Background: Bright light therapy has demonstrated efficacy and is an accepted treatment for seasonal depression. It has been suggested that bright light therapy may have efficacy in nonseasonal depressions. Also, there is evidence that bright light therapy may improve responsiveness to antidepressant pharmacotherapy.
Data Sources: We searched PubMed/MEDLINE, PsycINFO, PsycARTICLES, CINAHL, EMBASE, Scopus, and Academic OneFile for English-language literature published between January 1998 and April 2016, using the keywords bright light therapy AND major depression, bright light therapy AND depress*, bright light therapy AND bipolar depression, bright light therapy AND affective disorders, circadian rhythm AND major depression, circadian rhythm AND depress*, and circadian rhythm AND affective disorder.
Study Selection and Data Extraction: Studies that reported randomized trials comparing antidepressant pharmacotherapy with bright light therapy ≥ 5,000 lux for ≥ 30 minutes to antidepressant pharmacotherapy without bright light therapy for the treatment of nonseasonal depression were included. Studies of seasonal depression were excluded. Following review of the initial 112 returns, 2 of the authors independently judged each trial, applying the inclusionary and exclusionary criteria. Ten studies were selected as meeting these criteria. Subjects in these studies were pooled using standard techniques of meta-analysis.
Results: Ten studies involving 458 patients showed improvement using bright light therapy augmentation versus antidepressant pharmacotherapy alone. The effect size was similar to that of other accepted augmentation strategies, roughly 0.5.
Conclusions: Analysis of pooled data from randomized trials provides evidence for the efficacy of use of bright light therapy ≥ 5,000 lux for periods ≥ 30 minutes when used as augmentation to standard antidepressant pharmacotherapy in the treatment of major depressive disorder and bipolar depression without a seasonal pattern.
CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer the questions in the Posttest, and complete the Evaluation.
CME Objective
After studying this article, you should be able to:
• Consider the use of bright light therapy to augment antidepressant effects in the treatment of refractory nonseasonal depressive episodes of major depressive disorder and bipolar disorder
Accreditation Statement
The CME Institute of Physicians
Postgraduate Press, Inc., is
accredited by the Accreditation
Council for Continuing Medical
Education to provide continuing
medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1.0 AMA PRA Category 1 Credit™. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Academy of Physician Assistants (AAPA) accepts certificates of participation for educational activities certified for AMA PRA Category 1 Credit™ from organizations accredited by ACCME or a recognized state medical society. Physician assistants may receive a maximum of 1.0 hour of Category I credit for completing this program.
Date of Original Release/Review
This educational activity is eligible for AMA PRA Category 1 Credit™ through October 31, 2018. The latest review of this material was September 2016.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Larry Culpepper, MD, MPH, Editor in Chief, has been a consultant for Forest, Lundbeck, Merck, Shire, Takeda, and Elsevier Press; has been a stock shareholder of M3 My Mood Monitor; and has received royalties from UpToDate and Oxford University Press. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
Bright Light Therapy as Augmentation of Pharmacotherapy for Treatment of Depression:
A Systematic Review and Meta-Analysis
ABSTRACT
Background: Bright light therapy has demonstrated efficacy and is an accepted treatment for seasonal depression. It has been suggested that bright light therapy may have efficacy in nonseasonal depressions. Also, there is evidence that bright light therapy may improve responsiveness to antidepressant pharmacotherapy.
Data Sources: We searched PubMed/MEDLINE, PsycINFO, PsycARTICLES, CINAHL, EMBASE, Scopus, and Academic OneFile for English-language literature published between January 1998 and April 2016, using the keywords bright light therapy AND major depression, bright light therapy AND depress*, bright light therapy AND bipolar depression, bright light therapy AND affective disorders, circadian rhythm AND major depression, circadian rhythm AND depress*, and circadian rhythm AND affective disorder.
Study Selection and Data Extraction: Studies that reported randomized trials comparing antidepressant pharmacotherapy with bright light therapy ≥ 5,000 lux for ≥ 30 minutes to antidepressant pharmacotherapy without bright light therapy for the treatment of nonseasonal depression were included. Studies of seasonal depression were excluded. Following review of the initial 112 returns, 2 of the authors independently judged each trial, applying the inclusionary and exclusionary criteria. Ten studies were selected as meeting these criteria. Subjects in these studies were pooled using standard techniques of meta-analysis.
Results: Ten studies involving 458 patients showed improvement using bright light therapy augmentation versus antidepressant pharmacotherapy alone. The effect size was similar to that of other accepted augmentation strategies, roughly 0.5.
Conclusions: Analysis of pooled data from randomized trials provides evidence for the efficacy of use of bright light therapy ≥ 5,000 lux for periods ≥ 30 minutes when used as augmentation to standard antidepressant pharmacotherapy in the treatment of major depressive disorder and bipolar depression without a seasonal pattern.
