ABSTRACT
Objective: Coronavirus disease 2019 (COVID-19) vaccination uptake among individuals with severe mental illness (SMI) is a public health challenge due to various individual level as well as systemic level barriers. The objective of this study was to explore COVID-19 vaccination status among community-dwelling patients with SMI and identify associated factors.
Methods: A cross-sectional study was conducted among patients with SMI attending community psychiatry clinics in Northern Kerala from April 21, 2021, to August 3, 2021, using a structured questionnaire. Sociodemographic information and COVID-19–related information, including vaccination status and agreement with COVID-19 vaccination–related statements, were obtained.
Results: Of the 62 respondents, only 27.9% received COVID-19 vaccination. Also, 59.7% of respondents received a recommendation for vaccination from their health care providers. The mean age of the vaccinated group was significantly higher than that of the unvaccinated group (F = 1.3359, P < .001). The rate of vaccination uptake among respondents who were contacted by their health care provider for COVID-19 vaccination was significantly higher (P = .001). Respondents in the vaccinated group perceived the vaccine to be more effective in preventing COVID-19 infection than those in the unvaccinated group (2.06 vs 2.64, P = .031). Also, vaccinated respondents were less in agreement regarding the statement about the risk of COVID-19 vaccine worsening mental illness (4.18 vs 3.67, P = .049). Age and recommendation for vaccination from health care providers were found to be significant predictors of COVID-19 vaccination uptake.
Conclusions: On the basis of the study findings, it is recommended that tailored educational activities regarding the safety and efficacy of the COVID-19 vaccine along with recommendation by health care providers can significantly improve COVID-19 vaccination uptake among patients with SMI.
Prim Care Companion CNS Disord 2022;24(3):21m03227
To cite: Uvais NA. Factors associated with COVID-19 vaccination uptake among community-dwelling patients with severe mental illness: a cross-sectional study. Prim Care Companion CNS Disord. 2022;24(3):21m03227.
To share: https://doi.org/10.4088/PCC.21m03227
© Copyright 2022 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Iqraa International Hospital and Research Centre, Calicut, Kerala, India
*Corresponding author: N. A. Uvais, MBBS, DPM, Iqraa International Hospital and Research Centre, Malaparamba, Calicut, Kerala 673009, India ([email protected]).
Individuals with severe mental illness (SMI) are at an increased risk for coronavirus disease 2019 (COVID)–related morbidity and mortality compared to the general population due to multiple biological and psychosocial factors.1,2 A recent systematic review and meta-analysis3 exploring the association between psychiatric disorders and mortality in 7 countries found that patients with SMI had the highest odds ratios for mortality from COVID-19. Considering these vulnerabilities, many countries prioritized individuals with SMI for COVID-19 vaccination, which is the only available option at present to reduce the severity of COVID-19 infection.1 However, vaccination uptake among individuals with SMI is a public health challenge due to various individual level as well as systemic level barriers, such as lack of knowledge and awareness, accessibility problems, costs, fears about immunization, and lack of priority given by health care workers.4 Despite our understanding of vaccine hesitancy among individuals with SMI from previous pandemics, there are only a few studies exploring vaccination rates and associated factors among individuals with SMI.5,6 At the time of this writing, to the best of my knowledge, there are no studies exploring COVID-19 vaccination status and influencing factors among community-dwelling individuals with SMI from India. The current study is a preliminary attempt to explore COVID-19 vaccine uptake and associated factors among community-dwelling Indian patients with SMI.
