ABSTRACT
Despite several reports of the neuropsychiatric effects of coronavirus disease 2019 (COVID-19) in older adults, only a few cases of COVID-related psychosis have been reported in young patients. This case-based review compares the clinical presentations of 2 previously published cases of adolescent patients who developed psychosis in the context of COVID-related complications with a new case of a male adolescent who developed post-COVID psychosis. A discussion to raise clinicians’ awareness of COVID-related psychosis in young patients as well as the need for cautious use of antipsychotic medications in this highly vulnerable age group is also provided.
Prim Care Companion CNS Disord 2021;23(6):21nr03107
To cite: Javed S, Shad MU. COVID-related psychosis in adolescents: a case-based review. Prim Care Companion CNS Disord. 2021;23(6):21nr03107.
To share: https://doi.org/10.4088/PCC.21nr03107
© Copyright 2021 Physicians Postgraduate Press, Inc.
aNishtar Medical University, Multan, Pakistan
bUniversity of Nevada, Las Vegas, Nevada
cTouro University Nevada College of Osteopathic Medicine, Las Vegas, Nevada
dPsychiatry Residency Program, Valley Health System, Las Vegas, Nevada
*Corresponding author: Mujeeb U. Shad, MD, MSCS, Psychiatry Residency Program, Valley Health System, 5400 South Rainbow Blvd, Las Vegas, Nevada 89118 ([email protected]).
The unrestrained spread of the new coronavirus severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), which causes coronavirus disease 2019 (COVID-19), was an unanticipated and significant threat to the world, influencing every realm of society. Most countries shut down, allowing only essential activities and public interactions to control the spread and escalation of the infection.1 Even young individuals not directly infected with COVID-19 were negatively affected during the pandemic due to psychosocial stress from strict social distancing, family financial stress, fear of getting infected, and social isolation from school lockdowns.2 In addition, COVID-related disruptions in daily routines also drastically affected the young population.3 Research has shown children to have increased irritability, increased clinging behavior, inattention,4 poor sleep, poor appetite, agitation, and anxiety.5,6 Although data are lacking in young individuals, studies in older adults have shown that COVID-19 can affect the brain directly or indirectly to result in various neuropsychiatric symptoms.7 However, it is surprising that there are only 4 published cases8–11 of COVID-related psychosis in adolescents, 2 of which are associated with the high level of psychosocial stress and the other 2 cases due to biologically mediated effects of SARS-CoV-2 on a developing brain.
Interestingly, all these cases had different underlying mechanisms for the development of psychosis. Two of the 4 patients8,9 did not have active SARS-CoV-2 infection; however, they still developed psychosis due to COVID-related psychosocial and medical stress. The other 2 patients10,11 had new-onset psychosis during COVID-associated medical complications. However, none of the patients reviewed developed psychosis after a complete recovery from COVID-19 (ie, post-COVID psychosis) with no COVID-associated complications. Of note, post-COVID psychosis has been reported in the adult population after recovering from COVID-19.12,13 Here, we present, to our knowledge, the first report (case 3) of post-COVID psychosis in an adolescent male without prior history of psychiatric symptoms or COVID-associated medical complications. This review compares clinical presentations of the new and the 2 published cases of psychosis secondary to direct infection with SARS-CoV-2 to enhance clinicians’ awareness and to discuss the cautious use of antipsychotic medications in a young and vulnerable population.
METHODS
The current case (case 3) of post-COVID psychosis was discovered after the senior author (M.U.S.) was requested to assess an adolescent patient with new-onset psychosis. A literature search to find any prior instances of post-COVID psychosis in the younger population was conducted using PubMed, CINAHL, PsycINFO, Scopus, and Web of Science with no restrictions. The following search terms were employed for this search: COVID-19 OR SARS-CoV-2 OR coronavirus disease 2019 AND psychosis OR psychotic OR delusion OR hallucinations OR schizophrenia. The search yielded a total of 1,641 articles after deleting 346 duplicates. However, after children and adolescent were added to the search terms, we could find only 2 cases10,11 of psychosis that were directly linked to infection with SARS-CoV-2. The new case was added to the 2 published cases for this review after informed consent was obtained from the patient’s family.