Prim Care Companion CNS Disord 2016;18(5):doi:10.4088/PCC.15r01906
© Copyright 2016 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry and Behavioral Medicine, Brody School of Medicine, East Carolina University, Greenville, North Carolina
bDepartment of Psychology, East Carolina University, Greenville, North Carolina
*Corresponding author: Department of Psychiatry and Behavioral Medicine, Brody School of Medicine, East Carolina University, Ste 400E, 600 Moye Blvd, Greenville, NC 27834 ([email protected]).
Depressive disorders are highly prevalent worldwide. Lifetime prevalence is estimated to be 21% of the population of the United States1 and at least 15% globally. Depression is a strong contributor to disability and burden of disease,2,3 as well as a risk for death by suicide. Depression is a factor affecting the course, morbidity, and mortality of several common and chronic medical illnesses such as heart disease, cancer, and diabetes. Depression contributes to untold suffering for those affected and their loved ones. Analysis of large naturalistic clinical trials4,5 has shown the limits of current treatments for both major depressive disorder and bipolar disorder. Development of new approaches to treatment of refractory depression has been identified as a significant unmet need among psychiatric clinicians.6
When a single antidepressant agent fails to produce significant improvement or remission in a patient with a depressive disorder, use of multiple pharmacologic agents or psychosocial interventions has been an accepted standard. Such augmentation