METHODS
A cross-sectional study was conducted to investigate COVID-19 vaccination status and assess factors associated with COVID-19 vaccination decisions among patients with mental illness. The study protocol was approved by the institutional research ethics committee. Purposive sampling technique was utilized to recruit participants. Patients with severe mental illness, > 18 years of age, attending community psychiatric clinics in Northern Kerala, India, from April 21, 2021, to August 3, 2021, were contacted for the study. Only those patients who were willing to give consent were interviewed using a structured questionnaire, which contains 2 sections. The first section was created to obtain patients’ demographic information including age, sex, marital status, psychiatric diagnosis, employment, and education level. The second part was created to obtain COVID-19–related information and COVID-19 vaccination status, as well as respondent agreements with COVID-19 vaccination–related statements. The COVID-19–related information includes history of COVID-19 infection in self or any family member, health care provider recommendation for the COVID-19 vaccine, and COVID-19 vaccination status. The questionnaire asked the respondents to select their plan to receive COVID-19 vaccination from 3 options: they were uncertain about their plan to take COVID-19 vaccination, they were planning to get COVID-19 vaccination, and they have already received COVID-19 vaccination. The questionnaire also asked respondents to rate the level of their agreement/disagreement with 5 statements: (1) the COVID-19 vaccine is effective at preventing the COVID-19 infection, (2) I can get the COVID-19 infection from the COVID-19 vaccine, (3) COVID-19 vaccines can cause mental illness, (4) it is harmful to take COVID-19 vaccination while taking medications for mental illness, and (5) COVID-19 vaccines can worsen mental illness. The response categories ranged from strongly agree (1) to strongly disagree (5).
Data were analyzed using SPSS Statistics version 20. The respondents’ sociodemographic and clinical characteristics were described by descriptive statistics. Categorical data were compared using χ2 test, and continuous data were compared using independent t tests. A binary logistic regression was done to determine factors associated with vaccination status. All statistical analyses were based on a significance level of .05.
RESULTS
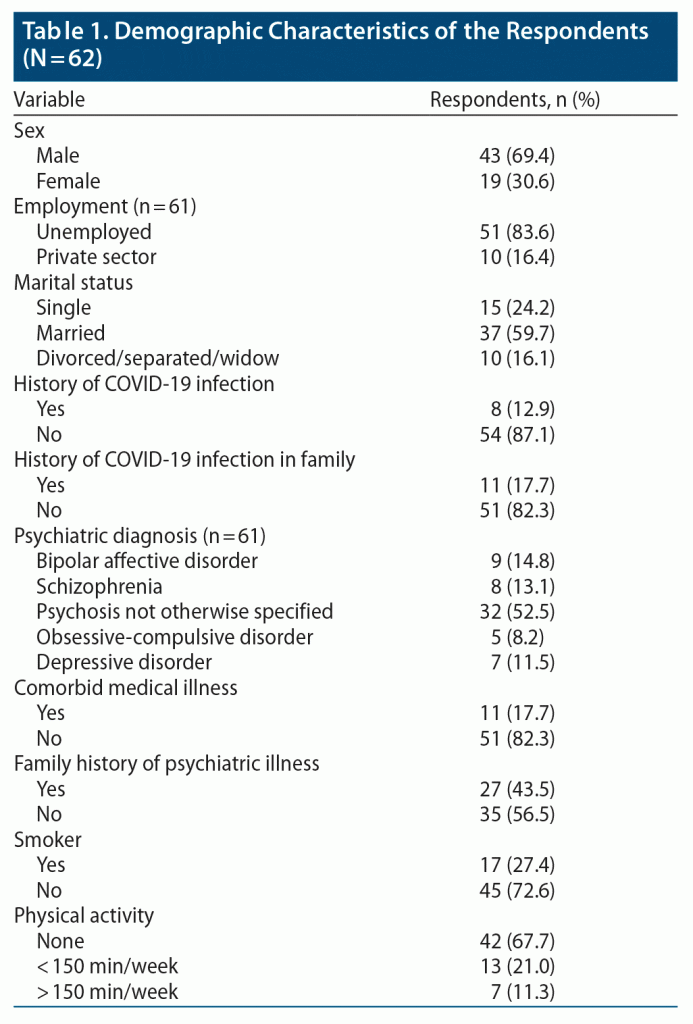
Sixty-two patients with SMI attending 7 community psychiatry clinics in Northern Kerala participated in the study. Forty-three (69.4%) of the participants were male, and 59.7% of the respondents were married. The majority had a high school level or lesser educational attainment and were unemployed (83.6%). Only 12.9% of the respondents had a history of COVID-19 infection, and 17.7% had a family history of COVID-19 infection. The most common psychiatric diagnosis was psychosis not otherwise specified (52.5%), followed by bipolar affective disorder (14.8%) and schizophrenia (13.1%). Also, 17.7% of the respondents had comorbid medical illnesses, 43.5% had a family history of psychiatric illness, 27.4% were smokers, and 67.7% were not engaged in any physical activity. Table 1 summarizes the demographic characteristics of the respondents. Only 17 (27.9%) of the respondents received the first dose of COVID-19 vaccination, and 59.7% were recommended for vaccination from a health care provider. The characteristics of the respondents specific to COVID-19 vaccination are summarized in Table 2.
