A Cross-Sectional Survey of Childhood Trauma and Compliance With General Health Care Among Adult Primary Care Outpatients

ABSTRACT
Objective: Beyond the examination of medication compliance among individuals with substance abuse or human immunodeficiency virus (HIV)/acquired immunodeficiency syndrome (AIDS), few studies have examined relationships between childhood trauma and health care compliance in adulthood—the focus of the present study.
Method: Using a cross-sectional approach and a self-report survey methodology, we examined 5 types of childhood trauma (ie, witnessing violence, physical neglect, emotional abuse, physical abuse, sexual abuse) in relationship to 4 measures of general health care compliance (ie, self-rated general conscientiousness with medical treatment; 5 items pertaining to general health care compliance such as scheduling regular dental checkups, timely arrival for doctor’s appointments, and timely completion of laboratory work; 2 medication compliance items; and the Medical Outcomes Study general adherence score) among a sample of adult primary care outpatients (N = 272). Data were collected in March 2014.
Results: According to findings, some health care adherence variables demonstrated relationships with the summed childhood trauma score, whereas others did not. It could be interpreted that the more subjective health care compliance variables (eg, self-rated conscientiousness with regard to medical treatment) demonstrated no relationship with a summed childhood trauma score, whereas the more objective health care compliance variables (eg, frequency of regular dental checkups, ability to remember to take all medications, Medical Outcomes Study general adherence score) did demonstrate statistically significant relationships with a summed childhood trauma score (most at P < .01).
Conclusions: Patients with histories of childhood trauma demonstrate some deficits with health care compliance in comparison to those without childhood trauma. One interpretation is that the mistreated appear to believe that they are fairly compliant with health care treatment, but objective variables appear to suggest otherwise.
Prim Care Companion CNS Disord 2014;16(6):doi:10.4088/PCC.14m01692
© Copyright 2014 Physicians Postgraduate Press, Inc.
Submitted: August 14, 2014; accepted September 8, 2014.
Published online: November 13, 2014.
Corresponding author: Randy A. Sansone, MD, Sycamore Primary Care Center, 2115 Leiter Rd, Miamisburg, OH 45342 ([email protected]).
According to the existing literature, trauma in childhood appears to be associated with greater health care utilization in adulthood. For example, in a study of 150 primary care outpatients in a health maintenance organization (HMO), both physical and emotional abuses demonstrated statistically significant relationships with several measures of health care utilization.1 Likewise, in HMO samples of women, sexual abuse in childhood was associated with higher treatment costs2 and higher numbers of physician visits.3 Finally, in a study of 129 patients in specialty clinics, childhood adversity was correlated with a significantly greater number of office visits over the study period.4 Given this general theme of greater health care utilization among individuals who experienced childhood abuse, what about treatment compliance once health care is sought?
Published data on childhood trauma and health care compliance in adulthood frequently originate in the substance abuse literature. For example, Hien and Levin5 reported that untreated trauma may result in nonadherence with methadone treatment. The other vein of research has been treatment compliance among individuals with human immunodeficiency virus (HIV) and acquired immunodeficiency syndrome (AIDS). For example, treatment noncompliance among adult individuals with HIV/AIDS has been associated with the number of lifetime traumatic events,6 childhood sexual abuse,7 childhood sexual and physical abuse,8 trauma symptoms,9 childhood trauma,10 and the number of traumatic events in childhood.11 In addition, Aaron et al12 indicated that among women, childhood sexual abuse heightens the risk for nonadherence to HIV medications as well as sporadic medical treatment.
As with most topics, there are opposing findings in the literature as well. For example, Liu et al13 reported that childhood sexual abuse was not associated with medication adherence difficulties among women with HIV. In a similar vein, Mugavero et al14 reported that participants with a history of childhood abuse were more likely to present early for HIV treatment. However, while subsequent compliance was not empirically examined in this latter study, the authors explicitly affirmed that childhood sexual abuse was associated with medication noncompliance.14
Data outside of the areas of substance abuse and HIV/AIDS treatment appear to be sparse. In the only other article that we could locate, Lurie et al15 found that sexual and physical abuses were statistically significantly associated with treatment noncompliance among pediatric liver transplant recipients.
Overall, the existing literature on childhood trauma and compliance with medical treatment in adulthood is fairly sparse. Moreover, the limitations of the current literature include (1) nominal examination of childhood trauma variables in many cases (eg, childhood sexual abuse only, childhood sexual and physical abuses only), (2) unique study populations (substance abusers, HIV/AIDS samples) with an unknown ability to generalize findings to primary care outpatients, and (3) limited outcome variables (eg, compliance with a single treatment). In this study, we examined 5 forms of childhood trauma in relationship to 4 categories of general health care compliance in adulthood.