strategies include addition of lithium carbonate, thyroid hormone, a second antidepressant, or certain second-generation antipsychotics. In the case of bipolar depression, strategies include use of mood stabilizers or antipsychotic medications.7,8
Bright light therapy is an accepted modality for treatment of major depressive disorder with a seasonal pattern, commonly referred to as seasonal affective disorder.9 Studies10 have also suggested that bright light monotherapy may have some efficacy in the treatment of depressive illnesses with no seasonal pattern. Also, several studies11 have suggested that bright light therapy may augment the efficacy of established pharmacotherapies in the treatment of nonseasonal depression. A comprehensive review11 published in 2005 of literature relating to the use of bright light therapy for treatment of mood disorders concluded that “bright light for nonseasonal depression is efficacious, with effect sizes equivalent to those in most antidepressant pharmacotherapy trials.”(p31) Despite the very limited risks and costs associated with the use of bright light therapy, there has been little utilization in clinical practice outside treatment for seasonal affective disorder.12 This systematic review and meta-analysis was conducted to assess the current state of evidence favoring use of bright light therapy as an augmentation to antidepressant pharmacotherapy in the treatment of depressive disorders with no seasonal pattern.
METHODS
This meta-analysis complies with the criteria provided in the Preferred-Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA). Two members of the research team (T.M.P. and C.N.S.) reviewed initial returns and selected trials on the basis of predefined inclusionary and exclusionary criteria.13–23
Data Sources
We searched PubMed/MEDLINE, PsycINFO, PsycARTICLES, CINAHL, EMBASE, Scopus, and Academic OneFile for English-language medical literature published between January 1998 and April 2016 using the search terms bright light therapy AND major depression, bright light therapy AND depress*, bright light therapy AND bipolar depression, bright light therapy AND affective disorders, circadian rhythm AND major depression, circadian rhythm AND depress*, and circadian rhythm AND affective disorder. Search results were supplemented by references gleaned from recent reviews and citations of searched returns.
Inclusion and Exclusion Criteria and Study Selection
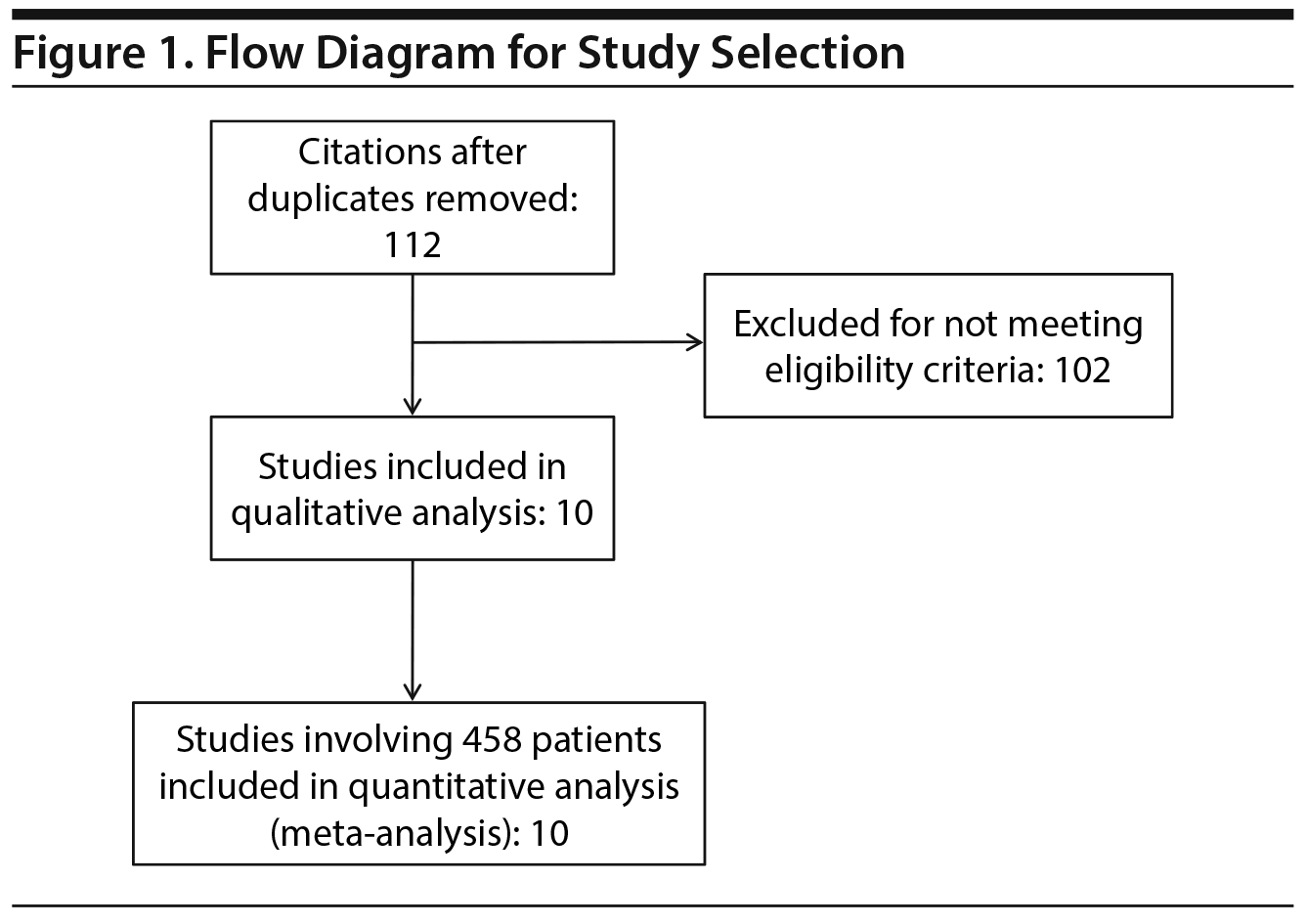
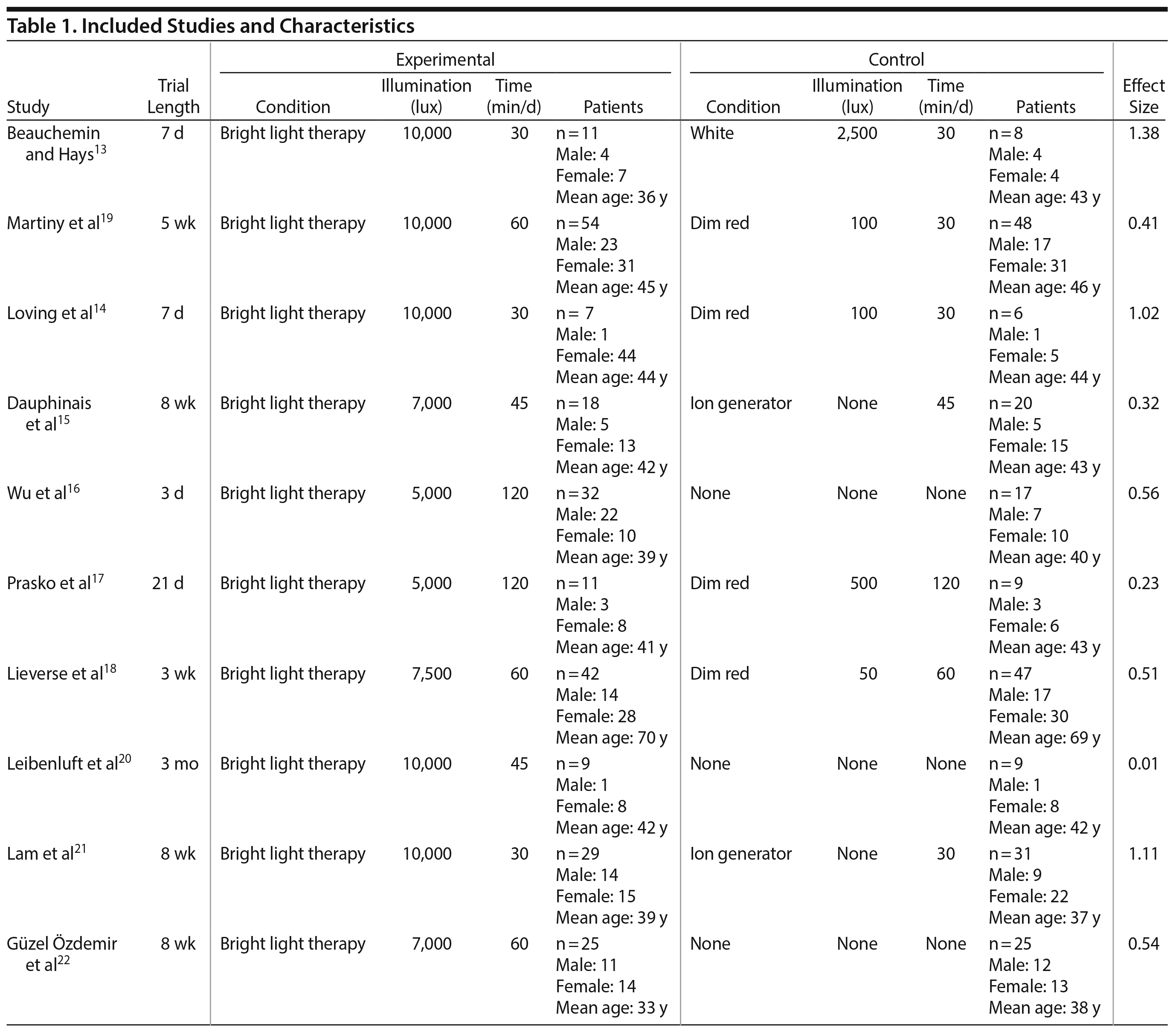
All studies that reported randomized trials comparing antidepressant pharmacotherapy with bright light therapy ≥ 5,000 lux for ≥ 30 minutes to antidepressant pharmacotherapy without bright light therapy for the treatment of nonseasonal depression were included. Studies that included subjects with seasonal depression, subsyndromal symptoms, dementia, eating disorders, bright light therapy alone, or premenstrual dysphoric disorder were excluded. The original search yielded 112 reports. After elimination of studies with exclusionary criteria, 10 studies13–22 met our original search criteria (Figure 1, Table 1). In the case of 2 disputed exclusions, 1 reviewer (S.A.S.) mediated an agreement on proper allocation.
