CrossRef
5.Siskind D, Honer WG, Clark S, et al. Consensus statement on the use of clozapine during the COVID-19 pandemic. J Psychiatry Neurosci. 2020;45(4):200061. PubMed
6.Goyal DK, Mansab F, Iqbal A, et al. Early intervention likely improves mortality in COVID-19 infection. Clin Med (Lond). 2020;20(3):248-250. PubMed CrossRef
7.de Leon J, Ruan C-J, Schoretsanitis G, et al. A rational use of clozapine based on adverse drug reactions, pharmacokinetics, and clinical pharmacopsychology [published online ahead of print April 14, 2020]. Psychother Psychosom. PubMed CrossRef
8.Beck E-M, Cavelti M, Wirtz M, et al. How do socio-demographic and clinical factors interact with adherence attitude profiles in schizophrenia? a cluster-analytical approach. Psychiatry Res. 2011;187(1-2):55-61. PubMed CrossRef
9.Clark SR, Warren NS, Kim G, et al. Elevated clozapine levels associated with infection: a systematic review. Schizophr Res. 2018;192:50-56. PubMed CrossRef
aDepartment of Psychiatry, Brightpoint Health, a member of Hudson River Healthcare, Bronx, New York
bDepartment of Psychiatry, NYU Langone Health, New York, New York
*Corresponding author: Joan Roig Llesuy, MD, Department of Psychiatry, Brightpoint Health, a member of Hudson River Healthcare, 459 E 149th St, Bronx, NY 10455 ([email protected]).
Prim Care Companion CNS Disord 2020;22(4):20l02699
To cite: Roig Llesuy J, Sidelnik SA. Death from COVID-19 in a patient receiving clozapine: factors involved and prevention strategies to consider. Prim Care Companion CNS Disord. 2020;22(4):20l02699.
To share: https://doi.org/10.4088/PCC.20l02699
© Copyright 2020 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!