- Few studies have examined relationships between childhood trauma and compliance with health care in adulthood, with the exception of several investigations in substance abuse and/or human immunodeficiency virus/acquired immunodeficiency syndrome populations; in addition, many, if not most, of these studies have examined only 1 health care adherence variable (eg, compliance with medication).
- In this study, we examined 272 adult primary care patients with regard to 5 measures of childhood trauma and 4 measures of general health care compliance.
- Findings indicate associations between childhood trauma and some, but not all, of the health care compliance variables studied. One interpretation is that, in contrast to the more subjective variables, the more objective variables were more likely to evidence compliance deficits.
METHOD
Participants
Potential participants in this study were men and women, aged 18 years or older, being seen at an internal medicine outpatient clinic for nonemergent medical care. The clinic is located in a midsized midwestern city in the United States and is staffed by both residents and faculty in the Department of Internal Medicine. However, the majority of patients in this clinic are seen by resident providers. We excluded individuals with compromising medical (eg, debilitating pain), intellectual (eg, mental retardation), cognitive (eg, dementia), or psychiatric symptoms (eg, psychotic) of a severity to preclude the candidate’s ability to successfully complete a survey (n = 5; 2 with vision impairment, 2 with cognitive impairment, 1 with mental retardation). This exclusion process was informal and undertaken by the recruiter as patients registered for clinical service, because surveys needed to be completed before appointments with providers.
At the outset, 354 individuals were approached and 300 agreed to participate, for a participation rate of 84.7%. As for the 54 individuals who declined the invitation to participate, 17 stated they were feeling too ill to participate, 19 indicated not enough time, 14 stated "don’ t like surveys," 3 stated "pleased with current care," and 1 stated "too angry" to participate. Of the 300 individuals who agreed to participate, 278 returned the survey, and 272 completed the measures of childhood adversity. The effective sample thus consisted of 214 (78.7%) women and 58 (21.3%) men, ranging in age from 18 to 89 years (mean = 45.50, SD = 13.89). Most participants were white (85.7%); however, 8.5% of participants were black, 2.2% Native American, 0.4% Asian, 1.1% Hispanic, and 2.2% "other." With regard to educational attainment, all but 5.5% had at least graduated high school, yet only 10.7% had earned at least a bachelor’s degree.
Procedure
During clinic hours, one of the authors (R.J.B.) positioned himself in the lobby of the outpatient clinic, approached incoming patients following registration, and informally assessed exclusion criteria. With potential candidates, the recruiter reviewed the focus of the project (ie, a study examining childhood experiences and health care in adulthood) and then invited each to participate. Each participant was asked to complete a 5-page anonymous survey, which took about 10 minutes. Surveys were completed onsite in the lobby. Participants were asked to place completed surveys into sealed envelopes and then into a collection box in the lobby.
In addition to a demographic query, in which we asked participants about their age, sex, race, marital status, and highest level of completed education, participants were asked whether they had experienced any of 5 different forms of childhood trauma. Specifically, participants were asked, "Prior to the age of 12, did you ever experience (1) the witnessing of violence (ie, the first-hand observation of violence that did not directly involve you), (2) physical neglect (ie, not having your basic life needs met), (3) emotional abuse (ie, verbal and nonverbal behaviors by another individual that were purposefully intended to hurt and control you, not kid or tease you), (4) physical abuse (ie, any physical insult against you that would be considered inappropriate by either yourself or others and that left visible signs of damage on your body either temporarily or permanently or caused pain that persisted beyond the ‘ punishment’ ), and (5) sexual abuse (ie, any sexual activity against your will)." Response options for each item were "yes" and "no." We elected this succinct assessment because of our previous research experience with this measure and our belief that the measure accommodates well to the demands of a busy medical clinic.
Next, the survey contained queries in 4 categories pertaining to various facets of adherence to medical treatment in adulthood. The first author-developed query was, "In general, how conscientious are you about following through with medical treatment?" with Likert-style response options from 1 (very conscientious) to 5 (not conscientious at all). Responses were subsequently recoded so that higher scores indicated greater self-reported conscientiousness. The second author-developed measure consisted of 5 queries, each exploring general compliance with various health care behaviors (eg, regular dental checkups, arrival to doctors’ appointments on time, completion of laboratory work, exercise instructions, diet instructions), with 5 Likert-style response options from 0 (never) to 4 (always) as well as "not applicable." The third measure examined compliance with medication by asking, "Did you take your medicine yesterday?" with yes/no response options, and, "How often do you have difficulty remembering to take your medication?" with Likert-style responses from 1 (never/rarely) to 5 (all the time). This latter variable was reverse-scored so that higher scores indicated greater ability to remember to take medications.