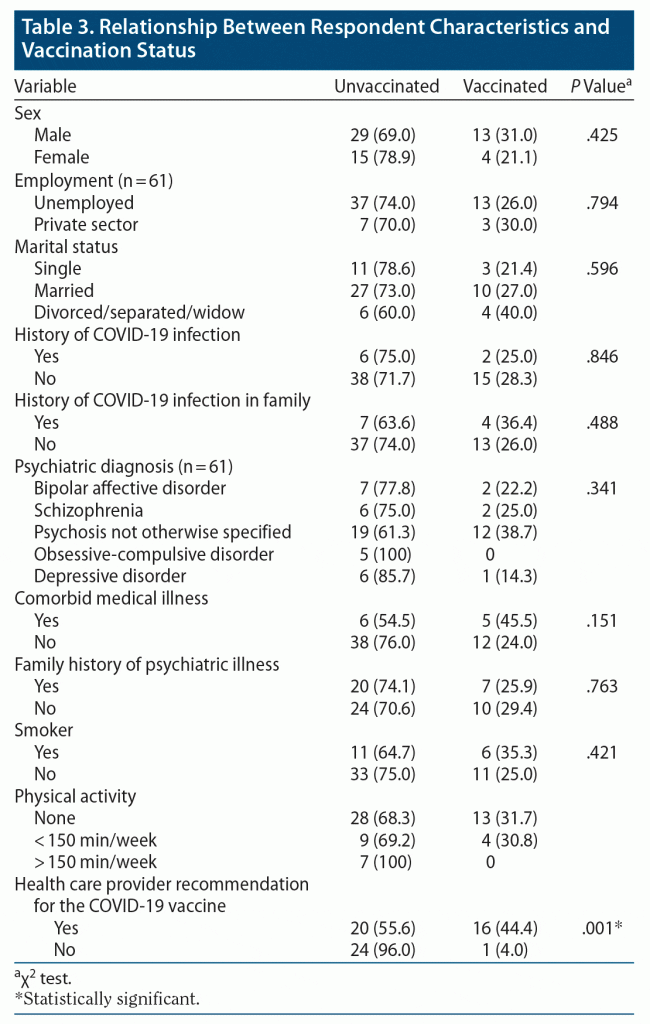
Two characteristics differed between the unvaccinated (n = 44) and vaccinated (n = 17) groups: age and health care provider recommendation for the COVID-19 vaccine. The χ2 test results are summarized in Table 3. The mean age in the unvaccinated group was 40.66 years (SD = 9.88), while the mean age for the vaccinated group was 53.52 years (SD = 12.35); the difference was statistically significant (F = 1.3359, P < .001). Among the respondents who were contacted by their health care provider for COVID-19 vaccination, 55.6% received vaccination, whereas among those respondents who were not contacted by a health care provider for COVID-19 vaccination, 96% did not receive vaccination at the time of the study. The difference was statistically significant (P = .001).
