ABSTRACT
Objective: To investigate the prevalence of depression, anxiety, and insomnia among hospital staff working in a tertiary care private hospital in India during the early period of the coronavirus disease 2019 (COVID-19) pandemic.
Methods: This cross-sectional study was conducted May 5–25, 2020, among 347 hospital staff (nursing and other hospital staff, with the exception of doctors). Depression, anxiety, and insomnia were measured using the 9-item Patient Health Questionnaire, the 7-item Generalized Anxiety Disorder Scale, and the Insomnia Severity Index, respectively.
Results: Of respondents, 16.4% reported clinically significant depression, 13.8% reported clinically significant anxiety, and 13.3% reported insomnia. Among the nursing staff, 20.9% reported clinically significant depression, 15.9% reported clinically significant anxiety, and 17.0% reported insomnia. There was significantly higher depression (P = .000), anxiety (P = .002), and insomnia (P = .007) among nursing staff compared with other hospital staff in 2-tailed t tests. There was a significantly higher prevalence of insomnia among females (χ2 = 5.85, df = 2, P = .05).
Conclusions: Study results show that more than 1 in 10 hospital staff suffer from mental health conditions, even during the beginning of the pandemic, and there is a need for active psychiatric support for the hospital staff during this pandemic. Depression, anxiety, and insomnia are significantly higher among nurses compared to other hospital staff. The results of this research suggest that comprehensive support measures should be implemented to protect and maintain mental health of hospital staff, especially nurses, while fighting the COVID-19 pandemic.
Prim Care Companion CNS Disord 2021;23(2):20m02843
To cite: Uvais NA, Nalakath MJ, Jose K. Facing COVID-19: psychological impacts on hospital staff in a tertiary care private hospital in India. Prim Care Companion CNS Disord. 2021;23(2):20m02843.
To share: https://doi.org/10.4088/PCC.20m02843
© Copyright 2021 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Iqraa International Hospital and Research Centre, Calicut, Kerala, India
bDepartment of Hospital Administration, Iqraa International Hospital and Research Centre, Calicut, Kerala, India
cDepartment of Psychiatric Social Work, Thanal, Vadakara, India
*Corresponding author: N. A. Uvais, MBBS, DPM, Iqraa International Hospital and Research Centre, Calicut, Kerala, India ([email protected]).
Coronavirus disease 2019 (COVID-19) emerged in Wuhan, China and was declared a pandemic by the World Health Organization on March 11, 2020.1 The first case of COVID-19 in India was detected in a medical student returning from Wuhan on January 30, 2020. There was a steady increase in the number of cases in India from that point forward. At the time of this writing, India’s COVID-19 cases surpassed 50 million.
The emergence of COVID-19 exerted unprecedented pressure on the Indian health care system. There are multiple reports2–4 from across the world regarding the effects of the COVID-19 pandemic on the mental health of health care workers. Multiple Indian studies5–7 among doctors and nurses dealing with the COVID-19 pandemic also showed significant psychological distress. Moreover, a review and meta-analysis3 of published articles evaluating psychological distress among health care workers also showed that variables like sex, profession, age, place of work, and department of work were associated with increased stress, anxiety, depressive symptoms, and insomnia in health care workers. However, most of the studies used online survey methodology and included mainly doctors and nurses. Moreover, there is no literature, to our knowledge, assessing psychiatric morbidities among health care providers working in the private sector, especially during the early stages of the COVID-19 pandemic. Furthermore, there are no studies evaluating psychiatric distress among different sections of hospital staff such as office workers, pharmacists, and laboratory and other technicians in comparison to frontline health care staff such as nurses or doctors.
In the present study, we analyzed the prevalence of depression, anxiety, and insomnia during the early period of the COVID-19 pandemic among the nursing and other hospital staff, excluding doctors, working in a private hospital setting in the Indian state of Kerala, wherein India’s first case of COVID-19 was detected.
METHODS
The data were collected May 5–25, 2020, and participants were cluster sampled from Iqraa International Hospital and Research Centre, Calicut, Kerala, India. The inclusion criteria were staff, with the exception of doctors, working in the hospital during the time of the study. The participants were asked to complete the self-administered questionnaires. Informed consent was obtained from all the participants. The study was approved by the Ethical Committee of the Iqraa International Hospital and Research Centre.