The fourth measure was the Medical Outcomes Study general adherence items.16 This scale explores general medical compliance with "my doctor" over the past 4 weeks, and consists of 5 items (I had a hard time doing what the doctor suggested I do; I followed my doctor’s suggestions exactly; I was unable to do what was necessary to follow my doctor’s treatment plan; I found it easy to do the things my doctor suggested I do; Generally speaking, how often during the past 4 weeks were you able to do what the doctor told you?), with 6 Likert-style response options from 1 (none of the time) to 6 (all of the time). After recoding 2 of the items, scores were summed across items to render a composite score. Note that with all measures used, higher scores indicate higher levels of compliance.
This project was reviewed and exempted by the institutional review boards of the sponsoring hospital and the local university. Completion of the survey was assumed to be implied consent, which was explained to participants on the cover page of the survey. Data were collected in March 2014.
RESULTS
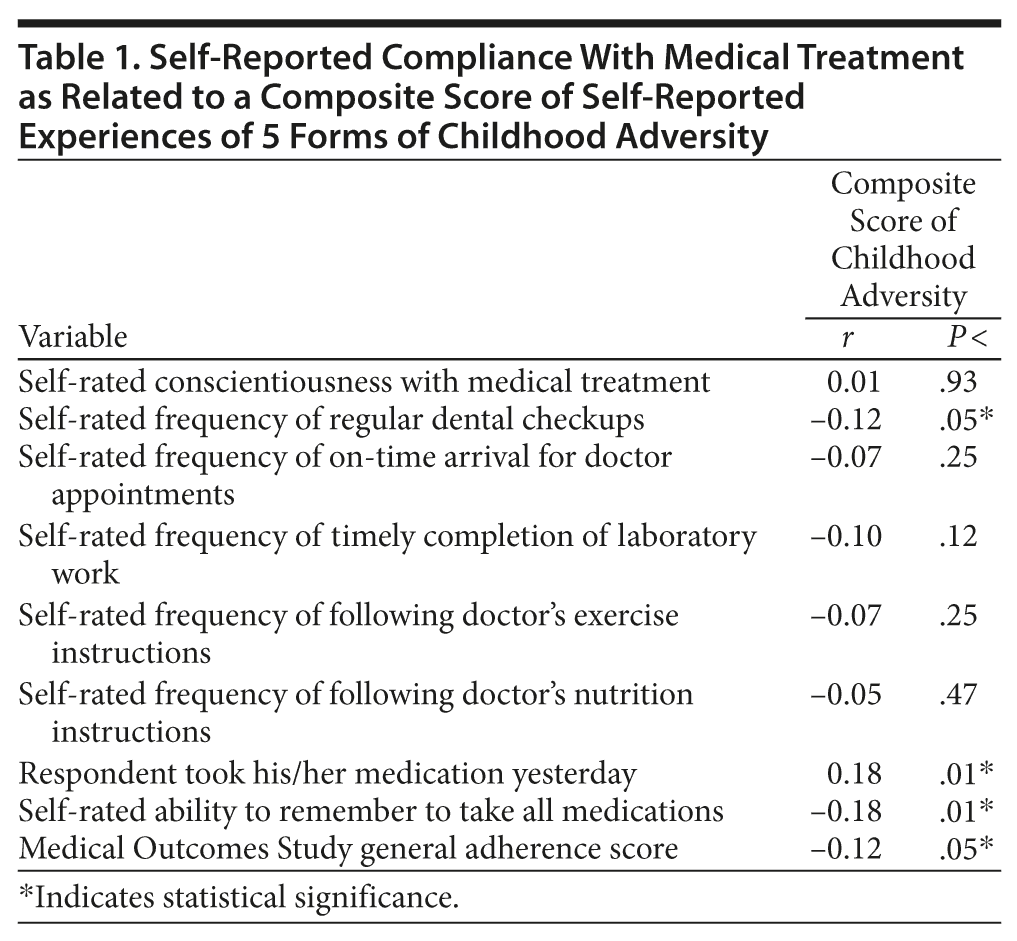
Of the 272 respondents, 45.2% reported witnessing violence during childhood, 15.1% physical neglect, 51.8% emotional abuse, 32.7% physical abuse, and 23.5% sexual abuse. First, we examined relationships between each of the 5 forms of childhood trauma and each of the measures of health care compliance by conducting a series of 1-way analyses of variance on each of the health care compliance variables as a function of whether the respondent reported having experienced each particular form of childhood trauma. The general pattern was that either all of the forms of childhood trauma were related to a particular health care compliance variable or none were. So, to efficiently present the findings, we created an overall childhood trauma score by summing across all 5 forms of childhood trauma. Possible scores could range from 0 to 5, and actual scores did as well. The most common score was 0 (38.6% of respondents), and the least frequent score was 5 (7.0%). Simple correlations between the composite childhood trauma score and the measures of health care compliance are presented in Table 1.