RESULTS
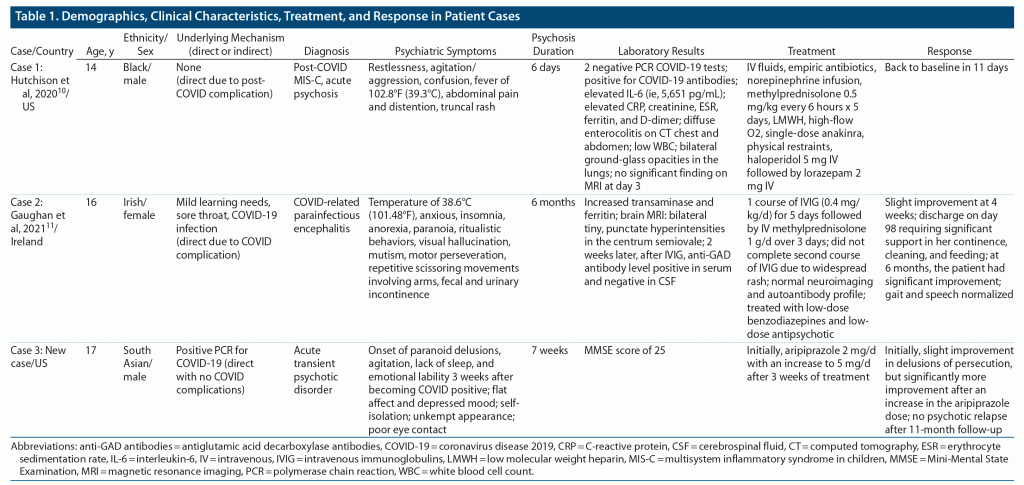
As shown in Table 1, a total of 3 cases were reviewed (1 new and 2 published cases) with 2 female and 3 male adolescents and a mean ± SD age of 15.7 ± 1.5 years. Case 110 was reported in a Black male and case 211 in an Irish female. The new case (case 3) was reported in a South Asian male. Cases 2 and 3 were positive on the PCR (polymerase chain reaction) test for COVID-19, but case 1 was only positive for COVID-19 antibodies. All patients in the reviewed cases received psychiatric and medical treatment, including antipsychotic medications. However, antipsychotic treatment was not effective in case 1, in which the patient only responded to combined treatment with steroids, antibiotics, and intravenous fluids for the post-COVID complication multiple inflammatory syndrome in children (MIS-C). The patient in case 2 was managed with intravenous immunoglobulins, low-dose benzodiazepine, and antipsychotic medication for her COVID-associated complication, which was parainfectious encephalitis. None of the patients had a history of psychiatric illness, except for the patient in case 2 who had a mild learning disorder.
History for Case 3 (new case)
A 17-year-old South Asian male adolescent with no prior psychiatric history presented with bizarre behavior, paranoid delusions, and auditory hallucinations after 3 weeks of testing positive on the PCR test for COVID-19. The patient’s family reported only mild respiratory symptoms and low-grade fever with mild fatigue and tiredness without losing taste or smell. The patient was reported to recover completely within 2 weeks of testing positive with no complications. However, a week later, the patient started to have persecutory symptoms of being followed by someone accompanied by severe agitation, aggression, emotional lability, and lack of sleep. There were no symptoms of racing thoughts, flight of ideas, self-injurious behavior, or goal-directed activities to suggest bipolarity in this patient. Initially, the patient refused to visit a physician but eventually agreed to be seen virtually. On psychiatric consultation, the patient presented with flat affect and a depressed mood with an unkempt appearance and poor eye contact. The urine drug screen was negative, and the patient scored 25 on the Mini-Mental State Examination.14 On mental status examination, the patient was noted to have poor insight with intact memory and orientation. The patient refused to take any medications for his psychosis, but after the family encouraged him to start a low dose of antipsychotic medication, he was started on aripiprazole 2 mg/d. Although the patient showed mild improvement in psychosis and agitated behavior, he continued to have agitation, lack of sleep, decreased appetite, self-isolation, and blunted affect. After 3 weeks, he agreed to increase the aripiprazole dose from 2 mg/d to 5 mg/d, which significantly reduced his psychosis and depressive symptoms within a week.