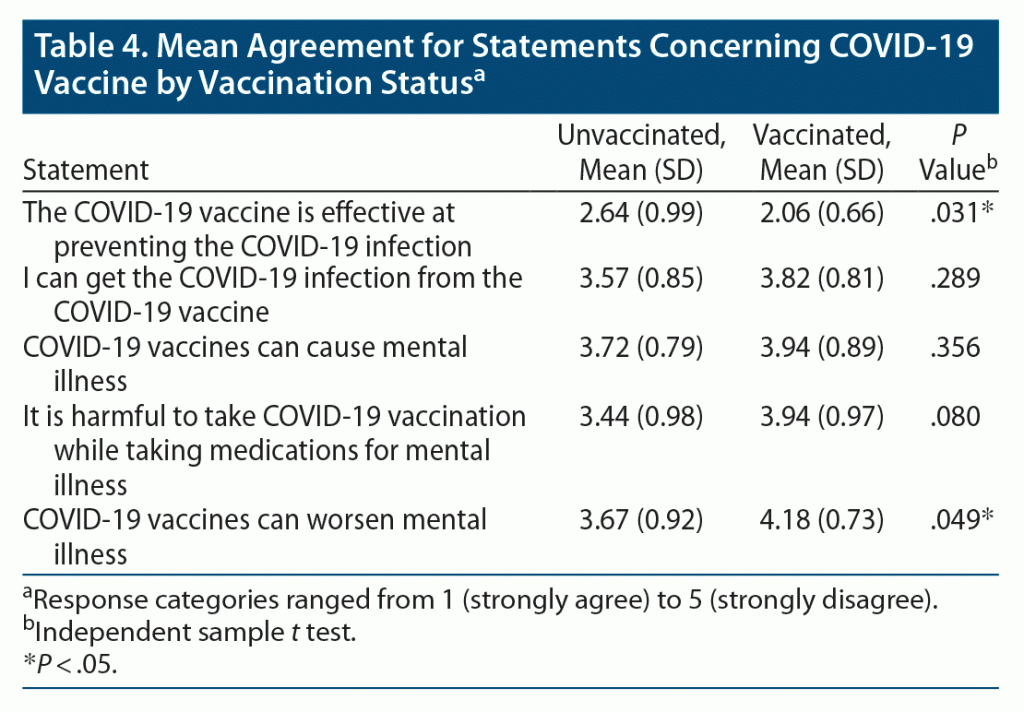
Unvaccinated and vaccinated groups also differed in their perceptions concerning the COVID-19 vaccine and its effects on mental health. Five statements were given to the respondents to rate the level of disagreement/agreement. The score for each item ranged between 1 (strongly agree) and 5 (strongly disagree), while 3 was neutral. Specifically, respondents in the vaccinated group perceived the vaccine to be more effective in preventing COVID-19 infection than those in the unvaccinated group (2.06 vs 2.64, P = .031). Also, vaccinated respondents were less in agreement with the statement about the risk of COVID-19 vaccine worsening mental illness (4.18 vs 3.67, P = .049). Regarding the other 3 statements, respondents in both groups tended to disagree, as the score was > 3. The mean agreement for statements concerning COVID-19 vaccine by vaccination status are summarized in Table 4. A binary logistic regression analysis was also conducted to identify factors associated with respondents’ vaccination status and showed that only age and recommendation for vaccination from health care providers were significant factors associated with vaccination status.
DISCUSSION
This study explored the COVID-19 vaccination rate and associated factors among community-dwelling individuals with SMI. The major finding of this study was that the recommendation of COVID-19 vaccination by health care provider was a significant modifiable factor influencing COVID-19 vaccination status among individuals with SMI, which is consistent with previous published literature. Lorenz et al7 studied influenza vaccination decisions among patients with mental illness and found that participants who received recommendation for vaccination from their health care provider were 4 times more likely to accept vaccination compared to others who did not receive such a recommendation. The study result highlights the relevance of involving regular health care providers to improve the COVID-19 vaccination rate among individuals with SMI from a public health perspective. The treating mental health team should recommend COVID-19 vaccination to their patients and should set up vaccination clinics in community psychiatry clinics with the help of public health departments, if possible, to improve vaccination rates among this vulnerable population.