Data Extraction and Analysis
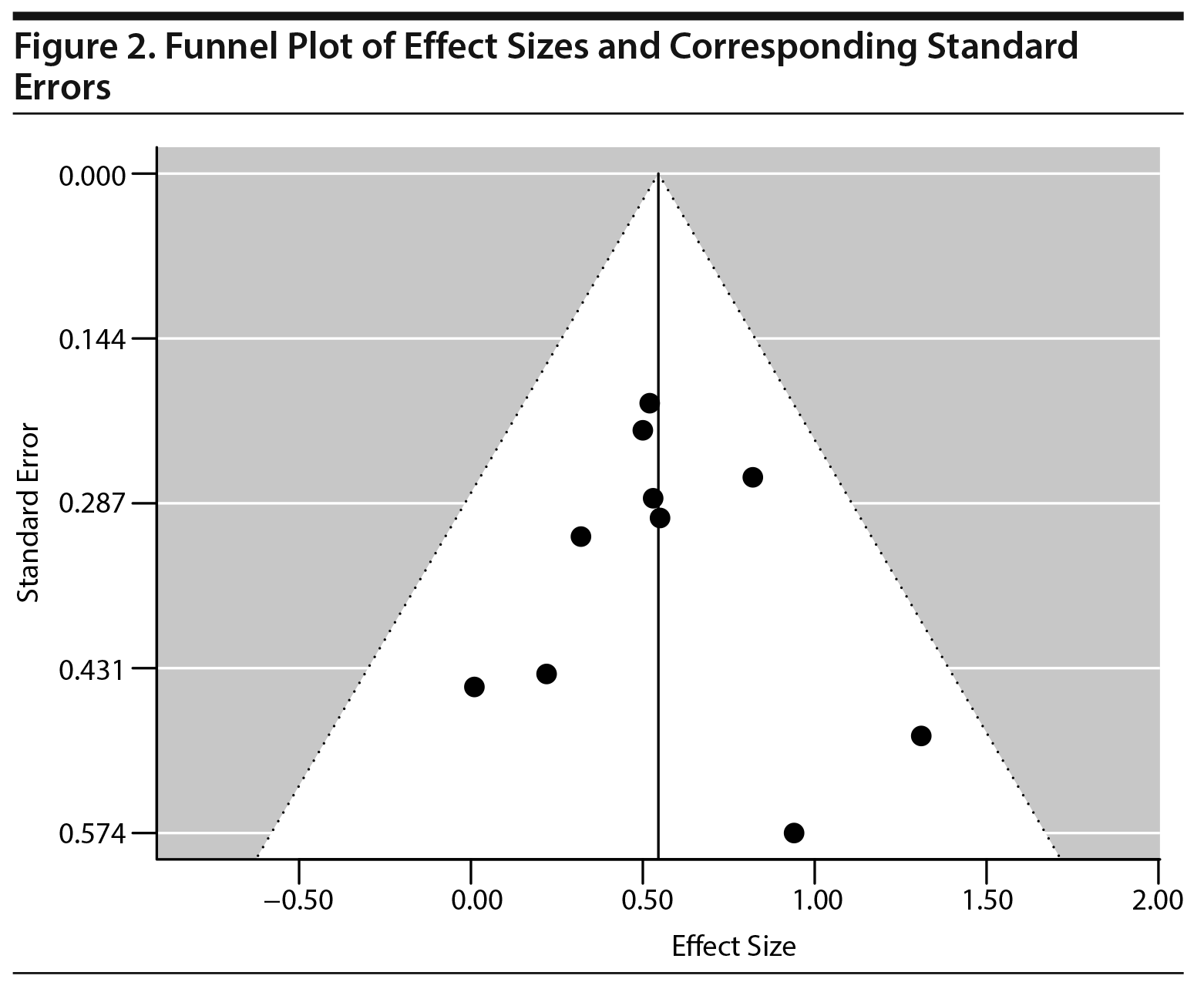
Our statistician (A.M.S.) extracted the number of subjects and the outcomes by trial arm. All studies meeting inclusion criteria that reported the statistical information necessary to compute an effect size were included in all analyses. We used standard meta-analytic methods based on Lipsey and Wilson.23 On the basis of the reported results for each study, we computed a standardized mean effect size and its 95% confidence interval, with small sample size corrections when appropriate.24 Across the 10 studies, the weighted mean of the effect sizes and the variance of the effect sizes were computed using inverse variance weights from each study (Figure 2). All analyses were conducted with the metafor25 package using the statistical software R.26
RESULTS
Publication bias was assessed with a visual inspection of a funnel plot and a rank correlation test of funnel plot asymmetry.27 Neither the funnel plot (Figure 2) nor the rank correlation test (Kendall τ = −0.022, P = .999) showed evidence of publication bias among the studies.
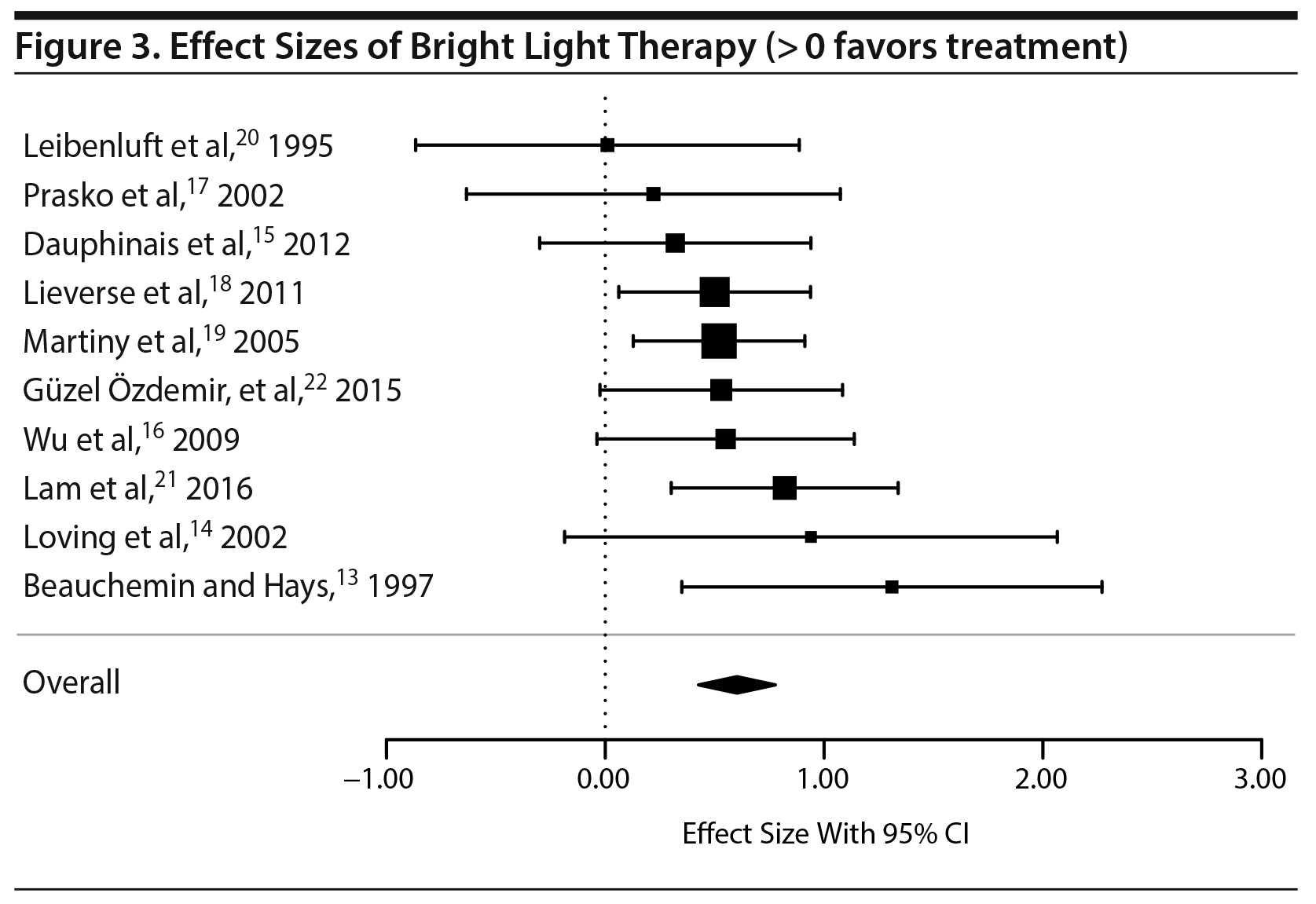
Across the 10 studies that met inclusion criteria, bright light therapy had a positive and significant effect (g = 0.545, P < .001; 95% CI, 0.385–0.732). The variance of the effect sizes was not significantly different from zero (τ2 = 0.00; 95% CI, 0.000–0.170), and there was no significant heterogeneity in effect sizes (Q9 = 6.54, P = .685) (Figure 3).