DISCUSSION
Although this review is based on only 3 cases linked to SARS-CoV-2 infection, the differences in underlying diagnosis, clinical presentation, and treatment of psychosis for each of these cases can be clearly observed (Table 1). The lack of prior psychiatric history in the reviewed cases suggests that psychosis was most likely associated with infection with SARS-CoV-2. Although the COVID-related psychosis in these cases could have been exacerbated by the psychosocial stress from the social isolation and school lockdowns,15 the primary reason for new-onset psychosis was most likely due to the biologically mediated brain effects of SARS-CoV-2 infection. Here, we will attempt to describe various mechanisms underlying COVID-related psychosis in the new and published cases.10,11
As can be seen in Table 1, psychosis in cases 1 and 3 occurred several days after the patients recovered from the COVID-19 symptoms. However, in case 1, psychosis only occurred during the MIS-C, which is a postinfectious inflammatory process recently observed in many instances of SARS-CoV-2 infection.16 The presence of COVID antibodies in case 1 suggests that a past exposure to COVID-19 triggered an inflammatory response to precipitate autoimmune psychosis. Acute psychosis in case 211 was also observed during a severe COVID-19 complication, parainfectious encephalitis. This case resembled the clinical presentation of akinetic mutism, which includes lack of spontaneous movements and loss of speech. This case had the most devastating consequences of all the reviewed cases, with incomplete recovery until the time the case report was submitted.10 At hospital discharge, this patient was recommended for long-term neuropsychiatric follow-up. None of the other patients had such long-lasting neuropsychiatric effects from COVID-19.
Case 3 is the only patient that presented with post-COVID psychosis with no COVID-related complications. The psychosis started after a week of complete medical recovery from 2 weeks of relatively mild COVID-19 symptoms. The patient became extremely paranoid about someone persecuting him, followed by agitation, aggression, emotional lability, and insomnia. We found no other cause for new-onset psychosis, and his urine drug screen was also negative. The presentation was consistent with first-episode psychosis, and had we not known that the patient had tested positive for COVID-19, it would have been a plausible diagnosis; however, the patient did not require any antipsychotic treatment after being discontinued from aripiprazole for 11 months.
The neuropsychiatric symptoms from COVID-19 differ in severity and range from deficits in taste and smell to encephalitis and acute brain dysfunction.17 These symptoms may be mediated by direct or indirect biological effects of SARS-CoV-2 infection. However, there seems to be much more evidence for the indirect than the direct brain effects of the virus. Postmortem brain studies in COVID-19 patients did not find evidence for direct brain effects of the virus.18 The indirect effects are thought to be mediated by the hypoxic injury to a young brain from acute respiratory distress from COVID-19.18 A young developing brain may also be more vulnerable than an adult brain to the other central nervous system effects of COVID-19.3 Increased levels of proinflammatory cytokines; interleukin-6 (IL-6); tumor necrosis factor-α, IL-8, IL-10, and IL-2R; and C-reactive protein (CRP) observed with SARS-Cov-2 infection have been significantly correlated with the severity of COVID-19 symptoms.19,20 An overwhelming increase in proinflammatory cytokines, known as the cytokine storm, has been frequently associated with COVID-related deaths.21–23 Although proinflammatory markers were not assessed in all cases, significant elevations in IL-6 and CRP levels were reported in case 3,10 which correlated with symptom severity. Cytokine-induced neuroinflammation, in turn, may activate autoantibodies, such as autoantibodies against N-methyl-D-aspartate (NMDA) receptors,24 which could be the mechanism underlying psychosis in case 2.8
Finally, we will discuss why clinicians need to take a cautious approach when using antipsychotic medications in a vulnerable age group with medical complications. Although all cases, regardless of the underlying mechanism, received antipsychotic treatment, the patient in case 1 presented the most complex management issues due to neuroinflammation, exemplifying the interface between psychiatric and medical disorders. The antipsychotic medication haloperidol worsened this patient’s behavior, consistent with the MIS-C diagnosis. It took a relatively long time for this patient to respond to combined treatment with steroids, antibiotics, and intravenous fluids. However, a high-dose methylprednisolone therapy may have also contributed to the neuropsychiatric symptoms in this patient, which started after the initiation of the steroid and improved after its discontinuation.