DISCUSSION
Findings indicate an inconsistent relationship between childhood trauma and compliance with health care in adulthood. In other words, while childhood trauma appears to affect some health care compliance variables, it does not affect others. Overall, this observation suggests that childhood trauma exerts a potentially detrimental effect on some aspects of health care compliance, but not all aspects.
Upon closer examination, a possible interpretation of this subtle irregularity in the pattern of health care compliance emerges. Participants appeared to rate themselves as more compliant when variables were softer, less tangible, and/or less concrete (eg, conscientiousness with following through with general medical treatment, arriving on time for doctor appointments, timely completion of laboratory work, compliance with the doctor’s exercise and nutrition instructions). In contrast, with more definitive health care variables (eg, frequency of regular dental checkups, remembering to take all medications, Medical Outcomes Study items—ie, following doctor’s orders precisely), the childhood trauma score was statistically significantly associated with lower health care adherence. Thus, one could interpret that while the more subjective health care variables did not demonstrate a relationship with childhood trauma, the more objective health care variables did demonstrate a relationship (albeit small). This interpretation warrants replication and emphasizes the relevance in future research of developing highly objective queries for participants, as conclusions based on overly subjective items might be misleading.
One peculiar finding in this study is the seeming paradox between the 2 queries about medication compliance—both statistically significant. While respondents with childhood trauma were statistically significantly more likely to have taken "medication yesterday," they were also statistically significantly more likely to have had difficulty remembering to take all of their medications. This seemingly inconsistent finding may either reflect a temporal phenomenon (ie, individuals could verify medication adherence yesterday, but not beyond yesterday) or a subjective versus objective phenomenon ("I seemed to have taken my medication yesterday, but overall, I have pills left over"). This particular item could be easily re-examined in conjunction with pharmacy records to heighten the objectivity of data collection.
Weaving together findings in the literature with findings from the current study, it appears that victims of childhood trauma tend to seek out care more often than those without such histories. However, after securing care, they demonstrate some deficits with health care compliance. One interpretation of these deficits is that those exposed to childhood trauma may believe that they are generally treatment compliant (subjective variables) but may actually be less compliant with objective treatment variables.
What might generally explain the finding of reduced health care compliance among those traumatized in childhood? First, a number of psychiatric comorbidities may partially contribute to this finding. These comorbidities might include posttrauma depression, substance abuse, posttraumatic stress disorder, personality pathology, and health anxiety—all feasible explanations for reduced health care compliance. Second, perhaps being traumatized at a young age diminishes one’s personal sense of value. Literally, "I am not worth being medically treated." Third, perhaps early childhood trauma results among some individuals in either self-regulatory disturbances or a self-defeating pattern that extends to health care compliance. Whatever the explanation, findings suggest that, among the noncompliant, exploration of trauma in childhood may be relevant.
This study has a number of potential limitations. First and foremost, all data were self-report in nature and thus subject to the vicissitudes of recollection, denial, suppression, repression, and deceit. Second, the sample is relatively small. Third, this sample was from a predominantly resident provider clinic; findings may not generalize to more traditional private practice settings. Fourth, there is the possibility of type 2 error; thus, replication of these findings is warranted in further research endeavors. However, this is one of the few studies to examine childhood trauma in relationship to health care compliance in adulthood in a primary care sample, the sample was consecutive, and the health care compliance variables were diverse (not just 1 variable, such as medication compliance). Findings indicate that patients with childhood trauma demonstrate erratic compliance with health care, and one interpretation is that victims may believe that they are fairly compliant with health care treatment, but objective variables appear to suggest otherwise.
Drug names: methadone (Methadose and others).