Quality of Studies
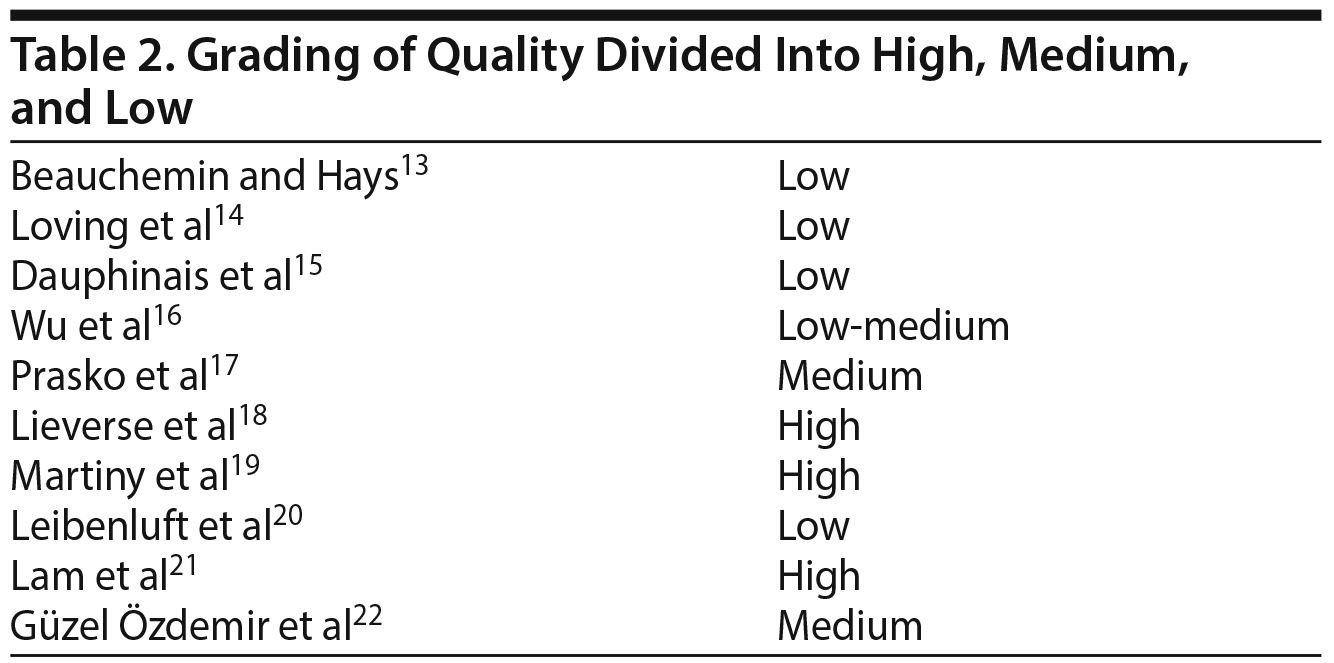
Two reviewers (P.T.N. and R.B.) independently evaluated the quality of each study using guidelines established by the GRADE28 (Grading of Recommendations, Assessment, Development, and Evaluation) method. Only 3 studies18,19,21 were judged to be of high quality. Three others16,17,22 were rated as medium or low to medium. The remaining studies13,14,15,20 were rated as low quality (Table 2). Studies included subjects with bipolar and major depressive disorder, introducing a possible bias on the basis of this selection.