In case 2, the effects of initial treatment with low-dose antipsychotic medication are not described, but the patient gradually responded to intravenous immunoglobulins and methylprednisolone for suspected autoimmune encephalitis. This patient continued to have intellectual and physical symptoms even after 4 months of symptom onset. In contrast to cases 1 and 2, the patient in case 3 responded well to low-dose treatment with aripiprazole (2–5 mg/d) with no adverse effects. Aripiprazole was selected for its partial agonism at the dopamine-2 receptors,25 which may carry a lower risk of adverse effects, especially at low doses and in a young patient. Although these management observations are based on only 3 cases, they underscore the need to identify the mechanisms underlying psychosis as the antipsychotic response and tolerability may differ between patients. In addition, adolescents with underlying severe medical conditions are highly vulnerable to the adverse effects of antipsychotic therapy, especially with high-dose antipsychotic treatment. Although the 2 cases of stress-induced psychosis during the pandemic are not discussed here, it is worth mentioning that 1 of these patients diagnosed with anti-NMDA receptor encephalitis8 had a similar intolerance and lack of efficacy with antipsychotic medications as reported in cases 1 and 2. These observations suggest that young patients are more likely to respond to and tolerate lower antipsychotic doses, which in turn help develop a positive attitude toward psychotropic medications with increased medication adherence. Finally, although steroids have saved thousands of patients with cytokine storm, their use in a vulnerable young population requires caution, as steroids are known for their mood-altering effects.
CONCLUSION
Young patients with COVID-related neuropsychiatric symptoms, including psychosis, need to be monitored closely and diagnosed quickly, and their management should be based primarily on their underlying medical condition. To facilitate diagnosis and timely and effective management, mental health care providers should be aware of different clinical presentations of COVID-related psychosis. At the same time, active and effective psychosocial support is crucial for young individuals to prevent psychosis and any negative long-term effects of the pandemic. Furthermore, clinicians should avoid using high-dose antipsychotic pharmacotherapy to prevent adverse effects in young and vulnerable patients.
Submitted: August 20, 2021; accepted October 19, 2021.
Published online: December 16, 2021.
Potential conflicts of interest: None.
Funding/support: None.
Patient consent: Consent was received from the guardian of patient 3 to publish this case report, and every effort was made to maintain confidentiality.
Clinical Points
- Only 2 cases of COVID-induced psychosis have been reported in young patients, each with a different clinical presentation.
- The new case added in this case-based review is the only report of post-COVID psychosis in an adolescent male after a complete recovery from COVID-19 symptoms.
- Antipsychotic treatment of COVID-induced psychosis may be temporary and may respond to short-term low-dose antipsychotic therapy.
References (25)

- Shen K, Yang Y, Wang T, et al; China National Clinical Research Center for Respiratory Diseases; National Center for Children’s Health, Beijing, China; Group of Respirology, Chinese Pediatric Society, Chinese Medical Association; Chinese Medical Doctor Association Committee on Respirology Pediatrics; China Medicine Education Association Committee on Pediatrics; Chinese Research Hospital Association Committee on Pediatrics; Chinese Non-government Medical Institutions Association Committee on Pediatrics; China Association of Traditional Chinese Medicine, Committee on Children’s Health and Medicine Research; China News of Drug Information Association, Committee on Children’s Safety Medication; Global Pediatric Pulmonology Alliance. Diagnosis, treatment, and prevention of 2019 novel coronavirus infection in children: experts’ consensus statement. World J Pediatr. 2020;16(3):223–231. PubMed CrossRef