Author affiliations: Departments of Psychiatry (Dr Sansone) and Internal Medicine (Drs Sansone and Bohinc), Wright State University School of Medicine, Dayton, Ohio; Department of Psychiatry Education, Kettering Medical Center, Kettering, Ohio (Dr Sansone); and Department of Psychology, Columbia College, Columbia, South Carolina (Dr Wiederman).
Potential conflicts of interest: None reported.
Funding/support: None reported.
REFERENCES
1. Sansone RA, Wiederman MW, Sansone LA. Health care utilization and history of trauma among women in a primary care setting. Violence Vict. 1997;12(2):165-172. PubMed
2. Walker EA, Unutzer J, Rutter C, et al. Costs of health care use by women HMO members with a history of childhood abuse and neglect. Arch Gen Psychiatry. 1999;56(7):609-613. PubMed doi:10.1001/archpsyc.56.7.609
3. Newman MG, Clayton L, Zuellig A, et al. The relationship of childhood sexual abuse and depression with somatic symptoms and medical utilization. Psychol Med. 2000;30(5):1063-1077. PubMed doi:10.1017/S003329179900272X
4. Fiddler M, Jackson J, Kapur N, et al. Childhood adversity and frequent medical consultations. Gen Hosp Psychiatry. 2004;26(5):367-377. PubMed doi:10.1016/j.genhosppsych.2004.04.001
5. Hien D, Levin FR. Trauma and trauma-related disorders for women on methadone: prevalence and treatment considerations. J Psychoactive Drugs. 1994;26(4):421-429. PubMed doi:10.1080/02791072.1994.10472462
6. Mugavero M, Ostermann J, Whetten K, et al. Barriers to antiretroviral adherence: the importance of depression, abuse, and other traumatic events. AIDS Patient Care STDS. 2006;20(6):418-428. PubMed doi:10.1089/apc.2006.20.418
7. Markowitz SM, O’ Cleirigh C, Hendriksen ES, et al. Childhood sexual abuse and health risk behaviors in patients with HIV and a history of injection drug use. AIDS Behav. 2011;15(7):1554-1560. PubMed doi:10.1007/s10461-010-9857-y
8. Pence BW. The impact of mental health and traumatic life experiences on antiretroviral treatment outcomes for people living with HIV/AIDS. J Antimicrob Chemother. 2009;63(4):636-640. PubMed doi:10.1093/jac/dkp006
9. Meade CS, Hansen NB, Kochman A, et al. Utilization of medical treatments and adherence to antiretroviral therapy among HIV-positive adults with histories of childhood sexual abuse. AIDS Patient Care STDS. 2009;23(4):259-266. PubMed doi:10.1089/apc.2008.0210
10. Pence BW, Mugavero MJ, Carter TJ, et al. Childhood trauma and health outcomes in HIV-infected patients: an exploration of causal pathways. J Acquir Immune Defic Syndr. 2012;59(4):409-416. PubMed doi:10.1097/QAI.0b013e31824150bb
11. Whetten K, Shirey K, Pence BW, et al; CHAT Research Team. Trauma history and depression predict incomplete adherence to antiretroviral therapies in a low-income country. PLoS ONE. 2013;8(10):e74771. PubMed doi:10.1371/journal.pone.0074771
12. Aaron E, Criniti S, Bonacquisti A, et al. Providing sensitive care for adult HIV-infected women with a history of childhood sexual abuse. J Assoc Nurses AIDS Care. 2013;24(4):355-367. PubMed doi:10.1016/j.jana.2013.03.004
13. Liu H, Longshore D, Williams JK, et al. Substance abuse and medication adherence among HIV-positive women with histories of child sexual abuse. AIDS Behav. 2006;10(3):279-286. PubMed doi:10.1007/s10461-005-9041-y
14. Mugavero MJ, Pence BW, Whetten K, et al. Childhood abuse and initial presentation for HIV care: an opportunity for early intervention. AIDS Care. 2007;19(9):1083-1087. PubMed doi:10.1080/09540120701351896
15. Lurie S, Shemesh E, Sheiner PA, et al. Nonadherence in pediatric liver transplant recipients: an assessment of risk factors and natural history. Pediatr Transplant. 2000;4(3):200-206. PubMed doi:10.1034/j.1399-3046.2000.00110.x
16. Hays RD. The Medical Outcomes Study (MOS) Measures of Patient Adherence. http://www.rand.org/content/dam/rand/www/external/health/surveys_tools/mos/mos_adherence_survey.pdf. Accessed April 14, 2014.