DISCUSSION
Many patients with depressive disorder fail to respond to standard antidepressant pharmacotherapy, psychotherapy alone, or the combination. Augmentation strategies improve outcome in many cases, but treatment resistance remains common, leaving many patients with disabling or distressing residual symptoms. Adoption of bright light therapy for treatment of nonseasonal depression by psychiatric clinicians remains quite limited despite a recommendation for use by the American Psychiatric Association.29 Insurance coverage for bright light therapy for nonseasonal depression is also severely limited. However, the quality of current evidence supports a recommendation for efficacy. This meta-analysis supports conclusions reached by others,10 suggesting that bright light therapy is effective and can add to the armamentarium of interventions available to patients with refractory depressive disorders. Recently reported studies30 add substantially to evidence in support of bright light therapy to augment the therapeutic actions of antidepressant agents.
The studies meeting criteria for inclusion in this analysis varied substantially in their design, measured outcomes for improvement in depression, length of light exposure, type of placebo, and lengths of the trials. Antidepressant treatments varied from study to study. The study19 with the largest number of subjects utilized a single antidepressant and controlled dosing. Another study16 provided outcomes after only 3 days and also included an additional intervention, wake therapy, introducing additional significant confounds. Leibenluft et al20 reported a study of a limited number of subjects with rapid-cycling bipolar disorder, a group substantially different from those of most other included studies.
Limitations
The resultant heterogeneity in the studies included in this pooled analysis somewhat confounds interpretation of the data. However, all included studies were consistent in reporting antidepressant action of bright light therapy for depressions with no seasonal pattern. Future trials will benefit from designs that limit these confounds as attempts are made to better define the effect of bright light therapy in the several subtypes of depressive disorders. There also may be a potential for development of markers and predictors of response to bright light therapy when used as an augmentation strategy.
CONCLUSION
Analysis of pooled data from randomized trials provides evidence for the efficacy for use of bright light therapy administered at ≥ 5,000 lux for periods ≥ 30 minutes when used as augmentation to standard antidepressant treatment. Methodological flaws, small sample sizes, and heterogeneity of published studies have resulted in strength of evidence that is moderate overall.
Submitted: November 6, 2015; accepted August 2, 2016.
Published online: October 20, 2016.
Drug names: lithium (Lithobid and others).
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, lithium is not approved by the US Food and Drug Administration for augmentation of antidepressant action.
Financial disclosure: Dr Ninan has served as a consultant to Lundbeck. Drs Penders, Stanciu, Schoemann, Bloch, and Saeed have no personal affiliations or financial relationships with any commercial interest to disclose relevant to the activity.
Funding/support: None.
REFERENCES
1. Kessler RC, Berglund P, Demler O, et al. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2005;62(6):593–602. PubMed doi:10.1001/archpsyc.62.6.593
2. Global Burden of Disease Study 2013 Collaborators. Global, regional and national incidence, prevalence and years lived with disability for 301 acute and chronic diseases and injuries in 188 counties, 1990–2013: a systematic analysis from the Global Burden of Disease Study, 2013. Lancet. 2015;386(9995):743–800. PubMed doi:10.1016/s0140-6736(15)60692-4
3. Ferrari AJ, Charlson FJ, Norman RE, et al. Burden of depressive disorders by country, sex, age, and year: findings from the Global Burden of Disease Study 2010. PLoS Med. 2013;10(11):e1001547. doi:10.1371/journal.pmed.1001547 PubMed
4. Gaynes BN, Warden D, Trivedi MH, et al. What did STAR*D teach us? results from a large-scale, practical, clinical trial for patients with depression. Psychiatr Serv. 2009;60(11):1439–1445. PubMed doi:10.1176/ps.2009.60.11.1439
5. Sachs GS, Thase ME, Otto MW, et al. Rationale, design, and methods of the Systematic Treatment Enhancement Program for Bipolar Disorder (STEP-BD). Biol Psychiatry. 2003;53(11):1028–1042. PubMed doi:10.1016/S0006-3223(03)00165-3
6. Zarate C, Duman RS, Liu G, et al. New paradigms for treatment-resistant depression. Ann N Y Acad Sci. 2013;1292:21–31. PubMed doi:10.1111/nyas.12223
7. Work Group on Major Depressive Disorder. Practice Guideline for the Treatment of Patients with Major Depressive Disorder. 3rd ed. Arlington, VA: American Psychiatric Association; 2010.
8. Nierenburg AA, Ostacher MJ, Delgado PL et al. Antidepressant and Antimanic Medications. In: Gabbard G, ed. Gabbard’s Treatments of Psychiatric Disorders. 4th ed. Arlington, VA: American Psychiatric Publishing; 2010.