- Cui Y, Li F, Leckman JF, et al. The prevalence of behavioral and emotional problems among Chinese school children and adolescents aged 6-16: a national survey. Eur Child Adolesc Psychiatry. 2021;30(2):233–241. PubMed CrossRef
- Lee J. Mental health effects of school closures during COVID-19. Lancet Child Adolesc Health. 2020;4(6):421. PubMed CrossRef
- Marques de Miranda D, da Silva Athanasio B, Sena Oliveira AC, et al. How is COVID-19 pandemic impacting mental health of children and adolescents? Int J Disaster Risk Reduct. 2020;51:101845. PubMed CrossRef
- Jiao WY, Wang LN, Liu J, et al. Behavioral and emotional disorders in children during the COVID-19 epidemic. J Pediatr. 2020;221:264–266.e1. PubMed CrossRef
- Graham EL, Clark JR, Orban ZS, et al. Persistent neurologic symptoms and cognitive dysfunction in non-hospitalized Covid-19 “long haulers”. Ann Clin Transl Neurol. 2021;8(5):1073–1085. PubMed CrossRef
- Kumar S, Veldhuis A, Malhotra T. Neuropsychiatric and cognitive sequelae of COVID-19. Front Psychol. 2021;12:577529. PubMed CrossRef
- Moideen S, Thomas R, Suresh Kumar PN, et al. Psychosis in a patient with anti-NMDA-receptor antibodies experiencing significant stress related to COVID-19. Brain Behav Immun Health. 2020;7:100125. PubMed CrossRef
- Mahapatra A, Sharma P. Case series associated with COVID-19 pandemic in causing psychiatric morbidity. Gen Psychiatr. 2021;34(1):e100343. PubMed CrossRef
- Hutchison L, Plichta AM, Lerea Y, et al. Neuropsychiatric symptoms in an adolescent boy with multisystem inflammatory syndrome in children. Psychosomatics. 2020;61(6):739–744. PubMed CrossRef
- Gaughan M, Connolly S, O’Riordan S, et al. Pediatric parainfectious encephalitis associated with COVID-19. Neurology. 2021;96(11):541–544. PubMed CrossRef
- Elfil M, Selby L, Van Schooneveld TC, et al. Acute psychosis associated with recent SARS-CoV-2 infection: a case report. IDCases. 2021;24:e01140. PubMed CrossRef
- Chacko M, Job A, Caston F 3rd, et al. COVID-19-induced psychosis a suicidal behavior: case report. SN Compr Clin Med. 2020:1–5. PubMed
- Folstein MF, Folstein SE, McHugh PR. “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12(3):189–198. PubMed CrossRef
- Araújo LA, Veloso CF, Souza MC, et al. The potential impact of the COVID-19 pandemic on child growth and development: a systematic review. J Pediatr (Rio J). 2021;97(4):369–377. PubMed CrossRef
- Payne AB, Gilani Z, Godfred-Cato S, et al; MIS-C Incidence Authorship Group. Incidence of multisystem inflammatory syndrome in children among us persons infected with SARS-CoV-2. JAMA Netw Open. 2021;4(6):e2116420. PubMed CrossRef
- Esakandari H, Nabi-Afjadi M, Fakkari-Afjadi J, et al. A comprehensive review of COVID-19 characteristics. Biol Proced Online. 2020;22(1):19. PubMed CrossRef
- Wu Y, Xu X, Chen Z, et al. Nervous system involvement after infection with COVID-19 and other coronaviruses. Brain Behav Immun. 2020;87:18–22. PubMed CrossRef
- Wang L. C-reactive protein levels in the early stage of COVID-19. Med Mal Infect. 2020;50(4):332–334. PubMed CrossRef
- Wang C, Pan R, Wan X, et al. A longitudinal study on the mental health of general population during the COVID-19 epidemic in China. Brain Behav Immun. 2020;87:40–48. PubMed CrossRef
- Ford T, John A, Gunnell D. Mental health of children and young people during pandemic. BMJ. 2021;372:n614. PubMed
- Alpert O, Begun L, Garren P, et al. Cytokine storm induced new onset depression in patients with COVID-19: a new look into the association between depression and cytokines -two case reports. Brain Behav Immun Health. 2020;9:100173. PubMed CrossRef
- Thepmankorn P, Bach J, Lasfar A, et al. Cytokine storm induced by SARS-CoV-2 infection: the spectrum of its neurological manifestations. Cytokine. 2021;138:155404. PubMed CrossRef
- Ford B, McDonald A, Srinivasan S. Anti-NMDA receptor encephalitis: a case study and illness overview. Drugs Context. 2019;8:212589. PubMed CrossRef
- Fryefield K, Shad MU. Can low-dose aripiprazole reverse some of the adverse effects from a long-acting injectable? Schizophr Res. 2019;204:417–418. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!