Sociodemographic data were collected using a semistructured pro forma designed for the study. Sociodemographic data evaluated age, sex, and education. The sociodemographic variables included age, sex, working years, job title, marital status, staying with family, history of exposure to COVID-19, and any history of quarantine.
The 7-item Generalized Anxiety Disorder Scale (GAD-7)8 was used to assess anxiety symptoms. Patients were asked to rate how often they have been bothered by the described symptoms over the last 2 weeks using a 4-point rating scale from 0 (not at all) to 3 (every day). Total scores range from 0 to 21, with higher scores reflecting higher severity levels of generalized anxiety disorder symptomatology. Cutoff points of 5, 10, and 15 are interpreted as representing mild, moderate, and severe levels of anxiety, respectively, on the GAD-7.
Depressive symptoms were measured using the 9-item Patient Health Questionnaire (PHQ-9).9 This questionnaire comprises 9 items with scores between 0 and 27. At a score ≥ 10, the PHQ-9 has a sensitivity and specificity of 88% and a positive likelihood ratio of 7.1 to detect major depressive disorder. For the PHQ‐9, scores of 5 to 9, 10 to 14, 15 to 19, and 20 to 27 corresponded to mild, moderate, moderately severe, and severe depression symptoms, respectively.
The Insomnia Severity Index (ISI)10,11 was used to measure the severity of insomnia. Each item is rated on a 0–4 scale, and the total score ranges from 0 to 28. A higher score suggests more severe insomnia symptoms. A patient with a total score ≥ 8 is considered to have symptoms of insomnia.
Statistical analysis was performed with SPSS version 22.0. Descriptive statistics such as mean, standard deviation (SD), and percentages were calculated. Continuous variables were compared using 2-tailed t tests depending on data distribution. χ2 was used to compare categorical variables. For all tests, values of P ≤ .05 were considered statistically significant.
RESULTS
We received responses from 347 hospital staff. The majority of the respondents were between the ages of 20 and 40 years (93.4%), 82.1% were female, 46.4% had 1–5 years of work experience, and 67.7% were married. By profession, 57.9% were nurses, 13.0% were office staff, 11.0% were laboratory technicians, and 6.9% were pharmacists. Of the respondents, 68.0% were living with their family at the time of the study, 6.9% had a history of exposure to COVID-19, and 7.1% were quarantined before the study. The sociodemographic details are summarized in Table 1.
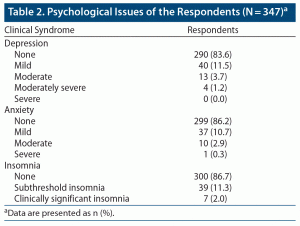
Fifty-seven (16.4%) respondents reported clinically significant depression; 40 respondents reported mild depression, 13 reported moderate depression, and 4 reported moderately severe depression. Forty-eight (13.8%) respondents reported clinically significant anxiety; 37 reported mild anxiety, 10 reported moderate anxiety, and 1 reported severe anxiety. Subthreshold insomnia was reported by 11.3% of respondents, and 2.0% reported clinically significant insomnia. The psychological morbidities of the respondents are summarized in Table 2.
Among the nursing staff, 20.9% reported clinically significant depression, 15.9% reported clinically significant anxiety, and 17.0% reported insomnia.
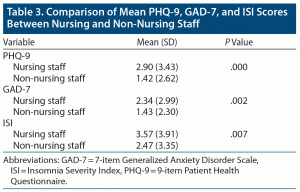
There was a significantly higher prevalence of depression (P = .000), anxiety (P = .002), and insomnia (P = .007) among nursing staff compared with other hospital staff in 2-tailed t tests (Table 3). There was a significantly higher prevalence of insomnia among females (χ2 = 5.85, df = 2, P = .05). There was a significant positive correlation between depression, anxiety, and insomnia scores. There were no other significant associations between depression, anxiety, or insomnia and other sociodemographic variables.