9. Kasper S, Rogers SLB, Yancey A, et al. Phototherapy in individuals with and without subsyndromal seasonal affective disorder. Arch Gen Psychiatry. 1989;46(9):837–844. PubMed doi:10.1001/archpsyc.1989.01810090079011
10. Even C, Schröder CM, Friedman S, et al. Efficacy of light therapy in nonseasonal depression: a systematic review. J Affect Disord. 2008;108(1-2):11–23. PubMed doi:10.1016/j.jad.2007.09.008
11. Golden RN, Gaynes BN, Ekstrom RD, et al. The efficacy of light therapy in the treatment of mood disorders: a review and meta-analysis of the evidence. Am J Psychiatry. 2005;162(4):656–662. PubMed doi:10.1176/appi.ajp.162.4.656
12. Oldham MA, Ciraulo DA. Use of bright light therapy among psychiatrists in Massachusetts: an e-mail survey. Prim Care Companion CNS Disord. 2014;16(3):PCC.14m01637. PubMed
13. Beauchemin KM, Hays P. Phototherapy is a useful adjunct in the treatment of depressed in-patients. Acta Psychiatr Scand. 1997;95(5):424–427. PubMed doi:10.1111/j.1600-0447.1997.tb09656.x
14. Loving RT, Kripke DF, Shuchter SR. Bright light augments antidepressant effects of medication and wake therapy. Depress Anxiety. 2002;16(1):1–3. PubMed doi:10.1002/da.10036
15. Dauphinais DR, Rosenthal JZ, Terman M, et al. Controlled trial of safety and efficacy of bright light therapy vs negative air ions in patients with bipolar depression. Psychiatry Res. 2012;196(1):57–61. PubMed doi:10.1016/j.psychres.2012.01.015
16. Wu JC, Kelsoe JR, Schachat C, et al. Rapid and sustained antidepressant response with sleep deprivation and chronotherapy in bipolar disorder. Biol Psychiatry. 2009;66(3):298–301. PubMed doi:10.1016/j.biopsych.2009.02.018
17. Prasko J, Horacek J, Klaschka J, et al. Bright light therapy and/or imipramine for inpatients with recurrent non-seasonal depression. Neuroendocrinol Lett. 2002;23(2):109–113. PubMed
18. Lieverse R, Van Someren EJW, Nielen MMA, et al. Bright light treatment in elderly patients with non-seasonal major depressive disorder. Arch Gen Psychiatry. 2011;68:61–70. PubMed doi:10.1001/archgenpsychiatry.2010.183
19. Martiny K, Lunde M, Undén M, et al. Adjunctive bright light in non-seasonal major depression: results from clinician-rated depression scales. Acta Psychiatr Scand. 2005;112(2):117–125. PubMed doi:10.1111/j.1600-0447.2005.00574.x
20. Leibenluft E, Turner EH, Feldman-Naim S, et al. Light therapy in patients with rapid cycling bipolar disorder: preliminary results. Psychopharmacol Bull. 1995;31(4):705–710. PubMed
21. Lam RW, Levitt AJ, Levitan RD, et al. Efficacy of bright light treatment, fluoxetine, and the combination in patients with nonseasonal major depressive disorder: a randomized clinical trial. JAMA Psychiatry. 2016;73(1):56–63. PubMed doi:10.1001/jamapsychiatry.2015.2235
22. Güzel Özdemir P, Boysan M, Smolensky MH, et al. Comparison of venlafaxine alone versus venlafaxine plus bright light therapy combination for severe major depressive disorder. J Clin Psychiatry. 2015;76(5):e645–e654. PubMed doi:10.4088/JCP.14m09376
23. Lipsey MW, Wilson DB. Applied Social Research Methods: Practical Meta-Analysis. Vol 49. London, UK: Sage Publications; 2000.
24. Hedges LV. Distribution theory for Glass’s estimator of effect size and related estimators. J Educ Stat. 1981;6:107–128. doi:10.2307/1164588
25. R Core Team. R: a language and environment for statistical computing. Vienna, Austria. 2014. R Foundation for Statistical Computing Web site. http://www.R-project.org/. Accessed September 6, 2016.
26. Viechtbauer W. Conducting meta-analyses in R with the metafor package. J Stat Softw. 2010;36(3):1–48. doi:10.18637/jss.v036.i03
27. Begg CB, Mazumdar M. Operating characteristics of a rank correlation test for publication bias. Biometrics. 1994;50(4):1088–1101. PubMed doi:10.2307/2533446
28. Guyatt G, Oxman AD, Akl EA, et al. GRADE guidelines, 1: introduction-GRADE evidence profiles and summary of findings tables. J Clin Epidemiol. 2011;64(4):383–394. PubMed doi:10.1016/j.jclinepi.2010.04.026
29. American Psychiatric Association. Practice Guideline for the Treatment of Patients with Major Depressive Disorder. 3rd Edition. American Washington DC: Psychiatric Association; 2010. https://psychiatryonline.org/pb/assets/raw/sitewide/practice_guidelines/guidelines/mdd.pdf. Accessed September 19, 2016.
30. Perera S, Eisen R, Bhatt M, et al. Light therapy for non-seasonal depression: systematic review and meta-analysis. BJPsych Open. Mar 2016;2(2):116–126. doi:10.1192/bjpo.bp.115.001610
Enjoy this premium PDF as part of your membership benefits!