Also, only 27.9% of the respondents were vaccinated at the time of the present study. The rate of COVID-19 vaccination among the studied population is significantly lower than that of the population of Kerala state during the study period.8 Further, the vaccination rate found in this study was significantly lower than the rate among individuals with mental illness staying in residential and community care in Belgium (91.7%), which is comparable to the rate of COVID-19 vaccine uptake in the general population.5 However, another study6 from Israel showed that people with schizophrenia have lower rates of vaccination uptake than the general population. The reduced rate of preventive vaccinations among individuals with SMI is well documented for illnesses such as influenza and pneumonia due to individual and systemic factors.9 This study finding indicates that there is a need to plan targeted public health interventions to increase COVID-19 vaccination rates among community-dwelling patients with SMI.
This study also found that belief in the effectiveness of the vaccine in preventing COVID-19 infection and safety of the vaccine in patients with mental illness significantly influenced vaccine uptake. Educating patients regarding the effectiveness and safety of the COVID-19 vaccine could be an effective public health strategy in improving vaccination uptake among patients with SMI.
CONCLUSION
This study found significantly lower COVID-19 vaccination uptake and associated factors among patients with SMI. It is recommended that educational activities regarding the safety and efficacy of the COVID-19 vaccine along with recommendation by health care providers can significantly improve COVID-19 vaccination uptake among patients with SMI.
Submitted: December 23, 2021; accepted March 11, 2022.
Published online: May 26, 2022.
Relevant financial relationships: None.
Funding/support: None.
Clinical Points
- Studies exploring COVID-19 vaccination rates and associated factors among individuals with severe mental illness (SMI) are limited.
- The rate of COVID-19 vaccination among individuals with SMI was significantly lower compared to that of the general population.
- Medical provider recommendation for COVID-19 vaccination is a modifiable factor that increases vaccination in those with SMI.
References (9)

- Varshney P, Mamtani H, Kumar CN, et al. COVID-19 vaccination for persons with severe mental illnesses: an Indian perspective. Indian J Psychol Med. 2021;43(5):436–441. PubMed CrossRef
- Uvais NA. COVID-19 vaccine hesitancy among patients with psychiatric disorders. Prim Care Companion CNS Disord. 2021;23(6):21br03028. PubMed CrossRef
- Fond G, Nemani K, Etchecopar-Etchart D, et al. Association between mental health disorders and mortality among patients with COVID-19 in 7 countries: a systematic review and meta-analysis. JAMA Psychiatry. 2021;78(11):1208–1217. PubMed CrossRef
- Mazereel V, Van Assche K, Detraux J, et al. COVID-19 vaccination for people with severe mental illness: why, what, and how? Lancet Psychiatry. 2021;8(5):444–450. PubMed CrossRef
- Mazereel V, Vanbrabant T, Desplenter F, et al. COVID-19 vaccination rates in a cohort study of patients with mental illness in residential and community care. Front Psychiatry. 2021;12:805528. PubMed CrossRef
- Tzur Bitan D, Kridin K, Cohen AD, et al. COVID-19 hospitalisation, mortality, vaccination, and postvaccination trends among people with schizophrenia in Israel: a longitudinal cohort study. Lancet Psychiatry. 2021;8(10):901–908. PubMed CrossRef
- Lorenz RA, Norris MM, Norton LC, et al. Factors associated with influenza vaccination decisions among patients with mental illness. Int J Psychiatry Med. 2013;46(1):1–13. PubMed CrossRef
- Unnithan PSG. Kerala vaccinates over 50% population with first dose of Covid-19 vaccine: Health Minister. India Today website. Accessed August 17, 2021. https://www.indiatoday.in/india/story/kerala-vaccinates-50-percent-population-with-first-dose-of-covid-vaccine-says-health-minister-1841788-2021-08-17
- Lord O, Malone D, Mitchell AJ. Receipt of preventive medical care and medical screening for patients with mental illness: a comparative analysis. Gen Hosp Psychiatry. 2010;32(5):519–543. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!