DISCUSSION
This study evaluated the prevalence of depression, anxiety, and insomnia and related factors in hospital staff during the early period of the COVID-19 pandemic in South India. The prevalence rates of depression, anxiety, and insomnia among the hospital staff in the study were 16.4%, 13.8%, and 13.3%, respectively. The prevalence of depression, anxiety, and insomnia in this research was relatively lower compared to similar studies from across the globe.4,12–14 A recent meta-analysis4 explored the prevalence of depression, anxiety, and insomnia among health care workers and found that the pooled prevalence of depression from 10 studies was 22.8%, the pooled prevalence of anxiety from 12 studies was 23.2%, and the pooled prevalence of insomnia from 5 studies was 38.9%. The lower prevalence rates among our respondents could be due to the study being conducted when the COVID-19 pandemic was well controlled and there was no community transmission. Also, the hospital staff was not dealing with COVID-19 patients actively, as all diagnosed cases were shifted to government-designated COVID-19 treatment facilities according to government protocol. Moreover, differences in the study instruments and the mode of study, most of the previous studies were online surveys, might also have influenced the prevalence rate. Similar to past studies, we also found that the majority of the hospital staff experienced mild depressive and anxiety symptoms, while moderate and severe symptoms were less common among the participants.4 However, we found that more than 1 in 10 hospital staff suffered from mental health conditions even during the beginning of the pandemic, and there is a need for active psychiatric support for the hospital staff during this crisis.
We also found that significantly higher rates of depression, anxiety, and insomnia were observed in nurses compared to other hospital staff. Results showed that 20.9% of the nursing staff has clinically significant depression, 15.9% had clinically significant anxiety, and 17.0% had insomnia. Liu et al15 studied the prevalence of anxiety in medical workers fighting COVID-19 in China and found a 12.5% prevalence of anxiety, which is similar to our results. However, another study among frontline nurses in China by Tu et al16 found that 60% had poor sleep quality, 46% had depression symptoms, and 40% reported anxiety symptoms.
Most of the past studies that compared psychiatric morbidity among hospital staff included doctors and nurses only, and the meta-analysis4 of the study results established that nursing staff exhibited higher prevalence estimates both for anxiety and depression compared to doctors. However, our study did not include doctors, and we found that nurses harbor significantly higher psychiatric morbidity when compared to other hospital staff like pharmacists, laboratory technicians, office staff, or dialysis technicians. Moreover, we found no association of sex with this higher prevalence of anxiety and depression. Liu et al15 also reported that the health worker anxiety did not increase with regard to sex. Most of the other studies consistently found significantly higher prevalence rates of anxiety and depression among women, and some argued that the higher prevalence of psychiatric morbidity among nurses might be due to the confounding sex factor.4 The higher prevalence of psychiatric morbidity among nurses in our study might be due to their apprehensions regarding higher risk of exposure to COVID-19 patients, as they spend more time on the frontline with respect to managing COVID-19 patients.
Studies conducted among hospital staff during previous epidemics also showed significant psychiatric morbidities among these individuals. Lu et al17 studied the mental health of hospital staff dealing with severe acute respiratory syndrome and found that 17.3% of the study participants developed significant psychiatric symptoms. Su et al18 evaluated the prevalence of psychiatric morbidity among nurses during the severe acute respiratory syndrome outbreak and found that 38.5% of nurses had clinically significant depression and 37% had insomnia.
In conclusion, rates of depression, anxiety, and insomnia are significantly higher among nurses compared to other hospital staff. The results of this research suggest that comprehensive support measures should be implemented to protect and maintain the mental health of hospital staff, especially nurses, while fighting the COVID-19 pandemic.
Submitted: October 17, 2020; accepted December 11, 2020.
Published online: March 25, 2021.
Potential conflicts of interest: None.
Funding/support: None.
Clinical Points
- Rates of depression, anxiety, and insomnia are significantly higher among nurses compared to other hospital staff.
- Comprehensive support measures should be implemented to protect and maintain the mental health of hospital staff, especially nurses, during the COVID-19 pandemic.
References (18)

- Roy D, Tripathy S, Kar SK, et al. Study of knowledge, attitude, anxiety & perceived mental healthcare need in Indian population during COVID-19 pandemic. Asian J Psychiatr. 2020;51:102083. PubMed CrossRef NLM
- Gupta AK, Mehra A, Niraula A, et al. Prevalence of anxiety and depression among the healthcare workers in Nepal during the COVID-19 pandemic. Asian J Psychiatr. 2020;54:102260. PubMed CrossRef NLM
- Spoorthy MS, Pratapa SK, Mahant S. Mental health problems faced by healthcare workers due to the COVID-19 pandemic—a review. Asian J Psychiatr. 2020;51:102119. PubMed CrossRef NLM
- Pappa S, Ntella V, Giannakas T, et al. Prevalence of depression, anxiety, and insomnia among healthcare workers during the COVID-19 pandemic: a systematic review and meta-analysis. Brain Behav Immun. 2020;88:901–907. PubMed CrossRef NLM
- Wilson W, Raj JP, Rao S, et al. Prevalence and predictors of stress, anxiety, and depression among healthcare workers managing COVID-19 pandemic in India: a nationwide observational study. Indian J Psychol Med. 2020;42(4):353–358. CrossRef
- Uvais NA, Shihabudheen P, Hafi NAB. Perceived stress and stigma among doctors working in COVID-19-designated hospitals in India. Prim Care Companion CNS Disord. 2020;22(4):20br02724. PubMed CrossRef NLM
- Uvais NA, Aziz F, Hafeeq B. COVID-19-related stigma and perceived stress among dialysis staff. J Nephrol. 2020;33(6):1121–1122. PubMed CrossRef NLM
- Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16(9):606–613. PubMed CrossRef NLM
- Spitzer RL, Kroenke K, Williams JB, et al. A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med. 2006;166(10):1092–1097. PubMed CrossRef NLM
- Bastien CH, Vallières A, Morin CM. Validation of the Insomnia Severity Index as an outcome measure for insomnia research. Sleep Med. 2001;2(4):297–307. PubMed CrossRef NLM
- Morin CM, Belleville G, Bélanger L, et al. The Insomnia Severity Index: psychometric indicators to detect insomnia cases and evaluate treatment response. Sleep. 2011;34(5):601–608. PubMed CrossRef NLM
- Şahin MK, Aker S, Şahin G, et al. Prevalence of depression, anxiety, distress and insomnia and related factors in healthcare workers during COVID-19 pandemic in Turkey. J Community Health. 2020;45(6):1168–1177. PubMed NLM
- Lai J, Ma S, Wang Y, et al. Factors associated with mental health outcomes among health care workers exposed to coronavirus disease 2019. JAMA Netw Open. 2020;3(3):e203976. PubMed CrossRef NLM
- Zhang C, Yang L, Liu S, et al. Survey of insomnia and related social psychological factors among medical staff involved in the 2019 novel coronavirus disease outbreak. Front Psychiatry. 2020;11:306. PubMed CrossRef NLM
- Liu CY, Yang YZ, Zhang XM, et al. The prevalence and influencing factors in anxiety in medical workers fighting COVID-19 in China: a cross-sectional survey. Epidemiol Infect. 2020;148:e98. PubMed CrossRef NLM
- Tu ZH, He JW, Zhou N. Sleep quality and mood symptoms in conscripted frontline nurse in Wuhan, China during COVID-19 outbreak: a cross-sectional study. Medicine (Baltimore). 2020;99(26):e20769. PubMed CrossRef NLM
- Lu YC, Shu BC, Chang YY, et al. The mental health of hospital workers dealing with severe acute respiratory syndrome. Psychother Psychosom. 2006;75(6):370–375. PubMed CrossRef NLM
- Su TP, Lien TC, Yang CY, et al. Prevalence of psychiatric morbidity and psychological adaptation of the nurses in a structured SARS caring unit during outbreak: a prospective and periodic assessment study in Taiwan. J Psychiatr Res. 2007;41(1–2):119–130. PubMed CrossRef NLM
Enjoy this premium PDF as part of your membership benefits!